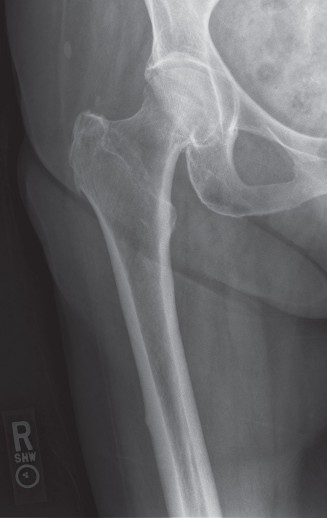
Optimizing the Anteromedial Approach for Distal Femur: Anatomy, Biomechanics, & Applications
Key Takeaway
The anteromedial approach to the distal femur is a versatile surgical corridor for complex fractures and reconstructive needs. It offers direct visualization of the medial femoral cortex, crucial for restoring alignment and stability. This approach provides critical medial column support, particularly in comminuted or osteoporotic fractures, significantly impacting surgical outcomes.
Optimizing the Anteromedial Approach for Distal Two-thirds of the Femur
Introduction & Epidemiology
The anteromedial approach to the distal two-thirds of the femur is a versatile and invaluable surgical corridor for addressing a spectrum of pathologies, primarily focusing on complex fractures and reconstructive needs of the distal femur. While traditionally less utilized than the lateral approach for distal femoral fractures, its utility has been increasingly recognized, particularly with the advent of anatomically precontoured locking plates designed for medial buttress or anterior plating. This approach offers direct visualization and access to the medial femoral cortex, crucial for restoring alignment and stability in fractures with significant medial comminution or those extending into the medial femoral condyle.
Epidemiologically, distal femoral fractures represent approximately 4-7% of all femoral fractures and a smaller proportion of all fractures. These injuries exhibit a bimodal distribution: high-energy trauma in younger individuals and low-energy falls in osteoporotic elderly patients. The latter group, in particular, often presents with metaphyseal comminution and poor bone quality, necessitating robust fixation strategies that may benefit from medial column support. Furthermore, periprosthetic fractures around total knee arthroplasties are a growing concern, and the anteromedial approach can be critical for their management, especially when the fracture pattern or existing implant dictates medial exposure. The strategic selection of this approach can significantly impact surgical outcomes, particularly concerning fracture reduction, stability, and complication rates.
Surgical Anatomy & Biomechanics
A thorough understanding of the regional anatomy is paramount for safe and effective utilization of the anteromedial approach.
Musculature
The quadriceps femoris group forms the bulk of the anterior thigh, comprising the rectus femoris, vastus lateralis, vastus intermedius, and vastus medialis. The vastus medialis is the most medial component, originating from the intertrochanteric line, medial lip of the linea aspera, and medial supracondylar line, inserting into the patella via the quadriceps tendon. It forms a distinct bulge superomedial to the patella, although its definition can be diminished in patients with atrophy. The anteromedial approach typically involves navigating this muscle, either by splitting its fibers or, more commonly for extensile exposure, by retracting it.
Neurovascular Structures
The vital neurovascular structures in this region require meticulous identification and protection:
*
Femoral Artery and Vein:
These vessels transition into the popliteal artery and vein as they pass through the adductor hiatus in the adductor magnus tendon, typically at the junction of the middle and distal thirds of the femur. While the anteromedial approach primarily targets the anterior and medial aspects of the femur, awareness of these deep vessels, positioned posteromedially, is crucial during deep retraction and screw placement.
*
Saphenous Nerve:
This is the largest cutaneous branch of the femoral nerve. It accompanies the femoral artery and vein through the adductor canal (Hunter's canal), located anterior to the artery. It exits the canal proximally to the medial femoral epicondyle, piercing the sartorius fascia to become superficial. It supplies sensation to the skin on the medial side of the leg and foot. The anteromedial approach traverses the region where this nerve emerges; therefore, careful dissection of the sartorius and vastus medialis fascia is essential to prevent iatrogenic injury.
*
Nerves to the Vastus Medialis:
Branches of the femoral nerve supply the vastus medialis. Muscle-splitting approaches through the vastus medialis should be performed parallel to its fibers to minimize denervation.
*
Medial Superior Genicular Artery:
This vessel, originating from the popliteal artery, runs around the medial femoral epicondyle and can be encountered distally.
Bone
The distal two-thirds of the femur encompasses the diaphysis, metaphysis, and condylar segments. The medial femoral condyle is readily palpable. Key landmarks include the medial epicondyle and the adductor tubercle, where the adductor magnus inserts and the adductor canal terminates. The complex anatomy of the distal femur, including the intercondylar notch, provides critical reference points for articular reduction.
Internervous Plane
The anteromedial approach typically utilizes the interval between the vastus medialis muscle and the adductor musculature (adductor longus, adductor magnus), or more commonly, a muscle-splitting approach through the vastus medialis itself, or by retracting the vastus medialis laterally after incising its fascial sheath. A true internervous plane is not consistently utilized in the classical sense across its entire length.
The approach can be conceptualized as:
1.
Proximal:
Between the vastus medialis (innervated by femoral nerve) and the adductor longus/magnus (innervated by obturator nerve). This provides access to the medial femoral shaft.
2.
Distal:
Primarily involving retraction or splitting of the vastus medialis. The adductor canal contents (femoral artery, vein, saphenous nerve) are protected by remaining deep to the vastus medialis and sartorius.
Biomechanics
For distal femoral fractures, particularly those with articular extension (AO/OTA 33-B, 33-C) or severe metaphyseal comminution (33-A3), medial column stability is a critical determinant of successful outcome. While lateral locked plates provide strong lateral support, they are primarily tension-band devices on the lateral side. In cases with medial void or comminution, particularly in osteoporotic bone, the lateral plate may subside into the medial defect, leading to varus collapse or fixation failure. The anteromedial approach facilitates the application of a medial buttress plate , which directly resists varus forces, prevents medial collapse, and provides additional fixation, thereby enhancing construct stability. This concept is particularly relevant in osteopenic bone where primary bone healing is often compromised.
Indications & Contraindications
Indications
The anteromedial approach offers an excellent view of the lower two-thirds of the femur and the medial aspect of the knee joint. Its uses are diverse:
-
Fractures of the Distal Femur:
- Distal Femoral Supracondylar and Intercondylar Fractures (AO/OTA 33-A, 33-B, 33-C): Especially those with medial comminution, medial epicondyle involvement, or requiring medial buttress plating. This is a major use for fractures requiring direct reduction and stabilization of the medial column.
- Periprosthetic Fractures: Around total knee arthroplasty, particularly if medial plate fixation is indicated due to fracture pattern or existing implant.
- Nonunions/Malunions: Of the distal femur, requiring revision fixation and potentially bone grafting.
-
Femoral Shaft Fractures: Distal third femoral shaft fractures, particularly when a medial plate is advantageous or when combined with a lateral approach for complex patterns.
-
Infectious Processes:
- Treatment of Chronic Osteomyelitis: Affecting the distal femur, allowing for debridement and sequestrectomy.
-
Oncologic Conditions:
- Biopsy and Treatment of Bone Tumors: Located in the medial aspect of the distal femur.
-
Soft Tissue Procedures:
- Quadricepsplasty: For severe knee stiffness due to quadriceps contracture or adhesion.
-
Deformity Correction:
- Distal Femoral Osteotomy: For correction of angular deformities (e.g., valgus osteotomy for genu varum, or rarely, varus osteotomy for genu valgum) in the metaphyseal region.
Contraindications
While versatile, the anteromedial approach is not universally indicated:
*
Significant Lateral Soft Tissue Injury:
Open wounds or severe soft tissue compromise on the medial side that would preclude a safe incision and wound closure.
*
Pre-existing Medial Scarring or Infection:
May increase the risk of wound complications.
*
Vascular Compromise:
Severe peripheral vascular disease requires extreme caution during dissection to avoid iatrogenic injury to fragile vessels.
*
Fractures Solely Requiring Lateral Fixation/Exposure:
If the fracture pattern is amenable to lateral plating alone without medial instability, a lateral approach may be sufficient, avoiding the additional morbidity of a medial incision.
*
Severe Edema or Compartment Syndrome:
While not a direct contraindication, immediate decompression and fixation may necessitate an approach that minimizes further soft tissue insult.
Operative vs. Non-Operative Indications
The anteromedial approach itself is an operative technique. Therefore, the indications relate to when surgery via this approach is chosen over non-operative management for specific conditions, primarily distal femoral fractures.
| Condition | Operative Indication via Anteromedial Approach | Non-Operative Indication (for a given fracture type) | Rationale |
|---|---|---|---|
| Distal Femur Fractures | - Displaced intra-articular fractures (AO/OTA 33-B, 33-C) | - Minimally displaced, stable extra-articular fractures (e.g., some 33-A1) | - Restores articular congruity, stability, and alignment; prevents post-traumatic arthritis and malunion. |
| - Displaced extra-articular fractures (AO/OTA 33-A2, 33-A3) with medial comminution or instability requiring buttress plate | - Non-displaced, stable extra-articular fractures in patients unsuitable for surgery | - Medial plate provides crucial stability against varus collapse. | |
| - Periprosthetic fractures requiring medial fixation or exposure. | - Non-displaced stable periprosthetic fractures (rare). | - Addresses unique challenges of fracture around existing implants. | |
| Femoral Shaft Fractures | - Displaced distal third shaft fractures where medial plating is beneficial (e.g., highly comminuted) | - Most shaft fractures are treated with IM nailing or lateral plating. | - Alternative when IM nailing is not feasible or medial plate complements lateral fixation. |
| Nonunions/Malunions | - Symptomatic nonunions/malunions of the distal femur requiring revision and bone grafting. | - Asymptomatic, stable nonunions/malunions in patients unsuitable for surgery (rare). | - Restores union, alignment, and function. |
| Osteomyelitis/Tumors | - Biopsy, debridement, or resection of pathologically confirmed lesions on the medial distal femur. | - Systemic treatment for osteomyelitis without surgical debridement or benign lesions for observation. | - Direct access for definitive diagnosis and treatment. |
| Distal Femoral Osteotomy | - Correction of angular deformity (e.g., genu varum) requiring medial opening or closing wedge osteotomy. | - Mild, asymptomatic deformities. | - Precision in deformity correction and fixation. |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is the cornerstone of a successful outcome, particularly with complex distal femoral pathologies.
Diagnostic Imaging
- Plain Radiographs: Anteroposterior (AP), lateral, and oblique views of the entire femur and knee joint are essential. Contralateral limb films can aid in templating and assessing pre-injury alignment.
- Computed Tomography (CT) Scan: Crucial for detailed assessment of fracture morphology, especially articular involvement, comminution, and bone loss. 3D reconstructions are invaluable for understanding complex intra-articular patterns, planning reduction maneuvers, and guiding screw trajectories.
- Magnetic Resonance Imaging (MRI): Indicated for suspected soft tissue injuries (e.g., ligamentous injuries in acute trauma), tumor evaluation, or osteomyelitis.
- Angiography: Rarely required, but considered if vascular injury is suspected, particularly in high-energy trauma.
Pre-operative Templating
- Plate Selection: Choice of plate (e.g., anatomically precontoured locking compression plate for distal femur, medial distal femoral plate, or general shaft plate) based on fracture pattern, bone quality, and desired construct stability.
- Plate Length and Contour: Templating helps determine appropriate plate length to achieve adequate working length and number of screws. Pre-contoured plates are generally preferred.
- Screw Trajectory: Pre-operative CT can help plan screw placement, especially for avoiding articular penetration or neurovascular structures.
Anesthesia
- General Anesthesia: Typically preferred for muscle relaxation and patient comfort during prolonged procedures.
- Regional Anesthesia (e.g., femoral nerve block, spinal): Can be used as an adjunct for post-operative pain control, or as the primary anesthetic in select cases.
Antibiotic Prophylaxis
- Administer broad-spectrum intravenous antibiotics (e.g., Cefazolin) within 60 minutes prior to incision, following institutional protocols.
Patient Positioning
The patient is
placed supine on the operating table.
The key elements of positioning are:
*
Supine Position:
This allows for good access to the medial aspect of the thigh and knee.
*
Bump/Support:
A small bump or roll placed under the ipsilateral hip can help internally rotate the limb slightly, presenting the medial aspect more prominently and facilitating access.
*
Free Draping:
The extremity must be draped from the iliac crest to the foot so that it can be moved freely during the procedure. This allows for manipulation of the hip and knee to aid in reduction maneuvers and assessment of alignment.
*
Image Intensifier Access:
Ensure the operating table and positioning allow for unobstructed anteroposterior and lateral fluoroscopic views of the distal femur and knee joint.
*
Tourniquet:
A pneumatic tourniquet is often applied high on the thigh. While not always mandatory, its use provides a bloodless field, which can significantly improve visualization, especially for articular reduction and identification of fine neurovascular structures. Its duration should be monitored strictly.
*
Foot Support:
The foot should be supported in a neutral position to prevent unwanted rotation. A well-padded foot holder or an assistant can maintain proper alignment.
Sterile Prep and Drape
- The entire lower extremity, from the iliac crest to the toes, is prepped using an antiseptic solution.
- Sterile draping isolates the operative field while allowing the necessary freedom of movement for the limb.
Detailed Surgical Approach / Technique
Landmarks and Incision
Landmarks:
*
Vastus Medialis Muscle:
A distinct bulge superomedial to the upper pole of the patella. While its inferior portion can be seen and palpated, it often atrophies, making it difficult to identify clearly. Its medial border is the target for dissection.
*
Patella:
Provides a distal reference point.
*
Medial Femoral Epicondyle and Adductor Tubercle:
Key distal bony landmarks, with the adductor tubercle serving as the termination point of the adductor canal.
Incision:
* A longitudinal incision is made on the anteromedial aspect of the thigh, centered over the medial femoral shaft and distal femur.
*
Length:
Typically 15-25 cm, extending from just proximal to the adductor tubercle distally, to proximally cover the extent of planned plate fixation. For distal femur fractures, it often starts at the medial epicondyle and extends proximally for 10-15 cm. For more proximal lesions or longer plates, it can extend significantly further proximally along the course of the femoral shaft.
*
Trajectory:
The incision is generally straight or slightly curved posteriorly towards the hamstrings proximally, running parallel to the medial border of the vastus medialis.
Skin and Subcutaneous Dissection
- The skin and subcutaneous fat are incised. Careful hemostasis is maintained.
- Superficial veins, particularly the great saphenous vein and its branches, may be encountered and should be ligated or cauterized.
- The medial cutaneous nerve of the thigh (a branch of the femoral nerve) and branches of the saphenous nerve supplying sensation to the skin of the medial thigh may be encountered and ideally preserved, though small terminal branches are often unavoidable.
Fascial Incision and Muscle Mobilization
The deep fascia (fascia lata) covering the vastus medialis is incised longitudinally. At this point, two primary strategies exist for gaining access to the femur:
-
Vastus Medialis Splitting Approach:
- A longitudinal incision is made through the vastus medialis muscle fibers, parallel to their orientation. This is a true muscle-splitting approach.
- The vastus medialis is innervated by branches of the femoral nerve that typically enter its superior aspect. Splitting the muscle in its inferior aspect generally minimizes injury to its innervation.
- This technique is suitable for less extensive exposure, such as for isolated medial epicondyle fractures or small tumor biopsies.
- Advantage: Less disruption of the muscle's origin and insertion.
-
Disadvantage:
Provides a narrower surgical window, potentially limiting exposure for complex fracture reduction and plating.
-
Vastus Medialis Retraction Approach (More Common for Distal Femur Fractures):
- This method provides a more extensile and versatile exposure.
- The deep fascia is incised along the medial border of the vastus medialis.
- The vastus medialis muscle is then carefully elevated from its underlying fascia and attachments and retracted laterally.
- As the vastus medialis is retracted laterally, the adductor canal contents are revealed. Meticulous dissection is required to identify and protect the saphenous nerve and the femoral artery and vein (now popliteal vessels more distally). These structures lie deep and slightly posterior to the vastus medialis within the canal. They are generally retracted posteriorly and laterally with the vastus medialis and the medial septum.
- The sartorius muscle is typically retracted medially to aid exposure and protect the neurovascular bundle.
- The adductor magnus muscle , which forms the posterior boundary of the adductor canal, is identified. Its insertion at the adductor tubercle is a key landmark.
-
The
periosteum
on the medial aspect of the femur is then sharply incised longitudinally. A subperiosteal dissection is performed using periosteal elevators to expose the medial and anteromedial surfaces of the femur. This should be done carefully to preserve the periosteal blood supply, especially in osteoporotic patients.
Exposure of the Femur
- With the vastus medialis retracted laterally and the sartorius medially, the medial aspect of the distal two-thirds of the femur is exposed.
-
Broad retractors (e.g., Hohmanns, malleable retractors) are carefully placed subperiosteally to maintain exposure, ensuring protection of the neurovascular bundle posteriorly.
Fracture Reduction
- Articular Reduction (if applicable): For intra-articular fractures, reduction of the articular fragments is the first priority. This is achieved by direct manipulation, temporary K-wire fixation, and careful assessment under direct vision and fluoroscopy.
-
Restoration of Length, Alignment, and Rotation:
- Length: Achieved through traction, ligamentotaxis, or manipulation with bone hooks or clamps.
- Alignment: Coronal and sagittal plane alignment is crucial. Varus/valgus and procurvatum/recurvatum deformities are corrected. Fluoroscopy (AP and lateral views) is essential for monitoring.
- Rotation: Compared to the contralateral limb if possible, or by aligning the posterior condylar axis with the anterior superior iliac spine.
- Temporary Fixation: K-wires, bone clamps (e.g., Verbrugge, pointed reduction clamps), or external fixators can be used to hold the reduction while definitive plating is prepared.
Fixation
The anteromedial approach is particularly well-suited for the application of medial buttress plates , often used in conjunction with a lateral locked plate (hybrid construct) or as a primary medial plate if the fracture pattern permits.
-
Plate Application:
- Anatomically precontoured medial distal femoral locking plates are ideal.
- The plate is applied to the medial or anteromedial aspect of the femur, ensuring proper contouring to the bone.
- Initial fixation can be achieved with non-locking screws proximally and distally to draw the plate to the bone and confirm preliminary reduction and positioning.
-
Screw Placement:
- Distal Fragment: Locking screws are generally preferred in the metaphyseal and epiphyseal fragments for angular stability, particularly in osteoporotic bone. Care must be taken to avoid intra-articular penetration. Fluoroscopy in multiple planes is critical. Bicortical fixation is ideal where possible.
- Proximal Fragment: Both locking and non-locking screws can be used. Non-locking screws achieve compression between the plate and bone, while locking screws provide fixed-angle stability.
- Buttress Function: Screws placed through the medial plate act as a buttress, preventing medial collapse and absorbing varus stress.
-
Adjuncts:
- Bone Grafting: If there is a significant medial metaphyseal defect after reduction, autogenous or allogenous bone graft (e.g., cancellous chips) can be placed to fill the void and promote healing.
- Cerclage Wires: May be used for comminuted shaft fragments, though less common with modern locking plate constructs.
-
Final Assessment:
- Once the plate is secured, stability of the construct is tested.
-
Final fluoroscopic images (AP and lateral) are taken to confirm anatomical reduction, appropriate implant position, and correct screw lengths/trajectories, ensuring no intra-articular penetration.
Wound Closure
- Irrigation: The wound is thoroughly irrigated with copious amounts of sterile saline.
- Hemostasis: Meticulous hemostasis is achieved.
- Fascial and Muscle Closure: The periosteum is often loosely reapproximated. The vastus medialis is allowed to fall back into its anatomical position, and its fascia is reapproximated with absorbable sutures. Care is taken not to strangulate muscle tissue.
- Subcutaneous Closure: The subcutaneous layer is closed with absorbable sutures to obliterate dead space.
- Skin Closure: The skin is closed with staples or non-absorbable sutures, according to surgeon preference.
- Dressing: A sterile dressing is applied.
Complications & Management
Despite meticulous surgical technique, complications can arise following the anteromedial approach and fixation of distal femur pathologies. Vigilant post-operative monitoring and prompt intervention are critical for optimal outcomes.
| Complication | Incidence (Approximate) | Salvage/Management Strategy |
|---|---|---|
| Infection |
Superficial: 2-5%
Deep: 1-3% |
Superficial:
Oral antibiotics, local wound care.
Deep: Surgical debridement, thorough irrigation, intravenous antibiotics (culture-directed), potentially implant removal and staged reconstruction (e.g., external fixator, then reimplantation). |
| Nonunion/Malunion | 5-20% (higher in open fractures, comminuted patterns, osteoporotic bone, smoking) |
Nonunion:
Revision open reduction and internal fixation (ORIF) with stable construct (often medial + lateral plates), bone grafting (autograft/allograft/bone morphogenetic protein), potentially exchange nailing if suitable.
Malunion: Corrective osteotomy and revision fixation if symptomatic and functional deficit. |
| Neurovascular Injury |
Saphenous nerve neuropraxia/paresthesia: 5-15% (often transient)
Vascular injury (femoral/popliteal): <1% |
Saphenous nerve:
Conservative management for paresthesia (reassurance, time), neuropathic pain medication. Rare surgical exploration for persistent, severe neuralgia.
Vascular: Immediate vascular surgical consultation for repair; fasciotomy for limb ischemia/compartment syndrome. |
| Hardware Failure | Plate breakage, screw pullout: 5-10% (often associated with nonunion, poor bone quality) | Revision ORIF, often with a stronger construct (e.g., dual plating), longer plate, or exchange to intramedullary nail. Bone grafting if nonunion present. |
| Knee Stiffness / Arthrofibrosis | Variable, 10-30% (related to prolonged immobilization, intra-articular involvement) | Intensive physical therapy, continuous passive motion (CPM). Manipulation under anesthesia (MUA). Arthroscopic or open arthrolysis for recalcitrant cases. Patellar mobilization. |
| Refracture after Hardware Removal | Rare (<1%) | Revision fixation as per primary fracture management principles. Often avoided by delaying hardware removal until bone remodeling is robust. |
| Heterotopic Ossification (HO) | Clinically significant: 5-10% (higher in TBI/SCI patients, extensive soft tissue trauma) |
Prophylaxis: Indomethacin or single-dose radiation.
Treatment: Surgical excision if mature, symptomatic, and limiting function, typically after 6-12 months. |
| Compartment Syndrome | Very rare (<0.5%) in closed distal femur fractures, higher in high-energy trauma. | Immediate emergent fasciotomy. |
| Wound Dehiscence | 1-3% | Local wound care, secondary closure, or vacuum-assisted closure (VAC) for minor dehiscence. Revision closure for significant dehiscence, potentially with flap coverage. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical fixation itself for achieving optimal functional outcomes. Protocols are tailored to the individual patient, fracture stability, bone quality, and the security of the fixation.
Immediate Post-operative Phase (Days 0-7)
- Pain Management: Multimodal analgesia (opioids, NSAIDs, acetaminophen, regional nerve blocks if applicable) to facilitate early mobilization.
- Deep Vein Thrombosis (DVT) Prophylaxis: Pharmacologic (e.g., low molecular weight heparin) and mechanical (e.g., sequential compression devices) prophylaxis according to institutional guidelines.
- Wound Care: Daily wound checks, dressing changes as per protocol. Monitor for signs of infection.
-
Weight-Bearing (WB):
- Non-Weight Bearing (NWB): Often prescribed initially for 6-12 weeks, particularly for unstable fracture patterns, articular involvement, or poor bone quality, to protect the construct.
- Touch-Down Weight Bearing (TDWB) or Partial Weight Bearing (PWB): May be initiated earlier (e.g., 25% body weight) for stable extra-articular fractures with robust fixation.
- Use of crutches or a walker for ambulation.
-
Range of Motion (ROM):
- Continuous Passive Motion (CPM): May be initiated early (e.g., 0-30 degrees gradually progressing to 90 degrees) particularly for intra-articular fractures, if tolerated and deemed safe by the surgeon. Evidence for routine CPM use is mixed but can aid in pain control and early ROM.
- Gravity-assisted knee flexion/extension: Gentle, active-assisted ROM exercises within tolerated limits, typically avoiding active quadriceps contraction against gravity initially.
- Patellar Mobilization: Gentle, superior-inferior and medial-lateral glides to prevent patellar adhesion and stiffness.
-
Muscle Activation:
- Quadriceps Isometrics (quads sets): Gentle activation without joint motion.
- Gluteal Sets: To maintain hip strength.
- Ankle Pumps: To improve circulation and reduce DVT risk.
Early Mobilization Phase (Weeks 1-6)
- Weight-Bearing: Progress weight-bearing status as per surgeon's discretion, based on radiographic healing (callus formation) and clinical stability. This typically involves progression from NWB to TDWB, then PWB.
- Range of Motion: Gradually increase active and passive knee ROM. Aim for 0-90 degrees by 6 weeks if possible.
-
Strengthening:
- Isometric exercises: Continue quadriceps and hamstring isometrics.
- Assisted knee flexion/extension: With minimal resistance.
- Hip strengthening: Abduction, adduction, flexion, extension with resistance bands.
- Gait Training: Continue with assistive devices, focusing on proper gait mechanics.
Intermediate Phase (Weeks 6-12)
- Weight-Bearing: Progress to full weight-bearing (FWB) once radiographic evidence of union or stable nonunion is apparent, and clinical pain has resolved.
- Range of Motion: Continue to work on achieving full knee ROM.
-
Strengthening:
- Progressive Resistance Exercises (PREs): Gradually increase resistance for quadriceps, hamstrings, and hip musculature.
- Closed Kinetic Chain Exercises: Partial squats, leg presses, step-ups.
- Proprioceptive Training: Balance exercises, single-leg stance.
- Functional Activities: Start incorporating activities of daily living that require more robust knee function.
Advanced Rehabilitation Phase (>12 Weeks)
- Return to Activity: Gradual return to work, recreational activities, and sports. This is highly individualized and depends on the patient's goals, bone healing, and functional recovery.
- High-Level Strengthening: Advanced PREs, plyometrics, agility drills for athletes.
- Sport-Specific Training: For athletes, a structured return-to-sport program is essential.
- Hardware Removal: Considered typically 12-24 months post-operatively, after complete radiographic union and resolution of symptoms, and if hardware is symptomatic. Not routinely performed.
Throughout all phases, close collaboration between the surgeon, physical therapist, and patient is essential. Regular radiographic follow-up is necessary to monitor fracture healing and guide the progression of weight-bearing and activity.
Summary of Key Literature / Guidelines
The management of distal femoral fractures, particularly complex intra-articular patterns, has evolved significantly with advances in implant technology and surgical approaches. The anteromedial approach, especially for medial buttress plating, has gained traction based on biomechanical rationale and clinical outcomes.
- AO Principles: The Arbeitsgemeinschaft für Osteosynthesefragen (AO Foundation) principles emphasize anatomical reduction of articular surfaces, stable internal fixation, preservation of blood supply, and early, safe mobilization. The anteromedial approach facilitates direct articular reduction and provides access for fixation strategies that align with these principles, particularly for medial column reconstruction.
- Biomechanical Studies: Numerous biomechanical studies have demonstrated the superior stability of dual-plate constructs (lateral locked plate + medial buttress plate) compared to a lateral locked plate alone, especially in comminuted or osteoporotic distal femoral fractures. The medial plate effectively resists varus collapse, which is a common mode of failure for isolated lateral locked plates. This evidence strongly supports the use of the anteromedial approach for supplemental medial fixation in high-risk fractures.
-
Clinical Outcomes:
Retrospective and prospective studies have shown favorable clinical outcomes with the use of medial buttress plating via the anteromedial approach for distal femur fractures. These studies often report good union rates, restoration of alignment, and acceptable functional outcomes, particularly in comminuted or osteoporotic fractures that might otherwise be prone to varus collapse or nonunion.
- "Double Plating" Concept: The concept of utilizing a medial buttress plate in addition to a lateral locked plate (often applied through a separate percutaneous or limited lateral approach, or an extensile lateral approach) has gained widespread acceptance for specific fracture patterns (e.g., C3 fractures, severe medial comminution, osteoporotic bone). The anteromedial approach provides the optimal corridor for the medial plate.
- Comparison to Other Approaches: While the extensile lateral approach (often utilizing a subvastus or vastus-splitting technique) remains a workhorse for many distal femur fractures, it often provides indirect access to the medial column. The anteromedial approach offers direct visualization and reduction of medial fragments, making it advantageous when precise medial anatomical restoration or a strong medial buttress is required.
- Evolution of Implants: The development of anatomically precontoured locking plates for the medial distal femur has further optimized this approach. These plates are designed to match the contour of the medial femoral condyle and shaft, facilitating stable fixation with minimal intraoperative bending.
In summary, the anteromedial approach to the distal two-thirds of the femur is a powerful tool in the orthopedic surgeon's armamentarium. Its utility is grounded in a sound understanding of surgical anatomy, biomechanical principles, and supported by a growing body of literature demonstrating its effectiveness in achieving stable fixation and favorable outcomes, particularly in complex distal femoral fractures requiring medial column reconstruction. The decision to employ this approach should be based on careful pre-operative planning, patient-specific factors, and a thorough assessment of the fracture pattern.
Clinical & Radiographic Imaging
You Might Also Like