Multidirectional Instability (MDI) of the Shoulder: Anatomy, Biomechanics & Management
Key Takeaway
Multidirectional Instability (MDI) of the shoulder is symptomatic laxity in two or more directions (anterior, posterior, inferior) of the glenohumeral joint. Unlike traumatic instability, MDI often arises insidiously from factors like generalized ligamentous laxity, repetitive microtrauma, or neuromuscular dyscoordination, leading to global capsular redundancy and excessive humeral head translation.
Multidirectional Instability (MDI): Spot & Treat Shoulder Instability
Introduction & Epidemiology
Multidirectional instability (MDI) of the glenohumeral joint is a complex clinical entity characterized by symptomatic laxity in two or more directions (anterior, posterior, inferior). Unlike unidirectional instability, which often results from a distinct traumatic event causing a clear capsulolabral tear, MDI frequently presents without a significant initiating macrotrauma. It typically develops insidiously, often due to repetitive microtrauma, generalized ligamentous laxity, or neuromuscular dyscoordination.
The prevalence of MDI is challenging to quantify precisely, as it exists on a spectrum from asymptomatic laxity to debilitating instability. It is most commonly observed in young, active individuals, particularly those involved in overhead sports such such as swimming, gymnastics, and throwing, where repetitive microtrauma can lead to capsular stretching and inadequate muscular stabilization. Females are often disproportionately affected due to a higher incidence of generalized ligamentous laxity. While some patients present with a history of minor trauma or repetitive overhead activities, others have no identifiable cause beyond inherent connective tissue predispositions. The hallmark is the subjective sensation of instability or pain associated with specific positions or activities, often accompanied by demonstrable glenohumeral translation during clinical examination.
Surgical Anatomy & Biomechanics
A comprehensive understanding of shoulder anatomy and biomechanics is critical for managing MDI. The glenohumeral joint, often likened to a golf ball on a tee, relies heavily on soft tissue restraints for stability, given the inherent bony incongruity between the large humeral head and the shallow glenoid fossa.
Key Anatomical Stabilizers:
-
Static Stabilizers:
- Glenoid Labrum: A fibrocartilaginous ring that deepens the glenoid fossa, increasing the contact area and providing an attachment site for the glenohumeral ligaments and joint capsule. In MDI, the labrum is typically intact, or any minor fraying is secondary to chronic subluxation rather than a primary traumatic detachment (e.g., Bankart lesion).
-
Glenohumeral Ligaments (GHLs):
These are thickenings of the anterior capsule.
- Superior Glenohumeral Ligament (SGHL): Contributes to stability with the arm adducted and externally rotated.
- Middle Glenohumeral Ligament (MGHL): Important for anterior stability, especially with the arm abducted 45 degrees.
- Inferior Glenohumeral Ligament (IGHL) Complex: The primary static stabilizer against anterior, posterior, and inferior translation when the arm is abducted above 45 degrees. It consists of an anterior band, a posterior band, and an intervening axillary pouch. Redundancy or attenuation of the IGHL complex is frequently implicated in MDI.
- Joint Capsule: The primary structure affected in MDI. It is typically globally redundant or attenuated, allowing for excessive translation in multiple directions. The volume of the capsule is often increased.
- Negative Intra-articular Pressure: Contributes to static stability by creating a suction effect, resisting distraction.
- Glenoid Version: Retroversion of the glenoid can predispose to posterior instability, while anteversion can contribute to anterior instability.
-
Dynamic Stabilizers:
- Rotator Cuff Muscles (Supraspinatus, Infraspinatus, Teres Minor, Subscapularis): These muscles provide concavity-compression, actively compressing the humeral head into the glenoid fossa during movement. Their coordinated contraction contributes significantly to dynamic stability, particularly during overhead activities. Weakness or dyscoordination can exacerbate MDI.
- Scapular Stabilizers (Trapezius, Rhomboids, Serratus Anterior, Levator Scapulae): Provide a stable base for glenohumeral motion. Scapular dyskinesis is a common finding in MDI and contributes to altered glenohumeral mechanics.
- Long Head of the Biceps: While often debated, it can contribute to superior stability and modest anterior stability, especially in specific positions.
Biomechanics of MDI:
The pathophysiology of MDI typically involves a global increase in capsular volume and laxity, leading to insufficient passive constraint. This allows the humeral head to translate excessively on the glenoid, causing pain, apprehension, and/or symptomatic subluxation. The exact etiology is often multifactorial, including:
*
Generalized Ligamentous Laxity:
Patients often exhibit signs of hypermobility in other joints (e.g., elbow hyperextension, thumb-to-forearm apposition), as assessed by the Beighton score.
*
Repetitive Microtrauma:
Overuse in overhead activities can gradually stretch the capsule and ligaments.
*
Neuromuscular Imbalance:
Poor coordination or weakness of the rotator cuff and scapular periscapular muscles can compromise dynamic stability, allowing the static restraints to bear excessive load and eventually stretch.
*
Connective Tissue Disorders:
Ehlers-Danlos syndrome, Marfan syndrome, and other conditions can lead to inherent tissue laxity.
The characteristic clinical finding is often a positive sulcus sign (inferior instability), combined with apprehension or symptomatic translation in anterior and/or posterior directions. Unlike traumatic instability, significant bony defects (e.g., Hill-Sachs, bony Bankart) are less common in MDI, although chronic microtrauma can eventually lead to glenoid erosion or labral fraying. The goal of treatment, both conservative and surgical, is to restore a harmonious balance between the static and dynamic stabilizers, reducing capsular volume and enhancing neuromuscular control.
Indications & Contraindications
The management of MDI is predominantly non-operative initially, with surgery reserved for carefully selected patients who fail a comprehensive rehabilitation program.
Indications for Non-Operative Management:
- Primary Treatment Strategy: Non-operative management is the first-line approach for virtually all patients with MDI.
-
Emphasis on Rehabilitation:
A dedicated and supervised physical therapy program is crucial, focusing on:
- Proprioception and Neuromuscular Control: Retraining the dynamic stabilizers to function effectively.
- Rotator Cuff Strengthening: Enhancing concavity-compression.
- Scapular Stabilization: Improving the base of support for glenohumeral motion.
- Core Strengthening: Indirectly supports shoulder girdle mechanics.
- Activity Modification: Avoiding positions and activities that provoke symptoms.
- Patient Education: Understanding the condition and the importance of compliance with the rehabilitation protocol.
- Successful Conservative Course: Patients who achieve satisfactory pain control and functional stability with non-operative measures.
Indications for Operative Management:
- Failure of Extensive Non-Operative Management: This is the primary indication. Typically, a minimum of 6 to 12 months of high-quality, supervised physical therapy should be completed without significant improvement in symptoms or function. The duration may be shorter in high-demand athletes with debilitating symptoms affecting their careers.
- Recurrent Symptomatic Subluxation/Dislocation: Despite maximal conservative efforts, patients continue to experience episodes of instability that significantly impact their quality of life or ability to perform daily activities/sports.
- Specific Patient Cohorts: Certain athletes (e.g., overhead throwing athletes with posterior MDI and internal impingement) may have specific anatomical or biomechanical issues that warrant earlier surgical consideration if rehab fails.
- Progressive Degenerative Changes: Although rare, long-standing MDI with chronic microtrauma could potentially lead to glenoid erosion or early arthrosis, which may prompt surgical intervention.
Contraindications for Operative Management:
- Adequate Response to Non-Operative Treatment: If the patient is stable and functional with conservative care, surgery is unnecessary.
- Poor Surgical Candidate: Significant medical comorbidities that preclude safe anesthesia or surgery.
- Unrealistic Patient Expectations: Patients who expect a complete "cure" or immediate return to high-level activity without a commitment to post-operative rehabilitation.
- Psychological Morbidities: Undiagnosed or poorly managed psychological conditions (e.g., somatization, anxiety, depression) can negatively impact surgical outcomes and compliance.
- Non-Compliance with Rehabilitation: Historically, patients with poor compliance in the non-operative phase are likely to be non-compliant post-operatively, leading to poor outcomes.
- Active Infection: Absolute contraindication.
- Primary Unidirectional Traumatic Instability: While MDI can have a traumatic component, surgery for classic traumatic unidirectional instability (e.g., isolated Bankart lesion) follows different principles (labral repair). However, some MDI cases may have a dominant direction of instability along with generalized laxity.
Table 1: Operative vs. Non-Operative Indications for MDI
| Feature/Criterion | Non-Operative Management | Operative Management |
|---|---|---|
| Primary Approach | First-line treatment for nearly all MDI patients. | Reserved for failure of thorough non-operative care. |
| Duration of Rehab | Minimum 6-12 months of structured, supervised therapy. | After 6-12 months of failed intensive rehabilitation. |
| Symptom Resolution | Achieving functional stability and pain control. | Persistent, debilitating symptoms despite rehab. |
| Instability Episodes | Reduced frequency or severity of subluxation/apprehension. | Recurrent symptomatic subluxations/dislocations. |
| Patient Commitment | High compliance with exercise and activity modification. | Commitment to demanding post-operative rehabilitation. |
| Associated Pathology | Isolated capsular laxity, intact labrum. | May consider if specific associated lesions are noted. |
| General Health | Good general health, suitable for physical activity. | Good surgical candidate, acceptable anesthetic risk. |
| Psychological Factors | Stable, realistic expectations. | Stable, realistic expectations, no significant comorbidities. |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is paramount for successful MDI surgery, encompassing thorough patient evaluation, appropriate imaging, and meticulous surgical setup.
Pre-Operative Planning:
-
History and Physical Examination:
- History: Detailed history of onset, duration, nature of symptoms (pain, apprehension, clunking, giving way), aggravating and alleviating factors, previous treatments, and impact on daily life and sports. Document any history of trauma, but acknowledge MDI often lacks a significant traumatic event.
-
Physical Exam:
- Generalized Ligamentous Laxity: Assess Beighton score (thumb to forearm, elbow/knee hyperextension, spinal flexion, fifth MCP hyperextension). A score ≥4/9 indicates generalized laxity.
-
Glenohumeral Instability Tests:
- Sulcus Sign: Assesses inferior laxity. Grasp the forearm, apply inferior traction. A visible sulcus or dimple below the acromion and measurement of the distance (e.g., >2 cm is significant) indicates inferior laxity.
- Apprehension Test (Anterior/Posterior): Identifies directional instability. For anterior, abduct and externally rotate the arm. For posterior, flex and internally rotate with a posterior load. A positive test elicits a sensation of impending subluxation or pain.
- Relocation Test (Jobe's Test): Often performed after a positive apprehension test. While maintaining the provocative position, apply a posterior force to the humeral head. Reduction of apprehension or pain suggests instability.
- Load and Shift Test: Assesses anterior, posterior, and inferior translation with the patient supine or seated. The examiner loads the humeral head into the glenoid and then translates it anteriorly, posteriorly, and inferiorly, noting the degree of translation (Grade 0: no translation; Grade 1: humeral head rides up glenoid rim but reduces; Grade 2: humeral head over the rim but spontaneously reduces; Grade 3: humeral head remains dislocated).
- Rotator Cuff and Scapular Strength: Assess for weaknesses or imbalances that might contribute to dynamic instability.
-
Imaging Studies:
- Standard Radiographs: AP, scapular Y, and axillary views to rule out bony abnormalities (fractures, glenoid dysplasia, significant bony defects like Hill-Sachs or glenoid bone loss, which are less common in MDI but should be excluded).
- Magnetic Resonance Imaging (MRI) / Magnetic Resonance Arthrography (MRA): Essential for evaluating soft tissue structures. MRA is superior for visualizing the labrum and subtle capsular abnormalities. It helps to rule out labral tears (e.g., SLAP lesions), rotator cuff pathology, or occult ganglion cysts that might mimic or contribute to instability. In MDI, the capsule may appear globally redundant or attenuated, but there is typically no discrete capsulolabral avulsion as seen in traumatic instability.
- Computed Tomography (CT) Scan: Rarely indicated unless significant bony abnormalities are suspected or for precise measurements of glenoid version or bone loss if revision surgery or open reconstruction is contemplated.
Patient Positioning:
Two primary positions are used for shoulder arthroscopy:
-
Beach Chair Position (Semi-Fowler):
-
Advantages:
- Anatomically familiar orientation for the surgeon.
- Easier conversion to an open procedure if necessary.
- Better visualization of anterior and superior structures.
- Lower risk of brachial plexus neuropathy compared to lateral decubitus.
- Allows for easy access to the entire circumference of the glenoid for capsular plication.
-
Setup:
- Patient is semi-recumbent, typically at a 60-70 degree angle.
- Head secured in a headrest (e.g., "donut" or Mayfield clamp) to prevent movement and protect the cervical spine.
- Torso secured to the operating table with a chest strap.
- Operative arm draped free. The non-operative arm is tucked or placed on an arm board.
- A specialized arm holder (e.g., Spider arm holder) or a limb positioner may be used to allow dynamic manipulation of the arm during arthroscopy.
- Ensure adequate padding to all pressure points, especially the contralateral elbow, sacrum, and heels.
- Careful monitoring of blood pressure, as the beach chair position can cause orthostatic hypotension.
-
Advantages:
-
Lateral Decubitus Position:
-
Advantages:
- Allows for controlled traction on the operative arm, which can aid in joint distraction and visualization, particularly for posterior structures.
- May be preferred by some surgeons for specific posterior instability repairs.
-
Disadvantages:
- Higher risk of traction-related neuropathy (brachial plexus, ulnar nerve).
- More complex patient positioning and securing.
- Less familiar anatomical orientation for some surgeons.
-
Setup:
- Patient positioned on their side with the operative arm superior.
- Axillary roll placed inferior to the dependent axilla to protect the brachial plexus.
- Torso secured to the table with straps.
- Operative arm suspended in traction (e.g., 10-15 lbs of weight) in 70-90 degrees of abduction and 15-20 degrees of forward flexion.
- Padding for all dependent bony prominences.
-
Advantages:
For MDI, the beach chair position is generally preferred by many surgeons as it allows excellent global access to the capsule for plication and avoids the traction-related risks.
Regional Anesthesia:
- Interscalene brachial plexus block is often used in conjunction with general anesthesia to provide excellent post-operative pain control and facilitate early rehabilitation.
- The block should be administered prior to positioning to avoid discomfort.
Detailed Surgical Approach / Technique
The primary surgical technique for MDI is arthroscopic capsular plication or shift. This procedure aims to reduce the overall volume of the joint capsule, thereby tightening the redundant capsular tissue and restoring glenohumeral stability. Thermal capsulorrhaphy has largely been abandoned due to high failure rates and potential for chondrolysis.
1. Patient Preparation and Portals:
- Sterile Prep and Drape: Standard sterile preparation of the shoulder and arm.
- Anatomical Landmarks: Identify the acromion, coracoid, and glenoid spine. Mark the planned portal sites.
-
Standard Portals:
- Posterior Portal (Standard): Typically 2-3 cm inferior and 1 cm medial to the posterior aspect of the acromion. This is the primary viewing portal.
- Anterosuperior Portal: Created under direct arthroscopic visualization. Lateral to the coracoid process, usually above the subscapularis tendon. Used for instrumentation and anchor placement.
- Anteroinferior Portal (5 o'clock for right shoulder): Also created under direct visualization. Inferior to the subscapularis tendon, typically 1 cm lateral to the anterior glenoid rim. Critical for working on the inferior capsule.
- Accessory Portals: May include a far posterior lateral portal for better visualization of the anterior capsule or additional anterior portals as needed.
2. Diagnostic Arthroscopy:
-
Perform a systematic diagnostic arthroscopy through the posterior portal to evaluate all intra-articular structures:
- Rotator Cuff: Assess integrity of supraspinatus, infraspinatus, subscapularis.
- Biceps Tendon and Anchor: Evaluate for fraying, tears (e.g., SLAP lesion).
- Labrum: Inspect the entire labrum circumferentially. In MDI, the labrum is usually intact or shows only mild fraying. Rule out specific traumatic tears (Bankart, reverse Bankart).
- Glenoid and Humeral Head Articular Cartilage: Assess for chondral lesions.
- Joint Capsule: Critically assess capsular laxity and redundancy, particularly the inferior capsular pouch (axillary recess). Provocative testing under arthroscopic visualization (e.g., manipulating the arm to demonstrate excessive translation) helps confirm the extent and direction of instability. Confirm the presence of generalized capsular redundancy.
3. Capsular Plication / Shift Technique:
The goal is to reduce the volume of the capsule by plicating or folding the redundant tissue. This is typically achieved using suture anchors placed along the glenoid rim. The plication sequence addresses the most symptomatic direction first, but often involves inferior, anterior, and posterior components.
A. Inferior Capsular Plication (Key for MDI):
- Debridement/Preparation: Debride any loose tissue or synovitis from the inferior capsule and glenoid neck to prepare for anchor placement. A shaver or radiofrequency ablator can be used for this.
-
Anchor Placement:
- Working from the anterosuperior or anteroinferior portal, introduce a suture anchor guide system.
- Place 2-3 suture anchors along the inferior glenoid neck, just medial to the articular cartilage (typically at the 4, 5, and 6 o'clock positions for a right shoulder). Use non-absorbable or long-term absorbable anchors.
- Each anchor will have two sutures.
-
Capsular Capture and Plication:
- Using a suture passer (e.g., BirdBeak, Scorpion), capture a generous amount of the redundant inferior capsule with one limb of the suture from the most inferior anchor. The goal is to gather a "fold" of capsule.
- Pass the captured tissue more medially and superiorly, then tie the knot, effectively tightening the inferior pouch and shifting it superiorly.
- Repeat this process for the remaining sutures and anchors, creating a continuous plication that reduces the inferior capsular volume. Ensure sutures are tied securely, but not excessively tight, to avoid stiffness. A common strategy involves plicating from inferior to superior, or from the symptomatic direction towards the asymptomatic.

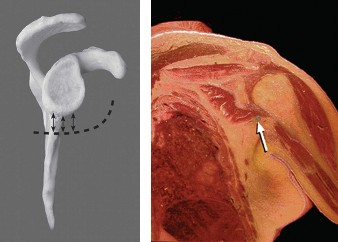
Figure 1: Arthroscopic view demonstrating suture anchor placement and initial capsular tissue capture for inferior glenohumeral ligament (IGHL) plication.
B. Anterior Capsular Plication:
- Anchor Placement: Place 1-2 suture anchors along the anterior glenoid neck (e.g., 2 and 3 o'clock positions).
- Capsular Capture and Plication: Capture the redundant anterior capsule with sutures and plicate it. The goal is to tighten the anterior band of the IGHL and MGHL, reducing anterior translation.
C. Posterior Capsular Plication:
- Anchor Placement: Place 1-2 suture anchors along the posterior glenoid neck (e.g., 7 and 8 o'clock positions).
- Capsular Capture and Plication: Capture the redundant posterior capsule with sutures and plicate it, tightening the posterior band of the IGHL and posterior capsule, reducing posterior translation. This may require a separate posterior working portal.
4. Intra-operative Assessment of Stability:
- After completing the plication, remove all instruments and arthroscope.
- Dynamically assess glenohumeral stability under fluoroscopic or direct visualization.
- Perform translation tests (anterior, posterior, inferior) to ensure a firm endpoint in all directions.
- Check for the absence of the sulcus sign.
- Perform gentle range of motion (ROM) to confirm that the shoulder is stable but not overtly stiff. The goal is a "goldilocks" tension – not too loose, not too tight.
5. Closure:
- Remove instruments.
- Close portal sites with simple sutures or sterile strips.
- Apply a sterile dressing.
- Place the arm in a sling, often with an abduction pillow or specific positioning to protect the repair (e.g., neutral rotation).
Complications & Management
While generally safe, arthroscopic capsular plication for MDI is associated with potential complications, which orthopedic surgeons must be prepared to identify and manage.
Table 2: Common Complications, Incidence, and Salvage Strategies
| Complication | Estimated Incidence | Salvage Strategies |
|---|---|---|
| Stiffness / Loss of ROM | 10-20% (most common) | Aggressive physical therapy, stretching, NSAIDs. If refractory, manipulation under anesthesia. Rarely, arthroscopic capsular release. Prevention: Avoid overtightening. |
| Recurrent Instability / Failure | 5-15% (can be higher in hyperlax patients) | Intensive rehabilitation. Revision surgery (arthroscopic plication, possible open capsular shift, Latarjet for significant bone loss if misdiagnosed as MDI). Consider allograft/autograft for poor tissue quality. |
| Neurovascular Injury | <1% (rare but severe) |
Axillary Nerve:
Observation, EMG/NCS. Nerve grafting if severe deficit.
Musculocutaneous Nerve: Observation, EMG/NCS. Brachial Plexus: Observation, EMG/NCS. Vascular: Direct repair, ligature. |
| Infection | <1% | Surgical debridement, irrigation, antibiotics. Retained hardware removal if persistent. |
| Persistent Pain | Variable (5-10%) | Rule out underlying pathology (e.g., missed labral tear, chondral injury, hardware irritation). Physical therapy, pain management. Rarely, revision surgery. |
| Chondrolysis | Rare | Primarily associated with thermal capsulorrhaphy. Salvage involves arthroplasty (hemiarthroplasty, TSA) for advanced cases. |
| Hardware-Related Issues | <1% (suture irritation, anchor migration) | Hardware removal if symptomatic. |
| CRPS (Complex Regional Pain Syndrome) | Rare (<1%) | Early recognition, sympathetic blocks, physical therapy, pain management. |
| Adhesive Capsulitis | 2-5% | See Stiffness/Loss of ROM. Distinguish from surgical overtightening. |
Detailed Management Strategies:
-
Stiffness / Loss of Range of Motion:
- Prevention: The most critical step is avoiding overtightening the capsule during surgery. Intra-operative dynamic assessment of stability and ROM is crucial.
-
Management:
- Early: Aggressive, supervised physical therapy focusing on regaining motion. NSAIDs.
- Late / Refractory: If stiffness persists beyond 3-6 months despite dedicated therapy, manipulation under anesthesia (MUA) may be considered. Care must be taken to avoid fracture or detachment of the repair.
- Severe: Rarely, arthroscopic capsular release may be required if MUA fails, but this risks compromising the previous plication.
-
Recurrent Instability / Failure:
- Etiology: Can result from undertightening, inadequate rehabilitation, severe underlying generalized ligamentous laxity, or subsequent trauma.
-
Management:
- Conservative: If symptoms are mild, a repeat course of intensive physical therapy may be beneficial.
-
Revision Surgery:
If significant symptomatic instability persists, revision surgery is indicated. This may involve:
- Repeat Arthroscopic Plication: If the initial plication was deemed insufficient.
- Open Capsular Shift: Historically, this was the gold standard for MDI and may be considered for revision cases, especially if capsular tissue quality is poor or a more robust repair is desired. This allows for direct visualization and precise tissue handling.
- Augmentation: In cases of extremely poor tissue quality or severe hyperlaxity, augmentation with allograft tissue (e.g., Achilles tendon) may be considered, but this is a complex and less common approach.
- Bony Procedures: While rare for primary MDI, if significant glenoid bone loss is identified (which would suggest a misdiagnosis of true MDI, and rather a chronic traumatic instability), a Latarjet procedure or glenoid bone grafting may be necessary.
-
Neurovascular Injury:
- Axillary Nerve: Most commonly at risk due to its proximity to the inferior capsule and glenoid neck. Injury can occur during anchor placement or aggressive capsular release.
- Musculocutaneous Nerve: At risk during anterosuperior portal placement.
- Prevention: Careful portal placement under direct visualization, awareness of anatomical danger zones, and precise instrument handling.
- Management: For neurapraxia, observation, electrodiagnostic studies (EMG/NCS) at 3-6 weeks to assess nerve function. Surgical exploration and nerve grafting may be necessary for complete transections, though extremely rare.
-
Infection:
- Prevention: Strict aseptic technique, prophylactic antibiotics.
- Management: Early detection is key. Superficial infections may respond to oral antibiotics. Deep intra-articular infection requires urgent surgical debridement, thorough irrigation, and intravenous antibiotics. Hardware removal may be necessary if the infection persists.
-
Persistent Pain:
- Etiology: Can be multifactorial: incomplete resolution of instability, capsular inflammation, missed concomitant pathology (e.g., chondral lesion, labral fraying), impingement, or hardware irritation.
- Management: Thorough diagnostic work-up including repeat imaging. Symptomatic management with physical therapy and pain medications. Arthroscopic débridement or hardware removal if indicated.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as crucial as the surgery itself for achieving successful outcomes in MDI repair. The protocol is typically conservative and prolonged, emphasizing protection of the repair while gradually restoring motion, strength, and neuromuscular control. Individualized adjustments are frequently necessary based on the extent of surgical repair, tissue quality, and patient-specific factors (e.g., generalized laxity).
Phase 1: Protection and Early Motion (Weeks 0-6)
-
Goals:
- Protect the capsular plication/shift.
- Minimize pain and inflammation.
- Initiate gentle range of motion without stressing the repair.
- Maintain integrity of the repair.
-
Immobilization:
- Sling immobilization, often with an abduction pillow, for 3-6 weeks. The exact duration depends on surgeon preference, intra-operative findings (extent of laxity, number of plications), and patient compliance. For MDI, a longer period of immobilization in neutral rotation (e.g., 4-6 weeks) is common.
- Patient education on proper sling wear and hygiene.
-
Exercises (Passive/Active-Assistive):
-
Weeks 0-3:
- Pendulum exercises: Gentle, gravity-assisted circular motions (passive).
- Scapular setting exercises: Gentle isometric contractions of scapular retractors without glenohumeral motion.
- Elbow, wrist, hand ROM exercises: To prevent stiffness in uninvolved joints.
- Ice and pain medication: As needed for swelling and pain.
-
Weeks 3-6 (Gradual progression):
- Passive Range of Motion (PROM): Initiated by a therapist within protected arcs. Avoid end-range external rotation, abduction, and extension. The exact limits are surgeon-specific (e.g., ER to 0-30 degrees, flexion to 90-120 degrees).
- Active-Assisted Range of Motion (AAROM): Progress from PROM using a wand or the uninvolved arm.
- Isometrics: Gentle rotator cuff and periscapular isometrics in neutral rotation. No resisted movements.
-
Weeks 0-3:
-
Precautions:
- NO active glenohumeral elevation, abduction, or external rotation.
- Avoid combined positions that stress the repair (e.g., abduction + external rotation).
- No lifting, pushing, or pulling with the affected arm.
Phase 2: Intermediate Motion and Early Strengthening (Weeks 6-12)
-
Goals:
- Gradually restore full pain-free range of motion.
- Initiate light strengthening of rotator cuff and scapular stabilizers.
- Improve neuromuscular control.
-
Exercises:
- Full AROM: Progress to active range of motion, working towards full flexion, abduction, and rotation (as tolerated).
-
Rotator Cuff Strengthening:
- Isometric exercises with increasing resistance.
- Light elastic band exercises for internal and external rotation, scapular retraction, and abduction (e.g., sidelying ER, standing IR/ER).
- Scapular Stabilization: Progress scapular protraction/retraction exercises (e.g., push-up plus), rows, seated press-ups.
- Proprioceptive Exercises: Closed-chain exercises (e.g., wall slides, weight shifts) to enhance joint awareness.
-
Precautions:
- Avoid heavy lifting or sudden, uncontrolled movements.
- No overhead activities involving resistance.
- Continue to protect against sudden external rotation and abduction.
Phase 3: Advanced Strengthening and Proprioception (Weeks 12-24)
-
Goals:
- Achieve full strength of the rotator cuff and periscapular muscles.
- Enhance dynamic stability and proprioception.
- Prepare for return to specific activities or sports.
-
Exercises:
- Progressive Resistance Training: Increase intensity and resistance for rotator cuff and scapular muscles. Include exercises like overhead press (light), rows, lat pulldowns, shoulder shrugs.
- Plyometrics/Sport-Specific Drills: For athletes, introduce controlled plyometric exercises (e.g., medicine ball throws) and sport-specific movements (e.g., throwing mechanics, swimming strokes) at low intensity.
- Advanced Proprioception: Unstable surface training (e.g., wobble board, Bosu ball), rhythmic stabilization drills.
- Core Strengthening: Continue to emphasize trunk stability as it impacts shoulder function.
-
Precautions:
- Listen to pain. Do not push into pain.
- Gradual progression of resistance and intensity.
- Avoid uncontrolled ballistic movements.
Phase 4: Return to Sport / Activity (Weeks 24+)
-
Goals:
- Gradual and safe return to full activity or sport.
- Maintain strength and flexibility.
- Prevent re-injury.
-
Return to Activity:
- Requires successful completion of functional testing, demonstration of full pain-free ROM, and adequate strength compared to the contralateral side.
- Sport-specific return-to-play protocol with gradual increase in intensity, duration, and complexity.
- For throwing athletes, interval throwing programs are crucial.
-
Maintenance:
- Continue a regular exercise program focusing on shoulder and core strength, flexibility, and proprioception.
Key Considerations for MDI Rehabilitation:
- Individualization: Protocols must be tailored. Patients with generalized ligamentous laxity may require a slower progression and longer protection phase.
- Neuromuscular Control: Emphasis on motor control and proprioception is critical, as MDI often involves dynamic instability.
- Scapular Dyskinesis: Address any scapular dyskinesis throughout all phases.
- Patient Education: Constant reinforcement of proper body mechanics, activity modification, and adherence to the rehabilitation plan is essential. Non-compliance is a significant risk factor for failure.
Summary of Key Literature / Guidelines
The surgical management of multidirectional instability has evolved significantly, moving from open capsular shifts to predominantly arthroscopic techniques. Understanding the current evidence base is crucial for informed clinical decision-making.
Evolution of Surgical Techniques:
- Open Inferior Capsular Shift (ICS): Historically considered the gold standard. Developed by Neer and Foster, it involves detaching the inferior capsule and plicating it superiorly and medially. While effective, it carries higher morbidity, including a larger incision, increased post-operative pain, and a higher risk of stiffness compared to arthroscopic methods. Results generally showed good stability rates (80-90%) but with a higher incidence of ROM loss.
- Arthroscopic Plication/Capsular Shift: With advancements in arthroscopic instrumentation and techniques, arthroscopic capsular plication has become the preferred method for MDI. It offers the advantages of smaller incisions, less pain, and faster initial recovery while achieving comparable stability outcomes to open techniques in well-selected patients. The technique involves systematically reducing capsular volume by plicating the redundant capsule onto the glenoid neck using suture anchors, often addressing the inferior, anterior, and posterior aspects.
Key Findings from Literature:
-
Efficacy of Arthroscopic Plication:
Numerous studies report good to excellent outcomes with arthroscopic capsular plication for MDI, with stability rates generally ranging from 70% to 90%. However, results can be more variable in patients with extreme generalized ligamentous laxity or those with significant psychological factors.
- A systematic review by Lo and Burkhart (2004) highlighted the importance of a comprehensive arthroscopic approach, addressing all planes of instability, and emphasized that careful patient selection and a dedicated post-operative rehabilitation program are paramount.
- Mair et al. (2004) published a series demonstrating good results with arthroscopic MDI repair in a mixed cohort, noting that consistent results depended on meticulous technique.
- Impact of Generalized Ligamentous Laxity: Patients with a high Beighton score or other signs of generalized hypermobility tend to have slightly less predictable outcomes and potentially higher recurrence rates after capsular plication. Some surgeons may advocate for more aggressive capsular tightening or consider open techniques in select cases, though this remains debated. Counseling these patients regarding realistic expectations is critical.
- Comparison to Thermal Capsulorrhaphy: Thermal capsulorrhaphy, once popular, has been largely abandoned due to high rates of recurrence and the potential for chondrolysis and joint stiffness. This technique used heat to shrink the collagen fibers of the capsule, but the long-term integrity of the denatured tissue was poor, and the thermal damage could lead to severe irreversible cartilage damage.
- Role of Rehabilitation: All literature unequivocally emphasizes the critical role of a prolonged, structured, and supervised physical therapy program, both pre-operatively and post-operatively. Failure of non-operative management is the primary surgical indication, and meticulous post-operative rehabilitation is crucial for allowing the capsular repair to heal and for restoring dynamic stabilization.
- Long-term Outcomes: Long-term follow-up studies generally show durable results for arthroscopic plication, though some patients may experience mild residual stiffness or occasional mild symptoms. Progression to significant glenohumeral arthrosis directly attributable to the plication is uncommon if overtightening is avoided.
Current Guidelines and Consensus:
-
AAOS (American Academy of Orthopaedic Surgeons) Guidelines:
While specific MDI guidelines can be broad, the general consensus aligns with:
- Initial Non-Operative Treatment: A prolonged course of physical therapy (6-12 months) is the cornerstone.
- Surgical Indication: Reserved for patients with persistent, debilitating symptoms after failed comprehensive non-operative management.
- Preferred Surgical Approach: Arthroscopic capsular plication is generally preferred over open techniques for primary MDI due to reduced morbidity, while providing comparable stability outcomes.
- Emphasis on Rehabilitation: A critical component of successful outcomes.
- Shared Decision-Making: Given the multifactorial nature of MDI and potential for varied outcomes, shared decision-making with the patient, discussing the pros and cons of surgery, potential complications, and the demanding rehabilitation process, is essential.
In summary, arthroscopic capsular plication for MDI is a well-established and generally effective procedure for patients who have failed conservative management. Success hinges on precise surgical technique, thorough intra-operative assessment of stability, and strict adherence to a comprehensive post-operative rehabilitation program. While the results are often good, orthopedic surgeons must be mindful of the challenges posed by generalized ligamentous laxity and the potential for complications such as stiffness or recurrence.
