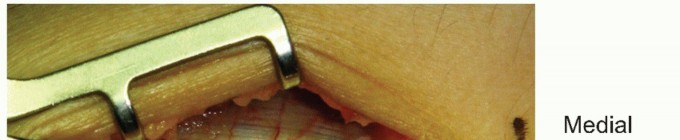
Deep Palmar Space Infections: Epidemiology, Anatomy, and Surgical Principles
Key Takeaway
Deep palmar space infections are severe hand pathologies requiring urgent surgical management due to their proximity to vital neurovascular structures. They arise from trauma or spread, affecting specific hand compartments (lateral/medial spaces) and posing significant risks like tendon rupture and functional loss without prompt intervention, underscoring their critical importance in hand surgery.
Deep Palmar Space Infection: A Critical Threat to Hand Function
Introduction & Epidemiology
Deep palmar space infections represent a severe and potentially limb-threatening pathology within hand surgery. Despite their relative rarity, accounting for a small percentage of all hand infections, their anatomical location and proximity to vital neurovascular structures and tendon sheaths necessitate immediate and aggressive management. Failure to diagnose and treat these infections promptly can lead to profound functional deficits, including severe stiffness, chronic pain, tendon rupture, neurovascular compromise, and even digit loss. The morbidity associated with these infections underscores their critical importance in the surgical armamentarium of the orthopedic hand surgeon.
Historically, before the advent of modern antibiotics, deep palmar infections frequently resulted in severe hand contractures, functional impairment, and widespread sepsis. While systemic antibiotics have significantly altered the natural history of these infections, surgical intervention remains paramount for source control. Current epidemiology suggests that deep palmar space infections often arise from direct penetrating trauma, contiguous spread from tenosynovitis or web space infections, or in the context of immunocompromise, intravenous drug use, or diabetes mellitus. They are distinct from more common superficial infections and demand a high index of suspicion, particularly when standard empirical treatments for less severe infections fail to yield improvement.
Surgical Anatomy & Biomechanics
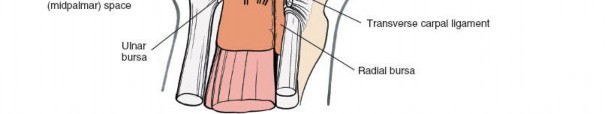
A thorough understanding of the intricate anatomy of the deep palmar spaces is fundamental to effective diagnosis and surgical management. The central compartment of the palm is a critical area, defined by its position deep to the flexor tendons and lumbricals, but superficial to the metacarpals and their associated muscles, including the adductor pollicis and the interossei. This compartment is further subdivided by a crucial fascial septum. This septum originates from the fascia surrounding the flexor tendons of the middle finger and courses radially to attach to the third metacarpal. This division delineates two primary deep palmar spaces: the lateral space and the medial space.
For clarity and to avoid the historical confusion with the thenar musculature, the term lateral space is preferred over "thenar space" when referring to the deep compartment radial to the third metacarpal septum. Similarly, medial space is preferred over "midpalmar space" for the compartment ulnar to this septum.
Lateral Space (Thenar Space Proper)
The lateral space, often conceptually aligned with the deeper "thenar space" in some classifications, is bounded:
*
Radially:
By the adductor pollicis muscle.
*
Ulnarly:
By the fascial septum attaching to the third metacarpal.
*
Dorsally:
By the first and second metacarpals and interossei.
*
Volarly:
By the flexor pollicis longus tendon and the flexor tendons of the index finger, along with their associated lumbricals.
*
Proximally:
It communicates with the radial bursa, which often contains the flexor pollicis longus tendon sheath.
*
Distally:
It can communicate with the first and second lumbrical canals and the first web space.
Infections here typically affect the thumb and index finger, compromising their independent motion.
Medial Space (Midpalmar Space Proper)
The medial space is bounded:
*
Radially:
By the fascial septum attaching to the third metacarpal.
*
Ulnarly:
By the hypothenar muscles and the fifth metacarpal.
*
Dorsally:
By the third, fourth, and fifth metacarpals and their interossei.
*
Volarly:
By the flexor tendons of the middle, ring, and small fingers, along with their respective lumbricals.
*
Proximally:
It communicates with the ulnar bursa (common flexor sheath).
*
Distally:
It can communicate with the third and fourth lumbrical canals and the third and fourth web spaces.
Infections in this space typically present with functional deficits in the middle and ring fingers.

(Figure depicting the intricate fascial planes and compartmentalization of the deep palmar spaces, illustrating the lateral and medial spaces relative to the metacarpals and flexor tendons.)
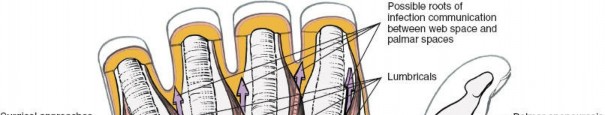
Communicating Pathways
Crucially, understanding the communication pathways of these deep spaces is vital for predicting infection spread and planning thorough debridement.
*
To the Forearm:
Both the radial and ulnar bursae (flexor sheaths) extend proximally into Parona's space in the forearm, creating a potential pathway for infection to spread from the palm to the forearm, or vice versa.
*
To the Dorsum:
Infections can spread dorsally through the lumbrical canals, which connect the palmar spaces with the dorsal subcutaneous space. This explains why dorsal hand swelling can be a prominent feature of palmar infections.
*
To the Web Spaces:
Distally, infections can track into the interdigital web spaces, often manifesting as a "collar button" abscess or a dorsal furuncle.
*
Carpal Tunnel:
The carpal tunnel, though more proximally located, houses the common flexor sheath (ulnar bursa) and the flexor pollicis longus (radial bursa), making it a significant conduit for infection spread between the palm and the forearm.
Biomechanics of Infection
The rigid, unyielding fascial boundaries of the deep palmar spaces, coupled with the dense tissue packing, create a high-pressure environment when inflammation and exudate accumulate. This increased compartmental pressure leads to:
*
Tendon Ischemia and Necrosis:
Direct compression of the flexor tendons and their surrounding vascular supply, impairing gliding mechanisms and potentially leading to adhesions or rupture.
*
Nerve Compression:
Compression of the digital nerves, leading to paresthesias, sensory deficits, and motor weakness.
*
Vascular Compromise:
Direct pressure on digital arteries and the palmar arches, potentially compromising digit viability.
*
Functional Deficit:
The accumulation of inflammatory exudate restricts the normal excursion of flexor tendons and lumbricals. This results in the characteristic inability to actively move the affected digits, and excruciating pain upon passive motion due to stretching of inflamed tissues and increased compartmental pressure. The gross swelling, often described as an "inflated rubber glove," visually represents this critical increase in interstitial pressure.
Indications & Contraindications
The management of deep palmar space infections is predominantly surgical, given the critical nature of the contained structures and the high risk of severe sequelae.
Indications for Operative Management
Surgical drainage and debridement are indicated in nearly all confirmed cases of deep palmar space infection. Specific indications include:
*
Clinical Signs of Abscess:
Localized exquisite tenderness, fluctuance (though deep abscesses may not always be fluctuant), tense swelling, and erythema.
*
Systemic Signs of Infection:
Fever, leukocytosis, elevated C-reactive protein (CRP), and erythrocyte sedimentation rate (ESR).
*
Functional Deficit:
The classic presentation of limited active motion and severe pain with passive motion of the digits corresponding to the infected space (thumb and index for lateral space; middle and ring for medial space).
*
Failure of Conservative Management:
Lack of improvement or worsening of symptoms despite appropriate empiric intravenous antibiotic therapy and hand elevation within 24-48 hours.
*
Imaging Evidence:
Presence of a fluid collection or abscess cavity on ultrasound or magnetic resonance imaging (MRI).
*
Progressive Infection:
Any evidence of spreading cellulitis, lymphangitis, or signs of impending sepsis.
*
Immunocompromised Patients:
A lower threshold for surgical intervention should be maintained due to atypical presentations and rapid progression in these patient populations.
Contraindications for Operative Management
True contraindications to surgical drainage of a deep palmar space infection are exceedingly rare, as this is often a limb-salvaging procedure.
*
Early Cellulitis Without Abscess Formation:
In very early stages, prior to the formation of a macroscopic abscess, a trial of intravenous antibiotics, splinting, and elevation may be considered. However, this necessitates close monitoring, and any sign of progression warrants immediate re-evaluation for surgical drainage. This situation is rare given the typical presentation of deep palmar infections.
*
Patient Unstability:
A patient who is critically unstable and unable to tolerate general or regional anesthesia might pose a relative contraindication. However, local anesthesia with sedation, or even incision and drainage under local infiltration alone, may be employed in emergent, life-threatening situations to achieve source control. The risks of delaying drainage typically outweigh the risks of surgery in a medically optimized patient.
| Management Strategy | Indications |
|-------------------|-------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------- | Off-White | White |
| Light Grey | Dark Grey |
| Grey |
| Black |
| Charcoal |
Table: Fabric Colors
| Color | Fabric Type | Pattern | Style |
|---|---|---|---|
| Off-White | Polyester | Floral | Contemporary |
| Light Grey | Cotton Blend | Geometric | Modern |
| Grey | Linen | Solid | Minimalist |
| Black | Velvet | Stripe | Traditional |
| Charcoal | Chenille | Plaid | Rustic |
| White | Satin | Abstract | Eclectic |
| Dark Grey | Microfiber | Dot | Transitional |
Table: Fabric Properties
| Fabric Type | Durability | Softness | Water Resistance | Stain Resistance | Hypoallergenic | Care Instructions |
|---|---|---|---|---|---|---|
| Polyester | High | Medium | Low | High | Yes | Machine Wash |
| Cotton Blend | Medium | High | Low | Medium | Yes | Machine Wash |
| Linen | Medium | Medium | Low | Low | Yes | Dry Clean Only |
| Velvet | Medium | High | Low | Low | No | Dry Clean Only |
| Chenille | High | High | Low | Medium | No | Machine Wash |
| Satin | Low | High | Low | Low | Yes | Dry Clean Only |
| Microfiber | High | High | High | High | Yes | Machine Wash |
Table: Fabric Maintenance
| Care Instruction | Description |
|---|---|
| Machine Wash | Wash in cold water with mild detergent. Tumble dry low. |
| Dry Clean Only | Professional dry cleaning recommended. |
| Spot Clean | Blot spills immediately with a clean cloth and mild soap. |
| Vacuum | Regularly vacuum with a soft brush attachment. |
| Avoid Direct Sun | Protect from prolonged exposure to direct sunlight to prevent fading. |
| Fluff Cushions | Regularly fluff and rotate cushions to maintain shape and even wear. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for a successful outcome in deep palmar space infections. This involves a comprehensive diagnostic workup, appropriate antibiotic prophylaxis, and careful consideration of anesthesia and patient positioning.
Diagnostic Workup
- Clinical Assessment: The cornerstone remains a detailed history and physical examination. Assess the extent of swelling, erythema, tenderness, and crucially, the specific digits affected by pain and limited motion. Palpate carefully for fluctuance, though deep collections may not be readily palpable. Document neurovascular status.
- Laboratory Studies: Obtain a complete blood count (CBC) with differential, C-reactive protein (CRP), and erythrocyte sedimentation rate (ESR). These markers help assess systemic inflammation and track response to treatment. Blood cultures should be drawn, especially in febrile or systemically unwell patients, prior to antibiotic administration if possible.
-
Imaging:
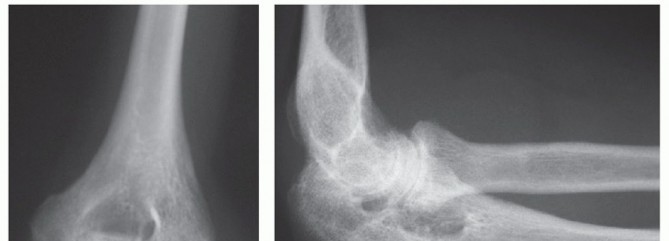
- Plain Radiographs: Primarily to rule out foreign bodies (especially radiopaque ones), osteomyelitis, or septic arthritis if bone or joint involvement is suspected.
- Ultrasound: Can be highly valuable for identifying fluid collections, guiding aspiration (though rarely indicated for deep palmar spaces due to risk), and distinguishing between cellulitis and abscess. It is operator-dependent.
- Magnetic Resonance Imaging (MRI): The gold standard for delineating deep space infections, identifying the extent of abscess, differentiating between pus and edema, and assessing involvement of tendons, bones, and joints. MRI provides excellent soft tissue contrast but is often not immediately available in an emergency setting.
- Computed Tomography (CT): Useful if osteomyelitis or complex bone architecture is a concern, but less effective than MRI for soft tissue definition.
Antibiotic Management
-
Empiric Broad-Spectrum Therapy:
Initiate intravenous broad-spectrum antibiotics immediately upon diagnosis, particularly before surgery. Coverage should target common skin flora, including
Staphylococcus aureus
(often MRSA) and
Streptococcus
species.
- Common regimens include vancomycin (for MRSA coverage) plus a beta-lactamase inhibitor (e.g., piperacillin-tazobactam) or a carbapenem.
- In cases of suspected animal bites or specific exposures, adjust coverage accordingly (e.g., amoxicillin-clavulanate for animal bites).
- Tailored Therapy: Once intraoperative cultures are obtained, modify antibiotic therapy based on sensitivities.
Anesthesia
- Regional Anesthesia: An axillary or supraclavicular block is often preferred as it provides excellent analgesia and motor block, often with prolonged post-operative pain control. This avoids the systemic effects of general anesthesia and allows the patient to remain awake or lightly sedated.
- General Anesthesia: May be necessary for anxious patients, prolonged cases, or when regional blocks are contraindicated or fail.
- Local Anesthesia: Seldom sufficient for deep palmar space infections due to the diffuse nature of the inflammation and the need for thorough exploration.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Arm Abduction: The affected arm is abducted on a specialized hand table, ensuring comfortable access for the surgical team.
- Tourniquet Application: A pneumatic tourniquet is applied to the upper arm. This is crucial for achieving a bloodless field, which is indispensable for precise dissection in the intricate anatomy of the hand. Inflation to 250-300 mmHg (or 100 mmHg above systolic BP) is typical.
- Prep and Drape: The entire hand and forearm are meticulously prepped with an antiseptic solution (e.g., povidone-iodine or chlorhexidine) and draped in a sterile fashion to allow for potential extension of incisions proximally into the forearm if necessary.
- Magnification: Loupe magnification (2.5x to 4.0x) is highly recommended to aid in the precise identification and protection of vital neurovascular structures.
Detailed Surgical Approach / Technique
The primary goal of surgical management is complete drainage of the pus, debridement of necrotic tissue, reduction of compartmental pressure, and collection of cultures, while preserving vital structures.
General Principles
- Adequate Exposure: Incisions must provide sufficient access for thorough exploration and drainage, without compromising future hand function or vascularity.
- Protection of Neurovascular Structures: Meticulous dissection is paramount to avoid injury to digital nerves and arteries, superficial palmar arch, deep palmar arch, and their branches.
- Thorough Debridement: All purulent material and non-viable tissue must be removed.
- Copious Irrigation: The infected spaces must be thoroughly irrigated with sterile saline.
- Culture Collection: Swabs for Gram stain, aerobic and anaerobic cultures, and potentially fungal/mycobacterial cultures should be obtained from multiple sites within the infected space.
- Drainage: Placement of drains (Penrose or suction) is crucial to prevent re-accumulation of fluid.
- Delayed Closure: Wounds are typically left open, often with loose packing, to allow for continued drainage and facilitate inspection during subsequent dressing changes. Delayed primary closure or secondary healing is the norm.

(Figure illustrating various palmar incision approaches for drainage of deep palmar spaces, emphasizing the optimal placement for accessing lateral and medial compartments while avoiding major neurovascular bundles.)
Incisions for Drainage
1. Lateral Space (Thenar Space) Drainage:
*
Incision:
A longitudinal incision is typically made along the ulnar border of the thenar eminence. This incision courses parallel to the thenar crease, extending from the distal palmar crease to the proximal aspect of the thumb metacarpal. Alternatively, a more curved incision following the thenar crease can be used. Another approach involves a longitudinal incision in the intermetacarpal space between the first and second metacarpals on the palmar aspect, carefully retracting the thenar muscles radially.
*
Dissection:
1. Incise skin and subcutaneous tissue.
2. Carefully identify and protect the digital neurovascular bundles to the thumb and index finger. The recurrent motor branch of the median nerve to the thenar muscles must be protected, usually lying more radially and superficial.
3. Bluntly dissect through the subcutaneous tissue and the thin fascia overlying the lateral space.
4. The space lies deep to the flexor pollicis longus tendon and the flexor tendons of the index finger, and superficial to the adductor pollicis muscle and the first metacarpal.
5. Once the space is entered, purulent material will typically be evident.
6. Perform thorough irrigation and debridement.
7. Place a Penrose drain and secure it.

(Figure demonstrating the surgical exposure of the lateral palmar space, showing the key anatomical structures encountered during dissection.)
2. Medial Space (Midpalmar Space) Drainage:
*
Incision:
A longitudinal incision is preferred for direct access and can be made along the length of the third or fourth metacarpal on the palmar aspect, avoiding the major palmar creases. A common approach is to make a longitudinal incision between the third and fourth metacarpals, or directly over the third metacarpal. Transverse incisions following palmar creases may be considered for cosmetic reasons but often provide less adequate exposure for deep space infections.
*
Dissection:
1. Incise skin and subcutaneous tissue.
2. Identify and protect the digital neurovascular bundles, particularly those running between the metacarpals, as well as branches of the median and ulnar nerves to the lumbricals.
3. Carefully incise the deep palmar fascia. The medial space lies deep to the common flexor sheath and the flexor tendons of the middle, ring, and small fingers, and superficial to the third, fourth, and fifth metacarpals and the interossei.
4. The fascial septum arising from the middle finger's flexor tendons and attaching to the third metacarpal serves as a key landmark, separating the medial from the lateral space.
5. Upon entry, drain pus, obtain cultures, and perform thorough irrigation.
6. Explore the space thoroughly with a blunt instrument to ensure all loculations are broken down. Pay attention to communications with the lumbrical canals and potential proximal spread.
7. Place a Penrose drain, ensuring it exits through a separate stab incision if necessary to avoid direct irritation to the main incision.
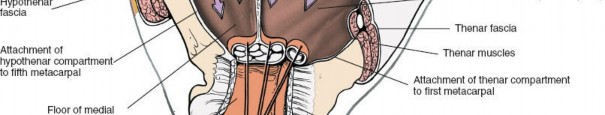
(Figure illustrating the surgical access to the medial palmar space, detailing the anatomical landmarks and safe dissection planes.)
General Steps Following Incision and Drainage (Both Spaces)
- Debridement: Remove any obviously necrotic or unhealthy tissue.
- Irrigation: Copiously irrigate the entire cavity with warm sterile saline. Avoid harsh antiseptics that can damage healthy tissue.
- Culture: Take multiple culture swabs from different areas of the purulent material and infected tissue. Send for Gram stain, aerobic, anaerobic, and potentially fungal/mycobacterial studies.
- Drain Placement: Position a Penrose drain or small suction drain within the deepest part of the cavity, securing it with a skin stitch to prevent migration. The drain should exit through a separate incision or the primary incision without undue tension.
- Wound Management: The primary incision is typically left open or loosely approximated with a few interrupted sutures if skin closure is desired without tension. Some surgeons prefer to pack the wound loosely with saline-soaked gauze.
- Dressing: Apply a bulky, sterile dressing that provides gentle compression and elevates the hand.
- Splinting: The hand is typically immobilized in a position of safety (wrist slightly extended, MP joints flexed 70-90 degrees, IP joints extended) to reduce pain, prevent stiffness, and protect the surgical site.

(Figure depicting the post-operative appearance of a drained deep palmar space infection, showing drain placement and open wound management.)
Complications & Management
Deep palmar space infections, by their nature and anatomical location, carry a high risk of significant complications despite optimal surgical and medical management. These complications can range from immediate surgical issues to long-term functional impairments.
Common Complications
| Complication | Incidence (General Estimate) | Salvage Strategy |
|---|---|---|
| Incomplete Drainage | 10-20% | Re-exploration, additional incisions, wider debridement, improved drain placement |
| Persistent or Recurrent Infection | 5-15% | Culture-guided antibiotics, repeat surgical drainage/debridement, debridement of sequestrum (osteomyelitis) |
| Tendon Adhesions & Stiffness | High (30-60%) | Aggressive hand therapy, dynamic splinting, tenolysis (delayed, after infection clear) |
| Tendon Rupture | Rare-Moderate (2-10%) | Tendon repair/reconstruction (graft or transfer) after infection resolution |
| Nerve Injury (Sensory/Motor) | Rare-Moderate (2-5%) | Nerve repair/grafting (delayed), neurolysis, targeted hand therapy, pain management |
| Osteomyelitis/Septic Arthritis | Rare-Moderate (1-5%) | Prolonged antibiotics, serial debridement, sequestrectomy, joint fusion/arthroplasty |
| Contractures (e.g., MP flexion) | Moderate-High (20-40%) | Serial splinting, dynamic splinting, Z-plasties, skin grafting, capsulotomy |
| Chronic Pain/CRPS | Moderate (10-20%) | Multidisciplinary pain management, physical therapy, sympathetic blocks, medications |
| Digital Ischemia/Necrosis | Rare (<1%) | Revascularization attempts, amputation (as a last resort) |
| Functional Impairment | High (overall) | Comprehensive hand therapy, occupational therapy, assistive devices, vocational retraining |
Management Strategies
- Incomplete Drainage: Often manifests as persistent pain, swelling, and systemic signs despite initial surgery. Requires prompt re-exploration, identifying missed loculations or inadequate incisions, and ensuring complete evacuation of pus.
- Persistent/Recurrent Infection: Guided by intraoperative cultures and post-operative monitoring. If cultures suggest resistant organisms or if there's clinical deterioration, adjust antibiotic regimen. Repeat debridement may be necessary. If osteomyelitis is suspected, MRI and potentially bone biopsy are indicated, with prolonged antibiotic courses (often 6 weeks or more) and serial debridement of infected bone.
- Tendon Adhesions and Stiffness: This is arguably the most common and debilitating long-term complication. Prevention begins with careful surgical technique to minimize tissue trauma and early, controlled post-operative mobilization. Once established, aggressive hand therapy, including passive and active range of motion exercises, dynamic splinting, and scar massage, is critical. Tenolysis, a surgical procedure to release adhesions, may be considered once the infection is definitively resolved and the inflammatory phase has subsided (typically 6-12 months post-infection).
- Tendon Rupture: If flexor tendons are compromised by infection, they may rupture. Management involves delayed tendon repair or reconstruction, often requiring tendon grafting or transfer, after the infection has completely cleared.
- Nerve Injury: Can occur either iatrogenically during surgery or due to direct compression/inflammation from the infection. Neuropraxia or axonotmesis may resolve spontaneously with time. Neurotmesis or significant injury may require delayed nerve repair or grafting, usually 3-6 months after the acute infection is resolved.
- Contractures: Particularly common are metacarpophalangeal (MP) joint flexion contractures and web space contractures due to scarring of the palmar fascia. Aggressive therapy with splinting (static progressive or dynamic) is the first line. Surgical release (capsulotomy, Z-plasties, skin grafting) may be necessary for recalcitrant contractures.
- Chronic Pain/CRPS: A challenging complication requiring a multidisciplinary approach involving pain specialists, physical therapists, and occupational therapists. Treatments may include medication, nerve blocks, sympathetic blocks, and neuromodulation techniques.
- Digital Ischemia/Necrosis: A rare but devastating complication, typically resulting from overwhelming infection and vascular thrombosis. Requires urgent re-evaluation for revascularization and debridement. Amputation may be the only option in cases of irreversible tissue loss.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgery itself in maximizing functional recovery and minimizing long-term disability. A structured, progressive, and individualized hand therapy program is essential.
Phase I: Acute Inflammatory/Protection Phase (Days 0-2 Weeks)
Goals:
Control pain and edema, protect the surgical site, prevent further infection, maintain joint mobility in uninvolved digits, introduce gentle motion in involved digits.
*
Wound Care:
Daily dressing changes with meticulous hygiene. Monitor for signs of persistent infection (erythema, purulence, increasing pain). Drains are typically removed once output is minimal (24-72 hours).
*
Edema Control:
Strict hand elevation (above heart level), gentle active range of motion (AROM) of uninvolved joints (shoulder, elbow, wrist), light compression garment once wounds are healing.
*
Pain Management:
Opioids, NSAIDs, and regional nerve blocks as needed.
*
Splinting:
Custom or off-the-shelf splint maintaining the hand in a "position of safety" or "intrinsic plus" position (wrist 15-30° extension, MP joints 70-90° flexion, IP joints near full extension). This position minimizes collateral ligament shortening and prevents MP joint hyperextension contractures.
*
Gentle Motion:
*
Passive Range of Motion (PROM):
Initiated carefully for involved digits, within pain limits, to prevent capsular stiffness and tendon adhesions.
*
Active Range of Motion (AROM):
Gentle active hook and straight fisting exercises for digits adjacent to the infection, gradually increasing as pain allows for involved digits. The goal is early tendon gliding without excessive tension.
*
Patient Education:
Instructions on wound care, signs of infection, importance of elevation, and adherence to therapy.
Phase II: Subacute/Mobilization Phase (Weeks 2-6)
Goals:
Improve range of motion, minimize scar tissue formation, begin light strengthening, and enhance functional use.
*
Scar Management:
Initiate scar massage once wounds are closed and stable. Silicone gel sheets or scar pads may be used to soften and flatten scars.
*
Progressive Range of Motion:
*
AROM and PROM:
Intensify exercises for all affected joints. Focus on full flexion and extension of all digital joints, and full thumb motion.
*
Blocking Exercises:
Isolate motion to specific joints (e.g., blocking MP flexion to encourage IP flexion).
*
Place and Hold Exercises:
Passively position the finger into flexion and then actively hold it to recruit intrinsic muscles.
*
Dynamic/Static Progressive Splinting:
May be introduced to address developing contractures or persistent stiffness, applying low-load, long-duration stretch.
*
Light Strengthening:
Begin with gentle isometric exercises, progressing to light resistance with therapy putty or resistance bands as appropriate.
*
Fine Motor Coordination:
Introduce tasks to improve dexterity and coordination.
Phase III: Return to Function/Strengthening Phase (Weeks 6-12+)
Goals:
Maximize strength, endurance, fine motor skills, and return to work/activity-specific function.
*
Advanced Strengthening:
Progress to heavier resistance exercises, grip strengthening, and pinch strengthening.
*
Functional Activities:
Incorporate occupation-specific or sport-specific training. Simulate daily activities requiring dexterity and strength.
*
Endurance Training:
Repetitive tasks to build muscular endurance.
*
Advanced Scar Management:
Continue scar management as needed.
*
Addressing Residual Deficits:
Evaluate for any remaining range of motion deficits, weakness, or pain. Consider advanced interventions (e.g., further splinting, surgical tenolysis, or capsulotomy) if therapy plateaus.
*
Proprioception and Sensory Re-education:
If nerve injury occurred, initiate sensory re-education protocols.
Throughout all phases, close communication between the surgeon and the hand therapist is paramount to adjust the protocol based on patient progress and surgical healing. Patients must be diligently followed for months, and sometimes years, to address potential late complications such as chronic stiffness or pain.
Summary of Key Literature / Guidelines
Deep palmar space infections, while rare, consistently feature in foundational texts and surgical guidelines due to their potential for severe functional morbidity. The literature consistently emphasizes several key principles that have remained steadfast despite advancements in medical technology:
- Early Diagnosis and High Index of Suspicion: Numerous case reports and retrospective series highlight the challenge in early diagnosis given the deep location and often non-specific initial symptoms. The characteristic "inflated rubber glove" appearance and specific digital immobility (index/thumb for lateral, middle/ring for medial) are critical clinical pearls. Imaging, particularly MRI, has evolved to provide definitive confirmation, reducing diagnostic delay compared to historical reliance solely on clinical signs.
- Aggressive Surgical Drainage and Debridement: This remains the cornerstone of treatment, universally endorsed across surgical specialties. Classic texts like Green's Operative Hand Surgery and Campbell's Operative Orthopaedics provide detailed surgical approaches, emphasizing the need for adequate exposure, thorough irrigation, and protection of neurovascular structures. Incomplete drainage is a frequent cause of treatment failure and demands a low threshold for re-exploration. The principle of leaving wounds open for delayed closure or secondary intention to allow for continued drainage is widely accepted.
- Appropriate Antibiotic Therapy: Prompt initiation of empiric broad-spectrum intravenous antibiotics is critical, targeting common pathogens such as S. aureus (including MRSA) and Streptococcus species. Subsequent tailoring of antibiotics based on intraoperative culture and sensitivity results is standard practice. Recent literature also emphasizes the increasing prevalence of polymicrobial infections and the need to consider atypical pathogens in specific patient populations (e.g., immunocompromised, IV drug users).
- Meticulous Post-Operative Wound Care and Rehabilitation: The literature strongly supports the necessity of early, structured hand therapy to mitigate stiffness, adhesions, and contractures, which are the most common long-term sequelae. Protocols advocating for early, controlled range of motion within the limits of pain and wound healing are widely practiced. The importance of edema control and scar management is also consistently highlighted.
- Understanding of Anatomy and Communication: Studies consistently refer back to the intricate fascial anatomy of the hand as described by Kanavel, confirming the critical role of the deep palmar spaces and their communication pathways (e.g., lumbrical canals, Parona's space) in guiding surgical intervention and predicting infection spread.
- Multidisciplinary Approach: Successful outcomes often involve a collaborative effort between the orthopedic hand surgeon, infectious disease specialists, and certified hand therapists.
While the incidence of these infections remains low, their potential to devastate hand function necessitates unwavering adherence to these established principles. Continued vigilance in diagnosis, decisive surgical management, targeted antibiotic therapy, and diligent rehabilitation remain paramount to achieving optimal functional recovery for patients afflicted with deep palmar space infections.
Clinical & Radiographic Imaging
You Might Also Like