The Ilioinguinal Approach: Comprehensive Surgical Anatomy & Acetabular Fracture Management

Key Takeaway
The ilioinguinal approach is a fundamental anterior surgical exposure for complex acetabular fractures. It offers comprehensive access to the inner ilium, quadrilateral surface, and pubic symphysis via three distinct windows (lateral, middle, medial), enabling precise fracture reduction and fixation crucial for optimal patient outcomes.
Introduction & Epidemiology
The ilioinguinal approach is a fundamental anterior surgical exposure used primarily in the management of complex acetabular fractures, particularly those involving the anterior column, anterior wall, and specific patterns of both-column fractures. Developed and popularized by Letournel and Judet, this approach provides comprehensive visualization and access to the inner aspect of the ilium, the quadrilateral surface, the superior pubic ramus, and the pubic symphysis, while minimizing disturbance to hip musculature. Its strength lies in its ability to address fractures extending from the sacroiliac joint to the pubic symphysis along the pelvic brim.
Acetabular fractures are typically the result of high-energy trauma, such as motor vehicle collisions or falls from height, and exhibit a bimodal age distribution affecting young, active individuals and, increasingly, osteopenic elderly patients sustaining low-energy falls. Accurate anatomical reduction and stable internal fixation are paramount to restore joint congruity, optimize load distribution, and mitigate the risk of post-traumatic arthritis, which remains a significant long-term complication. The choice of surgical approach is dictated by the fracture pattern, as classified by Judet and Letournel, the surgeon's expertise, and the associated injuries. The ilioinguinal approach is a versatile and powerful tool within the armamentarium for managing these challenging injuries.
Surgical Anatomy & Biomechanics
Surgical Anatomy
A thorough understanding of the regional anatomy is critical for safe and effective utilization of the ilioinguinal approach. The approach exposes the medial aspect of the ilium and the anterior column of the acetabulum through specific internervous planes and three distinct surgical "windows."
Surface Anatomy and Incision:
The incision typically extends from the anterior superior iliac spine (ASIS) to the pubic symphysis, following a curvilinear or "bikini" line. Key bony landmarks include the ASIS, iliac crest, pubic tubercle, and pubic symphysis.
Layers of Dissection:
- Skin and Subcutaneous Tissue: The incision is carried through the skin and subcutaneous fat.
- Scarpa's Fascia: This deeper membranous layer of subcutaneous tissue is encountered and incised.
- External Oblique Aponeurosis: This constitutes the anterior wall of the inguinal canal. It is incised longitudinally, typically parallel to its fibers, allowing creation of superior and inferior flaps. This step exposes the spermatic cord in males or the round ligament in females. The ilioinguinal nerve, which pierces the internal oblique and then runs anterior to the spermatic cord within the inguinal canal, should be identified and protected, usually retracted superiorly. The iliohypogastric nerve is typically superior and not directly in the field. The lateral femoral cutaneous nerve (LFCN) should also be identified as it emerges from beneath the inguinal ligament, lateral to the sartorius, to prevent iatrogenic injury.
The Three Windows of the Ilioinguinal Approach:
The hallmark of the ilioinguinal approach is the development of three distinct windows to access different anatomical regions, created by selective detachment and retraction of key structures.
-
Lateral Window:
- This window is developed by detaching the origins of the sartorius and tensor fascia lata (TFL) from the ASIS and retracting them laterally.
- The superior flap of the external oblique aponeurosis is retracted superiorly.
- Subperiosteal dissection is carried out along the inner table of the iliac wing, posterior to the iliacus muscle. The iliacus and psoas muscles are retracted medially.
- This window provides access to the inner surface of the ilium from the ASIS to the sacroiliac joint, the greater sciatic notch, and the pelvic brim. It is primarily used for fixation of the posterior superior aspects of the anterior column and reduction of superior iliac fragments.
-
Image Integration Point:

-
Middle Window:
- This window is created by carefully dissecting and retracting the femoral neurovascular bundle (femoral artery, vein, and nerve), along with the psoas and iliacus muscles, medially.
- The inguinal ligament (inferior border of the external oblique aponeurosis) is elevated from the iliopectineal eminence.
- This is arguably the most critical and delicate window, as it directly exposes the external iliac vessels and the femoral nerve. Injury to these structures is a serious complication.
- It provides access to the quadrilateral surface, the anterior aspect of the sacroiliac joint, and the anterior column from the iliopectineal eminence to the pubic ramus. It is often used for reduction and fixation of the quadrilateral plate.
-
Image Integration Point:

-
Medial Window:
- This window is developed by mobilizing the spermatic cord/round ligament inferiorly and exposing the posterior aspect of the rectus abdominis muscle.
- The rectus abdominis and pyramidalis muscles are usually partially or completely detached from the pubic tubercle and reflected superiorly.
- Care is taken to identify and ligate or coagulate the "corona mortis," an anatomical variant involving an anastomosis between the obturator and external iliac/inferior epigastric vessels, which can cause significant bleeding if injured.
- This window provides access to the pubic symphysis, the superior pubic ramus, and the medial aspect of the obturator foramen. It is critical for reduction and fixation of fractures involving the pubic ramus and medial extension of anterior column fractures.
-
Image Integration Point:

Internervous Planes:
The ilioinguinal approach exploits several internervous planes to minimize muscle disruption:
1. Between the external oblique and the internal oblique/transversus abdominis (for the inguinal canal).
2. Between the sartorius/TFL and the inner table of the ilium (for the lateral window).
3. Between the psoas/iliacus muscles and the inner table of the ilium (for the lateral and middle windows).
4. Between the rectus abdominis and the underlying bladder/pelvic wall (for the medial window).
Biomechanics
The acetabulum is a critical component of the pelvic ring, designed to transmit axial loads from the spine and pelvis to the lower extremities. Its structural integrity is essential for stable hip joint function.
- Load Transmission: The weight-bearing dome of the acetabulum, particularly the posterior column, is crucial for transmitting forces from the femoral head to the ischium. The anterior column transmits forces to the pubic ramus and ilium. The quadrilateral surface, located medially, resists medial displacement of the femoral head.
-
Fracture Patterns:
Disruption of these columns leads to instability and joint incongruity.
- Anterior Column Fractures: Affect the iliopectineal line and may extend from the iliac crest to the pubic symphysis.
- Anterior Wall Fractures: Involve only the anterior portion of the acetabulum, often associated with anterior hip dislocations.
- Both-Column Fractures: These are complex patterns where the articular surface is separated from the intact ilium. The ilioinguinal approach is often indicated for these when the primary displacement is anterior and medial, with the posterior column involvement being less severe or secondary.
- Fixation Principles: Anatomical reduction and rigid internal fixation are paramount. This restores the spherical shape of the acetabulum, maintains congruity with the femoral head, and allows early rehabilitation. Plates and screws placed along the pelvic brim and quadrilateral surface help to buttress the fragments, preventing secondary displacement and medialization of the femoral head.
Indications & Contraindications
The decision for operative intervention via the ilioinguinal approach is complex, weighing fracture characteristics against patient factors.
Indications for Operative Management
| Indication Category | Specific Features |
|---|---|
| Fracture Pattern | Displaced anterior column fractures |
| Displaced anterior wall fractures | |
| Displaced both-column fractures where the primary displacement is anterior and medial, and the posterior column is less severely involved or the ilioinguinal approach can adequately address the posterior component (e.g., via the middle window) | |
| Transverse fractures with anterior extension | |
| Articular Incongruity | Articular step-off or gap >2 mm |
| Impingement of intra-articular fragments | |
| Hip Joint Stability | Irreducible hip dislocation |
| Gross instability of the hip joint after reduction | |
| Patient Factors | Young, physiologically robust patients with high functional demands |
| Patients with good bone quality amenable to stable fixation | |
| Specific Deformities | Medial displacement of the femoral head due to quadrilateral plate fracture or severe anterior column displacement. |
Contraindications
-
Absolute Contraindications:
- Patient Instability: Unresuscitatable polytrauma patient (ABC priorities always supersede orthopedic fixation).
- Active Infection: Systemic sepsis or local infection at the surgical site.
- Severe Soft Tissue Compromise: Extensive degloving injuries, burns, or open wounds in the proposed surgical field.
- Surgeon Inexperience: Lack of expertise with this complex approach.
-
Relative Contraindications:
- Excessive Swelling/Blistering: Delay surgery until soft tissues improve.
- Morbid Obesity: May complicate exposure and increase operative time and risks.
- Severe Comorbidities: Medical conditions precluding general anesthesia or prolonged surgery.
- Extensive Scarring: Previous abdominal or pelvic surgery may make dissection hazardous.
- Specific Fracture Patterns: Pure posterior column or posterior wall fractures, where a posterior approach (e.g., Kocher-Langenbeck) is more appropriate.
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical to optimize outcomes and minimize complications.
Pre-Operative Planning
-
Imaging Review:
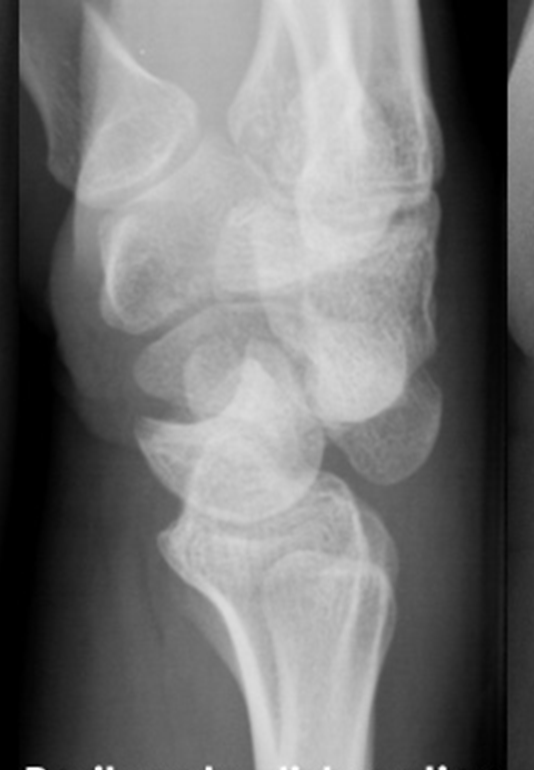
- Plain Radiographs: AP pelvis, iliac oblique, and obturator oblique views are essential for initial assessment and Judet and Letournel classification.
- Computed Tomography (CT) Scan: Mandatory. This provides detailed information regarding fracture lines, displacement, comminution, impaction, and intra-articular fragments. 3D reconstructions are invaluable for understanding complex fracture morphology and planning reduction maneuvers.
- Angiography (Selective): May be considered in cases of suspected major vascular injury or difficult reoperations where the corona mortis is a concern.
-
Fracture Classification and Strategy:
- Confirm the Judet and Letournel classification.
- Determine the primary fracture components to be reduced and fixed.
- Anticipate specific reduction tools (e.g., pointed reduction clamps, ball-spikes, push-pull screws, pelvic clamps).
-
Implant Selection and Templating:
- Pre-contoured plates (e.g., pelvic brim plates, quadrilateral surface plates) are often utilized. Reconstruction plates may also be needed.
- Screw length and trajectory should be estimated to avoid intra-articular penetration or neurovascular injury.
- Templating on printed CT images helps visualize plate contour and screw placement.
- Neurovascular Assessment: Identify any pre-existing neurological deficits or vascular injuries.
- Timing of Surgery: Typically performed once the patient is medically optimized, within 7-10 days of injury to avoid extensive callus formation and soft tissue contracture.
Patient Positioning
- Operating Table: The patient is positioned supine on a radiolucent operating table, allowing unrestricted fluoroscopic access. A beanbag or specialized hip table may be used to stabilize the pelvis.
- Pressure Point Padding: All pressure points are meticulously padded to prevent neuropathies or skin breakdown.
- Leg Positioning: The ipsilateral leg is positioned to allow full range of motion, particularly external and internal rotation, which can aid in reduction and assessment of hip stability. The leg may be placed in a sterile stockinette or suspended to allow free movement.
- Fluoroscopy Access: The C-arm is positioned for easy access to obtain AP, iliac oblique, and obturator oblique views of the pelvis.
- Surgical Prep and Drape: The surgical field is prepared and draped from the mid-chest to the mid-thigh, extending laterally to the contralateral iliac crest, to allow for extensive exposure and potential harvest of autograft if needed.
- Foley Catheter: A Foley catheter is inserted pre-operatively to decompress the bladder and monitor urine output.
Detailed Surgical Approach / Technique
The ilioinguinal approach is performed in a systematic, layered fashion, emphasizing careful identification and protection of neurovascular structures.
1. Incision and Initial Dissection
- Incision: A curvilinear incision is made, extending from 2 cm posterior and inferior to the ASIS, along the iliac crest, continuing along the inguinal crease towards the pubic symphysis. The length varies depending on the anticipated fracture extension and exposure required.
- Superficial Dissection: The incision is deepened through the skin and subcutaneous tissue to Scarpa's fascia. The superficial circumflex iliac artery and vein may be encountered and ligated.
- Lateral Femoral Cutaneous Nerve (LFCN): Identify the LFCN emerging from under the inguinal ligament, lateral to the sartorius. It is highly variable in its course; meticulous dissection and protection are paramount. It is usually retracted laterally or inferiorly.
2. Exposure of the Inguinal Canal
- External Oblique Aponeurosis: The external oblique aponeurosis is identified. Its fibers run inferomedially. An incision is made along the fibers of the external oblique, starting just above the ASIS and extending towards the pubic tubercle, parallel and superior to the inguinal ligament. This incision is extended to create a superior flap and an inferior flap.
- Spermatic Cord/Round Ligament: The spermatic cord in males or the round ligament in females is identified. The ilioinguinal nerve, which typically runs on the anterior surface of the spermatic cord, should be identified and carefully protected, usually retracted superiorly with the superior flap. The cord/ligament is mobilized and encircled with a Penrose drain or vessel loop for retraction.
3. Development of the Three Windows
A. Lateral Window
- Sartorius and TFL Release: The origins of the sartorius and tensor fascia lata (TFL) are detached from the ASIS using electrocautery or a knife. These muscles are then retracted laterally, exposing the lateral aspect of the iliac wing.
- Subperiosteal Dissection: A subperiosteal dissection is initiated along the inner surface of the iliac wing, exposing the iliac fossa. The iliacus muscle is carefully elevated from its origin on the ilium. The psoas muscle, typically lying more medially, is identified.
-
Retraction:
The iliacus and psoas muscles, along with their overlying fascia, are retracted medially to expose the inner table of the ilium from the ASIS posteriorly towards the sacroiliac joint. This provides excellent access to the pelvic brim and the superior aspects of the anterior column.
-
Image Integration Point:

-
Image Integration Point:
B. Medial Window
- Rectus Abdominis Release: The rectus abdominis and pyramidalis muscles are identified. These muscles are typically detached from the pubic tubercle and reflected superiorly. This step exposes the superior pubic ramus and the pubic symphysis.
- Spermatic Cord/Round Ligament Mobilization: The spermatic cord/round ligament is retracted inferiorly using its Penrose drain.
- Corona Mortis: Meticulous dissection is performed along the superior pubic ramus, deep to the pubic tubercle. The "corona mortis" (aberrant obturator vessels) crossing the superior pubic ramus in 10-30% of cases must be anticipated. These vessels should be carefully identified and either ligated and divided or protected if possible.
-
Exposure:
This window provides access to the pubic symphysis, the superior pubic ramus, and the medial aspect of the obturator foramen.
-
Image Integration Point:

-
Image Integration Point:
C. Middle Window
- Femoral Neurovascular Bundle Mobilization: This is the most challenging and critical step. The femoral artery, vein, and nerve are situated immediately deep to the inguinal ligament. A careful blunt and sharp dissection is performed along the posterior aspect of the inguinal ligament, lateral to the spermatic cord.
- Retraction: The entire femoral neurovascular bundle (contained within the femoral sheath), along with the iliopsoas muscle, is retracted medially using broad, flat retractors. Specific self-retaining retractors (e.g., Judet retractors, ring retractors with broad blades) are ideal to maintain exposure without compromising blood flow or neural function.
-
Exposure:
This window provides access to the external iliac vessels, the iliopectineal eminence, the pelvic brim, and importantly, the quadrilateral surface. Care must be taken to protect the obturator nerve and vessels, which cross the medial aspect of this window, often deep to the external iliac vein.
-
Image Integration Point:

-
Image Integration Point:
4. Fracture Reduction and Fixation
The sequence of reduction often involves establishing key reduction points and proceeding from the most stable to the least stable fragments.
- Fragment Identification: Visualize all fracture lines and fragments, using all three windows.
- Temporary Fixation: K-wires are invaluable for temporary stabilization of reduced fragments.
-
Reduction Maneuvers:
- Traction: Longitudinal traction on the leg can help restore length and de-impact fragments.
- Ball-Spike Pusher/Pointed Reduction Clamps: These are used to manipulate fragments under direct vision.
- Pelvic Reduction Clamps: Various clamps (e.g., Matta, Farabeuf) can be applied from the iliac wing to the superior pubic ramus, or across the symphysis, to compress and reduce fragments.
- Push-Pull Screws: May be used to manipulate displaced fragments, particularly the quadrilateral surface.
- Leverage: Instruments can be used as levers to disimpact or elevate depressed fragments.
-
Assessing Reduction:
- Direct Vision: Visual inspection of the fracture lines and articular surface (if accessible).
- Palpation: Palpate the inner table of the ilium and the quadrilateral surface to assess step-off and rotation.
- Fluoroscopy: Essential for confirming anatomical reduction. Standard views (AP, iliac oblique, obturator oblique) are used. An intra-operative arthrotomy through the fracture site may be rarely considered to visualize the joint directly.
-
Definitive Fixation:
- Plates: Pre-contoured acetabular plates are commonly used along the pelvic brim. Reconstruction plates can be molded to fit complex contours. Plates are typically placed along the pelvic brim from the sacroiliac joint to the pubic symphysis, providing buttress and neutralization. A separate plate or lag screws may be used to address the quadrilateral surface, preventing medialization.
- Screws: Cortical and lag screws are used for fixation. Screw lengths must be meticulously measured to avoid intra-articular penetration. Fluoroscopy is crucial to verify screw position and length.
-
Image Integration Point:

5. Closure
- Hemostasis: Thorough irrigation and meticulous hemostasis are achieved.
- Drainage: A suction drain is often placed in the retroperitoneal space, particularly if there is significant dead space or anticipated bleeding.
- Rectus Abdominis Repair: The rectus abdominis muscle is reattached to the pubic tubercle.
- Inguinal Canal Repair: The external oblique aponeurosis is repaired. Care is taken to ensure adequate closure of the inguinal canal to prevent future herniation, while avoiding constriction of the spermatic cord/round ligament or ilioinguinal nerve.
- Sartorius/TFL Reattachment: The origins of the sartorius and TFL are reattached to the ASIS.
- Layered Closure: Scarpa's fascia, subcutaneous tissue, and skin are closed in layers.
Complications & Management
The ilioinguinal approach is associated with a specific set of complications, reflecting the complex anatomy of the anterior pelvis. Early recognition and appropriate management are crucial.
Common Complications and Management Strategies
| Complication | Incidence | Salvage Strategy |
|---|---|---|
| Neurovascular Injury | ||
| - Lateral Femoral Cutaneous Nerve (LFCN) Neuropraxia/Neuralgia | Up to 80% (sensory deficits), 5-10% (persistent symptoms) | Conservative management (medications, nerve blocks). Surgical neurolysis or neurectomy for persistent, debilitating symptoms. Prevention: meticulous identification and retraction. |
| - Femoral Nerve/Vessels | Rare (0.5-2%) | Immediate surgical exploration and repair by a vascular surgeon. Aggressive monitoring. Prevention: careful medial retraction of the bundle, avoidance of excessive force or prolonged retraction. |
| - Corona Mortis Hemorrhage | Up to 3% | Intraoperative ligation or coagulation of vessels. Prevention: careful identification during medial window dissection. |
| - Obturator Nerve/Vessels | Rare (<1%) | Immediate exploration and repair. Prevention: meticulous dissection and retraction in the middle window. |
| Infection | 2-5% | Superficial: Wound care, oral antibiotics. Deep: Surgical debridement, intravenous antibiotics, removal of hardware if stable. Prevention: sterile technique, appropriate antibiotic prophylaxis, meticulous hemostasis, drainage. |
| Heterotopic Ossification (HO) | 15-50% (radiographic), <5% (symptomatic) | Prophylaxis: Indomethacin (25 mg TID for 6 weeks) or radiation therapy (single dose 700-800 cGy within 72 hours post-op). Surgical excision for symptomatic HO after maturation (usually >1 year post-op). Prevention: atraumatic technique, thorough irrigation. |
| Non-union/Malunion | 2-5% | Non-union: Revision surgery with debridement, bone grafting, and rigid internal fixation. Malunion: Corrective osteotomy for symptomatic deformity. Prevention: anatomical reduction, stable fixation, appropriate post-operative weight-bearing. |
| Post-traumatic Arthritis (PTA) | 10-20% | Management of symptoms (NSAIDs, injections). Total hip arthroplasty (THA) or hip arthrodesis for end-stage arthritis. Prevention: anatomical reduction of articular surface, stable fixation, early range of motion. |
| Inguinal Hernia | 1-3% | Surgical repair of the hernia defect. Prevention: careful and anatomical repair of the external oblique aponeurosis and inguinal canal structures during closure, avoidance of tension on suture lines. |
| Thromboembolic Events | DVT 5-10%, PE <1% | Prophylaxis: pharmacological (LMWH, fondaparinux, aspirin) and mechanical (SCDs, early mobilization). Treatment: anticoagulation, IVC filter if indicated. Prevention: early mobilization, adherence to prophylaxis guidelines. |
| Bladder/Bowel Injury | Very Rare | Immediate consultation with general surgery/urology, direct repair. Prevention: meticulous subperiosteal dissection in the medial window, careful retraction of bladder with Foley catheter in place. |
| Hardware Related Complications | Variable | Prominent hardware may require removal after fracture union. Intra-articular screws require immediate revision. Infection, loosening. Prevention: careful templating, appropriate screw length, confirmation with fluoroscopy. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing functional recovery and preventing complications following acetabular fracture fixation via the ilioinguinal approach. Protocols vary based on fracture stability, bone quality, patient comorbidities, and surgeon preference.
Immediate Post-Operative Period (Days 0-7)
- Pain Management: Multimodal analgesia including regional blocks, NSAIDs, acetaminophen, and opioids.
- Deep Vein Thrombosis (DVT) Prophylaxis: Pharmacological (e.g., LMWH) and mechanical (e.g., sequential compression devices) prophylaxis initiated immediately.
-
Weight-Bearing (WB) Status:
- Typically non-weight bearing (NWB) or touch-down weight bearing (TDWB) (10-15 kg) on the affected extremity for 8-12 weeks, depending on fracture stability and fixation strength.
- Crutches or a walker are used for ambulation.
-
Range of Motion (ROM):
- Continuous Passive Motion (CPM): May be used for 2-4 hours/day to prevent stiffness and reduce HO, though evidence is variable.
- Gentle Active-Assisted ROM: Initiated within pain limits, focusing on hip flexion, abduction, and rotation. Avoid extremes of motion, especially internal rotation and adduction, which can stress the anterior column repair.
- Ankle Pumps, Quadriceps Sets, Gluteal Sets: To maintain muscle tone and promote circulation.
- Transfers and Mobility: Training for safe bed mobility, transfers, and use of assistive devices.
Early Rehabilitation Phase (Weeks 2-8)
- Progressive ROM: Gradually increase hip ROM, respecting pain and stability.
- Isometric Strengthening: Continue and progress isometric exercises for hip flexors, abductors, and extensors.
- Core Stability: Begin gentle core strengthening exercises.
- Scar Management: Initiate scar massage and desensitization once the incision is healed.
- Modalities: Therapeutic modalities (e.g., heat, ice, ultrasound) as indicated for pain and swelling.
Intermediate Rehabilitation Phase (Weeks 8-12)
- Radiographic Assessment: Repeat radiographs (AP, oblique views) at 8-10 weeks to assess fracture healing.
- Progression of Weight-Bearing: If radiographic healing is evident and the patient tolerates it, progress to partial weight-bearing (PWB) with assistive devices (e.g., 25-50% body weight).
- Progressive Strengthening: Initiate gentle isotonic strengthening for hip musculature.
- Gait Training: Focus on normalized gait pattern with reduced weight bearing.
- Aquatic Therapy: May be beneficial to facilitate early weight-bearing and strengthen in a low-impact environment.
Advanced Rehabilitation Phase (Months 3-6+)
- Full Weight-Bearing (FWB): Once fracture union is confirmed radiographically, progress to FWB and discontinue assistive devices.
- Functional Strengthening: Advance to more challenging exercises, including closed-chain activities, proprioceptive training, and sport-specific drills (if applicable).
- Endurance Training: Incorporate cardiovascular activities.
- Return to Activity: Gradual return to activities of daily living and recreational sports, typically after 6-12 months, contingent on full strength, pain-free ROM, and radiographic union. High-impact activities are often restricted for 12 months.
Summary of Key Literature / Guidelines
The management of acetabular fractures, including the application of the ilioinguinal approach, is built upon decades of research and clinical experience. The seminal work of Emile Letournel and Robert Judet in the 1960s and 1970s established the comprehensive classification system and detailed surgical approaches, including the ilioinguinal, which remain the cornerstone of current practice. Their anatomical descriptions and operative techniques revolutionized the treatment of these complex injuries, moving from largely conservative management to a focus on anatomical reduction and stable internal fixation.
Key Principles from Literature:
- Anatomical Reduction: Multiple studies consistently demonstrate that anatomical reduction (defined as <1-2 mm articular step-off or gap) is the single most important predictor of long-term functional outcomes and reduces the risk of post-traumatic arthritis.
- Timing of Surgery: While immediate fixation in polytrauma patients is generally contraindicated, elective fixation is typically performed within 7-14 days of injury. Delaying beyond this window can lead to increased difficulty of reduction due to fracture healing and soft tissue contracture, often resulting in poorer outcomes.
- Surgeon Experience: The complexity of acetabular fracture surgery, particularly approaches like the ilioinguinal, necessitates significant surgeon experience. High-volume centers and surgeons tend to report lower complication rates and superior outcomes.
- Imaging Modalities: Contemporary guidelines emphasize the indispensable role of advanced imaging, specifically CT with 3D reconstructions , for accurate fracture classification, surgical planning, and intra-operative assessment of reduction. Fluoroscopy remains critical for real-time intraoperative guidance during reduction and fixation.
- Complication Management: The high incidence of specific complications, such as LFCN neuropraxia and heterotopic ossification, necessitates proactive prophylaxis (e.g., Indomethacin or radiation for HO, careful nerve identification for LFCN). Thorough knowledge of regional anatomy is key to preventing neurovascular injuries.
- Evolving Techniques: While the open ilioinguinal approach remains a standard, ongoing research explores minimally invasive percutaneous techniques for select fractures, often aided by navigation or robotic assistance. However, for complex displaced anterior column and both-column fractures requiring extensive exposure, the open ilioinguinal approach continues to be the gold standard.
- Evidence-Based Protocols: Post-operative rehabilitation protocols are increasingly standardized, advocating for early, controlled range of motion and delayed weight-bearing based on the stability of fixation and radiographic signs of union.
In summary, the ilioinguinal approach is a powerful and indispensable tool in the orthopedic surgeon's armamentarium for managing complex anterior acetabular fractures. Its successful application demands a deep understanding of surgical anatomy, meticulous pre-operative planning, precise surgical execution, and diligent post-operative rehabilitation, all guided by principles derived from foundational literature and modern evidence-based practice.
You Might Also Like