Femoral Neck Fracture Case Study: Comprehensive Clinical and Diagnostic Approach
Key Takeaway
Femoral neck fractures are diagnosed through detailed clinical examination revealing pain, inability to bear weight, limb shortening, and external rotation, confirmed by plain radiographs. They are classified using systems like Garden (e.g., Type III for displaced fractures with valgus impaction) and Pauwels (e.g., Type II for significant shear forces) to guide treatment and prognosis.
Femoral Neck Fracture Case: What's the Best Treatment?
Patient Presentation & History
A 78-year-old female presented to the emergency department following a mechanical fall from a standing height. She reportedly tripped over a rug and landed directly onto her right hip. She immediately experienced severe pain in her right groin and hip, rendering her unable to bear weight or move the limb.
Her medical history includes well-controlled hypertension, Type 2 Diabetes Mellitus managed with oral hypoglycemics, and osteoporosis, for which she is on alendronate. She is generally active, living independently, and walks with a cane for ambulation outdoors but is unassisted indoors. Her baseline functional status (pre-injury) was a Modified Harris Hip Score of 85. She takes aspirin 81mg daily for primary cardiovascular prevention. No history of previous falls.
Clinical Examination
On initial assessment, the patient was in moderate distress due to pain.
- Inspection: The right lower limb was noted to be subtly shortened and externally rotated compared to the left. No obvious open wounds or significant abrasions were present. Mild diffuse swelling was observed around the right hip joint.
- Palpation: Significant tenderness was elicited over the right greater trochanter and within the femoral triangle. Palpation of the anterior superior iliac spine, pubic symphysis, and sacroiliac joints did not elicit tenderness.
- Range of Motion (ROM): Active hip ROM was severely restricted and excruciatingly painful in all planes. Passive ROM revealed a fixed external rotation deformity, with any attempt at internal rotation or flexion exacerbating pain. Pseudo-flexion was observed on attempted passive hip extension.
- Neurological Assessment: Sensation to light touch was intact throughout the right lower extremity in all dermatomes (L2-S1). Motor strength was difficult to assess accurately due to pain but was grossly intact in ankle dorsiflexion/plantarflexion and toe movements. Sciatic and femoral nerve function appeared grossly normal.
- Vascular Assessment: Distal pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were strong and symmetric bilaterally. Capillary refill was brisk in the right foot.
The clinical presentation was highly consistent with a right hip fracture.
Imaging & Diagnostics
Plain radiographs of the pelvis and a dedicated cross-table lateral view of the right hip were obtained in the emergency department.
Radiographic Findings:
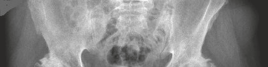
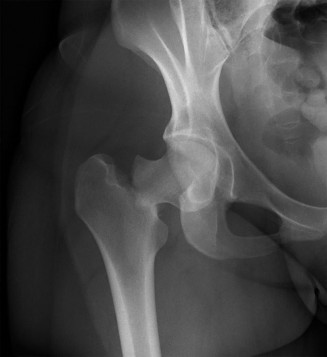
- AP Pelvis: Demonstrated a displaced intracapsular fracture of the right femoral neck. The fracture line was oblique, extending from the subcapital region inferomedially. The femoral head was in valgus with respect to the shaft, and there was approximately 1 cm of superior displacement of the femoral shaft relative to the head. The greater trochanter appeared intact.
- Cross-table Lateral Hip: Confirmed the displacement and provided a clearer view of the fracture morphology, showing significant posterior comminution and extension of the fracture into the basicervical region.
- Classification: Based on the AP pelvis, the fracture was classified as Garden Type III , indicating an incomplete fracture of the femoral neck with valgus displacement and impaction, but still some trabecular continuity on the AP view (though the lateral view suggests more significant displacement). The fracture angle, estimated at approximately 50-60 degrees to the horizontal, placed it in Pauwels Type II , suggesting significant shear forces.

This image depicts a Garden Type III femoral neck fracture with valgus impaction and displacement.
Further Imaging Considerations:
-
CT Scan:
While not routinely indicated for straightforward, clearly displaced femoral neck fractures, a CT scan can be invaluable in specific scenarios:
- To rule out associated acetabular or pelvic ring injuries, especially in higher-energy trauma.
- To evaluate comminution or complex fracture patterns for pre-operative planning, particularly for internal fixation in younger patients.
- To assess for occult fractures when plain radiographs are equivocal but clinical suspicion remains high.
- For pre-operative templating for arthroplasty, though modern digital templating with calibrated plain films is often sufficient.
- MRI Scan: The gold standard for diagnosing occult femoral neck fractures not visible on plain radiographs or CT. It can also be utilized to assess for pre-existing avascular necrosis (AVN) or other bone pathologies, though this is less common in acute trauma. In cases where the diagnosis remains unclear, MRI offers superior soft tissue and bone marrow edema visualization.
- Templating: For arthroplasty, pre-operative templating is crucial. This involves using scaled radiographs (AP pelvis and lateral hip) or digital imaging software to estimate appropriate implant size (femoral stem length and diameter, head size, acetabular component diameter, offset) and predict leg length restoration. This minimizes intraoperative surprises and optimizes component fit and function.
Differential Diagnosis
The acute presentation of hip pain and inability to weight bear after a fall necessitates a focused differential diagnosis, particularly in the elderly population.
| Feature | Femoral Neck Fracture | Intertrochanteric Fracture | Acetabular Fracture | Hip Dislocation (Posterior) |
|---|---|---|---|---|
| Location | Intracapsular, between head and trochanters | Extracapsular, between greater and lesser trochanters | Articular surface of acetabulum | Femoral head displaced from acetabulum |
| Mechanism | Low-energy fall (elderly); High-energy (young) | Low-energy fall (elderly) | High-energy trauma (MVA, fall from height) | High-energy (dashboard injury, fall from height) |
| Clinical Exam | Shortened, externally rotated, painful ROM, groin pain | Shortened, externally rotated (often more), painful ROM, swelling over trochanter | Painful ROM, often associated pelvic instability/other injuries, bruising | Shortened, internally rotated, adducted, flexed, painful ROM, immediate deformity |
| X-ray Appearance | Garden/Pauwels classifications, displacement, impaction, visible fracture line across neck | Extracapsular, often comminuted, involvement of trochanters, may extend to subtrochanteric region | Fracture lines involving acetabular columns/walls, often complex | Femoral head out of acetabulum, empty acetabular fossa |
| Blood Supply Risk | High risk of AVN (intracapsular location) | Low risk of AVN (extracapsular location) | Risk of post-traumatic arthritis, nerve injury (sciatic) | High risk of AVN if reduction is delayed >6-8 hours |
| Treatment Goal | Preserve head vs. replace (age, displacement, activity level) | Stable fixation for early mobilization | Restore articular congruence, stabilize hip, nerve protection | Urgent closed reduction, assess stability, treat associated fractures |
Surgical Decision Making & Classification
Surgical intervention for displaced femoral neck fractures is almost universally indicated due to the high risk of nonunion and avascular necrosis (AVN) if treated non-operatively, especially in active patients. Non-operative management is reserved for extremely frail, non-ambulatory patients with significant comorbidities where the risks of surgery outweigh the benefits, or in truly impacted, stable Garden I fractures in patients with very limited functional demands.
Factors influencing surgical choice:
-
Patient Age and Physiological Status:
- Younger Patients (typically < 60-65 years): The primary goal is to preserve the femoral head due to the long life expectancy and high functional demands. Internal fixation (IF) is the preferred treatment, striving for anatomical reduction.
-
Elderly Patients (typically > 65-70 years):
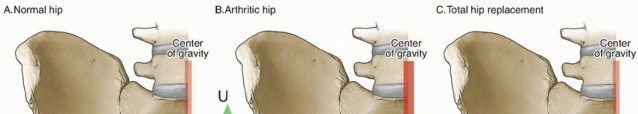
The focus shifts to rapid mobilization and minimizing reoperation rates. The choice is often between hemiarthroplasty (HA) and total hip arthroplasty (THA).
- Hemiarthroplasty (HA): Replacing only the femoral head and neck with a prosthetic component. Suitable for less active elderly patients, those with significant comorbidities, or those with pre-existing hip pathology like severe degenerative changes. Lower dislocation rates and operative time compared to THA.
- Total Hip Arthroplasty (THA): Replacing both the femoral head and neck and the acetabular cartilage with prosthetic components. Preferred for active, physiologically younger elderly patients with good bone stock, or those with pre-existing symptomatic arthritis of the ipsilateral hip. Offers better long-term functional outcomes and lower reoperation rates due to conversion to THA for acetabular erosion, but carries a slightly higher risk of dislocation and longer operative time.
-
Fracture Classification:
-
Garden Classification (Based on Displacement on AP Radiograph):
- Garden Type I (Incomplete/Impacted Valgus): Stable, undisplaced or minimally displaced. Management: Usually internal fixation (screws) to prevent displacement.
- Garden Type II (Complete, Non-Displaced): Complete fracture line but no displacement. Management: Internal fixation (screws) to prevent displacement and promote healing.
- Garden Type III (Complete, Partially Displaced): Valgus impaction with some displacement. Management: Internal fixation for younger patients; HA or THA for elderly. This was the case described.
- Garden Type IV (Complete, Fully Displaced): Complete loss of trabecular continuity, often varus displacement. Management: Internal fixation for younger patients; HA or THA for elderly due to high risk of AVN and nonunion with IF.
-
Pauwels Classification (Based on Fracture Line Angle):
- Pauwels Type I (<30°): Low angle, stable, primarily compressive forces.
- Pauwels Type II (30-50°): Moderate angle, mixed compressive and shear forces.
- Pauwels Type III (>50°): High angle, unstable, primarily shear forces.
- Higher Pauwels types are associated with increased risk of nonunion and AVN, even after internal fixation, due to greater shear forces. This reinforces the decision for arthroplasty in displaced elderly fractures.
-
Garden Classification (Based on Displacement on AP Radiograph):
In this 78-year-old active female with a Garden Type III, Pauwels Type II femoral neck fracture, the decision would likely be in favor of arthroplasty. Given her activity level and lack of pre-existing symptomatic hip arthritis, a Total Hip Arthroplasty (THA) would be a strong consideration, as it offers superior functional outcomes and a lower reoperation rate compared to HA in appropriately selected active elderly patients. If there were significant comorbidities or very poor bone quality, a Hemiarthroplasty might be considered as a less extensive procedure.
Surgical Technique / Intervention
For this case, assuming a decision for Total Hip Arthroplasty (THA) given the patient's activity level and physiological age, the general surgical steps would be as follows:
Pre-operative Planning:
* Review imaging, confirm classification, and identify any specific anatomical considerations.
* Pre-operative templating (digital or manual) to estimate implant sizes and anticipate leg length restoration.
* Discuss anesthetic plan (spinal vs. general) and confirm patient comorbidities are optimized.
* Administer prophylactic antibiotics (e.g., Cefazolin) within 60 minutes of incision.
Patient Positioning:
* The patient is positioned in the
lateral decubitus position
on a specialized operating table with appropriate padding at all pressure points. The operative hip is anterior.
* The limb is draped to allow for full range of motion, particularly internal rotation and extension for exposure, and external rotation and flexion for dislocation.
* Alternatively, a
supine position
can be used for an anterior or direct anterior approach. For this discussion, we'll assume a posterior approach from the lateral decubitus.
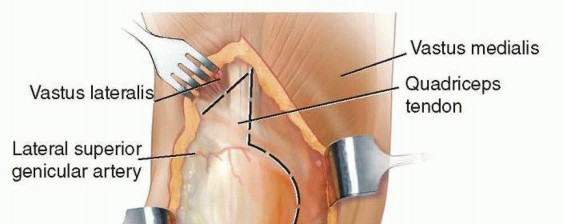
Surgical Approach (Posterior Approach):
*
Incision:
A curvilinear incision is made centered over the posterior aspect of the greater trochanter, extending proximally towards the posterior superior iliac spine and distally along the line of the femur.
*
Dissection:
* The gluteus maximus fascia is incised, and muscle fibers are split bluntly.
* The short external rotators (piriformis, gemelli, obturator internus, quadratus femoris) are identified and released from their insertion on the greater trochanter, often with a small cuff of bone, allowing for later repair. The piriformis tendon is identified, and the sciatic nerve, which lies anterior to it, is carefully protected.
* The capsule is exposed. For a fractured neck, the capsule is often already disrupted or can be incised.
*
Dislocation and Femoral Neck Resection:
* The hip is internally rotated and flexed to dislocate the femoral head. Due to the fracture, the head may already be partially displaced.
* The fractured femoral head is removed from the acetabulum.
* The femoral neck is resected at the level templated pre-operatively, typically 1 cm above the lesser trochanter, with the appropriate neck angle and version.
Acetabular Preparation (for THA):
*
Exposure:
The acetabulum is exposed by retracting the femoral shaft anteriorly.
*
Reaming:
Progressive reaming of the acetabulum is performed using hemispherical reamers, starting with a smaller size and increasing until healthy, bleeding subchondral bone is exposed, and the reamer contacts the medial wall. Care is taken to avoid over-reaming or damaging the anterior and posterior columns.
*
Component Insertion:
The acetabular component (cup) is inserted. In most trauma cases, a cementless cup is preferred for initial stability and long-term osseointegration. Screws may be used for additional fixation if primary stability is suboptimal. The cup is placed in approximately 40-45 degrees of abduction and 15-20 degrees of anteversion.
Femoral Preparation:
*
Broaching:
The femoral canal is prepared by progressive broaching. Broaches are sequentially inserted to create a cavity that matches the shape and size of the chosen femoral stem. This process compacts cancellous bone, improving stability for cementless stems, or prepares the canal for cement mantle for cemented stems.
*
Trial Reduction:
A trial stem and head are inserted. The hip is reduced, and stability, leg length, and offset are assessed. Dynamic assessment through a full range of motion helps identify impingement or instability.
*
Definitive Implant Insertion:
*
Cemented Stem:
If a cemented stem is chosen (e.g., in osteoporotic bone or specific patient profiles), the canal is thoroughly cleaned and dried, bone cement is introduced, and the definitive stem is impacted.
*
Cementless Stem:
If a cementless stem is chosen, the final broach size determines the stem size, and the definitive stem is impacted for a press-fit.
* A definitive femoral head of appropriate size and neck length (based on trial) is then impacted onto the stem trunnion.
Reduction and Closure:
* The hip is reduced, and stability, leg length, and offset are re-assessed.
* The short external rotators and capsule (if intact) are repaired back to the greater trochanter through drill holes or sutures. This repair significantly enhances posterior stability.
* The gluteus maximus fascia and subcutaneous tissues are closed in layers.
* The skin is closed with staples or sutures.
* A sterile dressing is applied.
Internal Fixation (Alternative for Younger Patients / Garden I/II):
For younger patients or Garden I/II fractures, internal fixation with cannulated screws is common.
*
Positioning:
Supine on a fracture table, allowing for traction and image intensification.
*
Reduction:
Gentle traction, internal rotation, and slight abduction are applied to reduce the fracture. Assessment under fluoroscopy is critical. Anatomical reduction is paramount for success. A guide wire can be inserted anteriorly or superiorly into the head to help with reduction and de-rotation.
*
Fixation:
Typically three parallel cannulated screws are inserted percutaneously from the lateral femoral cortex, aiming for the femoral head. An inverted triangle or diamond configuration is often used. The inferior screw should be placed within the calcar for optimal biomechanical stability. Screw placement must avoid articular penetration, which is confirmed with fluoroscopy in multiple planes.
Post-Operative Protocol & Rehabilitation
Immediate Post-Operative Period (Day 0-3):
- Pain Management: Multimodal analgesia (opioids, NSAIDs/acetaminophen, regional blocks) to facilitate early mobilization.
- DVT Prophylaxis: Pharmacological (low molecular weight heparin, fondaparinux) and mechanical (intermittent pneumatic compression devices) prophylaxis.
-
Early Mobilization:
- THA/HA: Weight-bearing as tolerated (WBAT) with assistance from physical therapy (PT) is typically initiated on Post-Op Day 0 or 1.
- Internal Fixation: Weight-bearing status is often restricted (e.g., toe-touch weight-bearing or partial weight-bearing) for 6-12 weeks, depending on fracture stability, reduction quality, and surgeon preference.
- Physical Therapy: Focus on transfers, bed mobility, gait training with an assistive device (walker), and gentle range of motion exercises (ankle pumps, knee flexion/extension).
- Hip Precautions (for posterior approach THA/HA): Avoid hip flexion >90 degrees, adduction past midline, and internal rotation to prevent dislocation. These are typically maintained for 6-12 weeks.
Intermediate Phase (Weeks 1-6):
- Progressive Ambulation: Gradually increase walking distance and decrease reliance on assistive devices.
- Strengthening: Initiate gentle isometric and isotonic strengthening exercises for hip abductors, extensors, and quadriceps.
- Functional Training: Progress with activities of daily living (ADLs), including stair climbing, dressing, and hygiene.
- Wound Care: Monitor incision for signs of infection. Staples/sutures typically removed at 2-3 weeks.
Advanced Phase (Weeks 6-12+):
- Continued Strengthening: Advanced resistance exercises, balance training, and proprioceptive drills.
- Return to Activities: Gradually return to recreational activities, driving (once off narcotics and able to safely operate pedals), and work.
- Discontinuation of Hip Precautions: Often considered at 12 weeks post-op for stable THA/HA. For IF, return to full weight-bearing is based on radiographic signs of union.
- Long-term Monitoring: Regular follow-up with radiographs to monitor implant stability, signs of loosening, or complications.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Urgency: Displaced femoral neck fractures, especially in younger patients, are orthopedic emergencies due to the high risk of avascular necrosis (AVN). Surgery should ideally be performed within 24 hours to optimize outcomes, although the specific "golden window" is debated, 48 hours is commonly accepted as a reasonable target for all patients.
- Anatomical Reduction (for IF): For internal fixation, an anatomical reduction is paramount. Any residual displacement, particularly varus, significantly increases the risk of nonunion and AVN. Use lag screws with a compression washer to achieve interfragmentary compression.
- Optimal Screw Placement (for IF): The inferior screw should be placed in the calcar femorale, providing crucial biomechanical support. Screws should be parallel, centrally placed within the femoral neck and head, and avoid posterior penetration of the femoral neck. Three screws in an inverted triangle or diamond pattern are typically preferred.
- THA vs. HA Decision: In active, physiologically fit elderly patients with displaced femoral neck fractures, THA often yields better long-term functional outcomes and lower reoperation rates compared to HA, particularly if there is pre-existing symptomatic osteoarthritis of the hip. Consider cemented stems in patients with poor bone quality.
- Pre-operative Templating: Essential for arthroplasty to plan implant sizes, achieve optimal leg length, and restore offset, minimizing intraoperative surprises.
- DVT/PE Prophylaxis: Strict adherence to guidelines for deep vein thrombosis and pulmonary embolism prophylaxis is critical in all hip fracture patients.
- Comorbidity Management: Thorough pre-operative medical optimization of comorbidities is vital to minimize perioperative risks.
Pitfalls:
- Missed Occult Fractures: In patients with hip pain after a fall but negative initial X-rays, maintain a high index of suspicion. MRI is the gold standard for diagnosing occult femoral neck fractures.
- Inadequate Reduction (for IF): Residual varus or rotational malreduction significantly increases the risk of nonunion and AVN. This often necessitates revision to arthroplasty.
- Avascular Necrosis (AVN): A significant complication following IF for displaced femoral neck fractures, occurring in up to 30-40% of cases. Risk factors include fracture displacement, delayed surgery, and poor reduction.
- Nonunion: Failure of the fracture to heal, more common with displaced fractures, poor reduction, and inadequate fixation.
- Infection: A devastating complication in arthroplasty. Meticulous surgical technique, strict sterile protocols, and appropriate prophylactic antibiotics are crucial.
- Dislocation (Arthroplasty): Most common with the posterior approach, due to failure to repair the posterior capsule and external rotators, or non-adherence to hip precautions.
- Periprosthetic Fracture: A fracture around the implant, can occur intraoperatively or postoperatively. Risk factors include osteoporosis, implant malposition, and revision surgery.
- Leg Length Discrepancy: Can lead to gait abnormalities, back pain, and patient dissatisfaction. Careful pre-operative templating and intraoperative assessment (direct measurement, fluoroscopy) are essential.
- Vascular/Neurological Injury: Rare but serious complications. Careful surgical technique, particularly around the femoral and sciatic nerves, is imperative.
- Failure to Address Comorbidities: Poorly controlled diabetes, cardiac disease, or malnutrition can lead to increased surgical morbidity and mortality, as well as delayed wound healing.
You Might Also Like