Clinical Case Study: Diagnosing Right Ring Finger Stenosing Tenosynovitis
Key Takeaway
Trigger finger is primarily diagnosed through clinical examination, identifying focal tenderness at the A1 pulley, a palpable nodule, and characteristic catching during active finger extension. Imaging like X-rays typically appears normal, serving to rule out other bony pathologies. Patient history of pain and locking also guides diagnosis.
Patient Presentation & History
A 58-year-old right-hand dominant female, Mrs. Eleanor Vance, presented to the hand clinic complaining of progressive pain and intermittent catching in her right ring finger. Her chief complaint was a "clicking and locking sensation" that had been worsening over the past six months, particularly in the mornings or after prolonged gripping activities. She described the sensation as her finger getting "stuck" in a bent position, requiring her other hand to passively extend it, often accompanied by a painful "snap."
The onset of symptoms was insidious, approximately 8 months prior to presentation, starting as mild discomfort at the base of her right ring finger. Over time, the pain intensified, and the catching became more frequent and severe, progressing to a point where the finger would occasionally lock completely, necessitating manual manipulation. She denied any acute traumatic event.
Regarding past medical history, Mrs. Vance has a well-controlled Type 2 Diabetes Mellitus, diagnosed 10 years prior, currently managed with Metformin with an HbA1c of 6.8%. She also has a history of mild osteoarthritis in her knees, managed conservatively, and uses her hands extensively in her occupation as a seamstress. She denied any history of inflammatory arthropathies like rheumatoid arthritis or psoriasis, and no history of thyroid disease. She had previously tried over-the-counter NSAIDs with minimal relief. Two months prior, her primary care physician administered a corticosteroid injection (Dexamethasone 4mg mixed with 1mL 1% Lidocaine) into the flexor tendon sheath of the affected finger, which provided partial relief for approximately four weeks before symptoms gradually recurred to their previous severity. She reported no known allergies. Her social history was non-contributory, apart from her occupation requiring repetitive fine motor tasks. She is a non-smoker and consumes alcohol occasionally.
Clinical Examination
Upon clinical examination, the patient was cooperative and in no acute distress.
Inspection
- Right Hand: No overt swelling, erythema, or ecchymosis was noted. The skin appeared healthy, without any signs of scarring or previous surgical intervention. No gross deformity of the right ring finger or other digits was immediately apparent. There was no visible fixed flexion deformity at rest.
- Left Hand: Unremarkable.
Palpation
-
Right Hand:
- Direct palpation over the volar aspect of the A1 pulley of the right ring finger elicited focal tenderness.
- A discrete, firm, and painful nodule was palpable within the flexor tendon sheath at the level of the metacarpophalangeal (MCP) joint of the right ring finger. This nodule was noted to move proximally and distally with active finger flexion and extension, respectively.
- No palpable warmth or crepitus around the MCP joint.
- No palpable masses in the palm consistent with Dupuytren's nodules.
- Assessment for concomitant carpal tunnel syndrome was performed: Tinel's sign at the wrist was negative, and Phalen's test was negative.
Range of Motion (ROM)
-
Active Range of Motion (AROM):
- Right Ring Finger: Full active flexion was possible, but during active extension from a fully flexed position, a distinct "catching" or "triggering" sensation was observed and palpated at the A1 pulley level. The finger would briefly halt in a partially flexed position before snapping into full extension, often with associated pain. This was consistent with a Grade III triggering (Green's Classification), requiring conscious effort and often passive assistance to overcome the lock.
- Other digits and wrist ROM were full and pain-free.
-
Passive Range of Motion (PROM):
- Right Ring Finger: Full passive flexion and extension were achievable without mechanical restriction, though passive extension through the "sticking point" still elicited a similar palpable click and some residual discomfort. This confirmed the absence of a fixed capsular contracture or significant arthritic changes limiting joint movement.
- Strength: Grip strength and pinch strength were assessed and found to be symmetrical and within normal limits, though forceful gripping of the right hand exacerbated the pain and triggering in the ring finger.
Neurological/Vascular assessment
-
Neurological:
- Sensation to light touch and two-point discrimination (2PD) was intact in all digital nerve distributions of the right hand. 2PD was 5mm in the right ring finger.
- Motor function for median, ulnar, and radial nerve innervated muscles was intact (Medical Research Council Grade 5/5) with no signs of atrophy or weakness.
- Specifically, intrinsic muscle function (interossei, lumbricals) and extrinsic muscle function were normal.
-
Vascular:
- Capillary refill was brisk (<2 seconds) in all digits.
- Radial and ulnar pulses were strong and palpable at the wrist.
- Digital pulses were palpable in the right ring finger.
- No pallor or cyanosis was noted.
In summary, the clinical examination strongly supported a diagnosis of stenosing tenosynovitis of the right ring finger.
Imaging & Diagnostics
X-ray Findings
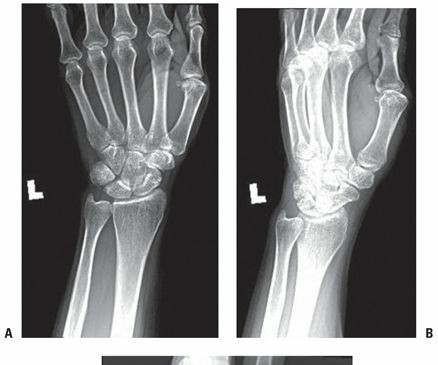
Plain radiographs of the right hand (AP, oblique, and lateral views) were obtained to rule out any underlying bony pathology or joint abnormalities that could mimic or contribute to the symptoms.
*
Findings:
The radiographs demonstrated normal osseous architecture and joint spaces throughout the carpus, metacarpals, and phalanges. No evidence of fracture, dislocation, osteophytes, joint space narrowing, or other degenerative changes were observed in the MCP, PIP, or DIP joints of the affected digit or adjacent digits. There were no visible soft tissue calcifications or foreign bodies.
*
Interpretation:
The normal radiographic findings are typical for primary stenosing tenosynovitis, which is primarily a soft tissue pathology. This effectively ruled out significant arthritis, fracture, or other overt bony abnormalities as the primary cause of the patient's symptoms.
Ultrasound (US)
Given the typical presentation and the absence of bony pathology on X-ray, an ultrasound examination of the right ring finger's flexor tendon sheath was performed. This was chosen over MRI due to its dynamic capabilities, lower cost, and ability to directly visualize the pathophysiology in real-time.
*
Technique:
A high-frequency linear array transducer (10-18 MHz) was used. The examination was performed with the patient's hand resting on a flat surface. Both static and dynamic images were acquired.
*
Findings:
*
A1 Pulley:
Significant thickening of the A1 pulley of the right ring finger was clearly visualized. The anteroposterior diameter of the A1 pulley was measured at 2.1 mm (normal range typically < 1.0-1.2 mm).
*
Flexor Tendon:
The flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP) tendons demonstrated fusiform thickening and hypoechoic changes within their substance just proximal to the A1 pulley, forming a distinct nodule. The cross-sectional area of the combined tendons was increased compared to the unaffected adjacent digits.
*
Tenosynovial Fluid:
A small amount of hypoechoic fluid (effusion) was noted within the flexor tendon sheath proximal to the A1 pulley, indicative of active inflammation.
*
Dynamic Assessment:
During active finger flexion and extension, the thickened flexor tendon nodule was observed to visibly impinge against the constricted A1 pulley, confirming the mechanical "catching" phenomenon. The movement was restricted and then suddenly released, corresponding to the clinical triggering.
*
Doppler:
Color Doppler imaging showed mild hyperemia within the thickened A1 pulley and surrounding tenosynovium, indicating inflammatory activity.
*
Interpretation:
The ultrasound findings provided definitive objective evidence of A1 pulley thickening, flexor tendon nodule formation, tenosynovitis, and the dynamic mechanical impingement characteristic of stenosing tenosynovitis. This confirmed the clinical diagnosis and obviated the need for further advanced imaging like MRI.
CT/MRI Indications (General Considerations, not specifically for this patient)
- CT Scan: Generally not indicated for routine trigger finger cases. It may be considered in cases with suspected complex bony pathology not adequately visualized on plain X-rays, such as occult fractures, osteomyelitis, or complex intra-articular degenerative changes, or for pre-operative planning in revision cases where bony landmarks are distorted.
-
MRI Scan:
While capable of demonstrating A1 pulley thickening, flexor tendon pathology, and tenosynovitis, MRI is typically reserved for cases where:
- The diagnosis remains unclear despite clinical and ultrasound assessment.
- There is suspicion of other soft tissue pathology, such as partial flexor tendon rupture, tumor, or severe inflammatory processes (e.g., in rheumatoid arthritis with extensive synovial proliferation).
- Coexisting conditions like severe carpal tunnel syndrome requiring detailed nerve imaging.
- Failure of surgery without clear explanation, to evaluate for occult adhesions or other causes of persistent symptoms.
- In this patient's case, the combination of clinical presentation, failed conservative management, and clear ultrasound findings made MRI unnecessary.
Differential Diagnosis
The clinical presentation of hand pain with a catching sensation necessitates a thorough differential diagnosis. Several conditions can present with similar symptoms, and distinguishing them is crucial for appropriate management.
| Feature | Stenosing Tenosynovitis (Trigger Finger) | Flexor Tendon Sheath Ganglion | MCP Joint Arthritis / Loose Body | Dupuytren's Contracture (Early) |
|---|---|---|---|---|
| Pathophysiology | Disproportion between flexor tendon volume (nodule) and A1 pulley lumen. | Synovial cyst originating from joint capsule or tendon sheath. | Degenerative changes, cartilage loss, osteophyte formation. | Fibroproliferative disorder of palmar fascia. |
| Primary Complaint | Painful catching, snapping, or locking of the digit. | Palpable mass, sometimes pain or mechanical blockage. | Localized joint pain, stiffness, swelling, crepitus. | Palpable nodule in palm, discomfort, progressive contracture. |
| Location of Signs | Volar aspect of MCP joint, directly over A1 pulley. | Often volar aspect of digit, usually over A2-A4 pulley. | Localized to the MCP joint line (dorsal or volar). | Palmar fascia, most commonly ring and small fingers. |
| Palpation | Tenderness at A1 pulley, palpable nodule or thickening of tendon sheath. | Smooth, firm, often mobile, non-tender or mildly tender mass. | Joint line tenderness, effusion, crepitus, osteophytes. | Firm, fixed nodule in palmar fascia, not tendon-related. |
| Triggering/Locking | Characteristic mechanical "snap" or "catch" on active extension. | May cause mechanical block if large, but not true "triggering." | Occasional "giving way" or mechanical block due to loose body. | No true triggering; causes progressive flexion contracture. |
| Range of Motion | Full passive ROM (often painful), active ROM limited by triggering. | May have full ROM, or limited by mass effect; no true snap. | Painful and restricted AROM/PROM, especially at end-range. | Early full ROM, later progressive flexion contracture develops. |
| Imaging | X-ray normal. US shows A1 pulley thickening, tendon nodule, tenosynovitis. | X-ray normal. US/MRI shows fluid-filled cystic structure. | X-ray: joint space narrowing, osteophytes, loose bodies. | X-ray normal. US/MRI shows fascial thickening and nodules. |
| Associated Factors | Diabetes Mellitus, Rheumatoid Arthritis, Hypothyroidism, repetitive grip. | Often idiopathic, minor trauma, may coexist with trigger finger. | Age, trauma, inflammatory arthropathies, occupational stress. | Genetic predisposition, Northern European descent, DM, alcoholism. |
| Treatment | Splinting, NSAIDs, steroid injection, A1 pulley release. | Observation, aspiration, excision. | NSAIDs, injections, physiotherapy, arthroplasty, fusion. | Observation, collagenase injection, fasciotomy, dermatofasciotomy. |
Surgical Decision Making & Classification
Mrs. Vance's presentation of a Grade III triggering (Green's Classification) in her right ring finger, coupled with a failed corticosteroid injection, makes her a suitable candidate for surgical intervention.
Non-operative Failures
The decision for surgical intervention was predicated on the failure of conservative management strategies:
1.
Corticosteroid Injection:
While the initial injection provided temporary relief, the recurrence of severe symptoms within a short timeframe (4 weeks) indicated that this non-operative approach was no longer effective in providing durable symptom resolution. Repeated injections carry risks of tendon atrophy, rupture, and skin changes, particularly in diabetic patients who are already at higher risk for recurrence and infection. Current guidelines typically suggest a maximum of 2-3 injections per site.
2.
NSAIDs and Splinting:
She had previously attempted NSAIDs with minimal effect. While splinting can be beneficial for Grade I/II triggering, her Grade III symptoms and fixed flexion requiring passive extension were unlikely to resolve with splinting alone.
Indications for Surgery (Open A1 Pulley Release)
- Failure of conservative management (persistent severe symptoms despite appropriate injections and physiotherapy).
- Severe triggering/locking (Quinnell Grade III or IV) that significantly impairs function and causes pain.
- Fixed flexion deformity (Quinnell Grade IV), although Mrs. Vance did not present with a fixed deformity at rest, her finger would lock in flexion requiring passive extension.
- Concomitant conditions (e.g., diabetes) which can predispose to recurrence with non-operative treatment, making surgery a more definitive solution.
Contraindications / Considerations
- Absolute Contraindications: Active local infection, severe uncontrolled systemic infection.
-
Relative Contraindications / Considerations:
- Poorly controlled diabetes: Mrs. Vance's diabetes was well-controlled (HbA1c 6.8%), which mitigates some of the increased risks, but diabetic patients still have higher rates of recurrence and potential for wound healing issues. Meticulous surgical technique and post-operative care are paramount.
- Bleeding diathesis / Anticoagulation: Requires careful pre-operative management of anticoagulants.
- Patient preference: Some patients may prefer continued non-operative management, even if less effective.
Classification of Trigger Finger Severity (Quinnell's Classification)
Mrs. Vance's condition falls into Grade III based on Quinnell's classification system for stenosing tenosynovitis:
*
Grade I (Pre-triggering):
Pain and tenderness at the A1 pulley, but no visible catching.
*
Grade II (Catching):
Active catching observed, but the patient can fully extend the finger actively.
*
Grade III (Locking):
The finger locks in flexion, requiring passive extension by the patient or examiner. This was the predominant presentation in Mrs. Vance's case.
*
Grade IV (Fixed Flexion Contracture):
A fixed flexion deformity exists, and the finger cannot be fully extended passively.
Choice of Surgical Technique: Open vs. Percutaneous Release
-
Open A1 Pulley Release:
This technique was chosen for Mrs. Vance. It is considered the gold standard with a high success rate and low recurrence. It allows for direct visualization of the A1 pulley and protection of neurovascular structures. It is particularly preferred in:
- Recurrent cases after injection.
- Cases with palpable nodules, which require thorough release.
- Patients with comorbidities like diabetes, where precise release and neurovascular protection are critical due to potentially compromised tissue healing and nerve fragility.
- Cases involving the thumb or index finger, where digital nerves are in closer proximity.
-
Percutaneous A1 Pulley Release:
This involves using a needle or fine scalpel through a small skin puncture to divide the A1 pulley without direct visualization. While less invasive, it carries a higher risk of:
- Incomplete release.
- Injury to digital nerves (especially in the thumb and index finger, or in patients with distorted anatomy).
- Flexor tendon injury.
- Higher recurrence rates reported in some series.
- It is generally reserved for uncomplicated, primary trigger fingers in non-diabetic patients, typically affecting the middle or ring fingers, where the risk of nerve injury is perceived to be lower. It was not deemed appropriate for Mrs. Vance given her history and comorbidities.
Based on her clinical presentation (Grade III triggering), failure of conservative management, and history of diabetes, an open A1 pulley release was deemed the most appropriate and definitive surgical approach to ensure complete release, minimize recurrence, and protect vital structures.
Surgical Technique / Intervention
The procedure, an open A1 pulley release of the right ring finger, was performed under strict sterile conditions in the operating theatre.
Patient Positioning
The patient was positioned supine on the operating table. The right upper limb was placed on a dedicated hand table, abducted to 90 degrees. A pneumatic tourniquet was applied to the upper arm to maintain a bloodless field.
Anesthesia
A regional anesthetic (axillary block) was administered by the anesthesia team. This provided excellent intraoperative analgesia and post-operative pain control. In addition, 3-5 mL of 1% Lidocaine with Epinephrine (1:100,000) was infiltrated locally at the incision site for hydrodissection and vasoconstriction, further aiding haemostasis.
Surgical Approach (Open A1 Pulley Release)
- Tourniquet Inflation: The tourniquet was inflated to 250 mmHg, ensuring a bloodless field. The hand was then prepped and draped in the usual sterile fashion for hand surgery.
- Incision: A small transverse incision, approximately 1.5 cm in length, was made in the distal palmar crease, directly overlying the palpable A1 pulley of the right ring finger. This transverse orientation minimizes scar contracture and is aesthetically favorable. The incision was made just proximal to the MCP joint crease to ensure it was directly over the pulley.
-
Dissection:
- Subcutaneous fat was carefully spread using fine dissecting scissors and blunt dissection with a mosquito hemostat. Care was taken to identify and protect any superficial veins and cutaneous nerves.
- The flexor tendon sheath was then identified. Its thickened, pearly white appearance distinguishes it from the surrounding loose connective tissue.
- Crucially, the digital neurovascular bundles, which run along the radial and ulnar sides of the flexor tendon sheath, were identified and protected. The radial digital nerve to the ring finger and the ulnar digital nerve to the ring finger were carefully retracted using small vessel loops or blunt hooks. This step is paramount to prevent iatrogenic nerve injury.
- A1 Pulley Identification: The thickened A1 pulley was clearly visualized as a distinct fibrous band extending transversely across the flexor tendons, just proximal to the MCP joint. The underlying flexor tendons (FDS and FDP) were visible through the translucent sheath. The characteristic nodule on the flexor tendons could be seen and palpated proximal to the constricted pulley.
-
Pulley Release:
- Using a fine-tipped scalpel (e.g., a #15 blade or ophthalmic scalpel), the A1 pulley was incised longitudinally along its entire length, from its proximal origin to its distal insertion. The incision was made precisely in the midline of the pulley, between the neurovascular bundles.
- Care was taken to ensure complete division of all fibrous bands of the A1 pulley. The release was confirmed by passing a small, curved mosquito hemostat or a probe through the released pulley, verifying that the opening was wide enough for unrestricted tendon gliding.
- The flexor tendons were then actively manipulated by the assistant flexing and extending the digit. A smooth, unhindered glide of the tendons was observed, and the "catching" or "triggering" phenomenon was completely eliminated. The previously palpable tendon nodule now glided freely through the released pulley. The edges of the released pulley were palpated to ensure no residual constricting bands remained.
- It is critical to avoid accidental incision of the underlying A2 pulley, which is essential for maintaining the mechanical advantage and preventing bowstringing of the flexor tendons. The A1 pulley is typically released only, not the A2.
- Hemostasis: The operative field was checked for any bleeding points, and meticulous hemostasis was achieved using bipolar cautery.
-
Wound Closure:
- The subcutaneous tissue was approximated using a single absorbable suture (e.g., 4-0 Vicryl Rapide) if needed, though often this layer is left open in such small incisions.
- The skin edges were then closed using fine non-absorbable sutures (e.g., 4-0 Nylon or Prolene) in an interrupted fashion.
- Dressing: A non-adherent sterile dressing (e.g., Adaptic), followed by sterile gauze pads and a light compression dressing (e.g., Coban wrap), was applied to the digit and hand. The tourniquet was then deflated. Capillary refill in the digit was confirmed to be normal immediately after deflation.
Post-Operative Protocol & Rehabilitation
The post-operative protocol is designed to facilitate early return of function, minimize stiffness, and optimize wound healing.
Immediate Post-Operative Period (Day 0-3)
- Pain Management: Oral analgesics (e.g., paracetamol, NSAIDs, weak opioids if necessary) were prescribed. The regional block typically provides good initial pain relief.
- Dressing: The light compression dressing was kept clean and dry. Patient was instructed to avoid getting the dressing wet.
- Elevation: The hand was kept elevated above heart level (e.g., on pillows) to reduce swelling.
- Early Active Range of Motion (AROM): Crucially, the patient was encouraged to begin gentle active flexion and extension exercises of the operated ring finger immediately upon recovery from anesthesia. This is vital to prevent adhesions between the flexor tendons and the surrounding soft tissues, and to promote tendon gliding. Full flexion and extension were encouraged, ensuring no active triggering occurred.
- Avoidance: Avoid forceful gripping or heavy lifting.
Early Phase (Day 3 - Week 2)
- Wound Care: The dressing was changed by the patient or district nurse as instructed. The wound site was monitored for any signs of infection (redness, increased pain, discharge, fever).
- Suture Removal: Non-absorbable sutures were typically removed at 10-14 days post-op in the clinic.
-
Exercises:
- Tendon Gliding Exercises: Continue active flexion and extension of the affected digit through its full pain-free range. Specific tendon gliding exercises (e.g., hook fist, straight fist, full fist) were taught to promote differential gliding of the FDS and FDP tendons.
- Edema Control: Continued elevation, gentle massage of the hand and digit, and light compression (e.g., a compression glove) to manage any residual swelling.
- Scar Care: Once sutures were removed and the wound was dry, gentle massage of the incision site with moisturizing cream was initiated to prevent scar adherence and promote pliability.
Mid Phase (Week 2 - Week 6)
- Progressive Strengthening: Once the wound was fully healed, the patient gradually progressed to light strengthening exercises. This included gentle squeezing of a soft ball, manipulation of small objects, and gradually increasing resistance as tolerated.
- Scar Management: Continue scar massage. Silicone gel sheeting or topical silicone products could be considered if there was any tendency towards hypertrophic scarring.
- Return to Activities: Gradually increase daily activities, avoiding activities that caused pain or excessive stress on the healing tissues. Light occupational duties can often be resumed. Mrs. Vance, as a seamstress, was advised to gradually reintroduce fine motor tasks.
- Addressing Comorbidities: Given Mrs. Vance's diabetes, close monitoring of blood glucose levels was maintained, as optimal glycemic control aids wound healing and reduces infection risk.
Late Phase (Beyond 6 Weeks)
- Full Activity: Most patients can resume full, unrestricted activities, including heavier gripping tasks and occupational demands, by 6-8 weeks post-operatively, provided there are no complications.
- Continued Monitoring: Patients are advised to monitor for any recurrence of symptoms, although this is rare after a complete open A1 pulley release. Persistent pain or stiffness may warrant further hand therapy or investigation.
- Expectations: The patient was advised that complete resolution of all symptoms might take a few weeks, and some residual soreness around the incision site is normal during the healing process.
Potential Post-operative Complications
- Stiffness: The most common complication, prevented by early active motion.
- Infection: Low risk with sterile technique and prophylactic antibiotics (if indicated), but vigilance is required, especially in diabetic patients.
- Recurrence: Rare after complete open release but possible with incomplete release.
- Nerve Injury: Though less common with open technique, digital nerve injury (neuroma, sensory deficit) is a risk if neurovascular bundles are not adequately protected.
- Tendon Bowstringing: Extremely rare, only if the A2 pulley is inadvertently released.
- Hypertrophic Scarring/Keloid: More common in certain individuals, managed with scar massage, silicone, or intralesional injections.
- Persistent Pain/Tenderness: May occur due to nerve irritation or incomplete resolution of inflammation.
- Swelling/Edema: Managed with elevation and compression.
- Reflex Sympathetic Dystrophy (CRPS): A rare but serious complication, characterized by disproportionate pain, swelling, and autonomic dysfunction. Early recognition and aggressive treatment are vital.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Pathognomonic Findings: The key to diagnosing trigger finger is the combination of localized tenderness over the A1 pulley, a palpable nodule (often with movement), and characteristic mechanical triggering/locking.
- Ultrasound Utility: Dynamic ultrasound is an invaluable diagnostic tool, capable of confirming A1 pulley thickening, tendon nodule, tenosynovitis, and real-time visualization of the triggering phenomenon. It can also guide injections.
- Open vs. Percutaneous: For definitive treatment, especially in recurrent cases, fixed flexion deformities, or in patients with comorbidities like diabetes, open A1 pulley release remains the gold standard due to direct visualization and lower recurrence rates.
- Neurovascular Protection: Meticulous dissection and clear identification of the digital neurovascular bundles (running radially and ulnarly to the flexor sheath) are paramount to prevent iatrogenic injury. Always assume anatomical variations.
- Complete Pulley Release: Ensure the entire A1 pulley is longitudinally divided. A tactile and visual confirmation of smooth tendon gliding post-release is essential to prevent recurrence.
- Early Mobilization: Post-operative early active range of motion is crucial to prevent adhesions, stiffness, and accelerate functional recovery. Tendon gliding exercises should be initiated immediately.
- Comorbidity Management: Recognize the increased risks of recurrence and complications (e.g., infection, poor wound healing) in patients with diabetes, rheumatoid arthritis, or hypothyroidism. Optimize systemic control pre- and post-operatively.
- Distal Palmar Crease Incision: A transverse incision in the distal palmar crease is cosmetically superior and less prone to scar contracture than a longitudinal incision.
Pitfalls
- Incomplete Diagnosis: Failing to consider other differentials (e.g., flexor tendon sheath ganglion, MCP joint arthritis, Dupuytren's nodule, nerve entrapment) can lead to misdiagnosis and inappropriate treatment.
- Incomplete A1 Pulley Release: This is the most common cause of recurrence after surgery. Ensure the entire fibrous band is divided. Re-evaluate with active and passive motion during surgery.
- Digital Nerve Injury: A devastating complication, especially with blind percutaneous releases. Always know your anatomy, and in open surgery, visualize and protect the nerves. The radial digital nerve to the thumb and index finger are particularly vulnerable.
- A2 Pulley Injury: Inadvertent incision of the A2 pulley will lead to flexor tendon bowstringing and loss of mechanical advantage, causing significant functional deficit. The A2 pulley is more distal and should not be released.
- Excessive Incision: While transverse is better, an overly long incision can increase the risk of hypertrophic scarring or persistent scar tenderness.
- Fixed Flexion Deformity Neglect: In chronic cases with a fixed flexion contracture (Quinnell Grade IV), simply releasing the A1 pulley may not be sufficient. A capsulotomy of the MCP joint or tenolysis might be required in addition to the pulley release to fully restore extension. Failing to address this can result in persistent contracture.
- Ignoring Concomitant Carpal Tunnel Syndrome: Trigger finger often co-exists with carpal tunnel syndrome. A thorough neurological exam is necessary. If both are present and severe, a staged or concomitant carpal tunnel release may be indicated.
- Infection: While rare, improper sterile technique or inadequate post-operative wound care, especially in immunocompromised patients (e.g., diabetics), can lead to deep space infection.
- Patient Expectations: Manage patient expectations regarding recovery time, potential for residual tenderness, and the (low) risk of recurrence, particularly in complex cases or those with predisposing conditions.
You Might Also Like