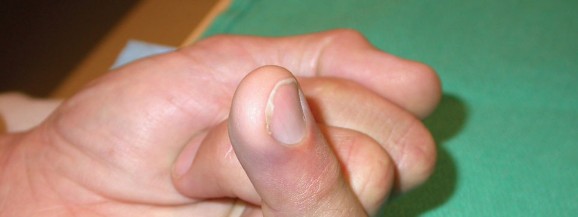
Jersey Finger: Tendon Avulsion at the Base of the Distal Phalanx

Key Takeaway
Learn more about Jersey Finger: Tendon Avulsion at the Base of the Distal Phalanx and how to manage it. A "jersey finger" is an avulsion injury where the flexor profundus tendon detaches from its insertion at the base of the distal phalanx. This injury typically prevents the patient from fully flexing the distal interphalangeal (DIP) joint and often presents with pain, swelling, and bruising, especially after a forceful hyperextension injury. Early surgical repair is usually recommended.
Introduction & Epidemiology
Jersey finger refers to an avulsion injury of the flexor digitorum profundus (FDP) tendon from its insertion at the palmar base of the distal phalanx. This injury typically occurs when the FDP tendon is subjected to forceful eccentric contraction while the distal interphalangeal (DIP) joint is rapidly and forcibly extended. The classic mechanism involves a finger, often the ring finger, catching on an opponent's jersey during athletic activities, leading to forced extension of an actively flexed DIP joint while the proximal interphalangeal (PIP) joint and metacarpophalangeal (MCP) joint remain relatively flexed. This dynamic places maximal stress on the FDP insertion.
While commonly associated with American football, Jersey finger can occur in various sports and occupational settings involving forceful gripping and tearing motions. The ring finger is most frequently affected due to its relative laxity and tendency to be more exposed during gripping activities. The injury can occur in isolation or, less commonly, as part of a more complex hand trauma.
Clinical presentation typically includes acute pain at the palmar aspect of the DIP joint, swelling, and ecchymosis. The hallmark sign is the inability of the patient to actively flex the DIP joint in isolation while the MCP and PIP joints are held in extension. Palpation may reveal tenderness at the base of the distal phalanx, and a palpable mass or fullness may be present in the palm if the tendon has retracted significantly. Early diagnosis and intervention are critical for optimal functional outcomes.
The most widely accepted classification system, introduced by Leddy and Packer in 1972, categorizes FDP avulsions based on the degree of tendon retraction and the presence of a bony avulsion fragment. This classification dictates the urgency and surgical approach:
- Type I: The FDP tendon is completely avulsed from the distal phalanx and retracts into the palm. This occurs because the vinculum longum is torn, compromising the tendon's blood supply and tethering. These are considered surgical emergencies due to the risk of tendon ischemia and permanent shortening.
- Type II: The FDP tendon retracts to the level of the PIP joint. The vinculum longum may be partially intact, providing some tethering and maintaining a blood supply. While less urgent than Type I, repair within 2-3 weeks is generally recommended.
- Type III: A large bony fragment is avulsed with the FDP tendon, which typically retracts to the level of the A4 pulley or proximal to the A3 pulley, blocked by its size. The fragment is often large enough to cause joint incongruity. This type requires surgical repair to restore joint stability and tendon function.
- Type IV: Described by Smith in 1981, this involves an avulsion of the FDP tendon and a small bony fragment, with the tendon itself having pulled through the bony fragment. This results in two fragments: the small piece attached to the tendon, which retracts, and a larger fragment left attached to the distal phalanx.
- Type V: An epiphyseal avulsion in skeletally immature patients, recently added to the classification, often treated similarly to Type III.
Understanding these types is paramount for guiding management decisions, particularly concerning surgical timing and technique.
Surgical Anatomy & Biomechanics
A thorough understanding of the flexor tendon anatomy and biomechanics is fundamental for successful repair of Jersey finger.
Flexor Digitorum Profundus (FDP) Tendon
The FDP originates from the ulna and interosseous membrane. Its muscle belly lies deep to the flexor digitorum superficialis (FDS) in the forearm. In the wrist, the four FDP tendons pass through the carpal tunnel, deep to the FDS tendons. Within the hand, each FDP tendon enters its respective fibrous flexor sheath at the level of the metacarpal neck.
The fibrous flexor sheath, composed of annular (A1-A5) and cruciate (C1-C3) pulleys, is crucial for maintaining the mechanical advantage of the flexor tendons and preventing bowstringing.
*
A1 pulley:
At the MCP joint.
*
A2 pulley:
At the proximal phalanx, proximal half.
*
A3 pulley:
At the PIP joint.
*
A4 pulley:
At the middle phalanx, middle.
*
A5 pulley:
At the DIP joint.
The FDP tendon passes through the split of the FDS tendon at the level of the proximal phalanx and continues distally, inserting onto the palmar base of the distal phalanx. This insertion is broad, allowing for strong flexion of the DIP joint.
Vascular Supply and Vinicula
The FDP tendon receives its vascular supply from segmental vessels and through the vincula. The vincula tendinum are mesotendinous structures that connect the flexor tendons to the palmar aspect of the phalanges.
*
Vinculum breve profundus (VBP):
Connects the FDP to the distal phalanx, just proximal to its insertion.
*
Vinculum longum profundus (VLP):
Connects the FDP to the proximal phalanx, typically at the level of the A2 pulley.
In Type I avulsions, both the VBP and VLP are typically disrupted, leading to complete retraction into the palm and compromised vascularity. In Type II injuries, the VLP may remain partially intact, tethering the tendon at the PIP joint level and preserving some blood supply. The integrity of these vincula significantly influences the degree of tendon retraction and the viability of the tendon stump.
Neurovascular Bundles
The digital neurovascular bundles run along the lateral aspects of the digits, volar to the mid-axial line, and must be carefully protected during surgical dissection. Each digit typically has two neurovascular bundles, containing the proper digital artery, proper digital nerve, and accompanying veins. These structures are superficial to the flexor tendon sheath but deep to the subcutaneous fat.
Biomechanics of Injury
The FDP tendon is the sole flexor of the DIP joint. Its avulsion results in a complete loss of active DIP joint flexion. The injury mechanism (forced hyperextension of an actively flexing digit) creates a substantial tensile load that exceeds the strength of the tendon's insertion, leading to either a pure tendinous avulsion or an avulsion fracture. The elasticity of the tendon and the tethering effect of the vincula determine the degree of retraction.
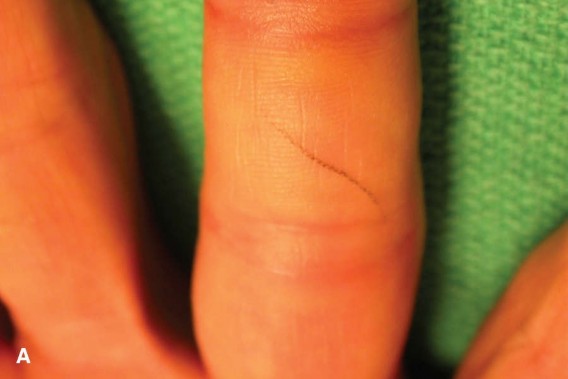
Indications & Contraindications
The decision for operative versus non-operative management of a Jersey finger injury is primarily guided by the Leddy and Packer classification, the acuity of the injury, and patient-specific factors.
Indications for Operative Treatment
- Leddy and Packer Type I Avulsion: Complete FDP avulsion with retraction to the palm. This is considered a surgical emergency due to the compromised vascularity of the tendon and the potential for irreversible shortening. Repair is ideally performed within 7-10 days of injury.
- Leddy and Packer Type II Avulsion: FDP avulsion with retraction to the PIP joint level. While less urgent than Type I, surgical repair is still recommended, typically within 2-3 weeks, to prevent tendon shortening and facilitate functional recovery.
- Leddy and Packer Type III Avulsion: FDP avulsion with a large bony fragment. Surgical repair is indicated to restore both tendon function and anatomical joint congruity, preventing long-term instability and degenerative changes.
- Leddy and Packer Type IV Avulsion: FDP tendon avulsed with a small bony fragment, with the tendon pulling through a larger avulsed bony fragment. This requires surgical intervention to reattach the tendon and address the remaining bony fragment.
- Leddy and Packer Type V Avulsion: Epiphyseal avulsion in pediatric patients. Operative fixation is generally indicated to restore growth plate alignment and tendon function.
- Acute complete FDP rupture: Regardless of the specific Leddy and Packer type, any acute, complete rupture of the FDP tendon resulting in a significant functional deficit (inability to actively flex the DIP joint) warrants surgical consideration in an otherwise healthy and compliant patient.
- Chronic injuries (typically >6 weeks) with functional deficit: While primary repair becomes more challenging due to tendon shortening and scarring, surgical options such as tendon reconstruction with grafting, FDP tenodesis, or DIP joint arthrodesis may be considered to improve hand function and alleviate symptoms. These require careful patient selection and realistic expectations.
Contraindications for Operative Treatment
- Significant Soft Tissue Compromise: Open wounds, severe contamination, or extensive tissue loss that precludes primary closure and successful tendon healing. These may require staged procedures or alternative management.
- Active Infection: Local or systemic infection must be controlled before elective tendon repair to minimize the risk of post-operative complications.
- Severe Concomitant Injuries: Other critical injuries that take precedence or make hand therapy impossible.
- Patient Unwillingness or Inability to Comply with Post-operative Rehabilitation: FDP repair requires a highly compliant patient for intensive and prolonged hand therapy. Non-compliance significantly increases the risk of rupture, stiffness, and poor outcomes.
- Severe Medical Comorbidities: Patients with significant comorbidities that make surgery or anesthesia too risky.
- Partial Tendon Tears: If the FDP tendon is only partially torn and there is active, albeit weak, DIP joint flexion, non-operative management with splinting and gradual rehabilitation may be considered. However, close monitoring is essential to detect progression to a complete rupture.
- Very Chronic Injuries (>6-12 weeks) with Significant Tendon Retraction and Poor Tendon Quality: In these cases, primary repair may not be feasible or durable. Alternatives such as FDP tenodesis (fixation of the FDP to the middle phalanx), DIP joint arthrodesis (fusion), or staged tendon reconstruction may be more appropriate.
Operative vs. Non-Operative Indications Summary
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Acuteness | Acute complete ruptures (Leddy & Packer Type I, II, III, IV, V) within 3 weeks. | Partial tears with preserved active DIP flexion. Acute injuries in patients with severe medical comorbidities, active infection, or profound non-compliance. |
| Injury Type | Tendon avulsion (Type I, II). Avulsion fracture (Type III, IV, V). Ruptures requiring reattachment. | Partial tears. Chronic injuries (>6-12 weeks) with significant tendon shortening and scarring where primary repair is unlikely to succeed, and patient declines reconstructive options or arthrodesis. Very old/debilitated patients where functional demand is low. |
| Functional Goal | Restoration of active DIP flexion, joint stability, and full functional range of motion. | Maintenance of existing function, pain relief. Acceptance of DIP joint inability to flex actively in exchange for avoiding surgery or managing high-risk patients. |
| Patient Factors | Healthy, motivated, and compliant patients capable of rigorous post-operative therapy. | Patients unwilling or unable to participate in post-operative rehabilitation. Patients with contraindications to surgery (e.g., severe comorbidities, active infection). Patients with low functional demands (e.g., very elderly, sedentary) who prioritize avoiding surgery risks. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential to optimize outcomes for Jersey finger repair. This includes accurate diagnosis, appropriate timing of surgery, thorough patient education, and careful preparation of the surgical field.
Diagnostic Workup
-
Clinical Examination: The cornerstone of diagnosis.
- Inability to actively flex the DIP joint of the affected finger while the PIP joint is held in extension (specific test for FDP integrity).
- Pain, swelling, and tenderness at the palmar base of the distal phalanx.
- Palpation for a retracted tendon mass (e.g., in the palm for Type I).
- Assessment of passive range of motion to rule out mechanical blocks or adhesions.
- Neurovascular examination of the digit.
-
Imaging:
- Plain Radiographs (AP, lateral, oblique views of the affected digit): Essential to rule out associated fractures, especially avulsion fractures of the distal phalanx (Leddy and Packer Type III, IV, V). The lateral view is crucial for assessing the size and displacement of any bony fragment.
- Ultrasound: Can be a useful adjunct, particularly in the acute setting, to visualize the retracted tendon stump, assess the extent of retraction, and confirm the absence of an avulsion fracture. It is operator-dependent.
- Magnetic Resonance Imaging (MRI): While not routinely required for acute, straightforward cases, MRI can be valuable in chronic injuries or equivocal presentations to assess tendon quality, extent of retraction, scar tissue, and integrity of surrounding structures. It offers excellent soft tissue contrast but is costly and not always immediately available.

Timing of Surgery
The urgency of surgical repair is dictated by the Leddy and Packer classification:
*
Type I:
Most urgent. Ideally within 7-10 days due to potential for tendon ischemia (loss of vincula) and irreversible shortening. Beyond this window, direct repair becomes progressively more difficult, and the risk of tendon necrosis increases.
*
Type II:
Less urgent than Type I, but still recommended within 2-3 weeks to minimize tendon retraction and scarring.
*
Type III, IV, V:
Repair within 2-3 weeks is generally accepted to ensure reduction of the bony fragment and reattachment of the tendon before significant scarring or malunion occurs.
Patient Education
Comprehensive patient counseling is crucial. Patients must understand:
* The nature of the injury and the surgical procedure.
* The importance of immediate and rigorous post-operative hand therapy.
* The potential for complications (e.g., re-rupture, stiffness, infection).
* Realistic expectations regarding functional recovery, which often takes several months, and the possibility of residual stiffness or reduced strength.
* The potential need for secondary procedures (e.g., tenolysis) if adhesions develop.
Anesthesia
- Regional Anesthesia: An axillary or supraclavicular block is frequently preferred, providing excellent intra-operative anesthesia and post-operative analgesia. This allows the patient to remain awake and comfortable, potentially aiding in intra-operative tendon tension assessment if needed (though not typically required for FDP repair).
- General Anesthesia: An alternative option, especially for anxious patients or those with contraindications to regional blocks.
Tourniquet Application
A pneumatic tourniquet (forearm or upper arm) is applied to achieve a bloodless field, which is critical for precise dissection and identification of delicate structures. Pressure should be set to 250-300 mmHg for the arm or 200-250 mmHg for the forearm, or approximately 100 mmHg above systolic blood pressure. The tourniquet time should be closely monitored.
Patient Positioning
The patient is positioned supine on the operating table. The affected arm is abducted and placed on a specialized hand table, ensuring comfortable access for the surgeon and assistant. The elbow is typically flexed to allow for full extension of the wrist and fingers.
Instrumentation
Standard small-hand surgical instruments are required, including:
* Fine dissecting scissors and forceps.
* Small malleable retractors.
* Microsurgical instruments (if available, for neurovascular dissection).
* Loupes (2.5x to 4.5x magnification) are highly recommended for improved visualization.
* Tendon repair sutures (e.g., 3-0 or 4-0 non-absorbable monofilament suture like Prolene or FiberWire).
* Small K-wires (0.028" or 0.035") for temporary stabilization or transosseous fixation.
* Suture anchors (mini-anchors, typically 1.3-2.0 mm) with pre-loaded sutures.
* Small drill and appropriate drill bits for suture anchors or transosseous tunnels.
* Pull-out button or small lead shot for transosseous pull-out technique.
Detailed Surgical Approach / Technique
The goal of surgical repair is to reattach the FDP tendon securely to the distal phalanx, restoring its functional length and minimizing gapping at the repair site, while preserving neurovascular structures and the flexor pulley system.
Incision
The choice of incision is critical to provide adequate exposure while minimizing scarring and neurovascular injury.
*
Brunner Zig-Zag Incision:
This is the preferred incision for FDP repair, particularly over the flexor sheath of the digit. It provides excellent exposure, allows for extension proximally or distally if needed, and minimizes the risk of flexion contractures. The zig-zag limbs should be centered over the non-articulating parts of the phalanges and avoid the joint creases.
*
Mid-Axial Incision:
Can be used, particularly on the ulnar side of the ring finger. However, care must be taken to avoid violating the neurovascular bundle which is in close proximity. A curved mid-axial incision, slightly volar to the true mid-axial line, can offer good exposure.
Regardless of the incision, meticulous skin dissection and subcutaneous tissue handling are paramount.
Exposure and Tendon Retrieval
-
Skin and Subcutaneous Dissection: Elevate skin flaps, taking care to identify and protect the digital neurovascular bundles. These bundles lie volar to the mid-axial line, superficial to the flexor sheath, and must be gently retracted dorsally using small vessel loops or blunt retractors.

-
Flexor Sheath Incision: Incise the flexor sheath longitudinally to expose the FDP tendon and its contents. The A3 and A4 pulleys are often in the surgical field. It is generally recommended to preserve the A2 and A4 pulleys as much as possible to prevent bowstringing, but partial release or careful incision of A3 and a portion of A4 may be necessary for adequate exposure and tendon retrieval. If A2 or A4 must be completely released, reconstruction may be needed.
-
Tendon Retrieval: This is often the most challenging step, particularly for Type I injuries.
- Type I (retracted to palm): The tendon can be retrieved by milking it distally from the palm or proximal forearm. A "tendon retriever" tool, such as a small right-angle clamp or a Foley catheter, can be advanced proximally within the sheath to hook the tendon and pull it distally. In some cases, a separate small incision in the palm may be necessary to directly identify and mobilize the tendon.
- Type II (retracted to PIP joint): The tendon is usually located within the flexor sheath at the level of the proximal phalanx or PIP joint. It can typically be retrieved with fine forceps or a small tendon hook.
- Type III/IV/V (bony avulsion): The tendon (with or without bone fragment) will be found at the level of the distal phalanx or slightly proximal, often tethered by the avulsed fragment.
-
Tendon End Preparation: Once retrieved, the proximal tendon stump is inspected. Any frayed or necrotic tissue is carefully debrided. The tendon end is typically prepared for suture placement using a "fish-mouth" or oblique cut to create a larger surface area for repair and minimize bulk.
Preparation of the Distal Phalanx
The insertion site on the palmar aspect of the distal phalanx must be meticulously prepared.
*
Debridement:
Remove any remaining tendon remnants, granulation tissue, or non-viable bone. The bone surface should be decorticated (freshened) to promote tendon-to-bone healing.
*
Drill Holes/Trough:
For direct tendon reinsertion, drill holes or a small trough are created.
*
Transosseous tunnels:
Typically two tunnels are drilled from the palmar aspect of the distal phalanx, exiting dorsally through the nailbed. These holes should be placed distal to the articular cartilage, converging slightly.
*
Suture anchor placement:
For suture anchor techniques, a small pilot hole is drilled into the palmar base of the distal phalanx, and the anchor is inserted, ensuring secure purchase in the bone.
Fixation Techniques
Several techniques are available, each with advantages and disadvantages. The choice depends on surgeon preference, tendon quality, and the presence of a bony fragment.
-
Transosseous Pull-Out Suture Technique (Common for Type I and II):
- Suture Placement: A strong non-absorbable suture (e.g., 3-0 or 4-0 FiberWire, Prolene) is woven through the prepared FDP tendon stump using a modified Kessler, modified Bunnel, or Krakow stitch. This creates a robust core purchase.
- Tunneling: The ends of the tendon repair sutures are then passed through the previously drilled transosseous tunnels in the distal phalanx, exiting dorsally through the nail. A Keith needle or a suture passer can facilitate this.
-
Tensioning and Securing:
The sutures are retrieved dorsally and tied over a button (e.g., orthopedic button or a piece of sterile tubing) or lead shot placed on the dorsum of the nail. The DIP joint is held in 30-45 degrees of flexion during tensioning to achieve appropriate tension, avoiding excessive slack or overtensioning. The knot is tied securely.
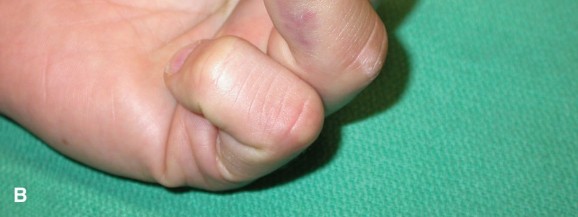
-
Suture Anchor Technique (Increasingly Popular for Type I and II):
- Anchor Placement: One or two mini-suture anchors are implanted into the palmar base of the distal phalanx, distal to the articular surface. Ensure adequate bone purchase.
- Suture Placement: The sutures pre-loaded on the anchors are passed through the FDP tendon stump using a robust stitch (e.g., modified Kessler or Krakow).
- Tensioning and Securing: With the DIP joint positioned in slight flexion (30-45 degrees), the sutures are tied down over the tendon stump directly to the anchor. This creates a secure tendon-to-bone interface without the need for dorsal hardware. This technique avoids breaching the nailbed and potential nail deformity.
-
Repair of Bony Avulsion (Type III, IV, V):
- Fragment Reduction: The bony fragment, often still attached to the FDP tendon, is carefully reduced to its anatomical position on the distal phalanx.
-
Fixation:
- Small Screws/Plates: For larger, stable fragments, small screws (e.g., 1.0-1.5 mm cortical screws) or a mini-fragment plate can be used for rigid internal fixation.
- K-wires: For smaller fragments or when screw fixation is not feasible, one or two fine K-wires (e.g., 0.028" or 0.035") can be drilled percutaneously across the fragment and into the distal phalanx to provide stable fixation. The K-wires can exit either dorsally or through the fingertip.
- Transosseous Sutures: If the fragment is very small or comminuted, transosseous sutures similar to the pull-out technique can be passed through the fragment and then through the distal phalanx, tied dorsally.
Ancillary Procedures
- Pulley Repair/Reconstruction: If a significant portion of the A2 or A4 pulley was necessarily released or damaged during exposure, consider reconstruction using a portion of the FDS tendon or a free tendon graft (e.g., palmaris longus) to prevent FDP bowstringing, which would compromise grip strength and mechanical efficiency.
- Vincula Repair: Rarely feasible or necessary, as the goal is primary tendon-to-bone reattachment.
Final Assessment and Closure
- Tension Assessment: Gently flex and extend the digit to ensure that the repair is stable, there is no gapping at the repair site, and the tendon tension is appropriate. The finger should assume a cascade of increasing flexion from radial to ulnar side.
- Wound Irrigation: Thoroughly irrigate the wound with sterile saline.
- Layered Closure: Close the subcutaneous tissue and skin carefully using fine sutures.
- Dressing and Splinting: Apply a sterile dressing. A dorsal blocking splint is then applied, holding the wrist in 30-40 degrees of flexion, the MCP joints in 70 degrees of flexion, and the PIP and DIP joints in 30-45 degrees of flexion. This position protects the repair by minimizing tension on the FDP. The dorsal splint should prevent extension of the DIP joint beyond the desired angle.

Complications & Management
Despite meticulous surgical technique and dedicated rehabilitation, complications can arise following FDP avulsion repair. Proactive identification and appropriate management are crucial for salvage and optimizing long-term outcomes.
| Complication | Incidence | Management / Salvage Strategy
Clinical & Radiographic Imaging