Comprehensive Guide to Fifth Metacarpal Neck Fractures: Anatomy, Biomechanics & Management
Key Takeaway
Fifth metacarpal neck fractures, or boxer's fractures, typically occur from axial loading on a clenched fist. They account for 10% of hand fractures, primarily affecting young adult males. The characteristic apex dorsal angulation results from extrinsic extensor tendon pull and intrinsic muscle forces on the distal fragment, alongside shortening from axial compression.
Introduction & Epidemiology
Fifth metacarpal neck fractures, commonly known as "boxer's fractures," represent a significant proportion of metacarpal injuries, accounting for approximately 10% of all hand fractures. They typically occur following an axial load applied to a clenched fist, often from punching a hard object. This mechanism results in a characteristic pattern of dorsal angulation at the fracture site due to the deforming forces of the interosseous and extrinsic extensor musculature.
Epidemiologically, these fractures are most prevalent in young adult males, aligning with the common mechanism of injury. While often considered benign, inappropriate management can lead to substantial functional impairment, including persistent pain, reduced grip strength, metacarpophalangeal (MCP) joint stiffness, and cosmetic deformity. Therefore, a thorough understanding of their anatomical, biomechanical, diagnostic, and treatment considerations is paramount for optimizing patient outcomes. The primary goals of management are to restore metacarpal length, alignment, and rotation, allowing for early functional rehabilitation.
Surgical Anatomy & Biomechanics
The fifth metacarpal forms the ulnar column of the hand and articulates proximally with the hamate and distally with the proximal phalanx of the little finger at the MCP joint. Its unique anatomy and surrounding soft tissues dictate the fracture patterns and deforming forces encountered in neck fractures.
Metacarpal Structure
- Base : Articulates with the hamate (a saddle-shaped joint, but functionally acts like a plane joint allowing limited motion) and the fourth metacarpal. This articulation is inherently stable due to strong interosseous ligaments.
- Shaft : The diaphysis is triangular to quadrangular in cross-section, providing attachment for intrinsic muscles.
- Neck : The most common site of fracture, located just proximal to the metaphyseal-diaphyseal junction. This region is relatively cancellous and often involved in comminution.
- Head : The distal articular surface that forms the MCP joint with the proximal phalanx. It is covered by articular cartilage and is crucial for MCP joint function.
Ligamentous & Tendinous Attachments
- Collateral Ligaments : Strong fibrous bands originating from the metacarpal head and inserting onto the base of the proximal phalanx and volar plate. They are taut in flexion and lax in extension, contributing significantly to MCP joint stability.
- Volar Plate : A thick fibrocartilaginous structure on the palmar aspect of the MCP joint, preventing hyperextension. It can become interposed in irreducible fractures.
- Extensor Tendons : The extensor digiti minimi (EDM) and the extensor digitorum communis (EDC) tendons course dorsally over the fifth metacarpal. Their dorsal position contributes to the deforming force causing dorsal angulation.
- Intrinsic Muscles : The hypothenar muscles (abductor digiti minimi, flexor digiti minimi brevis, opponens digiti minimi) originate from the hamate and metacarpal base, contributing to the pull on the metacarpal shaft. The interossei originate from the metacarpal shafts and insert into the proximal phalanges and extensor hoods; their oblique pull can contribute to shortening and rotational deformity.
Neurovascular Structures
- Dorsal Cutaneous Branch of the Ulnar Nerve : Courses over the dorsal and ulnar aspects of the fifth metacarpal, susceptible to injury during surgical dissection.
- Dorsal Venous System : A superficial network of veins that must be carefully preserved during surgical approaches to minimize swelling and improve wound healing.
- Digital Nerves and Vessels : Located volar to the metacarpal neck, requiring protection during fracture reduction and fixation.
Biomechanics of Injury & Deformity
The typical mechanism of direct axial loading with the MCP joint in flexion leads to a fracture through the neck. The deforming forces are critical to understand:
1.
Dorsal Angulation
: This is the hallmark deformity. The extrinsic extensor tendons (EDC, EDM) pull the proximal fragment dorsally, while the intrinsic muscles (interossei, hypothenar) and the flexor tendons pull the distal fragment (metacarpal head and proximal phalanx) volarly. This creates a flexion moment at the fracture site, resulting in apex dorsal angulation.
2.
Shortening
: The compressive axial load combined with the muscle pull (interossei) contributes to telescoping of the fracture fragments, leading to metacarpal shortening.
3.
Rotation
: Although less common than angulation, rotational deformity can occur and is poorly tolerated functionally. The fifth digit's natural cascade should maintain parallel alignment when making a fist. Rotational malunion results in scissoring or overlap of fingers during grasping. The hypothenar muscles can contribute to rotational forces on the distal fragment.
Acceptable Angulation & Biomechanical Implications
Historically, the fifth metacarpal neck fracture was considered to tolerate higher degrees of dorsal angulation (up to 40-70 degrees) compared to other metacarpals due to the greater physiological laxity and compensatory hyperextension available at the fifth MCP joint. However, modern understanding emphasizes that even in the fifth metacarpal, excessive angulation (>30-40 degrees, depending on patient factors and demands) can lead to:
* Prominence of the metacarpal head in the palm.
* Impaired grip strength.
* Mechanical impingement during MCP joint flexion.
* Cosmetic deformity.
* Reduced push-off strength.
Rotational deformity, even slight (5-10 degrees), is functionally devastating and universally considered an indication for anatomical reduction. Shortening exceeding 5-10 mm can also significantly impair grip strength and overall hand function.
Indications & Contraindications
The decision between non-operative and operative management for fifth metacarpal neck fractures hinges on a careful assessment of fracture characteristics, patient factors, and functional demands. The primary goal is to achieve a functional outcome with an acceptable range of motion, strength, and minimal pain.
Indications for Operative Management
Absolute Indications:
- Open Fractures : Any breach of the skin communicating with the fracture site (Gustilo-Anderson classification applies). Requires urgent debridement and fixation to prevent infection.
- Irreducible Fractures : Failure to achieve or maintain an acceptable reduction by closed means, often due to interposition of soft tissues (e.g., volar plate, extensor tendon, intrinsic muscle).
- Significant Rotational Deformity : Any detectable rotational malalignment (e.g., scissoring or overlap of the little finger when making a fist) which is poorly tolerated functionally.
- Concomitant Neurovascular Injury : Fractures associated with damage to major nerves or vessels requiring repair, which necessitates an open approach.
- Multiple Metacarpal Fractures : Especially if adjacent metacarpals are also fractured, potentially leading to a unstable hand architecture (e.g., in crush injuries).
- Loss of Reduction : Following an initial successful closed reduction and cast application.
Relative Indications:
- Excessive Dorsal Angulation : Generally, persistent dorsal angulation exceeding 30-40 degrees after closed reduction attempts. While some historical literature cited higher acceptable angulations for the fifth metacarpal, current practice often aims for more anatomical reduction, especially in high-demand patients. The exact threshold is patient-specific and influenced by age, hand dominance, occupation, and existing hand pathology.
- Significant Shortening : Persistent shortening greater than 5-10 mm.
- Associated Tendon/Ligament Injury : Particularly if the injury compromises MCP joint stability or function.
- Patient Demands : Athletes, manual laborers, or individuals requiring fine motor skills may benefit from more rigid fixation and earlier rehabilitation to minimize recovery time and maximize functional return.
- Polytrauma Patient : In patients with multiple injuries where early mobilization is desired for global rehabilitation.
- Delayed Presentation : With established malunion causing functional deficit or pain.
Contraindications for Operative Management
Absolute Contraindications:
- Active Infection : At the proposed surgical site, unless it's an open fracture requiring urgent debridement.
- Severe Systemic Comorbidities : Uncontrolled medical conditions that preclude safe anesthesia or surgical intervention.
Relative Contraindications:
- Minimally Displaced, Stable Fractures : That are amenable to closed reduction and immobilization within acceptable parameters.
- Patient Unwillingness/Non-compliance : Patients who cannot or will not adhere to post-operative rehabilitation protocols.
- Unrealistic Patient Expectations : Regarding surgical outcomes or recovery.
Table: Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Fracture Type | Closed, stable, minimally displaced, reducible | Open, irreducible, unstable, significant displacement/angulation/rotation |
| Dorsal Angulation | Typically ≤ 30-40 degrees (variable, up to 50-70 for 5th MC in older literature) | > 30-40 degrees (contemporary threshold), or progressive angulation |
| Shortening | ≤ 5 mm (some sources up to 10 mm for 5th MC) | > 5-10 mm |
| Rotational Deformity | None or minimal (≤ 5-10 degrees, without functional overlap) | Any detectable or symptomatic rotational deformity (e.g., finger overlap on fisting) |
| Associated Injuries | Isolated injury, no significant soft tissue compromise | Associated nerve/tendon/vessel injury, open fracture, multiple metacarpal fractures |
| Patient Factors | Low functional demand, compliant with immobilization, no pre-existing hand pathology | High functional demand (athlete, manual laborer), non-compliance with cast, pre-existing stiffness, adjacent finger/hand injury |
| Failed Non-Operative Trial | N/A (initial treatment) | Failure of closed reduction or loss of reduction during cast immobilization |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning is essential to ensure optimal outcomes and minimize potential complications.
Diagnostic Imaging
-
Plain Radiographs
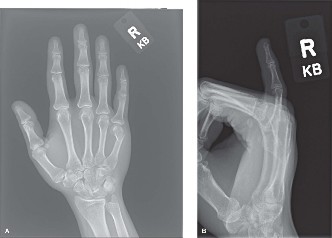
: Standard PA, lateral, and oblique views of the hand are crucial.
- The true lateral view is vital for accurately assessing dorsal angulation, which can be underestimated on oblique or standard lateral views.
- Assessment should include fracture pattern (transverse, oblique, comminuted), location (neck), degree of dorsal angulation, shortening, and any signs of rotation.
- Contralateral Hand Radiographs : May be useful for comparison, especially in assessing true metacarpal length and rotational alignment if uncertainty exists, though often not routinely required for isolated neck fractures.
- Computed Tomography (CT) Scan : Rarely indicated for isolated, simple fifth metacarpal neck fractures. Its utility is primarily reserved for highly comminuted fractures, articular involvement (which is less common in neck fractures but can occur with severe trauma), complex associated carpal injuries, or for detailed pre-operative planning in revision cases for malunion.
Patient Evaluation & Education
- A thorough history focusing on mechanism of injury, hand dominance, occupation, and functional demands.
- A detailed physical examination to assess for open wounds, neurovascular status, associated soft tissue injuries, and rotational deformity (by having the patient make a gentle fist and observing the convergence of the fingertips towards the scaphoid tubercle without overlap or scissoring).
- For surgical candidates, a comprehensive discussion regarding the risks (infection, nonunion, malunion, stiffness, hardware issues, nerve injury), benefits (improved function, reduced deformity), alternatives, and expected post-operative course is mandatory.
Equipment & Anesthesia
- Surgical Instrumentation : A dedicated hand surgery set, including small fragment instruments (e.g., 1.5 mm or 2.0 mm screw and plate systems), K-wires (0.035-inch, 0.045-inch, 0.062-inch), small bone clamps, blunt elevators, and K-wire drivers.
- Fluoroscopy : A C-arm fluoroscopy unit is indispensable for intraoperative assessment of reduction and hardware placement for both closed and open techniques.
- Hand Table : A specialized hand table is used to provide a stable, sterile working surface for the extremity.
- Tourniquet : An upper arm pneumatic tourniquet is routinely used to provide a bloodless field, typically inflated to 250-300 mmHg for the duration of the procedure.
- Anesthesia : Regional anesthesia (e.g., axillary or supraclavicular block) combined with sedation is often preferred due to its post-operative analgesic benefits. General anesthesia is also a viable option.
Patient Positioning & Preparation
- The patient is positioned supine on the operating table.
- The affected arm is abducted and supported on a radiolucent hand table. The hand is pronated to facilitate a dorsal approach.
- The tourniquet is applied to the upper arm.
- Standard surgical prep and draping of the entire upper extremity, from the tourniquet down to the fingertips, is performed to ensure a sterile field.
Detailed Surgical Approach / Technique
The choice of surgical technique depends on the fracture characteristics, surgeon preference, and patient factors. The overarching principles are anatomical reduction, stable fixation, and preservation of soft tissues to facilitate early rehabilitation.
1. Closed Reduction and Percutaneous Pinning (CRPP)
CRPP is a minimally invasive technique suitable for acute, reducible, and relatively stable fractures without significant comminution, and is often the first-line operative intervention.
Technique:
- Anesthesia : Regional or general anesthesia is administered.
-
Reduction Maneuver (Jahss Maneuver)
:
- Apply gentle longitudinal traction to the fifth digit.
- Flex the MCP and proximal interphalangeal (PIP) joints of the little finger to 90 degrees.
- Apply firm dorsal pressure with the surgeon's thumb to the volar aspect of the proximal phalanx, while simultaneously applying pressure volarly to the dorsal prominence of the metacarpal head. This maneuver levers the metacarpal head dorsally, correcting the apex dorsal angulation.
- Maintain reduction manually while confirming alignment with fluoroscopy in PA, lateral, and oblique views. Ensure rotational alignment by having the patient make a fist (if awake) or by aligning the fingernails with the distal wrist crease.
-
Pin Insertion
:
-
Intramedullary (IM) K-wires
: This is a common and effective method for neck fractures. Typically, two 0.035-inch or 0.045-inch K-wires are used.
- The K-wires are inserted retrograde from the dorsal-ulnar aspect of the metacarpal head, just proximal to the articular surface. The entry point should be carefully chosen to avoid the joint.
- The wires are driven across the fracture site and into the medullary canal of the proximal fragment.
- Alternatively, antegrade pinning from the metacarpal base can be performed, but this is less common for neck fractures and can be technically challenging due to anatomical constraints.
- Crossed K-wires : Two K-wires are inserted from the dorsal aspect of the metacarpal shaft, crossing at the fracture site. This provides a stable construct, but may require slightly more soft tissue dissection for insertion points.
- Technique Refinement : After drilling, the wires are bent at a right angle and cut short, leaving enough length for easy removal but ideally buried beneath the skin level to minimize pin tract infection risk. Alternatively, wires can be left exposed and incorporated into the cast.
-
Intramedullary (IM) K-wires
: This is a common and effective method for neck fractures. Typically, two 0.035-inch or 0.045-inch K-wires are used.
- Post-Reduction Confirmation : Fluoroscopic images in multiple planes are taken to confirm anatomical reduction and satisfactory pin placement, ensuring no joint penetration.
- Immobilization : A well-padded short arm ulnar gutter splint or cast is applied to maintain the reduction and protect the pins. The MCP joint is usually immobilized in 70-90 degrees of flexion to tighten the collateral ligaments, minimizing stiffness. The PIP and DIP joints are left free.

Figure 1: Post-operative radiograph demonstrating internal fixation of a fifth metacarpal neck fracture.
2. Open Reduction and Internal Fixation (ORIF)
ORIF is indicated for irreducible fractures, significantly comminuted or unstable fractures, open fractures, or when more rigid fixation is desired for early rehabilitation.
Surgical Approach:
- Incision : A dorsal longitudinal incision is made directly over the fifth metacarpal. A slightly ulnar or radial curvilinear incision can be used to minimize direct scar adhesion to the extensor tendons. The incision length should allow adequate exposure for reduction and fixation.
-
Dissection
:
- Carefully dissect through the subcutaneous tissue. Identify and protect the dorsal cutaneous branches of the ulnar nerve, which typically course along the ulnar aspect of the fifth metacarpal. Also protect the underlying dorsal venous system.
- Retract the extensor digiti minimi (EDM) tendon, which lies directly over the fifth metacarpal. The internervous plane is typically between the EDM and the extensor digitorum communis (EDC) tendon to the little finger. Alternatively, the EDM can be retracted radially or ulnarly, or a subperiosteal dissection beneath the tendon can be performed.
- Fracture Exposure : Incise the periosteum longitudinally along the dorsal aspect of the metacarpal and elevate it minimally (subperiosteal dissection) to expose the fracture site. Excessive periosteal stripping should be avoided to preserve blood supply.
-
Debridement and Reduction
:
- Evacuate any hematoma and debride interposed soft tissues (e.g., volar plate, intrinsic muscle fibers) that may impede reduction.
- Achieve anatomical reduction under direct visualization. This may involve using small bone hooks, blunt elevators, K-wires used as joysticks, or small bone-holding clamps.
- Restore metacarpal length, sagittal and coronal alignment, and crucially, rotational alignment. Assess rotation by ensuring the natural cascade of the fingers when making a fist is restored.
Fixation Options:
-
Plate and Screws
:
- Mini-fragment Plating (1.5mm or 2.0mm) : This is the most common and biomechanically robust method for ORIF of metacarpal neck fractures.
- Plate Application : A pre-contoured or malleable mini-fragment plate is selected. Dorsal application of the plate effectively neutralizes bending forces that cause dorsal angulation. The plate should be contoured to match the dorsal surface of the metacarpal.
- Screw Placement : At least two bicortical screws (preferably three) should be placed on each side of the fracture site to achieve stable fixation. Consider utilizing a lag screw through the plate for oblique fracture components to achieve interfragmentary compression, followed by neutralization screws.
- Biomechanical Considerations : While dorsal plating effectively combats dorsal angulation, severe volar comminution can lead to difficulty in maintaining reduction with a purely dorsal plate. In rare, highly comminuted cases, a combined dorsal-volar approach or alternative fixation might be considered, though less commonly for neck fractures.
-
Intramedullary (IM) Fixation (Pins/Nails)
:
- Can be used as an alternative to plating, offering less soft tissue disruption.
- Technique : Retrograde insertion of K-wires or specialized IM nails from the metacarpal head, or antegrade from the base, similar to CRPP but under direct visualization.
- Advantages : Less soft tissue stripping, potentially less hardware prominence.
- Disadvantages : May not be as rotationally stable or as rigid as plate fixation, particularly in comminuted or unstable fractures.
-
K-wires (Open)
:
- While often used for temporary stabilization during ORIF, K-wires can also be used as definitive fixation under direct visualization for certain stable fracture patterns, similar to CRPP.
- This allows for precise placement and immediate confirmation of reduction.
Final Steps:
- Intraoperative Fluoroscopy : Confirm final reduction and hardware position in PA, lateral, and oblique views.
- Irrigation : Copiously irrigate the wound.
- Closure : Close the periosteum if possible, followed by subcutaneous tissue and skin. Ensure careful handling of the skin edges to prevent tension. A sterile dressing is applied, followed by a protective short arm splint (often an ulnar gutter).
Pearls & Pitfalls
- Pearls : Anatomic reduction (length, alignment, rotation) is paramount. Protect vital soft tissues (nerves, veins, tendons). Minimize periosteal stripping. Confirm reduction and fixation adequacy with intraoperative fluoroscopy in multiple planes.
- Pitfalls : Inadequate reduction leading to malunion. Damage to dorsal cutaneous ulnar nerve branches. Pin tract infections with exposed K-wires. Hardware prominence, especially with dorsal plating. Stiffness from prolonged immobilization or aggressive soft tissue dissection.
Complications & Management
Despite meticulous surgical technique and post-operative care, complications can occur following treatment of fifth metacarpal neck fractures. Prompt recognition and appropriate management are crucial to mitigate long-term sequelae.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approximate) | Management/Salvage Strategies |
|---|---|---|
| Malunion (Angulation, Shortening, Rotation) | Varies (e.g., up to 20-30% for non-operative, lower for ORIF, higher if initial deformity was significant) | Symptomatic : For significant functional impairment or pain from angulation or shortening, a corrective osteotomy (e.g., dorsal closing wedge osteotomy for dorsal angulation, opening wedge osteotomy with bone graft for shortening) with ORIF (plate and screws) is indicated. For rotational malunion, a rotational osteotomy is performed. Asymptomatic : Observation, activity modification. |
| Nonunion | Rare (< 5%) | Management : Revision ORIF with rigid fixation (e.g., compression plating) and bone grafting (autograft, allograft, or bone graft substitutes) to stimulate healing. Address contributing factors such as infection, inadequate immobilization, or poor soft tissue envelope. Exclude underlying metabolic disorders. |
| Infection | Low (1-5% for ORIF, higher for pin tracts with CRPP) | Superficial : Oral antibiotics (culture-guided if possible), local wound care. Deep : Urgent surgical debridement, irrigation, IV antibiotics (culture-guided). Hardware removal may be necessary if persistent infection (usually after fracture union, or staged approach if union is delayed). |
| Hardware Prominence / Irritation | Common (5-15% for plating) | Management : Symptomatic hardware removal after complete fracture union (typically 6-12 months post-operatively). Ensure fracture stability before removal. |
| Stiffness / Loss of Range of Motion (ROM) | Common (10-20%) | Prevention : Early supervised hand therapy, careful soft tissue handling, minimal dissection. Management : Aggressive physical therapy, including active and passive ROM exercises, dynamic splinting. Consider tenolysis or capsulectomy in refractory cases leading to significant functional deficit (typically after 6-12 months of failed conservative management). |
| Nerve Injury (Dorsal Cutaneous Ulnar) | Low (< 1-2%) | Prevention : Meticulous surgical dissection, identification, and protection of the dorsal cutaneous branches of the ulnar nerve. Management : Observation for neurapraxia (often resolves spontaneously). Surgical exploration and direct repair for confirmed transection. Neurolysis for entrapment or neuroma formation. |
| Tendon Adhesions | Low-moderate (5-10%) | Prevention : Gentle soft tissue handling, minimal periosteal stripping, meticulous closure, early mobilization. Management : Intensive hand therapy focusing on tendon gliding exercises. Tenolysis (surgical release of adhesions) if severe adhesions significantly restrict tendon excursion and motion after 6-12 months of failed conservative management. |
| Complex Regional Pain Syndrome (CRPS) | Rare (< 1%) | Prevention : Early pain control, early mobilization, Vitamin C supplementation post-injury (controversial but suggested by some studies). Management : Multimodal approach including early diagnosis, physical therapy, pain management specialists (e.g., regional nerve blocks, oral medications), psychological support. Prognosis is better with early intervention. |
| Loss of Reduction (post-CRPP) | Varies, higher than ORIF | Management : If early and within acceptable parameters, repeat closed reduction and pinning. If significant loss of reduction or instability, conversion to ORIF with plate and screws is indicated. |
| Pin Tract Infection (with CRPP) | 5-10% | Prevention : Aseptic technique during pin insertion, careful pin care (daily cleaning). Management : Oral antibiotics for superficial infection. Pin removal for deep or persistent infection (after fracture union), followed by oral antibiotics. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical component of successful management following fifth metacarpal neck fracture fixation. The protocol aims to protect the healing fracture while restoring maximal hand function, minimizing stiffness, and preventing complications. The timeline and specific exercises are tailored to the stability of fixation and individual patient progress.
General Principles
- Early Motion : Encouraged for adjacent uninvolved joints and, if fixation is stable, for the fractured digit itself, to prevent stiffness.
- Protection : The fracture site requires protection from excessive stress, particularly rotational or shear forces, until radiographic and clinical union.
- Edema Control : Crucial throughout recovery to minimize stiffness and pain.
- Pain Management : Adequate pain control facilitates participation in therapy.
Phase 1: Immobilization and Initial Healing (Weeks 0-3)
Goals
:
* Protect fracture fixation.
* Control pain and swelling.
* Maintain range of motion (ROM) in uninvolved joints.
Protocol
:
*
Immobilization
:
*
CRPP
: Short arm ulnar gutter splint or cast. The MCP joint of the little finger is typically immobilized in 70-90 degrees of flexion to keep the collateral ligaments taut and prevent MCP joint stiffness. The PIP and DIP joints are left free for movement.
*
ORIF (Plate and Screws)
: A short arm ulnar gutter splint or cast for initial protection, often removable for wound care and gentle active ROM as dictated by surgical stability. MCP joint position is typically the same as CRPP.
*
Activities
:
*
Elevation
: Hand elevated above heart level, especially in the first few days, to reduce swelling.
*
Ice
: Applied for 15-20 minutes every 2-3 hours to manage swelling and pain.
*
Active ROM (AROM) of Uninvolved Digits
: Immediate active flexion/extension of the thumb, index, middle, and ring fingers to maintain mobility.
*
AROM of Fractured Digit (if stable fixation and surgeon allows)
: Gentle active flexion and extension of the little finger's PIP and DIP joints. Gentle active MCP flexion/extension may be initiated
only
if fixation is extremely stable and with specific surgeon approval. Avoid resisted movements or heavy gripping.
*
Wound Care
: Daily dressing changes as per surgeon's instructions. Keep surgical incision dry until sutures/staples are removed (typically 10-14 days).
Phase 2: Early Mobilization and Strengthening (Weeks 3-6)
Goals
:
* Begin active and gentle passive ROM of the fractured digit.
* Start light strengthening.
* Improve scar mobility and reduce edema.
Protocol
:
*
Hardware Removal (CRPP)
: K-wires are typically removed at 3-4 weeks post-operatively, once clinical and radiographic signs of union are present.
*
Mobilization
:
*
Increased AROM
: Gradually increase active flexion and extension of the little finger's MCP, PIP, and DIP joints.
*
Gentle Passive ROM (PROM)
: Initiate gentle passive movements as tolerated, progressing carefully. Avoid aggressive stretching that could compromise fracture healing.
*
Blocking Exercises
: To isolate motion at individual joints.
*
Tendon Gliding Exercises
: To prevent adhesions of extensor tendons.
*
Strengthening
:
* Begin with very light isometric contractions.
* Progress to gentle strengthening exercises using soft putty or light resistance bands for grip and pinch.
*
Scar Management
: Once the wound is closed, scar massage (desensitization) and moisturization to prevent hypertrophic scarring and improve tissue pliability.
*
Edema Control
: Continued elevation, retrograde massage, compression garments (e.g., Isotoner glove) if significant swelling persists.
*
Precautions
: Avoid heavy gripping, lifting, pushing, or impact activities. Avoid forceful twisting motions.
Phase 3: Progressive Strengthening and Functional Return (Weeks 6-12+)
Goals
:
* Achieve full, pain-free ROM.
* Restore grip and pinch strength to pre-injury levels.
* Return to activities of daily living (ADLs), work, and sport.
Protocol
:
*
Strengthening
:
* Progressive resistive exercises using hand putty, Theraband, grip strengtheners, and light weights.
* Focus on functional tasks requiring grip, pinch, and dexterity.
*
Endurance
: Gradual increase in repetitions and duration of activities.
*
Return to Activity
:
* Gradual return to work-specific tasks, recreational activities, and sports. Contact sports may require longer periods of protection (e.g., 3-4 months or until full union and strength).
*
Hardware Removal (ORIF)
: Optional, and typically not performed before 6-12 months post-operatively. It is considered for symptomatic hardware (pain, impingement, tendon irritation).
*
Long-term Monitoring
: Continue to monitor for residual stiffness, pain, or any signs of malunion or nonunion.
Throughout all phases, a close collaboration between the surgeon, physical or occupational therapist, and the patient is paramount to tailor the protocol to individual needs and optimize functional outcomes.
Summary of Key Literature / Guidelines
Management of fifth metacarpal neck fractures has evolved, moving towards more aggressive intervention for unstable fractures and a focus on early functional recovery. The literature highlights several key principles:
-
Acceptable Angulation : Historically, the fifth metacarpal was considered to tolerate significant dorsal angulation (up to 40-70 degrees) due to compensatory MCP joint hyperextension. However, a growing body of literature suggests that better functional and cosmetic outcomes are achieved with more anatomical reduction. For instance, Ali et al. (2011) suggested that angulation above 30-40 degrees warrants consideration for intervention, especially in active patients. De Visser et al. (2017) , in a systematic review, found a trend towards improved outcomes with less angulation. Rotational deformity, regardless of metacarpal, is universally considered unacceptable and requires correction due to its severe functional impact. Shortening of greater than 5-10 mm also correlates with poorer functional outcomes.
-
Comparison of Fixation Methods :
- Closed Reduction and Percutaneous Pinning (CRPP) : Several studies support CRPP as a reliable and less invasive method for acute, reducible fifth metacarpal neck fractures. Hegeman et al. (2012) demonstrated good results with CRPP, though acknowledging the risk of pin tract infection and potential for loss of reduction if not adequately immobilized. Meger et al. (2019) , in a comparative study, found no significant difference in functional outcomes between CRPP and ORIF with plates for specific fracture types, but CRPP had fewer hardware-related complications.
- Open Reduction and Internal Fixation (ORIF) with Plating : This method provides rigid, stable fixation, allowing for earlier mobilization and is preferred for unstable, significantly displaced, comminuted, or irreducible fractures. Cannon et al. (2015) highlighted the biomechanical advantages of dorsal plating in neutralizing dorsal angulation. Kim et al. (2018) reported good to excellent outcomes with mini-plate fixation, emphasizing the importance of anatomical reduction. The main drawbacks include higher invasiveness, potential for hardware prominence, and soft tissue irritation.
- Intramedullary Fixation : Intramedullary K-wires or specialized nails offer a less invasive alternative to plating while providing more stability than simple cast immobilization. Firoozabadi et al. (2018) described favorable results with intramedullary fixation for selected metacarpal fractures, noting benefits in reducing soft tissue dissection. It is often considered for transverse or short oblique fractures.
-
Role of Early Mobilization : Across all fixation methods, early supervised hand therapy and mobilization are critical to prevent stiffness, improve functional range of motion, and reduce the incidence of complications like CRPS. O'Brien et al. (2014) underscored the importance of early rehabilitation protocols tailored to the stability of fixation. Immobilization, when required, should be for the shortest effective duration.
-
Functional Outcomes : Key outcome measures include grip strength, range of motion (MCP, PIP, DIP joints), patient-reported outcome measures (e.g., QuickDASH score), and patient satisfaction. The literature consistently emphasizes that anatomical reduction of length, alignment, and rotation is directly correlated with superior functional outcomes.
In summary, while non-operative management remains appropriate for stable, minimally displaced fifth metacarpal neck fractures within acceptable parameters, surgical intervention is indicated for significant angulation, shortening, rotation, or instability. The choice between CRPP, ORIF with plating, or IM fixation is individualized based on fracture characteristics and surgeon expertise, with a consistent emphasis on achieving anatomical reduction and facilitating early, guided rehabilitation.
