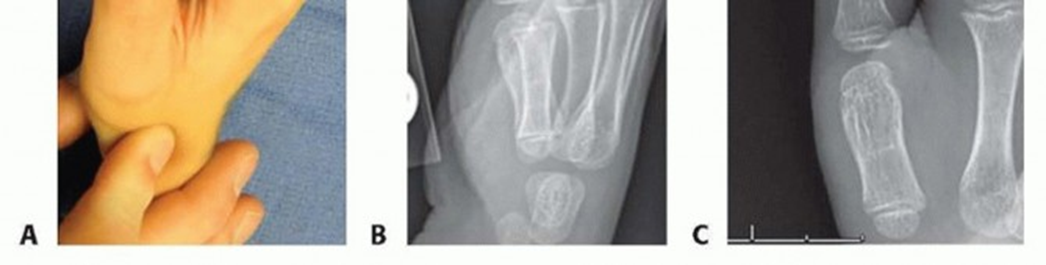
Clinodactyly: Comprehensive Orthopedic Review of Etiology, Anatomy, and Management
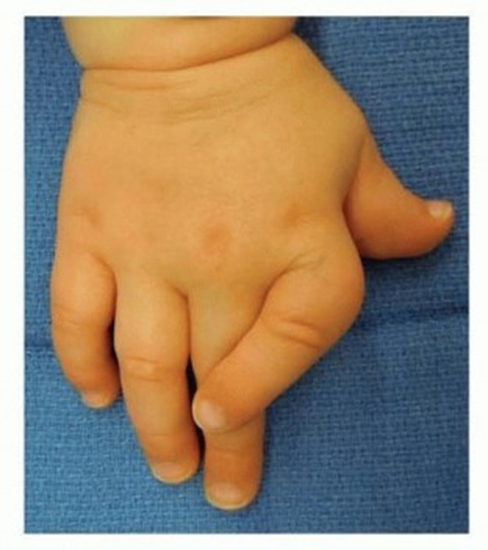
Key Takeaway
Clinodactyly is a congenital deformity causing fixed angular deviation of a digit, most commonly the small finger, due to abnormal phalanx development. Often involving a 'delta phalanx' (longitudinal bracket epiphysis) that tethers growth, it can affect function. Orthopedic evaluation determines if surgical correction is warranted, balancing deformity, function, and psychosocial impact.
Introduction & Epidemiology
Clinodactyly, derived from Greek "klino" (to bend) and "daktylos" (finger), is a congenital deformity characterized by a fixed angular deviation of a digit in the radioulnar plane. The anomaly typically manifests as a curvature towards the ulnar side of the hand, most commonly affecting the small finger (fifth digit). While often described as innocuous and not mandating intervention, understanding its etiology, biomechanical implications, and potential for functional or cosmetic sequelae is crucial for the orthopedic surgeon.
The condition is defined as an abnormal radioulnar angulation exceeding 15 degrees, though some literature cites 10 degrees as a diagnostic threshold. It is frequently bilateral, affecting approximately 60% of cases, and can present as an isolated anomaly or as part of a syndromic constellation.
Epidemiological data suggest a prevalence ranging from 1% to 19% in the general population, with significant variability influenced by diagnostic criteria and population studied. Its incidence is notably higher in individuals with certain genetic disorders, including but not limited to:
*
Down Syndrome (Trisomy 21):
Affecting up to 60% of individuals, typically with hypoplasia of the middle phalanx of the fifth digit.
*
Fanconi Anemia:
Often associated with radial ray deficiencies and other skeletal anomalies.
*
Aarskog-Scott Syndrome:
Characterized by facial, genital, and skeletal abnormalities, including brachydactyly and clinodactyly.
*
Cornelia de Lange Syndrome:
A developmental disorder with growth retardation, intellectual disability, and limb malformations.
*
Fetal Alcohol Syndrome:
Linked to various birth defects, including digital anomalies.
Clinodactyly is generally considered an autosomal dominant condition with variable expressivity when inherited. However, sporadic cases are also common. The primary cause is typically attributed to abnormal development of a phalanx, most frequently the middle phalanx (P2), leading to a trapezoidal or triangular configuration, or an abnormal physis. While usually not associated with significant functional impairment in its mildest forms, severe angulation can impede fine motor skills, grip strength, and cause psychosocial distress, particularly in adolescents.
Surgical Anatomy & Biomechanics
The digital skeleton comprises three phalanges (proximal, middle, and distal) in digits two through five, and two phalanges in the thumb. Each phalanx possesses a proximal and distal articular surface, with the exception of the distal phalanx which has a single proximal articulation. The normal phalangeal physis (growth plate) is located at the proximal portion of each phalanx, responsible for longitudinal growth.
In clinodactyly, the fundamental anatomical deviation lies within the middle phalanx, though involvement of the proximal phalanx can occur. The primary pathological entity is often an irregular physis, specifically a longitudinal bracket epiphysis , also referred to as a delta phalanx .
A delta phalanx is a triangular or trapezoidal-shaped phalanx characterized by a C-shaped epiphysis that extends longitudinally along one side of the bone, forming a "bracket." This abnormal epiphysis essentially tethers or bridges the growth plate along its concave side, preventing normal longitudinal growth on that aspect while allowing continued growth on the opposite, convex side. This differential growth pattern results in progressive angular deformity, typically causing the digit to curve towards the side of the bracketed epiphysis.
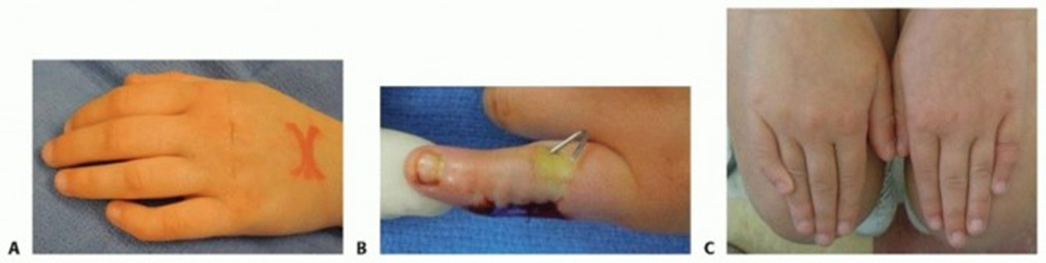
In the context of the small finger, this tethering effect on the radial side of the middle phalanx is the most common etiology, leading to ulnar deviation of the digit. The biomechanical consequence is a loss of normal longitudinal growth vector, replaced by an angular vector. The longer the bracket and the earlier its manifestation, the more pronounced the angular deformity tends to be.

Associated anatomical considerations include:
*
Phalangeal Hypoplasia:
The affected phalanx, particularly the middle phalanx of the small finger, may be intrinsically shorter than normal.
*
Joint Stability:
While the deformity originates in the phalanx itself, severe angulation can lead to secondary adaptive changes in the collateral ligaments and joint capsule of the adjacent interphalangeal joints, potentially affecting stability and range of motion.
*
Neurovascular Bundles:
The digital neurovascular bundles run along the lateral aspects of the digits. Surgical correction must meticulously avoid iatrogenic injury to these critical structures.
*
Extensor and Flexor Tendons:
The tendons glide dorsally and palmarly to the phalanges. Their mechanical axis can be altered by severe angular deformities, potentially leading to inefficient force transmission or secondary contractures.
Understanding these anatomical nuances is paramount for surgical planning, ensuring accurate deformity correction while preserving or restoring digital function.
Indications & Contraindications
The decision to intervene surgically for clinodactyly is complex and multifactorial, balancing the degree of deformity, functional impairment, age of the patient, and psychosocial impact against the potential risks of surgery. Conservative management, primarily observation, is the initial approach for most mild cases.
Non-Operative Indications
- Asymptomatic Deformity: Mild angulation (typically <15-20 degrees) without functional limitation (e.g., no difficulty gripping, typing, or performing daily activities).
- Non-Progressive Deformity: Stable angulation over time, particularly after skeletal maturity.
- Acceptable Cosmesis: When the patient (or parents, in pediatric cases) expresses no significant aesthetic concern.
- Mild Associated Syndromes: In syndromic patients where the clinodactyly is a minor component and does not warrant isolated intervention.
Operative Indications
- Significant Angular Deformity: Generally defined as angulation >20-30 degrees, especially if progressive or causing functional impairment. The threshold may vary based on the affected digit and individual patient factors.
- Progressive Deformity: Evidence of increasing angulation on serial radiographs, particularly in skeletally immature patients. This often indicates an active growth plate anomaly (e.g., longitudinal bracket epiphysis).
- Functional Impairment: Difficulty with pinch grip, power grip, finger opposition, or interference with adjacent digits during activities of daily living.
- Cosmetic Concern: In adolescents and adults, significant psychological distress due to the appearance of the digit, even in the absence of severe functional deficits. This must be carefully evaluated to ensure realistic patient expectations.
- Pain: While rare for clinodactyly itself, chronic irritation or pressure from an adjacent digit due to severe angulation can be an indication.
Contraindications
- Mild, Asymptomatic Deformity: As outlined above, observation is appropriate.
- Significant Comorbidities: Medical conditions that render general anesthesia or surgery excessively risky.
- Unrealistic Expectations: Patients or parents with expectations of "perfect" cosmetic or functional outcomes that cannot be reliably achieved.
- Skeletally Immature Patient with Mild Deformity: Unless progression is documented, intervention in very young children with mild deformity is generally deferred, given the potential for growth disturbance.
Table: Operative vs. Non-Operative Indications
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Angular Deformity | Mild (<15-20 degrees), stable | Moderate to severe (>20-30 degrees), progressive, or functionally limiting |
| Functional Impact | None to minimal | Significant impairment (grip, pinch, adjacent digit interference) |
| Progression | No documented progression | Documented radiographic progression of angulation |
| Patient Age | Any age (observation for mild cases, especially in young children) | Typically school-age to adult, or younger with severe, progressive deformity |
| Cosmetic Concern | None or minor, well-accepted by patient/family | Significant psychological distress due to appearance |
| Pain | Absent | Secondary pain (e.g., from adjacent digit impingement) |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is critical to achieving successful outcomes in clinodactyly correction.
Clinical Assessment
- Detailed History: Including age of onset, progression, family history of clinodactyly or associated syndromes, hand dominance, and specific functional complaints.
-
Physical Examination:
- Visual Inspection: Note the specific digit involved, degree and plane of angulation (often multiplanar), presence of rotational deformity, and overall hand appearance.
- Range of Motion: Assess passive and active range of motion of all digital joints, looking for fixed contractures or hyperlaxity.
- Neurovascular Status: Sensation, capillary refill, and digital perfusion.
- Associated Deformities: Brachydactyly, camptodactyly, syndactyly, or other skeletal anomalies.
- Functional Assessment: Observe grip, pinch, and fine motor tasks.
Radiographic Evaluation
-
Standard Views:
High-quality posteroanterior (PA), lateral, and oblique views of the affected digit and hand. These are essential for:
- Deformity Measurement: Quantification of the angular deviation (e.g., using a digital goniometer or specific phalanx-to-phalanx angles). True angulation can be challenging to measure accurately on 2D images if rotational deformity is present.
- Phalangeal Morphology: Identification of the abnormal phalanx (typically middle phalanx) and its characteristic triangular or trapezoidal shape.
- Physeal Status: Assessment of the growth plate, particularly to identify a longitudinal bracket epiphysis (delta phalanx).
- Skeletal Maturity: Assessment of open or closed physes to guide surgical timing and choice of procedure. Carpal bone ossification can also be used as a proxy for skeletal age.
- Advanced Imaging (Rarely Needed): In complex cases, or where a physeal bar is suspected but not clearly visualized on plain radiographs, MRI or CT scans may offer additional detail regarding the cartilaginous anatomy or osseous architecture.
Surgical Goals
- Correction of angular deformity to acceptable functional and cosmetic levels.
- Restoration of digital alignment to prevent impingement on adjacent digits.
- Preservation of joint motion and stability.
- Prevention of recurrence (especially in skeletally immature patients).
Pre-Operative Discussion
- Thorough discussion with the patient and family regarding realistic expectations, potential complications (e.g., undercorrection, overcorrection, non-union, growth disturbance, stiffness), and the necessity for post-operative rehabilitation.
Patient Positioning
- Anesthesia: General anesthesia is typically employed for pediatric patients. Regional anesthesia (e.g., brachial plexus block) can be an adjunct or primary anesthetic for older cooperative patients, providing excellent post-operative analgesia.
- Supine Position: Patient is placed supine on the operating table.
- Arm Table: The affected upper extremity is positioned on a radiolucent hand table, allowing for fluoroscopic imaging during the procedure.
- Tourniquet: A pneumatic tourniquet is applied to the upper arm for exsanguination and creation of a bloodless field.
- Sterile Prep and Drape: Standard sterile preparation of the hand and arm up to the tourniquet, followed by sterile draping to isolate the operative field.
Detailed Surgical Approach / Technique
The choice of surgical technique depends primarily on the patient's skeletal maturity, the severity of the deformity, and the presence of a longitudinal bracket epiphysis. The primary goals are to correct the angulation and, if applicable, to address the growth plate anomaly.
1. Physeal Bar Resection (for Longitudinal Bracket Epiphysis/Delta Phalanx)
This technique is indicated for skeletally immature patients with an active delta phalanx and significant growth potential remaining. The aim is to excise the abnormal physeal bar, allowing the unaffected side of the physis to resume normal growth and thus correct the deformity over time.
- Incision: A mid-lateral incision over the involved phalanx or a zigzag incision (Bruner incision) can provide good exposure while minimizing scar contracture. The incision should be carefully placed to avoid underlying neurovascular structures.
- Dissection: Meticulous dissection through subcutaneous tissue, identifying and carefully retracting the digital neurovascular bundles (which run volarly to the mid-lateral line). The periosteum over the involved phalanx is incised and elevated.
- Identification of Delta Phalanx: The characteristic triangular or trapezoidal shape of the phalanx and the longitudinally oriented C-shaped epiphysis are identified. Fluoroscopy can aid in precise localization.
- Excision of Physeal Bar: Using fine osteotomes, burrs, or ronguers, the abnormal cartilaginous physeal bar bridging the epiphysis and metaphysis on the concave side of the deformity is meticulously resected. The goal is to create a clear, rectangular defect (epiphyseodesis defect) measuring approximately 3-4 mm in width and extending the full depth of the physis. Care is taken to avoid damaging the healthy growth plate on the convex side.
-
Interposition Material:
To prevent recurrence of bridging, the defect created by the bar resection is filled with an interposition material. Options include:
- Fat Graft: Autologous fat harvested from the forearm or gluteal region is commonly used.
- Bone Wax: Can be packed into the defect.
- Silicone Membrane: Less commonly used, but provides a barrier.
- The interposition material serves to block bone formation across the resected physis.
- Wound Closure: The periosteum is closed (if possible), followed by subcutaneous tissue and skin closure. A soft dressing is applied.
2. Corrective Osteotomy (Closing Wedge Osteotomy)
This is the most common technique for skeletally mature patients or those nearing maturity with established angular deformity, or for patients where physeal bar resection has failed or is not indicated.
- Incision: Similar mid-lateral or zigzag incision over the apex of the deformity, typically the middle phalanx.
- Dissection: Careful dissection, protecting neurovascular structures. Periosteum is elevated.
- Osteotomy Site: The osteotomy is typically performed through the metaphysis of the affected phalanx, close to the center of the deformity. Fluoroscopy is used to confirm precise localization.
-
Wedge Resection:
A precisely measured closing wedge osteotomy is performed on the convex side of the deformity. The size and shape of the wedge are determined pre-operatively based on radiographic measurements to achieve optimal correction. The base of the wedge is resected from the convex side, with the apex directed towards the concave side.
- Often, an osteotomy that is not purely perpendicular to the long axis of the phalanx is required due to the trapezoidal shape. A reverse wedge osteotomy or complex multiplanar osteotomy may be considered in specific cases to address rotational components.
-
Correction and Fixation:
Once the wedge is resected, the bone fragments are carefully manipulated to close the osteotomy gap and correct the angulation.
- K-wire Fixation: One or two smooth Kirschner wires (0.028" to 0.045") are typically used to transfix the osteotomy site and hold the correction. The K-wires are driven percutaneously from the distal phalanx across the interphalangeal joint and osteotomy site, or directly across the osteotomy.
- Mini-Plates and Screws: For larger digits or more stable fixation requirements, small dorsal plates with cortical screws can be used, though K-wires are generally sufficient for phalangeal osteotomies.
- Confirmation: Intra-operative fluoroscopy confirms satisfactory alignment and stable fixation.
- Wound Closure: Layered closure, followed by a soft, protective dressing or splint.

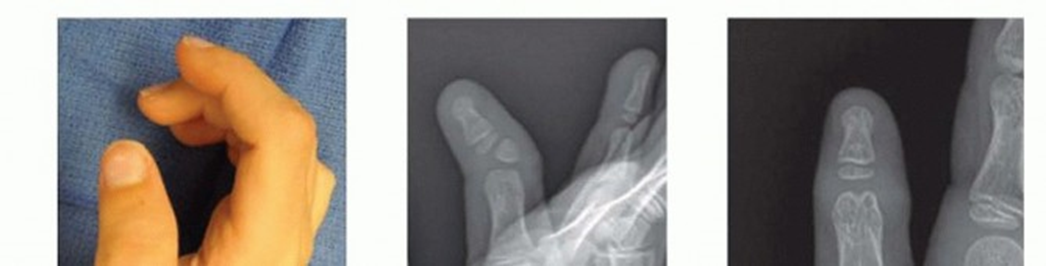
3. Opening Wedge Osteotomy / Distraction Osteogenesis
Less commonly used for primary clinodactyly correction unless significant length discrepancy or hypoplasia is also present. An opening wedge osteotomy would involve creating a transverse cut and inserting a bone graft (autograft or allograft) into the gap to lengthen the phalanx and correct angulation. Distraction osteogenesis uses an external fixator to gradually lengthen the phalanx after an osteotomy, allowing for concurrent deformity correction. These methods are more complex and carry a higher risk profile.
General Surgical Principles:
- Magnification: Use of loupes is highly recommended for meticulous dissection and protection of delicate neurovascular structures.
- Delicate Tissue Handling: Avoid excessive retraction or crushing of soft tissues.
- Hemostasis: Maintain a bloodless field with a tourniquet.
- Precision: Exact measurements and careful execution are essential for optimal deformity correction.
Complications & Management
Surgical intervention for clinodactyly, while generally safe, carries potential risks and complications that require diligent pre-operative counseling and post-operative monitoring.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Management / Salvage Strategy |
|---|---|---|
| Undercorrection / Recurrence | 10-20%, higher in physeal bar resections if not complete or interposition fails. | For physeal bar: Repeat bar resection with more meticulous interposition. For osteotomy: Revision osteotomy after skeletal maturity with definitive fixation; consider distraction osteogenesis for length preservation. |
| Overcorrection | <5% | Mild cases may be observed. Significant overcorrection requiring revision osteotomy; consider reverse wedge osteotomy. |
| Non-union / Delayed Union | 2-5%, higher with extensive bone resection or poor fixation. | Optimize fixation (e.g., plate fixation if K-wires fail); bone grafting (autograft or allograft); pulsed electromagnetic field stimulation. Address underlying issues (e.g., infection). |
| Malunion | 5-10% (angular, rotational, or shortening) | Revision osteotomy to correct the deformity after adequate healing. Precise pre-operative planning for multiplanar deformities. |
| Growth Disturbance | 5-15% (physeal bar resection); <5% (osteotomy in mature physis). | Shortening or angular deformity (due to continued differential growth) may necessitate further corrective osteotomy, lengthening procedures, or epiphyseal arrest if severe and progressive. |
| Infection (Superficial/Deep) | 1-2% | Superficial: Oral antibiotics, local wound care. Deep: Surgical debridement, intravenous antibiotics, hardware removal if necessary. Culture-directed therapy. |
| Neurovascular Injury | <1% (digital nerve paresthesia, vascular compromise). | Immediate exploration and repair if identified intra-operatively (microvascular repair for vessels, microsurgical neurorrhaphy for nerves). Post-operative symptoms require prompt investigation; nerve grafting may be required for significant defects. |
| Stiffness / Range of Motion Loss | 5-15% | Intensive hand therapy, dynamic splinting, judicious K-wire removal. Surgical release (tenolysis, capsulotomy) for persistent, severe contractures after conservative measures fail. |
| Hardware Complications | 5-10% (K-wire migration, breakage, irritation). | Removal of symptomatic hardware. Re-insertion or alternative fixation if stability is compromised. |
| Pain / Scar Sensitivity | 5-10% | Desensitization exercises, massage. Surgical scar revision if severe and impacting function/cosmesis. Local anesthetic injections for neuromas. |
| Reflex Sympathetic Dystrophy (CRPS) | Rare | Early diagnosis and multi-modal treatment including physical therapy, pharmacotherapy (NSAIDs, gabapentin, tricyclics), regional nerve blocks. |
General Management Principles:
- Prevention: Meticulous surgical technique, precise measurement and correction, appropriate fixation, and careful soft tissue handling are paramount.
- Early Recognition: Prompt identification of complications allows for timely intervention, often improving outcomes. Close post-operative follow-up is essential.
- Multidisciplinary Approach: Management of complex complications may involve collaboration with hand therapists, pain specialists, and microvascular surgeons.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing functional outcomes, preventing stiffness, and ensuring proper healing following clinodactyly correction. The protocol varies based on the specific surgical technique employed, patient age, and surgeon preference.
Immediate Post-Operative Phase (Days 0-14)
-
Immobilization:
- K-wire Fixation: The digit is typically immobilized in a protective dressing or a dorsal blocking splint (often incorporating the adjacent digits) for approximately 3-6 weeks to protect the osteotomy or physeal bar resection site. The interphalangeal joints are usually held in slight flexion (e.g., 20-30 degrees) to prevent collateral ligament shortening.
- Plate Fixation: May allow for earlier, controlled motion, but often still requires protective splinting.
- K-wire Care (if applicable): Regular cleaning of K-wire exit sites with antiseptic solution to prevent pin tract infection.
- Edema Control: Elevation of the hand above heart level, gentle compression (if not interfering with K-wires/dressings), and early shoulder/elbow range of motion exercises to promote venous and lymphatic drainage.
- Pain Management: Oral analgesics as prescribed.
- Wound Care: Keep the wound clean and dry. Monitor for signs of infection (redness, swelling, purulent discharge).
Early Rehabilitation Phase (Weeks 3-6)
- K-wire Removal: Typically performed in the clinic at 3-6 weeks post-operatively, once radiographic evidence of early bone healing is present and stability is confirmed. The timing depends on the nature of the osteotomy and patient age.
-
Initiation of Range of Motion (ROM):
- Once K-wires are removed (or if fixed with plates and surgeon permits), gentle active and passive range of motion exercises are initiated for the involved interphalangeal joints.
- Emphasis on full flexion and extension, guided by a certified hand therapist.
- Avoidance of forceful movements or stress across the osteotomy site until robust healing is confirmed.
- Scar Management: Gentle massage, silicone gel sheets, or topical emollients to minimize scar adhesion and hypertrophy.
- Custom Splinting: Static or dynamic splinting may be prescribed to maintain corrected alignment, prevent contractures, and aid in regaining ROM, particularly at night or during rest periods.
Intermediate Rehabilitation Phase (Weeks 6-12)
- Progressive Strengthening: Once adequate bone healing is confirmed radiographically (typically by 6-8 weeks), progressive strengthening exercises for grip and pinch can be initiated.
- Functional Activities: Incorporate activities of daily living that progressively challenge digital dexterity and strength.
- Continue ROM: Focus on achieving full, pain-free range of motion. Joint mobilization techniques may be employed by the hand therapist.
- Dynamic Splinting: May be used to address persistent flexion or extension deficits.
Advanced Rehabilitation Phase (Months 3-6+)
- Return to Activity: Gradual return to sports and strenuous activities, typically after 3-6 months, once full strength, range of motion, and radiographic healing are achieved.
- Monitoring for Recurrence: In skeletally immature patients undergoing physeal bar resection, ongoing clinical and radiographic monitoring is essential for several years to detect any recurrence of angular deformity due to incomplete bar resection or growth plate issues.
- Long-Term Follow-up: Periodic review to assess long-term functional and cosmetic outcomes, especially in growing children.
Key Principles of Rehabilitation:
*
Individualization:
Protocols must be tailored to the individual patient, considering age, co-morbidities, specific surgical procedure, and rate of healing.
*
Patient Education:
Comprehensive patient and family education regarding the importance of adherence to the therapy program is vital.
*
Collaboration:
Close collaboration between the surgeon and hand therapist ensures a coordinated and effective rehabilitation plan.
Summary of Key Literature / Guidelines
The surgical management of clinodactyly has evolved significantly, with various techniques described in the literature, reflecting the diversity of its presentation and underlying etiologies. Key studies and guidelines emphasize a tailored approach based on skeletal maturity and deformity severity.
Seminal Papers & Concepts:
- Longitudinal Bracket Epiphysis (Delta Phalanx): This concept, elucidated by Thevenard and others, forms the basis for understanding the growth disturbance in many cases of clinodactyly. Key contributions have described its morphology and pathomechanics, establishing the rationale for physeal bar resection. Early studies often focused on diagnostic criteria and anatomical variations.
- Osteotomy Techniques: Descriptions of corrective osteotomies, particularly closing wedge osteotomies, have been refined over decades. Seminal work by authors like Miura and Torii (1975) popularized the closing wedge osteotomy for clinodactyly of the small finger, detailing techniques for precise wedge removal and K-wire fixation. Subsequent refinements have addressed rotational components and improved fixation methods.
- Interposition Materials: Research into various interposition materials following physeal bar resection (e.g., fat grafts, bone wax, silicone) has aimed to optimize prevention of recurrence. Studies, particularly in pediatric orthopedic literature, have compared the efficacy of these materials. Autologous fat grafts are generally favored due to biocompatibility and low rates of adverse reactions.
- Growth Modification: The principles of guided growth (hemiepiphysiodesis) and physeal bar resection draw heavily from broader orthopedic experience in managing angular deformities in long bones. While not always a 'growth plate staple' in the same way as lower extremity deformities, the concept is directly applicable.
Consensus and Guidelines:
- Lack of Universal Guidelines: There is no single, globally accepted, evidence-based guideline for the management of clinodactyly due to its relatively low incidence, varied presentation, and the lack of large, prospective, randomized controlled trials. Most recommendations stem from expert opinion, case series, and retrospective studies.
-
Consensus Recommendations:
- Observation for Mild Cases: Most authors agree that mild, asymptomatic clinodactyly (<15-20 degrees) does not require surgical intervention.
- Skeletal Maturity Dictates Technique: The patient's skeletal age is the primary determinant for the choice of procedure. Physeal bar resection is preferred for skeletally immature patients with an active delta phalanx, aiming for growth modulation. Corrective osteotomy is the standard for skeletally mature patients or those nearing maturity with established deformity.
- Functional vs. Cosmetic Indications: While functional impairment is a clear indication for surgery, cosmetic concerns, particularly in adolescents, are increasingly recognized as valid indications, provided patient expectations are realistic.
- Small Finger Predominance: The small finger is most commonly affected, and outcomes for its correction are generally favorable.
- Outcomes: Studies generally report good functional and cosmetic outcomes with low complication rates for appropriate indications and techniques. Residual mild angulation or stiffness can occur.
- Evolution of Management: Earlier techniques sometimes involved simply removing an accessory bone (e.g., in some cases of pseudo-clinodactyly) or less precise osteotomies. Modern approaches emphasize precise radiographic measurement, meticulous soft tissue handling, micro-surgical principles for neurovascular protection, and stable fixation, leading to improved, predictable results. The understanding of the delta phalanx as a primary pathology rather than simply an anatomical variant has significantly refined surgical strategies.
Future Directions:
- Further research is needed to refine criteria for surgical intervention, particularly regarding the threshold for cosmetic indications.
- Long-term outcome studies, especially comparing different surgical techniques in pediatric populations, would strengthen the evidence base.
- Advancements in imaging technology may allow for earlier and more precise diagnosis of subtle physeal anomalies.
- Biomaterials research could lead to improved interpositional grafts to prevent physeal re-bridging.
In summary, the current understanding and management of clinodactyly are grounded in a solid comprehension of digital anatomy and growth plate pathology. Surgical intervention is reserved for cases with significant deformity, functional compromise, or substantial psychosocial impact, with the chosen technique carefully matched to the patient's skeletal maturity and specific anatomical aberration.
Clinical & Radiographic Imaging