Navigating Femoral Shaft Fractures: Diagnosis to Successful Recovery
Key Takeaway
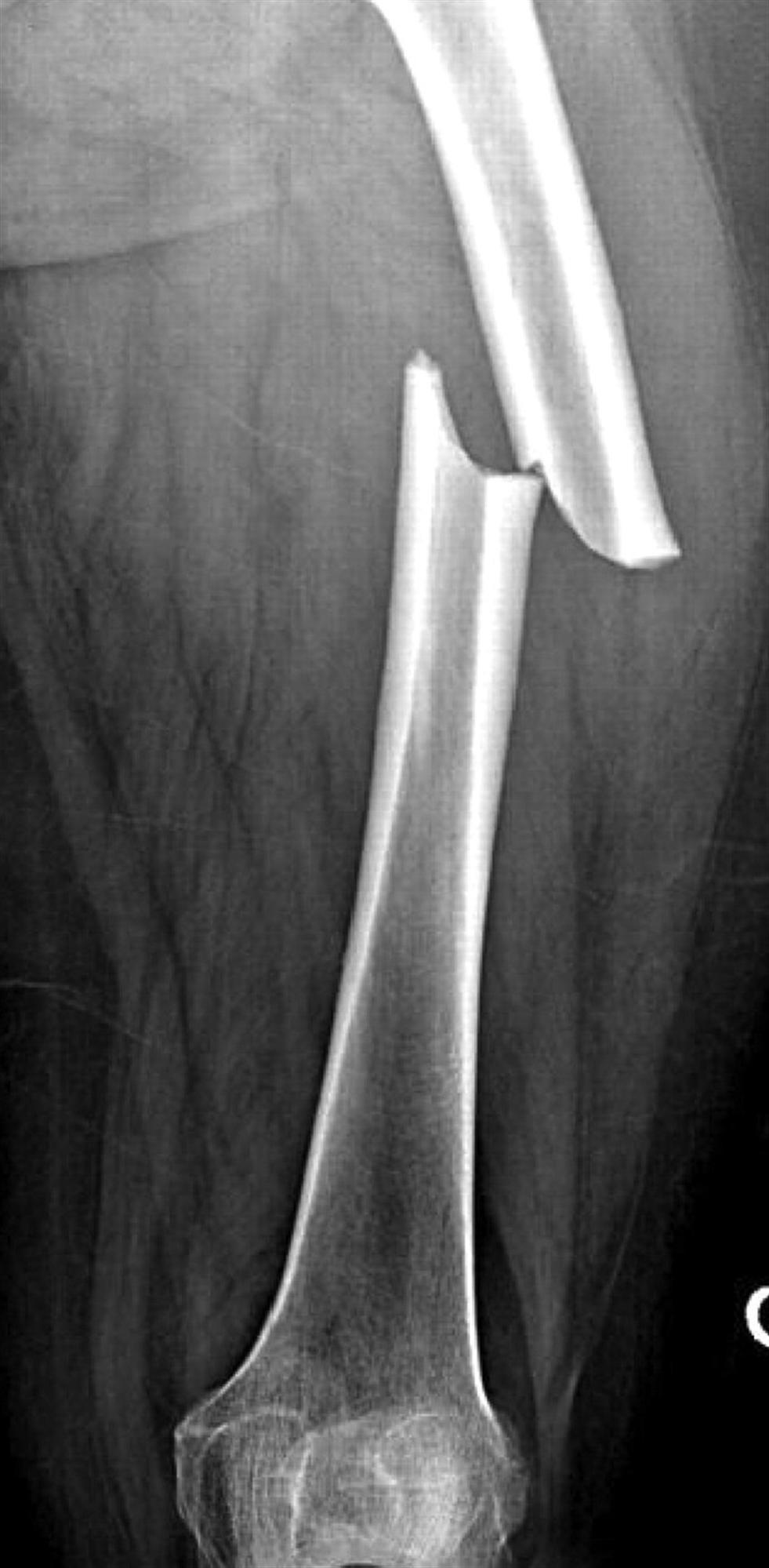
We review everything you need to understand about Navigating Femoral Shaft Fractures: Diagnosis to Successful Recovery. Femoral shaft fractures are life-threatening injuries to the femur's strong, central shaft, often caused by high-energy trauma. Diagnosis primarily involves radiography of the femur and hip. Treatment frequently utilizes intramedullary nailing, boasting a high success rate exceeding 95%. These fractures are relatively common, with an annual incidence of 37.1 per 100,000 persons, and require prompt medical attention.
Navigating Femoral Shaft Fractures: Diagnosis to Successful Recovery
Mohammad Hutaif
(
 ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
Introduction & Epidemiology
Femoral shaft fractures represent high-energy injuries that demand astute diagnostic acumen and precise surgical intervention. These fractures are frequently associated with significant systemic morbidity and mortality, particularly in the polytraumatized patient, necessitating a comprehensive understanding of their presentation, management, and potential sequelae. A multidisciplinary approach, often involving trauma surgeons, intensivists, and orthopedic surgeons, is paramount for optimizing patient outcomes.
The incidence of femoral shaft fractures is approximately 37.1 per 100,000 persons annually, demonstrating a bimodal distribution. In younger patient populations (typically males under 30), these injuries predominantly result from high-velocity trauma, such as motor vehicle collisions, motorcycle accidents, or falls from significant heights. This cohort often presents with isolated femoral shaft fractures but may also sustain associated injuries, including head trauma, thoracic trauma, abdominal trauma, or other orthopedic injuries (e.g., ipsilateral femoral neck fractures, tibial fractures – constituting a "floating knee" injury). The energetic impact required to fracture a healthy adult femur underscores the potential for widespread systemic insult.
Conversely, in the elderly population (over 65 years), femoral shaft fractures are more commonly the result of low-energy mechanisms, such as falls from standing height. This demographic often presents with osteoporotic bone quality, which influences fracture morphology and fixation stability. Additionally, atypical femoral fractures (AFFs) associated with long-term bisphosphonate use are an increasingly recognized entity in this group, often presenting as prodromal thigh pain preceding a complete fracture. Gunshot wounds can also result in femoral shaft fractures, ranging from low-velocity injuries with minimal soft tissue damage to high-velocity blast injuries with extensive comminution and soft tissue devitalization, posing unique challenges regarding infection risk and stabilization. Pathologic fractures, arising from metastatic disease or primary bone tumors, represent another distinct subgroup requiring specialized oncologic considerations in their management.
Prompt initial assessment following Advanced Trauma Life Support (ATLS) protocols is critical. Diagnosis typically commences with plain radiography of the entire femur, extending from the hip joint to the knee joint, to fully characterize the fracture pattern and rule out ipsilateral femoral neck or distal femoral articular involvement. Importantly, an ipsilateral femoral neck fracture coexists in 5-10% of femoral shaft fractures, and failure to identify this concurrent injury can lead to devastating consequences such as avascular necrosis or nonunion of the femoral neck. Computed tomography (CT) scans may be utilized in cases of complex comminution, articular extension, or when assessing polytrauma patients for associated injuries.
Surgical Anatomy & Biomechanics
A thorough understanding of femoral anatomy and biomechanics is fundamental to successful surgical management. The femur is the longest and strongest bone in the body, primarily designed to withstand significant compressive, tensile, and torsional forces.
Gross Anatomy of the Femoral Shaft
The femoral shaft is a cylindrical structure, bowed anteriorly, extending from the lesser trochanter proximally to the supracondylar flare distally. Its diaphysis is characterized by a dense cortical bone, which gradually thins towards the metaphyses. The medullary canal is narrowest in the mid-diaphysis (isthmus) and widens proximally and distally, a critical consideration for intramedullary nail diameter and length. The linea aspera, a prominent longitudinal ridge on the posterior surface, serves as the attachment site for numerous muscles and is an important landmark for nutrient artery entry.
Muscular Attachments and Deforming Forces
The powerful musculature surrounding the femur exerts significant deforming forces on fracture fragments, often dictating displacement patterns and challenging reduction:
*
Proximal Fragment:
*
Abduction and External Rotation:
Gluteus medius and minimus, inserting on the greater trochanter.
*
Flexion:
Iliopsoas, inserting on the lesser trochanter.
*
Distal Fragment:
*
Adduction:
Adductor magnus, longus, brevis.
*
Shortening:
Quadriceps femoris (rectus femoris, vastus lateralis, medialis, intermedius) and hamstrings (semimembranosus, semitendinosus, biceps femoris).
*
Rotation:
Hamstrings.
*
Angulation:
Gastrocnemius (flexion of the knee joint, causing posterior angulation of distal fragment in very distal fractures).
These forces explain the characteristic varus and anterior angulation, and external rotation often seen in midshaft fractures, and the flexion deformity of the distal fragment in supracondylar or very distal shaft fractures.
Vascular Supply
The vascularity of the femoral shaft is predominantly derived from two sources:
1.
Nutrient Artery:
A branch of the profunda femoris artery, it typically enters the femur posteromedially at the level of the linea aspera, supplying the inner two-thirds of the cortex and the medullary canal. This intramedullary blood supply is critical for endosteal healing.
2.
Periosteal Vessels:
These arise from the surrounding muscular arteries (profunda femoris, gluteal arteries, circumflex femoral arteries) and supply the outer one-third of the cortex. Reaming for intramedullary nailing can disrupt the endosteal blood supply, making the periosteal supply even more crucial for early bone healing. However, reaming also creates a biological environment conducive to healing by introducing mesenchymal stem cells and growth factors.
Preservation of both these blood supplies is vital for robust bone healing. Extensive soft tissue stripping during open reduction should be minimized to protect the periosteal blood supply.
Biomechanics of Fixation
Intramedullary nailing (IMN) has become the gold standard for most femoral shaft fractures due to its load-sharing characteristics, which minimize stress shielding and promote secondary bone healing.
*
Load Sharing:
The nail shares axial load with the bone, allowing controlled micromotion at the fracture site, which stimulates callus formation.
*
Stability:
Locking screws provide rotational and angular stability.
*
Biological Environment:
IMN is a relatively "biologically friendly" fixation method as it preserves the periosteal blood supply and minimizes soft tissue dissection. Reaming, while disrupting endosteal blood supply temporarily, also introduces bone marrow elements and growth factors which enhance healing.
Fracture morphology, classified by AO/OTA system (e.g., 32-A/B/C for simple, wedge, complex comminution), influences biomechanical stability and fixation strategy. Simple fractures (transverse, oblique, spiral) generally provide good cortical contact and stability. Comminuted fractures (wedge or complex) often require careful reduction and stable locking mechanisms to prevent shortening or collapse.
Indications & Contraindications
Indications for Operative Management
The vast majority of adult femoral shaft fractures are managed operatively. The goal is to restore alignment, length, and rotation, and to achieve stable fixation, allowing early mobilization and promoting fracture healing.
Absolute Indications for Operative Intervention:
* Displaced, unstable, or irreducible fractures in adults.
* Open fractures (requiring urgent debridement and stabilization).
* Polytrauma patients (early stabilization is crucial for damage control orthopedics and reducing systemic complications like fat embolism and ARDS).
* Vascular injury requiring repair (fixation provides skeletal stability for vascular repair).
* Pathologic fractures (for pain control, stability, and facilitating adjuvant therapies).
* Nonunions or symptomatic malunions.
* Ipsilateral femoral neck and shaft fractures (often termed "floating hip").
* Ipsilateral femoral shaft and tibia fractures ("floating knee").
* Periprosthetic femoral fractures.
Contraindications for Operative Management
Absolute contraindications are rare and primarily related to the patient's physiological status.
Absolute Contraindications:
* Moribund patient unstable for any surgical intervention (though damage control orthopedics principles may apply for temporary stabilization).
* Active, uncontrolled infection at the operative site or systemic sepsis (relative if surgical debridement can address local infection).
Relative Contraindications:
* Severe ipsilateral soft tissue compromise (e.g., extensive degloving, burns), requiring staged management.
* Pre-existing hardware that prevents access for IMN.
* Extreme obesity (can make surgical access and fluoroscopy challenging).
Operative vs. Non-Operative Indications
| Indication Type | Operative Management
All FSFs except:
* Children with certain stable, undisplaced fractures or fractures with acceptable angulation.
* Patients with extremely grave medical comorbidities, where the risks of surgery clearly outweigh the benefits of stabilization.
* Specific palliative care scenarios. | Non-Operative Management | Non-operative management is reserved for select circumstances. In adult femoral shaft fractures, this is most rare and typically limited to:
*
Extremely ill or nonambulatory patients:
Where the risks of surgery outweigh the benefits of definitive internal fixation, and external support provides adequate comfort and care.
*
Palliative care settings:
Where the primary goal is comfort.
*
Certain incomplete or stress fractures:
Without displacement and with minimal symptoms.
* Historically, skeletal traction was used, but it's largely obsolete for definitive management in adults due to prolonged hospitalization, increased complications, and inferior outcomes compared to IMN. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is the cornerstone of a successful outcome in femoral shaft fracture fixation.
Pre-Operative Planning
-
Imaging Review:
- Plain Radiographs: Obtain AP and lateral views of the entire femur, including the hip and knee joints. This is crucial for assessing fracture morphology (AO/OTA classification), location, comminution, and identifying ipsilateral injuries (e.g., femoral neck fracture). Obtain radiographs of the contralateral femur for templating nail length and diameter.
- CT Scan: Indicated for highly comminuted fractures, articular extension, or when a femoral neck fracture is suspected but not clearly visualized on plain films. It provides detailed information on fracture pattern, bone loss, and helps guide reduction strategies.
- Angiography: If clinical suspicion for vascular injury is high (e.g., absent pulses, expanding hematoma, pulsatile bleeding), especially with gunshot wounds or severe crush injuries.
-
Patient Assessment:
- Systemic Review: Address any associated injuries (head, chest, abdomen, pelvis, other extremities) in polytrauma patients. Optimize patient physiology (respiratory, cardiovascular status) before definitive fixation.
- Soft Tissue Envelope: Assess for open wounds, degloving injuries, severe swelling, or blistering. Stage management if necessary (e.g., external fixation followed by delayed definitive IMN).
-
Implant Selection:
- Intramedullary Nail (IMN): Select an appropriate nail type (e.g., antegrade vs. retrograde, titanium vs. stainless steel). Consider nail diameter (based on canal width, often estimated from contralateral femur or pre-operative CT), length (from trochanteric entry point to just proximal to the physis or epiphysis), and locking options (static vs. dynamic, multi-planar screws).
- Plate Fixation: Rarely indicated for diaphyseal fractures, but may be considered for highly comminuted distal/proximal metaphyseal-diaphyseal junction fractures not amenable to IMN, or for periprosthetic fractures.
-
Surgical Strategy:
- Entry Point: Antegrade nails can use piriformis fossa, greater trochanter tip, or trochanteric entry portals. Each has specific indications and potential complications (e.g., piriformis entry for certain proximal fractures, trochanteric for ease of access and reducing trochanteric pain). Retrograde nails typically enter the intercondylar notch.
- Reduction Techniques: Plan for manual traction, fracture table, femoral distractor, clamps, or intramedullary joystick techniques.
- Reaming vs. Unreamed: Reaming allows for larger diameter nails, which are biomechanically stronger and typically promote faster healing but can increase intramedullary pressure and potentially systemic insult (fat embolism). Unreamed nails are often used in open fractures or polytrauma with pulmonary compromise to minimize systemic inflammatory response.
Patient Positioning
Proper patient positioning is critical for successful reduction, fixation, and fluoroscopic imaging. The most common positions are supine on a fracture table or supine on a radiolucent table.
1. Supine on a Fracture Table (Most Common for Antegrade Nailing)
- Advantages: Provides continuous longitudinal traction, which aids in reducing fracture shortening and can help align fragments. Facilitates C-arm imaging.
-
Setup:
- The patient is placed supine on the fracture table.
- The affected leg is placed in a traction boot or skeletal traction (distal femur/tibia pin) with appropriate padding. Counter-traction is applied via a well-padded perineal post.
- The contralateral leg is abducted and flexed at the hip and knee, placed in a padded leg holder to allow unimpeded C-arm access to the injured femur.
- Ensure adequate padding at all pressure points (sacrum, heels, perineum) to prevent pressure sores or nerve palsies.
- The entire trunk and pelvis should be supported to prevent rotation and maintain spinal alignment.
- C-arm Positioning: The C-arm can be brought in from the contralateral side or from the foot of the bed, allowing for both AP and lateral views of the fracture site and the entire femur, including the entry point and locking screws.
2. Lateral Decubitus (Less Common for Antegrade Nailing, or for Obese Patients)
- Advantages: Allows easier access to the greater trochanter, particularly in obese patients. Reduces dependency on a traction table.
-
Setup:
- The patient is positioned in a true lateral decubitus position on a standard operating table, with the injured side up.
- Pillows are placed between the knees. The torso is supported to prevent rolling.
- C-arm Positioning: Requires careful manipulation for AP and lateral views, often necessitating oblique projections.
3. Supine on a Radiotranslucent Table (For Retrograde Nailing or Free-Hand Reduction)
- Advantages: Allows easier manipulation of the extremity for reduction and for ipsilateral concomitant injuries (e.g., floating knee). Ideal for retrograde nailing.
-
Setup:
- The patient is placed supine on a standard operating table.
- The injured leg is draped free to allow for full range of motion of the hip and knee during reduction and nailing.
- C-arm Positioning: The C-arm can be positioned to visualize the entire femur, typically brought in from the side.
Regardless of positioning, correct assessment of rotational alignment is paramount. This can be assessed clinically (patella alignment, foot alignment relative to ASIS) or with fluoroscopy (cortical step-off, lesser trochanter visibility). Pre-operative assessment of the contralateral leg can aid in rotational comparisons.
Detailed Surgical Approach / Technique: Intramedullary Nailing
Intramedullary nailing (IMN) is the preferred treatment for nearly all adult femoral shaft fractures. The choice between antegrade and retrograde nailing depends on fracture location, associated injuries, patient morphology, and surgeon preference.
Antegrade Intramedullary Nailing (AIMN)
This is the most common technique for midshaft and proximal shaft fractures.
1. Incision and Entry Portal
- Patient Position: Typically supine on a fracture table with traction, or lateral decubitus.
- Incision: A longitudinal incision (5-10 cm) is made centered over the tip of the greater trochanter. The skin, subcutaneous tissue, and fascia lata are incised. The abductor muscles (gluteus medius and minimus) are split bluntly in line with their fibers, or partially released from the tip of the greater trochanter.
-
Entry Point Confirmation:
Fluoroscopy is used to identify the optimal entry point.
- Piriformis Fossa Entry: Traditionally preferred for proximal fractures to optimize nail trajectory. Located just medial to the tip of the greater trochanter, at the junction of the superior and medial quadrants. Requires care to avoid damaging the piriformis tendon and potentially causing osteonecrosis of the femoral head (ONFH), though this risk is now recognized as minimal with appropriate technique.
- Greater Trochanteric Entry: More lateral entry, through the tip of the greater trochanter. Newer nail designs with more angulated proximal bends allow for this more lateral entry, reducing piriformis fossa morbidity. It is often technically easier, has a lower incidence of hip pain post-op, and is associated with reduced risk of ONFH.
- Awl/Reamer Insertion: A large curved awl or specific trochanteric entry reamer is used to create an opening into the medullary canal. Ensure correct angulation of the awl/reamer to follow the femoral axis.
2. Guide Wire Insertion and Medullary Canal Preparation
- Guide Wire Insertion: A ball-tipped guide wire is carefully advanced down the femoral canal, ensuring it crosses the fracture site and enters the distal fragment. Fluoroscopy (AP and lateral views) confirms correct guide wire position and trajectory. Careful manipulation is required to navigate comminuted fragments without creating false passages.
-
Fracture Reduction:
Once the guide wire is across, reduction maneuvers begin.
- Traction: Provided by the fracture table, adjusted to restore length.
- Manual Manipulation: External pressure or internal joystick maneuvers with the guide wire or a reduction tool.
- Table Controls: Fine-tuning traction, rotation, and angulation.
- Femoral Distractor: Can be applied on the lateral side to aid in length restoration and distraction.
- Open Reduction (Limited): If closed reduction fails, a small incision can be made at the fracture site to insert reduction clamps (e.g., Verbrugge clamps) or joystick K-wires to achieve anatomical alignment. Minimize soft tissue stripping.
- Reaming (if applicable): If a reamed nail is planned, flexible reamers are passed sequentially over the guide wire, starting with a size smaller than the guide wire and increasing by 0.5-1.0 mm increments until cortical chatter is felt or the desired canal diameter is achieved. Reaming creates a larger canal, allowing for a stronger, larger-diameter nail, but also produces biological debris that contributes to healing. Unreamed nails avoid the systemic inflammatory response of reaming, often preferred in patients with pulmonary compromise or open fractures.
3. Nail Insertion
- Nail Selection: Choose a nail length and diameter determined during pre-operative planning. The nail should be long enough to provide adequate fixation in both proximal and distal fragments, typically extending to 1-2 cm proximal to the physis of the distal femur. The diameter should match the reamed canal.
- Insertion: The selected IMN is attached to the insertion handle. It is then carefully advanced over the guide wire, past the fracture site. Gentle rotational and axial force may be needed. Avoid forceful insertion, which can lead to iatrogenic fracture or implant malposition. Fluoroscopy monitors nail progression.
- Final Seating: The nail is advanced until its proximal end is flush with or slightly proud of the entry point, or as per manufacturer's recommendations, ensuring no proximal prominence that might cause trochanteric pain.
4. Proximal Locking
- Purpose: Provides rotational and angular stability to the proximal fragment.
- Technique: A targeting jig attached to the insertion handle guides the drilling for proximal locking screws. Ensure the jig is securely attached and properly aligned. Drill holes through the cortex, implant, and contralateral cortex. Insert appropriately sized locking screws. Fluoroscopy confirms screw position and length. If a jig is not available or reliable, free-hand locking using fluoroscopy can be performed, requiring expertise to align the drill bit with the nail holes.
5. Distal Locking
- Purpose: Provides rotational and angular stability to the distal fragment and prevents shortening. This is often the most challenging step.
-
Technique:
- Targeting Jig: Some nail systems offer a distal targeting jig, but these are often less accurate than proximal jigs due to the nail's distal curve.
- Free-Hand Technique: This is commonly employed. The C-arm is positioned for a perfect circle view of the distal locking holes. The limb is internally or externally rotated as needed. A drill bit is then guided visually and with fluoroscopic feedback to pass through the cortex, nail hole, and contralateral cortex.
-
Image Intensifier (
): The C-arm image intensifier is critical here to ensure precise alignment. Oblique fluoroscopic views (often called "perfect circles") are used to confirm the drill bit is perfectly centered in the nail hole before final drilling. - Screw Insertion: Once all distal holes are drilled, appropriately sized locking screws are inserted and tightened.
- Confirm Alignment: Before distal locking, ensure final length, rotation, and alignment are acceptable. Rotational assessment is critical: compare patella alignment, foot position, or use cortical step-off signs on fluoroscopy.
6. Final Assessment and Closure
- Image Confirmation: Obtain AP and lateral fluoroscopic views of the entire femur to confirm satisfactory fracture reduction, nail position, and screw placement.
- Wound Irrigation and Closure: Thoroughly irrigate the surgical site. Close the fascia lata, subcutaneous tissues, and skin in layers. Apply a sterile dressing.
Retrograde Intramedullary Nailing (RIMN)
RIMN is an alternative technique indicated for certain fracture patterns and patient comorbidities.
1. Indications
- Distal femoral shaft fractures (junctional or supracondylar extension).
- Ipsilateral tibial shaft fractures ("floating knee").
- Ipsilateral acetabular fractures (allowing easier access without repositioning).
- Obese patients where antegrade access is difficult.
- Polytrauma patients with head or chest injuries where supine positioning is preferred to avoid respiratory compromise associated with hip flexion.
- Pathologic fractures of the distal femur.
2. Incision and Entry Portal
- Patient Position: Supine on a standard radiolucent table with the knee flexed to 90 degrees, allowing free leg manipulation.
- Incision: A longitudinal incision (typically 3-5 cm) is made distal to the patella, either medial or lateral parapatellar, or a transpatellar approach.
- Entry Point: The patella is retracted. The entry point is located in the intercondylar notch, just anterior to the origin of the posterior cruciate ligament (PCL). An awl or drill is used to open the canal, directing the trajectory proximally along the femoral axis. Avoid damaging the PCL and the articular cartilage of the femoral condyles.
3. Guide Wire, Reaming, and Nail Insertion
- The technique proceeds similarly to AIMN: guide wire insertion across the fracture site, reduction maneuvers (often easier with free leg manipulation), sequential reaming (if desired), and nail insertion. The nail is advanced proximally until its tip is at the desired level (e.g., lesser trochanter, or across the fracture if it is more proximal).
4. Locking Screws
- Distal Locking (Fixed): Retrograde nails often have fixed distal locking screws that are inserted first through a targeting jig.
- Proximal Locking (Free-Hand): Proximal locking is typically performed free-hand with fluoroscopic guidance, similar to distal locking in AIMN, to secure the proximal fragment.
- Final Assessment and Closure: As per AIMN.
Complications & Management
Despite high success rates (>95% for healing), femoral shaft fracture fixation, primarily IMN, carries a risk of complications. Vigilant post-operative monitoring and timely intervention are crucial.
Common Complications and Salvage Strategies
| Complication | Incidence | Description & Management |
|---|---|---|
| The current literature overwhelmingly supports intramedullary nailing (IMN) as the gold standard for stabilizing diaphyseal femoral fractures in adults. This preference stems from its biomechanical advantages, excellent healing rates, and the ability to achieve stable anatomical reduction. The success rate for healing is reported to be over 95%, with studies consistently demonstrating superior outcomes compared to external fixation or plate osteosynthesis for isolated femoral diaphyseal fractures. | ||
| --- | --- | |
| Nonunion (5-10%) | Failure of fracture healing by 6-9 months post-fixation. Risk factors include inadequate stability, biological deficiency (e.g., open fracture, severe comminution), infection, patient comorbidities (smoking, diabetes). | Salvage: |
| * Exchange Nailing: For aseptic oligotrophic nonunions, removing the existing smaller nail and replacing it with a larger diameter reamed nail. This provides increased stability and introduces viable bone graft. | ||
| * Plate Fixation with Bone Graft: For atrophic or hypertrophic nonunions with significant bone defect, malalignment, or if IMN failed multiple times. Requires debridement of nonunion site and autogenous bone graft (iliac crest, fibula). | ||
| * Dynamic Compression: Convert static locking to dynamic to promote controlled compression at the fracture site. | ||
| * Electrical/Ultrasound Stimulation: Adjunctive therapy. | ||
| Malunion (5-20%) | Healing of a fracture in an unacceptable anatomical position (angular deformity >10°, rotational deformity >15-20°, shortening >1.5-2 cm). More common with comminuted fractures or inadequate reduction. | Salvage: |
| * Corrective Osteotomy: If symptomatic, malunion can be corrected by osteotomy at the malunion site, acute correction, and re-fixation (often with plating or re-nailing). | ||
| * Rotational Osteotomy: Specifically for rotational malunion, often performed in the subtrochanteric region. | ||
| * Limb Length Discrepancy (LLD) Management: Heel lifts for minor shortening; limb lengthening procedures for significant LLD if symptomatic. | ||
| Infection (1-5%) | Acute or chronic infection at the surgical site or involving the implant. Risk factors include open fractures, prolonged surgery, polytrauma, poor soft tissue coverage. | Salvage: |
| * Acute Infection (within weeks): Surgical debridement, thorough irrigation, intravenous antibiotics, and retention of a stable implant if possible. If unstable, consider external fixation, then delayed definitive fixation. | ||
| * Chronic Infection (months-years): Staged protocol: debridement, hardware removal, radical excision of infected bone/soft tissue (often with cement spacer and antibiotic beads), prolonged IV antibiotics, followed by delayed reconstruction (e.g., re-nailing, free flap, bone transport). | ||
| * Wound Vac/Negative Pressure Wound Therapy: For complex open wounds. | ||
| Hardware Complications (5-15%) | Breakage, migration, screw loosening, prominent hardware. | Salvage: |
| * Hardware Removal: For prominent screws or nail causing bursitis or soft tissue irritation (e.g., trochanteric pain from prominent nail, distal knee pain from prominent screws), usually after fracture union. | ||
| * Exchange Nailing: For nail breakage (often indicative of nonunion). | ||
| * Screw Replacement/Revision: For broken or loose screws. | ||
| Iatrogenic Nerve/Vascular Injury (Rare, <1%) | Injury to neurovascular structures during surgery. | Salvage: |
| * Immediate Exploration: Surgical exploration, nerve repair/grafting, or vascular repair (often by vascular surgeon). | ||
| * Prevention: Meticulous surgical technique, clear knowledge of anatomy, careful drilling, and reduction maneuvers. | ||
| Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE) (0.5-5%) | Formation of blood clots, particularly in polytrauma patients. | Salvage: |
| * Prophylaxis: Routine chemical (low molecular weight heparin) and mechanical (intermittent pneumatic compression) prophylaxis. | ||
| * Treatment: Anticoagulation, IVC filter if contraindications to anticoagulation. | ||
| Fat Embolism Syndrome (FES) (1-10% clinical, <1% severe) | Systemic inflammatory response due to fat globules entering the circulation, especially with reamed nailing or polytrauma. | Salvage: |
| * Supportive Care: Respiratory support (ventilation), hemodynamic stabilization. | ||
| * Prevention: Early stabilization, unreamed nailing in high-risk patients, careful reaming technique. | ||
| Reflex Sympathetic Dystrophy (CRPS) (Rare) | Chronic regional pain syndrome, often triggered by trauma or surgery. | Salvage: |
| * Multidisciplinary Pain Management: Physical therapy, pharmacological interventions (neuropathic agents, sympathetic blocks), psychological support. Early diagnosis and intervention are key. | ||
| Loss of Reduction/Fixation Failure (2-5%) | Displacement of fragments or loosening of implant post-operatively. | Salvage: |
| * Revision Surgery: Re-reduction and re-fixation, potentially with a stronger implant, bone graft, or different fixation strategy (e.g., adding a plate). |
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is integral to achieving optimal functional outcomes and minimizing long-term disability. The specific protocol is tailored to the individual patient, considering fracture stability, bone quality, comminution, associated injuries, and the chosen fixation method.
Initial Post-Operative Period (Days 0-14)
- Pain Management: Aggressive pain control with multimodal analgesia (opioids, NSAIDs, acetaminophen, nerve blocks) to facilitate early mobilization.
-
Weight-Bearing (WB) Status:
- Protected Weight-Bearing (PWB) / Touch-Down Weight-Bearing (TDWB): For most femoral shaft fractures, PWB (e.g., 25-50% body weight) or TDWB (foot on floor for balance) is initiated immediately post-op. This allows controlled axial loading to stimulate callus formation while protecting the repair.
- Non-Weight-Bearing (NWB): Reserved for highly unstable fractures, severe comminution, open fractures with soft tissue defects, or significant bone loss where initial fixation is tenuous.
- Full Weight-Bearing (FWB): May be allowed immediately for stable, simple fractures with strong fixation, particularly in younger patients.
-
Early Mobilization:
- Bed Mobility: Instruct patient on log-rolling, bed transfers.
- Transfers: Supervised transfers to chair/commode.
- Gait Training: With appropriate assistive devices (walker, crutches) and adherence to prescribed weight-bearing status. Emphasis on proper gait mechanics.
-
Range of Motion (ROM):
- Hip and Knee: Gentle, active-assisted and active ROM exercises for the hip and knee within pain limits. Patellar mobilization exercises to prevent stiffness. Avoid aggressive, forced ROM that could compromise fixation.
- Ankle Pumps/Foot Circles: To prevent DVT.
-
Muscle Activation:
- Quadriceps Sets, Gluteal Sets: Isometric exercises to maintain muscle tone and prevent atrophy.
- Ankle dorsiflexion/plantarflexion.
- Wound Care: Daily wound checks, dressing changes as per protocol.
Intermediate Phase (Weeks 2-8)
- Progressive Weight-Bearing: Advance weight-bearing status based on clinical healing (decreasing pain, improving stability) and radiographic evidence of callus formation. Progress from PWB to FWB as tolerated, typically around 4-8 weeks for stable fractures.
-
Strengthening:
- Hip: Abduction, adduction, flexion, extension (e.g., straight leg raises, hip hikes).
- Knee: Quadriceps strengthening (mini-squats, leg presses, terminal knee extension), hamstring strengthening (hamstring curls).
- Core Strengthening: Important for overall stability and balance.
- Cardiovascular Conditioning: Stationary biking, elliptical, or swimming (once wounds healed) to maintain fitness.
- Gait Re-education: Progress from assistive devices to independent ambulation as strength and balance improve. Focus on symmetrical gait pattern.
- Balance and Proprioception Exercises.
Advanced Phase (Months 2-6+)
- Full Weight-Bearing and Strengthening: Aim for full, pain-free weight-bearing. Continue progressive resistance exercises to restore full muscle strength and endurance.
- Functional Training: Incorporate activities specific to the patient's lifestyle and work demands.
- Sport-Specific Rehabilitation: For athletes, a gradual return to sport-specific drills and activities.
- Impact Loading: Introduce controlled impact activities (e.g., jumping, running) only after complete radiographic union and full strength restoration.
- Addressing Complications: Monitor for signs of nonunion, malunion, infection, or hardware irritation.
- Hardware Removal: If symptomatic, hardware removal may be considered typically 12-18 months post-union, depending on fracture consolidation and patient symptoms.
Follow-up and Imaging
- Clinical Appointments: Bi-weekly for the first 4-6 weeks, then monthly until union, then less frequently.
- Radiographs: Follow-up AP and lateral radiographs are obtained at each clinical visit to assess for fracture healing, alignment, and hardware integrity. Union is typically defined by radiographic evidence of bridging callus across at least three cortices on two orthogonal views and clinical stability.
Key Principles of Rehabilitation:
*
Individualization:
Protocols must be customized.
*
Progression:
Gradual increase in load and activity based on healing and tolerance.
*
Pain-Limited:
Avoid activities that cause significant pain.
*
Early Motion:
Encourage early, controlled motion to prevent stiffness and promote healing.
*
Education:
Educate the patient on the healing process, expected timelines, and potential complications.
Summary of Key Literature / Guidelines
The management of femoral shaft fractures has evolved significantly over the past decades, with intramedullary nailing emerging as the unequivocal gold standard for adult diaphyseal fractures. This consensus is robustly supported by extensive clinical evidence, including numerous randomized controlled trials (RCTs), prospective cohort studies, and meta-analyses.
-
Intramedullary Nailing as Gold Standard:
- Multiple studies, dating back to the late 20th century, have demonstrated the superiority of IMN over other fixation methods (e.g., cast bracing, external fixation, plate osteosynthesis) for adult femoral shaft fractures. IMN offers a high union rate (>95%), allows early weight-bearing, reduces hospital stay, and minimizes complications such as shortening, angular deformity, and nonunion compared to older techniques. The load-sharing nature of the implant and its minimal soft tissue disruption contribute to superior biological healing.
- The OTA (Orthopaedic Trauma Association) Guidelines and similar international consensus statements consistently recommend IMN as the primary treatment modality for nearly all displaced adult femoral shaft fractures.
-
Reamed vs. Unreamed Nailing:
- The debate regarding reamed versus unreamed nailing has been a significant area of research. While unreamed nailing was initially proposed to reduce the risk of fat embolism syndrome (FES) in polytrauma patients, meta-analyses and large clinical series have generally shown reamed nailing to have higher union rates and fewer mechanical complications (e.g., screw breakage, nail failure) than unreamed nailing, particularly in comminuted fractures. The reaming process, while transiently disrupting endosteal blood flow, also creates an autogenous bone graft and stimulates a biological healing response.
- Exceptions: Unreamed nailing may still be favored in specific high-risk scenarios, such as patients with severe pulmonary compromise (e.g., ARDS) or multiple concomitant severe injuries, where minimizing the systemic inflammatory response is prioritized (Damage Control Orthopedics principles).
-
Antegrade vs. Retrograde Nailing:
- Both approaches are effective, with the choice largely dictated by fracture location, associated injuries, and surgeon preference.
- Antegrade IMN is generally preferred for midshaft and proximal third fractures. Recent literature supports the use of a trochanteric entry portal over a piriformis fossa entry portal to reduce the incidence of avascular necrosis of the femoral head and minimize post-operative hip pain related to abductor muscle irritation or piriformis tendon damage.
- Retrograde IMN is well-suited for distal femoral shaft fractures, ipsilateral tibial fractures ("floating knee"), and in polytrauma patients where supine positioning is advantageous for respiratory management. Concern for knee pain related to entry portal site, articular cartilage damage, and potential PCL injury requires careful surgical technique.
-
Damage Control Orthopedics (DCO) vs. Early Total Care (ETC):
- In severely injured polytrauma patients, the timing of definitive fixation is crucial. DCO involves initial temporary stabilization (often with external fixation) to avoid adding a "second hit" of systemic inflammation from prolonged definitive surgery, followed by definitive IMN once the patient's physiological status has stabilized. This strategy is particularly relevant for patients with significant thoracic or head injuries, hemorrhagic shock, or severe inflammatory states.
- ETC involves immediate definitive fixation (within 24 hours) for stable polytrauma patients, which has been shown to reduce overall complications, hospital stay, and resource utilization. The decision between DCO and ETC relies on a comprehensive assessment of the patient's "physiologic reserve" and injury severity.
-
Ipsilateral Femoral Neck and Shaft Fractures:
- This challenging injury pattern requires diligent diagnosis (often missed femoral neck fracture) and sequential fixation. Current guidelines recommend fixing the femoral neck fracture first, followed by the femoral shaft fracture. This can be achieved with cannulated screws or a reconstructive nail (cephalomedullary nail).
-
Prevention and Management of Complications:
- Literature emphasizes meticulous pre-operative planning, precise surgical technique (including accurate rotational and length alignment), and appropriate implant selection to minimize complications like nonunion and malunion.
- Management strategies for nonunion typically involve exchange nailing (for aseptic oligotrophic nonunions) or plate fixation with bone grafting (for atrophic nonunions or significant bone defects).
- Infection rates are low but devastating; protocols for open fracture management (urgent debridement, antibiotics) are critical.
In conclusion, the current academic landscape underscores IMN as the benchmark for femoral shaft fracture treatment, advocating for tailored approaches based on fracture characteristics and patient status, supported by robust evidence and evolving technical refinements.
