Femoral Shaft Fractures: Comprehensive Management & Surgical Principles
Key Takeaway
Femoral shaft fractures are high-energy traumatic injuries requiring ATLS assessment. Diagnosis involves X-rays and CT. Surgical stabilization, predominantly with intramedullary (IM) nailing, is the primary treatment, achieving high union rates. Effective management demands understanding epidemiology, surgical anatomy, biomechanics, and deforming muscle forces for optimal patient outcomes.
Treatment of Femoral Shaft Fractures: What You Need to Know
Introduction & Epidemiology
Femoral shaft fractures represent high-energy traumatic injuries to the diaphysis of the femur. Their inherent association with significant force necessitates a thorough assessment for life-threatening concomitant injuries, including but not limited to pulmonary contusions, cerebral trauma, major thoracoabdominal injuries, and ipsilateral femoral neck fractures. Timely and accurate diagnosis, coupled with appropriate management, is paramount for optimizing patient outcomes and minimizing morbidity and mortality.
Initial evaluation in a trauma setting must adhere to Advanced Trauma Life Support (ATLS) protocols, prioritizing airway, breathing, and circulation before addressing orthopedic injuries. Once the patient is hemodynamically stable, attention can be directed to the musculoskeletal system.
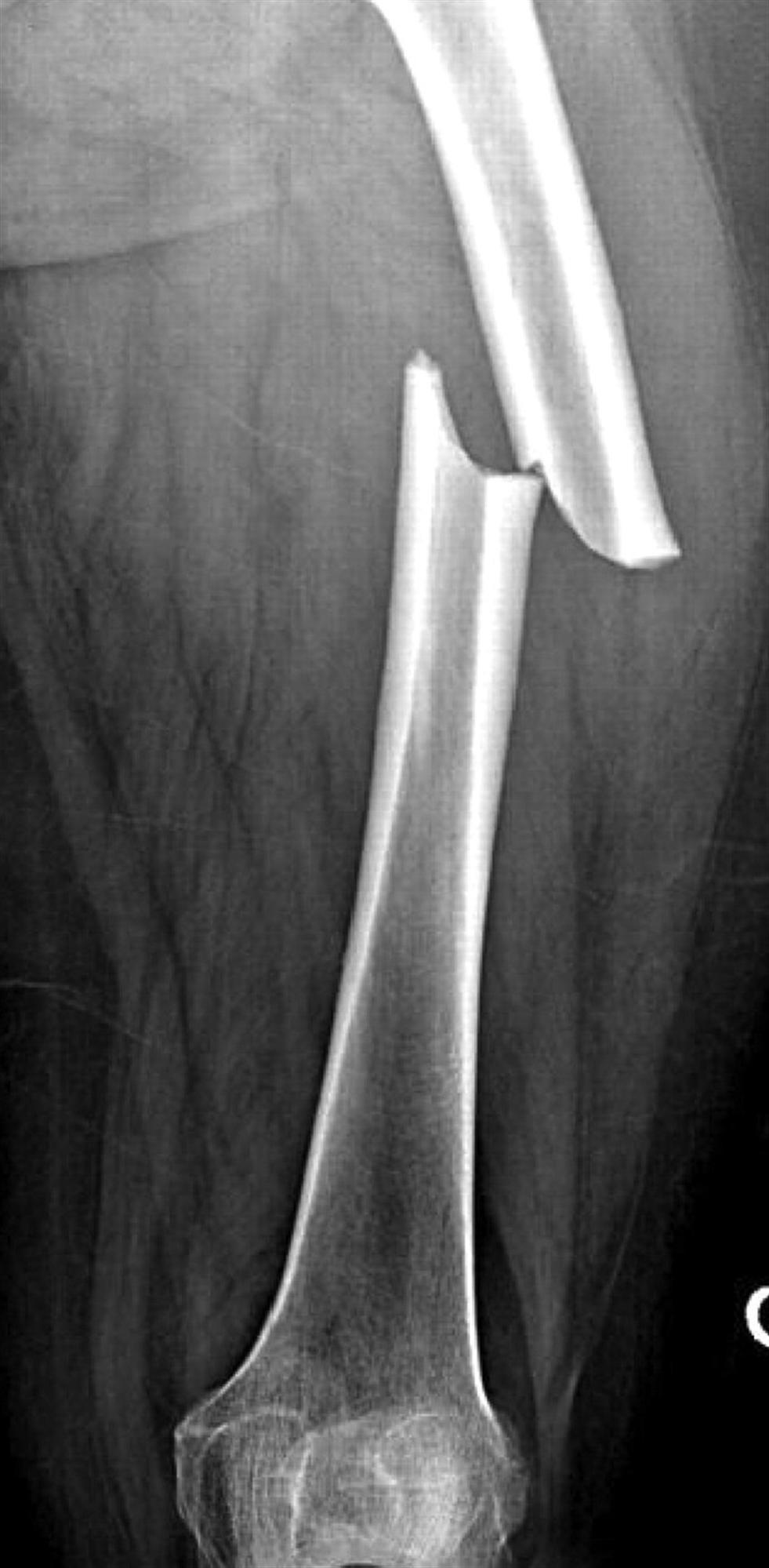
Diagnosis of femoral shaft fractures is primarily achieved through standard orthogonal radiographs (anteroposterior and lateral views) of the entire femur, extending from the hip joint to the knee joint. Crucially, dedicated AP and lateral radiographs of the ipsilateral hip and knee are mandatory to rule out concurrent injuries, particularly femoral neck fractures, which are identified in 5-9% of cases and are easily missed without specific imaging. Computed tomography (CT) scans may be indicated for complex fracture patterns, suspected articular involvement, or in the context of polytrauma for comprehensive assessment. Angiography or duplex ultrasound should be considered if there is suspicion of vascular injury, although this is rare in closed femoral shaft fractures.
The treatment paradigm for most adult femoral shaft fractures involves surgical stabilization, predominantly with intramedullary (IM) nailing, which is associated with union rates exceeding 95%. This approach minimizes complications associated with prolonged immobilization and facilitates early rehabilitation.
Epidemiology:
Femoral shaft fractures are common, exhibiting a reported incidence of approximately 37.1 per 100,000 persons annually. The demographic distribution is bimodal. In younger patients, these fractures are typically the sequelae of high-energy trauma, with high-speed motor vehicle accidents being the most frequent mechanism. This patient population often presents with polytrauma, necessitating a comprehensive, multidisciplinary approach. In contrast, low-energy fractures, often resulting from a simple fall from standing, are more prevalent in the elderly population, frequently associated with underlying osteoporosis. Additional etiologies include gunshot wounds, pathological fractures (secondary to tumors or metabolic bone disease), and periprosthetic fractures.
The comprehensive management of these complex injuries requires a deep understanding of relevant surgical anatomy, biomechanics, appropriate indications, meticulous surgical technique, and diligent post-operative care.
Mohammad Hutaif
(
 ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
Surgical Anatomy & Biomechanics
Surgical Anatomy
The femoral shaft comprises the diaphysis of the femur, extending from the lesser trochanter proximally to the flare of the condyles distally. It is the longest and strongest bone in the body, designed to withstand significant axial, bending, and torsional forces.
- Bone Structure: The femoral shaft is composed of dense cortical bone, particularly thick in the mid-diaphyseal region, which gradually thins towards the metaphyses. The medullary canal, which houses the nutrient artery, runs longitudinally through the diaphysis.
- Vascularity: The primary blood supply to the femoral shaft is derived from the nutrient artery, typically a branch of the profunda femoris artery, which enters the posteromedial cortex in the middle third of the shaft. This vessel provides a rich endosteal blood supply. Additionally, the periosteal circulation, supplied by numerous muscular branches, contributes significantly to healing, particularly after trauma that disrupts the endosteal supply. Preservation of both systems is crucial for fracture union.
-
Muscular Attachments and Deforming Forces:
Numerous powerful muscles attach to the femoral shaft, exerting significant deforming forces on fracture fragments.
- Proximal Fragment: The gluteus medius and minimus, attaching to the greater trochanter, abduct the proximal fragment. The iliopsoas, attaching to the lesser trochanter, flexes and externally rotates it. The adductor magnus can adduct the distal fragment relative to the proximal.
- Mid-Shaft Fragment: The quadriceps femoris (rectus femoris, vastus lateralis, medialis, intermedius) and hamstrings (biceps femoris, semitendinosus, semimembranosus) surround the shaft. Imbalance in these muscle groups can lead to characteristic fragment malalignment, such as apex posterior angulation due to the pull of the gastrocnemius or shortening.
- Nerve and Vascular Structures: The sciatic nerve lies posteriorly and medially in the thigh, deep to the hamstrings, and is at risk during posterior surgical approaches or with severe displacement. The femoral artery and vein, along with their deep branches (profunda femoris artery and vein), are located anteromedially. Awareness of these structures is paramount to avoid iatrogenic injury during dissection and hardware placement.
Biomechanics
The biomechanics of femoral shaft fractures are complex, dictated by the magnitude and direction of the applied forces, as well as the inherent properties of the bone.
- Force Distribution: The femur normally sustains axial compression, bending, and torsional loads during daily activities. High-energy trauma introduces supraphysiologic forces that exceed the bone's elastic limit, leading to fracture.
-
Fracture Patterns:
- Transverse fractures: Typically result from a direct bending force, indicating a high-energy mechanism.
- Spiral fractures: Caused by isolated torsional forces, often seen in lower energy twisting injuries or sport-related trauma.
- Oblique fractures: A combination of axial compression and bending/torsional forces.
- Comminuted/Segmental fractures: Result from very high-energy impacts, where multiple fragments or distinct segments are created. These often involve significant soft tissue injury.
- Impact on fixation: The fracture pattern significantly influences the stability achievable with different fixation methods.
-
 Illustrative depiction of various femoral shaft fracture patterns.
Illustrative depiction of various femoral shaft fracture patterns.
-
Intramedullary Nailing Biomechanics:
- IM nailing is the preferred method for femoral shaft fractures due to its load-sharing capabilities, which allow for controlled micromotion at the fracture site, promoting secondary bone healing (callus formation).
- The nail acts as a central column, resisting bending and axial forces, while interlocking screws prevent rotation and shortening.
- Reamed vs. Unreamed Nailing: Reaming the medullary canal before nail insertion allows for a larger diameter nail, which offers greater mechanical strength and rotational stability. However, reaming disrupts the endosteal blood supply, potentially increasing the risk of fat embolization and transient osteonecrosis. Unreamed nails preserve the endosteal blood supply but provide less absolute stability and require a smaller diameter nail. The choice depends on fracture characteristics, patient physiology, and surgeon preference.
- Entry Point Biomechanics: The entry point for IM nailing impacts potential iatrogenic injury. Piriformis fossa entry, historically common, carries a theoretical risk of osteonecrosis of the femoral head due to disruption of retinacular vessels. Greater trochanteric entry, now widely adopted, may be associated with trochanteric pain but is generally considered safer for the femoral head.
Indications & Contraindications
Indications for Operative Treatment
The vast majority of adult femoral shaft fractures warrant operative stabilization. Non-operative management is rarely indicated due to the significant deforming muscle forces, high rates of malunion and nonunion, and the complications associated with prolonged recumbency and immobilization (e.g., decubitus ulcers, pneumonia, deep vein thrombosis, joint stiffness).
Primary Indications for Intramedullary Nailing:
- Nearly all diaphyseal fractures of the femur in adults: This includes transverse, oblique, spiral, comminuted, and segmental patterns.
- Open Fractures (Gustilo-Anderson Type I, II, IIIa): After thorough debridement and irrigation, early definitive fixation with IM nailing is preferred to facilitate wound care and rehabilitation. For Gustilo-Anderson IIIB and IIIC, external fixation may be used initially as part of damage control orthopedics, followed by delayed IM nailing once soft tissues improve.
- Polytrauma Patients: Early stabilization of femoral shaft fractures (within 24 hours, often within 6-12 hours) in hemodynamically stable polytrauma patients (Early Total Care - ETC) is associated with reduced pulmonary complications and improved outcomes. In patients with severe physiological derangement (e.g., acute respiratory distress syndrome, severe head injury, hemodynamic instability), a damage control orthopedics (DCO) approach using temporary external fixation is preferred, with definitive IM nailing performed once the patient's condition stabilizes.
- Pathological Fractures: Due to underlying bone weakness, IM nailing provides immediate stability, pain relief, and facilitates adjuvant treatments such as radiotherapy.
- Impending Pathological Fractures: Prophylactic nailing may be considered for large lytic lesions (>2.5 cm or >50% cortical involvement) in the femur to prevent fracture.
- Periprosthetic Femur Fractures: IM nailing can be used, often with specialized nails or techniques, depending on the location relative to existing implants.
Contraindications for Operative Treatment (Relative or Temporary)
Absolute contraindications for IM nailing are rare. Most are relative or temporary, necessitating a modified approach or a staged procedure.
- Active Infection at the Proposed Entry Site or in the Canal: Relative contraindication. Requires initial debridement and antibiotics. External fixation may be used as a temporary measure.
- Severe Comminution or Bone Loss: If there is insufficient bone for stable interlocking, external fixation or plating may be considered. However, advanced nailing techniques often address this.
- Medically Unstable Patient: In the context of polytrauma, severe physiological derangement mandates a DCO approach (external fixation) until the patient is stable enough for definitive IM nailing.
- Extremely Wide Medullary Canal: Can make stable IM nailing challenging. May require larger diameter nails or adjunctive techniques (e.g., blocking screws).
- Pre-existing Hardware in the Medullary Canal: Requires removal of existing hardware or a different fixation strategy (e.g., plate osteosynthesis).
- Non-Ambulatory Status/Limited Life Expectancy: Consideration for less invasive or palliative measures may be made in select cases.
- Skeletally Immature Patients: IM nailing is generally avoided in patients with open physes to prevent growth disturbance. Flexible IM nails or external fixation are often used in younger pediatric patients.
Summary Table: Operative vs. Non-Operative Indications
| Feature | Operative Treatment (IM Nailing) | Non-Operative Treatment (Rare/Specific) |
|---|---|---|
| Adult Femoral Shaft Fx | Primary Indication for nearly all patterns | Extremely rare; generally contraindicated |
| Polytrauma Patient | Preferred in hemodynamically stable patients (ETC) | Temporary external fixation in unstable patients (DCO) |
| Open Fractures | After debridement (Type I, II, IIIa) | Initial external fixation for Type IIIB/IIIC until soft tissue permits |
| Pathological Fx / Impending Fx | Primary method for stability and pain relief | Seldom indicated; typically requires surgical stabilization |
| Skeletally Immature | Generally avoided due to physeal injury risk | Preferred in younger pediatric patients (spica cast, flexible nails) |
| Specific Contraindications for IMN | N/A | Active infection, severe instability for IMN, prohibitive medical status |
| Expected Outcome | High union rates, early mobilization, reduced complications | High risk of nonunion, malunion, prolonged immobilization complications |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is crucial for successful outcomes and minimizing complications in femoral shaft fracture fixation.
Pre-Operative Planning
-
Patient Resuscitation and Assessment:
- Adherence to ATLS protocols for polytrauma patients.
- Stabilization of hemodynamic status, management of associated life-threatening injuries.
- Thorough clinical examination for associated neurovascular compromise, compartment syndrome, and open wounds.
-
Radiographic Evaluation:
- High-quality AP and lateral radiographs of the entire femur, including the hip and knee joints.
- AP pelvis radiograph to rule out associated pelvic or acetabular fractures.
- Specific AP and lateral views of the ipsilateral hip and knee to identify ipsilateral femoral neck or patellar fractures.
- CT scans are often employed for complex intra-articular extension, highly comminuted patterns, or in polytrauma settings.
-
Fracture Classification:
- AO/OTA Classification: Standardized system for describing fracture location (diaphyseal), morphology (simple, wedge, complex), and severity.
- Gustilo-Anderson Classification: For open fractures, guides debridement and antibiotic management.
-
Implant Selection and Templating:
- Nail Type: Reamed vs. unreamed, antegrade vs. retrograde, specific nail designs (e.g., supracondylar for distal fractures).
- Nail Length: Measured on the contralateral uninjured femur or estimated from the anterior superior iliac spine (ASIS) to the knee joint line. Critical for appropriate fixation.
- Nail Diameter: Templating from true-size radiographs of the intact contralateral femur, or utilizing intraoperative measurement. The goal is to select the largest possible nail that can be inserted without excessive reaming, ideally filling 80-90% of the medullary canal for optimal stability.
- Entry Point Strategy: Predetermine piriformis versus greater trochanteric entry based on fracture pattern (e.g., proximal fractures may benefit from a trochanteric entry), patient anatomy, and surgeon preference.
-
Timing of Surgery:
- Early Total Care (ETC): In isolated femoral shaft fractures or hemodynamically stable polytrauma patients, definitive fixation within 6-24 hours is optimal to minimize systemic complications.
- Damage Control Orthopedics (DCO): In severely injured polytrauma patients with significant physiological derangement (e.g., severe chest injury, head injury, hemorrhagic shock), temporary external fixation is applied, followed by definitive IM nailing once the patient's condition stabilizes (usually 5-10 days later).
- Antibiotic Prophylaxis: Administered pre-operatively, especially for open fractures or for any surgical intervention.
Patient Positioning
The most common and preferred position for antegrade femoral nailing is supine on a fracture table.
-
Fracture Table Setup:
- The patient is positioned supine on a radiolucent fracture table.
- The injured leg is placed in traction, typically through a boot or ankle hitch, allowing for controlled reduction and maintenance of length and rotation.
- The uninjured leg is abducted and flexed at the hip and knee, resting in a well-padded stirrup or support, to provide adequate space for C-arm access from both AP and lateral directions.
- Reduction: Before definitive draping, closed reduction of the fracture should be attempted and confirmed with C-arm imaging. Correct length, alignment, and rotation are crucial at this stage. Excessive traction can lead to distraction at the fracture site, impeding healing.
-
C-arm Access:
- The C-arm must have unrestricted access to the entire femur, from the femoral head to the knee joint, for both AP and lateral views. This often requires positioning the C-arm obliquely for the proximal femur and perpendicular for the distal femur.
-
Alternative Positioning:
- Lateral Decubitus: Occasionally used, particularly for retrograde nailing or in specific complex cases. Requires meticulous padding and support.
- Supine on a Regular Table: Can be used with careful patient draping to allow for manipulation of the injured leg and C-arm access. However, maintaining reduction can be more challenging without traction.
-
Sterile Preparation and Draping:
- The entire ipsilateral lower extremity, from the iliac crest to the foot, is prepped and draped in a sterile fashion. The perineum should also be prepped if a piriformis entry point is anticipated, as this area is notoriously difficult to maintain sterile.
Detailed Surgical Approach / Technique
Intramedullary nailing is the gold standard for most femoral shaft fractures. The technique relies on achieving stable fixation by inserting a nail into the medullary canal, providing relative stability that promotes callus formation and secondary bone healing.
General Principles
- Closed Reduction: Whenever possible, closed reduction techniques are preferred to minimize additional soft tissue stripping and preserve the fracture hematoma, which is biologically active.
- Reaming: Reamed nailing generally offers greater stability due to a larger diameter nail and provides biologic stimulation through reaming debris. However, it carries risks of fat embolism and endosteal heat necrosis. Unreamed nailing preserves endosteal blood supply but offers less mechanical strength. The choice depends on fracture characteristics and patient factors.
- Entry Point: The choice between piriformis fossa and greater trochanteric entry is critical and depends on fracture location, patient anatomy, and surgeon preference.
- Interlocking: Proximal and distal interlocking screws are essential for rotational stability and preventing shortening or distraction.
Antegrade Intramedullary Nailing (Standard Technique)
-
Incision and Entry Point Preparation:
- Piriformis Fossa Entry: Traditionally a longitudinal incision, approximately 5-8 cm long, centered over the greater trochanter and extending proximally. The gluteus medius is split bluntly or incised in line with its fibers to expose the piriformis fossa, which lies at the junction of the superior aspect of the femoral neck and the greater trochanter. This entry point is directly in line with the femoral canal.
- Greater Trochanteric Entry: A longitudinal or oblique skin incision, 3-5 cm long, is made just anterior or posterior to the tip of the greater trochanter. The vastus lateralis is split or incised to expose the tip of the trochanter. A trochanteric entry portal is created slightly medial and anterior to the tip of the greater trochanter, ensuring it is within the confines of the trochanter and aligned with the central axis of the femoral canal. This approach is increasingly popular, especially for proximal shaft fractures, to minimize the risk of femoral head avascular necrosis (AVN) associated with piriformis entry.
- Initial Entry: A sharp awl or guide pin is used to create the cortical opening. Confirm correct entry point and trajectory with fluoroscopy (AP and lateral views). The guidewire should be positioned centrally in both planes down the femoral canal.
-
Guidewire Insertion:
- A flexible guidewire with an olive tip is advanced across the fracture site and down the distal fragment into the epiphysis.
- Reduction Aids: For difficult reductions, manual manipulation, external clamps (e.g., Verbrugge, pointed reduction clamps), joysticks (K-wires), or temporary cerclage wires (used cautiously to preserve vascularity) may be employed to align fragments. "Blocking screws" (Poller screws) can be invaluable for correcting malalignment in wide canals or metaphyseal fractures by strategically placed K-wires or small screws to guide the nail centrally.
- Fluoroscopic confirmation of reduction and guidewire position is essential.
-
Reaming (if applicable):
- If using a reamed technique, sequential flexible reamers are advanced over the guidewire. Start with a small diameter and gradually increase in 0.5 mm increments until cortical chatter is felt. Ream to 1.0-1.5 mm larger than the chosen nail diameter.
- Ensure constant irrigation to dissipate heat and minimize thermal necrosis. Monitor for fat embolization syndrome, particularly in polytrauma patients.
-
Nail Insertion:
- Select the appropriate nail length and diameter based on templating.
- The nail is attached to the insertion handle and carefully advanced over the guidewire. Gentle, controlled force with rotation is applied. Avoid aggressive impaction to prevent iatrogenic fracture or distraction.
- Verify nail depth and position with fluoroscopy. The proximal end of the nail should be flush with or slightly proud of the cortex at the entry point to prevent impingement.
- Achieve anatomic length and rotation before locking. Rotational alignment is critical; compare with the contralateral side or use the cortical step sign (medial and lateral cortices should match proximally and distally).
-
Distal Locking:
- This is typically the first set of locking screws inserted.
- Using a distal targeting guide or freehand technique with fluoroscopy, drill holes for the distal interlocking screws. Aim for at least two screws for rotational stability.
- Measure screw lengths and insert appropriate screws. Confirm position with fluoroscopy.
-
Fracture Compression (Optional):
- If a static nail is chosen, compression can be applied at the fracture site by seating the nail further into the bone or using a compression device through the nail. This is generally performed before proximal locking.
-
Proximal Locking:
- Attach the proximal targeting jig to the nail insertion handle.
- Drill holes for the proximal interlocking screws through the jig. Typically two screws are inserted for rotational and bending stability.
- Measure screw lengths and insert appropriate screws. Verify screw placement with fluoroscopy.
- In cases of subtrochanteric or very proximal shaft fractures, the nail and proximal locking must effectively stabilize the greater and lesser trochanteric fragments.
-
Final Checks:
- Confirm adequate length, alignment, and rotation with AP and lateral fluoroscopic views of the entire femur, hip, and knee.
- Check for stability.
-
Closure:
- Irrigate the wound thoroughly.
- Layered closure of the soft tissues and skin.
Retrograde Intramedullary Nailing
- Indications: Often preferred for distal femoral shaft fractures (up to 5 cm from the knee joint), ipsilateral tibia and femur fractures ("floating knee"), proximal ipsilateral tibia fractures, or in patients with associated hip pathology.
- Technique: A small incision is made just proximal to the patella, usually through a medial or lateral parapatellar approach. An entry portal is created in the intercondylar notch, aiming for the central axis of the femoral canal. The nail is then inserted proximally. Distal and proximal locking are performed similarly to antegrade nailing.
- Advantages: Less hip pain, easier for simultaneous knee and distal femur fractures.
- Disadvantages: Risk of knee pain, limited to certain fracture types, potential for intra-articular damage during entry.
Complications & Management
Despite high success rates, femoral shaft fracture management can be associated with significant complications. Proactive recognition and appropriate management are crucial.
Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (%) | Pathophysiology / Risk Factors | Management Strategy |
|---|---|---|---|
| Nonunion | 1-5% | Inadequate reduction/fixation, poor biology, infection, distraction | Exchange nailing (reamed), bone grafting, plate fixation, re-revision IMN |
| Malunion | 5-15% (rotational) | Inadequate reduction, fixation instability, technical error | Revision osteotomy with IMN or plating, often for rotational (>15-20°) or angular (>10°) malunion |
| Infection | 1-3% (closed) | Open fracture, surgical technique, host factors | Debridement, antibiotics, implant retention/removal, external fixation, muscle flap, bone reconstruction |
| Fat Embolism Syndrome (FES) | 1-2% (clinical) | Reaming, multiple fractures, hypovolemic shock | Supportive care (respiratory support), prevention (careful reaming, fluid management) |
| Vascular Injury | <1% | High-energy trauma, severe displacement, iatrogenic during surgery | Urgent vascular repair, fasciotomy if indicated |
| Nerve Injury | <1% | High-energy trauma, severe displacement, iatrogenic during surgery | Observation, neurolysis, nerve repair, or grafting |
| Iatrogenic Fracture | <1% | During reaming/nail insertion, stress riser from entry point | Extended fixation, revision nailing, plating |
| Hardware Failure | 2-5% | Nonunion, inadequate fixation, early weight-bearing | Revision surgery, plate osteosynthesis, or exchange nailing |
| Pain at Entry Site (GT Bursitis) | 10-20% | Prominent nail, soft tissue irritation | NSAIDs, steroid injection, hardware removal (after union), surgical bursectomy |
| Limb Length Discrepancy (LLD) | 5-10% | Shortening (inadequate reduction/compression) or distraction | Shoe lifts, epiphysiodesis (pediatric), limb lengthening (rarely for femur fractures) |
| Rotational Malalignment | 10-30% | Inadequate intraoperative assessment of rotation | Revision osteotomy (if symptomatic and >15-20° discrepancy) |
| Avascular Necrosis (AVN) of Femoral Head | <1% | Piriformis entry (iatrogenic vascular compromise) | Observation, joint preservation procedures (core decompression), total hip arthroplasty |
| Heterotopic Ossification (HO) | 10-20% (minor) | High-energy trauma, head injury, prolonged ventilation | NSAIDs/radiation prophylaxis, surgical excision (after maturation) |
Detailed Management Considerations
-
Nonunion:
Defined as failure of fracture healing after 6-9 months without progressive radiographic signs of healing.
- Management: Exchange nailing (removing the existing nail and inserting a larger, reamed nail) is often the first line. Bone grafting (autograft or allograft) can be used for atrophic nonunions or significant bone loss. Plate fixation may be considered for hypertrophic nonunions with significant malunion or failed IMN.
-
Malunion:
Occurs when the fracture heals in an unacceptable position (e.g., angular deformity, significant shortening, rotational malalignment). Rotational malalignment is particularly insidious and difficult to assess clinically.
- Management: Corrective osteotomy and refixation (often with IMN or plate) are indicated for symptomatic malunions (e.g., gait disturbance, hip/knee pain, functional limitation), typically for >15-20° rotational or >10° angular deformities.
- Infection: Superficial infections can be managed with oral antibiotics. Deep infections require aggressive surgical debridement, intravenous antibiotics, and potentially implant retention if the fracture is stable and healing, or implant removal with external fixation and subsequent reconstruction if necessary. Biofilm formation on implants necessitates removal.
-
Hardware-Related Pain:
Pain at the greater trochanteric entry site is common and often related to prominent hardware or trochanteric bursitis.
- Management: NSAIDs, corticosteroid injections, or hardware removal (after fracture union) are common strategies.
- Vascular/Nerve Injury: Immediate surgical exploration and repair are required for significant vascular injuries. Nerve injuries are initially observed; exploration is indicated for progressive deficits or no recovery.
- Rotational Malalignment: Prevention is key, using intraoperative cues like cortical step signs, comparison with the contralateral extremity, and careful positioning. Once established, symptomatic rotational malalignment may require a corrective osteotomy. Clinical thresholds for revision vary, often >15-20° difference from the contralateral limb.
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is essential to optimize functional recovery, restore strength, and facilitate return to pre-injury activity levels. The protocol must be individualized based on fracture stability, fixation achieved, associated injuries, patient comorbidities, and compliance.
Immediate Post-Operative Phase (Days 0-7)
- Pain Management: Multimodal analgesia is critical to facilitate early mobilization.
-
Weight-Bearing (WB) Status:
- Stable Fixation: Partial weight-bearing (PWB) with crutches or a walker is often initiated immediately or within a few days, typically 25-50% body weight.
- Unstable Fixation (e.g., highly comminuted, poor bone quality): Touch-down weight-bearing (TDWB) or non-weight-bearing (NWB) may be prescribed initially, with gradual progression based on radiographic union and pain.
- Retrograde Nailing: Often allows earlier weight-bearing on the foot than antegrade due to load transfer.
-
Range of Motion (ROM):
- Ankle and Foot: Active ROM exercises for ankle dorsiflexion/plantarflexion to prevent stiffness and deep vein thrombosis (DVT).
- Knee: Gentle active and passive knee flexion/extension exercises, aiming for 0-90 degrees flexion by 1 week post-op.
- Hip: Gentle active and passive hip flexion/extension/abduction/adduction within comfortable limits, avoiding extreme ranges initially.
-
Isometric Strengthening:
- Quadriceps sets, gluteal sets, and ankle pumps to maintain muscle tone and promote circulation.
-
Transfers and Mobility:
- Instruction in safe bed mobility, transfers (bed to chair), and assistive device use (walker/crutches).
Early Rehabilitation Phase (Weeks 1-6)
- Weight-Bearing Progression: Gradual progression from PWB to weight-bearing as tolerated (WBAT) as pain decreases and radiographic signs of early callus formation emerge. Typically, full weight-bearing (FWB) can commence when there is evidence of bridging callus on at least two cortices.
-
ROM Progression:
- Continue to increase knee flexion, aiming for >110-120 degrees.
- Progress hip ROM, focusing on restoring functional ranges.
-
Strengthening:
- Initiate gentle isotonic exercises for hip and knee musculature (e.g., straight leg raises, hip abduction/adduction in supine, short arc quads).
- Resistance bands can be introduced for progressive strengthening.
-
Gait Training:
- Focus on normalizing gait pattern with assistive devices, progressing to single crutch/cane and eventually independent ambulation.
- Scar Management: Gentle massage and stretching to prevent adhesions.
Intermediate Rehabilitation Phase (Weeks 6-12)
- Weight-Bearing: Full weight-bearing as tolerated.
-
Strengthening:
- Progressive resistance exercises for the entire lower extremity, including squats, lunges, leg press, hamstring curls, and calf raises.
- Core strengthening exercises.
- Initiate proprioceptive and balance training (e.g., single-leg stance, wobble board).
-
Functional Activities:
- Stair climbing, inclined walking.
- Stationary cycling or swimming for cardiovascular fitness.
- Radiographic Assessment: Regular radiographs to monitor fracture union. FWB is often permitted once three cortices demonstrate bridging callus.
Advanced Rehabilitation Phase (Weeks 12+)
-
Strengthening and Conditioning:
- Advanced strengthening exercises, plyometrics (if appropriate), and sport-specific drills.
- Focus on power, agility, and endurance.
-
Return to Activity/Sport:
- Gradual return to recreational or competitive sports, typically 6-12 months post-surgery, provided there is complete radiographic union, full ROM, symmetric strength, and no pain.
- A functional assessment or return-to-sport testing may be performed.
- Patients should be educated on the risk of refracture if hardware is removed prematurely or if return to high-impact activities occurs before full bone remodeling.
-
Hardware Removal:
- Considered after complete radiographic union, typically 12-24 months post-op, especially for symptomatic hardware (e.g., prominent nail, trochanteric pain).
- Hardware removal is not universally required for asymptomatic patients.
Summary of Key Literature / Guidelines
The management of femoral shaft fractures has evolved significantly, with intramedullary nailing firmly established as the gold standard. A robust body of literature and consensus guidelines underpins current practice.
- AO Foundation Principles: The Arbeitsgemeinschaft für Osteosynthesefragen (AO) has been instrumental in defining principles of stable internal fixation. For diaphyseal fractures, the concept of "biological fixation" with relative stability, achieved through IM nailing, is favored to promote secondary bone healing and callus formation.
- IM Nailing as Gold Standard: Numerous meta-analyses and systematic reviews consistently demonstrate that intramedullary nailing provides superior outcomes compared to plate osteosynthesis or external fixation for adult femoral shaft fractures in terms of union rates, time to weight-bearing, and functional results. Union rates greater than 95% are routinely reported with IM nailing.
- Timing of Fixation in Polytrauma: The debate between Early Total Care (ETC) and Damage Control Orthopedics (DCO) continues, but the prevailing evidence suggests that early definitive fixation (within 24 hours) for hemodynamically stable polytrauma patients is associated with a reduced incidence of pulmonary complications, particularly Acute Respiratory Distress Syndrome (ARDS), and improved patient survival. However, in unstable patients (e.g., severe head injury, chest injury, hemorrhagic shock), DCO with temporary external fixation followed by delayed definitive nailing is crucial to avoid "second hit" injury.
- Reamed vs. Unreamed Nailing: While unreamed nailing was initially popularized to preserve endosteal blood supply and potentially reduce fat embolism risk, subsequent studies have shown reamed nailing to provide superior mechanical stability, higher union rates, and potentially faster healing, especially in comminuted fractures. The risks of FES with reaming are manageable with careful technique and patient selection. The choice often depends on fracture type and patient physiology.
- Entry Point Controversy (Piriformis vs. Greater Trochanter): Historical piriformis entry has been linked to a theoretical risk of femoral head AVN, although clinically significant rates are low. Greater trochanteric entry has become increasingly popular, particularly with specialized nails, as it avoids the piriformis fossa. While trochanteric entry may be associated with a higher incidence of trochanteric pain/bursitis, it is generally considered a safe and effective approach, especially for fractures with proximal extension.
- Ipsilateral Femoral Neck Fractures: The diagnosis of concurrent ipsilateral femoral neck and shaft fractures (floating hip injury) requires a high index of suspicion and meticulous imaging. Management often involves fixation of the femoral neck fracture first, followed by IM nailing of the shaft, to ensure anatomical reduction and stable fixation of both components.
- Rotational Malalignment: A significant concern following IM nailing, with reported incidences up to 30%. It is often poorly tolerated if significant (>15-20° difference from the contralateral side) and can lead to functional impairment. Intraoperative assessment of rotation is critical, often relying on the cortical step sign, C-arm imaging of the lesser trochanter, or comparison with the contralateral extremity.
In conclusion, the treatment of femoral shaft fractures has been refined over decades. Intramedullary nailing remains the cornerstone, offering high union rates and allowing early mobilization. Mastery of surgical technique, comprehensive pre-operative planning, diligent attention to potential complications, and structured post-operative rehabilitation are all fundamental to achieving optimal outcomes for our patients.
