Ipsilateral Femoral Neck & Shaft Fractures: A Comprehensive Management Guide
Key Takeaway
Ipsilateral femoral neck and shaft fractures are complex, high-energy injuries. The femoral neck fracture is often missed, risking avascular necrosis. Optimal management involves prompt anatomical reduction and stable fixation of both components. This requires a deep understanding of surgical anatomy and biomechanics to preserve femoral head vascularity and ensure successful patient outcomes.
Ipsilateral Femoral Neck & Shaft Fractures: Guide to Management
Introduction & Epidemiology
Ipsilateral femoral neck and shaft fractures represent a rare but challenging injury pattern, often resulting from high-energy trauma. The reported incidence varies widely, ranging from 2.5% to 9% of all femoral shaft fractures, but is likely underreported due to missed diagnoses. These injuries typically affect young, otherwise healthy individuals involved in motor vehicle collisions, falls from height, or industrial accidents. The energy transfer required to generate both a neck and shaft fracture concurrently underscores the severity of the initial trauma, frequently leading to associated injuries in up to 50-90% of cases, including head trauma, thoracic and abdominal injuries, and other musculoskeletal pathologies.
Historically, the femoral neck fracture component was notoriously missed, with diagnostic delays occurring in 19-50% of cases, primarily due to the obvious displacement of the femoral shaft fracture drawing immediate attention. Such delays significantly increase the risk of devastating complications, notably avascular necrosis (AVN) of the femoral head and femoral neck nonunion. Prompt recognition and accurate characterization of both fracture components are paramount for successful outcomes. Advances in imaging, particularly the routine use of computed tomography (CT) scans, have significantly improved diagnostic accuracy.
The management of ipsilateral femoral neck and shaft fractures demands a comprehensive understanding of complex fracture biomechanics, advanced surgical techniques, and meticulous attention to detail. The primary goals are anatomical reduction and stable fixation of both the femoral neck and shaft, restoration of limb length and alignment, preservation of femoral head vascularity, and early mobilization to prevent secondary complications. The choice of surgical implant and approach is dictated by the specific fracture patterns, patient comorbidities, surgeon experience, and available resources.
Surgical Anatomy & Biomechanics
A thorough understanding of femoral anatomy and biomechanics is critical for the effective management of these injuries.
Femoral Head and Neck Vascularity
The blood supply to the femoral head is predominantly derived from the medial and lateral circumflex femoral arteries, which give rise to the retinacular arteries (superior, inferior, anterior, posterior). These arteries ascend along the femoral neck within the synovial reflection and capsule, supplying the majority of the femoral head. The artery of the ligamentum teres (a branch of the obturator artery) provides a variable and often minor contribution, particularly in adults, becoming more important in pediatric populations or in cases of retinacular artery compromise. Femoral neck fractures, especially displaced ones (Garden III and IV), disrupt these critical retinacular vessels, placing the femoral head at high risk for ischemia and subsequent avascular necrosis. The posterior superior retinacular artery is considered the most critical.
Femoral Neck Morphology & Biomechanics
The femoral neck is an angled structure, exhibiting anteversion (typically 10-20 degrees) and an angle of inclination (normally 120-135 degrees) relative to the femoral shaft. These angles are crucial for hip joint mechanics and gait. Femoral neck fractures can be classified by location (subcapital, transcervical, basicervical), displacement (Garden classification), and fracture obliquity (Pauwel's classification). Displaced subcapital and transcervical fractures carry the highest risk of AVN due to extensive disruption of retinacular vessels. Basicervical fractures, being extracapsular, have a better prognosis for vascularity but still require stable fixation.
Femoral Shaft Morphology & Biomechanics
The femoral shaft is the longest and strongest bone in the human body, designed to withstand significant axial and torsional loads. Its bowed anterior curve and isthmic narrowing are important considerations for intramedullary nailing. Femoral shaft fractures are classified by location (proximal, mid-diaphyseal, distal) and morphology (spiral, oblique, transverse, comminuted) using the AO/OTA classification system. The muscular attachments (quadriceps, adductors, hamstrings) can lead to characteristic displacement patterns. For instance, proximal shaft fractures often exhibit flexion and abduction of the proximal fragment due to iliopsoas and gluteus medius/minimus pull, while distal fractures may demonstrate flexion of the distal fragment due to gastrocnemius pull.
Interplay of Injuries
The ipsilateral nature of these fractures presents unique biomechanical challenges. Fixation of the femoral shaft fracture must not compromise the integrity or stability of the femoral neck fixation. The chosen implants must withstand the combined forces across both fracture sites. For example, a stress riser can be created at the junction of the femoral neck implant and the intramedullary nail if not meticulously planned, increasing the risk of subsequent fracture or hardware failure. The ability to achieve anatomical reduction of the femoral neck fracture is paramount, as residual displacement significantly correlates with AVN and nonunion.
Indications & Contraindications
Management of ipsilateral femoral neck and shaft fractures is almost universally operative in physiologically stable patients.
Operative Indications
- All displaced or potentially unstable femoral neck fractures: This includes Garden II, III, and IV fractures, as well as unstable Garden I fractures. Anatomical reduction is critical.
- All femoral shaft fractures: Except in rare, highly selected cases, femoral shaft fractures require operative stabilization.
- Polytrauma patients requiring early mobilization: Stable fixation allows for essential nursing care, pulmonary hygiene, and transfer, preventing complications associated with prolonged immobilization.
- Pathologic fractures: While less common in this context, certain underlying bone pathologies may necessitate stabilization.
- Impending compartment syndrome: Although rare, progressive swelling and pain might indicate a need for surgical intervention.
Non-Operative Indications
Non-operative management for ipsilateral femoral neck and shaft fractures is extremely rare and typically reserved for patients who are not physiologically capable of tolerating surgery.
- Physiological instability (hemodynamic instability, severe head injury): In cases where the patient's overall medical condition precludes operative intervention, temporary external fixation or skeletal traction may be used as a damage control orthopedics measure. Definitive fixation is then performed once the patient is stable.
- Severe comorbidities: Patients with significant co-existing medical conditions that pose an unacceptably high anesthetic or surgical risk.
- Non-viable limb: In extreme cases of severe open injury or degloving that result in a non-viable limb, amputation may be indicated, precluding fracture fixation.
Summary of Indications
| Feature | Operative Management | Non-Operative Management |
|---|---|---|
| Femoral Neck Fracture | Garden I (unstable), Garden II, III, IV: All displaced or potentially unstable fractures requiring anatomical reduction and stable internal fixation to preserve vascularity and prevent AVN/nonunion. | Rare: Only in physiologically unstable patients where surgery is contraindicated. May involve skeletal traction for damage control, but definitive fixation is typically planned. |
| Femoral Shaft Fracture | All types (spiral, oblique, transverse, comminuted): Stable fixation to restore length, alignment, and rotation. Enables early mobilization and reduces complications associated with prolonged bed rest. | Rare: Reserved for patients with absolute contraindications to surgery (e.g., critical physiological instability, non-viable limb). May involve skeletal traction or external fixation as temporary measures until patient stabilization. |
| Patient Physiological Status | Hemodynamically stable: Patients who can tolerate general anesthesia and surgery. | Hemodynamically unstable/Critically ill: Patients with severe polytrauma, uncontrollable bleeding, severe head injury, or overwhelming comorbidities where surgical stress is deemed life-threatening. May undergo damage control orthopedics (e.g., external fixation) followed by definitive surgery once stable. |
| Associated Injuries | Management often prioritized in polytrauma protocols once life-threatening conditions are addressed. Stable orthopedic fixation facilitates definitive management of other injuries and aids rehabilitation. | In overwhelming polytrauma, orthopedic stabilization may be delayed until the patient is resuscitated and stabilized, sometimes utilizing temporary external fixation. |
| Limb Viability | Viable limb with salvageable fracture pattern. | Non-viable limb where primary amputation is indicated. |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for optimizing outcomes in these complex injuries.
Imaging and Diagnosis
- Radiographs: Anteroposterior (AP) pelvis, AP and lateral views of the entire femur including the hip and knee. Careful scrutiny of the femoral neck region is mandatory, as subtle neck fractures can be missed on standard shaft films.
- Computed Tomography (CT) Scan: Essential for definitive diagnosis and characterization of the femoral neck fracture. A CT hip and femur with thin cuts (1-2mm) through the neck allows for precise assessment of fracture morphology, displacement, and comminution. It also helps detect associated posterior wall or acetabular fractures. CT angiography may be considered if vascular injury is suspected in severe polytrauma.
- Magnetic Resonance Imaging (MRI): Not typically used for acute diagnosis but can be valuable in detecting occult femoral neck fractures or assessing femoral head vascularity in delayed presentations if suspicion for AVN is high.
Patient Workup and Optimization
- Polytrauma Protocol: Given the high-energy mechanism, patients must undergo a thorough Advanced Trauma Life Support (ATLS) protocol. Life-threatening injuries (e.g., hemorrhage, head trauma, chest trauma) take precedence. Orthopedic stabilization often follows resuscitation.
- Medical Optimization: Address coagulopathy, optimize cardiac and pulmonary status, manage pain, and administer prophylactic antibiotics.
- Timing of Surgery: Ideally, definitive fixation should be performed within 24-48 hours, especially for displaced femoral neck fractures, to minimize the risk of AVN. However, in critically ill polytrauma patients, temporary external fixation may be used (damage control orthopedics) with definitive fixation delayed until physiological stability is achieved.
Implant Selection
The choice of implants is critical and often a source of debate. Options include:
1.
Cephalomedullary Nail (Recon Nail):
A long intramedullary nail with an integrated lag screw (or two screws) directed into the femoral head. This is often the preferred option as it provides unified fixation of both fractures.
2.
Standard Antegrade Intramedullary Nail for the Shaft + Separate Cannulated Screws for the Neck:
Requires precise placement of neck screws to avoid collision with the nail. This approach allows for independent reduction and fixation of each fracture.
3.
Plate for the Shaft + Separate Cannulated Screws for the Neck:
Generally less favored due to the extensive soft tissue dissection required for plating, increased blood loss, and higher risk of infection, especially in polytrauma. However, it may be indicated for very distal shaft fractures where an IM nail might not provide adequate distal fixation, or in specific comminuted patterns.
Pre-operative templating with radiographs and CT scans is essential to determine nail length, diameter, and optimal lag screw length and position.
Patient Positioning
- Supine Position on a Radiographic Traction Table: This is the most common and often preferred position, especially for antegrade nailing. It allows for closed reduction of both fractures, fluoroscopic imaging in AP and lateral planes for the entire femur, and facilitates manipulation of the proximal fragment. The contralateral leg is typically placed in a well-padded boot and abducted to provide surgical access.
- Lateral Decubitus Position: Can be used if a traction table is unavailable or if significant soft tissue degloving requires extensive wound care. This position makes reduction of the shaft fracture more challenging and often requires a separate team or prolonged manipulation. Access to the hip joint for femoral neck reduction and fluoroscopy can also be more difficult.
- Considerations: Regardless of position, ensure adequate padding at all pressure points to prevent nerve palsies or skin breakdown. Prepare for potential intraoperative repositioning if necessary, particularly if open reduction of the femoral neck is required. The image intensifier must be positioned to allow full visualization of the hip joint and entire femoral shaft.
Detailed Surgical Approach / Technique
The sequence of reduction and fixation (neck first vs. shaft first) is a critical decision point. While there is no universally agreed-upon "best" approach, many surgeons advocate for achieving anatomical reduction and stable fixation of the femoral neck first, as this is the fracture with the higher potential for devastating complications (AVN, nonunion).
General Principles
- Anatomical Reduction of Femoral Neck: Crucial for preserving blood supply and optimizing biomechanical stability. Aim for valgus reduction if possible, avoiding varus.
- Stable Fixation: Both fractures require rigid internal fixation to allow for early mobilization.
- Restore Length, Alignment, and Rotation: For the femoral shaft.
- Minimize Soft Tissue Stripping: Especially around the femoral neck to protect its vascularity.
- Fluoroscopic Guidance: Indispensable throughout the procedure for accurate reduction and implant placement.
Step-by-Step Technique: Cephalomedullary Nail (Recon Nail)
This is a commonly favored approach due to its ability to address both fractures with a single implant construct, minimizing stress risers between separate implants.
-
Reduction of Femoral Neck Fracture:
- Place the patient supine on a traction table. Apply gentle longitudinal traction and internal rotation to reduce displacement of the femoral neck.
- Assess reduction fluoroscopically (AP and lateral views). If closed reduction is inadequate (e.g., persistent varus, rotation, or displacement >2mm), consider open reduction.
- Open Reduction (if necessary): This can be performed via an anterior Smith-Petersen approach, anterolateral approach, or a modified Hardinge approach, carefully dissecting to visualize the femoral neck. Minimize stripping of the superior and posterior aspects to protect retinacular vessels. Use a ball spike, periosteal elevators, or a small Hohmann retractor to manipulate fragments. Once reduced, temporarily fix with Kirschner wires (K-wires).
-
Guide Wire Insertion for Cephalomedullary Nail:
- Make a longitudinal incision over the greater trochanter (approximately 5-7 cm).
- Identify the piriformis fossa or tip of the greater trochanter. Create an entry portal using an awl or drill. The entry point is crucial: too medial can lead to varus malalignment or iatrogenic fracture; too lateral can lead to inadequate seating of the nail head.
- Insert a guide wire down the femoral shaft, traversing the shaft fracture. Ensure it is centrally placed in both AP and lateral views. This guide wire typically does not go into the femoral head.
-
Reduction of Femoral Shaft Fracture:
- With the femoral neck reduced and potentially temporarily stabilized (K-wires or holding clamp), focus on the shaft.
- Utilize the traction table to achieve length and rotation. Manipulate the fragments manually or with percutaneous clamps. Ensure correct rotation by comparing the patella or foot position to the contralateral limb, or by assessing the cortical step-off under fluoroscopy.
- A second guide wire for the nail is typically passed across the shaft fracture.
-
Reaming and Nail Insertion:
- Once the shaft guide wire is in place and the shaft is reduced, ream the medullary canal. Start with a small diameter reamer and incrementally increase, typically 1.5-2mm larger than the planned nail diameter. Pay attention to reamer pass through the neck fracture site to avoid displacement.
- Insert the cephalomedullary nail. Advance it carefully under fluoroscopic guidance, past the shaft fracture. Ensure proper seating in the proximal fragment without distraction or over-penetration.
-
Femoral Neck Lag Screw Insertion (Cephalomedullary Nail):
- With the nail in place, use the nail's aiming guide to drill for the cephalic lag screw(s) into the femoral head.
- Aim for a central or slightly inferior-central position in the femoral head on the AP view and central in the lateral view (anterior in the inferior portion, posterior in the superior portion) to avoid damage to the retinacular vessels.
- Measure the screw length and insert the lag screw(s). Dynamic compression of the femoral neck fracture can be achieved if the nail design allows for it. Ensure the screws are subchondral but do not penetrate the joint.

Depicts a common construct for ipsilateral femoral neck and shaft fractures, showing a long cephalomedullary nail spanning both fractures with a lag screw for the femoral neck component, as well as a separate construct of a standard IM nail for the shaft combined with separate cannulated screws for the femoral neck. This highlights the primary fixation strategies. -
Distal Locking:
- Perform distal locking of the nail using the aiming device or freehand technique. Confirm all screws are correctly placed and do not impinge on any neurovascular structures.
Step-by-Step Technique: Standard IM Nail + Separate Cannulated Screws
This approach allows independent optimization of each fracture's reduction and fixation.
-
Femoral Neck Fracture Reduction and Fixation (First Priority):
- Position patient supine on a traction table.
- Perform closed or open reduction of the femoral neck fracture, as described above. Anatomical reduction is paramount.
- Temporarily stabilize the neck fracture with K-wires.
- Insert 2-3 cannulated screws (typically 6.5mm or 7.3mm) in an inverted triangle configuration. Place them parallel or slightly converging, ensuring they are subchondral and do not penetrate the joint. The anterior-inferior screw often has the greatest purchase. Ensure the screws are long enough to engage the subchondral bone.
- Crucially, these screws must be placed in a position that will not interfere with the subsequent intramedullary nail for the shaft. This usually means positioning them relatively anterior or posterior in the femoral head and neck, away from the central axis where the nail will traverse. Pre-operative templating is essential for this.
-
Femoral Shaft Fracture Reduction and Fixation:
- Maintain femoral neck fixation with the cannulated screws.
- Proceed with standard antegrade intramedullary nailing of the femoral shaft.
- Create the trochanteric entry portal. This entry point is typically more lateral than for a cephalomedullary nail to avoid the neck screws, aiming for the piriformis fossa or tip of the greater trochanter. Careful planning is needed to avoid impingement on the neck screws.
- Pass the guide wire across the shaft fracture.
- Ream the medullary canal, ensuring not to dislodge the neck screws.
- Insert the standard intramedullary nail into the femoral shaft.
- Perform distal locking.
- Confirm all implant positions with fluoroscopy.
Considerations for Proximal Femoral Shaft Fractures (Subtrochanteric/Intertrochanteric component)
If the shaft fracture has a proximal component that extends into the subtrochanteric or intertrochanteric region, a long cephalomedullary nail (recon nail) becomes even more advantageous as it can better span this proximal metaphyseal-diaphyseal junction and provide superior fixation for these more complex proximal shaft patterns. A standard IM nail may not provide adequate stability for the proximal fragment if the shaft fracture extends very proximally.
Open Fractures
For open ipsilateral fractures, meticulous debridement and copious irrigation are paramount. The timing of definitive fixation may be influenced by the severity of contamination and soft tissue injury. Damage control orthopedics with external fixation may be used initially for grossly contaminated wounds, with delayed conversion to internal fixation.
Complications & Management
Ipsilateral femoral neck and shaft fractures are associated with a higher rate of complications than isolated fractures, primarily due to the severity of trauma and the inherent risks of femoral neck injuries.
Table of Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (%) | Pathophysiology/Clinical Presentation | Salvage Strategy / Management |
|
1. Missed Femoral Neck Fracture
| Reported between 19-50% in historical series, now reduced with widespread CT. | The subtle nature of non-displaced neck fractures, especially subcapital, can be obscured by the prominent shaft fracture. Delays in diagnosis lead to worsening displacement, increased ischemia risk. |
High index of suspicion:
Always assess the femoral neck thoroughly with dedicated radiographs (AP pelvis, cross-table lateral) and a routine CT scan of the hip and entire femur in all cases of femoral shaft fracture. Early anatomical reduction and stable fixation if diagnosed. |
|
2. Femoral Neck Nonunion
| Up to 30% without adequate reduction and fixation. | Failure of union at the femoral neck fracture site. May present with persistent groin pain, difficulty weight-bearing, limb shortening, or deformity. Associated with inadequate fixation, poor vascularity, and biological factors. |
Revision surgery:
Includes hardware removal, debridement of fibrous tissue, bone grafting (vascularized or non-vascularized), and stable revision internal fixation (e.g., dynamic hip screw, multiple cannulated screws, recon nail). Arthroplasty (THA/hemiarthroplasty) may be considered in older patients or those with severe head damage. |
|
3. Avascular Necrosis (AVN) of Femoral Head
| 10-25% in displaced femoral neck fractures, higher with delayed diagnosis. | Death of osteocytes and bone marrow components due to disruption of blood supply. Clinical presentation involves groin pain, limping, and eventual collapse of the femoral head. Diagnosis confirmed by MRI. |
Early Stages:
Core decompression +/- bone grafting or PRP.
Late Stages (Head Collapse):
Total Hip Arthroplasty (THA) is the gold standard for symptomatic collapse. Hemiarthroplasty may be an option in select older, less active patients. |
|
4. Femoral Shaft Nonunion
| 2-5% for closed, up to 15% for open fractures. | Persistent motion or instability at the shaft fracture site after an expected healing period (e.g., 6-9 months). Pain, deformity, progressive shortening, or hardware loosening. Diagnosed by radiographs and often CT scan. |
Revision fixation:
Usually involves exchange nailing (larger diameter nail), dynamization (if statically locked and no callus), revision plating, or external fixation. Often combined with bone grafting (autograft or allograft) for hypertrophic or atrophic nonunions. Removal of failed hardware. |
|
5. Malunion of Femoral Neck
| Up to 20%, depending on initial reduction quality. | Healing of the femoral neck fracture in a deformed position (e.g., varus or rotational malalignment). Leads to altered hip biomechanics, pain, limited range of motion, premature osteoarthritis. Can contribute to AVN risk. |
Corrective osteotomy:
Valgus osteotomy to realign the femoral neck, particularly for varus malunion. May involve revision fixation.
THA:
If symptomatic osteoarthritis or severe deformity is present, especially in older patients. |
|
6. Femoral Shaft Malunion
| 5-10% | Healing in malrotation (most common, often internal rotation), angulation, or shortening. Can lead to functional limitations, pain, abnormal gait, leg length discrepancy, patellofemoral pain. |
Corrective osteotomy:
If symptomatic and functional impairment is significant. Bone lengthening procedures for significant shortening (>2 cm). Revision nailing or plating with meticulous attention to rotational control and alignment. |
|
7. Infection (Peri-prosthetic/Osteomyelitis)
| 1-5% for internal fixation. | Local signs of inflammation, pain, fever, wound drainage, pus. May lead to nonunion, bone destruction, or septic complications. Diagnosis via cultures, inflammatory markers, imaging (X-ray, MRI, bone scan). |
Debridement and antibiotics:
Surgical debridement, copious irrigation, deep cultures, and long-term (6+ weeks) targeted antibiotic therapy.
Hardware removal:
If infection persists or nonunion.
Staged reconstruction:
Debridement, antibiotic spacer, then delayed definitive fixation (e.g., IM nail +/- bone graft).
Amputation:
In severe, uncontrollable cases. |
|
8. Periprosthetic Fracture
| 1-3% with IM nails. | New fracture occurring at the implant ends or due to creation of a stress riser from the implant (e.g., short femoral neck screws with a longer IM nail). Presents as new pain, inability to bear weight. |
Revision fixation:
Often with a longer implant to bypass the new fracture or a plate to augment the nail. Careful planning to avoid new stress risers or compromise existing fixation. |
|
9. Neurovascular Injury
| Rare, but possible with severe trauma. | Direct blunt force, vascular disruption leading to acute ischemia, neuropathy related to stretch, direct trauma, or surgical dissection. |
Immediate exploration:
If vascular injury suspected, emergent vascular repair.
Nerve repair/neurolysis:
If direct nerve injury confirmed. Careful monitoring of compartment pressures post-op. |
|
10. Deep Vein Thrombosis (DVT) & Pulmonary Embolism (PE)
| 1-5% for DVT, <1% for PE (despite prophylaxis). | DVT: Swelling, pain, erythema in affected leg. PE: Acute dyspnea, pleuritic chest pain, cough, hemoptysis, hypoxemia. Both life-threatening. Higher risk in trauma patients. |
Prophylaxis:
Chemical (LMWH or fondaparinux) and mechanical (intermittent pneumatic compression).
Treatment:
Anticoagulation (heparin, LMWH, oral anticoagulants) for DVT/PE. Consider IVC filter for recurrent PE or contraindication to anticoagulation. |
|
11. Compartment Syndrome
| Rare, but critical complication of leg trauma. | Increased pressure within a closed fascial compartment leading to muscle and nerve ischemia. Pain out of proportion to injury, pain on passive stretch, paresthesia, pallor, pulselessness (late sign). |
Emergent fasciotomy:
Decompression of the affected compartment(s) via surgical incisions. Post-operative wound care and delayed closure. |
|
12. Nerve Injuries
| Rare, but possible (e.g., sciatic nerve from direct trauma or traction). | Numbness, weakness, motor deficit in the distribution of the affected nerve. |
Expectant management:
Many traction neurapraxias resolve spontaneously.
Neurolysis/Repair:
Surgical exploration, neurolysis, or nerve repair depending on injury type and severity. |
|
13. Refracture
| Rare, but possible due to residual stress risers or premature removal of hardware. | New fracture at the site of the previous repair or adjacent to the old implant. |
Revision fixation:
Similar to nonunion or periprosthetic fracture management, typically with a longer or stronger implant. |
Post-Operative Rehabilitation Protocols
Early weight-bearing on the affected limb has been shown to be safe and beneficial for femoral shaft fractures, but the presence of an ipsilateral femoral neck fracture necessitates a more nuanced approach to rehabilitation. The primary concern is protecting the healing femoral neck and ensuring sufficient vascular recovery, typically delaying full weight-bearing.
Immediate Post-Operative (Day 0-7)
- Pain Management: Multimodal analgesia including regional blocks, NSAIDs (if no contraindications), acetaminophen, and opioids as needed.
- Wound Care: Daily dressing changes, monitoring for signs of infection.
-
Early Mobilization:
- Bed mobility: Encourage rolling, bridging exercises.
- Upper extremity strengthening: To assist with transfers and crutch ambulation.
- Initiate passive and active assisted range of motion (ROM) for hip and knee: Within pain limits. Focus on flexion and extension, gentle abduction/adduction. Avoid extreme rotation and hip extension that could stress the femoral neck.
- Isometrics: Quad sets, gluteal sets, ankle pumps.
- Weight-Bearing (WB): Typically toe-touch weight-bearing (TTWB) or non-weight-bearing (NWB) on the affected limb, particularly for displaced femoral neck fractures. Partial weight-bearing (PWB) might be considered for stable, non-displaced neck fractures with solid fixation, as per surgeon discretion. Use crutches or a walker for ambulation.
- DVT Prophylaxis: Continue chemical and mechanical prophylaxis.
Early Rehabilitation (Weeks 1-6)
- Progression of ROM: Gradually increase hip and knee ROM, working towards functional ranges (e.g., 0-120 degrees knee flexion, 0-90 degrees hip flexion).
-
Strengthening:
- Begin light resistance exercises for hip flexors, abductors, adductors, extensors, and knee extensors/flexors. Focus on core stability.
- Continue non-weight-bearing exercises (e.g., heel slides, short arc quads).
-
Weight-Bearing (WB):
- Maintain TTWB or NWB if the femoral neck fracture was displaced or concerns about vascularity remain.
- If the neck fracture was non-displaced and deemed highly stable, progression to 25-50% PWB might be initiated around 4-6 weeks, based on radiographic signs of healing and clinical comfort.
- Gait Training: Continue with assistive devices (crutches/walker), focusing on proper gait mechanics with restricted weight-bearing.
- Scar Mobilization: Once wounds are healed, initiate scar massage to prevent adhesions.
Intermediate Rehabilitation (Weeks 6-12)
- Radiographic Assessment: Obtain follow-up X-rays (AP pelvis, AP and lateral femur) at 6-8 weeks and 12 weeks to assess fracture healing and hardware integrity. Look for bridging callus at the shaft and signs of union at the neck.
-
Progression of Weight-Bearing:
- If radiographic healing is progressing well for both fractures and clinical pain is minimal, progress from TTWB/NWB to PWB (50%) between 6-8 weeks.
- Advance to full weight-bearing (FWB) on the affected limb typically between 10-12 weeks, contingent on robust radiographic evidence of union of both the neck and shaft fractures. This progression is slower than for isolated shaft fractures.
- Strengthening: Increase intensity of hip and knee strengthening exercises. Incorporate proprioceptive and balance training. Begin light closed-chain exercises (e.g., mini-squats, leg presses) if FWB is achieved.
- Activity Modification: Avoid high-impact activities, twisting, and heavy lifting.
Advanced Rehabilitation (Weeks 12-24 and Beyond)
- Continue Strengthening: Focus on functional strength, power, and endurance. Incorporate sport-specific or activity-specific drills for returning to work or hobbies.
- Return to Activity: Gradual return to light recreational activities (e.g., cycling, swimming) around 4-6 months, progressing to higher impact activities or sports generally after 6-12 months, and only after complete radiographic union, full strength, and physician clearance.
- Long-Term Monitoring: Patients must be educated about the long-term risk of AVN of the femoral head and potential for post-traumatic arthritis. Regular follow-up with radiographs for 1-2 years post-injury is advisable to monitor for these late complications.
Note: These are general guidelines. Individual rehabilitation protocols must be tailored to the specific fracture patterns, quality of fixation, patient comorbidities, and progress in healing. Close communication between the surgeon and physical therapist is essential.
Summary of Key Literature / Guidelines
The management of ipsilateral femoral neck and shaft fractures has evolved significantly over time, with a general consensus leaning towards surgical stabilization. Key areas of discussion in the literature include diagnosis, timing of surgery, implant selection, and outcomes.
Diagnostic Accuracy
Early literature highlighted the high rate of missed femoral neck fractures (19-50%) in the setting of ipsilateral shaft injuries. This led to a paradigm shift emphasizing thorough imaging. Current guidelines universally recommend a pre-operative CT scan of the hip and entire femur in all cases of femoral shaft fractures to rule out an occult femoral neck fracture. The sensitivity of standard radiographs alone for detecting femoral neck fractures in this context is inadequate.
Timing of Surgery
Prompt surgical fixation, ideally within 24 hours for displaced femoral neck fractures , is crucial to minimize the risk of AVN. While damage control orthopedics (e.g., temporary external fixation) is acceptable for unstable polytrauma patients, definitive fixation should not be unduly delayed once the patient is stable. Studies consistently demonstrate that delays beyond 24-48 hours significantly increase the risk of AVN and nonunion.
Implant Selection: Cephalomedullary Nail vs. Separate Implants
This remains a topic of considerable debate and is often surgeon-dependent.
- Cephalomedullary Nails (Recon Nails): Many authors advocate for cephalomedullary nails due to their single-implant construct, which theoretically provides more unified fixation, avoids creating an additional stress riser between two separate implants, and simplifies the surgical technique. They are particularly favored for subtrochanteric or proximal shaft fractures. Studies by authors like Alho and Watson have demonstrated good results with cephalomedullary nails. However, technical challenges can include proper entry point, difficulty in achieving anatomical neck reduction with the nail in place, and potential for malreduction of the neck.
- Standard Intramedullary Nail for Shaft + Separate Cannulated Screws for Neck: This technique allows for independent reduction and fixation of each fracture, which proponents argue can lead to better anatomical reduction of the femoral neck, as it can be fixed before the shaft nail is inserted. The primary challenge is ensuring appropriate placement of the neck screws to avoid collision with the subsequently placed IM nail. This requires meticulous pre-operative planning and intraoperative fluoroscopic control. It also carries the theoretical risk of creating a stress riser in the area between the most distal neck screw and the proximal tip of the shaft nail. Some studies suggest similar outcomes to recon nails if performed meticulously.
- Plating for Shaft + Separate Screws for Neck: Generally less favored for femoral shaft fractures due to increased soft tissue dissection, higher infection risk, and challenges in maintaining length and rotation. However, it may be indicated in very distal shaft fractures, certain open injuries, or in situations where an IM nail is contraindicated.
A meta-analysis by Bedi et al. (2009) comparing cephalomedullary nails to independent fixation (IMN + CS) found no significant difference in the rates of AVN or nonunion, suggesting that both methods can achieve acceptable outcomes when performed correctly. The critical factor emphasized is anatomical reduction of the femoral neck.
Reduction of Femoral Neck: Neck First vs. Shaft First
The sequence of reduction is often debated.
*
Neck First:
Many authors recommend reducing and fixing the femoral neck fracture first. This is because the neck fracture is more prone to complications, and anatomical reduction of the neck is paramount. Stabilizing the neck initially with K-wires or cannulated screws provides a stable platform before addressing the shaft. This approach is more amenable to open reduction of the neck if closed methods fail.
*
Shaft First:
Some argue for reducing the shaft first, especially when using a cephalomedullary nail, as the nail itself can help reduce the neck. However, this carries a higher risk of malreduction of the neck, which is often difficult to correct once the nail is seated.
Outcomes and Prognosis
Overall, modern surgical management has significantly improved outcomes. However, the complication rates remain higher than for isolated fractures.
*
AVN of Femoral Head:
Still the most feared complication, with rates varying from 10-25% for displaced neck fractures. Risk factors include displacement severity, delayed diagnosis, and inadequate reduction.
*
Nonunion of Femoral Neck:
Ranges from 5-30%. Factors include poor reduction, inadequate fixation, and compromised vascularity.
*
Nonunion/Malunion of Femoral Shaft:
Rates are comparable to isolated shaft fractures (2-15%) but can be influenced by implant choice and stress risers. Malrotation is a common sequela of shaft fractures.
Long-term follow-up is essential to detect delayed complications. Patient education regarding potential complications and the need for prolonged rehabilitation is vital. The overarching principle for successful management of ipsilateral femoral neck and shaft fractures remains prompt diagnosis, meticulous pre-operative planning, anatomical reduction of the femoral neck, stable internal fixation of both fractures, and appropriate post-operative rehabilitation.
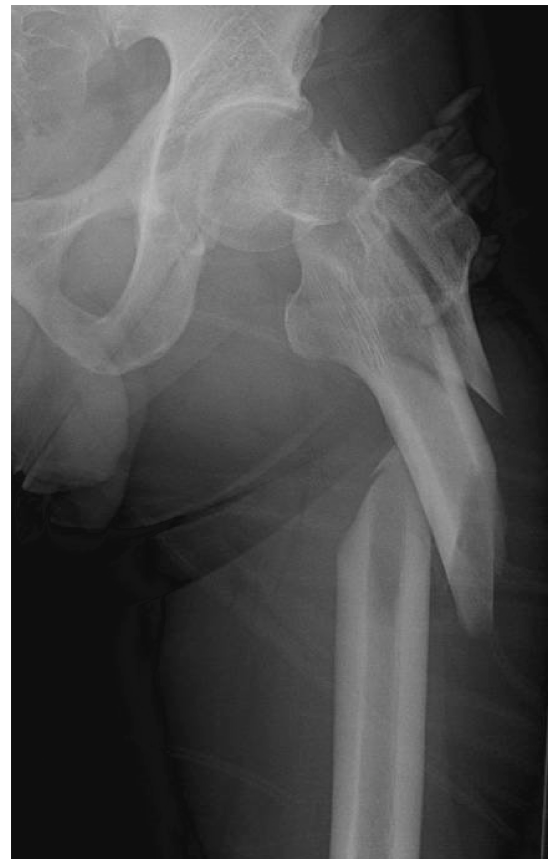
Clinical & Radiographic Imaging

