Periprosthetic Fractures: Epidemiology, Biomechanics, and Advanced ORIF Principles
Key Takeaway
Periprosthetic fractures, occurring around joint replacements, are complex due to altered bone mechanics and patient factors. Open Reduction Internal Fixation (ORIF) aims for stable fixation using principles like adequate bypass length, appropriate working length, and angular stable fixation with locking plates, especially crucial for achieving union in osteoporotic bone around rigid implants.
Periprosthetic Fractures: Is Open Reduction Internal Fixation Best?
Introduction & Epidemiology
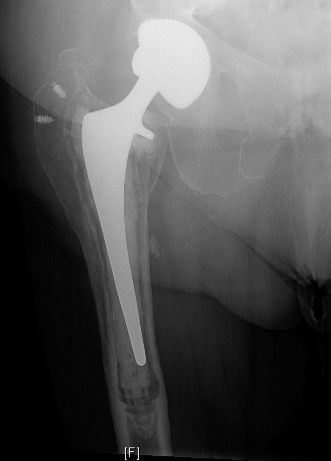
Periprosthetic fractures (PPFs) represent a formidable and increasingly common challenge in orthopedic surgery, directly correlating with the rising number of primary and revision total joint arthroplasties (TJAs) performed annually. The global incidence of PPFs is escalating, with projections indicating a substantial increase in the coming decades. Specifically, periprosthetic femoral fractures occur in approximately 0.1-1.9% of primary total hip arthroplasties (THAs) and up to 4.5% of revision THAs. Periprosthetic knee fractures, while less common, affect 0.3-2.5% of primary total knee arthroplasties (TKAs) and up to 5% of revision TKAs.
These fractures are distinct from native bone fractures due to the presence of an implanted prosthesis, which significantly alters local bone mechanics, vascularity, and subsequent healing potential. The complexity is compounded by factors such as patient demographics (often elderly with osteoporotic bone), polymorbidity, implant design, surgical approach, and the often comminuted nature of the fracture.
The primary goals in managing PPFs are fracture union, restoration of limb function, stable implant fixation, and minimization of complications. Treatment strategies range from non-operative management to open reduction internal fixation (ORIF), revision arthroplasty, or a combination of these. The decision-making process is nuanced, guided by fracture location, implant stability, bone stock, and patient physiological status. This review focuses specifically on the role and efficacy of ORIF in this complex landscape, exploring its indications, technical considerations, and outcomes.
Surgical Anatomy & Biomechanics
Successful management of periprosthetic fractures hinges upon a thorough understanding of the intricate surgical anatomy and altered biomechanics inherent to the prosthetic environment. The presence of an intramedullary stem or an extensive metallic implant creates distinct zones of stress shielding and stress concentration, predisposing the surrounding bone to fracture.
Bone-Implant Interface & Stress Risers
- Bone Stock Quality: Patients sustaining PPFs often have compromised bone quality, typically osteopenia or osteoporosis, exacerbating the challenge of achieving stable fixation. The cortical bone around a well-fixed stem may be denser due to load transfer, while other areas experience disuse osteoporosis.
-
Implant Design:
- Stem Characteristics: Stem length, diameter, geometry (tapered, cylindrical), and material (cobalt-chrome, titanium) influence the stress distribution. Stiff, long stems can create significant stress risers at their tips, while short stems may shift stress more proximally.
- Fixation Type: Cemented versus uncemented stems have different interfaces with bone. Cemented stems provide a more uniform load transfer, but the cement mantle itself can be a point of failure or stress concentration. Uncemented stems rely on bony ingrowth, and the interface can be a weak point if ingrowth is incomplete.
- Previous Surgical Insults: Prior surgical approaches can compromise soft tissue envelopes and blood supply, impacting healing. Screw holes or cortical defects from previous operations act as iatrogenic stress risers.
Fracture Patterns & Classification
The Vancouver classification system is the gold standard for periprosthetic femoral fractures, guiding treatment decisions based on fracture location, implant stability, and bone stock:
-
Type A (Trochanteric):
Fractures in the greater or lesser trochanteric region.
- AG: Greater trochanter.
- AL: Lesser trochanter.
-
Type B (Femoral Shaft):
Fractures around or immediately distal to the stem.
- B1: Fracture around a well-fixed femoral stem. The most amenable to ORIF.
- B2: Fracture around a loose femoral stem with adequate bone stock. Typically necessitates stem revision.
- B3: Fracture around a loose femoral stem with poor bone stock. Requires stem revision with bone grafting (allograft or structural autograft) or a more extensive reconstructive approach.
- Type C (Distal Femoral Shaft): Fractures well below the tip of the femoral stem, where the stem is not directly involved in the fracture propagation. These are often managed similarly to diaphyseal femur fractures in native bone, albeit with consideration for the existing implant proximally.
Periprosthetic knee fractures, particularly supracondylar femoral fractures above a TKA, are commonly classified using the Orthopaedic Trauma Association (OTA) system or a modified Su classification. The presence of the femoral component dictates challenges in distal fixation.
Biomechanical Principles of ORIF in PPFs
The primary challenge in ORIF for PPFs is achieving stable fixation in compromised bone, often around a rigid implant. Key biomechanical principles include:
- Bypass Length: The plate must bypass the fracture by at least two cortical diameters (or preferably three) on both sides of the fracture, and critically, extend well past the tip of the femoral stem to neutralize stress risers.
- Working Length: Longer working lengths (distance between inner screws) promote relative stability, beneficial for secondary bone healing in comminuted fractures. Shorter working lengths offer absolute stability, typically for simple fracture patterns.
- Angular Stable Fixation (Locking Plates): Locking compression plates (LCPs) are invaluable. Locking screws provide fixed-angle constructs, offering superior pullout strength in osteoporotic bone and preventing screw toggle. This is crucial as the screws do not rely on plate-to-bone compression for stability, thereby preserving periosteal blood supply.
- Bridging Principles: For comminuted fractures, the goal is often relative stability, bridging the comminuted zone without direct screw fixation into every fragment.
- Cerclage Cables/Wires: These provide circumferential compression, aiding in initial reduction and indirect stability, especially for spiral patterns or when comminution prevents direct screw purchase. They can also help coapt bone fragments to the plate.
- Allograft Struts: In cases of significant bone loss or comminution, structural allograft struts can be used to augment fixation, provide biological scaffolding, and improve mechanical stability, particularly in B3 type fractures when combined with revision.
Indications & Contraindications
The decision to proceed with ORIF for periprosthetic fractures is complex and multifactorial, heavily reliant on the Vancouver classification for femoral fractures, fracture morphology, implant stability, bone stock, and patient factors.
Indications for ORIF
Open reduction internal fixation is generally indicated when the prosthetic component is well-fixed and there is adequate bone stock to allow for stable osteosynthesis.
- Vancouver B1 Fractures: This is the quintessential indication for ORIF. The fracture occurs around a well-fixed femoral stem, with sufficient bone stock. The goal is to stabilize the fracture while retaining the existing, functional prosthesis. This type is highly amenable to plate and screw fixation, often augmented with cerclage wires.
-
Vancouver A Fractures:
Fractures of the greater or lesser trochanter.
- Non-displaced/Minimally Displaced: Often managed non-operatively.
- Significantly Displaced (esp. greater trochanter): If causing painful impingement or abductor insufficiency, ORIF may be indicated to restore trochanteric anatomy and abductor lever arm.
- Vancouver C Fractures: Fractures occurring distally to the tip of a well-fixed femoral stem. These are treated similarly to native femoral shaft fractures, utilizing principles of long-bone fixation (e.g., long locking plates or retrograde intramedullary nails, if feasible, bypassing the proximal stem). The key is to ensure the fixation construct bypasses the stem tip to prevent iatrogenic stress risers.
- Periprosthetic Supracondylar Femur Fractures (above TKA): For non-comminuted fractures with a stable prosthesis, ORIF with locking plates (e.g., pre-contoured distal femoral locking plates) is often the preferred method. This allows for stable fixation above the femoral component of the TKA, especially crucial in osteoporotic bone.
- Periprosthetic Tibial Fractures (below TKA): Depending on the stability of the tibial component and fracture pattern, ORIF with plates and screws can be used for stable patterns with an intact prosthesis.
Contraindications for ORIF
ORIF is contraindicated or less favorable in situations where stable fixation cannot be reliably achieved or when the underlying prosthesis is compromised.
- Loose Prosthetic Component (Vancouver B2 & B3): This is the primary contraindication for ORIF as a standalone treatment. Attempting to fix a fracture around a loose stem without addressing the stem itself is doomed to failure. In these cases, revision arthroplasty (with or without extensive bone grafting) is indicated.
- Severely Comminuted Fracture with Extensive Bone Loss (Vancouver B3): While ORIF might be used as an adjunct to stabilize segments, the primary treatment for B3 fractures involves revision arthroplasty with reconstruction of the bone defect (e.g., modular stems, structural allograft). Pure ORIF is insufficient.
- Infection: Active periprosthetic joint infection is an absolute contraindication for definitive ORIF. The infection must be addressed first, typically with a two-stage revision protocol, potentially involving external fixation or temporary implant removal, before definitive reconstruction.
- Poor Bone Quality (Severe Osteoporosis, Paget's Disease): If the bone quality is so poor that screw purchase and plate stability are highly questionable, the risk of early implant failure or nonunion is high. In such extreme cases, alternative strategies like allograft-prosthesis composite, extended revision stems, or even amputation might be considered, depending on the patient's functional demands and life expectancy.
- Severely Debilitated Patient with Limited Functional Goals: For patients with very limited life expectancy, severe comorbidities, or non-ambulatory status, less invasive treatments or palliative care may be more appropriate than a complex ORIF.
- Vascular Injury: Significant neurovascular compromise may necessitate immediate vascular repair prior to definitive fracture fixation, potentially delaying or altering the orthopedic approach.
Operative vs. Non-Operative Indications
| Indication Type | Scenario | Management Strategy |
|---|---|---|
| Non-Operative | Vancouver A (AG, AL): Non-displaced or minimally displaced (e.g., <1cm displacement for GT), stable. Patient able to bear weight within pain tolerance. | Protected weight-bearing (crutches, walker) for 6-12 weeks. Gradual increase in activity. Close radiographic follow-up. |
| Vancouver B1/C: Non-displaced or stable fracture in a low-demand patient with significant comorbidities rendering surgery high-risk, and the prosthesis remains intrinsically stable. (Rare, often a salvage or palliative approach). | Strict non-weight bearing or minimal weight bearing. Splinting/bracing may be considered. High risk of nonunion or progressive displacement. Reserved for highly selective cases. | |
| Operative (ORIF) | Vancouver B1: Displaced or unstable fracture around a well-fixed femoral stem with adequate bone stock. | Open Reduction Internal Fixation (ORIF): Long locking plate and screw construct, often augmented with cerclage wires. Bypassing the stem tip by at least 2-3 cortical diameters. Goal: Relative stability, secondary bone healing. |
| Vancouver A (AG, AL): Displaced greater trochanteric fracture causing impingement, abductor dysfunction, or painful nonunion. | ORIF with tension band wiring, cables, or screws. | |
| Vancouver C: Displaced or unstable fracture well below the tip of a well-fixed femoral stem. | ORIF: Long locking plate and screw construct (e.g., for distal femur). Intramedullary Nailing: Retrograde nail (if implant allows and fracture pattern suitable). | |
| Periprosthetic Supracondylar Femur (TKA): Displaced or unstable fracture above a well-fixed TKA femoral component. | ORIF: Distal femoral locking plate (pre-contoured). Techniques to maximize screw purchase around the implant. | |
| Operative (Revision Arthroplasty) | Vancouver B2: Fracture around a loose femoral stem with adequate bone stock. | Revision Arthroplasty: Removal of loose stem, implantation of a longer, often modular, revision stem that bypasses the fracture site by at least two cortical diameters. ORIF with a plate may be used as an adjunct for fracture stabilization after stem revision, especially for comminuted patterns. |
| Vancouver B3: Fracture around a loose femoral stem with poor bone stock (e.g., significant osteolysis, multiple cortical defects). | Complex Revision Arthroplasty: Removal of loose stem, extensive bone reconstruction (structural allograft, allograft-prosthesis composite), and/or mega-prosthesis, combined with a long, often cemented, revision stem. Adjunctive ORIF with plates/wires often needed to secure grafts and achieve stability. | |
| Active Periprosthetic Infection: Regardless of fracture type. | Two-Stage Revision: Stage 1: Debridement, implant removal, antibiotic spacer. Stage 2 (after infection eradication): Reimplantation with a new prosthesis, potentially combined with ORIF if fracture dictates. | |
| Severe Comminution/Bone Loss (non-reconstructible with ORIF alone): Especially if the prosthesis is stable but the bone defect prevents adequate fixation for union. (This overlaps with B3 concepts but can occur with stable implants). | Augmented ORIF: ORIF supplemented with structural allograft, bone grafting, or bone cement. In extreme cases, revision arthroplasty to a long stem bypassing the defect may be the only viable option, even if the prior implant was nominally stable. | |
| Failed Prior ORIF: Nonunion, malunion, or implant failure after previous ORIF for a periprosthetic fracture. | Revision ORIF, revision arthroplasty (if implant now loose or bone stock compromised), or allograft-prosthesis composite, depending on the etiology of failure. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is paramount for successful outcomes in periprosthetic fracture surgery, particularly for ORIF. These are often complex cases with inherent challenges due to patient comorbidities, compromised bone quality, and the presence of prior hardware.
Pre-operative Assessment & Imaging
-
Clinical Assessment:
- Patient History: Ascertain the mechanism of injury, prior surgeries (type of prosthesis, surgical approach, implant records), and current medications (anticoagulants, osteoporosis medications).
- Comorbidities: Assess for medical comorbidities (cardiac, pulmonary, renal disease, diabetes) that increase surgical risk. Optimize patient health status.
- Neurovascular Status: Thoroughly document neurovascular integrity of the affected limb.
-
Radiographic Evaluation:
-
Standard Radiographs:
AP and lateral views of the entire femur (or tibia/humerus as appropriate), including the joint above and below. Crucially, image the hip and knee for femoral fractures.
- Assess fracture location, pattern (simple vs. comminuted), and displacement.
- Evaluate implant stability : Look for cement mantle fractures, lucency, periosteal reaction, subsidence, or change in stem position. Dynamic stress views or comparison with prior radiographs can be invaluable.
- Assess bone stock: Note cortical thickness, osteolysis, prior screw holes, or existing defects.
- Computed Tomography (CT) Scan: Highly recommended for complex fracture patterns, comminution, and to better delineate the relationship of the fracture to the implant. CT can precisely identify the presence of rotational malunion or comminuted fragments. It is also invaluable for pre-operative templating.
- Contralateral Limb Radiographs: Useful for templating implant sizes, assessing canal morphology, and determining limb length discrepancies.
-
Standard Radiographs:
AP and lateral views of the entire femur (or tibia/humerus as appropriate), including the joint above and below. Crucially, image the hip and knee for femoral fractures.
-
Implant Identification:
- Operative Records: Obtain previous operative notes, implant stickers, and radiographs to identify the specific prosthesis type, manufacturer, and size. This information is critical for understanding stem geometry and material, guiding plate selection, and anticipating potential challenges.
- Radiographic Recognition: If records are unavailable, experienced surgeons can often identify implant types from radiographs based on characteristic designs.
-
Templating:
- Plate Length & Position: Template the desired length of the locking plate, ensuring it bypasses the fracture by at least 2-3 cortical diameters on both sides and, crucially, extends well past the tip of the existing femoral stem. This is non-negotiable for stable fixation and stress neutralization.
- Screw Length & Number: Estimate screw lengths, particularly around the prosthesis where bicortical purchase may not be possible. Plan for unicortical locking screws and bicortical non-locking screws where appropriate.
- Adjunctive Fixation: Plan for cerclage wires/cables, particularly for spiral or comminuted fractures, or when holding fragments to the plate. Consider the need for allograft struts in cases of significant bone loss.
-
Operating Room Setup:
- Ensure availability of a comprehensive range of locking plates (e.g., LCP systems for distal femur, broad LCPs for shaft), diverse screw lengths (locking and non-locking), cerclage wires/cables, and specialized reduction instruments.
- Have instruments for potential revision arthroplasty on standby, especially if implant stability is questionable (e.g., extractors, trial stems, bone grafts).
- Confirm fluoroscopy (C-arm) is functional and readily available.
Patient Positioning
Patient positioning depends on the fracture location and the chosen surgical approach.
-
Femoral Fractures (Hip/Shaft):
- Lateral Decubitus Position: Generally preferred for posterolateral or direct lateral approaches to the femur. This allows for excellent visualization of the lateral femur and accommodates C-arm imaging. Ensure adequate padding, particularly at pressure points. The non-operative leg should be flexed and draped out of the field.
- Supine Position: Can be used for anterior approaches or for periprosthetic distal femoral fractures treated with a lateral approach, especially if a fracture table is desired (though less common for PPFs due to implant interference).
-
Periprosthetic Supracondylar Femur (above TKA):
- Supine Position: Typically used for a lateral approach to the distal femur. A bump under the ipsilateral hip may be helpful. The knee should be slightly flexed to allow for posterior retraction.
-
General Considerations:
- Radiolucent Table: Essential for intraoperative fluoroscopy.
- Tourniquet: May be used depending on surgeon preference and location, but consider its impact on blood supply in compromised soft tissues.
- Sterile Prep & Drape: Ensure a wide sterile field, extending from the iliac crest to the foot for femoral fractures, allowing for potential extension of the incision or bone grafting. The entire limb should be prepped to allow for manipulation and visualization.
- C-arm Access: Position the patient and table to allow unimpeded C-arm access for AP and lateral views throughout the procedure, especially during reduction and fixation steps.

Detailed Surgical Approach / Technique
The surgical technique for ORIF of periprosthetic fractures demands meticulous attention to soft tissue handling, precise reduction, and robust fixation principles tailored to the compromised bone and existing implant.
Incision and Exposure
-
Skin Incision:
- Utilize the existing surgical incision if possible, especially if it provides adequate access to the fracture site. This minimizes devascularization of skin flaps.
- If the existing incision is too short or poorly placed, a new incision may be necessary, typically a direct lateral approach for most femoral periprosthetic fractures. For supracondylar femoral fractures above a TKA, a lateral approach extending proximally from the knee is common.
- Incision length must be sufficient for complete visualization of the fracture, implant, and adequate working room for plate application.
-
Soft Tissue Dissection:
- Careful, atraumatic dissection is paramount to preserve periosteal and muscular blood supply, which is often compromised in these revision settings.
- Internervous Plane: For femoral fractures, the most common approach is the direct lateral approach , splitting the vastus lateralis muscle longitudinally in line with its fibers. This muscle is innervated by the femoral nerve (anterior division), so splitting it longitudinally minimizes denervation.
- Subperiosteal dissection should be limited to the immediate fracture site to aid in reduction, but extensive stripping of the periosteum beyond the plate footprint should be avoided to preserve healing potential.
- Identify and protect crucial neurovascular structures. For the femur, this includes the femoral nerve (anterior), sciatic nerve (posterior), and femoral artery/vein (medial). For supracondylar fractures, the popliteal neurovascular bundle is at risk posteriorly.
Fracture Reduction
- Debridement: Remove any hematoma, loose bone fragments (unless critical for reconstruction), or necrotic tissue.
-
Temporary Stabilization:
- Traction: Longitudinal traction (manual or via a fracture table) can aid in restoring length.
- External Fixator: A temporary external fixator can provide provisional stability, especially in highly comminuted or unstable fractures, allowing for controlled manipulation and soft tissue protection.
- Cerclage Wires/Clamps: Provisional cerclage wires or reduction clamps can approximate fragments and assist in maintaining reduction.
-
Reduction Techniques:
- Indirect Reduction: Often preferred in comminuted fractures to preserve soft tissue attachments. This involves restoring length, alignment, and rotation without extensive direct exposure of individual fragments. Techniques include ligamentotaxis, joystick maneuvers (using Kirschner wires or small screws as handles), and traction.
- Direct Reduction: May be necessary for simple fracture patterns or when precise anatomical reduction is critical. This involves direct manipulation of fragments using bone hooks, clamps, or periosteal elevators.
- Ensure the existing prosthetic component is stable and well-reduced within the bone fragments. This is a critical assessment at this stage.
Fixation Strategy (Plating, Screws, Cerclage)
The choice of fixation relies heavily on the Vancouver classification and the principles of angular stability.
-
Plate Selection:
- Long Locking Compression Plate (LCP): The workhorse for femoral periprosthetic fractures (B1, C) and supracondylar femoral fractures. These plates offer angular stability, crucial in osteoporotic bone and when working around existing implants.
- Length: The plate must be long enough to bypass the fracture by at least 2-3 cortical diameters on either side, and crucially, extend well past the tip of the femoral stem. This is critical to neutralize stress risers created by the stem.
- Contour: Pre-contoured plates (e.g., distal femoral LCPs) simplify application. Custom contouring may be necessary, but care must be taken not to deform the locking screw holes.
-
Plate Application:
- Submuscular Tunneling: For femoral shaft fractures, consider submuscular tunneling of the plate to minimize periosteal stripping and preserve blood supply, especially for comminuted patterns where relative stability is desired.
- Positioning: Place the plate on the lateral aspect of the femur. Ensure the plate lies flat on the bone.
-
Screw Fixation:
-
Proximal Fixation (around the stem):
- Unicortical Locking Screws: These are essential when working around a cemented or uncemented stem. Screws should be directed away from the stem or engage only one cortex, locking into the plate. Avoid drilling into the prosthetic stem. Pre-operative templating and intraoperative fluoroscopy in two planes (AP and lateral) are crucial to confirm screw trajectory and length, avoiding the stem.
- Cerclage Wires/Cables: These are highly effective for proximal fragment fixation, particularly for spiral components or when bone quality is poor. They provide circumferential compression and hold the plate to the bone, acting as a "gasket." They are applied before definitive plate fixation and can improve stability around the stem. They should be applied carefully to avoid neurovascular injury, ensuring passage subperiosteally.
-
Distal Fixation (past the stem tip):
- Bicortical Locking Screws: Once past the stem tip, bicortical locking screws can be used for robust fixation, as long as adequate bone stock allows.
- Bicortical Non-locking Screws: Compression screws can be used if anatomical reduction and compression are desired in simple fracture patterns.
- Number of Screws: Aim for at least 3-4 locking screws on either side of the fracture, both proximally and distally. More screws in osteoporotic bone or for comminuted fractures.
-
Proximal Fixation (around the stem):
-
Adjunctive Fixation:
- Cerclage Wires/Cables: Used to secure comminuted fragments to the main bone shaft or to coapt the plate to the bone, improving stability. Can be used in conjunction with locking plates, particularly proximally around the stem, or for spiral fragments.
- Allograft Struts: In cases of significant metaphyseal comminution or bone loss, particularly in Vancouver B3, structural allograft struts can be placed under the plate to provide biological and mechanical augmentation. They are then secured with cerclage wires or screws passing through them.
- Bone Grafting: Autograft or allograft may be applied to encourage union, especially in comminuted areas or anticipated delayed healing.
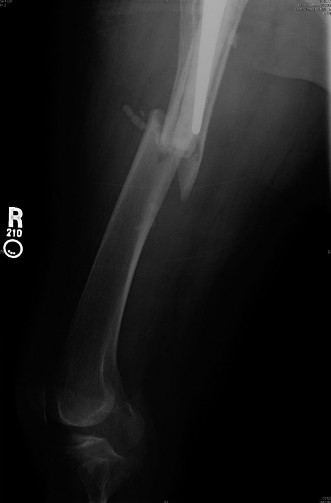
Intraoperative Assessment
- Fluoroscopy: Essential for confirming reduction, plate position, screw length, and trajectory in both AP and lateral planes. Verify that no screws impinge on the stem and that the construct bypasses the stem tip adequately.
- Stability: Physically test the construct for stability.
- Limb Length, Alignment, Rotation: Ensure restoration of acceptable limb length, mechanical axis alignment, and rotational stability.
Wound Closure
- Thorough hemostasis.
- Layered closure of deep fascia, subcutaneous tissue, and skin.
- Consider drains if significant bleeding is anticipated.
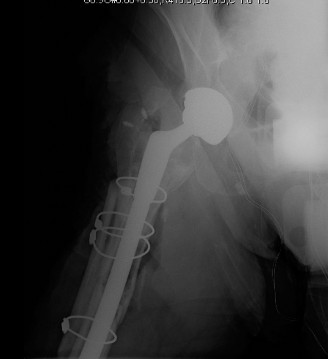
Complications & Management
Periprosthetic fractures treated with ORIF are associated with a significant complication rate due to patient comorbidities, compromised bone quality, and the challenges of fixation around a foreign body. Vigilant post-operative monitoring and prompt intervention are critical.
Table of Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approximate) | Description |
Important Notes:
- This table represents general incidences and broad salvage strategies. Specific outcomes vary greatly with the specific fracture type (e. Importantly, for B2 and B3, revision arthroplasty with an extended-length stem bypassing the fracture by at least two cortical diameters remains the definitive treatment. ORIF serves as an adjunct to stabilize fragments.
- Preventative measures during the primary surgery (e.g., careful reaming, appropriate stem size, proper implant seating) are crucial for reducing the risk of intraoperative PPFs. Post-operatively, patient education on fall prevention and careful follow-up are important.
- Antibiotic prophylaxis is essential for all operative cases.
- Thromboprophylaxis must be administered per institutional guidelines.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing outcomes following ORIF for periprosthetic fractures. The protocol must be individualized, considering the fracture stability, bone quality, type of fixation, patient's comorbidities, and functional goals. The primary objectives are to promote fracture union, prevent complications, and restore range of motion and strength.
Initial Phase (Days 0-6 Weeks)
- Pain Management: Aggressive, multimodal pain management (opioids, NSAIDs/acetaminophen, nerve blocks, regional anesthesia) is essential to facilitate early mobilization and patient comfort.
-
Weight-Bearing Status (Crucial Decision):
- Protected Weight-Bearing: Most periprosthetic fractures treated with ORIF require a period of protected weight-bearing. This often means toe-touch weight-bearing (TTWB) or partial weight-bearing (PWB) with an assistive device (walker, crutches) for 6-12 weeks.
- Non-Weight-Bearing (NWB): In cases of highly comminuted fractures, very poor bone quality, or tenuous fixation, strict NWB may be prescribed, typically for the initial 6 weeks.
- Factors influencing decision: Fracture stability after fixation, number of cortical defects, use of allograft struts, patient's ability to comply with restrictions.
- Serial Radiographs: Regular radiographs (e.g., at 2 weeks, 6 weeks) are used to monitor for signs of fracture healing and implant loosening or failure before advancing weight-bearing.
-
Range of Motion (ROM):
- Early, Gentle ROM: For hip fractures, continuous passive motion (CPM) or gentle active-assisted range of motion (AAROM) within a pain-free arc can begin within the first few days. Avoid extremes of motion that may stress the fracture site.
- Knee/Ankle/Foot ROM: Encourage early, active ROM to prevent stiffness and deep vein thrombosis (DVT).
-
Strengthening:
- Isometric Exercises: Quadriceps sets, gluteal sets, ankle pumps should begin immediately to maintain muscle tone and promote circulation.
- Upper Extremity Strengthening: Crucial for patients using walkers or crutches to facilitate independent mobility.
- DVT Prophylaxis: Continue chemical thromboprophylaxis per institutional guidelines. Mechanical prophylaxis (compression stockings, SCDs) should also be utilized.
- Wound Care: Monitor incision for signs of infection or dehiscence.
Intermediate Phase (6-12 Weeks)
-
Progression of Weight-Bearing:
- Based on radiographic evidence of early callus formation and clinical stability (minimal pain at fracture site with stress), weight-bearing is progressively advanced.
- Transition from TTWB/PWB to weight-bearing as tolerated (WBAT) with an assistive device.
- The goal is to gradually wean from assistive devices as strength and balance improve.
-
Increased ROM & Strengthening:
- Continue active and passive ROM exercises.
- Progress to more aggressive strengthening exercises for the hip and knee musculature (e.g., straight leg raises, hip abduction/adduction, knee flexion/extension with minimal resistance).
- Initiate core strengthening exercises.
- Gait Training: Intensive gait training with physical therapy to correct compensatory patterns and improve balance.
Advanced Phase (3-6 Months and Beyond)
- Full Weight-Bearing: Once radiographs demonstrate robust fracture healing and clinical exam confirms stability, full weight-bearing without assistive devices is permitted.
-
Functional Restoration:
- Focus on advanced strengthening (e.g., resistance band exercises, light weights, balance training, proprioceptive exercises).
- Stair climbing, uneven surface negotiation.
- Return to light recreational activities.
- Activity Modification: Advise patients on avoiding high-impact activities, repetitive heavy lifting, or activities that place excessive torsional stress on the limb, which could predispose to re-fracture or implant failure.
- Long-Term Follow-up: Continued radiographic monitoring for signs of implant loosening, nonunion, or late complications. This is especially important for patients with underlying osteoporosis, who may benefit from bone health optimization.
Key Considerations
- Communication: Clear communication between the surgeon, physical therapist, and patient is paramount for successful rehabilitation.
- Patient Education: Educate patients about the fragility of the bone during the healing phase, the importance of adherence to weight-bearing restrictions, and the signs of potential complications.
- Realistic Expectations: Manage patient expectations regarding recovery timelines and potential functional limitations. Full recovery can take 6-12 months or longer.
- Bone Health Optimization: Address underlying osteoporosis with appropriate medical management (e.g., bisphosphonates, PTH analogs, vitamin D, calcium) to improve bone density and reduce the risk of future fractures.
Summary of Key Literature / Guidelines
The management of periprosthetic fractures continues to evolve, driven by advancements in surgical techniques, implant design, and a deeper understanding of bone biology and biomechanics. Key literature and guidelines provide a framework for optimal care, though specific treatment decisions often remain at the discretion of the experienced surgeon.
-
Vancouver Classification System:
- Foundation: Developed by Duncan and Masri, this classification for periprosthetic femoral fractures (A, B1, B2, B3, C) remains the cornerstone for guiding treatment. Its widespread adoption allows for standardized communication and comparison of outcomes.
- Implication for ORIF: The Vancouver B1 fracture (well-fixed stem, adequate bone stock) is the primary indication for ORIF. Literature consistently supports good to excellent outcomes with appropriate plating techniques for B1 fractures.
-
AO Principles of Fracture Management:
- Core Concepts: The AO Foundation's principles of anatomical reduction, stable fixation, preservation of blood supply, and early, safe mobilization are highly relevant to PPF management.
- Specific to PPFs: The emphasis on relative stability for comminuted fractures, indirect reduction, and judicious soft tissue handling directly applies to periprosthetic ORIF, particularly with locking plates.
-
Locking Plate Technology (LCPs):
- Evolution: The introduction of locking compression plates (LCPs) has revolutionized PPF management, particularly for osteoporotic bone. Studies demonstrate superior pullout strength and angular stability compared to conventional non-locking plates.
- Biomechanical Advantage: LCPs function as internal fixators, creating a fixed-angle construct that does not rely on plate-bone compression, thereby minimizing periosteal stripping and preserving blood supply. This is critical in the often-compromised bone of PPF patients.
- Clinical Evidence: Numerous studies and meta-analyses show favorable union rates and functional outcomes for Vancouver B1 and C fractures treated with LCPs.
-
Cerclage Wires/Cables:
- Role: While once viewed as a primary fixation method, cerclage wires are now predominantly used as an adjunct to plate fixation, particularly for spiral components, comminuted fragments, or to improve plate-bone contact, especially around the proximal implant.
- Evidence: Studies indicate that combining cerclage with locking plates improves stability, particularly in osteoporotic bone, without increasing rates of nonunion or infection when applied atraumatically.
-
Allograft Struts:
- Indications: For periprosthetic fractures with significant bone loss or comminution (especially B3 type, but also occasionally B1/B2 with defects), structural cortical allograft struts can augment fixation.
- Mechanism: They provide mechanical support and a biological scaffold for healing. They are typically secured to the host bone and plate with cerclage wires or screws.
- Outcomes: While increasing complexity, allograft supplementation can improve construct stability and promote union in challenging cases.
-
Comparison of ORIF vs. Revision Arthroplasty (for B2/B3):
- Consensus: The literature overwhelmingly supports revision arthroplasty (with or without extensive bone grafting) as the treatment of choice for Vancouver B2 and B3 fractures, where the stem is loose. Attempting ORIF alone on a loose stem is associated with very high failure rates.
- Ongoing Debate: The optimal type of revision stem (e.g., modular tapered, cylindrical, cemented vs. uncemented) and the extent of bone grafting remain areas of active research and surgeon preference, depending on bone stock and patient factors.
-
Surgical Approach and Minimally Invasive Techniques:
- Direct Lateral Approach: Remains the most common and versatile approach for femoral periprosthetic fractures.
- Submuscular Plating: Techniques employing submuscular (or less invasive) plate insertion are gaining traction to minimize soft tissue dissection and periosteal stripping, potentially improving healing and reducing complications.
-
Management of Periprosthetic Supracondylar Femur Fractures:
- Similar Principles: ORIF with long, pre-contoured distal femoral locking plates is the preferred method for stable, non-comminuted fractures above a well-fixed TKA.
- Challenges: Limited distal bone stock, existing femoral component can make screw placement difficult, often requiring unicortical locking screws and careful trajectory planning. Retrograde intramedullary nailing is an alternative if the femoral component design allows for entry.
Conclusion: Is ORIF Best?
Based on current literature and clinical consensus, ORIF is the optimal treatment for well-selected periprosthetic fractures, specifically Vancouver B1 and C femoral fractures, and many periprosthetic supracondylar femoral fractures above a stable TKA. In these scenarios, the prosthesis is stable, and bone stock is sufficient to allow for robust fixation. Locking plate technology, often augmented with cerclage wires, provides the necessary stability to achieve high union rates and functional recovery.
However, ORIF is not "best" or even appropriate as a standalone treatment when the prosthetic component is loose (Vancouver B2 or B3) or when there is extensive bone loss (B3). In these complex situations, revision arthroplasty, often combined with advanced reconstructive techniques (e.g., long stems, structural allografts), is the definitive treatment. Therefore, the question of whether ORIF is "best" is highly contextual, emphasizing the critical importance of accurate classification and meticulous pre-operative planning to match the surgical strategy to the specific periprosthetic fracture type.
