Biceps Tendon Ruptures: Complete Guide to Repair & Techniques

Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Biceps Tendon Ruptures: Complete Guide to Repair & Techniques. Biceps tendon ruptures are tears, often complete, of the distal biceps tendon, most common in men aged 40-60. They typically result from eccentric muscle contraction, causing noticeable arm deformity and significant loss of flexion and supination strength (up to 40%). Partial tears, common in women, are more painful but lack deformity.
Introduction and Epidemiology
Distal biceps tendon ruptures represent a significant orthopedic injury that primarily affects the dominant extremity of males in the fourth to sixth decades of life. The typical mechanism of injury involves a sudden, unexpected eccentric muscle contraction. This classic presentation often occurs when an extension force is applied to a supinated arm held in 90 degrees of flexion, overwhelming the tensile capacity of the degenerated tendon.
While the initial acute pain often subsides quickly, patients typically present with a noticeable clinical deformity in the anterior brachium. As the biceps muscle contracts and retracts proximally, the characteristic "Popeye" deformity becomes apparent. The degree of this proximal retraction is highly variable and is primarily dictated by the integrity of the lacertus fibrosus (bicipital aponeurosis), which may remain intact and tether the muscle belly distally.
Patients routinely report a profound loss of flexion and supination strength. This functional deficit is especially debilitating in patients who require repetitive or forceful supination, such as mechanics, carpenters, and plumbers. While sharp pain is usually not the predominant chronic complaint, many patients experience persistent fatigue-type pain and cramping within the retracted muscle belly during sustained activities. Biomechanical and clinical studies have consistently revealed a 30 percent reduction in flexion strength and a 40 percent loss of supination strength in untreated complete ruptures.
Partial distal biceps tendon injuries present a distinct clinical entity and are paradoxically often more painful than complete tears. Patients with partial ruptures typically present with insidious or acute-on-chronic pain in the antecubital fossa, which is exacerbated by resisted flexion and supination. Unlike complete ruptures, there is an absence of clinical deformity. These partial tears represent a continuum of tendinopathy and can progress to complete structural failure if left untreated.
The demographic distribution of partial tears differs notably from complete ruptures. Women typically present with partial tears of the distal biceps rather than complete avulsions, and usually at a more advanced age, with a mean age of 63 years. In this specific demographic, a distinct palpable cystic mass can occasionally be identified in the antecubital fossa, representing localized fluid extravasation and chronic bursal inflammation. Partial tears in both genders are typically the result of chronic degeneration without an isolated acute traumatic event. Recognized predisposing factors for tendinopathy and subsequent rupture include the use of anabolic steroids, chronic tobacco use, cubital bursitis, and bony irregularities or osteophytic formations on the bicipital ridge.
Clinical Evaluation and Diagnostic Imaging
In acute cases of a complete distal biceps tendon rupture, physical examination typically reveals a significant amount of ecchymosis in the antecubital fossa and distal brachium. The distal biceps tendon, normally a prominent cord-like structure, is easily palpated in the antecubital fossa; the lack thereof is confirmed by comparing the involved extremity to the contralateral uninvolved side.
While profound local edema and hematoma formation can obscure the visual deformity and make the clinical diagnosis more challenging, specific provocative maneuvers are highly diagnostic. The "hook test" has been established as an exceptionally reliable diagnostic tool. To perform this test, the patient actively supinates the forearm while the examiner attempts to hook the index finger under the lateral edge of the distal biceps tendon, pulling from lateral to medial. An intact tendon allows the examiner to hook the finger securely behind the structure. The hook test has been demonstrated in the literature to possess 100 percent sensitivity and specificity for complete distal biceps tendon ruptures. Other adjunctive tests include the biceps squeeze test and the evaluation of the biceps crease interval.

Magnetic resonance imaging is usually not strictly necessary to make the diagnosis of a complete acute rupture, as the clinical presentation is often pathognomonic. However, advanced imaging is highly valuable in ambiguous cases. If the examiner feels that the distal biceps tendon is intact but the patient exhibits profound weakness and pain, the injury might be located more proximally at the myotendinous junction, or it may represent an isolated partial tear at the insertion site. It is critical to make the anatomical distinction between the common complete avulsion from the radial tuberosity and an injury at the myotendinous junction, as the more proximal myotendinous injuries are best treated nonoperatively.
For partial tears, which occur directly at the radial tuberosity and are usually not associated with ecchymosis or proximal retraction, patients present late with localized pain during resisted flexion and supination. The distal biceps tendon remains palpable but is frequently tender. In these instances, an MRI is essential to aid in the diagnosis, quantify the percentage of tendon footprint involvement, and evaluate for concomitant pathology. The FABS (Flexed, Abducted, Supinated) MRI view is particularly useful for visualizing the distal biceps tendon insertion in its entirety without the magic angle artifact.
The differential diagnosis for anterior elbow pain and weakness should always include cubital bursitis, elbow dislocation, radial head fracture, and entrapment of the lateral antebrachial cutaneous nerve.
Surgical Anatomy and Biomechanics
A profound understanding of the distal biceps anatomy is essential for safe surgical exposure and anatomical footprint restoration. The mean length of the distal biceps insertion footprint on the proximal radius is 22 to 24 mm, and the mean width is 15 to 19 mm. The biceps tendon does not insert as a simple cylindrical cord; rather, it inserts like a ribbon on the ulnar aspect of the radial tuberosity.
The tendon undergoes a complex rotation as it traverses from the musculotendinous junction to the radial tuberosity. The left distal biceps tendon spirals in a clockwise direction, while the right tendon spirals in a counterclockwise direction. This spiraling effect is critical to understand during surgical reattachment to prevent non-anatomic rotation of the tendon, which can alter the supination moment arm.

Recent anatomical studies have further delineated the insertion footprint into distinct zones for the short head and long head of the biceps. The short head typically inserts more distally and anteriorly on the tuberosity, providing a greater mechanical advantage for elbow flexion. Conversely, the long head inserts more proximally and posteriorly, maximizing its moment arm for forearm supination.
A relatively avascular zone exists just proximal to the tendon insertion site. This region of hypovascularity, combined with mechanical impingement against the ulnar border during full forearm pronation, is theorized to be the primary pathoanatomical mechanism driving chronic tendinosis and subsequent rupture.
The lacertus fibrosus, or bicipital aponeurosis, is a crucial fascial structure that typically originates from the distal short head of the biceps tendon and sweeps medially to blend with the fascia of the flexor-pronator mass. When intact, the lacertus fibrosus limits the proximal retraction of the ruptured tendon, tethering it in the antecubital fossa. However, if the lacertus is also torn during the injury, the muscle belly can retract significantly into the middle or proximal third of the brachium, complicating delayed surgical repair.
Indications and Contraindications
The decision to proceed with operative versus nonoperative management depends heavily on the patient's age, functional demands, medical comorbidities, and chronicity of the injury. Surgical repair is generally recommended for acute complete ruptures in active patients to restore full flexion and supination strength and endurance.
| Management Strategy | Primary Indications | Relative Contraindications | Expected Outcomes |
|---|---|---|---|
| Operative Repair | Acute complete ruptures in active individuals; High-demand laborers; Athletes; Partial tears failing conservative therapy | Severe medical comorbidities; Low-demand elderly patients; Active local infection; Chronic tears with fixed retraction (may require graft) | Restoration of near-normal supination and flexion strength; Resolution of fatigue cramping; Cosmetic restoration |
| Nonoperative Management | Sedentary lifestyle; Elderly patients with low functional demands; High surgical risk candidates; Injuries at the myotendinous junction | High-demand occupations (mechanics, carpenters); Athletes requiring overhead strength | 30% permanent loss of flexion strength; 40% permanent loss of supination strength; Persistent cosmetic deformity |
Nonoperative management of complete distal biceps tendon ruptures is generally reserved for patients who are willing to accept the permanent functional deficits. The nonoperative protocol involves a brief period of immobilization for pain control, followed by progressive range of motion and strengthening. While activities of daily living can often be performed without significant difficulty, patients will experience early fatigue during repetitive tasks. Furthermore, nonoperative management of myotendinous junction tears is the gold standard, as these injuries do not involve an avulsion from the bone and heal well with conservative care, whereas surgical repair of muscle tissue is biomechanically inferior and prone to failure.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning requires an assessment of the chronicity of the tear. Acute tears (less than 3 to 4 weeks old) can typically be repaired primarily. Chronic tears (greater than 4 weeks) present a unique challenge due to muscle contracture, tendon degeneration, and obliteration of the anatomical tunnel. The surgeon must be prepared with allograft tissue (such as Achilles tendon, semitendinosus, or fascia lata) if primary excursion to the radial tuberosity cannot be achieved with the elbow in 60 to 90 degrees of flexion.
The patient is typically positioned supine on the operating table with the operative extremity extended onto a radiolucent hand table. Regional anesthesia, such as a supraclavicular or axillary brachial plexus block, is highly recommended for optimal pain control and to provide muscle relaxation, which aids in mobilizing the retracted muscle belly. A non-sterile tourniquet is placed high on the brachium. The arm is prepped and draped in a standard sterile fashion, allowing full mobility of the elbow and forearm. Fluoroscopy should be available in the room to confirm proper seating of cortical buttons and to verify the anatomic location of the radial tuberosity.
Detailed Surgical Approach and Technique
The surgical management of distal biceps tendon ruptures has evolved significantly, with two primary approaches dominating the literature: the single anterior incision approach and the two-incision muscle-splitting approach. The choice of approach often dictates the fixation construct utilized.
Single Anterior Incision Approach
The single anterior incision approach is frequently utilized in conjunction with cortical button and interference screw fixation. A transverse or lazy-S incision is made in the antecubital fossa, approximately 3 to 4 cm distal to the elbow flexion crease.

Careful subcutaneous dissection is paramount to identify and protect the lateral antebrachial cutaneous nerve, which courses laterally in the subcutaneous tissues. The venous structures, including the median cubital vein, are mobilized or ligated as necessary. The deep fascia is incised, and the lacertus fibrosus is identified. If intact, the lacertus is sharply divided to allow mobilization of the retracted biceps tendon.
The internervous plane between the brachioradialis (radially innervated) and the pronator teres (median innervated) is developed. The recurrent radial vessels (the "leash of Henry") are frequently encountered crossing this interval and must be carefully ligated and divided to prevent postoperative hematoma and to allow adequate exposure of the deep structures.

The retracted distal biceps tendon is identified, often encased in a hematoma or pseudosheath. The tendon is grasped with an Allis clamp and mobilized. Adhesions are bluntly swept away using a finger or a blunt elevator to free the muscle belly proximally. The degenerated distal stump of the tendon is sharply debrided back to healthy, organized collagenous tissue.
Two Incision Muscle Splitting Approach
The two-incision approach, originally described by Boyd and Anderson and later modified by Morrey, was developed to minimize the risk of radial nerve and posterior interosseous nerve injuries associated with extensive anterior dissection.
In this technique, a small anterior transverse incision is made to retrieve the tendon and prepare it. A curved hemostat or blunt elevator is then passed through the original anatomical tunnel, sweeping along the ulnar border of the radius and tenting the skin posterolaterally. A second longitudinal incision is made over the tented skin. The extensor digitorum communis and the extensor carpi radialis brevis are identified, and the supinator muscle is bluntly split in line with its fibers. It is critical to split the supinator rather than elevating it off the ulna to minimize the risk of heterotopic ossification and radioulnar synostosis. The radial tuberosity is exposed through this posterolateral window for tendon preparation and fixation.
Tendon Preparation and Fixation Strategies
Regardless of the approach, robust tendon preparation is critical. The debrided tendon end is typically secured using a locking whipstitch technique. High-strength nonabsorbable sutures are utilized.

Biomechanical studies have demonstrated that the cortical button technique provides the highest load to failure and the least displacement during cyclic loading compared to suture anchors or bone tunnels. When utilizing a cortical button, the sutures are passed through the button eyelets.
The radial tuberosity is identified and cleared of remaining soft tissue footprint using a periosteal elevator or curette. The forearm is maximally supinated to deliver the tuberosity into the surgical field and to protect the posterior interosseous nerve, which wraps around the radial neck and moves away from the operative field during supination.
A guide pin is drilled through the center of the anatomic footprint on the radial tuberosity, penetrating both the anterior and posterior cortices. A reamer is then used to create a unicortical socket that matches the diameter of the prepared tendon. The cortical button is passed through the socket and deployed on the posterior cortex of the radius. Fluoroscopy is utilized to confirm that the button has flipped and is resting flush against the dorsal cortex.

The tendon is then tensioned into the socket. To augment the fixation and increase the stiffness of the construct, a tenodesis interference screw can be inserted into the socket alongside the tendon. This dual-fixation technique (cortical button plus interference screw) provides unparalleled biomechanical strength, allowing for early active range of motion. Alternatively, double suture anchors can be utilized, particularly in the two-incision approach, where the tendon is tied directly down to the decorticated footprint.
Complications and Management
Surgical repair of the distal biceps tendon is generally highly successful, but it is associated with a specific set of potentially severe complications. The anatomical complexity of the antecubital fossa places several critical neurovascular structures at risk.
| Complication | Estimated Incidence | Etiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Lateral Antebrachial Cutaneous Nerve Neuropraxia | 5% - 15% | Retractor injury during single anterior approach; Entrapment in scar tissue | Typically transient; Observation and supportive care. Gabapentinoids for neuropathic pain. Rarely requires surgical neurolysis. |
| Posterior Interosseous Nerve Palsy | 1% - 4% | Over-penetration of guide pins/drills; Retractor compression; Failure to fully supinate forearm during tuberosity exposure | Most are neuropraxias that resolve within 3-6 months. Baseline EMG at 6 weeks if no improvement. Tendon transfers if permanent deficit occurs. |
| Heterotopic Ossification / Radioulnar Synostosis | 2% - 7% | Bone debris from reaming; Subperiosteal dissection of the ulna (classic two-incision approach) | Prophylactic Indomethacin in high-risk patients. If synostosis develops causing rigid block to rotation, surgical excision is required after radiographic maturation (typically 6-12 months). |
| Tendon Rerupture | 1% - 2% | Premature return to heavy lifting; Poor tissue quality; Inadequate fixation construct | Revision surgery, almost universally requiring allograft reconstruction (Achilles or semitendinosus) due to tendon retraction and severe degeneration. |
| Superficial Radial Nerve Injury | < 1% | Aberrant retractor placement laterally | Observation. Surgical exploration if painful neuroma develops. |

The development of radioulnar synostosis is a devastating complication that severely limits forearm rotation. The risk of this complication has been drastically reduced by transitioning from the classic Boyd-Anderson ulnar subperiosteal elevation to the Morrey muscle-splitting technique through the supinator. Furthermore, copious irrigation to remove bone debris after reaming the radial tuberosity is mandatory to prevent heterotopic ossification.
Post Operative Rehabilitation Protocols
Modern robust fixation techniques, particularly the use of a cortical button with an interference screw, have allowed for the implementation of accelerated rehabilitation protocols.
Phase I: Immediate Postoperative Phase (Weeks 0-2)
The patient is typically placed in a posterior splint or a hinged elbow brace locked at 90 degrees of flexion with the forearm in neutral to slight supination. The primary goals during this phase are wound healing, edema control, and pain management. Active wrist and hand motion is encouraged immediately to prevent stiffness and promote venous return.
Phase II: Early Range of Motion (Weeks 2-6)
The splint is removed, and the patient is transitioned to a hinged elbow brace. Passive and active-assisted range of motion is initiated. The brace is typically set to allow full flexion but limits extension to protect the repair. The extension block is gradually advanced by 10 to 15 degrees per week until full extension is achieved. Forearm supination and pronation are performed with the elbow flexed at 90 degrees to minimize tension on the repair site.
Phase III: Strengthening (Weeks 6-12)
Once full, painless range of motion is achieved, the brace is discontinued. Progressive isometric strengthening is initiated, followed by light isotonic exercises for both the biceps and brachialis. Emphasis is placed on high-repetition, low-weight exercises to promote tendon remodeling without overloading the insertion site.
Phase IV: Return to Activity (Months 3-6)
Advanced strengthening and sport-specific or work-specific functional training begin. Eccentric loading exercises are gradually introduced. Return to heavy manual labor or unrestricted athletic activity is generally permitted between 4 and 6 months postoperatively, provided the patient has achieved symmetric strength and full range of motion.
Summary of Key Literature and Guidelines
The evolution of distal biceps tendon repair is heavily grounded in biomechanical and clinical literature.
Biomechanical studies by Mazzocca et al. definitively demonstrated that the cortical button technique yields the highest ultimate load to failure (approximately 3200 N) and the least cyclic displacement when compared to suture anchors, bone tunnels, and interference screws alone. This foundational research has driven the widespread adoption of the single-incision cortical button technique.
Clinical outcome studies by Morrey et al. highlighted the functional deficits associated with nonoperative management, establishing the benchmark data of 30 percent loss of flexion strength and 40 percent loss of supination strength. This data remains the primary justification for operative intervention in active individuals. Furthermore, Morrey's modification of the two-incision approach significantly reduced the incidence of radioulnar synostosis by advocating for a muscle-splitting approach through the supinator rather than subperiosteal elevation along the ulna.
Diagnostic literature, notably the work by O'Driscoll et al., validated the Hook Test as a clinical maneuver with 100 percent sensitivity and specificity for complete distal biceps ruptures. This has streamlined the clinical evaluation process, reducing the reliance on costly and time-consuming MRI studies for acute, obvious ruptures, while reserving advanced imaging for partial tears or ambiguous myotendinous junction injuries.
In summary, the precise anatomical restoration of the distal biceps tendon utilizing modern, biomechanically superior fixation constructs provides excellent clinical outcomes, reliable return of strength, and a low profile of major complications when meticulous surgical technique is employed.
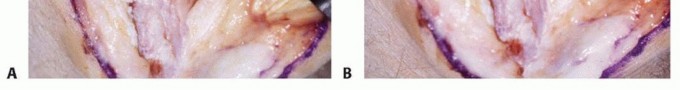
Clinical & Radiographic Imaging







You Might Also Like