Knee Special Tests: Expert Opinion Comments for Accurate Diagnosis

Key Takeaway
Here are the crucial details you must know about Knee Special Tests: Expert Opinion Comments for Accurate Diagnosis. The Valgus test primarily detects pain or laxity in the medial collateral ligament (MCL). Clinicians apply valgus stress to the knee at 20-30° flexion and full extension. A positive result, such as medial pain or excessive movement, indicates MCL injury. Expert opinion comments suggest that laxity in full extension signifies major knee disruption, potentially involving cruciate ligaments and the posterior capsule.
KNEE EXAMINATION SPECIAL TESTS
CHAPTER
6
KNEE
● A ONE-PLANE TESTS
183
Valgus test 183
Varus test 186
Posterior drawer test 188
Anterior drawer test 191
Lachman’s test 194
●
B
MULTI-PLANE TESTS
198
-
Anteromedial rotatory instability (AMRI)
198
Slocum (AMRI) test 198 -
Anterolateral rotatory instability (ALRI)
199
Slocum (ALRI) test 199 -
Posteromedial rotatory instability (PMRI)
204
Pivot shift test 201 -
Posterolateral rotatory instability (PLRI)
205
Posteromedial drawer test 204
181
Posterolateral drawer test 205
Reverse pivot shift test 207
Dial test 209
External rotation recurvatum test 211
● C MENISCAL TESTS
212
Apley’s test 212
McMurray’s test 215
Weight-bearing/rotation meniscal test 218
●
D
PATELLOFEMORAL TESTS
221
McConnell test 221
Patella apprehension test 224
Patellofemoral grind test 225
●
E
OTHER TESTS
227
Noble’s compression test 227
Mediopatellar plica test 229
●
A
ONE-PLANE TESTS
Valgus test

Aka
Abduction stress test
Purpose
To primarily detect pain and/or laxity of the medial collateral ligament (MCL).
Technique
Patient position
Lying supine with the leg relaxed.
Clinician position
Standing on the outside of the affected leg; the patient’s lower leg is lifted and supported between the waist and the inside of the clini-cian’s elbow with the knee flexed to about 20–30° and the hip positioned in a degree of internal rotation and abduction. The heel of the outside hand is placed just above the lateral joint line, the inside hand is placed just below the medial joint line where the thumb can palpate the medial tibiofemoral joint line.
Action
Firm inward pressure is applied with the outside hand and outward pressure with the inside hand while rotating the body away from the end of the couch to achieve a valgus stress to the knee. The test can then be repeated with the knee in full extension.
Positive test
The reproduction of medial knee pain alone is suggestive of injury to the MCL. An intact ligament produces a normal ligamentous end-feel where firm resistance to the valgus stress is noted. Loss of this normal resistance and an increase in valgus movement (in excess of 15°) suggests structural damage to the MCL indicative of a more significant injury involving other structures.
In full extension stability to the joint is afforded by the cruciate ligaments and laxity in this position is likely to represent major disruption to the knee and concurrent injury to the posterior capsule, posterior cruciate ligament (PCL) and possibly the anterior cruciate ligament (ACL) should be suspected (
Malanga et al
2003
,
Slocum & Larson
1968).

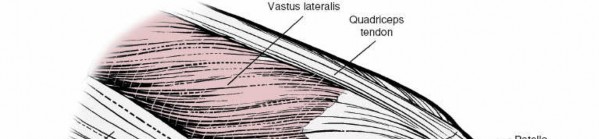
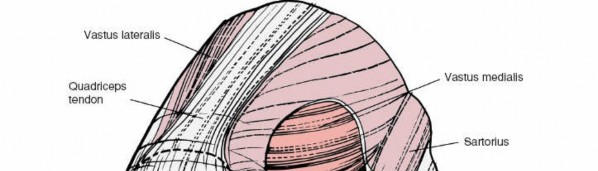
Fig. 6.1 ● Valgus test.
Clinical context
The MCL is the most commonly injured knee ligament and the valgus stress test is the primary tool for assessing the integrity of its deep and superficial fibres. In addition the posteromedial capsule, posterior oblique ligament, PCL and ACL will also be subject to stress during this manoeuvre.
In the acute injury, full physical assessment may not be possible because of pain, apprehension and swelling, so diagnosis may depend on assessment of the force and mechanism of injury, the degree of pain, the rapidity of swelling (immediate, significant swelling suggesting haemarthrosis) and the degree of disability.
Assessment of the subacute or chronic lesion allows the MCL injury to be graded (
Bulstrode et al
2002
,
Kesson & Atkins
2005):
Grade
|
Findings
| ---|---|
Minor/ grade I
| Pain, tenderness and diffuse swelling with medial joint gapping of less than 5 mm on valgus testing with maintenance of the normal joint end-feel and a minimal suction sign (drawing in the skin over the medial joint line) signifies some MCL microfailure but no instability
Moderate/ grade II
| Pain, tenderness and local swelling with medial joint gapping of 5–10 mm on valgus testing with maintenance of the normal joint end-feel and a marked suction sign caused by moderate to major MCL tear. Minor ligamentous laxity does not usually result in serious functional instability unless the demands on the knee are high
Grade
|
Findings
| ---|---|
Severe/ grade III
| Severe pain at the time of injury, significant swelling and possible haemarthrosis. Gapping of greater than 10 mm, with loss of the definite ligamentous end-feel, indicating a complete MCL rupture
Imaging with stress X-rays and/or MRI may help grade the injury more specifically and determine the presence of concurrent damage to other structures.
Although valgus stress is the most frequently used test in assessing injury to the MCL, the absence of an appropriate reference standard against which to measure the accuracy of mild injury or rupture has resulted in little evidence to support its use. Only one study reported a sensitivity of 86% for MCL tears using arthroscopy as a reference standard (
Malanga et al
2003).
Clinical tip
Ensuring that the hip is internally rotated prevents extraneous movement of the leg during testing and allows the application of selective stress on the structures responsible for stabilizing the medial aspect of the knee. A positive test in slight knee flexion incriminates the MCL and/or posterior capsule, as this position takes tension off the ACL which provides a secondary restraint to valgus in full extension. When repeated in full extension, a positive test suggests damage not only to the MCL and posterior capsule but also to one or both cruciate ligaments.
Tibial rotation has an opposite effect on the collateral and cruciate ligaments. In
external
rotation the MCL/lateral collateral ligament are more taut and the ACL/PCL more lax and in
internal
rotation the opposite is true. The degree of MCL stress during this test can therefore be increased by adding external rotation of the tibia.
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
|
Valgus test
*
Used in every patient as a screening test for medial knee stability and pain.

Varus test
-
Aka
Hughston’s varus stress test Adduction stress test -
Purpose
To primarily detect pain and/or laxity of the lateral collateral ligament (LCL). -
Technique
Patient position
Lying supine towards the edge of the couch.
Clinician position
Standing on the affected side, the leg is lifted off the couch and the hip is passively abducted far enough to allow the clinician to stand in the space between the inside of the leg and the side of the couch. The patient’s lower leg is supported between the waist and the outer elbow and the hip is positioned in some degree of internal rotation. The heel of the outside hand is placed on the upper tibia just below the lateral joint line and the inside hand is placed just above the medial joint line on the lower femur.
Action
With the knee in about 20° of flexion and the hip internally rotated, firm pressure is applied with both hands to achieve a varus stress while rotating the body in order to increase leverage.
Positive test
Lateral knee pain or laxity on stress testing. -
Clinical context
Lateral or posterolateral knee injuries are relatively uncommon as the mechanism of injury usually requires an external impact (e.g. being hit by a car or a rugby tackle) to force the knee into an extreme varus position. In contrast to the MCL, the ligament is quite independent of the lateral capsule and meniscus which makes the structure less vulnerable to injury. The normal degree of varus is variable (usually around 7°) and should be compared to the normal knee if laxity is suspected. Stress X-ray showing a lateral opening of more than 8 mm is suggestive of a grade III injury (see ligament injury table, p. 184) and the likelihood of injury to the other posterolateral

Fig. 6.2 ● Varus test.
structures (cruciate ligaments, posterolateral capsule, arcuate–popliteus complex, iliotibial band) increases with the degree of abnormal varus movement detected ( LaPrade & Terry 1997 , Larsen & Toth 2005). Lateral instability, though much less common, is potentially more disabling than medial instability.
Varus stress tests the integrity of the LCL ligament. Although laxity noted on this test may indicate one-plane lateral instability, it is more likely to be positive where there has been injury to the other structures that contribute to posterolateral stability ( Malanga et al 2003 ). If this is suspected, the posterolateral drawer test (see p. 205), dial test (see p. 209) or external recurvatum test (see p. 211) are considered to be more accurate in detecting posterolateral rotational instability (PLRI; Baker et al 1983 ). Conversely, a negative varus test does not rule out PLRI as an intact PCL contributes to varus stability in full extension and may limit varus excursion. In one large study, the LCL was found to be involved in only 23% of PLRI injuries ( LaPrade & Terry 1997).
There is little evidence on the accuracy of any of the tests for the lateral structures of the knee primarily due to the absence of an appropriate reference standard. The clinical findings for lateral and
posterolateral injuries of the knee are often subtle and, as a result, are more frequently misinterpreted ( Hughston et al 1976). -
Clinical tip
To maximize stress on the LCL, the tibia needs to be positioned in slight flexion and as much external rotation as possible as this reduces stress on the cruciates and leaves the iliotibial band lying centrally over the lateral joint line.
The test can be repeated with the knee in full extension and if instability is still detected, major disruption of the knee has occurred and injury to either the cruciates, popliteus or other lateral structures should be suspected along with injury to the LCL ( Larsen & Toth 2005 , Malanga et al 2003).
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Varus test
Used in every patient as a screening test for lateral knee instability.

Posterior drawer test
-
Purpose
To detect posterior (one-plane) instability and posterior cruciate ligament (PCL) laxity. -
Technique
Patient position
Supine with the hip flexed to 45°, the knee flexed to 90° and the foot placed on the couch.
Clinician position
The lower leg is stabilized by sitting on the dorsum of the forefoot. Both hands grasp around the upper tibia with thumbs placed anteriorly over the joint line with the thenar area of both hands positioned over the upper tibia. The fingers can also palpate the hamstring tendons posteriorly to ensure they are relaxed.
Action
The tibia is pushed backwards with both hands. The quality of the joint end-feel should be appreciated and a ligamentous ‘stop’ noted if the ligament remains intact.
Positive test
A positive test is indicated by increased posterior excursion of the tibia and an associated loss of the normal end-feel. An increase in the slope of the infrapatellar tendon may also be noted.

Fig. 6.3 ● Posterior drawer test. -
Clinical context
In a complete PCL tear, the average extent of posterior excursion of the tibia is 9.2 mm although incomplete tears will produce varied degrees of laxity ( Hewett et al 1997 ). Injury of other stabilizing structures (i.e. arcuate–popliteus complex, posterior oblique ligament, iliotibial band) should always be considered as a potential source of pain and/or instability. Posterior excursion can be assessed and graded by measuring the amount of ‘step-off’ between the anterior tibial plateau and the femoral condyles ( Larsen & Toth 2005).
Grade
| Amount of step-off between anterior tibial plateau and femoral condyles
| ---|---|
1
| Palpable step (approx 5 mm)
2
| The normal anterior step is eliminated and the medial femoral condyle and medial tibial plateau are level
3
| The medial tibial plateau is displaced posteriorly in relation to the medial femoral condyle resulting in a reverse ‘step off’. With this finding, posterolateral corner and medial injuries should also be considered
The posterior drawer test is considered to be the most accurate test for diagnosing isolated PCL injuries but this has not been verified in studies examining its use as an isolated test. A high degree of sensitivity and specificity has been recorded where it is used as part of a composite assessment to determine PCL injury, particularly when complemented by other tests such as the posterior sag test ( Malanga et al 2003); analysing the test in this context is helpful as it mirrors usual clinical practice.
Perhaps unsurprisingly, increased inter-examiner reliability has been noted in the presence of more significant grade II and III injuries ( Rubenstein et al 1994).
TABLE 6.1 POSTERIOR DRAWER TEST
Author and year
| LR +
| LR —
| Target condition
Jackson et al 2003
| 16.2
★★★
| 0.2
★★
| PCL tear as part of a composite assessment
Solomon et al 2001
| 21
★★★
| 0.05
★★★
| PCL tear as part of a composite assessment
Rubenstein et al 1994
| 90
★★★
| 0.10
★★
| PCL tear as part of a composite assessment -
Clinical tip
With an isolated tear of the PCL, the greatest degree of tibial excursion is noted at 90° flexion. Where the injury is located to the posterolateral corner, most excursion is found when the test is performed in 30°. In a combined posterolateral corner and PCL injury,
increased posterior tibial movement will be noted when the test is repeated at both 30° and 90° flexion ( Larsen & Toth 2005) and injury to other lateral stabilizers will be likely.
If the PCL is ruptured, the tibia, having lost some posterior restraint, tends to gravitate backwards (posterior sag sign). This false starting position can lead an inexperienced clinician to incorrectly record an increase in anterior tibial translation when in fact there is PCL insufficiency. Observing for a posterior sag of the tibia on the femur and performing the posterior drawer test prior to ACL assessment should guard against this (see related tests).
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Posterior drawer test
A standard test used in all patients which accurately identifies PCL tears. -
Related tests
The posterior sag sign/gravity drawer test/Godfrey’s test is a useful adjunct to the posterior drawer test. The patient lies supine with the hips and knees flexed to 90° and the lower legs supported by the clinician. If posterior instability is present, a posterior ‘sag’ appears and additional backward pressure will increase this posterior displacement.
The active drawer test/quadriceps active test can be helpful in confirming PCL insufficiency. In the drawer test position with the foot stabilized, the patient is asked to attempt to extend the knee. The backwards sag of the tibia will be reduced with this isometric contraction of the quadriceps (bringing the tibia back into its normal position) and increased with hamstring isometric contraction. This positions the tibia in its fully displaced position and provides a good starting position for maximum anterior translation to occur when the quadriceps contract again.

Anterior drawer test
-
Purpose
To detect anterior (one-plane) instability and anterior cruciate ligament (ACL) laxity. -
Technique
Patient position
Lying supine with the knee flexed to 90° and foot placed on the couch.
Clinician position
The patient’s foot is stabilized by sitting on the dorsum of the forefoot. Both hands grasp around the upper tibia with thumbs placed anteriorly over the joint line. Also, in this position the hamstring tendons can easily be palpated to ensure the muscle is completely relaxed and that voluntary or involuntary resistance to the test is avoided.
Action
The tibia is drawn forwards with both hands and a comparison of the degree of anterior translation is made with the other knee. The quality of the joint end-feel should be appreciated and a ligamentous ‘stop’ noted if the ligament remains intact.
Positive test
Increased anterior excursion of the tibia accompanied by the loss of normal ligamentous resistance usually indicates significant

Fig. 6.4 ● Anterior drawer test.
injury. In a healthy knee, it is normal for approximately 6 mm of anterior tibial translation to be present ( Magee 2008). If the ACL is injured in combination with the medial ligament/capsule, a much greater degree of anterior translation will be present (15 mm or more). -
Clinical context
In an evaluation of the evidence around physical tests at the knee, a composite assessment (which included the anterior drawer test) was found to be more accurate than any one single test in diagnosing ligament and meniscal lesions ( Solomon et al 2001 ). The test has also demonstrated a high degree of specificity ( Jackson et al 2003 ) although doubts over its degree of sensitivity led other studies to conclude that the test should be secondary to the more sensitive Lachman (see p. 194) or pivot shift test (see p. 201) ( Benjaminse et al 2006 , Jackson et al 2003 , Ostrowski 2006 , Scholten et al 2003). It is an easier test to perform, however, and for the less experienced practitioner, the findings may be more helpful than trying to detect abnormalities with the pivot shift test. The sensitivity of all these tests improves when testing in the acute stages is avoided and they are used either when the patient is anaesthetized or in the subacute/chronic stage of the condition.
In the test position of 90° knee flexion, the MCL and posterior capsule provide secondary restraints to anterior tibial translation. If these structures are intact and the ACL is injured in isolation, the drawer test will be normal, leading to a false negative result. Other factors that can lead to a false negative result are hamstring spasm, a bucket-handle meniscal tear which blocks anterior translation of the tibia, or a partial ACL tear which has attached to the PCL during the healing process ( Kim & Kim 1995 ). A false positive test can occur (increased anterior translation even when the ACL is intact) if the medial coronary (meniscotibial) ligament has been disrupted ( Magee 2008). Increased anterior excursion of the medial tibial condyle should lead the clinician to conduct further multiplanar tests (see Slocum AMRI, p. 198) to establish the extent of the rotational instability. If a click or sudden shift accompanies a positive drawer test, suspicion of a concurrent meniscal tear should be aroused. The sudden movement or jerk is known as Finochietto’s jump sign ( Magee 2008).
TABLE 6.2 ANTERIOR DRAWER TEST
Author and year
| LR +
| LR —
| Target condition
Scholten et al 200 3 (review)
| 5.17
★★
| 0.43
★
| ACL rupture
Solomon et al 2001 (systematic review and pooled data summary)
| 3.8
★
| 0.3
★
| ACL rupture
Benjaminse et al 2006 (systematic review and pooled data)
| 10.2
★★★
| 0.09
★★★
| Chronic ACL rupture
Katz & Fingeroth 1986
| 7.4
| 0.8
| Acute ACL rupture
★★
| |
under anaesthesia
| 17.93
| 0.48
| Chronic ACL rupture
| ★★★
| |
under anaesthesia
Lee et al 1988
| 78
★★★
| 0.2
★★
| ACL rupture -
Clinical tip
If the posterior cruciate ligament has been injured it can be difficult to establish the normal starting position for this test. PCL laxity or rupture will cause the tibia to drop backwards (posterior sag sign, see p. 191) which then falsely leads to an apparent increase in anterior drawer. It is therefore necessary to eliminate a positive sag sign before recording an increase in anterior drawer.
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Anterior drawer test
Useful as a secondary test if Lachman’s test is equivocal.

Lachman’s test
-
Aka
Anterior drawer in extension test Trillat test
Lachman–Trillat test Ritchie test -
Purpose
To detect anterior (one-plane) instability and anterior cruciate ligament (ACL) laxity. -
Technique
Patient position
Lying supine.
Clinician position
The patient’s foot is stabilized between the clinician’s thigh and the couch. The outside hand is placed over the lateral aspect of the thigh just above the knee joint and the fingers wrapped around the back of the lower thigh while counterpressure is applied anteriorly with the thumb. The inside hand is placed over the medial aspect of the leg just below the knee joint using an identical grip, with the thumb placed over the tibial tuberosity and the knee positioned in about 10–30° of flexion.
Action
With the outside hand stabilizing the femur, the lower hand firmly pulls the tibia forwards in an attempt to generate anterior translation. The quality of the joint end-feel should be appreciated and a firm ligamentous ‘stop’ noted in the normal knee.
Positive test
Increased anterior excursion of the tibia on the femur with an accompanying change in the end-feel usually indicates a significant injury. The firm resistance gives way to a softer or even absent end-feel. The normal slope of the infrapatellar tendon also diminishes.

Fig. 6.5 ● Lachman’s test. -
Clinical context
This is a test for one-plane anterior instability and is the most sensitive physical test for diagnosing an isolated ACL injury. It was originally described by Torg but he named the test after his boss, Lachman ( Torg et al 1976).
In studies using arthroscopy as the ‘gold standard’ for ACL diagnosis ( Jackson et al 2003 , Ostrowski 2006 ) Lachman’s test has been shown to be both more sensitive and specific compared with the anterior drawer (see p. 191) and pivot shift (see p. 201) tests. The Lachman test has also been found to be more accurate than MRI in the diagnosis of ligamentous injury ( Kocabey et al 2004 , Liu et al 1995 , Rose & Gold 1996 ), a negative test thereby effectively ruling out complete ACL rupture ( Scholten et al 2003).
The test is less sensitive where there is complex or acute injury (Frobell et al 2007, Yoon et al 1997 ) and, as with all ligament tests at the knee, is more sensitive when performed under anaesthesia ( Kim & Kim 1995 , Katz & Fingeroth 1986 ). Torg’s original study ( Torg et al 1976) examined its use on patients with combined ACL and meniscal lesions and reported high levels of sensitivity, largely unaffected by the presence of bucket-handle tears. False negative results have been reported however, in cases where there is only a partial tear of the ACL, in chronic lesions where the injured ACL has adhered to the PCL, or where there is a concurrent meniscal injury sufficiently significant to prevent anterior translation of the tibia (Kim & Kim 1995).
In the test position, maximum tension is found in all portions of the ACL ( Kim & Kim 1995). If instability is detected, stress X-rays can assist in grading the degree of injury (see below) although, in practice, clinicians are more likely to use their findings on examination to subjectively grade the degree of tibial translation.
Grade
| Amount of anterior tibial translation
| ---|---|
1
| 5 mm
2
| 5–10 mm
3
| 10 mm -
Clinical tip
In the larger patient, the knee can be supported in the required flexed position over the clinician’s knee, making handling a heavy leg easier.
TABLE 6.3 LACHMAN’S TEST
Author and year
| LR +
| LR —
| Target condition
Scholten et al 2003
| 9.6
★★
| 0.15
★★
| ACL rupture
Solomon et al 2001
| 25
★★★
| 0.1
★★
| ACL rupture
Benjaminse et al 2006
| 14.2
★★★
| 0.16
★★
| Chronic ACL rupture
Katz & Fingeroth 1986
| 15.4
★★★
16.9
★★★
| 0.23
★
0.16
★★
| Acute ACL rupture under anaesthesia
Chronic ACL rupture under anaesthesia
Lee et al 1988
| 88
★★★
| 0.12
★★
| ACL rupture
Jackson et al 2003
| 12.3
★★★
| 0.14
★★
| ACL rupture
The degree of anterior drawer can be palpated if the fingers of the outside hand are placed over the joint line while the tibia is drawn forwards.
The knee must be maintained in a degree of flexion throughout the test to reduce tension on the medial and lateral collateral ligaments and the iliotibial band, thereby minimizing their ability to restrain anterior movement of the tibia ( Magee 2008 ). Lerat et al (2000) suggested that sensitivity of the test was improved by positioning the tibia in slight external rotation with the anterior translatory force coming from a posteromedial direction, as anterior translation of the medial compartment is thought to be a better indication of ACL deficiency in chronic tears than translation of the lateral compartment.
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Lachman’s test
Extremely helpful, with a positive test confirming an ACL tear, but the range must be compared with the unaffected knee as this varies considerably in the normal population.
● B MULTI-PLANE TESTS

- Anteromedial rotatory instability (AMRI) Slocum (AMRI) test
-
Aka
Modified anterior drawer test Lemaire’s ‘T’ drawer test -
Purpose
To detect anteromedial rotatory instability (AMRI) of the knee. -
Technique
Patient position
Lying supine with the hip flexed to 45°, the knee flexed to 90° and the foot placed on the couch.
Clinician position
The foot is turned out so that the tibia is positioned in about 15° of external rotation and then stabilized by sitting on the dorsum of the forefoot. Both hands grasp around the upper tibia, with thumbs placed anteriorly over the joint line in order to be able to detect anterior movement of the tibia. The fingers are well placed to ensure the hamstrings are completely relaxed so that resistance to anterior movement of the tibia is avoided.
Action
The tibia is drawn forwards with both hands and the extent of anterior translation on the medial side of the knee is noted. The quality of the joint end-feel should be appreciated and a ligamentous ‘stop’ noted in the absence of significant injury.
Positive test
Increased anterior excursion of the medial tibial condyle. -
Clinical context
AMRI occurs as a result of a forceful external rotation injury to the flexed knee while the foot is planted (e.g. pivoting on the weight-bearing foot while running or jumping); the injury is therefore often sustained during sporting activities.
The sequence of injury originally described by Slocum & Larson (1968) started with rupture of the medial collateral ligament and medial joint capsule followed by the posterior oblique ligament.
If the knee continues to rotate into further external rotation, especially if accompanied by a valgus force, strain then falls on the anterior cruciate ligament which will ultimately rupture if the force is great enough. With this degree of instability, abnormal loading of the medial meniscus over time will predispose the knee to further injury. Given the structures implicated in AMRI, other physical tests should be used to fully assess the stability of the knee (see Lachman’s test, p. 194; valgus test, p. 183).
The degree of instability can be graded with stress X-rays by measuring the extent of anterior subluxation of the tibia ( Magee 2008) (see below) although, in practice, clinicians are more likely to use their findings on examination to subjectively grade the degree of tibial translation.
Grade
| Amount of anterior tibial translation
| ---|---|
1
| 12 mm
2
| 12–20 mm
3
| 20 mm -
Clinical tip
The tibia must not be fully rotated as this will tension the surrounding structures and could lead to a false negative finding. If abnormal external rotation is noted when placing the leg into the pre-test position, major disruption of the medial capsule and deep portion of the medial ligament should be suspected. Greater degrees of instability would also implicate injury to the more superficial layer of the medial ligament and ACL ( Slocum & Larson 1968).
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Slocum (AMRI) test
There is a lack of evidence to determine relative sensitivities and specificities for this test and it is considered by clinicians to be insufficient, if used in isolation, to diagnose AMRI with confidence. It should therefore be employed alongside other instability tests.

- Anterolateral rotatory instability (ALRI) Slocum (ALRI) test
-
Aka
Modified anterior drawer test -
Purpose
To detect anterolateral rotatory instability (ALRI) of the knee joint. -
Technique
Patient position
Lying supine with the hip flexed to 45°, the knee flexed to 90° and the foot placed on the couch.
Clinician position
The tibia is positioned in about 30° of internal rotation. The foot needs to be stabilized for this test and this can be achieved by sitting on the dorsum of the forefoot. Both hands grasp around the upper tibia with thumbs placed anteriorly over the joint line in order to be able to detect anterior movement of the tibia. The fingers are well placed to ensure the hamstrings are completely relaxed so that muscular resistance to anterior movement of the tibia is avoided.
Action
The tibia is drawn forwards with both hands and the extent of anterior translation on the lateral side of the knee is noted. The quality of the joint end-feel should be appreciated and a ligamentous ‘stop’ noted in the absence of significant injury.
Positive test
Increased anterior excursion of the lateral tibial condyle. -
Clinical context
This is a modification of the anterior drawer test and is thought to detect the degree of anterolateral rotational excursion more specifically. In the normal knee, forward translation of the tibia in this position of internal rotation is prevented by tension in the posterolateral capsule, cruciate ligaments, popliteus tendon, lateral collateral ligament and iliotibial band. A positive test may indicate injury to one or more of these structures ( Slocum & Larson 1968). Some laxity on varus testing (see p. 186) is also often evident, both with the knee flexed and in full extension. -
Clinical tip
The tibia must not be fully rotated as this will increase the tension of the cruciates and surrounding structures, which may reduce the sensitivity of the test and lead to a false negative finding.
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Slocum (ALRI) test
The test can be useful if ALRI is suspected; however it can be difficult to interpret and other, more sensitive and specific tests for ALRI (e.g. pivot shift) may be preferred.

Pivot shift test
-
Aka
Lateral pivot shift test Test of Macintosh -
Purpose
To assess for anterolateral rotational instability (ALRI) and laxity of the anterior cruciate ligament (ACL). -
Technique
Patient position
The patient lies supine with the head supported and leg relaxed.
Clinician position
The patient’s hip is flexed to 45° and abducted to about 30° with the knee in 50° of flexion (the reduced position). The tibia is internally rotated by using the heel as a lever with the thumb of the caudal hand over the lateral border of the calcaneus and the fingers gripping medially. The cephalic hand is placed on the outside of the leg just below the knee joint ( Fig. 6.6A).
Action
While maintaining the internal rotation, a valgus stress is applied with the cephalic hand as the knee is moved towards extension ( Fig. 6.6B).
Positive test
The lateral tibial condyle subluxes forwards on the tibial plateau as the knee approaches extension, sometimes accompanied with a clunk ( Fig. 6.6C).
The tibial condyle can also be reduced by reversing the manoeuvre. The knee is gradually taken into increasing flexion while maintaining the valgus and rotational torque. At around 30° the tibia reduces backwards with a sudden ‘jerk’ – caused by the iliotibial
band (ITB) changing its position and function from an extensor to a flexor and pulling the tibia back into its normal position as a result.
A
B
C






Fig. 6.6 ● The pivot shift test start position (A). As internal rotation, valgus and extension are added, the knee is most likely to sublux at about 30° off full extension (B) before the end position is achieved (C). -
Clinical context
The ACL is intimately involved in controlling the rolling and sliding that takes place during flexion/extension movements of the knee. When torn, the ACL is unable to control this complex mechanism and this leads to a repeated cycle of anterior subluxation (and reduction) of the lateral tibial plateau on the femoral condyle causing the patient to report pain, apprehension to certain movements and giving way on activity. The test assesses the dynamic stability of the knee and often reproduces the ‘giving way’ feeling reported so often by patients. In addition to testing the integrity of the ACL, stress is also placed on the other lateral stabilizers (posterolateral capsule, arcuate–popliteus complex, lateral collateral ligament and the ITB).
The pivot shift test is widely regarded as the primary test for ALRI ( Ostrowski 2006 ) as it is considered to have a high degree of sensitivity and specificity for diagnosing ACL injury ( Katz & Fingeroth 1986 , Malanga et al 2003 ). It has been found to be at least as accurate as MRI in the diagnosis of ACL injury ( Kocabey et al 2004 ) although much of the research has been conducted on anaesthetized patients. The test has been shown to have a much lower level of sensitivity in the alert patient, particularly in acute conditions where it drops as low as 35% ( Donaldson et al 1985). A false negative result can also arise from protective muscle spasm in the acute knee, the inability
of the patient to relax the muscles around the knee adequately or where other pathology/injury exists (e.g. medial collateral ligament injury, partial ACL tear, rupture of the iliotibial tract, lateral compartment osteoarthritis, meniscal injury) ( Kim & Kim 1995).
The test can be difficult to perform in the outpatient setting with an alert patient, and the drawer type tests (Lachman’s test, Slocum test, etc.) are regarded as being easier to perform and more likely to yield an accurate result in this environment. The pivot shift test can be quite uncomfortable for the alert patient (provocation of pain and muscle spasm in the acute knee is common) and is technically more challenging for the clinician – a combination which may lead to an inaccurate result ( Anderson et al 2000).
There are a number of variations on this test (e.g. soft pivot shift test , the jerk test of Hughston , active pivot shift test , Losee test ) but these are no easier to perform well and evidence to support their use is lacking.
TABLE 6.4 PIVOT SHIFT TEST
Author and year
| LR +
| LR —
| Target condition
Scholten et al 2003
| 16
★★★
| 0.69
| ACL rupture
Boeree & Ackroyd 1991
| 10.3
★★★
| 0.7
| ACL rupture and menisci
Benjaminse et al 2006
| 12
★★★
| 0.78
| ACL rupture
Katz & Fingeroth 1986
| 49.2
★★★
| 0.02
★★★
| ACL rupture under anaesthesia
Jackson et al 2003
| 20.3
★★★
| 0.4
★
| ACL rupture -
Clinical tip
The patient should recline in such a way as to ensure the muscles around the knee are completely relaxed when testing. Attention should be paid to the position of the hip as this has considerable bearing on the tension of the ITB – the test is more sensitive when
the hip is positioned into some abduction and less so in adduction. The ITB also needs to be intact in order for the tibia to ‘jerk’ back into a reduced position although the subluxation would still be evident regardless. It is important not to take the knee into full extension as the ‘locking home’ mechanism of the knee forces the joint into a stable position where rotatory instability cannot be detected.
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Pivot shift test
This test requires considerable experience to perform well and evaluate the findings accurately.

- Posteromedial rotatory instability (PMRI) Posteromedial drawer test
-
Aka
Hughston’s posteromedial drawer sign -
Purpose
To assess for posteromedial rotatory instability (PMRI). -
Technique
Patient position
Lying supine with the hip flexed to 45° and the knee flexed to about 90°. The foot is positioned inwards so that the tibia is internally rotated and stabilized on the couch.
Clinician position
The foot needs to be stabilized for this test and this can be achieved by sitting on the dorsum of the forefoot. Both hands grasp around the upper tibia with thumbs placed anteriorly over the joint line in order to be able to detect posterior movement of the tibia.
Action
The tibia is pushed posteriorly, noticing the degree of posterior excursion on the medial side of the knee compared with the unaffected side.
Positive test
The tibia subluxes posteriorly and the posterior part of the medial femoral condyle falls backwards into some internal rotation. This is best assessed by looking at differences in condylar prominences of the tibia when compared to the contralateral knee. -
Clinical context
This variation of the posterior drawer test is used to detect the possibility of PMRI, which should be considered when posterior cruciate and medial collateral ligament rupture co-exist. The anterior and posterior cruciate ligaments, posterior oblique ligament, posteromedial capsule, medial collateral ligament and semimembranosus can also be involved in PMRI. -
Clinical tip
In the test position, gravity acts on the tibia and causes it to drop back, potentially leading to a false positive test. Care should be taken to ensure that the tibia is in a neutral position prior to testing.
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Posteromedial drawer test
Although not used routinely, it is the test of choice when a diagnosis of PMRI is being considered.

- Posterolateral rotatory instability (PLRI) Posterolateral drawer test
-
Aka
Hughston’s posterolateral drawer sign -
Purpose
To assess for posterolateral rotatory instability (PLRI). -
Technique
Patient position
Lying supine with the hip flexed to 45° and the knee flexed to about 90°. The foot is positioned outwards so that the tibia is externally rotated to a maximum of 15° and stabilized on the couch.
Clinician position
The foot needs to be stabilized for this test which can be achieved by sitting on the dorsum of the forefoot. Both hands grasp around the upper tibia with thumbs placed anteriorly over the joint line in order to be able to detect posterior movement of the tibia.
Action
The tibia is pushed posteriorly noticing the degree of posterior excursion on the lateral side of the knee compared to the unaffected side.
Positive test
Essentially, in tests for PLRI, the clinician assesses for excessive posterior rotation of the lateral tibial condyle. In this test, increased posterior excursion or rotation of the lateral tibial condyle when compared to the contralateral knee indicates a tear of both the PCL and the lateral collateral ligament ( LaPrade & Terry 1997).
Clinical context
The terminology used in the literature regarding the anatomical structures involved in injuries at the posterolateral corner is inconsistent. Essentially, varus movement is controlled by the lateral ligament and capsule while external rotation of the femur is primarily controlled by the posterior cruciate ligament, arcuate–popliteus complex, lateral collateral ligament, biceps femoris tendon and the posterolateral capsule.
A high incidence of multiple ligament involvement and peroneal nerve trauma are associated with posterolateral injury and a variety of physical tests are recommended to provide a complete evaluation of stability including the external recurvatum test (see p. 211), varus test (see p. 186), posterolateral drawer test (see p. 205), the dial test (see p. 209) and the reverse pivot shift test (see p. 207) ( Hughston & Norwood 1980 , LaPrade & Wentorf 2002).
Although a positive posterolateral drawer test is said to be diagnostic of PLRI ( Baker et al 1983 ) there is an absence of rigorous studies to support this. Posterolateral corner injuries are comparatively rare and account for only 2% of all acute knee ligament injuries, most frequently occurring during high-energy/impact sporting activities ( Larsen & Toth 2005). -
Clinical tip
In the test position, gravity acts on the tibia and causes it to drop back, potentially leading to a false negative result. Care should
be taken to ensure that the tibia is in a neutral position prior to testing.
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Posterolateral drawer test
Although not used routinely, it is a useful test along with the dial test (see p. 209) where PLRI is a diagnostic possibility.

Reverse pivot shift test
-
Aka
Jakob test -
Purpose
To assess for posterolateral rotatory instability (PLRI). -
Technique
Patient position
The patient lies supine with the leg relaxed.
Clinician position
The caudal hand grasps the heel and places the forearm against the medial border of the foot in order to maintain external rotation of the tibia throughout the test while the cephalic hand supports the anterior and medial aspects of the knee. The hip is flexed to about 45°and the knee taken into about 80° flexion.
Action and positive test
The caudal hand maintains the external rotation of the tibia, at the same time applying a valgus stress to the knee ( Fig. 6.7A) . This position causes the lateral tibial plateau to sublux posteriorly in an unstable knee. The knee is then allowed to extend slowly and at around 20–30° of flexion, the iliotibial band then lies anterior to the axis of rotation, suddenly bringing the lateral tibial condyle back into a neutral position, indicating a positive test ( Fig. 6.7B). -
Clinical context
This tests posterolateral corner instability caused by injury to the lateral collateral ligament and the posterolateral stabilizers (see posterolateral drawer test, p. 205; Laprade & Terry 1997). Although
A
B




Fig. 6.7 ● Reverse pivot shift test. Start position of subluxation (A) and end position (B) of relocation in further knee extension.
comparatively rare, PLRI is considerably more disabling than medial instability as it involves injury to multiple structures and can be accompanied by anterolateral and anteromedial instability when the anterior cruciate ligament and medial capsular ligaments are also involved.
The reverse pivot shift test is considered to be a difficult test to perform and hard to reproduce consistently, even with an anaesthetized patient ( Larsen & Toth 2005 ) and this was verified in a study by Cooper (1991) in which the test was considered positive in 35% of normal knees examined under anaesthesia.
Many clinicians rely more on the drawer type tests (see posterolateral drawer test, p. 205) in the outpatient setting because they are more comfortable for the patient, easier to perform for the clinician and more likely to yield an accurate finding ( Anderson et al 2000 ). Given the complexity of PLRI, a variety of physical tests are recommended to provide a complete evaluation of the posterolateral stability of the knee including the external recurvatum test (p. 211), the varus test (see p. 186), the posterolateral drawer test (see p. 205) and the dial test (see p. 209) ( Bahk & Cosgarea 2006 ; LaPrade & Wentorf 2002).
There is little evidence on the accuracy of any of the tests for the lateral structures of the knee, possibly because lateral instability is much less frequently encountered. -
Clinical tip
The test can also be done with the patient standing, using a support for balance, with the weight equally distributed between both legs. The examiner places one hand above, and the other below the knee, applying a valgus stress; the patient initiates knee flexion while
weight-bearing. A positive test is indicated by the knee giving way or the tibia shifting posteriorly with a jerk (Magee 2008).
EXPERT OPINION
| COMMENTS
| ---|---|
★
| Reverse pivot shift test
Rarely used as other tests such as the dial test are easier to perform and more accurate.

Dial test
-
Aka
Tibial lateral rotation test -
Purpose
To assess for posterolateral rotatory instability (PLRI). -
Technique
Patient position
Lying supine with the thigh abducted so that the knee can flex over the side of the couch.
Clinician position
The thigh is stabilized with the cephalic hand while the other hand grasps the heel and uses the forearm to push the foot into dorsiflexion.
Action and positive test
Using the dorsiflexed foot as a lever, the knee is passively flexed to 30° and externally rotated. The extent of rotation is noted in comparison to the other knee ( Fig. 6.8A) but an excess of 10° is considered to be a positive test. The test is then repeated in 90° of flexion, still with the thigh comfortably supported on the couch. The clinician again assesses for excessive tibial rotation ( Fig. 6.8B) with increased external rotation in this position also incriminating the posterior cruciate ligament (PCL). -
Clinical context
The dial test assesses for posterolateral corner and PCL injury. As PLRI involves injury to multiple structures (see posterolateral
A
B




Fig. 6.8 ● In the dial test, the amount of tibial external rotation is compared in 30° (A) and 90° (B) knee flexion.
drawer test, p. 205) a variety of physical tests are recommended to provide a complete evaluation of the posterolateral stability of the knee ( Bahk & Cosgarea 2006 , LaPrade & Wentorf 2002).
There is little evidence on the accuracy of any of the tests for the lateral structures of the knee. These diagnostic tests require skilled handling and interpretation and, because of this, can be frequently misinterpreted ( Hughston et al 1976). -
Clinical tip
The foot and tibial tubercle provide useful visible markers to observe the extent of tibial rotation during this test.
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Dial test
The most helpful test in assessing for PLRI. -
Variations
Alternative positions have been described to perform the dial test. The patient’s leg and foot can remain on the couch and passive external rotation of the foot and tibia performed in a similar manner in first 30° and then 90° knee flexion. A second version starts with the patient in the prone position. The knee is flexed to 30° and the degree of tibial external rotation is noted. Maintaining the external rotation, the knee is flexed further to 90°.
In all cases, increased range of external rotation at 30° knee flexion indicates posterolateral corner injury. If increasing the knee flexion to 90° abolishes the external rotation discrepancy, the PCL can be assumed to be functioning; however, more pronounced discrepancy implicates both the posterolateral corner and the PCL.
With Loomer’s test/Bousquet external hypermobility test the patient lies supine with both hips and knees flexed to 90°. The clinician passively externally rotates both tibias to the end of range. Observation of excessive rotation and a posterior sag of the tibia on the femur indicate a positive test.

External rotation recurvatum test
-
Purpose
To detect the presence of posterolateral instability (PLRI). -
Technique
Patient position
Lying supine with the leg relaxed.
Clinician position
Standing at the end of the couch facing the patient, both big toes are grasped.
Action
The feet and legs are passively lifted from the couch using the big toes while observing the extension and rotation movement of the tibial tuberosity and lateral tibial condyle compared to the uninjured knee.
Positive test
As in all tests for PLRI, the clinician is looking for excessive posterior subluxation/rotation of the lateral tibial condyle. In this test, hyperextension and varus as well as increased external rotation of the tibia would be expected.

Fig. 6.9 ● External recurvatum test. -
Clinical context
In a study comparing physical assessment and surgical findings, a correlation was observed between a positive external rotation recurvatum test and injury to the lateral collateral ligament and the lateral head of gastrocnemius tendon ( LaPrade & Terry 1997 ). As PLRI can involve injury to multiple structures (see posterolateral drawer test, p. 205) a selection of physical tests are necessary to fully evaluate posterolateral stability ( LaPrade & Wentorf 2002).
In a small study, Baker et al (1983) suggested that a positive external rotation recurvatum test or posterolateral drawer test should be considered diagnostic of PLRI but there is limited evidence to support this, with reported sensitivity varying from 33% to 94% ( Larsen & Toth 2005). -
Clinical tip
Spasm or tension in the hamstrings during this test can mask PLRI, resulting in a false negative result.

● C MENISCAL TESTS
Apley’s test
-
Aka
Apley’s grinding test -
Purpose
To elicit pain and/or apprehension resulting from meniscal injury or pathology. -
Technique
Patient position
Prone lying with the knee positioned in 90° flexion. The couch needs to be low enough to allow the clinician’s knee to fix the lower thigh during the manoeuvre.
Clinician position
The clinician’s cephalic knee is positioned over the patient’s lower thigh and a firm but comfortable pressure is applied to maintain the thigh’s position against the couch during the test.
Action
This test involves rotation of the tibia with both distraction and compression.
Firstly, rotation with distraction is tested. Cupping the dorsum of the foot with the caudal hand and applying a firm hold around the ankle with the other, the knee is distracted by pulling longitudinally along the line of the tibia, using both hands to achieve this. Once the distraction is on, internal and external tibial rotation is applied with both hands ( Fig. 6.10A).
Rotation under compression is then applied. Both hands change position. The caudal hand fixes the forefoot in a plantigrade position while the other is placed over the heel in order to apply compression along the longitudinal axis of the tibia. Once the compression is added, internal and external tibial rotation is applied, using the foot as a lever ( Fig. 6.10B).
Positive test
Pain and/or apprehension elicited when rotation is applied under compression which reduces when the test is repeated with distraction. -
Clinical context
There are many meniscal tests recorded in the literature, most of which are variations on either Apley’s, McMurray’s (see p. 215) or the weight-bearing rotation test (see p. 218). Relying on Apley’s test in isolation has been found to be a poor predictor of meniscal pathology ( Malanga et al 2003 ) and the test is not sufficiently sensitive or specific to provide a definitive diagnosis, particularly when the injury is comparatively minor or accompanied by other pathology such as osteoarthritis. One study reported a greater sensitivity for the test in patients with a history suggesting a mensical tear ( Karachalios et al 2005), confirming work by other authors concluding that a combination of history and
A
B




Fig. 6.10 ● Apley’s test with distraction (A) and compression (B).
TABLE 6.5 APLEY’S TEST
Author and year
| LR +
| LR —
| Target condition
Karachalios et al 2005
| 5.86
★★
| 0.63
| Medial meniscus
Karachalios et al 2005
| 2.9
★
| 0.69
| Lateral meniscus
Fowler & Lubliner 1989
| 0.8
| 1.05
| Both menisci
Ryzewicz 2007
| 0.8–5.9
★★
| 0.6–1.1
| Both menisci
Malanga et al 2003
| 1.3
| 0.97
| Both menisci
examination findings provides an accurate predictor of patients likely to require arthroscopic surgery ( Solomon et al 2001). However, both the McMurray and weight-bearing rotation tests have been shown to be more accurate than Apley’s. -
Clinical tip
Unwanted stress to the ankle ligaments can be avoided by maintaining the foot in a plantigrade position during the manoeuvre.
The distraction element of this test should always be applied first in order to ascertain the response before the knee is tested under compression when provocation of both pain and apprehension are most likely.
In addition to testing the menisci, stress will also fall on the ligamentous structures and increased pain under traction is more likely to incriminate the ligaments which would then require further evaluation.
EXPERT OPINION
| COMMENTS
| ---|---|
★
| Apley’s test
The lack of sensitivity and the availability of other tests has resulted in a decline in its use.
McMurray’s test

Purpose
To elicit pain and/or apprehension resulting from meniscal injury or pathology.
Technique
Patient position
Lying supine.
Clinician position
The cephalic hand is placed above the patella and, using the index finger and thumb, the medial and lateral joint lines are palpated in order to detect clicking during the test. The patient’s heel is cupped with the caudal hand so that the forearm lies along the medial aspect of the foot enabling it to be used as a lever, so the tibia can be rotated externally.
Action
With the knee positioned in full flexion and external rotation, the leg is steadily extended to around 90°.
The test can then be repeated with the tibia held in internal rotation. The caudal hand is re-positioned so that the fingers cup the calcaneus medially with the thumb on the lateral aspect.
Positive test
Reproduction of the patient’s pain, click or apprehension.
A
B




Fig. 6.11 ● McMurray’s test carried out with internal rotation of the tibia. Start (A) and end (B) position.
Clinical context
The original test described by McMurray, before the advent of arthroscopy, suggested that the posterior segments of both menisci were the areas predominantly stressed by this test. External rotation of the tibia was thought to increase stress in the posteromedial compartment with internal rotation increasing loading posterolaterally (
McMurray
1942). There are several studies examining the accuracy of meniscal tests but their inclusion criteria vary, the presence of associated pathology is not always considered, and they differ in whether they consider pain, apprehension or a click to represent a positive test; this makes an overall judgement of their clinical usefulness difficult.
Across all studies, the sensitivity of the McMurray test is generally poor. A higher degree of sensitivity has been reported in populations of patients with a typical meniscal history (
Karachalios et al
2005
) and is lower where patients were selected based on a history of chronic knee pain or where no pre-test selection was attempted (
Fowler & Lubliner
1989
). However, a combination of a thorough history and examination has been found in several studies to be as accurate as MRI and on this basis, accurate clinical examination should provide sufficient grounds in most cases to determine the need for arthroscopy (
Fowler & Lubliner
1989
,
Jackson et al
2003
,
Miller
1996
,
Ryzewicz et al
2007
,
Solomon et al
2001
). A negative physical examination reduces the likelihood of a meniscal tear to less than 1.5% (
Jackson et al
2003). MRI was found to be less accurate
than examination in children, adolescents and patients with degenerative tibiofemoral changes (Dervin et al 2001
,
Ryzewicz et al
2007).
TABLE 6.6 McMURRAY’S TEST
Author and year
|
LR +
|
LR —
|
Target condition
Karachalios et al 2005
| 8
★★
| 0.55
| Medial meniscus
Boeree & Ackroyd 1991
| 2.3
★
| 0.8
| Medial meniscus
Karachalios et al 2005
| 4.6
★
| 0.41
★
| Lateral meniscus
Boeree & Ackroyd 1991
| 2.5
★
| 0.8
| Lateral meniscus
Evans et al 1993
| 8.0
★★
| 0.9
| Both menisci
Scholten et al 2001
| 8.0
★★
| 0.9
| Both menisci
Fowler & Lubliner 1989
| 7.8
★★
| 0.7
| Both menisci
Solomon et al 2001
| 1.3
| 0.8
| Both menisci
Ryzewicz et al 2007
| 2.2–9.3
★/★★
| 0.4–0.9
★
| Both menisci
Clinical tip
The conventional history of an acute locked knee following a weight-bearing, rotatory stress is often absent and in many patients with a meniscus lesion there may be no significant history of trauma, swelling or locking.
Diagnosing meniscal lesions in the presence of other knee pathology is more difficult, particularly if there is anterior cruciate ligament (ACL) involvement or underlying degenerative changes. If the ACL is normal, the combination of a block to full knee extension, a
positive McMurray test and pain on full flexion is highly suggestive of meniscal injury (
Fowler & Lubliner
1989
). Interestingly, joint line tenderness is also considered to be very sensitive in meniscal lesions and palpation is therefore a good accompaniment to the highly specific McMurray test (
Jackson et al
2003
,
Karachalios et al
2005
,
Ryzewicz et al
2007
,
Solomon et al
2001).
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
|
McMurray’s test
Frequently used but false negatives and positives are not uncommon. A history of localized sharp pain and giving way, together with joint line tenderness, helps to point towards a meniscal diagnosis.
Variations
*
A modification of the McMurray test is now widely used where a valgus or varus stress is added to the rotation component (
Atkins et al
2010). This enhancement is thought to further challenge the integrity of the menisci and potentially improve the test’s sensitivity but this variation has not been tested so these conclusions are speculative.

Weight-bearing/rotation meniscal test
-
Aka
Disco test Merke’s test Thessaly test -
Purpose
To elicit pain and/or apprehension resulting from injury or pathology to the medial and lateral menisci. -
Technique
Patient position
Standing.
Clinician position
The clinician allows the patient to hold lightly onto their hands for support.
Action
Standing on the affected leg, the patient flexes the weight-bearing knee to approximately 20°, then rotates the femur with the body-weight over the fixed foot and tibia. Rotation into internal and external rotation is repeated several times.
Positive test
Pain, locking or apprehension on testing are considered positive findings.
A
B




Fig. 6.12 ● (A, B) Weight-bearing rotation test performed on the left leg. -
Clinical context
This test aims to reproduce the likely mechanism of meniscal injury, but the forces exerted on the flexed knee may also expose ligamentous instability, so it is necessary for the clinician to assimilate all findings from the history and examination before suspicion falls on the menisci alone.
TABLE 6.7 WEIGHT-BEARING/ROTATION MENISCAL TEST
Author and year
| LR +
| LR —
| Condition
Karachalios et al 2005
| 29.7
★★★
| 0.11
★★
| Medial meniscus
Karachalios et al 2005
| 23
★★★
| 0.08
★★★
| Lateral meniscus
In a study carried out by the test originators, the sensitivity and specificity of joint line tenderness, McMurray’s, Apley’s and the weight-bearing rotation test were measured, prior to MRI and arthroscopy, on a population of young subjects with an absence of other knee pathology but a history suggestive of meniscal injury. The weight-bearing rotation test performed better than both the McMurray and Apley tests ( Karachalios et al 2005 ) and in a review of evidence around examination techniques at the knee, its accuracy was comparable to MRI in diagnosing meniscal lesions ( Ryzewicz et al 2007). -
Clinical tip
In the active, middle aged patient, the degenerative menisci may be responsible for symptoms that present without a dramatic history or presentation and, acutely, can be difficult to differentiate from degenerative arthritis.
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Weight-bearing/rotation meniscal test
Used inconsistently probably because it is a comparatively recent addition but it is a good functional test which replicates the likely mechanism of injury. -
**Variations
** -
**
Childress’s test
aims to isolate a lesion of the posterior horn of the meniscus. The patient squats and attempts to walk a few steps in this position, performing a ‘duck waddle’; a positive test is indicated by pain, apprehension or locking (
Magee
2008).
** -
Ege’s test
is a variation of the McMurray’s test in a weight-bearing position and involves squatting and rising with the knees first in an externally rotated position and then internally rotated; again, a positive test is indicated by pain, apprehension or locking (
Akseki et al
2004).

● D PATELLOFEMORAL TESTS
McConnell test
-
Purpose
To detect pain emanating from the patellofemoral articulation. -
Technique
Patient position
The patient sits on the edge of a raised couch, with the femur externally rotated and the knee flexed over the side.
Clinician position
Sitting on a low stool, resistance to isometric extension is given by one hand which is positioned over the front of the shin while the other hand stabilizes the thigh.
Action
The patient holds an isometric contraction of the quadriceps for several seconds in varying degrees of flexion (120°, 90°, 60°, 30° and 0°) ( Fig. 6.13A ). If pain is reproduced in any of these positions the test is repeated while the clinician passively maintains a medial glide to the patella ( Fig. 6.13B).
Positive test
Patellofemoral pain is indicated if pain is reproduced on isometric quadriceps contraction and lessened when the medial glide is applied in any of the positions tested. -
Clinical context
The McConnell test reproduces the concentric activity of the quadriceps through range with the vastus medialis obliquus functioning particularly in the final degrees of extension to stabilize the patella ( Bulstrode et al 2002).
In maximum flexion, the medial patellar facet is completely unloaded with the lateral and middle facets taking all the compressive force and the superior aspect of the patella providing the contact area. As the knee moves towards extension, the contact area of the patella moves inferiorly and the medial aspect starts to share some of the load (estimated to be around 40%) ( Bulstrode et al 2002). An understanding of the forces acting through various parts of the articular surfaces of the patellofemoral joint (PFJ) may theoretically help the clinician to isolate the facet responsible for the symptoms during the test.
A
B




Fig. 6.13 ● Resisted knee extension (A), repeated with a medial glide applied to the lateral aspect of the patella (B).
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| McConnell test
Useful to guide treatment for patellofemoral symptoms and anterior knee pain. -
Clinical tip
Because the patella is less mobile in positions of knee flexion, it can be helpful to return the knee to full extension before applying the medial glide and then maintain this as much as possible as the knee is taken back into the test position. -
Variations
The active patella grind test has the patient extending the knee from 90° of flexion while the patella is palpated for crepitus and the onset of pain noted.
The patellofemoral joint can also be tested using squat or step tests . The patient is asked to step up or down from a step. In a small
study looking at the diagnosis of patellofemoral pain syndrome, the step-down (eccentric) phase was found to be a more accurate predictor than Waldron’s test , a similar active test where the patient squats while standing ( Nijs et al 2006 ) (Tables 6.8, 6.9).
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Step test
Used frequently as it is a functional test and replicates what is usually the most painful activity for the patient.
TABLE 6.8 STEP DOWN TEST
Author and year
| LR +
| LR —
| Condition
Nijs et al 2006
| 2.34
★
| 0.71
| Patellofemoral pain syndrome
TABLE 6.9 WALDRON’S TEST
Author and year
| LR +
| LR —
| Condition
Nijs et al 2006
| 1.05
| 0.99
| Patellofemoral pain syndrome
A positive vastus medialis coordination test was found to indicate a small but significant increase in the probability of patellofemoral pain syndrome ( Nijs et al 2006). The patient lies with the knee flexed over the clinician’s clenched fist and is asked to extend the knee while maintaining uniform pressure on the clinician’s hand. A positive test is indicated by an uncoordinated contraction of the hip flexors/extensors, indicated by the patient pushing down or lifting away from the clinician’s fist.

Patella apprehension test
-
Aka
Fairbank’s apprehension test -
Purpose
To detect instability/pain emanating from the patellofemoral articulation. -
Technique
Patient position
Patient lying supine with the knee flexed to 30°.
Clinician position
Sitting on the edge of the couch with the patient’s knee flexed over the clinician’s thigh. Both thumbs are placed over the medial patella border.
Action
The patella is pushed laterally in a slow, controlled manner.
Positive test
The patient experiences pain and/or apprehension in anticipation of patella subluxation and usually attempts to contract the quadriceps to try to prevent further excursion.

Fig. 6.14 ● Patella apprehension test. -
Clinical context
Recurrent patella dislocation occurs most commonly among teenagers, who report symptoms of giving way, pseudolocking and pain. In addition to provocation testing, assessment of local and regional
TABLE 6.10 PATELLA APPREHENSION TEST
Author and year
| LR +
| LR —
| Target condition
Magee 2008
| 2.26
★
| 0.79
| Patella instability
strength and stability, generalized ligament laxity, femoral antever-sion, external tibial torsion, valgus deformity, patella alta and trochlear dysplasia may be required to determine any underlying predisposition to instability ( Bulstrode et al 2002).
If the patient is very apprehensive, they may actively contract the quadriceps to prevent lateral excursion of the patella hindering a satisfactory test, and in this situation, assessment under anaesthesia has been advocated ( Bulstrode et al 2002 ). The test has been evaluated under anaesthetic as part of a study examining the clinical and arthroscopic findings associated with patella dislocation ( Sallay et al 1996). Only 39% of patients had a positive patella apprehension test in contrast to 83% exhibiting a moderate to large effusion and 70% with tenderness over the tissues on the posteromedial aspect of the knee. Arthroscopic findings of gross laxity of the patellofemoral joint were most notable when the test was performed in 70–80° of knee flexion and this would suggest that the sensitivity of the test may be improved if carried out in a greater degree of flexion ( Malanga et al 2003). -
Clinical tip
In a study evaluating diagnostic tests for patellofemoral pain (not instability), a positive patella apprehension test was reported to increase the probability of patellofemoral joint syndrome to a small but significant degree ( Nijs et al 2006).
Patellofemoral grind test
-
Purpose
To elicit pain and/or apprehension emanating from the patellofemoral joint. -
Technique
Patient position
Lying supine with the knee extended.
Clinician position
Using a pinch grip of the index finger and thumb of both hands, the superior and inferior poles of the patella are fixed.
Action
The patella is gradually compressed against the femur and moved inferiorly and superiorly, sliding the posterior surface of the patella against the femoral condyles.
Positive test
Reproduction of the patient’s anterior knee pain.

Fig. 6.15 ●
Patellofemoral grind test. -
Clinical context
This test was originally used as a diagnostic test for chondromalacia patellae but subsequent studies have found little correlation between physical examination and arthroscopic findings of articular cartilage damage ( Malanga et al 2003 ). It now has a wider application and is used, along with a number of others (see variations below), to assess symptoms stemming from the patellofemoral joint. Although there are no studies on this test in isolation, a poor correlation was noted when the clinical history and physical/X-ray findings were compared to subsequent arthroscopic findings in a small group of subjects with traumatic knee disorders. These combined examination findings yielded a sensitivity of only 37% for patients with chondromalacia patellae ( O’Shea et al 1996). -
Clinical tip
It is necessary to gauge carefully the amount of downward pressure that is applied during this test, as, if sufficient force is applied, it is possible to elicit pain in the healthiest of knees. Pressure should be
added gradually and comparison with the opposite side is always valuable to detect differences.
It is also important to monitor the patient’s response to all these tests carefully as apprehension, with or without pain, is also considered to represent a positive finding.
EXPERT OPINION
| COMMENTS
| ---|---|
★★★
| Patellofemoral grind test
Commonly used for assessment of patellofemoral problems. -
**Variations
** -
Clarke’s test is performed with the patient lying with the knee extended and relaxed. The web of the clinician’s hand is placed over the superior pole of the patella. The patient then contracts their quadriceps, forcing the patella upwards into the clinician’s hand. As a slight variation, Zohler’s test requires the clinician to use a pincer grip to pull the patella inferiorly to provide resistance to the superior excursion of the patella during contraction. These tests are often found to be painful in otherwise asymptomatic subjects and their usefulness is therefore limited. The patella grind test can be repeated in various degrees of knee flexion (Frund’s sign
) to assess the integrity of different parts of the articular surface of the patella (
Magee
2008).

● E OTHER TESTS
Noble’s compression test
-
Purpose
To detect the presence of iliotibial friction syndrome. -
Technique
Patient position
Lying supine.
Clinician position
Standing on the side to be tested, the hip and knee are passively flexed to 90°.
Action
Using the cephalic thumb, pressure is applied over the lateral femoral condyle or slightly proximal to it (approximately 2–3 cm above the lateral knee joint line) and maintained while the knee is passively extended.
Positive test
The patient’s lateral knee pain is reproduced when the knee reaches around 30° off full extension with tenderness under the pressure of the clinician’s thumb. It may also be accompanied by crepitus.

Fig. 6.16 ● Noble’s compression test. -
Clinical context
The Noble compression test aims to replicate the movement of the ITB over the femoral condyle which occurs during locomotion. As the knee moves from flexion into the last 30° of extension, the ITB moves forward over the lateral femoral condyle and if this movement is repeated excessively, particularly in the presence of predisposing factors such as ITB tightness, genu varum, overpronation and leg length discrepancy (symptoms tend to occur in the longer leg), the distal extent of the ITB and its underlying bursa can become inflamed ( MacAuley 2007 , Narvani et al 2006). Rapid increases in distance, hill
running or sudden changes to training schedules can precipitate the problem. Ober’s test may also be positive (see p. 171). -
Clinical tip
Given the iliotibial band is both a dynamic lateral stabilizer of the knee and contributes to active isotonic extension and flexion, some clinicians prefer to get the patient to actively extend the knee from about 40° as this is thought to put maximum stress on the band as it crosses over the condyle.
EXPERT OPINION
| COMMENTS
| ---|---|
★★
| Noble’s compression test
This is a useful test particularly in the differential diagnosis of lateral knee pain in athletes.

Mediopatellar plica test
-
Aka
Mital–Hayden test -
Purpose
To identify pain emanating from the medial patellar plica. -
Technique
Patient position
Lying supine.
Clinician position
Standing on the side of the affected leg, the patient’s knee is flexed to about 30° and supported over the clinician’s knee. Both thumbs are placed over the lateral border of the patella.
Action
Firm pressure is applied with both thumbs to the patella, attempting to glide it medially.
Positive test
Reproduction of the pain is suggestive of an inflamed medial patellar plica.

Fig. 6.17 ● Mediopatella plica test. -
Clinical context
Plicae are folds of synovial tissue which are embryological in origin but which often persist into adult life, although they remain asymptomatic in most people. They are usually found around the margins of the patella – medially, superiorly and inferiorly ( Hardaker et al 1980 ). The medial patellar plica has been estimated to be present in 19–70% of the population. It consists of approximately five folds lying between the medial border of the patella and the medial femoral condyle and is the most problematic ( Abrahams & Kern 2001 ), causing impingement, usually between 40° and 80° of knee flexion. The suprapatellar plica lies in the suprapatellar pouch and the inferior plica, which despite being the largest is considered to be the least troublesome, lies anterior to the intercondylar notch inserting into the infrapatellar fat pad ( Abrahams & Kern 2001).
There is no evidence on the accuracy of physical tests or other assessment methods for plica pathology although there is agreement that it can mimic classic meniscal symptoms, making the diagnosis difficult ( Abrahams & Kern 2001 , Saengnipanthkul et al 1992 , Tindel & Nisonson 1992).
EXPERT OPINION
| COMMENTS
| ---|---|
★
| Mediopatellar plica test
Plicae tests have the tendency to produce inaccuracies and the symptoms can be difficult to distinguish from medial meniscal pathology, so MRI is sometimes necessary to confirm plica involvement. -
Clinical tip
It is necessary to apply the glide medially as this squeezes the most commonly involved medial plica between the undersurface of the patella and the medial femoral condyle. The test can be reversed if the symptoms emanate from the lateral aspect. Other tests such as McMurray’s (p. 215) and the patella apprehension tests (p. 224) may also be positive in the presence of a symptomatic medial plica ( Abrahams & Kern 2001 , Saengnipanthkul et al 1992) potentially leading to a false positive result.
In the symptomatic patient, tenderness and thickening may be found approximately 1 cm medial to the border of the patella over the medial femoral condyle -
**Variations
** -
Hughston’s plica test
is performed with the patient lying supine, the knee is taken to 30° and the tibia internally rotated by the caudal hand. A medial glide is applied to the patella using the heel of the cephalic hand while the fingers palpate the medial border of the patella to feel for crepitus or a ‘popping’ sensation as the knee is passively moved between extension and flexion. This may or may not be accompanied by pain (
Magee
2008).
The plica stutter test has the patient sitting with both knees flexed over the side of the couch. The margins of the patella on the affected knee are palpated to detect any sudden jump or ‘stutter’ as the knee is actively extended from a flexed position. This usually occurs in the mid-range ( Magee 2008).
To test the suprapatellar plica , the patient lies supine and the knee is passively flexed with the tibia internally rotated. The patella is palpated on the medial aspect for a ‘pop’ which may indicate a symptomatic suprapatellar plica ( Abrahams & Kern 2001).

Scientific References
-
Abrahams, S., Kern, J.H., 2001. Anterior knee pain: plica syndrome, the forgotten pathology? Physiotherapy 87 (10), 523–528.
Akseki, D., Ozcan, O., Boya, H., et al., 2004. A new weight bearing test and a comparison with McMurray’s test and joint line tenderness. Arthroscopy 20 (9), 951–958.
Anderson, A.F., Rennirt, G.W., Standeffer, W.C., 2000. Clinical analysis of the pivot shift tests: description of the pivot drawer test. Am. J. Knee Surg. 13 (1), 19–23.
Bahk, M.S., Cosgarea, A.J., 2006. Physical examination and imaging of the lateral collateral ligament and posterolateral corner of the knee. Sports Med. Arthrosc. 14 (1), 12–19.
Baker, C.L., Norwood, L.A., Hughston, J.C., 1983. Acute posterolateral rotatory instability of the knee. J. Bone Joint Surg. Am. 65 (5), 614–618.
Benjaminse, A., Gokeler, A., Van der Schans, C.P., 2006. Clinical diagnosis of an anterior cruciate ligament rupture: a meta-analysis. J. Orthop. Sports. Phys. Ther. 36 (5), 267–288.
Boeree, N.R., Ackroyd, C.E., 1991. Assessment of the menisci and cruciate ligaments: an audit of clinical practice. Injury 22, 291–294.
Bulstrode, C., Buckwalter, J., Carr, A., et al., 2002. Oxford Textbook of Orthopaedics and Trauma. Oxford University Press, Oxford.
Cooper, D.E., 1991. Tests for posterolateral instability of the knee in normal subjects: results of examination under anesthesia. J. Bone Joint Surg. Am. 73 (1), 30–36.
Dervin, G.F., Stiell, A.G., Wells, G.A., 2001. Physicians’ accuracy and interrater reliability for the diagnosis of unstable meniscal tears in patients having osteoarthritis of the knee. Can. J. Surg. 44 (4), 267–274.
Donaldson, W.F., Warren, R.F., Wickiewicz, T., 1985. A comparison of acute anterior cruciate ligament examinations: initial versus examination under anesthesia. Am. J. Sports Med. 13 (1), 5–10.
Evans, P.J., Bell, G.D., Frank, C., 1993. Prospective evaluation of the McMurray test. Am. J. Sports Med. 21 (4), 604–608.
Fowler, P.J., Lubliner, J.A., 1989. The predictive value of five clinical signs in the evaluation of meniscal pathology. Arthroscopy 5 (3), 184–186.
Frobell, R.B., Lohmander, L.S., Roos, H.P., 2007. Acute rotational trauma to the knee: poor agreement between clinical assessment and magnetic resonance imaging findings. Scand. J. Med. Sci. Sports 17 (2), 109–114.
Hardaker, W.T., Whipple, T., Bassett, F., 1980. Diagnosis and treatment of plica syndrome of the knee. J. Bone Joint Surg. Am. 66, 221–226.
Hewett, T.E., Noyes, F.R., Lee, M.D., 1997. Diagnosis of complete and partial cruciate ligament ruptures: stress radiography compared with KT-1000 arthrom-eter and posterior drawer testing. Am. J. Sports Med. 25 (5), 648–655.
Hughston, J.C., Norwood, L.A., 1980. The posterolateral drawer test and external rotational recurvatum test for posterolateral rotatory instability of the knee. Clin. Orthop. Relat. Res. 147, 82–87.
Hughston, J.C., Andrews, J.R., Cross, M.J., et al., 1976. Classification of knee ligament instabilities. Part II: the lateral compartment. J. Bone Joint Surg. Am. 58 (2), 173–179.
Jackson, J.L., O’Malley, P.G., Kroenke, K., 2003. Evaluation of acute knee pain in primary care. Ann. Intern. Med. 139, 575–588.
Karachalios, T., Hantes, M., Zibis, A.H., et al., 2005. Diagnostic accuracy of a new clinical test (the Thessaly test) for early detection of meniscal tears. J. Bone Joint Surg. 87 (5), 955–962.
Katz, J.W., Fingeroth, R.J., 1986. The diagnostic accuracy of ruptures of the anterior cruciate ligament comparing the Lachman test, the anterior drawer sign,
and the pivot shift test in acute and chronic knee injuries. Am. J. Sports Med. 14 (1), 88–91.
Kesson, M., Atkins, E., 2005. Orthopaedic Medicine: a Practical Approach, second edn. Butterworth Heinemann, Edinburgh.
Kim, S.J., Kim, H.K., 1995. Reliability of the anterior drawer test, the pivot shift test, and the Lachman test. Clin. Orthop. Relat. Res. 317, 237–242.
Kocabey, Y., Tetik, O., Isbell, W., et al., 2004. The value of clinical examination versus magnetic resonance imaging in the diagnosis of meniscal tears and anterior cruciate ligament rupture. Arthroscopy 20 (7), 696–700.
LaPrade, R.F., Terry, G.C., 1997. Injuries to the posterolateral aspect of the knee: association of anatomic injury patterns with clinical instability. Am. J. Sports Med. 25 (4), 433–438.
LaPrade, R.F., Wentorf, F., 2002. Diagnosis and treatment of posterolateral knee injuries. Clin. Orthop. Relat. Res. 402, 110–121.
Larsen, M.W., Toth, A., 2005. Examination of posterolateral corner injuries.
J. Knee Surg. 18 (2), 146–150.
Lee, J.K., Yao, L., Phelps, C.T., et al., 1988. Anterior cruciate ligament tears: MR imaging compared with arthroscopy and clinical tests. Radiology 166 (3), 861–864.
Lerat, J.L., Moyen, B.L., Cladiere, F., et al., 2000. Knee instability after injury to the anterior cruciate ligament: quantification of the Lachman test. J. Bone Joint Surg. Am. 82 (1), 42–47.
Liu, S.H., Osti, L., Henry, M., et al., 1995. The diagnosis of acute complete tears of the anterior cruciate ligament. J. Bone Joint Surg. Am. 77B, 586–588.
MacAuley, D., 2007. Oxford Handbook of Sport and Exercise Medicine. Oxford University Press, Oxford.
McMurray, T.P., 1942. The semilunar cartilages. Br. J. Surg. 29, 407–414.
Magee, D.J., 2008. Orthopaedic Physical Assessment, fifth edn. Saunders, Philadelphia.
Malanga, G.A., Andrus, S., Nadler, S.F., et al., 2003. Physical examination of the knee: a review of the original test description and scientific validity of common orthopaedic tests. Arch. Phys. Med. Rehabil. 84 (4), 592–603.
Miller, G.K., 1996. A prospective study comparing the accuracy of the clinical diagnosis of meniscus tear with magnetic resonance imaging and its effect on clinical outcome. Arthroscopy 12 (4), 406–413.
Narvani, A.A., Thomas, P., Lynn, B., 2006. Key Topics in Sports Medicine.
Routledge, London.
Nijs, J., Van Geel, C., Van der Auwera, C., et al., 2006. Diagnostic value of five clinical tests in patellofemoral pain syndrome. Man. Ther. 11, 69–77.
O’Shea, K.J., Murphy, K.P., Heekin, R.D., et al., 1996. The diagnostic accuracy of history, physical examination, and radiographs in the evaluation of traumatic knee disorders. Am. J. Sports Med. 24, 164–167.
Ostrowski, J.A., 2006. Accuracy of 3 diagnostic tests for anterior cruciate ligament tears. J. Athl. Train. 41 (1), 120–121.
Rose, N.E., Gold, S.M., 1996. A comparison of accuracy between clinical examination and magnetic resonance imaging in the diagnosis of meniscal and anterior cruciate ligament tears. Arthroscopy 12 (4), 398–405.
Rubenstein, R.A., Shelbourne, K.D., McCarroll, J.R., et al., 1994. The accuracy of the clinical examination in the setting of posterior cruciate injuries. Am. J. Sports. Med. 22 (4), 550–557.
Ryzewicz, M., Peterson, B., Siparsky, P.N., et al., 2007. The diagnosis of meniscus tears: the role of MRI and clinical examination. Clin. Orthop. Relat. Res. 455, 123–133.
Saengnipanthkul, S., Sirichativapee, W., Kowsuwon, W., et al., 1992. The effects of medial patellar plica on clinical diagnosis of medial meniscal lesion. J. Med. Assoc. Thai. 75 (12), 704–708.
Sallay, P.I., Poggi, J., Speer, K.P., et al., 1996. Acute dislocation of the patella: a cor-relative pathoanatomic study. Am. J. Sports Med. 24 (1), 52–60.
Scholten, R.J., Deville, W.L., Opstelten, W., 2001. The accuracy of physical diagnostic tests for assessing meniscal lesions of the knee. J. Fam. Pract. 50 (11), 938–942.
Scholten, R.J., Opstelten, W., Van der Plas, C.G., et al., 2003. Accuracy of physical diagnostic tests for assessing ruptures of the anterior cruciate ligament: a meta-analysis. J. Fam. Pract. 52 (9), 689–694.
Slocum, D.B., Larson, R.L., 1968. Rotatory instability of the knee. J. Bone Joint Surg. Am. 50, 211–225.
Solomon, D.H., Simel, D.L., Bates, D.W., et al., 2001. The rational clinical examination. Does this patient have a torn meniscus or ligament of the knee? Value of the physical examination. J. Am. Med. Assoc. 286 (13), 1610–1620.
Tindel, N., Nisonson, B., 1992. The plica syndrome. Orthop. Clin. North. Am. 23 (4), 613–618.
Torg, J.S., Conrad, W., Kalen, V., 1976. Clinical diagnosis of anterior cruciate ligament instability in the athlete. Am. J. Sports Med. 4 (2), 84–93.
Yoon, Y.S., Rah, J.H., Park, H.J., 1997. A prospective study of the accuracy of clinical examination evaluated by arthroscopy of the knee. Int. Orthop. 21 (4), 223–227.
You Might Also Like