Arthroscopy of the Upper Extremity: Advanced Surgical Principles of the Shoulder and Elbow
Key Takeaway
Diagnostic and surgical arthroscopy of the upper extremity demands a profound understanding of complex joint anatomy, precise portal placement, and advanced instrumentation. This comprehensive guide explores the indications, patient positioning, and specific operative techniques for shoulder and elbow arthroscopy. By mastering these foundational principles, orthopedic surgeons can optimize clinical outcomes, effectively manage intra-articular pathology, and minimize perioperative complications in advanced upper limb procedures.
Introduction to Upper Extremity Arthroscopy
Diagnostic and surgical arthroscopy of the upper extremity has evolved from a purely diagnostic modality into the gold standard for managing complex intra-articular and extra-articular pathology. As orthopedic surgeons have developed profound proficiency with the arthroscope, and as bio-engineering has yielded highly specialized instrumentation, the indications for minimally invasive upper extremity surgery have expanded exponentially.
A thorough, three-dimensional knowledge of regional anatomy, neurovascular proximity, arthroscopic anatomical variations, and pathological findings of each joint is absolutely essential. Mastery of these elements allows the surgeon to perform complex reconstructive procedures successfully while minimizing iatrogenic complications. This masterclass delineates the indications, patient positioning, portal anatomy, specific surgical techniques, and complication management for the shoulder and elbow joints.
Arthroscopy of the Shoulder
Shoulder arthroscopy is the cornerstone of modern sports medicine and upper extremity reconstruction. It provides unparalleled visualization of the glenohumeral joint and subacromial space, allowing for dynamic assessment of joint stability and rotator cuff integrity.
Indications
The indications for shoulder arthroscopy are broad and continually expanding. Primary indications include:
* Diagnostic evaluation: Unexplained shoulder pain, mechanical symptoms, or suspected intra-articular pathology not definitively diagnosed by MRI or MR arthrography.
* Instability: Anterior, posterior, and multidirectional instability (Bankart lesions, capsular laxity).
* Labral Pathology: Superior labrum anterior and posterior (SLAP) tears.
* Rotator Cuff Disease: Partial-thickness tears, full-thickness tears, massive contracted tears, and subscapularis tears.
* Impingement Syndromes: Subacromial impingement, internal impingement, and coracoid impingement.
* Biceps Tendon Pathology: Tenotomy or tenodesis for tendinopathy or partial tearing.
* Degenerative Conditions: Arthroscopic débridement for osteoarthritis, synovectomy for inflammatory arthropathies, and removal of loose bodies.
* Stiffness: Arthroscopic capsular release for adhesive capsulitis (arthrofibrosis).
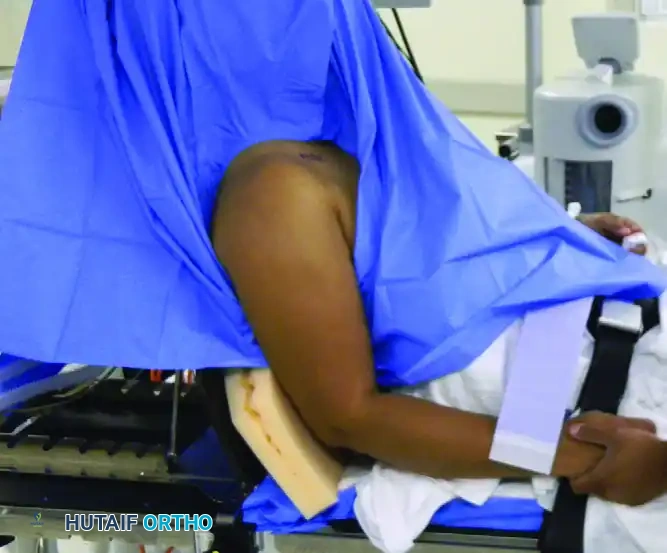
Patient Positioning and Anesthesia
Optimal patient positioning is critical for surgical success, dictating the ease of portal placement, joint visualization, and instrument maneuverability. The choice between the lateral decubitus and beach-chair positions depends on surgeon preference, the specific pathology, and anesthetic considerations.
Lateral Decubitus Position
The patient is placed in the lateral decubitus position with the operative arm suspended in longitudinal and lateral traction (typically 10 to 15 lbs).
* Advantages: Excellent visualization of the glenohumeral joint, particularly the inferior capsule and anterior labrum. The traction expands the joint space, facilitating procedures like Bankart repairs and SLAP repairs.
* Disadvantages: Orientation can be disorienting for novice arthroscopists. There is a risk of traction neurapraxia to the brachial plexus if excessive weight or prolonged surgical times are utilized.
Beach-Chair Position
The patient is seated upright at approximately 45 to 70 degrees. The operative arm is free and can be manipulated dynamically throughout the procedure.
* Advantages: Anatomical orientation is maintained, making it highly intuitive. It allows for seamless conversion to an open approach if necessary. It is particularly advantageous for rotator cuff repairs and subacromial work.
* Disadvantages: The posterior portal can be more challenging to establish.
Surgical Warning: The beach-chair position is associated with the Bezold-Jarisch reflex—a hypotensive, bradycardic event caused by venous pooling in the lower extremities. Meticulous anesthetic monitoring of cerebral perfusion is mandatory.
Hemostasis and Fluid Management
Maintaining a clear visual field is paramount. This is achieved through a combination of controlled fluid pressure and meticulous hemostasis.
- Control of Bleeding: Epinephrine (1 mg per 3 liters of irrigation fluid) is routinely added to induce local vasoconstriction. Hypotensive anesthesia (maintaining mean arterial pressure between 70-80 mm Hg) significantly reduces capillary bleeding.
- Fluid Extravasation: Arthroscopic pumps maintain joint distension but carry the risk of fluid extravasation into the surrounding soft tissues. Prolonged procedures or high pump pressures can lead to massive swelling, potentially compromising the airway (if fluid tracks into the neck) or causing compartment syndrome of the arm.
Portal Placement
Precise portal placement is the foundation of successful shoulder arthroscopy. Poorly placed portals lead to instrument crowding, poor trajectory for anchor insertion, and iatrogenic cartilage damage.
- Posterior Portal: The primary viewing portal. Located approximately 2 cm inferior and 1 cm medial to the posterolateral corner of the acromion. It traverses the "soft spot" between the infraspinatus and teres minor.
- Anterior Portal: Established via an outside-in technique using a spinal needle. It enters through the rotator interval, bounded by the subscapularis inferiorly, the supraspinatus superiorly, and the coracoid medially.
- Anteroinferior Portal (5 o'clock portal): Crucial for anterior instability repairs. It provides the optimal "deadman's angle" for anchor insertion into the anteroinferior glenoid.
- Lateral and Posterolateral Portals: Primarily used for subacromial viewing and working during rotator cuff repairs and subacromial decompression.
- Superior Portal (Neviaser Portal): Located in the supraspinatus fossa, medial to the acromion. Useful for SLAP repairs and superior capsular reconstruction.
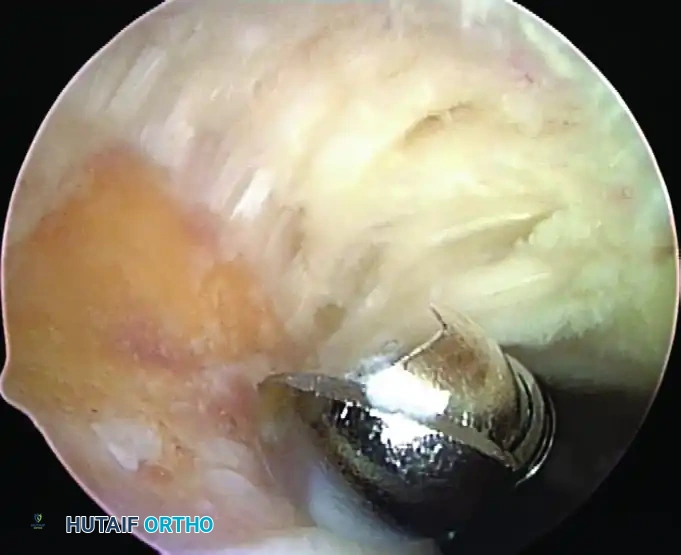
Specific Arthroscopic Surgical Procedures
Repair of Labral Tears and Anterior Instability
Anterior shoulder instability is frequently managed with an arthroscopic Bankart repair. The procedure involves mobilizing the anteroinferior labrum and capsule, decorticating the glenoid neck to promote healing, and securing the capsulolabral complex using suture anchors.
* Biomechanics: The goal is to restore the concavity-compression mechanism of the glenohumeral joint and retension the inferior glenohumeral ligament (IGHL).
Rotator Cuff Tears
Arthroscopic management of rotator cuff tears ranges from simple débridement to complex, massive tear reconstructions.
* Partial Tears: Managed by débridement if <50% of the tendon thickness is involved. If >50%, they are either completed and repaired or repaired in situ (transtendon repair).
* Complete Tears: Require meticulous footprint preparation. Single-row or double-row (suture bridge) techniques are employed. Double-row constructs provide superior biomechanical footprint coverage and pressurized contact area, theoretically enhancing biological healing.
* Massive Contracted Tears: May require extensive releases (coracohumeral ligament release, interval slides) to achieve a tension-free repair. If irreparable, options include superior capsular reconstruction (SCR), partial repair, or reverse total shoulder arthroplasty (RTSA).
Impingement Syndrome and Acromioclavicular Joint
Subacromial decompression (SAD) involves bursectomy, release of the coracoacromial ligament, and an anteroinferior acromioplasty to convert a Type II or III acromion to a flat Type I acromion. For AC joint arthrosis, an arthroscopic distal clavicle excision (Mumford procedure) removes 8-10 mm of the distal clavicle to prevent bony impingement.
Clinical Pearl: When performing a distal clavicle excision, preserve the superior and posterior AC capsular ligaments to prevent iatrogenic anteroposterior instability of the clavicle.
Arthroscopic Capsular Release
Indicated for refractory adhesive capsulitis. The procedure involves a systematic 360-degree release of the capsule, starting at the rotator interval, proceeding to the anterior capsule, inferior capsule, and finally the posterior capsule. Care must be taken at the 6 o'clock position to avoid injury to the axillary nerve, which lies in close proximity to the inferior capsule.
Complications of Shoulder Arthroscopy
While generally safe, complications can occur:
* Neurologic Injury: The axillary nerve is at risk during inferior capsular release and inferior portal placement. The musculocutaneous nerve is at risk during anterior portal placement if directed too medially.
* Chondrolysis: Historically associated with intra-articular pain pumps containing bupivacaine.
* Infection: Rare, but Propionibacterium acnes (Cutibacterium acnes) is an indolent organism frequently implicated in post-arthroscopic shoulder infections.
Arthroscopy of the Elbow
Elbow arthroscopy is technically demanding due to the highly congruent nature of the joint and the intimate proximity of major neurovascular structures. It requires meticulous technique and a profound understanding of cross-sectional anatomy.
Indications
- Removal of Loose Bodies: The most common indication. The elbow is highly susceptible to loose body formation secondary to osteoarthritis or osteochondritis dissecans.
- Osteochondritis Dissecans (OCD) and Panner Disease: Evaluation of capitellar lesions, microfracture, or fragment fixation in the adolescent throwing athlete.
- Throwing Injuries: Valgus extension overload syndrome, requiring resection of posteromedial olecranon osteophytes.
- Arthrofibrosis: Arthroscopic capsulectomy for post-traumatic or degenerative stiffness.
- Degenerative Joint Disease: Osteophyte resection, fenestration of the olecranon fossa, and synovectomy.
- Lateral Epicondylitis (Tennis Elbow): Arthroscopic release of the extensor carpi radialis brevis (ECRB) origin.
Patient Positioning and Anesthesia
Supine Position
The patient is supine with the arm suspended overhead in traction.
* Advantages: Excellent access to both anterior and posterior compartments. Airway management is straightforward.
* Disadvantages: The arm can swing, requiring an assistant to stabilize it.
Prone Position
The patient is prone, with the arm resting over a bolster or arm board, allowing the elbow to flex to 90 degrees.
* Advantages: Exceptional stability. Excellent access to the posterior compartment, which is highly beneficial for valgus extension overload and posterior loose bodies.
* Disadvantages: Airway access is restricted. Anterior portal placement can be slightly more cumbersome.
Lateral Decubitus Position
The patient is lateral, with the arm supported over a post. This offers a compromise, providing good stability and access without the airway concerns of the prone position.
Portal Placement and Neurovascular Anatomy
The fundamental rule of elbow arthroscopy is to maximize joint distension before establishing portals. Injecting 20-30 mL of normal saline into the joint pushes the neurovascular structures away from the capsule, significantly increasing the margin of safety.
- Anterolateral Portal: Established first. Located 3 cm distal and 1 cm anterior to the lateral epicondyle.
- Structure at risk: Radial nerve. Distension moves the nerve from 2 mm to approximately 10 mm away from the portal tract.
- Anteromedial Portal: Located 2 cm distal and 2 cm anterior to the medial epicondyle. Created under direct intra-articular visualization from the anterolateral portal.
- Structure at risk: Median nerve and brachial artery.
- Proximal Anteromedial Portal: Located 2 cm proximal to the medial epicondyle, anterior to the intermuscular septum. Often preferred as it keeps instruments further from the median nerve.
- Posterolateral Portal: Located 3 cm proximal to the olecranon tip, just lateral to the triceps tendon. Used for viewing the posterior compartment.
- Direct Posterior Portal: Located 3 cm proximal to the olecranon tip, directly through the triceps tendon.
Surgical Warning: Always use a "nick and spread" technique for elbow portals. Incise only the skin with a scalpel, then use a blunt hemostat to spread the subcutaneous tissues and muscle down to the capsule to avoid lacerating superficial cutaneous nerves (e.g., medial and lateral antebrachial cutaneous nerves).
Specific Arthroscopic Surgical Procedures
Removal of Loose Bodies
Loose bodies frequently hide in the coronoid fossa, olecranon fossa, and the radiocapitellar joint. A systematic diagnostic sweep of the anterior and posterior compartments is mandatory. Grasping forceps should be used carefully to avoid fragmenting the loose body during extraction.
Panner Disease and Osteochondritis Dissecans (OCD)
In the adolescent overhead athlete, repetitive valgus stress leads to compressive forces on the radiocapitellar joint, causing OCD of the capitellum. Arthroscopy allows for staging of the lesion. Intact but softened cartilage may be treated with retrograde drilling. Unstable lesions require fixation (e.g., bioabsorbable pins) or excision and microfracture to stimulate fibrocartilage healing.
Throwing Injuries and Posterior Impingement
Valgus extension overload results in impingement of the posteromedial olecranon against the olecranon fossa. Arthroscopic treatment involves a limited resection of the posteromedial osteophyte.
* Pitfall: Over-resection of the olecranon must be avoided, as it can increase strain on the ulnar collateral ligament (UCL), exacerbating valgus instability.
Arthroscopic Treatment for Arthrofibrosis
Arthroscopic capsular release of the elbow is highly effective but technically demanding. It involves a sequential release of the anterior capsule (often excising a strip of capsule to prevent recurrence) followed by the posterior capsule. The surgeon must maintain the arthroscope strictly within the joint and use a shaver or radiofrequency wand with the cutting window facing the bone to protect the anterior neurovascular bundle.
Tennis Elbow Release
For recalcitrant lateral epicondylitis, arthroscopic release of the ECRB tendon provides outcomes comparable to open surgery with faster rehabilitation. The capsule is incised just anterior to the lateral epicondyle, exposing the ECRB origin, which is then carefully resected off the footprint. Care is taken not to violate the lateral ulnar collateral ligament (LUCL), which lies immediately posterior and distal to the ECRB origin, to prevent iatrogenic posterolateral rotatory instability (PLRI).
Complications of Elbow Arthroscopy
The complication rate in elbow arthroscopy is historically higher than in the shoulder or knee, primarily due to neurovascular proximity.
* Nerve Injury: The most feared complication. The ulnar nerve is at risk during posteromedial portal placement and medial capsular releases. The radial and posterior interosseous nerves are at risk during anterolateral portal placement and lateral capsular work.
* Infection and Fistula: Synovial fistulas can occur if portals are not meticulously closed, particularly the posterior portals.
* Heterotopic Ossification: Can occur following aggressive capsular releases or débridement. Prophylaxis with NSAIDs (e.g., Indomethacin) or low-dose radiation may be considered in high-risk patients.
Conclusion
Arthroscopy of the upper extremity represents a pinnacle of modern orthopedic surgery, merging profound anatomical knowledge with advanced technical skill. Whether addressing a massive rotator cuff tear in the shoulder or performing a delicate capsular release in the elbow, the surgeon must adhere to strict principles of patient positioning, portal placement, and tissue handling. By respecting the complex biomechanics and neurovascular anatomy of the upper limb, orthopedic surgeons can consistently deliver superior, minimally invasive outcomes for their patients.
You Might Also Like