Moberg Advancement Flap: Comprehensive Guide to Surgical Technique & Outcomes for Thumb Reconstruction
Key Takeaway
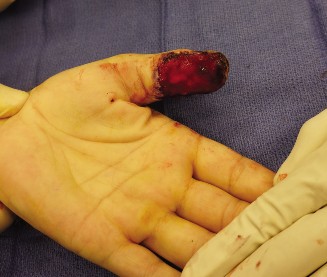
The Moberg advancement flap is a foundational technique in reconstructive hand surgery. It restores sensate soft tissue coverage to full-thickness distal thumb pulp defects (typically 1-3 cm), preserving critical tactile sensation and functional grip/pinch. This local, innervated, vascularized flap is crucial for optimal thumb function after trauma.
Introduction & Epidemiology
The Moberg advancement flap, first described by Moberg in 1964, represents a foundational technique in reconstructive hand surgery, specifically for restoring sensate soft tissue coverage to the distal thumb pulp. Its primary utility lies in addressing full-thickness palmar thumb defects of moderate size (typically 1-3 cm) where preservation of critical tactile sensation and durable soft tissue are paramount for functional grip and pinch.
Epidemiologically, distal thumb injuries are common, often resulting from crush mechanisms, lacerations, or avulsions due to industrial accidents, household mishaps, or sport-related trauma. The thumb's critical role in prehension dictates that any reconstruction prioritize not only coverage but also restoration of sensation and maintenance of range of motion. While smaller defects may be amenable to secondary intention, local flap closure, or skin grafting, these alternatives often fall short in providing the robust, sensate, and mobile pad required for optimal thumb function. The Moberg flap fills a crucial niche by providing a sensate, innervated, and vascularized flap utilizing local tissue, thereby minimizing donor site morbidity from distant flaps and providing superior functional outcomes compared to non-sensate grafts.
Surgical Anatomy & Biomechanics
A thorough understanding of thumb anatomy is critical for successful Moberg flap execution.
Thumb Anatomy Pertinent to the Moberg Flap
- Skin and Subcutaneous Tissue : The skin of the thumb pulp is highly specialized, characterized by numerous papillary ridges providing grip and a dense concentration of sensory receptors. The subcutaneous tissue is tethered to the underlying flexor sheath by fibrous septa, contributing to the stability of the pulp but also necessitating careful dissection for flap mobilization. The volar skin of the thumb, particularly proximal to the defect, is mobilized as the flap.
-
Neurovascular Bundles
: The Moberg flap is a bipedicled axial flap relying on the integrity of both proper digital neurovascular bundles of the thumb.
- Proper Digital Arteries : These originate from the radial and ulnar digital arteries, running along the palmar aspects of the metacarpophalangeal (MCP) and interphalangeal (IP) joints, deeply investing in the subcutaneous fat. They anastomose distally, forming an arcade within the pulp.
- Proper Digital Nerves : These are terminal branches of the median and radial nerves (or occasionally ulnar nerve variations). They accompany the proper digital arteries on their respective sides, supplying rich sensory innervation to the thumb pulp. These nerves are carefully preserved within the flap pedicles.
- Flexor Sheath : The fibrous flexor sheath overlies the flexor pollicis longus (FPL) tendon and its synovial sheath. This structure serves as a dissection plane for elevating the flap.
- Fibrous Septa : These vertical septa extend from the skin to the flexor sheath and periosteum, compartmentalizing the pulp space. Their release is essential for flap advancement.
Biomechanics of Thumb Function and Flap Contribution
The thumb contributes approximately 40-50% to overall hand function. Its unique opposable position facilitates precision pinch, power grip, and grasp.
*
Pinch and Grip
: Effective pinch and grip rely heavily on a stable, sensate, and mobile pulp pad that can conform to objects and provide proprioceptive and tactile feedback. A durable, sensate reconstruction is critical.
*
Sensory Feedback
: The Moberg flap's preservation of the bilateral neurovascular bundles ensures that the reconstructed pulp retains its crucial two-point discrimination and protective sensation, allowing for fine manipulation and preventing repetitive injury. This is a significant advantage over non-sensate coverage options.
*
Mobility
: The advancement achieved with the Moberg flap maintains the intrinsic mobility of the thumb skin, essential for accommodating the varied positions of the thumb during functional tasks.
The flap's axial design, incorporating the proper digital neurovascular bundles, is critical to its viability and the functional quality of the reconstruction. Disruption of these bundles, either traumatically or iatrogenically, would compromise the flap's vascularity and sensation, necessitating an alternative reconstructive strategy.
Indications & Contraindications
The Moberg advancement flap is a versatile technique but possesses specific indications where its advantages are maximized and contraindications where its use is ill-advised.
Indications for Moberg Advancement Flap
- Distal Thumb Pulp Defects : Primarily indicated for full-thickness defects of the volar thumb, distal to the MCP joint, often involving the IP joint or distal phalanx.
- Moderate Size Defects : Best suited for defects measuring approximately 1 to 3 cm in length or width. While some sources suggest up to 2.5 cm, advancements up to 3 cm have been reported with aggressive mobilization and potential proximal skin grafting.
- Preservation of Neurovascular Bundles : Critical requirement. The proper digital neurovascular bundles must be intact and functional proximal to the defect to ensure flap viability and sensation. Pre-operative assessment for digital artery patency (e.g., Allen's test if applicable, capillary refill) and nerve function is essential.
- Requirement for Sensate Coverage : When a sensate, durable, and aesthetically acceptable pulp is necessary for optimal thumb function (e.g., for precision pinch, fine motor tasks, or protective sensation).
- Local Tissue Match : The Moberg flap provides an excellent match in terms of skin texture, color, and thickness compared to skin grafts or distant flaps.
- Foucher Classification : Commonly indicated for Foucher Type 1 and Type 2 thumb pulp defects, which are primarily oblique or transverse injuries sparing the nail complex. Type 3 defects (transverse, often with significant bone loss) or Type 4 defects (total avulsion) typically require more complex reconstruction.
- Stable Skeletal Framework : The underlying bone and joint must be stable or appropriately stabilized prior to or concomitant with flap coverage.
Contraindications for Moberg Advancement Flap
- Large Defects : Defects exceeding 3 cm, particularly those with significant dorsal skin loss, exposed nail bed, or extensive bone exposure, are generally too large for reliable coverage with a Moberg flap without excessive tension or risk of necrosis.
- Proximal Neurovascular Injury : Any injury that compromises the vascularity or innervation of the proposed flap (i.e., damage to both proper digital neurovascular bundles proximal to the flap origin) is an absolute contraindication.
- Extensive Crush Injury or Scarring : If the soft tissues proximal to the defect are severely traumatized, scarred, or heavily contused, the vascularity and mobility of the flap may be compromised, leading to poor outcomes.
- Infection : Active infection at the defect site is a contraindication until adequately managed.
- Significant Bone Loss or Joint Instability : While minor bone loss can be managed, extensive skeletal defects or unstable joints may necessitate a different reconstructive approach (e.g., composite graft, free tissue transfer) or staged reconstruction.
- Patient Factors : Unrealistic patient expectations, severe comorbidities precluding surgery, or inability to comply with post-operative rehabilitation.
Table: Operative vs. Non-Operative Indications
| Feature | Operative Indication (Moberg Flap) | Non-Operative Indication (Secondary Intention, Local Flap, Skin Graft) |
|---|---|---|
| Defect Size | Moderate (1-3 cm), full-thickness | Small (<1 cm), partial-thickness, or very large defects not amenable to Moberg |
| Depth of Injury | Full-thickness skin loss, exposed tendon, bone, or joint | Epidermal/dermal loss, superficial |
| Vascular Status | Intact neurovascular bundles proximal to defect | Intact vascularity of surrounding tissue or compromised requiring different approach |
| Sensation Requirement | Critical need for sensate, durable pulp (e.g., thumb tip) | Sensation less critical, or expected to regenerate naturally |
| Associated Injuries | Isolated soft tissue loss, stable skeletal injury | Unstable or complex skeletal injury requiring alternative fixation/coverage |
| Tissue Availability | Adequate healthy volar skin proximal to defect for flap creation | Insufficient local healthy tissue for flap advancement |
| Functional Demand | High functional demand for pinch/grip | Lower functional demand |
Pre-Operative Planning & Patient Positioning
Careful pre-operative planning and meticulous patient positioning are paramount to optimize the success of a Moberg advancement flap.
Pre-Operative Planning
-
Comprehensive Patient Assessment
:
- History : Mechanism of injury, time since injury, dominant hand, occupation, relevant medical comorbidities (e.g., diabetes, peripheral vascular disease, smoking history, steroid use, anticoagulant use).
-
Physical Examination
:
- Defect Assessment : Meticulous measurement of defect size (length, width, depth), location, and involvement of adjacent structures (nail bed, joint capsule, bone). Assess tissue quality at the defect margins.
- Neurovascular Status : Crucial. Assess two-point discrimination of the thumb and adjacent digits, capillary refill, skin turgor, and temperature. Document pre-operative sensation. Check for adequate perfusion (e.g., Allen's test if digital arteries are of concern, although less specific for thumb proper digital arteries). Confirm intact proper digital neurovascular bundles proximal to the defect.
- Range of Motion : Assess active and passive range of motion of the thumb IP and MCP joints.
- Associated Injuries : Rule out concurrent fractures, tendon lacerations, or joint instability.
-
Imaging
:
- Radiographs : Standard anteroposterior, lateral, and oblique views of the thumb are essential to rule out occult fractures, dislocations, or foreign bodies.
-
Surgical Consent
: Detailed discussion with the patient regarding:
- The reconstructive plan, including the Moberg flap technique.
- Expected outcomes, including potential for restored sensation, pulp durability, and cosmetic appearance.
- Potential complications (e.g., flap necrosis, infection, stiffness, cold intolerance, sensory deficits, scarring).
- Alternative reconstructive options (e.g., skin graft, cross-finger flap, thenar flap, free tissue transfer) and reasons for choosing the Moberg flap.
- The potential need for a split-thickness skin graft (STSG) to the proximal donor site if extensive advancement is required.
- Photography : Standardized pre-operative photographs of the defect are advisable for documentation and outcome assessment.
- Tourniquet Time Management : Plan the operative sequence to minimize tourniquet time.
- Antibiotic Prophylaxis : Administer prophylactic broad-spectrum antibiotics, especially in traumatic open wounds.
Patient Positioning
- Supine Position : The patient is placed supine on the operating table.
- Arm Position : The affected arm is abducted approximately 90 degrees on a specialized hand table, allowing full access to the thumb and forearm. A soft arm board or pillow is used to support the arm comfortably.
- Tourniquet Application : A pneumatic tourniquet is applied to the upper arm. Esmarch bandage exsanguination is performed after elevating the limb, followed by inflation of the tourniquet to standard pressures (e.g., 250 mmHg for normotensive adults). A finger tourniquet can also be used for specific cases, though a brachial tourniquet is often preferred for more extensive dissection.
- Sterile Preparation and Drape : The entire hand, wrist, and forearm are prepped with an antiseptic solution and sterilely draped, ensuring the operative field is adequately exposed for both the thumb and potential donor sites for a skin graft (e.g., volar forearm).
- Magnification : Loupe magnification (e.g., 2.5x to 4.5x) is highly recommended for identifying and protecting the delicate neurovascular bundles and for precise flap dissection and inset.
Detailed Surgical Approach / Technique
The successful execution of a Moberg advancement flap demands meticulous dissection and precise handling of the delicate neurovascular structures.
Incision Design and Initial Debridement
- Defect Debridement : Thoroughly debride the wound edges and defect base of all devitalized tissue until healthy, bleeding tissue is encountered. The defect margins should be clean and clearly defined. Hemostasis is achieved.
-
Flap Markings : Using a sterile marking pen, delineate the defect. Then, mark the planned incisions for the Moberg flap. These typically consist of:
- Bilateral Mid-Axial Incisions : These incisions extend proximally from the corners of the pulp defect along the mid-axial lines of the thumb. The mid-axial line runs between the volar and dorsal skin of the digit.
- Proximal Extent : The incisions typically extend proximally to the level of the MCP joint crease, or even into the thenar crease, forming a "V" or "fishmouth" shape proximally. The length of these incisions dictates the amount of advancement achievable. The goal is to create a rectangular flap containing the pulp and the volar skin of the thumb, hinged proximally on its neurovascular bundles.
- Anatomical Landmark : Ensure the incisions are dorsal to the neurovascular bundles but volar to the dorsal digital nerves and veins, staying true to the mid-axial plane.

(Image depicting the typical Moberg flap incision design and advancement)
Flap Dissection and Mobilization
- Skin Incision : Incise the skin along the marked lines with a #15 blade.
-
Subcutaneous Dissection
:
- Carefully elevate the full-thickness skin and subcutaneous fat from the underlying flexor pollicis longus (FPL) tendon sheath. This is a critical step. The plane of dissection is superficial to the flexor tendon sheath but deep to the neurovascular bundles.
- Neurovascular Bundle Preservation : The proper digital neurovascular bundles (artery, nerve, and vein) run along the lateral aspects of the flexor sheath within the subcutaneous tissue. The dissection must proceed with extreme caution to protect these structures. The flap is effectively a bipedicled axial flap, with each pedicle containing a neurovascular bundle.
- Release of Fibrous Septa : The skin of the pulp is tethered to the flexor sheath by numerous fibrous septa. These must be carefully divided with fine scissors or a scalpel to allow the flap to mobilize and advance distally. The goal is to fully release the volar skin and subcutaneous tissue from the fibrous sheath, creating a mobile flap. This often includes releasing the oblique retinacular ligament if it restricts advancement.
- Dorsal Branches : Small dorsal sensory branches or veins may need to be ligated or cauterized to facilitate release, but every effort should be made to preserve them if possible.
-
Distal Advancement
:
- Once adequately mobilized, the flap is gently advanced distally to cover the defect. This is performed under minimal tension. Up to 1.5 to 2 cm of advancement is typically achievable.
- Assess Tension : After advancement, carefully assess the tension on the flap and the proximal donor site. Excessive tension is the primary cause of flap necrosis.
Closure and Grafting (if needed)
-
Flap Inset
:
- Suture the advanced flap to the recipient defect margins using fine, interrupted sutures (e.g., 6-0 or 7-0 non-absorbable monofilament nylon). Start with corner sutures and then fill in the gaps.
- Ensure precise skin edge approximation without tension.
-
Proximal Donor Site Closure
:
- After advancing the volar flap distally, a triangular or "V-shaped" defect is created proximally on the volar aspect of the thumb.
- Primary Closure : If the defect is small and can be closed without tension by advancing the lateral skin flaps, primary closure is performed. This can often be achieved by closing the proximal "V" incision into a "Y" shape (V-Y advancement principle).
-
Split-Thickness Skin Graft (STSG)
: If the advancement is significant (e.g., >1.5 cm), the proximal donor site defect may be too large to close primarily without excessive tension, which could compromise the main Moberg flap. In such cases, a thin STSG is harvested (e.g., from the volar forearm or thenar eminence) and sutured into the proximal defect. This allows for maximal advancement of the sensate pulp flap while avoiding undue tension. The STSG provides coverage but is non-sensate.
- The STSG is typically secured with fine interrupted sutures and then bolster dressing or tie-over sutures for even pressure.
- Hemostasis : Confirm meticulous hemostasis. The tourniquet can be deflated before final closure to ensure no bleeding under the flap.
- Dressing : A non-adherent dressing (e.g., Xeroform), followed by soft gauze and a protective splint. Avoid tight circumferential dressings.
Variations and Considerations
- Modified Moberg Flap (Unilateral Pedicle) : In specific scenarios, one neurovascular bundle may be divided to gain greater flap length (e.g., up to 3-4 cm). This converts the bipedicled flap into a unipedicled island flap. While offering more reach, it sacrifices sensation on the divided side and significantly increases the risk of vascular compromise. It is generally reserved for situations where maximal length is required and some sensory deficit is acceptable, or when one bundle is already compromised by trauma. Less commonly used for primary thumb pulp reconstruction due to sensory loss.
- V-Y Moberg Advancement : This variation involves extending the incisions proximally as a "V" which is then closed as a "Y" after advancement, allowing for some gain in length without creating a proximal defect that requires a skin graft. However, the amount of advancement is typically less than with the standard Moberg with a potential proximal STSG.
- Extended Moberg Flap : Incisions are extended even further proximally into the thenar eminence to recruit more tissue, often requiring more extensive subcutaneous dissection and potentially jeopardizing perforators to the thenar skin.
- Combination Techniques : The Moberg flap can sometimes be combined with a small full-thickness skin graft for very distal or lateral aspects of the defect not fully covered by the sensate flap.
Complications & Management
While the Moberg advancement flap is a reliable procedure, complications can occur. Prompt recognition and appropriate management are crucial for optimal outcomes.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence | Management / Salvage Strategy |
|---|---|---|
| Flap Necrosis | Partial: 5-15%; Full: <5% | Partial: Conservative management (dressing changes, debridement of necrotic edges), often heals by secondary intention. Full: Early recognition (pallor/cyanosis, absent capillary refill, cold, lack of bleeding after pinprick). If arterial: explore, remove tension, consider re-evaluation of vascular status, or revision. If venous: consider leeches, careful release of dressing, then exploration. Debridement and alternative coverage (e.g., cross-finger flap, thenar flap, free flap, skin graft) if necessary. |
| Hypesthesia / Anesthesia | Variable (often transient) | Expect initial sensory changes. Most resolve with time as nerve fibers recover/adapt. Sensory re-education post-op. Persistent deficits may require neurolysis if compression is suspected, or revision surgery if a nerve was transected and not repaired. Cold intolerance may persist. |
| Hypertrophic Scarring / Contracture | Common along incision lines; Pulp contracture: 5-10% | Scarring: Scar massage, silicone sheeting, steroid injections. Contracture: Early, aggressive hand therapy and splinting to prevent joint stiffness (especially IP joint). Dynamic splinting. Surgical release (e.g., Z-plasty, scar revision, capsulotomy) if severe and functionally limiting. |
| Infection | Low (<5%) | Prophylactic antibiotics. If superficial: local wound care, oral antibiotics. If deep (abscess/cellulitis): incision and drainage, IV antibiotics, debridement. |
| Hematoma / Seroma | Low | Careful hemostasis intraoperatively. If small: observation. If large/expanding: drainage (needle aspiration or surgical evacuation), compression dressing. May contribute to flap compromise. |
| Stiffness / Limited ROM | Variable (IP, MCP joints) | Primary issue with any hand surgery. Early, structured hand therapy is crucial. Splinting. If persistent: consider surgical tenolysis or capsulotomy. |
| Cold Intolerance | 10-20% (often persistent) | Patient education and reassurance. Protective measures (gloves). May improve partially over time but often remains a long-term issue. |
| Cosmetic Deformity | Variable | Scars are inevitable. Manage expectations pre-operatively. Scar revision may be considered for prominent or tethering scars. |
| Donor Site Morbidity | Minimal if primarily closed or STSG well-healed | If STSG used: issues with STSG take (hematoma, infection), scarring, contour irregularity. Manage according to standard graft principles. |
General Management Principles
- Early Recognition : Vigilant post-operative monitoring for signs of complications, particularly flap vascularity (color, capillary refill, temperature, sensation).
- Conservative Measures First : Many complications, especially partial flap necrosis or sensory changes, can be managed conservatively with good wound care and observation.
- Aggressive Hand Therapy : Essential for preventing stiffness and optimizing functional recovery, beginning early in the post-operative period.
- Patient Education : Clear communication about expected recovery, potential challenges, and adherence to rehabilitation protocols.
- Surgical Intervention : Reserved for significant complications (e.g., complete flap necrosis, persistent infection, severe contracture) that do not respond to conservative management.
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is crucial for maximizing functional recovery and mitigating potential complications after a Moberg advancement flap. The primary goals are to protect the flap, minimize edema, prevent stiffness, restore sensation, and regain functional use of the thumb.
Phase 1: Immobilization and Protection (Weeks 0-3)
- Goal : Flap healing and protection, edema control.
-
Immobilization
:
- Splinting : A dorsal block splint (thermoplastic or plaster) is typically applied immediately post-operatively. The splint holds the thumb IP and MCP joints in slight flexion (e.g., 10-20 degrees IP flexion, 20-30 degrees MCP flexion) to relax the flexor tendons and reduce tension on the flap. The wrist is typically held in slight extension (20-30 degrees). The splint should not be too tight or compress the flap.
- Duration : Typically worn continuously for 2-3 weeks, or until sutures are removed and adequate flap adherence is confirmed.
- Elevation : Maintain the hand elevated above heart level (e.g., resting on pillows) to minimize post-operative edema.
-
Wound Care
:
- Regular dressing changes (e.g., every 2-3 days by the surgeon/therapist initially, then daily at home).
- Monitor flap viability (color, capillary refill, temperature, signs of infection). Report any concerns immediately.
- Keep the wound clean and dry.
- Pain Management : Administer appropriate analgesia.
- Active Range of Motion (AROM) : Encourage gentle AROM of uninvolved joints (e.g., wrist, fingers 2-5, shoulder, elbow) to prevent stiffness and promote circulation. Avoid any movement of the thumb during this phase.
Phase 2: Gentle Mobilization and Scar Management (Weeks 3-6)
- Goal : Initiate controlled movement, reduce scar formation, begin sensory input.
- Splinting : The protective splint may be transitioned to night-time wear only, or a removable static/dynamic splint for specific activities.
-
Active Range of Motion (AROM)
:
- Begin gentle, pain-free active range of motion exercises for the thumb IP and MCP joints. Focus on flexion and extension within protected limits.
- Avoid aggressive passive stretching.
- Encourage composite thumb movements (e.g., opposition to other fingertips).
-
Scar Management
:
- Once sutures are removed and the wound is fully epithelialized, begin scar massage with moisturizing cream or lotion.
- Consider silicone gel sheeting or topical silicone products to help soften and flatten the scar.
- Edema Control : Continue elevation, light compression gloves, and gentle retrograde massage if edema persists.
- Sensory Desensitization (if hypersensitive) : Gentle tapping, rubbing, and exposure to various textures (e.g., cotton balls, soft cloth) if hypersensitivity or dysesthesia is present.
- Light Functional Activities : Begin very light activities of daily living (ADLs) that do not stress the flap or thumb.
Phase 3: Strengthening and Sensory Re-education (Weeks 6-12)
- Goal : Restore strength, improve fine motor control, enhance sensory discrimination, and return to more demanding activities.
-
Strengthening
:
- Progressive resistance exercises for thumb flexion, extension, abduction, and opposition.
- Use therapeutic putty, resistance bands, or light weights.
- Focus on pinch strength (tip-to-tip, key pinch, palmar pinch).
-
Sensory Re-education
:
- If significant sensory deficits persist, begin targeted sensory re-education. This involves tasks such as object identification (texture, shape, size) with visual occlusion, localization of touch, and progressive 2-point discrimination training.
- Address cold intolerance with education and protective strategies.
- Functional Activities : Gradually progress to more complex ADLs and work-related tasks. Simulate specific job requirements if possible.
- Joint Mobilization : If stiffness persists, gentle passive range of motion, joint mobilization techniques, and dynamic splinting may be employed by the therapist.
Phase 4: Return to Full Activity (Months 3-6+)
- Goal : Full return to pre-injury activities, continued maturation of sensation and scar.
- Progressive Loading : Gradually increase the intensity and duration of activities, including recreational sports and heavy labor, as tolerated and guided by the therapist.
- Long-Term Follow-up : Continue to monitor sensation, strength, and scar quality. Full sensory recovery can take up to 12-18 months.
- Patient Education : Reinforce the importance of protecting the thumb from re-injury and continued scar care.
Key Considerations
:
*
Individualization
: Rehabilitation protocols must be individualized based on the patient's progress, pain levels, and specific functional goals.
*
Communication
: Close collaboration between the surgeon, hand therapist, and patient is essential for optimal outcomes.
*
Patience
: Recovery, particularly sensory recovery, can be prolonged.
Summary of Key Literature / Guidelines
The Moberg advancement flap has a well-established history and continues to be a cornerstone technique in hand surgery for sensate pulp reconstruction of the thumb.
Seminal Work
:
*
Moberg (1964, 1967)
: Håkan Moberg originally described the flap as a bilateral palmar advancement flap, emphasizing the preservation of the neurovascular bundles for sensate reconstruction of the thumb pulp. His work underscored the functional importance of sensation in the thumb. He highlighted its advantage over non-sensate grafts for critical areas of pinch and grasp.
Comparative Studies and Modifications
:
*
Modified Moberg (Unilateral Pedicle)
: While Moberg's original description was bipedicled, modifications involving unilateral pedicle division were explored (e.g., by Lister et al., 1979) to achieve greater advancement. However, these modifications are associated with a higher risk of sensory deficit and vascular compromise on the divided side, limiting their routine application for primary thumb pulp reconstruction where full sensation is desired. Current consensus generally favors the bipedicled approach for its reliability in preserving sensation.
*
V-Y Advancement Flaps (e.g., Atasoy, Kutler)
: While related in principle (advancement), these flaps are typically smaller, non-axial (rely on subdermal plexus), and are usually applied to smaller, more distal fingertip defects. The Moberg flap's axial neurovascular pedicles distinguish it and allow for greater advancement and more reliable sensate coverage for larger thumb defects.
*
Cross-Finger Flap and Thenar Flap
: These are alternative local flaps. Cross-finger flaps provide durable, sensate coverage from an adjacent digit but involve a two-stage procedure, temporary tethering of the digits, and potential donor site morbidity and stiffness of the donor finger. Thenar flaps offer good tissue match but are prone to contracture if not carefully designed and are generally not sensate from the thumb's specific perspective unless transferred as an island. The Moberg flap offers the advantage of a single-stage procedure and direct re-establishment of thumb sensation.
*
Free Tissue Transfer
: For very large or complex defects, particularly those with significant bone loss or severe neurovascular compromise where local options are insufficient, free tissue transfer (e.g., groin flap, toe pulp transfer) may be indicated. These are more complex procedures with higher microsurgical demands but can provide bulk and sensation where local options fail. The Moberg flap is preferred when applicable due to its simpler technique and local tissue advantages.
Functional Outcomes
:
*
Sensation
: Studies consistently report good restoration of protective sensation and often satisfactory two-point discrimination (e.g., 6-10 mm) in the reconstructed pulp, although it may not return to completely normal levels. Some degree of cold intolerance can be a long-term sequela.
*
Pinch and Grip Strength
: Functional outcomes for pinch and grip strength are generally good, reflecting the restoration of a durable and sensate pulp.
*
Range of Motion
: Maintenance of good thumb IP and MCP joint range of motion is expected, provided post-operative stiffness is aggressively managed with therapy.
*
Patient Satisfaction
: High rates of patient satisfaction are typically reported due to the good functional and aesthetic outcomes achieved with local, sensate tissue.
*
Complication Rates
: Reported complication rates are generally low, with partial flap necrosis being the most common, followed by stiffness and sensory alterations. Complete flap loss is rare.
Current Guidelines and Principles
:
* The Moberg flap remains a first-line choice for sensate reconstruction of moderate-sized, full-thickness volar thumb pulp defects when the proximal neurovascular bundles are intact.
* Careful pre-operative assessment of neurovascular status and defect size is paramount.
* The bipedicled design is generally preferred for optimal sensation and reliability.
* The use of a split-thickness skin graft to close the proximal donor site, if tension is present after maximal advancement, is a widely accepted technique to prevent excessive tension on the primary flap and avoid complications.
* Post-operative hand therapy is a critical component of successful recovery.
In conclusion, the Moberg advancement flap stands as a reliable and effective procedure for thumb pulp reconstruction, offering excellent functional and aesthetic outcomes by providing durable, sensate, and well-vascularized local tissue coverage. Its continued relevance in modern hand surgery algorithms highlights its advantages over many alternative techniques for appropriate indications.
