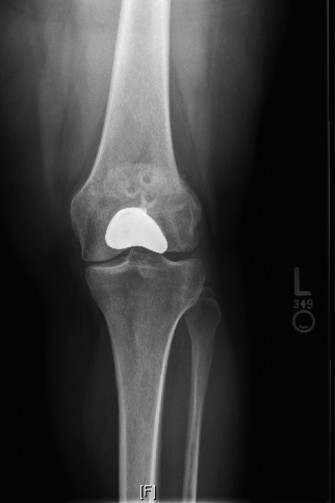
Patellofemoral Arthroplasty (PFA): Advanced Concepts, Indications & Patient Selection
Key Takeaway
Patellofemoral arthroplasty (PFA) is a targeted surgical intervention for debilitating, end-stage isolated patellofemoral osteoarthritis (PFOA), preserving healthy tibiofemoral compartments. It aims to alleviate anterior knee pain by resurfacing only the diseased joint. Key considerations include detailed surgical anatomy, biomechanics, and stringent patient selection, focusing on isolated PFOA unresponsive to non-operative treatment.
Introduction & Epidemiology
Patellofemoral arthroplasty (PFA) has evolved as a targeted surgical intervention for debilitating, end-stage isolated patellofemoral osteoarthritis (PFOA). Historically, PFOA was often managed non-operatively with activity modification, physiotherapy, non-steroidal anti-inflammatory drugs (NSAIDs), and intra-articular injections, or, in severe cases, by total knee arthroplasty (TKA), which sacrifices healthy tibiofemoral compartments. PFA offers a joint-preserving alternative, aiming to alleviate anterior knee pain by resurfacing only the diseased patellofemoral joint, thereby preserving tibiofemoral kinematics and proprioception.
Epidemiologically, PFOA is a distinct entity, often presenting earlier than tibiofemoral OA. It is estimated to affect a significant portion of the adult population, contributing to approximately 10-20% of knee osteoarthritis cases. While it can occur in isolation, it frequently coexists with mild tibiofemoral changes, making patient selection a critical determinant of surgical success. PFOA is more prevalent in females and can be associated with anatomical factors such as patella alta, trochlear dysplasia, and patellar maltracking. The primary goal of PFA is to restore a pain-free, functional patellofemoral articulation, thereby improving quality of life and potentially delaying or avoiding TKA in appropriately selected patients.
Surgical Anatomy & Biomechanics
A profound understanding of the surgical anatomy and biomechanics of the patellofemoral joint is paramount for successful PFA.
Surgical Anatomy
The patellofemoral joint comprises the patella, the largest sesamoid bone, articulating with the trochlear groove of the distal femur.
*
Patella:
Features a thick cartilage layer and multiple facets (medial, lateral, odd facet). Its thickness is a critical measurement for component selection, aiming to restore pre-disease thickness. Patellar height (e.g., Insall-Salvati ratio, Caton-Deschamps index) influences tracking and contact forces.
*
Femoral Trochlea:
The anatomical sulcus of the trochlea guides patellar tracking. Its morphology is crucial; trochlear dysplasia (e.g., Dejour classification types A-D) can predispose to maltracking and PFOA. The sulcus angle and trochlear depth are key parameters. The distal femoral condyles contribute to rotational alignment and determine the mediolateral position of the femoral component.
*
Extensor Mechanism:
Consists of the quadriceps muscle, quadriceps tendon, patella, patellar ligament (tendon), and tibial tuberosity. The vastus medialis obliquus (VMO) plays a critical role in medial stabilization of the patella.
*
Retinacula:
The medial patellofemoral ligament (MPFL) is a primary static stabilizer against lateral patellar translation. The lateral retinaculum provides lateral stability. Imbalance between these structures can lead to tracking abnormalities.
*
Nerve Supply:
The knee joint is innervated by branches from the femoral, obturator, and sciatic nerves. Specific attention to the infrapatellar branch of the saphenous nerve during medial approaches is necessary to prevent neuromas.

Biomechanics
The patellofemoral joint functions as a fulcrum, increasing the effective lever arm of the quadriceps muscle.
*
Contact Area and Forces:
Patellofemoral joint reaction forces increase significantly with knee flexion, particularly during activities like stair climbing and squatting. The contact area also shifts from the inferior patella in extension to the superior patella in deep flexion. PFOA disrupts this load distribution, leading to concentrated stress and pain.
*
Patellar Tracking:
The patella normally tracks within the trochlear groove throughout the range of motion. Maltracking, often lateral, results from a combination of bony morphology (e.g., shallow trochlea, valgus alignment) and soft tissue imbalance (e.g., tight lateral retinaculum, VMO insufficiency). This can lead to increased shear forces and accelerated cartilage wear.
*
Lower Extremity Alignment:
The Q-angle (quadriceps angle), representing the angle between the rectus femoris vector and the patellar ligament vector, provides an indirect measure of lateral pull on the patella. An increased Q-angle can contribute to lateral patellar maltracking. Tibial tubercle-trochlear groove (TT-TG) distance assesses bony alignment related to patellar tracking.
*
Rotational Stability:
Femoral and tibial torsion, as well as the rotation of the components, significantly influence patellar kinematics and must be considered during planning and execution.
Indications & Contraindications
Careful patient selection is paramount for optimizing outcomes in PFA.
Indications
The primary indication for PFA is isolated, symptomatic patellofemoral osteoarthritis refractory to comprehensive non-operative management.
-
Clinical:
- Persistent anterior knee pain localized to the patellofemoral joint, exacerbated by activities involving knee flexion (e.g., stair climbing, squatting, prolonged sitting).
- Pain unrelieved by activity modification, analgesics, physiotherapy, and intra-articular injections.
- Localized patellofemoral crepitus and tenderness.
- Absence of significant tibiofemoral pain or symptoms.
- Age: While there is no strict age limit, patients are typically younger than TKA candidates, often in their 40s-60s. However, isolated PFOA can affect older patients as well.
-
Radiographic:
- Radiographic evidence of severe chondral wear (Grade III/IV) confined predominantly to the patellofemoral compartment, with minimal to no degenerative changes in the tibiofemoral compartments on weight-bearing AP, lateral, and Rosenberg views.
- Merchant or sunrise views demonstrating significant patellofemoral joint space narrowing, subchondral sclerosis, osteophytes, and/or cyst formation.
- MRI may confirm isolated cartilage loss, bone edema patterns, and rule out meniscal or ligamentous pathology.
- CT scan may be valuable for assessing trochlear dysplasia, TT-TG distance, and rotational alignment abnormalities.
-
Intra-operative (Arthroscopy/Open Inspection):
- Confirmation of isolated full-thickness chondral loss within the patellofemoral joint.
- Healthy articular cartilage in the medial and lateral tibiofemoral compartments.
- Stable collateral and cruciate ligaments.
- Correctable patellar maltracking; severe uncorrectable maltracking may require concomitant procedures.
Contraindications
-
Absolute:
- Significant tibiofemoral osteoarthritis (Grade II or higher on Kellgren-Lawrence scale in either tibiofemoral compartment).
- Inflammatory arthropathy (e.g., rheumatoid arthritis).
- Active knee infection.
- Extensor mechanism insufficiency or rupture.
- Morbid obesity (BMI > 40 kg/m²), as it increases stress on the implant and risks of complications.
- Severe patellar instability or uncorrectable maltracking.
- Patella baja or alta that significantly compromises implant kinematics.
- Pre-existing generalized ligamentous laxity or instability requiring concomitant complex reconstruction.
-
Relative:
- Significant osteopenia.
- Previous complex knee surgery that has altered local anatomy.
- Patient unwillingness to comply with post-operative rehabilitation protocols.
- Certain occupations requiring heavy lifting or repetitive high-impact activities.
Operative vs. Non-Operative Indications
| Indication Type | Operative (PFA) | Non-Operative |
|---|---|---|
| Pain Severity | Persistent, severe anterior knee pain | Mild to moderate intermittent pain |
| Activity Limitation | Significant limitation of daily activities, work, and leisure due to pain | Manageable limitations, able to modify activities |
| Duration of Symptoms | Chronic, refractory symptoms (>6 months) | Acute or subacute symptoms, or chronic but responsive to conservative measures |
| Response to Conserv. | Failed comprehensive non-operative management (PT, injections, NSAIDs, braces) | Responsive to non-operative interventions |
| Radiographic OA | Isolated Kellgren-Lawrence Grade III/IV PFOA | Kellgren-Lawrence Grade I/II PFOA, or mild/no OA |
| Tibiofemoral Status | Healthy, asymptomatic tibiofemoral compartments | Healthy, asymptomatic tibiofemoral compartments |
| Patellar Tracking | Normal or correctable mild maltracking | Mild maltracking, responsive to VMO strengthening and taping |
| Patient Expectation | Realistic expectations regarding pain relief and functional improvement | May not be prepared for surgery or potential limitations |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for a successful PFA.
Pre-Operative Planning
-
Clinical Assessment:
- History: Detailed history of anterior knee pain, onset, duration, exacerbating/alleviating factors, previous treatments, and functional limitations. Assess for symptoms of tibiofemoral OA or ligamentous instability.
-
Physical Examination:
- Gait analysis: Observe for antalgic gait or limb malalignment.
- Inspection: Assess for swelling, atrophy of quadriceps (especially VMO).
- Palpation: Localize tenderness over patellofemoral facets, patellar tendon, quadriceps tendon.
- Range of Motion: Assess active and passive flexion and extension. Note any crepitus.
- Patellar Mobility: Assess for patellar tracking (J-sign), patellar tilt, and apprehension sign.
- Stability: Evaluate collateral and cruciate ligament integrity.
- Alignment: Clinical Q-angle assessment, femoral anteversion, tibial torsion.
- Neurovascular status: Peripheral pulses and sensation.
-
Radiographic Assessment:
- Standard Views: Weight-bearing AP, true lateral (30 degrees flexion), Merchant/sunrise view (30-45 degrees flexion), and Rosenberg view (45 degrees weight-bearing posteroanterior) are mandatory. These assess joint space narrowing, osteophytes, subchondral sclerosis, and patellar height (Insall-Salvati, Caton-Deschamps).
-
Advanced Imaging:
- MRI: Highly valuable for detailed assessment of articular cartilage in all compartments, meniscal integrity, ligamentous status, and identifying bone marrow edema or stress fractures. It helps confirm isolated PFOA.
- CT Scan: Indicated if there are concerns for significant trochlear dysplasia, rotational malalignment, or to accurately measure the tibial tubercle-trochlear groove (TT-TG) distance. Used for 3D templating and identification of osteophytes.
- Full-length weight-bearing alignment films: To rule out subtle coronal plane deformities or significant mechanical axis malalignment.
-
Templating:
- Use pre-operative radiographs and CT/MRI data to template for implant size (femoral trochlear component and patellar component) and potential position. Consider different implant designs (onlay vs. inlay trochlear components, dome vs. anatomic patellar components).
- Ensure appropriate component size to cover all diseased cartilage while minimizing over-resection or under-resection of bone.
-
Patient Counseling:
- Thorough discussion of the procedure, potential benefits (pain relief, functional improvement), risks (infection, instability, progression to TKA), and realistic post-operative expectations.
- Review rehabilitation protocols and expected recovery timeline.
- Discuss the possibility of staged or concomitant procedures if underlying issues like severe maltracking or ligamentous instability are identified.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Tourniquet Application: A pneumatic thigh tourniquet is applied high on the thigh. This helps maintain a bloodless field, which is crucial for precise bone cuts and cement fixation.
- Leg Holder/Support: The operative leg is positioned to allow for full knee flexion and extension intra-operatively. A soft leg holder or footrest can be used. Some surgeons prefer a free-draped limb to facilitate assessment of tracking and range of motion.
- Hip Position: Ensure the hip is in a neutral position to avoid compensatory rotations that might influence alignment.
- Anesthesia: General or spinal anesthesia is typically used. Femoral nerve block or adductor canal block can be used for post-operative pain management.
- Preparation and Draping: Standard sterile preparation and draping of the surgical limb from the thigh to the foot.
Detailed Surgical Approach / Technique
The surgical technique for patellofemoral arthroplasty requires precision in component placement to restore normal kinematics and alleviate pain. While specific steps may vary slightly between implant systems (e.g., onlay vs. inlay trochlear designs), the fundamental principles remain consistent.
1. Incision and Arthrotomy
- Incision: A straight anterior midline longitudinal skin incision (approximately 10-15 cm) is typically preferred, centered over the patella and extending distally to the tibial tubercle. This provides excellent exposure. Some surgeons may prefer a slightly medial parapatellar incision.
- Arthrotomy: A standard medial parapatellar arthrotomy is made, extending from the quadriceps tendon proximally, along the medial border of the patella, and distally through the patellar retinaculum. This approach facilitates patellar eversion and exposure of the trochlea. The retinaculum is sharply incised.
- Patellar Eversion: The patella is gently everted laterally to expose the articular surface of the patella and the femoral trochlea. Care must be taken to avoid excessive tension on the lateral retinaculum or extensor mechanism.
2. Intra-Articular Assessment and Debridement
- Inspection: A thorough intra-operative inspection of all knee compartments is performed to confirm that the articular cartilage damage is indeed isolated to the patellofemoral joint. The medial and lateral tibiofemoral compartments should appear healthy, with intact menisci and no significant chondral lesions.
- Ligamentous Stability: Assess collateral and cruciate ligament integrity. Any significant instability must be addressed or reconsidered as a contraindication.
- Osteophyte Removal: All significant patellofemoral osteophytes are meticulously removed from the patella and trochlea using an osteotome or rongeur. This prevents impingement and ensures proper component seating and tracking.
- Synovectomy: Limited synovectomy may be performed if hypertrophic synovitis is present.
3. Femoral Trochlear Preparation
This is the most critical step, as the accurate placement of the femoral component dictates patellar tracking and overall knee kinematics.
- Component Sizing: Trial femoral components are used to determine the optimal size. The goal is to cover all areas of patellofemoral cartilage wear without encroaching on the tibiofemoral articular cartilage or the intercondylar notch. The component should match the native trochlear anatomy as closely as possible in terms of width, depth, and curvature.
-
Alignment Guides:
Specific alignment guides provided by the implant system are utilized. These guides help determine the correct proximal-distal, medial-lateral, and rotational alignment of the femoral component.
- Proximal-Distal Placement: The trochlear component should be positioned to approximate the native trochlea's height, typically slightly proximal to the anterior-most aspect of the femoral condyles in extension. Avoid placing it too distal, which can cause patellar impingement in flexion, or too proximal, which can lead to patella alta.
- Medial-Lateral Placement: The component should be centered mediolaterally over the native trochlear groove, ensuring alignment with the patellar tracking axis.
- Rotational Alignment: This is crucial. The component should be aligned in the transverse plane to prevent internal or external rotation of the trochlear groove relative to the trans-epicondylar axis, which could lead to maltracking. Some systems use the Whiteside line (perpendicular to the trochlear groove, connecting the deepest part of the trochlea to the intercondylar notch) as a reference.
-
Bone Resection:
- The depth of resection is determined by the implant design (onlay vs. inlay). For onlay designs, only the diseased cartilage and minimal subchondral bone are removed to create a flat, stable bed. For inlay designs, a precisely shaped trochlear groove is created within the femur.
- Cutting blocks are used to make precise bony cuts. Often, a central sulcus cut is made first, followed by angled cuts to create the "wings" or anchoring surfaces for the femoral component. Use of specialized drills and burrs to prepare pegs or fins for fixation.
- Irrigate thoroughly to remove bone debris.
4. Patellar Preparation
-
Patellar Resection:
- Measure the pre-operative patellar thickness using a caliper. The goal is to resect sufficient bone to accommodate the patellar component, ensuring that the final patellar thickness (bone + implant) approximates the original, healthy patellar thickness. This avoids overstuffing the joint.
- A patellar cutting guide is used to make a flat resection of the posterior patellar surface. The cut should be perpendicular to the mechanical axis of the patella. Preserve enough posterior cortical bone for structural integrity.
-
Component Sizing and Fixation:
- Trial patellar components are used to select the appropriate size and confirm centering. The patellar component typically has a dome or anatomical shape.
- Drill holes or prepare a central keel slot in the patella according to the implant design for fixation.
5. Trial Reduction and Assessment
- Trial Components: Insert the trial femoral and patellar components.
- Range of Motion (ROM): Perform a full range of motion. Assess for smooth, congruent patellar tracking without impingement or subluxation.
- Stability: Check for patellar stability in extension and flexion.
- Soft Tissue Balance: If lateral patellar tightness or maltracking persists with trial components, a limited lateral retinacular release may be considered. However, this should be done cautiously, as over-release can lead to medial instability.
- Femoral Rotation: Verify correct femoral component rotation by observing patellar tracking. Adjust if necessary.
- Flexion Gap: Ensure adequate flexion gap without posterior impingement.
6. Final Component Implantation
- Cementing the Femoral Component: The femoral trochlear component is typically cemented. Prepare the bone surfaces by pulsatile lavage and drying. Apply bone cement (PMMA) to the posterior surface of the femoral component and press it firmly into position. Hold in place until cement hardens. Remove all extruded cement.
- Cementing the Patellar Component: Prepare the resected patellar surface. Apply bone cement to the back of the patellar component and to the patellar bone, then press it firmly onto the patella. Hold until cement hardens. Remove all extruded cement. Some patellar components are peg-fixation only and may not require cement.
7. Closure
- Hemostasis: Ensure meticulous hemostasis.
- Irrigation: Copious irrigation of the joint.
- Arthrotomy Closure: The medial parapatellar arthrotomy is closed in layers. The capsule is closed with a strong, absorbable suture.
- Skin Closure: Subcutaneous tissues and skin are closed in a standard fashion.
- Dressing: Apply a sterile dressing and a compressive bandage. A knee immobilizer may be applied in some cases, particularly if a lateral release was performed or if patellar stability is a concern.
Complications & Management
Despite careful patient selection and meticulous surgical technique, complications can occur following PFA. A thorough understanding of these potential issues and their management is crucial.
Common Complications
| Complication | Approximate Incidence (%) | Salvage Strategy |
|---|---|---|
| Persistent Anterior Knee Pain | 5-20 | Diagnosis: Rule out infection, loosening, maltracking, tibiofemoral progression, or referred pain. Management: Non-operative (physiotherapy, injections), targeted realignment procedures (e.g., TT transfer), revision PFA, or conversion to TKA. |
| Patellar Maltracking/Instability | 2-10 | Diagnosis: Clinical exam, dynamic imaging (e.g., fluoroscopy) if available. Management: Physiotherapy (VMO strengthening), bracing, lateral retinacular release (if not done previously), medial patellofemoral ligament (MPFL) reconstruction, or revision of components/conversion to TKA if malalignment is severe. |
| Aseptic Loosening of Components | 1-5 | Diagnosis: Radiographs (radiolucent lines), bone scan, CT. Management: Revision PFA (if only one component is loose and tibiofemoral compartments are still pristine), or conversion to TKA. |
| Infection (Superficial/Deep) | <1-2 | Diagnosis: Clinical signs (erythema, swelling, discharge, fever), elevated inflammatory markers (ESR, CRP), joint aspiration (cell count, culture, gram stain). Management: Superficial: Oral antibiotics. Deep: Surgical irrigation and debridement (I&D), component retention with suppressive antibiotics (if acute and stable), or two-stage revision (I&D + spacer, then TKA/PFA). |
| Patellar Fracture | 1-3 | Diagnosis: Radiographs. Management: Non-displaced: Immobilization, protected weight-bearing. Displaced: Open reduction internal fixation (ORIF), partial/total patellectomy (rare for PFA), or revision with TKA (if extensor mechanism compromised). |
| Progression of Tibiofemoral OA | 5-15 (long-term) | Diagnosis: Clinical worsening, weight-bearing radiographs. Management: Non-operative management, eventually conversion to TKA. |
| Arthrofibrosis/Stiffness | 2-5 | Diagnosis: Reduced range of motion (ROM) clinically. Management: Intensive physiotherapy, manipulation under anesthesia (MUA), or arthroscopic lysis of adhesions. |
| Extensor Mechanism Rupture | <1 | Diagnosis: Clinical inability to actively extend knee, patellar baja or alta. Management: Surgical repair/reconstruction (e.g., allograft reconstruction for chronic ruptures). |
| Neurovascular Injury | <1 | Diagnosis: Clinical (paresthesia, weakness, absent pulses). Management: Nerve repair/decompression, vascular repair. Rare but devastating. |
| Deep Vein Thrombosis (DVT)/PE | <1-2 (with prophylaxis) | Diagnosis: DVT: Doppler ultrasound. PE: CT pulmonary angiography. Management: Anticoagulation. |
General Principles of Management
- Early Diagnosis: Prompt recognition of complications is crucial for effective management.
- Infection Protocol: Adherence to strict perioperative infection prevention protocols, including prophylactic antibiotics and meticulous surgical technique.
- Revision vs. Conversion: The decision to revise the PFA components or convert to a TKA depends on the nature of the complication, the health of the remaining tibiofemoral compartments, and patient factors. Progression of tibiofemoral OA usually necessitates conversion to TKA.
- Multidisciplinary Approach: Management often requires collaboration with infectious disease specialists, rehabilitation therapists, and pain management teams.
- Patient Education: Patients must be counseled pre-operatively about the potential for complications and the possibility of further surgery, including conversion to TKA.
Post-Operative Rehabilitation Protocols
A structured and progressive rehabilitation protocol is essential for optimizing outcomes, restoring function, and preventing complications following PFA. The protocol is typically divided into phases, with clear goals and guidelines for progression.
Phase I: Immediate Post-Operative (Weeks 0-2)
Goals:
* Pain and edema control.
* Protect surgical site.
* Minimize muscle atrophy.
* Initiate early, controlled range of motion (ROM).
Guidelines:
*
Weight-Bearing:
Partial weight-bearing (PWB) with crutches or walker, progressing to weight-bearing as tolerated (WBAT) with the knee immobilizer locked in extension for transfers. Some surgeons advocate for immediate WBAT without immobilizer, depending on intra-operative stability.
*
ROM:
* Continuous Passive Motion (CPM) machine may be initiated, typically 0-70 degrees initially, progressing as tolerated.
* Gentle active-assisted and passive ROM exercises.
* Goal: 0-90 degrees by end of week 2.
*
Exercises:
* Ankle pumps (DVT prophylaxis).
* Quadriceps setting (isometric contractions).
* Gluteal sets.
* Gentle hamstring curls (supine).
* Patellar mobilizations (superior, inferior, medial, lateral) once incision is dry and closed.
*
Cryotherapy:
Regular application to reduce pain and swelling.
*
Wound Care:
Maintain clean and dry incision.
*
Pain Management:
Opioids, NSAIDs, and regional blocks as needed.
Phase II: Early Recovery (Weeks 2-6)
Goals:
* Restore full knee extension.
* Increase knee flexion to functional levels.
* Improve quadriceps and hamstring strength.
* Begin proprioceptive training.
Guidelines:
*
Weight-Bearing:
Progress to full weight-bearing (FWB) without assistive devices as pain allows and quadriceps control improves. Discontinue immobilizer.
*
ROM:
* Continue active and passive ROM exercises.
* Goal: 0-110 degrees flexion by end of week 6.
*
Exercises:
*
Strengthening:
* Wall slides (shallow squats, 0-60 degrees flexion).
* Mini-squats (controlled depth, avoiding deep flexion).
* Leg presses (limited range, light resistance).
* Hamstring curls (prone/standing).
* Calf raises.
* Step-ups/downs (small steps).
*
Proprioception:
Single leg stance (with support), weight shifts.
*
Cardiovascular:
Stationary bicycle (light resistance, seat high to limit flexion), elliptical trainer.
*
Scar Management:
Gentle massage and desensitization.
Phase III: Intermediate Rehabilitation (Weeks 6-12)
Goals:
* Achieve full, pain-free ROM.
* Normalize gait pattern.
* Progress strength, power, and endurance.
* Advance functional activities.
Guidelines:
*
ROM:
Continue working towards full ROM (0-125+ degrees).
*
Exercises:
*
Strengthening:
Increase resistance and depth for squats, lunges. Incorporate functional exercises.
* Leg extensions (light resistance, controlled range, avoiding full terminal extension with heavy loads).
* Eccentric quadriceps strengthening.
* Lateral band walks.
*
Proprioception:
Unilateral stance on unstable surfaces, balance board.
*
Plyometrics (low-level):
Single leg hops, box jumps (initially small heights) only for highly active patients without pain.
*
Cardiovascular:
Increase intensity and duration on bike/elliptical. Gentle swimming.
*
Return to Activity:
Gradual return to light recreational activities. Avoid high-impact or deep flexion activities initially.
Phase IV: Advanced Activity / Return to Sport (Weeks 12+)
Goals:
* Achieve maximal functional recovery.
* Safe return to desired activities/sports.
* Maintain strength and endurance.
Guidelines:
*
Functional Progression:
Tailored to patient's specific activity goals.
*
Sport-Specific Training:
Gradually introduce sport-specific drills, emphasizing proper technique and controlled movements.
*
High-Impact Activities:
Generally discouraged in the long term due to increased wear on the implant. Exceptions are made for select patients with appropriate counseling.
*
Maintenance Program:
Lifelong commitment to a home exercise program for strength, flexibility, and endurance.
*
Patient Education:
Emphasize avoiding activities that consistently cause anterior knee pain, protecting the knee, and recognizing signs of potential complications.
Important Considerations:
*
Individualization:
Protocols must be tailored to the individual patient's progress, pain levels, and specific surgical findings (e.g., if a lateral release was performed).
*
Communication:
Close communication between the surgeon and physical therapist is crucial.
*
Avoidance of Overloading:
Deep squats, prolonged kneeling, and high-impact activities should be approached cautiously or avoided, especially in the early stages, to prevent excessive stress on the patellofemoral joint.
Summary of Key Literature / Guidelines
Patellofemoral arthroplasty has undergone significant advancements since its inception in the 1970s, transitioning from early designs with variable success to modern, anatomically congruent implants yielding more predictable outcomes. Key literature and guidelines highlight critical aspects of patient selection, implant design, surgical technique, and long-term outcomes.
Historical Perspective and Evolution
Early PFA designs, particularly the "button" patellar implants without a femoral component, had high failure rates due to unaddressed trochlear pathology and subsequent patellar loosening or maltracking. The introduction of combined patellar and femoral trochlear components significantly improved results. Further refinements have included anatomically shaped femoral components (e.g., matching the sulcus angle and depth), patellar components designed to restore native patellar thickness, and advancements in fixation methods.
Outcomes and Survival Rates
- Pain Relief: Numerous studies report significant pain relief in a large percentage of appropriately selected patients, often exceeding 80% good to excellent results in the short to mid-term.
- Functional Improvement: Patients typically experience substantial improvements in activities of daily living, including walking, stair climbing, and getting up from a chair.
- Survival Rates: Mid-term survival rates (5-10 years) for modern PFA implants are generally reported in the range of 80-95%, with conversion to TKA being the primary endpoint for failure. Long-term studies (10-15 years) suggest survival rates may decrease to 70-80%, often due to progression of tibiofemoral OA or aseptic loosening.
- Comparison to TKA: PFA typically offers superior knee kinematics, proprioception, and functional scores compared to TKA in patients with isolated PFOA, as it preserves healthy tibiofemoral compartments and ACL/PCL function. However, the revision burden for PFA can be higher than primary TKA.
Key Factors Influencing Outcomes
- Patient Selection: This remains the most critical factor. Strict adherence to indications, particularly confirming isolated PFOA without significant tibiofemoral involvement or uncorrectable maltracking, is paramount. Studies consistently show that patients with pre-existing tibiofemoral OA, inflammatory arthritis, or significant patellar instability have poorer outcomes.
-
Implant Design:
- Onlay vs. Inlay Trochlear Components: Both designs have demonstrated success. Onlay components are generally less bone-resecting and may be preferred when trochlear dysplasia is less severe. Inlay components may offer better congruency in cases with deeper trochlear pathology.
- Patellar Component: Designs vary (dome, anatomical). Restoring native patellar thickness is critical to avoid overstuffing.
- Fixed vs. Mobile Bearing: While popular in unicompartmental knee arthroplasty, mobile-bearing PFA designs have not shown consistent superior outcomes and may carry higher risks of dislocation or wear in the patellofemoral joint.
- Surgical Technique: Meticulous technique in component sizing, alignment, and fixation is essential to optimize patellar tracking and minimize impingement or instability. Proper rotational alignment of the femoral component is especially crucial. Soft tissue balancing (e.g., lateral retinacular release) should be performed judiciously.
- Post-operative Rehabilitation: Adherence to a structured, progressive rehabilitation program is vital for restoring range of motion, strength, and function, while protecting the implant.
Current Guidelines and Recommendations
- Consensus: Most orthopedic societies and expert panels recommend PFA for patients with symptomatic, isolated PFOA refractory to conservative measures, provided they meet strict selection criteria.
- Advanced Imaging: Pre-operative MRI and often CT scans are recommended to confirm the isolation of the disease and to assess patellofemoral morphology (trochlear dysplasia, TT-TG distance) more precisely.
- Patient Expectations: Surgeons must thoroughly counsel patients about the realistic expectations of PFA, including potential limitations, the importance of rehabilitation, and the possibility of future conversion to TKA.
- Future Directions: Research continues into patient-specific instrumentation and implants, kinematic alignment principles for PFA, and further long-term outcome studies. The role of robotic-assisted PFA is also being explored.
In summary, PFA is a valuable and increasingly effective procedure for selected patients with end-stage isolated PFOA, offering a less invasive alternative to TKA with good mid-term results and preservation of native knee kinematics. Success hinges upon stringent patient selection, precise surgical execution, and diligent post-operative rehabilitation.
You Might Also Like