Comprehensive Arthroscopic Management of Spinoglenoid Cysts and Shoulder Contractures
Key Takeaway
Spinoglenoid cysts frequently arise secondary to labral flap tears, causing suprascapular neuropathy and external rotation weakness. Arthroscopic decompression combined with SLAP repair yields excellent outcomes. Conversely, shoulder contractures, particularly diabetic adhesive capsulitis, demand aggressive management. When physical therapy fails to improve motion within four weeks, early intervention via manipulation under anesthesia or complete arthroscopic circumferential capsular release is indicated to restore joint viscoelasticity and function.
INTRODUCTION TO COMPLEX GLENOHUMERAL PATHOLOGIES
The management of complex glenohumeral pathologies, specifically spinoglenoid cysts and recalcitrant shoulder contractures, requires a profound understanding of shoulder biomechanics, capsuloligamentous anatomy, and advanced arthroscopic techniques. While spinoglenoid cysts present as a focal compressive neuropathy secondary to intra-articular labral defects, shoulder contractures represent a global loss of capsular viscoelasticity. This comprehensive guide delineates the evidence-based surgical management, precise arthroscopic techniques, and postoperative protocols required to optimize clinical outcomes in these challenging patient populations.
SPINOGLENOID CYSTS AND SUPRASCAPULAR NEUROPATHY
Pathoanatomy and Biomechanics
Spinoglenoid cysts are paralabral ganglion cysts that typically form secondary to posterior or superior labral tears (SLAP lesions). The biomechanical mechanism is widely accepted as a "one-way valve" effect. Synovial fluid is forced through the labral defect during glenohumeral motion, accumulating in the spinoglenoid notch.
Because the suprascapular nerve traverses the spinoglenoid notch to innervate the infraspinatus muscle, a cyst in this location causes focal nerve compression. Clinically, this manifests as isolated infraspinatus atrophy, poorly localized posterior shoulder pain, and profound external rotation weakness.
Evolution of Surgical Management
Historically, the treatment of a spinoglenoid cyst with associated suprascapular nerve symptoms focused heavily on open or arthroscopic excision of the cyst itself, often with secondary repair of the labrum. However, contemporary orthopedic literature has shifted the paradigm toward addressing the primary intra-articular pathology: the labral flap tear.
A landmark series by Youm, Matthews, and El Attrache evaluated 10 patients treated with arthroscopic decompression of the cyst combined with labral repair. The clinical outcomes were definitive:
* Patient Satisfaction: 100% of patients were satisfied with their surgical treatment.
* Radiographic Resolution: 8 out of 10 patients demonstrated complete resolution of the cyst on postoperative MRI.
* Neurologic Recovery: 6 out of 6 patients who presented with external rotation weakness regained normal motor function and demonstrated normalized electromyographic (EMG) studies postoperatively.
Clinical Pearl: The primary driver of surgical success in treating spinoglenoid cysts is achieving a watertight, biomechanically stable labral repair. While cyst decompression accelerates neurologic recovery, failure to address the SLAP lesion will inevitably lead to cyst recurrence.
Arthroscopic Surgical Technique: Cyst Decompression and Labral Repair
1. Patient Positioning and Diagnostic Arthroscopy
The patient may be positioned in either the lateral decubitus or beach chair position, depending on surgeon preference. Standard posterior and anterior portals are established. A thorough diagnostic arthroscopy is performed to identify the posterior or superior labral tear.
2. Cyst Decompression
Decompression should be performed safely prior to or during the labral repair.
* Identify the capsulolabral junction adjacent to the labral tear.
* Carefully decorticate the glenoid neck to prepare the bone bed for anchor placement.
* During this preparation, utilize a motorized shaver or a blunt trocar to make a small, controlled puncture through the capsular defect into the cyst.
* Extrusion of thick, gelatinous ganglion fluid into the joint space confirms successful decompression.
3. SLAP / Posterior Labral Repair
Once decompressed, the labrum is mobilized, and the glenoid rim is prepared to bleeding subchondral bone. Suture anchors are placed at the articular margin. Suture shuttling techniques are utilized to pass sutures through the capsulolabral tissue, shifting it superiorly and laterally to obliterate the one-way valve mechanism.
SHOULDER CONTRACTURES AND ADHESIVE CAPSULITIS
Etiology and Pathophysiology
Shoulder contractures manifest as a profound restriction in both active and passive range of motion. The etiology is broadly categorized into three domains:
1. Trauma: Post-traumatic stiffness secondary to fractures or dislocations.
2. Surgery: Postsurgical contractures resulting from prolonged immobilization or overtightening of capsular structures.
3. Inflammation (Adhesive Capsulitis): Idiopathic or systemic-driven fibroblastic proliferation.
A particularly troublesome and recalcitrant form of contracture is associated with diabetes mellitus. The presentation typically involves a gradual progression of idiopathic adhesive capsulitis. Pathophysiologically, this is driven by advanced glycation end-products (AGEs) causing marked thickening, fibrosis, and a profound loss of viscoelastic properties within the joint capsuloligamentous complex.
Clinical Evaluation and Non-Operative Thresholds
Many shoulder contractures are preventable or treatable by intensive, goal-oriented physical therapy focusing on capsular stretching. However, recognizing when conservative management has failed is critical to preventing permanent disability.
Scarlat and Harryman noted that patients who experienced symptoms for more than 6 months were significantly less likely to respond favorably to closed manipulation than patients with posttraumatic or postsurgical stiffness.
Surgical Warning: In our clinical experience, patients presenting with symptoms of more than 4 months’ duration, combined with external rotation of less than 30 degrees and forward flexion of less than 100 degrees, generally respond poorly to physical therapy alone.
These high-risk patients, and all patients with diabetic capsulitis, must be monitored closely. If a patient is not gaining significant motion (defined as 10 to 15 degrees of improvement over 2 weeks) during a 4-week period of dedicated therapy, manipulation under anesthesia (MUA) or surgical intervention should be contemplated early.
The Diabetic Shoulder: A Distinct Clinical Entity
Scarlat and Harryman recommended early prophylactic range-of-motion programs specifically for patients with diabetes, particularly Type 1. When stiffness sets in, early treatment with manipulation and complete arthroscopic capsular release is highly recommended to prevent chronic, debilitating pain.
In their longitudinal study, approximately 20% of diabetic patients required early remanipulation. Interestingly, these patients achieved the best long-term outcomes if the second procedure was performed 3 to 4 years after the initial release.

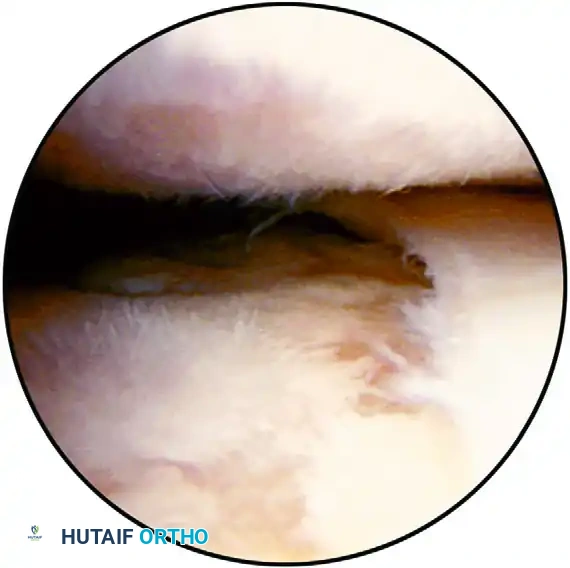
FIGURE 52-52: Arthroscopic débridement and joint space evaluation. In cases of severe contracture or concomitant osteoarthritis, thorough visualization and debridement of the intra-articular space are necessary precursors to capsular release.
Guidelines for the Surgical Treatment of Shoulder Contractures
The management of severe shoulder contractures requires a meticulous, step-wise approach. The following guidelines (adapted from Box 52-4) provide a strategic framework for addressing these difficult problems:
1. Patient Education and Informed Consent
The patient must fully understand the potential surgical procedures. They must be counseled that arthroscopic release may need to be converted to an open technique, and that the postoperative rehabilitation course will be painful, difficult, and requires immense patient compliance.
2. Portal Placement in the Contracted Shoulder
Establishing portals in a severely contracted shoulder is challenging due to the obliterated joint space.
* Initial portals should be placed superiorly: 1.5 cm below the posterolateral acromion and 1.5 cm below the acromioclavicular (AC) joint anteriorly.
* Due to the marked thickening of the contracted capsule, standard blunt obturators may fail to enter the joint. Sharp trocars may be necessary to penetrate the capsule carefully. Extreme caution must be exercised to avoid iatrogenic chondral damage to the humeral head or glenoid.
3. Selective Arthroscopic Releases (Bennett's Criteria)
Arthroscopic release allows for targeted sectioning of specific capsular regions to restore distinct planes of motion. Based on Bennett's biomechanical mapping, selective releases accomplish the following gains:
* Rotator Interval (Coracohumeral Ligament / SGHL): Release restores External Rotation with the arm at the side.
* Inferior Capsule (IGHL Complex): Release restores External Rotation in abduction, Forward Flexion, and Internal Rotation.
* Posterosuperior Capsule: Release restores Internal Rotation and cross-body adduction.
4. Circumferential Release for Diabetic Patients
Patients with diabetes mellitus possess a globally fibrotic capsule. If closed manipulation does not restore full, frictionless motion, a complete 360-degree circumferential arthroscopic release is strictly required. Partial releases in this population uniformly fail.
5. Management of Postsurgical Contractures
Postsurgical contractures (e.g., following an overtightened Putti-Platt or Bankart repair) usually require a combined arthroscopic and open approach. Arthroscopy is utilized to release the posterior and inferior capsule. However, an open subscapularis lengthening (such as a Z-plasty or fractional lengthening) may be necessary anteriorly to restore functional external rotation.
6. Axillary Nerve Protection and Open Conversion
If arthroscopic visualization remains poor despite initial releases, the surgeon must have a low threshold to convert to an open procedure to ensure safety.
Surgical Pitfall (The Danger Zone): When performing an arthroscopic release of the inferior capsule in the 5-o’clock to 7-o’clock position, the axillary nerve is at extreme risk. The surgeon must stay strictly within 1 cm of the glenoid labrum. Carefully use a radiofrequency wand or arthroscopic scissors to separate the capsule from the underlying muscle fibers of the triceps and teres minor to protect the axillary nerve.
7. Postoperative Protocol and Pain Control
The success of a capsular release is entirely dependent on postoperative pain control and immediate mobilization.
* Analgesia: Continuous interscalene nerve blocks are highly recommended for the first 48 to 72 hours to blunt the sympathetic pain response.
* Rehabilitation: Immediate, aggressive passive range of motion (PROM) begins in the recovery room.
* Follow-up: Patients require careful, high-frequency follow-up. If the patient begins to lose motion, early reintervention (within 3 to 4 weeks) with remanipulation or secondary arthroscopic procedures is indicated to break early fibrinous adhesions before mature collagen cross-linking occurs.
CONCLUSION
The operative management of spinoglenoid cysts and shoulder contractures represents two distinct ends of the arthroscopic spectrum. Spinoglenoid cysts require precise, targeted repair of the capsulolabral complex to decompress the suprascapular nerve and restore rotator cuff biomechanics. Conversely, shoulder contractures—particularly those driven by diabetes—demand aggressive, global capsular releases and rigorous postoperative pain management. By adhering to these evidence-based guidelines, orthopedic surgeons can reliably restore function, eliminate pain, and optimize long-term outcomes in these challenging clinical scenarios.
===```
You Might Also Like

