Nonunion Fractures: Orthopedic Epidemiology, Biomechanics, & Classification
Key Takeaway
Nonunion fractures are failures of bone healing, persisting beyond expected time, affecting 5-10% of fractures. They are classified into hypertrophic (biologically active with mechanical instability, often abundant callus) and atrophic (biologically deficient with minimal callus, compromised vascularity). Understanding their distinct pathophysiology is crucial for effective orthopedic management and restoring function.
Introduction & Epidemiology
Nonunion of fractures represents a significant challenge in orthopedic surgery, defined clinically by the absence of progressive healing for three consecutive months and radiographically by no signs of bridging callus across the fracture site within 6-9 months following injury, or an interval beyond which union would typically be expected for the specific fracture pattern. It signifies a failure of the physiological bone healing cascade, leading to persistent pain, functional impairment, and often considerable socioeconomic burden. The diagnosis of nonunion is typically established when a fracture has not healed despite an adequate period of time, usually exceeding twice the average healing time for that specific bone and location, or when there are clear clinical and radiographic signs of an unhealed fracture (e.g., persistent pain, motion at the fracture site, lucency at the fracture gap).
Epidemiologically, fracture nonunion affects approximately 5-10% of all fractures, with certain anatomical locations and patient populations exhibiting higher rates. Tibial shaft fractures, particularly open fractures or those with significant soft tissue injury, have a reported nonunion rate as high as 10-20%. Risk factors are broadly categorized into three groups:
*
Patient-related factors
: Advanced age, malnutrition (e.g., vitamin D deficiency, hypoalbuminemia), smoking, diabetes mellitus, peripheral vascular disease, chronic kidney disease, osteoporosis, use of NSAIDs, corticosteroids, or immunosuppressants.
*
Fracture-related factors
: High-energy trauma, severe soft tissue compromise (Gustilo-Anderson type III open fractures), segmental bone loss, significant comminution, pathological fractures, and fractures with substantial displacement or instability. Certain anatomical locations, such as the distal tibia, femoral neck, and scaphoid, are inherently more prone to nonunion due to tenuous blood supply or high mechanical stresses.
*
Treatment-related factors
: Inadequate reduction, unstable fixation, suboptimal surgical technique (e.g., excessive periosteal stripping, thermal necrosis from reaming), early weight-bearing on an unstable construct, or unrecognized infection.
The economic implications of nonunion are substantial, encompassing multiple surgical procedures, prolonged rehabilitation, lost productivity, and increased healthcare expenditures. Effective diagnosis and judicious management strategies are paramount to restoring function and improving patient outcomes.
Surgical Anatomy & Biomechanics
Successful nonunion management hinges on a thorough understanding of the surgical anatomy pertinent to the fracture site and the biomechanical principles governing bone healing. Anatomical considerations include the local vascularity, the surrounding soft tissue envelope, the presence of critical neural structures, and the native mechanical environment of the affected bone.
Bone Biology and Vascularity
Bone healing is a complex biological process that requires adequate vascularization, viable bone ends, and a stable mechanical environment. The presence of well-vascularized tissue is critical for delivering osteoprogenitor cells, growth factors, and nutrients essential for callus formation and remodeling. Bones such as the scaphoid or femoral head have precarious blood supplies, making them inherently susceptible to avascular necrosis and nonunion. Chronic nonunions often feature sclerotic bone ends and extensive fibrous tissue within the fracture gap, indicating a hostile biological environment with compromised vascularity.

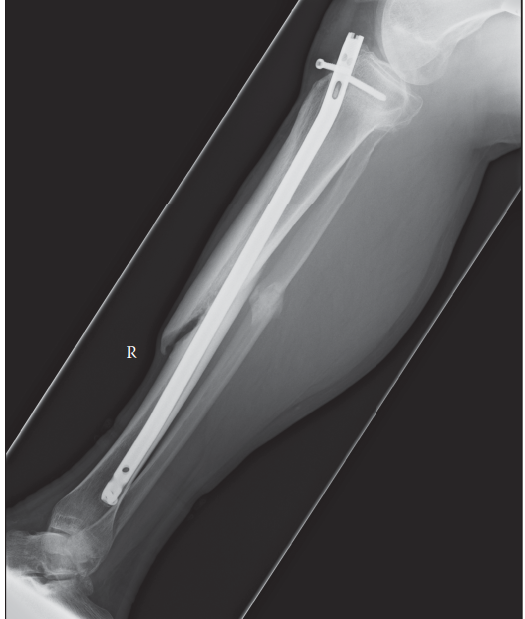
Figure 1: Radiographic appearance of a typical hypertrophic nonunion of the tibia, characterized by abundant callus formation but persistent lucency at the fracture site, indicative of mechanical instability rather than biological deficiency.
Biomechanical Principles of Nonunion
The "mechanobiology" of bone healing emphasizes the critical interplay between mechanical stability and biological activity. Nonunions are broadly classified based on their radiographic appearance and presumed pathophysiology:
*
Hypertrophic (or elephant's foot/horse hoof) nonunions
: Characterized by abundant callus formation visible on radiographs, but without bridging across the fracture gap. This morphology suggests a biologically active process attempting to heal, but failing due to
inadequate mechanical stability
at the fracture site. Treatment primarily involves enhancing stability and compression.
*
Atrophic (or avascular) nonunions
: Radiographically demonstrate minimal or no callus formation, with often resorbed, "pencil-point" or "tapered" bone ends. This morphology points to a
biological deficiency
, such as compromised vascularity, infection, or severe bone loss, often compounded by mechanical instability. Treatment requires addressing the biological deficit through debridement and bone grafting, in addition to achieving stable fixation.
The concept of strain theory is fundamental. Optimal bone healing occurs within a narrow range of interfragmentary strain. Excessive motion (high strain) disrupts callus formation, leading to fibrous tissue or pseudarthrosis (nonunion), while absolute rigidity (low strain) can lead to stress shielding and delayed remodeling, particularly if the biological environment is compromised. Fixation strategies for nonunions aim to provide an appropriate mechanical environment—stable enough to permit cellular differentiation and callus maturation, yet dynamic enough to promote load sharing and prevent stress shielding.
The chosen fixation method (plates, intramedullary nails, external fixators) influences the biomechanical environment:
*
Plates
: Can provide rigid compression (dynamic compression plating) or relative stability (bridging plates, locking plates). Locking plates are particularly useful in osteoporotic bone or comminuted fractures, but excessive rigidity can lead to stress shielding if not combined with proper biological augmentation.
*
Intramedullary Nails
: Provide axial and rotational stability, load sharing, and often promote revascularization through reaming. Exchange nailing for tibial or femoral nonunions is often highly effective due to improved stability and biological stimulus from reaming.
*
External Fixators
: Offer versatile fixation, particularly in infected nonunions, open fractures with significant soft tissue injury, or for limb reconstruction via distraction osteogenesis (Ilizarov, Taylor Spatial Frame). They allow for meticulous control of stability and compression/distraction.
Indications & Contraindications
The decision to intervene surgically for a nonunion is based on a comprehensive assessment of the patient's symptoms, functional demands, radiographic findings, and overall health status.
Indications for Surgical Intervention
- Established Nonunion : Clinical and radiographic confirmation of a nonunion, typically after conservative management (if appropriate) has failed.
- Persistent Pain : Significant pain at the fracture site interfering with daily activities, despite pain management.
- Functional Deficit : Impairment of limb function, muscle weakness, gait disturbance, or inability to bear weight.
- Progressive Deformity : Worsening angulation, rotation, or shortening of the limb due to an unstable nonunion.
- Instability : Gross motion at the fracture site on clinical examination, or significant instability on stress radiographs.
- Infection : Presence of an infected nonunion, requiring surgical debridement and stabilization.
- Anticipated Pathological Fracture : For patients with underlying bone pathology (e.g., tumors) where a nonunion could progress to a pathological fracture.
Contraindications for Surgical Intervention
Absolute contraindications are rare and usually relate to the patient's general health, whereas relative contraindications involve a careful risk-benefit analysis.
*
Absolute Contraindications
:
*
Active Systemic Infection
: Unless the surgery is to address the source of infection (e.g., infected nonunion).
*
Uncontrolled Medical Comorbidities
: Severe cardiac, pulmonary, or neurological conditions that preclude safe anesthesia and surgery.
*
Patient Refusal
: Competent patient declines surgical intervention.
*
Relative Contraindications
:
*
Minimal Symptoms/Functional Impact
: An asymptomatic nonunion that does not significantly affect the patient's quality of life or function may be managed conservatively, especially in low-demand patients.
*
Advanced Age/Frailty
: Increased surgical risk may lead to non-operative management if functional goals are limited.
*
Severe Soft Tissue Compromise
: If the soft tissue envelope is severely damaged or insufficient for closure, necessitating delayed intervention or advanced reconstructive techniques.
*
Non-compliance
: Patients unwilling or unable to adhere to post-operative protocols (e.g., weight-bearing restrictions, smoking cessation).
Operative vs. Non-Operative Indications
| Indication Category | Operative Management | Non-Operative Management |
|---|---|---|
| Nonunion Status | Established nonunion (clinical & radiographic) | Delayed union with progression toward healing |
| Symptoms | Persistent pain, significant functional deficit, instability | Asymptomatic or mild, manageable pain, minimal functional impact |
| Radiographic Features | No bridging callus, widening fracture gap, sclerotic bone ends, deformity | Evidence of ongoing callus formation, stable fracture, no progressive deformity |
| Infection | Diagnosed infected nonunion | Absence of infection |
| Patient Factors | Medically fit, compliant, high functional demand | Medically unfit for surgery, non-compliant, low functional demand |
| Specific Modalities | Revision internal fixation (plates/nails), bone grafting, external fixation, limb reconstruction | Pulsed electromagnetic fields (PEMF), low-intensity pulsed ultrasound (LIPUS), shockwave therapy (SWT) for select cases |
| Treatment Failure | Failed non-operative treatment attempts | N/A |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for optimizing outcomes in nonunion surgery. This phase involves a comprehensive assessment of the nonunion characteristics, patient comorbidities, and formulation of a detailed surgical strategy.
Diagnostic Evaluation
- Clinical Assessment : Detailed history (injury mechanism, previous surgeries, comorbidities, smoking, medications), physical examination (pain, stability, deformity, neurovascular status, soft tissue integrity, signs of infection).
-
Radiographic Studies
:
- Standard Radiographs : AP and lateral views, often oblique views, to assess fracture gap, bone quality, deformity, and existing hardware. Weight-bearing views may be indicated if partial weight-bearing is allowed to assess stability.
- Computed Tomography (CT) : Essential for precise 3D evaluation of bone loss, nonunion morphology (atrophic vs. hypertrophic), articular involvement, and precise hardware position. Thin cuts with 3D reconstructions are invaluable.
- Magnetic Resonance Imaging (MRI) : Useful for assessing soft tissue viability, edema, muscle atrophy, and may provide clues for occult infection (though less specific than other modalities).
- Nuclear Medicine Scans : Bone scan (Technetium-99m) can assess metabolic activity but is non-specific. Indium-111 labeled leukocyte scans or combined leukocyte/marrow scans (Technetium-99m sulfur colloid) are more specific for infection, particularly useful in the presence of metallic implants. PET/CT with FDG may also be employed for infection detection.
Infection Workup
The presence of infection must be rigorously excluded, as an undiagnosed infection is a primary cause of treatment failure.
*
Laboratory Markers
: Elevated C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) are suggestive but non-specific. Procalcitonin may also be elevated.
*
Aspiration
: Aspiration of the nonunion site for Gram stain, aerobic and anaerobic cultures, and potentially fungal and atypical mycobacterial cultures is crucial, especially in revision cases. Histopathology of tissue samples (e.g., intraoperative biopsies) can reveal inflammatory cells indicative of infection.
*
Molecular Diagnostics
: Alpha-defensin tests on synovial fluid or tissue are highly sensitive and specific for periprosthetic joint infection and can be useful in nonunion settings.
Patient Optimization
- Systemic Factors : Aggressive management of comorbidities (diabetes, vascular disease), smoking cessation (ideally >6 weeks pre-op), nutritional optimization (addressing vitamin D deficiency, hypoalbuminemia).
- Antibiotic Prophylaxis : Standard pre-operative intravenous antibiotics, adjusted based on culture results if infection is suspected.
- Blood Management : Type and cross-match for potential transfusions, especially in complex cases requiring significant debridement or bone graft harvest.
Surgical Planning
- Hardware Removal : Decide whether existing hardware needs to be removed. In infected nonunions, explantation is often necessary.
- Fixation Strategy : Determine the type of revision fixation (e.g., exchange nailing, revision plating with compression or bridging, external fixation). Select appropriate implant size and type.
- Bone Grafting : Plan for bone graft harvest (autograft: iliac crest, fibula; allograft) or the use of bone graft substitutes/biologics.
- Deformity Correction : Pre-operative templates, possibly using 3D models from CT scans, to plan for osteotomies and correction of any malunion component.
- Soft Tissue Coverage : Assess the need for plastic surgery consultation for local or free flap coverage if soft tissue deficits are anticipated, particularly in open fractures or previous failed interventions.
Patient Positioning
Positioning depends entirely on the nonunion location and the chosen surgical approach.
*
General Principles
: Ensure patient safety, maintain anatomical alignment, allow adequate access to the nonunion site and potential bone graft donor sites (e.g., iliac crest), and facilitate intraoperative imaging (fluoroscopy).
*
Common Positions
:
*
Supine
: For femoral nonunions (anterior approaches), distal tibial nonunions (anterior approaches), upper extremity nonunions. May require a bump for certain areas.
*
Lateral Decubitus
: For proximal humeral, femoral, or posterior tibial nonunions.
*
Prone
: For posterior spinal nonunions or posterior approaches to lower extremities.
*
Draping
: Wide sterile field, typically from the hip to the foot for lower extremity nonunions, or from shoulder to hand for upper extremity. This allows flexibility for various approaches and bone graft harvesting. Ensure limb mobility for reduction maneuvers and full joint range of motion if required.
Detailed Surgical Approach / Technique
The core principles guiding the surgical management of nonunions involve creating an optimal biological and mechanical environment for healing. This often necessitates a combination of aggressive debridement, stable fixation, and biological augmentation with bone graft.
General Principles of Nonunion Surgery
-
Debridement and Resection : The first critical step, especially for atrophic or infected nonunions. This involves excising all non-viable, sclerotic, and fibrous tissue from the fracture gap, including any pseudarthrosis membrane. Debridement should continue until punctate bleeding is observed from the bone ends, indicating viable bone. In cases of infected nonunion, this is typically accompanied by copious irrigation with pulsatile lavage and collection of tissue samples for culture and histopathology. The goal is to convert an uninfected nonunion into an acute fracture environment or an infected nonunion into a clean, well-vascularized bed.
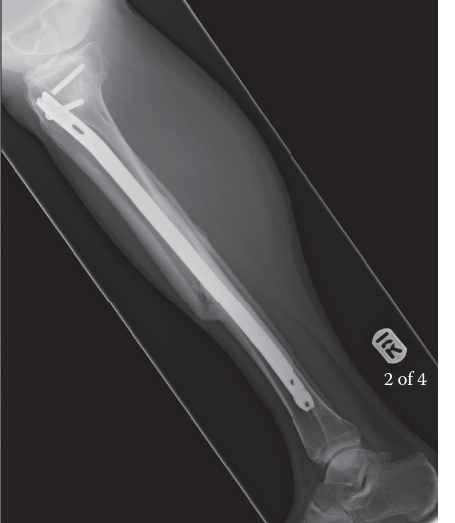
Figure 2: Intraoperative view during debridement of a tibial nonunion. Note the fibrous tissue and sclerotic bone ends that require excision until viable, bleeding bone is reached. -
Correction of Deformity and Gap Management : Any existing malalignment (angulation, rotation, shortening) must be corrected to restore anatomical alignment and function. Significant bone loss or aggressive debridement can result in a critical-sized bone defect. Strategies for gap management include:
- Acute Shortening and Compression : If limb length discrepancy is acceptable or can be managed later.
- Bone Grafting : Filling the defect with autograft, allograft, or bone graft substitutes.
- Distraction Osteogenesis : Using external fixation (e.g., Ilizarov, spatial frame) to gradually lengthen the limb and fill the gap over time, particularly for large defects.
-
Achieving Stable Fixation : The chosen fixation method must provide adequate stability for the nonunion to heal, considering the bone quality, nonunion type, and patient's activity level.
- Compression : For hypertrophic nonunions, direct compression across the fracture site is often key to stimulating healing. This can be achieved with lag screws, compression plates (e.g., dynamic compression plate), or external fixators.
- Load Sharing : Intramedullary nails are excellent load-sharing devices, which is advantageous for long bone nonunions, as they allow for some controlled micromotion while providing axial stability. Exchange nailing (removing a prior nail and reaming for a larger diameter nail) is particularly effective in tibial and femoral nonunions due to reaming's biological stimulus and improved mechanical fit.
- Bridging Fixation : For comminuted or bone loss nonunions, locking plates can provide stable bridging fixation, preventing excessive strain at the nonunion site.
- External Fixation : Indicated for infected nonunions, open fractures, or where internal fixation is not feasible due to soft tissue issues. Circular frames (Ilizarov, TSF) allow for precise control of compression/distraction and deformity correction.
-
Biological Augmentation (Bone Grafting) : For atrophic nonunions, or any nonunion with compromised biology, bone grafting is essential to provide osteogenic, osteoinductive, and osteoconductive properties.
-
Autogenous Bone Graft (Autograft)
: Considered the gold standard.
- Cancellous Autograft : Typically harvested from the iliac crest (anterior or posterior) or proximal tibia. Provides osteoprogenitor cells (osteogenic), growth factors (osteoinductive), and a scaffold (osteoconductive). It is often placed directly into the debrided nonunion gap.
- Corticocancellous Autograft : Provides structural support in addition to biological properties. Can be used for small defects.
- Vascularized Bone Graft (e.g., Vascularized Fibula Graft) : Indicated for large bone defects (>6-8 cm), avascular necrosis, or recalcitrant nonunions. It introduces a live, vascularized bone segment that can remodel and incorporate.
- Allograft : Demineralized bone matrix (DBM) or cancellous chips provide an osteoconductive and osteoinductive scaffold but lack osteogenic cells. They can augment autograft or be used in non-critical defects.
-
Bone Graft Substitutes/Biologics
:
- Ceramics : Hydroxyapatite, tricalcium phosphate. Osteoconductive.
- Growth Factors : Bone morphogenetic proteins (BMPs, particularly BMP-2 and BMP-7) are potent osteoinductive agents. They are used off-label in some countries or for specific indications to stimulate bone formation.
- Platelet-Rich Plasma (PRP) : Contains growth factors, but evidence for efficacy in nonunions is mixed.
- Mesenchymal Stem Cells (MSCs) : Emerging therapeutic, can differentiate into osteoblasts. Often used in conjunction with a scaffold.
-
Autogenous Bone Graft (Autograft)
: Considered the gold standard.
Step-by-Step Example: Management of a Tibial Shaft Nonunion
This example illustrates the principles applied to a common long bone nonunion.
-
Patient Positioning and Exposure :
- Patient positioned supine on a radiolucent table. Tourniquet application to the thigh (if permissible).
- Preparation and draping from above the ipsilateral iliac crest (for potential bone graft harvest) to the toes.
- Incision directly over the nonunion site, typically via the previous surgical incision if present. For the tibial shaft, this often involves an anterior or anterolateral approach, carefully preserving the soft tissue envelope and periosteum where viable.
- Careful dissection through subcutaneous tissue, identifying and protecting neurovascular structures (e.g., superficial peroneal nerve, saphenous nerve).
- Subperiosteal exposure of the nonunion site.
-
Debridement and Preparation of Bone Ends :
- Identification of the pseudarthrosis. Excision of all fibrous tissue, sclerotic bone, and avascular fragments from the nonunion gap using osteotomes, burrs, and rongeurs.
- The goal is to achieve broad, viable bone surfaces at the nonunion site, indicated by punctate bleeding.
- Deformity correction is performed at this stage. If significant shortening has occurred or is anticipated, strategies for lengthening or acute shortening must be implemented.
-
Bone Graft Harvest (if autograft planned) :
- If posterior iliac crest graft is chosen, the patient may need to be re-positioned or the procedure performed simultaneously by a second team. Anterior iliac crest graft is harvested concurrently.
- A separate incision is made. Corticocancellous strips and cancellous chips are harvested as needed, ensuring sufficient quantity to fill the nonunion gap and augment healing. Closure of the donor site is performed meticulously.
-
Fixation Strategy (Example: Exchange Nailing for Tibial Nonunion) :
- If a previous intramedullary nail is present, it is removed.
- The medullary canal is reamed sequentially to a larger diameter than the previous nail or the initial nail in primary cases. This achieves cortical contact proximally and distally, stimulates bleeding from the endosteum, and removes sclerotic bone.
- A larger diameter, often stronger, intramedullary nail is inserted.
- Distal and proximal locking screws are placed to achieve absolute rotational and axial stability. Dynamic locking may be considered in certain cases.
- Alternatively, for plating: A contoured locking plate or dynamic compression plate is applied. Compression across the nonunion site is achieved using lag screws or eccentrically placed screws if applicable. Bone graft is then packed around the nonunion site.
-
Bone Graft Application :
- The harvested autograft (or other chosen graft material) is packed circumferentially into and around the debrided nonunion site, ensuring maximal contact with viable bone and adequate fill of the defect. This is critical for biological stimulation.
-
Wound Closure :
- Copious irrigation of the wound.
- Closure of deep fascial layers and subcutaneous tissue.
- Skin closure, often with drains if significant dead space or fluid collection is anticipated.
- Application of a sterile dressing. A cast or splint may be applied for additional protection depending on the stability of the construct.
Complications & Management
Despite meticulous surgical technique, complications can arise in nonunion surgery, often requiring further intervention. Their management requires a systematic approach and understanding of their incidence.
Common Complications and Management Strategies
| Complication | Incidence | Salvage Strategies |
|---|---|---|
| Persistent Nonunion | 5-15% of revisions | Re-revision surgery with alternative fixation (e.g., plate to nail, external fixator), aggressive debridement, vascularized bone graft (e.g., free fibula), distraction osteogenesis, pulsed electromagnetic fields (PEMF) or low-intensity pulsed ultrasound (LIPUS) as adjuncts. |
| Infection (Superficial/Deep) | 2-10% | Superficial : Local wound care, oral antibiotics. Deep : Surgical debridement, intravenous antibiotics (culture-directed), implant retention (if stable and early) vs. implant removal (if unstable or late), staged reconstruction (e.g., external fixator followed by delayed internal fixation and bone graft). |
| Hardware Failure | 5-10% | Often a sign of persistent nonunion; requires revision surgery, removal of failed hardware, new fixation (stronger construct, different modality), and typically bone grafting. Evaluate for underlying infection. |
| Malunion | 3-8% | Corrective osteotomy (if symptomatic and functional deficit), often with internal fixation. Requires precise pre-operative planning and intraoperative execution. |
| Nerve Injury | <1-3% | Neurapraxia : Observation, physiotherapy. Axonotmesis/Neurotmesis : Neurolysis, nerve repair, or grafting depending on the extent of injury and functional deficit. |
| Vascular Injury | Rare (<1%) | Immediate surgical exploration, primary repair or interpositional vein grafting by vascular surgeon. Compartment syndrome monitoring. |
| Hematoma/Seroma | 2-5% | Aspiration (sterile technique), compression dressings, possibly drain placement. Large or symptomatic hematomas may require surgical evacuation. |
| Donor Site Morbidity | 5-20% | Pain : Analgesics, nerve blocks. Numbness : Reassurance, observation. Hernia : Surgical repair. Fracture : Open reduction and internal fixation (ORIF). Infection : Debridement, antibiotics. |
| Stiffness/Arthrofibrosis | Variable (depending on joint) | Early physiotherapy, continuous passive motion (CPM) where indicated. Manipulation under anesthesia (MUA), arthrolysis. |
| Deep Vein Thrombosis (DVT)/Pulmonary Embolism (PE) | <1-5% | Prophylactic anticoagulation (chemical/mechanical). Treatment involves therapeutic anticoagulation, rarely IVC filter placement. |
Principles of Complication Management
- Early Recognition : Prompt identification of complications through clinical vigilance and appropriate diagnostic studies is key to effective management.
- Systematic Workup : For suspected infection, a comprehensive workup (labs, imaging, aspiration, cultures) is mandatory prior to re-intervention.
- Multidisciplinary Approach : Complex complications, especially infection or significant soft tissue deficits, often require collaboration with infectious disease specialists, plastic surgeons, and vascular surgeons.
- Addressing the Root Cause : Salvage strategies must address why the initial treatment failed. Was it biological (infection, avascularity) or mechanical (unstable fixation, excessive strain)?
- Patient Counseling : Open and honest communication with the patient about the nature of the complication, prognosis, and potential need for further surgery is crucial.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is a critical component of successful nonunion management, designed to protect the surgical repair while progressively restoring function. Protocols vary significantly based on the nonunion location, type of fixation, bone quality, and patient-specific factors.
General Principles
- Protection of Fixation : The primary goal in the early post-operative period is to protect the newly achieved stability at the nonunion site. This often involves a period of non-weight-bearing or protected weight-bearing.
- Early Motion : While protecting the nonunion, early range of motion (ROM) of adjacent joints is encouraged to prevent stiffness and promote cartilage health.
- Progressive Loading : As radiographic signs of healing emerge and clinical stability improves, weight-bearing or loading is gradually increased. Controlled micromotion within a stable construct can stimulate bone healing.
- Muscle Strengthening : Progressive strengthening exercises for muscles crossing the affected joint are introduced to improve stability, power, and functional recovery.
- Functional Restoration : The ultimate goal is to return the patient to their highest possible level of function, including activities of daily living and work/sport.
Phased Rehabilitation Approach
Phase I: Early Protection and Inflammation Control (Weeks 0-6)
- Goals : Protect the surgical site, minimize pain and swelling, maintain adjacent joint ROM, prevent muscle atrophy.
- Weight-Bearing : Typically non-weight-bearing (NWB) or touch-down weight-bearing (TDWB) for lower extremity nonunions. For upper extremity, activity of daily living (ADL) restrictions apply.
- Motion : Passive or active-assisted ROM exercises for adjacent joints, avoiding direct stress on the nonunion site. For instance, knee ROM for tibial nonunions, elbow/shoulder ROM for humeral nonunions.
- Exercises : Gentle isometric contractions of muscles proximal and distal to the nonunion site. Core stability exercises.
- Modalities : Ice, compression, elevation to control edema. Pain management.
Phase II: Gradual Loading and Early Strengthening (Weeks 6-12)
- Goals : Gradually increase load, initiate light strengthening, improve ROM, promote bone healing.
- Weight-Bearing : Progressive weight-bearing (PWB) as tolerated, guided by clinical stability and radiographic evidence of early callus. For lower extremity, this progresses from partial to full weight-bearing with assistive devices.
- Motion : Active ROM exercises. Gentle stretching to improve flexibility.
- Exercises : Low-impact strengthening (e.g., theraband, light weights). Proprioceptive exercises (e.g., balance board) once weight-bearing permits.
- Monitoring : Regular clinical and radiographic follow-up to assess healing progression.
Phase III: Advanced Strengthening and Functional Return (Weeks 12-24+)
- Goals : Restore full strength, endurance, and functional capacity. Prepare for return to desired activities.
- Weight-Bearing : Full weight-bearing without assistive devices.
- Motion : Full, pain-free ROM in all planes.
- Exercises : Progressive resistance training. Plyometric exercises (if appropriate for the nonunion location and patient goals). Sport-specific drills. Gait training refinement.
- Monitoring : Continue radiographic assessment until definitive union is achieved. Clinical evaluation for pain, strength, and function.
Specific Considerations
- External Fixation : Rehabilitation with external fixators requires specific care regarding pin sites and potential frame adjustments. Gradual weight-bearing and early motion are often integrated into the frame design (e.g., dynamic external fixators). Distraction osteogenesis protocols involve daily adjustments and precise monitoring.
- Vascularized Grafts : Initial protection of the vascularized graft is paramount, often requiring a longer period of non-weight-bearing.
- Patient Education : Emphasize the importance of adherence to protocols, especially regarding weight-bearing restrictions, and the risks associated with non-compliance (e.g., refracture, hardware failure). Smoking cessation remains critical throughout healing.
- Psychological Support : Nonunion patients often face prolonged recovery and psychological distress. Support and realistic expectations are essential.
Summary of Key Literature / Guidelines
The management of nonunion fractures is a continuously evolving field, supported by a growing body of literature ranging from basic science to large clinical trials. Current practices are often informed by consensus guidelines and systematic reviews.
Diagnostic Algorithms
- The Orthopaedic Trauma Association (OTA) and other national bodies emphasize a structured diagnostic algorithm, beginning with thorough clinical evaluation and standard radiographs, progressing to CT scans for detailed bone morphology and surgical planning, and incorporating advanced imaging (MRI, nuclear medicine scans) when infection is suspected or soft tissue assessment is critical.
- The role of serological markers (ESR, CRP, procalcitonin, alpha-defensin) in ruling out infection is well-established, particularly in the context of revision surgery. Aspiration with culture remains the gold standard for definitive diagnosis of osteomyelitis.
Treatment Modalities and Evidence
-
Surgical Intervention : The consensus is that surgical intervention is generally required for established symptomatic nonunions, particularly atrophic and infected types.
- Mechanical Stability : Multiple studies support the principle that achieving adequate mechanical stability is paramount for hypertrophic nonunions. Exchange nailing for femoral and tibial nonunions has demonstrated success rates of 80-95%, often considered a first-line revision strategy when appropriate. The biological stimulus of reaming and improved stability are key factors.
- Biological Augmentation : For atrophic nonunions, autogenous bone graft remains the gold standard for biological enhancement, providing osteoinductive, osteoconductive, and osteogenic elements. Studies show significantly improved union rates when autograft is combined with stable fixation for atrophic nonunions.
- Vascularized Fibula Grafts : Indicated for large segmental bone defects (>6-8 cm) and recalcitrant nonunions, demonstrating high success rates in complex limb salvage cases (e.g., Papineau technique). Meta-analyses highlight their efficacy but acknowledge the donor site morbidity and technical complexity.
- Bone Morphogenetic Proteins (BMPs) : While approved for specific indications (e.g., open tibial fractures requiring reamed IMN, lumbar spinal fusion), their off-label use in established nonunions, particularly for critical-sized defects, is supported by some clinical series, but large-scale, high-level evidence demonstrating superiority over autograft or cost-effectiveness in routine nonunion management is still debated. BMP-7 (OP-1) and BMP-2 have shown promise in accelerating union in challenging cases.
- External Fixation (e.g., Ilizarov, Spatial Frames) : Highly effective for infected nonunions, nonunions with significant bone loss, or complex deformities. The ability to control stability, compression, and distraction osteogenesis simultaneously offers versatile solutions for challenging cases.
-
Non-Operative Adjuncts :
- Pulsed Electromagnetic Fields (PEMF) and Low-Intensity Pulsed Ultrasound (LIPUS) : These modalities are FDA-approved and have been shown to accelerate healing in delayed unions and some established nonunions, particularly in cases where surgery is contraindicated or as an adjunct. However, their efficacy is higher in delayed unions than in established, atrophic nonunions. Systematic reviews suggest a modest benefit, but the quality of evidence varies.
- Extracorporeal Shockwave Therapy (ESWT) : Emerging evidence suggests potential benefits in recalcitrant nonunions, possibly by stimulating angiogenesis and osteogenesis, though more high-quality studies are needed.
Consensus and Emerging Trends
- There is a strong consensus on the need for multidisciplinary care for complex nonunions, involving orthopedic surgeons, infectious disease specialists, plastic surgeons, and rehabilitation therapists.
- Patient optimization , particularly smoking cessation and nutritional support, is increasingly emphasized as a critical pre-operative and post-operative factor influencing union rates.
- The concept of personalized medicine in nonunion management is gaining traction, with a focus on understanding the patient's individual biological and mechanical factors to tailor treatment. This includes genetic predispositions, specific biomarker analysis, and advanced tissue characterization.
- Research into stem cell therapies (e.g., mesenchymal stromal cells) and novel growth factor delivery systems continues to evolve, aiming to provide more potent biological augmentation strategies, though these are largely experimental or investigational at present.
- 3D printing and custom implants are being used for complex bone loss cases, allowing for precise restoration of anatomy and mechanical stability.
In conclusion, effective management of fracture nonunion requires a holistic approach, integrating precise diagnosis, meticulous surgical planning and execution, judicious biological augmentation, and comprehensive post-operative rehabilitation, all guided by the best available evidence and current understanding of bone healing mechanobiology.
