Comprehensive Guide to Dupuytren's Contracture: Etiology, Surgical Anatomy & Indications
Key Takeaway
Dupuytren's contracture is a progressive fibroproliferative disorder causing fixed flexion deformities in the hand, primarily affecting MCP and PIP joints. Etiology is multifactorial, including genetics and age. Surgical intervention is indicated based on functional impairment, degree of contracture, and progression, aiming to restore hand function.
Introduction & Epidemiology
Dupuytren's contracture is a progressive fibroproliferative disorder affecting the palmar and digital fascia of the hand, leading to nodule formation and subsequent cord contracture, most commonly of the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints. While traditionally described as a "Viking disease" due to its higher prevalence in individuals of Northern European descent, its etiology is multifactorial, with a strong genetic predisposition inherited in an autosomal dominant pattern with variable penetrance.
Epidemiologically, Dupuytren's contracture predominantly affects males, with incidence increasing significantly with age, typically manifesting after the fourth decade of life. Global prevalence varies widely, from less than 1% in some populations to over 20% in individuals over 60 in Nordic countries. Associated risk factors include epilepsy (particularly with phenobarbital use), diabetes mellitus, smoking, excessive alcohol consumption, and HIV infection. While often linked anecdotally to repetitive manual labor, a clear causal relationship with occupational trauma remains debated in the literature, with most studies suggesting a weak or no direct association.
The pathophysiology involves the transformation of fibroblasts into myofibroblasts within the palmar fascia. These myofibroblasts produce excessive amounts of type III collagen, leading to the formation of characteristic nodules and cords. Over time, these cords contract, causing fixed flexion deformities that functionally impair hand use. The disease typically progresses through several stages: the proliferative phase (characterized by cellular nodules), the involutional phase (increased myofibroblasts and collagen), and the residual phase (dense, acellular collagenous cords). The predictable progression and anatomical distortion form the basis for surgical intervention.
Surgical Anatomy & Biomechanics
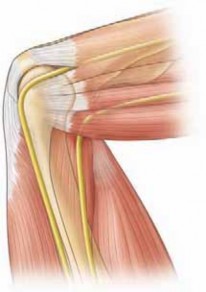
A thorough understanding of the intricate anatomy of the palmar aponeurosis and its digital extensions is paramount for safe and effective surgical management of Dupuytren's contracture. The disease primarily affects the longitudinal and transverse fibers of the palmar aponeurosis, as well as its extensions into the digits.
Normally, the palmar aponeurosis is a triangular fibrous structure in the central palm, distally dividing into pretendinous bands that extend into each digit. These bands insert into the dermis and the fibrous flexor sheath at the level of the MCP joint. Transverse fibers, known as natatory ligaments, connect the pretendinous bands at the web spaces. Cleland's and Grayson's ligaments are important obliquely oriented fibers within the digits, passing dorsal and volar to the neurovascular bundles, respectively, inserting into the skin and flexor sheath.
In Dupuytren's disease, pathological cords form from the contraction and thickening of these normal fascial structures. The nomenclature of these cords is critical for identifying their location, their effect on specific joints, and their relationship to vital neurovascular structures:
- Pretendinous cords: Form from the pretendinous bands, originating in the palm and inserting into the base of the proximal phalanx. These primarily cause MCP joint flexion contracture . They lie superficial to the flexor tendons and neurovascular bundles in the palm.
-
Spiral cords:
These are the most common cause of
PIP joint flexion contracture
and represent the most challenging anatomical distortion. A spiral cord forms from the contraction of a pretendinous band, the spiral band, the lateral digital sheath, and Grayson's ligament. As it contracts, it pulls the neurovascular bundle volarly and centrally/medially (relative to the affected finger), making it highly susceptible to injury during dissection. The relationship depends on the digit:
- Index and Middle Finger: The neurovascular bundle is typically displaced radially and superficially.
- Ring and Little Finger: The neurovascular bundle is typically displaced ulnarly and superficially.
- Natatory cords: Form from the natatory ligaments in the web spaces. These cords restrict finger abduction and cause web space contracture , often pulling the fingers together.
- Central cords: These cords arise directly from the palmar aponeurosis and extend distally along the central aspect of the digit, inserting into the middle phalanx. They directly cause PIP joint contracture and lie superficial to the flexor tendons but deep to the neurovascular bundles at the PIP level.
- Retrovascular cords: These are less common and originate from the palmar fascia, passing dorsal to the neurovascular bundles to insert onto the distal phalanx. They cause DIP joint contracture .
- Commisural cords: Found in the thumb web space, causing adduction contracture of the thumb.
Biomechanically, the contracted cords exert a constant flexion force on the affected joints. The MCP joint, being a biaxial condyloid joint, allows more complete correction than the PIP joint, which is a uniaxial hinge joint. The fibrous plate and collateral ligaments of the PIP joint can undergo adaptive shortening and stiffening in chronic contractures, making full extension more difficult to achieve and maintain, even after complete cord release. The complex interplay of skin contracture, joint capsular changes, and fascial pathology contributes to the challenge of achieving lasting correction.
Indications & Contraindications
The decision for surgical intervention in Dupuytren's contracture is based on a careful assessment of the patient's functional impairment, the degree of contracture, the rate of progression, and overall patient health. The primary goal of surgery is to restore functional range of motion and improve the patient's ability to perform activities of daily living.
Operative Indications
The generally accepted indications for surgical intervention in Dupuytren's contracture are:
- Positive "Tabletop Test": The inability to flatten the palm and affected digit(s) completely against a flat surface. This indicates a contracture severe enough to interfere with common hand functions.
- MCP Joint Contracture: Typically, an MCP joint flexion contracture of 30 degrees or greater . Contractures of this magnitude often lead to functional limitations in grasping large objects, donning gloves, or performing hygiene tasks.
- PIP Joint Contracture: Any degree of PIP joint flexion contracture is often considered significant, as these are more difficult to correct and have a greater impact on fine motor skills. A common threshold is 15-20 degrees or greater , or any contracture causing functional deficit.
- DIP Joint Contracture: While less common, functionally limiting DIP joint contracture (e.g., interfering with tip pinch or object manipulation) can also be an indication.
- Rapid Progression: Documented rapid progression of contracture, even if the absolute degree of contracture is below the conventional thresholds, may warrant earlier intervention to prevent severe fixed deformities.
- Functional Impairment: Any degree of contracture that significantly interferes with the patient's daily activities, occupational tasks, or hobbies, even if it does not meet strict goniometric thresholds. This is a patient-specific indication.
- Pain: While Dupuytren's contracture is typically painless, localized pain associated with nodules or tight cords that is refractory to conservative management may occasionally be an indication for excision.
- Web Space Contracture: Contracture of the thumb or digital web spaces (due to natatory or commissural cords) leading to restricted abduction or impaired object manipulation.
Non-Operative Indications / Relative Contraindications
Certain situations may favor observation, non-operative treatments, or contraindicate surgery:
- Nodules without Contracture: The presence of palpable nodules without any measurable joint contracture is typically managed by observation, as not all nodules progress to contracture.
- Mild Contracture without Functional Deficit: If the contracture is minimal (e.g., MCP < 30 degrees, PIP < 15 degrees) and the patient experiences no functional limitations or pain, observation is usually appropriate.
- Patient Preference: A well-informed patient's preference to defer surgery, especially if symptoms are mild.
- Significant Medical Comorbidities: Severe cardiovascular disease, uncontrolled diabetes, active infection, or other conditions that significantly increase surgical and anesthetic risks.
- Poor Skin Quality or Vascular Compromise: Compromised local skin integrity, active skin infections, or significant peripheral vascular disease that may impair wound healing or compromise digital viability post-surgery.
- Recurrence in Previously Operated Fields: In cases of recurrence after extensive surgery, particularly dermofasciectomy, alternative less invasive treatments (e.g., needle aponeurotomy, collagenase injection) or revision surgery with skin grafting may be considered based on the extent of recurrence and tissue quality.
- Early Disease Stage: For disease that has not yet progressed to significant contracture or functional impairment, non-surgical options like collagenase clostridium histolyticum injection or percutaneous needle aponeurotomy may be considered. These are generally less invasive but associated with higher recurrence rates compared to fasciectomy.
Table: Operative vs. Non-Operative Indications
| Feature | Operative Indication | Non-Operative Indication / Relative Contraindication |
|---|---|---|
| Tabletop Test | Positive (inability to flatten hand) | Negative (able to flatten hand) |
| MCP Joint Contracture | ≥ 30 degrees flexion | < 30 degrees flexion |
| PIP Joint Contracture | ≥ 15-20 degrees flexion, or any functional impairment | < 15 degrees flexion and no functional impairment |
| DIP Joint Contracture | Functionally limiting | Present, but not functionally limiting |
| Progression | Documented rapid progression | Slow or no progression |
| Functional Impact | Significant interference with ADLs, work, hobbies | No significant functional limitation |
| Pain | Localized pain, refractory to conservative management | Asymptomatic or mild, manageable pain |
| Web Space Involvement | Contracture causing functional impairment | No significant web space contracture |
| Nodules | Associated with contracture | Isolated nodules without contracture |
| Patient Comorbidities | Medically fit for surgery | Severe comorbidities (cardiac, pulmonary, uncontrolled diabetes) |
| Local Tissue Status | Healthy, viable skin and neurovascular status | Active infection, poor skin quality, vascular compromise, previous extensive scarring |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for optimizing outcomes and minimizing complications in Dupuytren's surgery. This involves comprehensive patient assessment, careful surgical site marking, and appropriate anesthesia and positioning.
Pre-Operative Assessment
-
Detailed History:
- Disease Progression: Onset, duration, rate of progression, number of affected digits/hands, prior treatments (including injections, needle aponeurotomy, or previous surgeries for Dupuytren's).
- Functional Impact: Specific difficulties with activities of daily living (e.g., washing face, putting on gloves, grasping objects), occupation, and hobbies.
- Medical Comorbidities: Focus on conditions like diabetes mellitus (impaired wound healing, neuropathy), epilepsy, peripheral vascular disease, smoking status (vasoconstriction, impaired healing), and any cardiac or pulmonary issues that might affect anesthesia or recovery.
- Social History: Hand dominance, occupation, support system for post-operative rehabilitation.
-
Physical Examination:
- Inspection: Identify all visible nodules and cords. Assess skin quality, presence of skin puckering, and digital ischemia. Check for extra-digital manifestations (Garrod's pads on knuckles, plantar fibromatosis, Peyronie's disease).
- Palpation: Map out all palpable cords. Assess their depth and relationship to underlying structures.
- Range of Motion Assessment: Systematically measure MCP, PIP, and DIP joint flexion contractures using a goniometer. Document passive and active range of motion. The "tabletop test" should be performed and documented.
- Neurovascular Status: Assess digital sensation (two-point discrimination) and capillary refill to establish a baseline and identify any pre-existing compromise.
- Skin Tension: Estimate the amount of skin deficit that will be created by contracture release, guiding the decision for skin grafting.
-
Ancillary Investigations:
- Routine pre-operative blood tests as per anesthetic guidelines.
- Imaging (e.g., X-rays, MRI) is generally not required for typical Dupuytren's contracture but may be considered for atypical presentations, unclear masses, or to rule out concomitant joint pathology.
Informed Consent
Thorough discussion of the surgical procedure, anticipated outcomes, potential complications (e.g., nerve/vessel injury, infection, hematoma, skin necrosis, recurrence, persistent stiffness, CRPS), and the necessity of post-operative hand therapy is paramount. Manage patient expectations regarding full correction, especially for severe or long-standing PIP contractures.
Anesthesia
Regional anesthesia (e.g., axillary, supraclavicular, or infraclavicular block) is often preferred, particularly for longer procedures. It provides excellent intraoperative anesthesia, prolonged post-operative analgesia, and avoids the need for general anesthesia. It also permits the use of a tourniquet without systemic vasoconstrictive effects that might be seen with epinephrine-containing local anesthetics in some cases. General anesthesia is also an option, especially for complex or prolonged cases, or when regional block is contraindicated or unsuccessful.
Tourniquet Application
A pneumatic tourniquet applied to the upper arm is essential for maintaining a bloodless surgical field, which significantly improves visualization of delicate structures and facilitates precise dissection. The tourniquet should be inflated to an appropriate pressure (e.g., 250-300 mmHg or 100 mmHg above systolic blood pressure) after exsanguination of the limb using an Esmarch bandage. Tourniquet time should be carefully monitored, typically aiming for less than 90-120 minutes.
Patient Positioning
The patient is positioned supine on the operating table. The affected arm is abducted and supported on a specialized hand table, ensuring comfort and stability. The hand and forearm are prepared and draped in a sterile fashion, typically extending above the elbow to allow for tourniquet management.
Skin Marking
Crucial pre-incision marking is performed while the hand is in its contracted state:
1.
Palpable Cords:
Trace the outline of all identifiable Dupuytren's cords.
2.
Skin Creases:
Mark the natural flexion creases in the palm and digits.
3.
Neurovascular Bundles:
Based on anatomical knowledge and careful palpation (if possible), approximate the expected course of the digital neurovascular bundles, noting their distortion by spiral cords.
4.
Incisions:
Plan the incisions, typically using Bruner zig-zag incisions along the digits and curved transverse incisions in the palm. The apices of the zig-zags should lie over the flexion creases, and the skin flaps should be of generous width to ensure viability. For severe contractures, a transverse McCash incision in the palm may be considered, leaving the wound open to heal by secondary intention, thereby minimizing skin tension and hematoma risk.
Detailed Surgical Approach / Technique
The surgical approach to Dupuytren's contracture depends on the extent and location of the disease, prior treatments, and surgeon preference. The gold standard remains fasciectomy, with variations including regional fasciectomy, segmental fasciectomy, and dermofasciectomy.
General Principles of Fasciectomy
- Magnification: Use of surgical loupes (2.5x to 4.5x magnification) is highly recommended for enhanced visualization of neurovascular bundles and fine fascial structures.
- Tourniquet: Maintain a bloodless field with the pneumatic tourniquet.
-
Incision:
- Bruner Zig-zag Incisions: The most common digital incision. Apex of the zig-zag is typically placed over the joint crease. This allows for excellent exposure and, upon closure, lengthens the skin envelope, preventing linear scar contracture.
- Transverse Incisions: In the palm, a curved transverse incision (e.g., at the distal palmar crease) or multiple short transverse incisions can be used.
- McCash Palmar Fasciotomy: A single transverse incision across the palm, leaving the wound open to heal by secondary intention. Indicated for severe contractures or high-risk patients to minimize skin tension and hematoma, but requires prolonged wound care.
- Z-plasty: Can be incorporated into longitudinal incisions or used to release severe local skin contracture.
- Skin Flap Elevation: Carefully elevate full-thickness skin flaps (containing subcutaneous fat) to expose the underlying diseased fascia. Handle skin edges gently to preserve their vascularity.
-
Identification and Protection of Neurovascular Bundles:
This is the most critical step. Digital neurovascular bundles lie immediately beneath the subcutaneous fat.
- Always begin dissection on the side of the digit where the neurovascular bundle is least likely to be involved or displaced by the cord. For the index and middle fingers, this is usually the ulnar side; for the ring and little fingers, the radial side.
- Trace the neurovascular bundles proximally and distally into healthy tissue before approaching the area of dense scarring and cord involvement.
- Remember that spiral cords displace the neurovascular bundle superficially and medially (ulnar side of ring/little finger, radial side of index/middle finger).
- Use fine-tipped forceps and sharp dissection with a #15 blade or tenotomy scissors. A nerve stimulator can be used to confirm nerve integrity, especially in revision cases.
-
Excision of Diseased Fascia (Fasciectomy):
- Systematically identify and excise the offending cords. Start proximally and work distally.
- Pretendinous cords: Excised in the palm to release MCP contracture.
- Spiral cords: Carefully dissect around the displaced neurovascular bundle, excising the contracted components (pretendinous band, spiral band, lateral digital sheath, Grayson's ligament) that form the spiral cord.
- Natatory cords: Excised from the web spaces to improve abduction.
- Central cords: Excised along the length of the digit to release PIP contracture.
- Retrovascular cords: Excised to address DIP contractures.
- The goal is to excise only diseased tissue, leaving healthy fascia, tendons, nerves, and vessels intact. Avoid aggressive stripping of subcutaneous fat unnecessarily.
- Contracture Release Assessment: After excising the cords, gently extend the affected joint(s). Assess the completeness of the release. Any remaining restriction often indicates an overlooked cord, joint capsule contracture, or collateral ligament shortening. For PIP joints, accessory collateral ligament release or volar plate release may be necessary in very chronic, severe contractures, but this adds to stiffness risk.
- Hemostasis: Prior to tourniquet release, ensure meticulous hemostasis using bipolar cautery. This minimizes post-operative hematoma formation, which can compromise skin flaps and contribute to stiffness.
-
Skin Closure:
- Primary Closure: If skin tension is minimal, direct closure of the zig-zag flaps is preferred.
- Z-plasty/local flaps: If skin length is deficient after contracture release, local Z-plasty can be performed to lengthen the incision.
- Full-Thickness Skin Graft (FTSG): For significant skin deficit, particularly in recurrent disease or dermofasciectomy. Common donor sites include the ipsilateral forearm, medial arm, or groin. The FTSG is meshed or fenestrated and secured with sutures. A bolster dressing is applied for immobilization and even pressure.
- Open Wound Management (McCash): For palmar wounds, leaving the wound open for secondary intention healing.
- K-wire Fixation: For severe PIP joint contractures (especially > 60-70 degrees) that are difficult to hold in extension post-operatively, a temporary K-wire (e.g., 0.035" or 0.045") can be inserted across the PIP joint to maintain extension for 2-3 weeks. This helps prevent early re-contracture but may increase stiffness risk.
- Dressing: Apply a bulky, soft compressive dressing with the digits placed in extension (or as much extension as safely tolerated without excessive skin tension). A volar splint may be incorporated.
Dermofasciectomy
This technique involves excising not only the diseased fascia but also the overlying skin. It is indicated for:
* Recurrent Dupuytren's disease with extensive skin involvement.
* Aggressive disease with rapid progression.
* Cases where the skin is tightly adherent to the underlying cords or compromised.
The resulting skin defect necessitates skin grafting, usually with a full-thickness graft. This technique has a lower recurrence rate compared to standard fasciectomy but is more invasive and requires longer healing time.
Fasciotomy (Open or Percutaneous)
Fasciotomy involves simple division of the contracted cords without excision.
*
Percutaneous Needle Aponeurotomy (PNA):
Cords are divided using a small-gauge needle under local anesthesia. Less invasive, quicker recovery, but higher recurrence rates. Suitable for isolated cords, particularly MCP contractures, in elderly or less active patients.
*
Open Fasciotomy:
Surgical division of cords through small incisions. Also less invasive than fasciectomy but carries higher recurrence risk.
These are often considered for less severe cases, elderly or frail patients, or as a temporizing measure.
Complications & Management
Surgical treatment of Dupuytren's contracture, while generally safe and effective, is associated with a range of potential complications. A thorough understanding of these complications, their incidence, and appropriate management strategies is essential.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Management / Salvage Strategy |
|---|---|---|
| Neuropraxia/Nerve Injury | 5-20% (transient); <1% (permanent) | Prevention: Meticulous dissection under magnification, identification/protection of neurovascular bundles. Management: Observation for neuropraxia (often resolves in weeks/months). If suspected transection, immediate micro-surgical repair. If late presentation with painful neuroma, excision/burial or grafting. |
| Digital Artery Injury/Thrombosis | <1% | Prevention: Careful dissection. Management: Immediate micro-surgical repair (if vessel large enough). If thrombosis, anticoagulation, exploration. If irreversible, consideration of revascularization or observation (risk of digital necrosis). |
| Hematoma | 5-10% | Prevention: Meticulous hemostasis, compression dressing. Management: Elevation, compression. If expanding or significantly painful, surgical evacuation, re-exploration for bleeding control. |
| Infection | 1-5% | Prevention: Strict aseptic technique, prophylactic antibiotics (per institutional guidelines). Management: Oral or IV antibiotics based on culture results. Wound care, debridement if abscess or necrotizing infection. |
| Skin Necrosis/Wound Healing Issues | 5-15% | Prevention: Careful skin flap elevation, avoid excessive tension during closure, appropriate incision design, meticulous hemostasis. Management: Local wound care, débridement of necrotic tissue, secondary intention healing, skin grafting (full-thickness, split-thickness) if defect too large for secondary closure. |
| Recurrence | 20-50% (by 5-10 years) | Prevention: Complete excision of diseased tissue (fasciectomy/dermofasciectomy). Management: Observation for mild cases. Non-operative (collagenase, needle aponeurotomy) for isolated cords. Revision surgery (often dermofasciectomy with skin grafting) for significant, symptomatic recurrence. |
| Persistent Contracture/Incomplete Correction | Varies (higher for severe PIP) | Prevention: Thorough cord release, assessment intraoperatively. Management: Intensive hand therapy, static/dynamic splinting. If persistent functional deficit, consideration of revision surgery (fasciotomy, further fasciectomy, volar plate release, arthrodesis for severe PIP joint arthritis). |
| Stiffness/Reduced Range of Motion | Common | Prevention: Early mobilization, aggressive hand therapy. Management: Intensive hand therapy, static progressive or dynamic splinting, scar massage. Joint mobilization, sometimes requiring release of joint capsule (secondary procedure). |
| Complex Regional Pain Syndrome (CRPS) | 1-5% | Prevention: Gentle tissue handling, good pain control, early mobilization. Management: Early recognition, aggressive pain management (NSAIDs, neuropathic agents, sympathetic blocks), physical therapy, occupational therapy, psychological support. |
| Pain | Common (post-op) | Prevention: Good surgical technique, gentle tissue handling. Management: Multimodal analgesia (acetaminophen, NSAIDs, opioids as needed), nerve blocks, ice. |
| Scar Issues (Hypertrophic/Keloid) | Varies | Prevention: Careful incision planning, tension-free closure. Management: Scar massage, silicone gel sheets, steroid injections, laser therapy, surgical revision (rare). |
General Management Principles
- Early Recognition: Prompt identification of complications is key to effective management. Educate patients on warning signs.
- Proactive Prevention: Many complications can be mitigated by meticulous surgical technique, appropriate patient selection, and comprehensive pre-operative planning.
- Multidisciplinary Approach: Management often requires collaboration with hand therapists, pain specialists, and other medical professionals.
- Patient Education: Clearly communicate risks and potential complications pre-operatively and provide clear post-operative instructions for monitoring and self-care.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an indispensable component of successful Dupuytren's contracture management. Its primary objectives are to optimize range of motion, prevent recurrence of contracture, minimize stiffness and edema, and restore functional hand use. Rehabilitation protocols are typically initiated within the first few days post-surgery, emphasizing early, controlled motion.
Phase 1: Immediate Post-Operative (Day 0 - Day 7)
- Dressing: A bulky, protective soft dressing is applied immediately post-surgery. The dressing should immobilize the digits in extension (or near-full extension, avoiding excessive tension on the wound). A volar splint may be incorporated to maintain extension at the MCP and PIP joints. For skin grafts, a bolster dressing is applied to provide continuous, even pressure.
- Elevation: Emphasize strict hand elevation above heart level at all times (especially the first 48-72 hours) to minimize edema formation.
- Wound Care: Monitor the dressing for signs of bleeding or infection. The initial dressing change typically occurs between post-operative days 2-5, with careful inspection of incisions and any skin grafts. Staples or sutures are usually left in place during this phase.
-
Early Active Range of Motion (AROM):
- Uninvolved Joints: Encourage immediate active range of motion of the wrist, elbow, and shoulder to prevent stiffness.
- Involved Digits: Under the guidance of a hand therapist, begin gentle, protected AROM exercises for the operated digits, typically starting within 1-3 days post-surgery, depending on wound stability and surgical technique. This usually involves active flexion and extension, within the limits of pain and wound tension, to prevent adhesions and promote glide.
- Edema Control: Continued elevation, light compression (after initial dressing removal), and gentle retrograde massage.
Phase 2: Early Mobilization & Splinting (Weeks 1-3)
- Hand Therapy Commencement: Intensive hand therapy sessions (2-3 times per week) begin.
-
Splinting:
- Night Splinting: A custom-fabricated, static extension splint (e.g., a volar thermoplastic splint) is provided and worn at night to maintain maximum extension of the MCP and PIP joints. This is crucial to counteract the tendency for re-contracture.
- Daytime Splinting: Dynamic or static progressive splints may be introduced during the day, particularly for PIP joint contractures, to gradually increase extension while allowing for functional activity. Alternatively, patients may wear the static extension splint during rest periods.
-
Range of Motion Exercises:
- Active Flexion/Extension: Continue and progress AROM exercises, focusing on full active digital flexion (hook fist, full fist) and active extension to the limits of the splinted position.
- Passive Range of Motion (PROM): Gentle, controlled PROM may be introduced by the therapist, especially for resistant PIP joint contractures, ensuring not to disrupt wound healing or grafts.
- Scar Management: Once incisions are well-healed, gentle scar massage is initiated to soften the scar tissue and prevent adherence. Silicone gel sheets or scar pads may be applied.
- K-wire Removal: If K-wires were used for PIP joint fixation, they are typically removed by week 2-3, followed by immediate progression of ROM exercises.
Phase 3: Strengthening & Functional Integration (Weeks 3-6)
- Splinting: Continue night extension splinting. Daytime splinting may be gradually reduced as range of motion improves and is maintained.
-
Therapy Progression:
- Strengthening: Begin progressive strengthening exercises for grip and pinch, using therapy putty, stress balls, or light weights.
- Advanced ROM: Focus on achieving full functional range of motion, addressing any remaining deficits.
- Functional Activities: Incorporate activities of daily living and simulated occupational tasks into therapy to enhance functional recovery and dexterity.
- Scar Management: Continue vigorous scar massage and silicone applications.
- Desensitization: For areas of hyper-sensitivity (e.g., around nerve repair sites or sensitive scars), desensitization techniques may be employed.
Phase 4: Return to Activity & Long-Term Management (Weeks 6-12+)
- Weaning from Splinting: Gradual discontinuation of daytime splinting, with continued night splinting for several months (typically 3-6 months, sometimes longer for severe PIP contractures or high-risk for recurrence).
- Full Activity Resumption: Gradual return to full work, sports, and recreational activities, guided by functional assessment and patient tolerance.
- Home Exercise Program: Patients are provided with a comprehensive home exercise program to maintain gains and prevent recurrence.
- Monitoring for Recurrence: Patients are educated on the signs of recurrence and the importance of long-term follow-up with the surgeon and therapist.
Throughout all phases, close communication between the surgeon and hand therapist is paramount to tailor the protocol to individual patient needs, surgical findings, and progress. Vigilance for complications such as CRPS or persistent stiffness guides modifications to the rehabilitation plan.
Summary of Key Literature / Guidelines
The literature on Dupuytren's contracture spans over a century, providing a rich history of understanding and managing this enigmatic disease. Key insights and guidelines have emerged from numerous studies, shaping current surgical practice.
Historical Context & Foundation
- Guillaume Dupuytren (1831): First described the disease and performed open fasciotomy, recognizing the fibrous contracture.
- Skoog (1948): Pioneered regional fasciectomy, emphasizing excision of diseased fascia, which became the gold standard. His work detailed the anatomical distribution of the disease and its surgical implications.
- McCash (1964): Introduced the concept of leaving palmar wounds open to heal by secondary intention, particularly for severe contractures, to minimize hematoma and skin tension, thus reducing complications.
Modern Surgical Guidelines & Evidence
- Indications for Surgery: The "tabletop test" and specific goniometric thresholds (e.g., MCP > 30 degrees, any PIP contracture > 15-20 degrees) remain widely accepted indications for surgical intervention (American Society for Surgery of the Hand - ASSH, British Society for Surgery of the Hand - BSSH). These are primarily based on consensus and expert opinion, backed by clinical experience demonstrating functional improvement with correction.
-
Surgical Techniques:
- Regional Fasciectomy: Remains the most commonly performed and widely recommended surgical procedure for established Dupuytren's contracture. High-level evidence (Level I and II studies) supports its efficacy in achieving contracture correction and long-term functional improvement.
- Dermofasciectomy: Reserved for recurrent disease, aggressive forms, or cases with significant skin involvement. Literature suggests lower recurrence rates (e.g., 8-15% vs. 20-50% for fasciectomy at 5-10 years) but at the cost of increased invasiveness and graft-related complications.
- Percutaneous Needle Aponeurotomy (PNA) and Collagenase Clostridium Histolyticum (CCH): These less invasive techniques have gained prominence, particularly for isolated, palpable cords and less severe contractures. Multiple randomized controlled trials (RCTs) have demonstrated their effectiveness in correcting contractures, especially at the MCP joint, with shorter recovery times compared to fasciectomy. However, they are associated with higher recurrence rates (e.g., 5-year recurrence rates up to 50% for PNA, 30-40% for CCH) compared to fasciectomy, and CCH specifically has a higher rate of skin tears and local reactions. They are generally considered for patients who prefer a less invasive approach, are elderly, or have comorbidities precluding formal surgery.
- Anatomical Considerations: Contemporary literature consistently emphasizes the critical importance of meticulous dissection and neurovascular bundle identification, particularly in the presence of spiral cords. Studies by Hueston and subsequent anatomical dissections highlight the variable and often superficial displacement of neurovascular bundles by these cords.
- Complication Rates: Modern series report overall complication rates for fasciectomy ranging from 15-30%, with nerve injury (transient neuropraxia) being the most common, followed by hematoma, infection, and skin healing issues. CRPS, while uncommon, is a severe complication requiring vigilance.
- Recurrence and Progression: Dupuytren's disease is a genetic condition, and recurrence is an inherent characteristic, not a failure of surgery. Recurrence rates after fasciectomy are influenced by genetic predisposition, severity of initial disease, number of digits involved, family history, and the presence of extra-digital manifestations (e.g., Garrod's pads, plantar fibromatosis). Long-term follow-up studies confirm that recurrence continues over decades.
- Rehabilitation: Evidence strongly supports early and intensive hand therapy, including splinting, to optimize post-operative range of motion and functional outcomes. Protocols vary but generally follow the phases outlined previously, with consensus on the importance of extension splinting, especially at night.
In summary, surgical management of Dupuytren's contracture, primarily through regional fasciectomy, remains the gold standard for functionally significant contractures. Newer, less invasive options like PNA and CCH offer alternatives for select patients, but surgeons must weigh the benefits of quicker recovery against higher recurrence rates. A comprehensive understanding of the disease's anatomy, careful patient selection, meticulous surgical technique, and dedicated post-operative rehabilitation are cornerstones of successful treatment. Continuous long-term monitoring is essential due to the chronic and recurrent nature of the disease.
You Might Also Like