Bilateral Cervical Facet Dislocation: Comprehensive Review of Anatomy, Biomechanics, & Surgical Management
Key Takeaway
Bilateral cervical facet dislocation (BCFD) is a severe cervical spine injury involving complete posterior ligamentous disruption and often significant anterior vertebral subluxation, typically from hyperflexion-distraction forces. It carries a high spinal cord injury risk. Management is primarily surgical, focusing on spinal cord decompression, alignment restoration, and stable fixation to optimize patient outcomes.
Bilateral Cervical Facet Dislocation: Expert Management
Introduction & Epidemiology
Bilateral cervical facet dislocation (BCFD) represents a severe, high-energy injury to the cervical spine, characterized by complete disruption of the posterior ligamentous complex and often associated with significant anterior subluxation of the superior vertebral body on the inferior. These injuries typically result from a combination of hyperflexion and distraction forces, commonly seen in motor vehicle collisions, falls from height, or diving accidents. Due to the profound ligamentous instability, BCFD inherently carries a high risk of spinal cord injury (SCI), with reported neurological deficit rates ranging from 40% to 70% at presentation. The extent of neurological compromise can range from transient radiculopathy to complete tetraplegia, underscoring the urgency and criticality of expert management.
Epidemiologically, cervical spine trauma constitutes a significant portion of all spinal injuries, with facet dislocations accounting for approximately 10-20% of these cases. While unilateral facet dislocations are more common, bilateral dislocations are indicative of greater force and thus more severe instability. The C5-C6 and C6-C7 levels are most frequently involved due to their greater mobility and transitional biomechanics. Prompt diagnosis, meticulous neurological assessment, and timely, appropriate surgical intervention are paramount to optimize patient outcomes and prevent further neurological deterioration.
Surgical Anatomy & Biomechanics
A thorough understanding of cervical spine anatomy and biomechanics is fundamental to managing BCFD. The cervical spine comprises seven vertebrae, each articulating through anterior intervertebral discs and posterior facet (zygapophyseal) joints. The facet joints are true synovial joints, formed by the superior articular process of the vertebra below and the inferior articular process of the vertebra above. Their orientation, typically 45 degrees to the horizontal plane, allows for significant flexion, extension, lateral bending, and rotation, but also dictates their vulnerability to dislocation under extreme loads.
Key supporting structures include:
*
Anterior Longitudinal Ligament (ALL):
Resists extension.
*
Posterior Longitudinal Ligament (PLL):
Resists flexion.
*
Ligamentum Flavum:
Provides elastic stability, resists flexion.
*
Interspinous and Supraspinous Ligaments:
Resist flexion.
*
Capsular Ligaments:
Enclose the facet joints, providing significant stability against translation and rotation.
*
Nuchal Ligament:
Continuation of the supraspinous ligament in the cervical spine, providing posterior stability.
*
Intervertebral Discs:
Contribute significantly to anterior column stability and bear compressive loads.
In BCFD, the mechanism involves severe hyperflexion with simultaneous distraction. This leads to complete disruption of the posterior ligamentous complex, including the capsular ligaments, ligamentum flavum, interspinous, and supraspinous ligaments. The ALL may also be compromised or completely torn. The facet joints become completely dislocated, with the inferior articular processes of the superior vertebra typically lying anterior to the superior articular processes of the inferior vertebra, creating a "perched" or "locked" configuration. This profound instability results in significant anterior translation of the superior vertebral body, often exceeding 50% of the vertebral body width. The integrity of the intervertebral disc is frequently compromised, with a reported incidence of disc herniation in 30-60% of cases. The potential for the herniated disc to retropulse into the spinal canal upon reduction is a critical consideration, particularly in awake or anesthetized closed reduction attempts, and can lead to acute neurological deterioration.
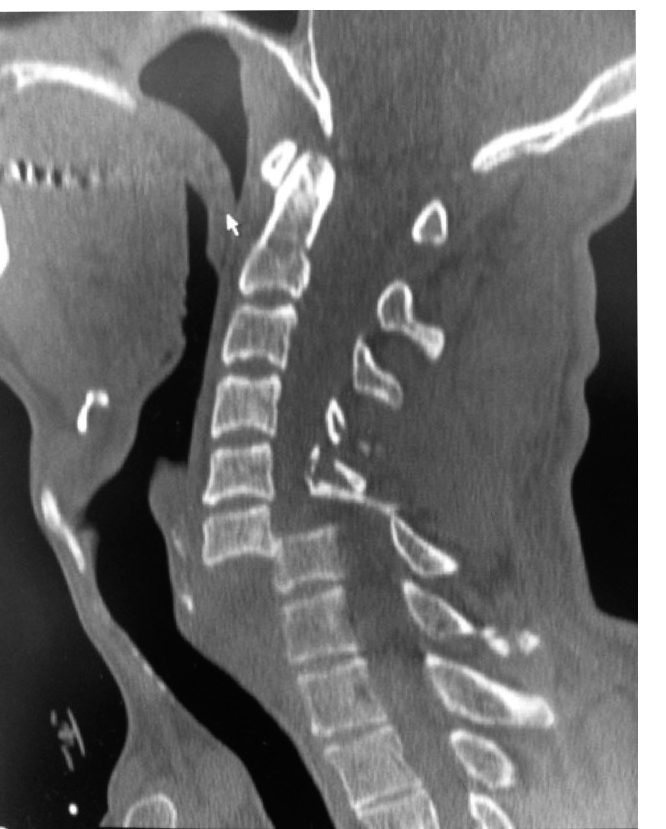
The image below illustrates the complex anatomical relationships in the cervical spine, highlighting structures often implicated in such dislocations.

Indications & Contraindications
Management of BCFD is predominantly surgical, given the inherent instability and high risk of neurological compromise. The primary goals are spinal cord decompression, restoration of spinal alignment, stable fixation, and promotion of fusion.
Operative Indications
- Neurological Deficit: Any new or progressing neurological deficit, or a pre-existing deficit, is a strong indication for urgent surgical intervention to decompress neural elements and stabilize the spine.
- Irreducible Dislocation: If closed reduction attempts are unsuccessful, open reduction and stabilization are mandated.
- Spinal Instability: BCFD, by definition, represents a highly unstable injury. Even if reduced, the extensive ligamentous disruption necessitates surgical stabilization to prevent recurrent dislocation and protect neurological function.
- Significant Disc Herniation: The presence of a significant intervertebral disc herniation retropulsed into the spinal canal, especially if it is compromising the spinal cord or nerve roots, requires anterior discectomy and fusion (ACDF) as the primary approach, often preceding posterior stabilization. Failure to address a herniated disc before posterior reduction carries a substantial risk of acute neurological deterioration.
- Vertebral Artery Injury: While not a direct indication for surgery, if a vertebral artery injury is diagnosed, it requires careful consideration in surgical planning, potentially impacting approach or requiring angiography and endovascular management.
Non-Operative Indications
Non-operative management for true bilateral cervical facet dislocation is exceedingly rare and generally contraindicated due to the severe instability. It may be considered only in specific, unusual circumstances:
*
Medically Unstable Patient:
Patients with severe, life-threatening comorbidities that preclude surgical intervention. In such cases, immobilization (e.g., halo vest) might be employed as a temporizing measure, but the long-term prognosis for stability and neurological recovery is guarded.
*
Complete Quadriplegia without Hope of Recovery:
In rare instances, if a patient has complete, irreversible quadriplegia and severe comorbidities, a discussion with the patient/family may lead to a decision against surgical intervention, focusing on comfort care. This remains a highly controversial area.
Contraindications
- Severe Medical Comorbidities: Absolute contraindications are rare, but severe, uncontrolled systemic illness (e.g., uncontrolled sepsis, massive hemorrhage, severe cardiac failure) that places the patient at unacceptable risk for general anesthesia and major surgery. These are relative contraindications and often necessitate medical optimization before surgical intervention.
- Pre-existing Conditions: Extreme cervical spondylosis or severe ankylosing spondylitis can complicate reduction and fusion, requiring modified surgical techniques, but generally do not contraindicate surgery given the severity of the injury.
Table: Operative vs. Non-Operative Indications for Bilateral Cervical Facet Dislocation
| Indication Category | Operative Management | Non-Operative Management (Rare/Relative) |
|---|---|---|
| Neurological Status | Any neurological deficit (new or progressive), spinal cord compromise | No neurological deficit (highly unlikely with BCFD), severe irreversible neurological injury with poor prognosis and high surgical risk |
| Reduction Status | Irreducible dislocation after closed attempts | Spontaneously reduced and stable (extremely rare for BCFD) |
| Spinal Stability | Gross instability (inherent with BCFD) | Medically unstable patient with contraindication to surgery (focus on palliative care) |
| Disc Integrity | Significant intervertebral disc herniation | No disc herniation (requires MRI verification) |
| Associated Injuries | Vertebral artery injury (may influence timing/approach, but stabilization still needed) | Severe, life-threatening polytrauma overriding immediate spine surgery |
| Patient Factors | Medically fit for surgery | Severe medical comorbidities precluding surgery |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial to prevent iatrogenic injury and ensure a successful outcome.
Imaging
- Plain Radiographs: Lateral, AP, and odontoid views are initial screening tools. The lateral view is essential for assessing alignment, identifying the level of dislocation, and estimating the degree of anterior translation.
- Computed Tomography (CT): A thin-cut cervical CT scan with 3D reconstructions is indispensable. It provides detailed bony anatomy, identifies facet fractures, laminal fractures, and helps characterize the exact nature of the dislocation (e.g., completely locked facets). It is critical for surgical planning.
- Magnetic Resonance Imaging (MRI): MRI is mandatory for assessing soft tissue structures. It identifies intervertebral disc herniation, spinal cord compression, cord edema or contusion, and posterior ligamentous complex disruption. The presence of a significant disc herniation is a game-changer in terms of reduction strategy, often necessitating an anterior approach prior to posterior stabilization.
Neurological Assessment
A detailed baseline neurological examination must be performed and meticulously documented upon admission and prior to any intervention. This includes motor function, sensory function, reflexes, and rectal tone. Serial neurological examinations are crucial to detect any deterioration, particularly during closed reduction attempts or patient repositioning.
Closed Reduction
Closed reduction using Gardner-Wells tongs with gradual traction is often attempted.
*
Awake Reduction:
Considered by some, allowing for continuous neurological monitoring. Incremental weights (5-10 lbs per level, starting at 10-15 lbs, up to 60-80 lbs maximum) are applied with serial lateral radiographs to monitor reduction. Muscle relaxants can be helpful. If neurological deterioration occurs, traction must be immediately removed.
*
Anesthetized Reduction:
Performed under general anesthesia in the operating room, often with intraoperative neurophysiological monitoring (SSEPs, MEPs). This allows for muscle relaxation, which can facilitate reduction, but necessitates careful monitoring due to the inability to assess clinical neurological status.
*
Pre-reduction MRI:
Essential to rule out significant disc herniation prior to closed reduction. If a disc herniation is present, direct open anterior decompression is generally preferred before any attempt at posterior reduction to avoid potentially pushing the herniated disc further into the spinal canal.
Anesthesia Considerations
- Airway Management: In patients with unstable cervical spine injuries, fiberoptic intubation or video laryngoscopy are often preferred techniques to minimize cervical spine movement. In-line cervical stabilization by an assistant is paramount during intubation.
- Neurophysiological Monitoring: Somatosensory evoked potentials (SSEPs) and motor evoked potentials (MEPs) should be used during open reduction and fixation to monitor spinal cord function. A significant persistent decrement in signals during surgery warrants immediate investigation and potential adjustment of surgical maneuvers.
Patient Positioning
- Posterior Approach (Prone): The patient is carefully turned prone using a log-roll technique with in-line cervical stabilization. The head is typically secured in a Mayfield head holder to ensure rigid stabilization and control of cervical alignment. The chest and pelvis are supported on bolsters or a specialized spinal table to allow the abdomen to hang free, reducing intra-abdominal pressure and epidural venous bleeding. C-arm fluoroscopy access must be ensured.
- Anterior Approach (Supine): The patient is positioned supine with the head gently extended and rotated slightly away from the surgical side. A bolster may be placed under the shoulders to enhance cervical lordosis.
Detailed Surgical Approach / Technique
The surgical strategy for BCFD depends critically on the reducibility of the dislocation and the presence of a significant disc herniation. The options include a posterior approach, an anterior approach, or a combined anterior-posterior (360-degree) fusion.
Reduction Strategy
- Closed Reduction First (if no disc herniation): If pre-reduction MRI shows no significant disc herniation, a trial of closed reduction with gradual traction can be performed, either awake or under anesthesia with neuromonitoring. Once reduced, posterior stabilization is typically performed.
- Anterior Decompression and Reduction (if disc herniation): If a significant disc herniation is present, an anterior cervical discectomy and fusion (ACDF) is usually performed first. The discectomy decompresses the spinal canal, allowing for safer subsequent reduction. Reduction can often be achieved with gentle traction and distraction across the disc space after discectomy.
- Open Reduction (if closed reduction fails): If closed reduction is unsuccessful, open reduction is required. This can be performed via a posterior or, less commonly, an anterior approach.
Posterior Surgical Approach and Fixation
The posterior approach is commonly utilized for direct visualization and reduction of locked facets, especially after failed closed reduction or for definitive stabilization of an already reduced BCFD.
- Incision and Exposure: A midline posterior incision is made from approximately one level above to one level below the injury. Subperiosteal dissection using Cobb elevators exposes the laminae, lateral masses, and facet joints bilaterally. Care is taken to stay strictly midline to minimize muscle denervation. The paraspinal muscles are carefully reflected subperiosteally to expose the lateral masses.
- Decompression (if needed): If there are posterior compressing elements (e.g., fractured lamina, significant ligamentum flavum hypertrophy), a laminectomy or laminotomy may be performed.
-
Open Reduction:
- Once the facet joints are exposed, the dislocated facets are identified.
- Reduction maneuvers involve a combination of gentle distraction, translation, and often levering. A laminar spreader or custom reduction instrument can be used to distract the involved levels.
- For unilaterally locked facets, a specifically designed reduction tool (e.g., facet reduction clamp) or a small osteotome can be used to elevate the inferior articular process of the superior vertebra over the superior articular process of the inferior vertebra. For bilateral dislocations, this is performed sequentially or simultaneously if possible.
- Flexion of the neck can sometimes aid in unlocking the facets, followed by extension to reduce them. This must be done with extreme caution and under direct visualization or neuromonitoring.
- A 'push-pull' maneuver, where the assistant applies gentle traction and the surgeon levers the facets, can also be employed.
- Once reduced, the joint is usually "gapped" open posteriorly, indicating the need for robust stabilization.
-
Fixation:
- Lateral Mass Screws: For C3-C6, lateral mass screws are the standard fixation technique. Entry points are typically 1-2 mm medial to the center of the lateral mass and 1 mm superior to the inferior articular facet, angled 30 degrees laterally and 30-45 degrees superiorly to avoid the vertebral artery, nerve root, and facet joint. Screw length is typically 12-18 mm.
- Pedicle Screws: For C7 and sometimes C2, pedicle screws offer superior biomechanical stability. Precise trajectory is critical to avoid vertebral artery or spinal cord injury. Image guidance (navigation) is highly recommended for cervical pedicle screw placement.
- Rods and Bone Graft: Contoured rods are secured to the screws. Autogenous bone graft (local bone, iliac crest) or allograft is placed over the decorticated lateral masses and laminae to promote arthrodesis.
- Facet Fusion: The facets themselves are often decorticated and packed with bone graft after reduction to facilitate a solid fusion.
- Wound Closure: Standard layered closure.
Anterior Surgical Approach and Fixation (for disc herniation or irreducible anteriorly)
An anterior approach is indicated when there is a significant disc herniation or if reduction cannot be achieved from posterior.
- Incision and Exposure: A standard anterior cervical approach is utilized, typically on the right side for C3-C7 levels. The platysma is divided, and the interval between the sternocleidomastoid muscle (lateral) and the strap muscles (medial) is developed. The carotid sheath is retracted laterally, and the trachea/esophagus medially. The prevertebral fascia is incised, and the longus colli muscles are partially elevated from the vertebral bodies to expose the anterior disc space.
- Discectomy and Decompression: After confirming the correct level with fluoroscopy, a complete anterior cervical discectomy is performed. The intervertebral disc and posterior longitudinal ligament are meticulously removed to decompress the spinal cord and exiting nerve roots. Any retropulsed disc fragments are carefully extracted.
- Reduction: With the disc space clear, reduction can often be achieved by applying distraction across the disc space using a Caspar pin distractor or other specialized instrumentation. Gentle manual traction and manipulation can also be employed.
-
Fusion:
- Cage/Graft Insertion: An appropriately sized interbody fusion cage (PEEK or titanium) filled with bone graft (autograft, allograft, or synthetic bone substitute) is inserted into the disc space to restore disc height and lordosis.
- Anterior Plate Fixation: A cervical plate is then applied to the anterior vertebral bodies, spanning the treated segment, securing the cage/graft and providing immediate stability. Screws are placed into the vertebral bodies, ensuring proper length and trajectory to avoid perforating the posterior cortex or adjacent soft tissues.
- Wound Closure: Standard layered closure.
Combined Anterior-Posterior (360-degree) Fusion
A combined anterior-posterior approach is often indicated for high-grade instability, multi-level involvement, or where a single approach does not provide sufficient stability or adequate decompression.
*
Sequencing:
Typically, the anterior decompression and fusion are performed first to address any disc herniation and achieve reduction, followed by posterior instrumentation and fusion to provide robust, circumferential stability. Some surgeons prefer posterior reduction and fixation first, followed by anterior decompression and fusion, particularly if the posterior elements are difficult to reduce or if significant posterior ligamentous complex injury is present. The decision on sequencing is individualized based on patient factors, imaging findings, and surgeon preference.
*
Benefits:
Offers maximal stability and fusion rates, particularly beneficial in patients with severe ligamentous disruption, multiple levels of injury, or those at high risk for pseudarthrosis.
Complications & Management
Despite meticulous surgical technique, complications can arise in the management of BCFD.
| Complication | Incidence | Salvage / Management Strategy | Com Initial Presentation: BCFD is an unstable injury. The following are typical associated presentations and potential complications during initial evaluation and management.
-
Neurological Deficit:
Ranges from radiculopathy to complete tetraplegia.
- Incidence: 40-70% at presentation.
- Management: Immediate spinal immobilization, meticulous neurological assessment, urgent imaging (MRI), and prompt reduction/decompression. Neuromonitoring during closed reduction.
-
Vertebral Artery Injury (VAI):
Can occur due to direct trauma or stretching during dislocation/reduction.
- Incidence: Up to 10-20% in severe cervical trauma, often asymptomatic.
- Management: Pre-operative CTA/MRA if suspected. If identified, consider antiplatelet/anticoagulant therapy or endovascular stenting/coiling depending on severity and symptoms. Caution during surgical approach to avoid further injury.
-
Dural Tear / CSF Leak:
Especially during open reduction or decompression.
- Incidence: 1-5% in spine surgery.
- Management: Intraoperative primary repair with sutures, fascia graft, or dural sealant. Post-operative lumbar drain for 3-5 days. Bed rest.
-
Infection (Surgical Site Infection):
Superficial or deep.
- Incidence: <1% to 5% depending on approach/patient.
- Management: Superficial: wound care, antibiotics. Deep: surgical debridement, IV antibiotics, possibly hardware removal (after fusion).
-
Hardware Failure (Screw pullout, rod fracture, plate fracture):
Can lead to loss of reduction or pseudarthrosis.
- Incidence: 2-10%.
- Management: Revision surgery for hardware removal/replacement, augmentation of fusion, possible extension of fusion. Address underlying pseudarthrosis.
-
Pseudarthrosis (Non-union):
Failure of bony fusion across the instrumented segments.
- Incidence: 5-15%, higher in smokers or with extensive debridement.
- Management: Revision surgery, often with anterior/posterior augmentation, additional bone graft, possible hardware revision. Bone stimulator.
-
Neurological Deterioration During Reduction:
Most critical complication, especially during closed reduction or during initial surgical manipulation.
- Incidence: <1% (closed reduction with disc herniation).
- Management: Immediately cease reduction maneuver, reverse traction, assess neurologically and with imaging (MRI). Re-evaluate surgical plan (e.g., anterior approach first). Intraoperative neuromonitoring is crucial.
-
Dysphagia / Hoarseness (Anterior Approach):
Due to retraction of esophagus/trachea or recurrent laryngeal nerve injury.
- Incidence: Temporary dysphagia common (up to 50%), persistent rare (<5%). Hoarseness rare (<1-2%).
- Management: Temporary: soft diet, steroids. Persistent: swallow study, speech therapy, ENT consultation. Careful surgical technique to minimize retraction.
-
Adjacent Segment Disease:
Degeneration at levels above or below the fused segment.
- Incidence: 2-3% per year.
- Management: Conservative management initially. If symptomatic with neurological compromise, repeat surgery (decompression, fusion, or arthroplasty) at the adjacent level.
-
Malreduction:
Incomplete or incorrect reduction of the facet joints.
- Incidence: Varies, especially in complex cases.
- Management: Immediate intraoperative correction. If identified post-operatively and symptomatic or unstable, revision surgery.
Post-Operative Rehabilitation Protocols
Post-operative management focuses on pain control, progressive mobilization, and protection of the fusion construct. Protocols are typically individualized but follow general principles:
-
Immediate Post-Operative Phase (Days 0-14):
- Pain Management: Multimodal analgesia (opioids, NSAIDs, muscle relaxants) to facilitate early mobilization.
- Immobilization: A rigid cervical collar (e.g., Miami J, Philadelphia collar) is typically worn continuously for 6-12 weeks, except for hygiene. Halo vest immobilization is rarely used for BCFD after stable internal fixation but may be considered for patients with particularly tenuous fixation, severe osteoporosis, or non-compliant patients.
- Early Mobilization: Out-of-bed activity begins on post-operative day 1. Patients are encouraged to ambulate with assistance, focusing on trunk and lower extremity strengthening.
- Wound Care: Standard wound care instructions.
-
Early Rehabilitation Phase (Weeks 2-6):
- Collar Weaning: Gradual weaning of the cervical collar may begin after 6 weeks, depending on radiographic signs of healing and stability, and the extent of the fusion.
- Gentle Range of Motion (ROM): Passive or active-assisted cervical ROM exercises within pain-free limits are initiated. Emphasis on gentle flexion, extension, lateral bending, and rotation.
- Isometric Strengthening: Gentle isometric exercises for cervical paraspinal muscles and deep neck flexors.
- Scapular and Upper Extremity Strengthening: Exercises to improve posture and shoulder girdle strength, avoiding direct cervical loading.
-
Intermediate Rehabilitation Phase (Weeks 6-12):
- Increased ROM and Strengthening: Progression to active cervical ROM exercises. Increased resistance for isometric and isotonic cervical strengthening exercises.
- Core Stabilization: Focus on core muscle strengthening to support spinal stability.
- Proprioception and Balance: Exercises to improve head and neck proprioception.
- Activity Modification: Avoid heavy lifting, twisting, or impact activities. Education on proper body mechanics.
-
Advanced Rehabilitation Phase (Months 3-6+):
- Radiographic Assessment: Follow-up radiographs at 3 and 6 months post-operatively to assess fusion progress. CT scan may be performed if pseudarthrosis is suspected.
- Functional Strengthening: Progression to functional exercises tailored to the patient's daily activities and goals.
- Return to Activity: Gradual return to light recreational activities. Contact sports or activities with high risk of cervical impact are generally discouraged or contraindicated depending on the extent of fusion and surgeon's discretion.
- Long-Term Follow-up: Regular clinical and radiographic follow-up to monitor fusion status, adjacent segment health, and address any long-term complications.
Summary of Key Literature / Guidelines
The management of bilateral cervical facet dislocation has evolved significantly, but several key principles and ongoing debates persist in the literature:
- Timing of Surgery: Early surgical intervention (within 24-72 hours) for cervical spine trauma with neurological deficit is generally favored. Multiple studies and meta-analyses suggest improved neurological outcomes with early decompression and stabilization, particularly in incomplete SCI. The STASCIS trial (Surgical Timing in Acute Spinal Cord Injury Study) provided significant evidence for the benefits of early decompression for neurological recovery.
- Role of Closed Reduction: The utility and safety of closed reduction remain a subject of debate. While traditionally advocated, the critical role of pre-reduction MRI to rule out significant disc herniation is now widely accepted. Attempting closed reduction in the presence of a large retropulsed disc fragment carries a substantial risk of neurological deterioration. If a disc herniation is present, anterior discectomy and decompression are almost universally recommended prior to any posterior reduction attempt.
-
Choice of Surgical Approach (Anterior vs. Posterior vs. Combined):
- Posterior approach is excellent for direct visualization of the facets, open reduction, and robust posterior stabilization, particularly when a disc herniation is not a primary concern or has been addressed. It allows for direct reduction of the locked facets.
- Anterior approach is paramount when a significant disc herniation requires decompression. It also allows for direct reduction of the dislocation by distraction and provides anterior column support.
- Combined anterior-posterior (360-degree) fusion is increasingly recognized as the gold standard for severe BCFD, especially with significant instability, multi-level injury, or in patients at high risk for pseudarthrosis. Systematic reviews often report higher fusion rates and potentially better biomechanical stability with combined approaches, though this must be weighed against increased surgical morbidity and operative time.
- Instrumentation: The use of lateral mass screws (C3-C6) and pedicle screws (C7, C2) for posterior fixation is well-established. Anterior plate and cage constructs are standard for anterior fusion. The choice of fixation depends on the surgeon's experience, bone quality, and specific anatomical considerations.
- Neuromonitoring: Intraoperative neurophysiological monitoring (SSEPs, MEPs) is strongly recommended during all stages of open reduction and fixation to detect spinal cord compromise early and guide surgical maneuvers, especially during reduction.
Current guidelines emphasize a multidisciplinary approach involving neurosurgeons, orthopedic spine surgeons, intensivists, and rehabilitation specialists. Individualized treatment plans based on comprehensive imaging, neurological status, and patient comorbidities remain essential for optimal management of this complex and challenging injury.
Clinical & Radiographic Imaging

