Superficial Radial Nerve Injury: A Clinical Case Study on Diagnosis in the Anatomical Snuffbox
Key Takeaway
Superficial radial nerve (SRN) injury is diagnosed via meticulous sensory assessment in its distribution, especially the dorsal thumb web space. Intact radial nerve motor function rules out deeper involvement. Key diagnostic tests include two-point discrimination, light touch, and pinprick sensation, comparing with the contralateral hand to confirm isolated sensory loss after wrist laceration.
Patient Presentation & History
A 34-year-old right-hand dominant male presented to the emergency department following a fall onto broken glass during a DIY accident. He sustained a laceration to the dorsoradial aspect of his left wrist, specifically over the anatomical snuffbox. The injury occurred approximately 2 hours prior to presentation. He reports immediate, sharp pain and significant bleeding, which he managed with direct pressure. He also noticed a "pins and needles" sensation and numbness dorsally, particularly over the thumb and index finger web space, immediately after the injury.
His past medical history includes well-controlled essential hypertension, for which he takes lisinopril. He has no known allergies and no prior surgical history. He is a non-smoker and consumes alcohol socially. His tetanus immunization status is up to date. He is an IT professional, requiring fine motor skills and significant computer use with his dominant right hand, but also requires full function of his non-dominant left hand for bimanual tasks and leisure activities (e.g., cycling).
The mechanism of injury suggests a direct, sharp transection. The location is highly suspicious for superficial radial nerve (SRN) involvement, given its superficial course in this region, particularly as it emerges from beneath the brachioradialis tendon and divides into its terminal sensory branches.
Clinical Examination
Upon initial assessment, the patient was hemodynamically stable.
Inspection
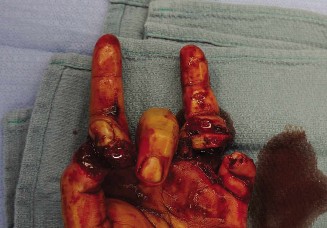
- A 3 cm, clean, linear laceration was noted obliquely across the anatomical snuffbox of the left wrist, extending distally towards the first web space.
- No active bleeding was observed, but a significant hematoma was present around the wound, indicating recent hemorrhage.
- No obvious gross deformity of the wrist or hand.
- Skin color, temperature, and turgor appeared normal, indicating intact peripheral perfusion.
- No significant swelling of the hand or digits, suggesting compartment syndrome was unlikely at this early stage.
-

- Caption: Dorsoradial laceration over the anatomical snuffbox, concerning for superficial radial nerve injury.
Palpation
- Tenderness was localized to the laceration site and surrounding soft tissues.
- No crepitus was elicited, suggesting no underlying fracture.
- Capillary refill was brisk (<2 seconds) in all digits.
- Radial and ulnar pulses were strong and palpable at the wrist.
- No palpable foreign body was identified, though the hematoma obscured definitive assessment.
Range of Motion
- Wrist: Active and passive range of motion were full and pain-free in flexion, extension, ulnar deviation, and radial deviation.
- Thumb: Full range of motion for carpometacarpal (CMC), metacarpophalangeal (MCP), and interphalangeal (IP) joints, with intact opposition and adduction.
- Fingers: Full active and passive range of motion in all MCP and IP joints, with no deficits in flexion or extension.
- All tendon gliding appeared normal, and no tendon lacerations were evident based on active movement.
Neurological Assessment
This was the cornerstone of the examination, specifically focusing on the radial nerve and its branches:
-
Motor Function (Deep Radial Nerve / Posterior Interosseous Nerve - PIN):
-
Wrist Extension:
Strong and pain-free against resistance.
- ECRL/ECRB: Tested by radial and central wrist extension respectively. Both were intact, indicating robust radial nerve motor function proximal to its division.
- Finger Extension: Full and strong extension of MCP joints of all fingers against resistance (extensor digitorum communis, EDC).
- Thumb Extension: Full and strong extension of the MCP and IP joints of the thumb (extensor pollicis longus, EPL; extensor pollicis brevis, EPB).
- Thumb Abduction: Strong abduction of the thumb in the plane of the palm (abductor pollicis longus, APL).
- Supination: Strong supination against resistance (supinator).
- Interpretation: The integrity of these motor functions effectively ruled out a complete deep radial nerve or PIN injury at the level of the forearm, confirming the injury was distal to the motor branch innervation.
-
Wrist Extension:
Strong and pain-free against resistance.
-
Sensory Function (Superficial Radial Nerve - SRN): This required meticulous assessment.
-
Two-point Discrimination (2PD):
- Dorsal aspect of thumb web space (SRN territory): >10 mm (significantly impaired or absent).
- Dorsal aspect of radial side of index finger: >10 mm (significantly impaired or absent).
- Dorsal aspect of ulnar side of index finger and radial side of middle finger: >10 mm (significantly impaired or absent).
- Comparison with contralateral hand: Contralateral values were typically 5-7 mm in these areas.
-
Light Touch (Cotton Swab):
Absent or severely diminished sensation in the typical distribution of the SRN:
- Dorsal thumb.
- Dorsal radial aspect of the index finger.
- Dorsal aspect of the first web space (the most consistent and reliable test area for SRN).
- Dorsal aspects of the radial half of the middle finger.
- Pinprick Sensation: Consistent with light touch deficits in the SRN distribution.
- Temperature Sensation: Impaired in the same distribution.
- Specific Testing for SRN: Special attention was paid to the dorsal thumb web space. This area is innervated exclusively by the SRN and is a critical zone for diagnosis. Pressure on the nerve proximal to the laceration did not elicit paresthesias distally, which might be expected with incomplete laceration or neuropraxia.
- Interpretation: The selective sensory loss in the superficial radial nerve distribution, with intact motor function of radial nerve-supplied forearm muscles, strongly indicated a laceration or severe injury to the SRN or its terminal branches distal to the motor innervation.
-
Two-point Discrimination (2PD):
-
Other Nerves (for completeness and ruling out concomitant injuries):
-
Median Nerve:
- Motor: Intact opposition (abductor pollicis brevis, opponens pollicis), flexion of thumb IP (flexor pollicis longus), and flexion of index/middle finger DIPs (flexor digitorum profundus).
- Sensory: Intact sensation over the palmar aspect of the thumb, index, middle, and radial half of the ring finger; normal 2PD on volar index fingertip.
-
Ulnar Nerve:
- Motor: Intact abduction of the little finger (abductor digiti minimi), adduction of the index finger (first dorsal interosseous), and thumb adduction (adductor pollicis).
- Sensory: Intact sensation over the palmar and dorsal aspects of the little finger and ulnar half of the ring finger; normal 2PD on volar little fingertip.
- Interpretation: Median and ulnar nerve functions were entirely intact, further localizing the injury to the radial nerve territory.
-
Median Nerve:
Vascular Assessment
- Allen's test: Performed for both radial and ulnar arteries; demonstrated good collateral flow.
- Capillary refill: Brisk in all digits.
- Pulses: Radial and ulnar pulses palpable and strong.
- Interpretation: No evidence of vascular compromise.
Imaging & Diagnostics
Radiographs
-
Left Wrist (PA, Lateral, Oblique views):
- No evidence of fracture, dislocation, or subluxation involving the carpals, metacarpals, or distal radius/ulna.
- No radiopaque foreign body was identified.
- Soft tissue swelling was noted dorsoradially, correlating with the clinical findings.
- Interpretation: Ruled out skeletal injury and metallic foreign bodies, but cannot exclude non-radiopaque foreign bodies (e.g., glass) or soft tissue injuries.
Ultrasound (Bedside / Point-of-Care)
-
Left Dorsal Wrist:
- Linear transducer was used to assess the soft tissues around the laceration.
- A hypoechoic defect consistent with a hematoma was visualized adjacent to the laceration.
- Careful scanning identified a transected superficial radial nerve within the hematoma, characterized by disrupted nerve fascicles and a retracted nerve stump proximally. The distal stump was also identified.
- No clear foreign body was definitively visualized; however, glass can be challenging to detect ultrasonographically due to acoustic shadowing, depending on its size and orientation.
- Interpretation: Provided direct evidence of superficial radial nerve transection, which significantly aided surgical planning.
Further Imaging Considerations (Not performed in this immediate acute setting but relevant for teaching)
- CT Scan: While not routinely indicated for isolated soft tissue lacerations, a CT scan would be invaluable if there was suspicion of an occult fracture or a non-radiopaque foreign body (e.g., small glass fragments) that could not be localized by X-ray or ultrasound. Fine-cut CT can often detect glass.
- MRI: Generally not indicated in the acute setting for a clear laceration. However, in cases of closed traction injuries or blunt trauma with persistent nerve deficit and no obvious laceration, MRI could help evaluate nerve continuity, edema, or neuroma formation in a subacute or chronic phase.
Templating
- Not applicable in this acute nerve laceration repair scenario. Templating is typically used for joint arthroplasty, fracture fixation with plates, or reconstructive procedures requiring precise implant sizing.
Differential Diagnosis
The clinical presentation, particularly the isolated sensory deficit in the superficial radial nerve distribution following a laceration in the anatomical snuffbox, strongly points to a superficial radial nerve injury. However, a comprehensive differential diagnosis is crucial for all hand injuries.
| Feature / Condition | Superficial Radial Nerve Laceration (Our Case) | Posterior Interosseous Nerve (PIN) Palsy / Injury | Radial Sensory Branch of the Median Nerve Injury (e.g., Palmar Cutaneous Nerve) | Cervical Radiculopathy (e.g., C6) |
|---|---|---|---|---|
| Mechanism | Direct laceration, crush injury, iatrogenic during surgical approach to distal radius/DRUJ. | Proximal forearm trauma (e.g., Monteggia fracture-dislocation), direct trauma to supinator region, chronic compression (arcade of Frohse), tumor. | Laceration at the volar-radial aspect of the wrist, carpal tunnel surgery. | Disc herniation, foraminal stenosis, tumor, trauma to cervical spine. |
| Motor Deficit | None (SRN is purely sensory). | Weakness/Paralysis of forearm/hand extensors: Wrist extension (radial deviation), finger MCP extension, thumb MCP/IP extension, thumb abduction (APL). Wrist radial deviation is often preserved (ECRL). | None (Palmar cutaneous nerve is purely sensory). | Weakness/Atrophy: Biceps, brachioradialis, wrist extensors. |
| Sensory Deficit | Dorsal aspect: Thumb, first web space (most consistent), radial side of index finger, radial half of middle finger. | None (PIN is purely motor). | Volar aspect: Thenar eminence, proximal palmar radial aspect of the hand. Not digits. | Dermatomal distribution: C6 (thumb and index finger, radial forearm). Can be both volar and dorsal. |
| Pain Pattern | Localized wound pain, neuropathic pain (dysethesias, hyperalgesia) in SRN distribution. | Deep aching pain in proximal forearm, potential radial nerve territory pain. | Localized wrist pain, neuropathic pain in palmar cutaneous nerve distribution. | Neck and shoulder pain, radiating into arm and hand. Radicular pain. |
| Tinel's Sign | Positive at the laceration site, radiating distally in SRN territory. | Usually negative in the wrist/hand. Positive at site of compression/injury in proximal forearm. | Positive at volar wrist, proximal to median nerve distribution. | Negative at wrist/hand. Positive over cervical spine nerve root. |
| Imaging Findings | Soft tissue laceration, nerve discontinuity on ultrasound. | Normal X-ray/MRI of wrist/hand. MRI forearm may show nerve edema/compression, or cause. | Soft tissue laceration. | MRI cervical spine: Disc herniation, stenosis, nerve root compression. |
| Key Differentiating Factor | Pure sensory deficit on the dorsum of the hand, no motor involvement. | Pure motor deficit of extensors, no sensory deficit in the hand. | Pure sensory deficit on the volar-radial aspect of the hand, not digits. | Myotomal and dermatomal distribution (proximal to distal), often with neck symptoms. |
Caption: Anatomic course and sensory distribution of the superficial radial nerve (green) relative to the posterior interosseous nerve (yellow). Note the purely sensory role of the SRN in the hand/wrist.
Surgical Decision Making & Classification
The decision for operative intervention in this case was straightforward and made urgently due to the clear evidence of a sharp, traumatic superficial radial nerve laceration.
Why Operative Intervention?
- Clear Nerve Transection: Clinical examination demonstrated a complete sensory deficit consistent with SRN laceration. Ultrasound confirmed nerve discontinuity. Sharp lacerations generally do not heal spontaneously with functional nerve regeneration across a gap.
- Location: The injury was distal to the motor branches of the radial nerve, meaning the functional deficit would be purely sensory, but in a critical area for sensation (first web space, dorsal thumb, radial index finger). Loss of sensation here significantly impairs fine motor tasks and grip, impacting quality of life and increasing risk of unnoticed injury.
- Nature of Injury: A clean laceration typically allows for primary nerve repair with good outcomes, especially when performed early. Delay can lead to nerve stump retraction, fibrosis, and neuroma formation, making repair more challenging and prognostically less favorable.
- Foreign Body Exclusion: While X-ray showed no radiopaque foreign body, the potential for embedded glass fragments (non-radiopaque) within the wound or nerve tissue necessitated surgical exploration for thorough debridement and foreign body removal to prevent chronic infection or inflammatory response.
Why Not Non-Operative?
Non-operative management (observation) would only be considered for:
*
Neuropraxia or Axonotmesis without Laceration:
If the nerve was thought to be bruised or stretched but in continuity, observation for spontaneous recovery would be appropriate. Our case involved a laceration.
*
Minor Sensory Branches:
While the SRN is primarily sensory, its terminal branches supply significant areas. Minor, isolated sensory branch injuries might be observed, but a laceration of the main SRN trunk or its significant divisions warrants repair.
Classification (Not a formal classification system for SRN injury but rather principles of nerve injury)
-
Sunderland Classification (Modified Seddon's):
- Type V (Neurotmesis): This injury involves complete transection of the nerve, including the epineurium, perineurium, and endoneurium. This is the presumed classification in our case based on clinical and ultrasound findings. Sunderland Type V injuries require surgical repair for any chance of meaningful recovery.
Surgical Technique / Intervention
Pre-operative Planning
- Informed consent was obtained, detailing the risks of nerve repair (infection, bleeding, persistent deficit, neuroma formation, stiffness, complex regional pain syndrome) and potential need for nerve grafting if primary repair was not possible.
- Antibiotic prophylaxis (e.g., Cefazolin 2g IV) was administered.
- Tourniquet time management was discussed.
Patient Positioning
- The patient was placed supine on the operating table with the left arm extended and abducted on a hand table.
- The elbow was slightly flexed, and the forearm pronated to expose the dorsoradial aspect of the wrist.
- A tourniquet was applied to the upper arm.
Anesthesia
- General anesthesia was administered. Regional block (e.g., axillary block) could also be considered for post-operative pain management.
Surgical Approach
- Sterile Preparation and Draping: The entire left arm and hand were prepped and draped in a sterile fashion.
- Tourniquet Inflation: The tourniquet was inflated to 250 mmHg.
-
Wound Debridement & Extension:
- The existing laceration was meticulously debrided to remove devitalized tissue and foreign contaminants.
- The incision was extended proximally and distally along the anatomical course of the superficial radial nerve in a curvilinear fashion to allow for adequate exposure and identification of healthy nerve ends. This curvilinear extension avoids crossing skin creases at right angles, which can lead to scar contractures.
- Hematoma Evacuation: The significant hematoma was evacuated, improving visualization.
-
Identification of Anatomical Structures:
- Careful blunt and sharp dissection was performed, preserving vital surrounding structures.
- The extensor pollicis longus (EPL) and extensor pollicis brevis (EPB) tendons were identified, forming the borders of the anatomical snuffbox.
- The cephalic vein was identified and carefully retracted or ligated if necessary.
- The main trunk of the superficial radial nerve was identified proximal to the laceration, emerging from beneath the brachioradialis. Its branching pattern distally was also followed.
- Crucial Step: Both the proximal and distal stumps of the transected superficial radial nerve were identified. The nerve typically divides into several branches in this region: dorsal digital nerves to the thumb, dorsal digital nerves to the radial side of the index finger, and a branch to the first web space. All suspected branches were systematically identified and tagged with fine sutures (e.g., 6-0 Prolene on a non-cutting needle) to prevent retraction and facilitate repair.
- Careful irrigation and exploration for any glass fragments were performed. No embedded glass was found.
-
Nerve Preparation:
- Under high magnification (loupes 3.5x and operative microscope 10x-20x), the nerve ends were sharply debrided back to healthy fascicular tissue using a fresh razor blade on a cutting block. This ensures clean, viable tissue for coaptation and minimizes the risk of neuroma formation.
- The nerve stumps were inspected for any tension-free approximation. In this case, due to the clean laceration and minimal retraction, a tension-free repair appeared feasible.
-
Nerve Repair (Epineurial Repair):
- The nerve stumps were carefully aligned to ensure fascicular orientation was maintained (rotational alignment). This is critical for optimal regeneration.
- Primary epineurial repair was performed using 8-0 or 9-0 non-absorbable monofilament sutures (e.g., nylon) on a delicate micro-needle.
- Initially, two cardinal sutures were placed 180 degrees apart to secure rotational alignment.
- Subsequently, 4-6 interrupted sutures were placed around the circumference of the epineurium, ensuring that no fascicles were "dog-eared" or trapped outside the repair site. The goal was watertight coaptation without tension.
- Consideration: If a tension-free primary repair was not possible (e.g., due to significant nerve gap or retraction), nerve grafting (e.g., sural nerve autograft) would have been necessary. This was not required in this case.
-
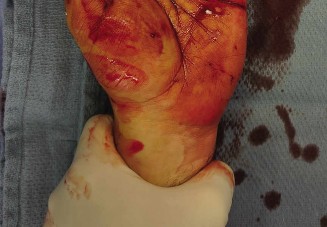
Wound Closure:
- The tourniquet was deflated, and hemostasis was achieved.
- The subcutaneous tissues were closed with interrupted 4-0 absorbable sutures (e.g., Vicryl).
- The skin was closed with 4-0 non-absorbable sutures (e.g., nylon) in an interrupted fashion.
- A sterile dressing was applied.
Post-Operative Dressing
- A bulky soft dressing was applied, followed by a volar plaster splint, immobilizing the wrist in slight extension (approximately 20-30 degrees) to minimize tension on the nerve repair. The thumb was included in the splint in a position of rest.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Phase (0-3 weeks)
- Immobilization: The wrist and thumb remained immobilized in the volar plaster splint, protecting the nerve repair site from tension and accidental movement.
- Pain Management: Oral analgesics (e.g., acetaminophen, NSAIDs) were prescribed. Neuropathic pain medications (e.g., gabapentin, pregabalin) were considered if dysesthesia was significant.
- Wound Care: The dressing was kept dry and clean. Suture removal typically occurred at 10-14 days post-op.
- Patient Education: Patients were counseled on protecting the hand, avoiding excessive movement, and recognizing signs of infection. Importance of not relying on sensation in the affected area was emphasized.
- Elevation: Continued elevation of the hand to reduce swelling.
Early Mobilization Phase (3-6 weeks)
- Splint Removal and Transition: At 3 weeks, the plaster splint was removed, and a custom thermoplastic removable splint was fabricated, maintaining the wrist in a neutral to slight extension position.
-
Hand Therapy Initiation:
Formal hand therapy was initiated.
- Gentle Passive Range of Motion (PROM): Careful, gentle PROM of the wrist and thumb, ensuring no excessive tension on the nerve.
- Nerve Gliding Exercises: These were introduced cautiously to encourage nerve mobility and prevent adhesions, guided by the hand therapist. Examples include radial nerve gliding exercises with wrist flexion/extension, forearm pronation/supination, and elbow extension.
- Edema Management: Gentle massage, compression gloves, and elevation techniques.
- Scar Management: Desensitization, massage, and silicone sheeting to minimize hypertrophic scarring.
- Sensory Re-education (Initial Stages): Patients were encouraged to explore various textures with their radial hand but reminded that functional sensation might take many months to return.
Intermediate Rehabilitation Phase (6 weeks - 3 months)
- Progressive ROM and Strengthening: Gradual increase in active and passive range of motion for the wrist and thumb. Gentle isometric strengthening exercises for hand and wrist muscles not affecting the repair site.
- Nerve Gliding: Continued emphasis on nerve gliding exercises.
-
Sensory Re-education (Intermediate Stages):
- Protective Sensation: Begin to re-test light touch, pinprick, and temperature.
- Localization and Discrimination: Use sensory mapping tools, varying textures (cotton, felt, sandpaper), and object identification with eyes closed.
- Graphesthesia and Stereognosis: Introduce these once basic sensation improves.
- Fine Motor Coordination: Introduction of activities requiring increasing dexterity.
- Desensitization: If hypersensitivity or neuropathic pain persists.
Late Rehabilitation Phase (3 months - 1 year)
- Functional Integration: Progressive return to daily activities, work, and leisure.
- Strengthening: Advanced strengthening exercises.
- Sensory Re-education (Advanced Stages): Intensive sensory re-education to optimize cortical reorganization and maximize functional recovery. This phase can be prolonged and requires patient dedication.
- Monitoring for Complications: Close monitoring for signs of neuroma formation, persistent neuropathic pain, or scar adhesions. Revision surgery for symptomatic neuroma might be considered if conservative measures fail.
- Return to Activity: Gradual return to full activity based on functional assessment and nerve regeneration progress (typically 1 mm per day).
Expected Outcome:
Superficial radial nerve repairs generally have a favorable prognosis for sensory recovery, particularly with early, tension-free primary repair. Full recovery of normal sensation is rare, but useful protective sensation, and often good discriminative sensation, can be achieved over 12-18 months. Patients are educated that residual numbness, dysesthesia, or altered sensation may persist.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls for Radial Nerve Diagnosis and Management
- Anatomical Precision: The superficial radial nerve is purely sensory. Any motor deficit indicates a more proximal radial nerve injury (e.g., in the forearm or arm) or a deep radial nerve/PIN injury. Distinguish this clearly.
- Sensory Distribution is Key: The dorsal thumb web space (first interdigital cleft) is the most consistent and reliable area for testing SRN function, as it has minimal overlap with other nerve territories.
- Anatomical Variation: Be aware of the significant variability in the branching pattern of the superficial radial nerve. It typically divides into two or more branches near the snuffbox, so meticulous exploration is crucial to identify all affected branches.
- Careful Examination in Distracted Patients: In cases of significant pain or multiple injuries, a subtle sensory deficit can be missed. Re-examination once pain is controlled is essential.
- Tourniquet Time: Be mindful of tourniquet time during nerve repair; prolonged ischemia can compromise nerve viability.
- Magnification is Mandatory: Nerve repair, even for "purely sensory" nerves, requires high magnification (loupes at minimum, operating microscope preferred) and microsurgical instruments for optimal coaptation.
- Tension-Free Repair: The most critical factor for successful nerve regeneration is a tension-free repair. If a gap exists, nerve grafting (e.g., sural nerve, medial antebrachial cutaneous nerve) is preferable to a high-tension repair.
- Early Referral to Hand Therapy: Prompt initiation of specialized hand therapy post-operatively is paramount for optimal functional recovery, including edema control, scar management, nerve gliding, and sensory re-education.
- Differential Diagnosis for Dorsal Wrist Pain/Numbness: Always consider other entities such as De Quervain's tenosynovitis (may cause radial-sided wrist pain, but specific sensory loss is absent), Intersection Syndrome, and even cervical radiculopathy for radial-sided arm symptoms (though usually more proximal).
Pitfalls to Avoid
- Missing a Nerve Laceration: Underestimating the extent of injury based solely on X-rays or a quick clinical assessment. Always assume nerve involvement with lacerations crossing known nerve pathways until proven otherwise.
- Inadequate Exploration: Not adequately exploring the wound to identify all nerve stumps or associated foreign bodies. Retraction of nerve ends can make them difficult to find without extending the incision.
- Poor Rotational Alignment: Failing to correctly align the nerve stumps rotationally. This can lead to axons growing into inappropriate distal fascicles, resulting in poor functional recovery.
- Repair Under Tension: Attempting to force a nerve repair if there is a gap, leading to suture line disruption or poor regeneration. This necessitates a nerve graft.
- Inadequate Post-Operative Immobilization: Premature or excessive motion can disrupt the delicate nerve repair.
- Neglecting Sensory Re-education: Assuming the nerve will spontaneously recover sensation without active patient participation and guided therapy. Sensory re-education is a long and arduous process, but essential.
- Overlooking Neuroma Formation: Persistent or increasing localized pain at the repair site, especially with percussion (Tinel's sign), may indicate a painful neuroma, which might require further intervention.
- Iatrogenic Injury: During surgical approaches to the distal radius or DRUJ, the superficial radial nerve is at risk. Always identify and protect it.
- Misdiagnosis of Wartenberg's Syndrome: Wartenberg's syndrome (cheiralgia paresthetica) is an entrapment neuropathy of the superficial radial nerve, typically at the point where it exits the fascia between brachioradialis and extensor carpi radialis longus (ECRL). This presents with similar sensory symptoms but no history of acute laceration. Differentiate traumatic injury from compression.
- Ignoring Psychiatric Impact: Chronic nerve pain and sensory loss can have significant psychological effects. Address these proactively.
