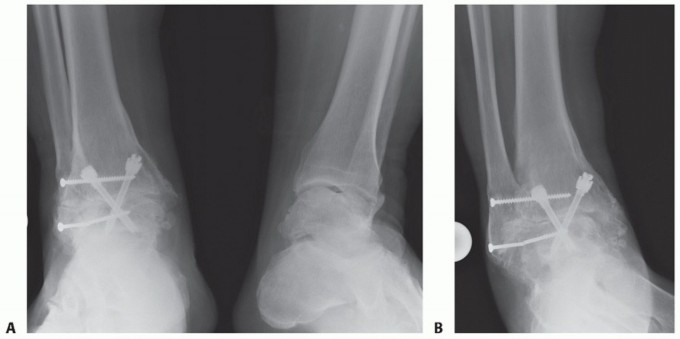
Ankle Arthroscopy & Microfracture for Osteochondral Lesions of the Talus: A Masterclass
Key Takeaway
Welcome to the OR for an immersive masterclass on microfracture for osteochondral lesions of the talus (OLT). We'll cover comprehensive surgical anatomy, meticulous preoperative planning, and a granular, step-by-step intraoperative execution from the surgeon's viewpoint. Understand critical pearls, potential pitfalls, and detailed postoperative management protocols to optimize patient outcomes. This session provides an exhaustive guide for fellows.
Introduction to Osteochondral Lesions of the Talus (OLT)
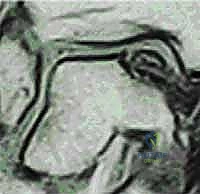
Alright, fellows, welcome to the operating theater. Today, we’re addressing a common yet often challenging pathology: an osteochondral lesion of the talus, or OLT. This patient presents with persistent ankle pain and swelling, and our MRI confirms an identifiable bone bruise and cartilage defect on the medial talar dome. The terminology surrounding these lesions can be quite varied—transchondral fractures, osteochondral fractures, flake fractures, or osteochondritis dissecans (OCD)—but "osteochondral lesion of the talus" has become the most widely accepted and accurate description.
The long-term impact of subchondral effusion, perhaps hemorrhage, on the cartilage layers is a critical question. Is it minor trauma to the tide zone leading to prolonged separation, or something more insidious? In our experience, chronic ankle instability often leads to medial talar dome lesions with an abrasive character, suggesting repetitive microtrauma rather than a classic OCD’s subchondral origin. These are full-thickness cartilage lesions, often associated with varus hindfoot alignment, and can even be bilateral in cases of recurrent ankle sprains. Essentially, OLTs are characterized by the aseptic separation of an articular cartilage fragment, which may or may not include subchondral bone. The crucial distinction to make, both preoperatively and intraoperatively, is whether the lesion is acute or chronic. Acute injuries involve a fresh separation, while chronic lesions often result from repetitive trauma.
Etiology and Pathogenesis
The precise causes of OLTs remain a subject of debate. Lateral lesions, for instance, are most frequently linked to acute trauma, typically a dorsiflexed ankle forced into inversion, causing impaction of the talus against the fibula. These tend to be shallower and located more anteriorly on the talar dome. Medial lesions, conversely, are predominantly associated with single or repetitive supination trauma—microtrauma—and are often deeper and cup-shaped, located in the middle or posterior third of the talus. The mechanism here is usually impaction of the medial talus on the tibia with a plantarflexed ankle forced into hindfoot inversion combined with external rotation. While genetic predisposition and endogenous factors have been theorized, they lack significant evidence-based support.
It's vital to recognize that our primary objective in managing symptomatic OLTs is pain relief, not necessarily preventing osteoarthritis. Over two decades of experience have shown us that untreated OLTs do not reliably progress to widespread ankle osteoarthritis. Many asymptomatic OLTs, incidentally discovered on imaging, never cause problems and should not be treated surgically. Pain, not imaging findings, is our benchmark for intervention.
Comprehensive Surgical Anatomy
Before we make any incisions, let’s meticulously review the relevant anatomy. The talus is a unique bone, approximately 60% covered by articular cartilage, and its blood supply is notoriously precarious.
Osteology and Articular Surfaces
The talar body is trapezoidal, wider anteriorly (about 2.5 mm) than posteriorly. Its superior dome articulates with the tibial plafond, while the medial and lateral facets articulate with the respective malleoli. Understanding this trapezoidal shape is crucial for appreciating ankle kinematics and for identifying the precise location of the lesion. The tibia and fibula form the ankle mortise, providing stability, and any impingement or instability here can contribute to OLT pathology.
Neurovascular Structures
We must be acutely aware of the neurovascular structures surrounding the ankle, especially during portal placement for arthroscopy.
- Anteromedial Portal: Located just medial to the tibialis anterior tendon. Be wary of the saphenous nerve and great saphenous vein which lie subcutaneously.
- Anterolateral Portal: Positioned lateral to the extensor digitorum longus tendons, often between the peroneus tertius and the lateral malleolus. The superficial peroneal nerve is the primary structure at risk here, particularly its intermediate dorsal cutaneous branch. Blunt dissection is paramount.
- Posteromedial Portal: Medial to the Achilles tendon, just superior to the flexor hallucis longus (FHL) tendon. The tibial nerve and posterior tibial artery are critical structures here, running just anterior to the FHL tendon. A safe zone exists, but careful palpation and visualization are required.
- Posterolateral Portal: Lateral to the Achilles tendon. The sural nerve runs superficially in this region.
- Deep Peroneal Nerve: While less directly at risk with standard ankle arthroscopy portals compared to more anterior approaches, its branches supply sensation to the first web space and motor function to the extensors.
Blood Supply of the Talus
The talus receives its blood supply from multiple sources, predominantly through the neck via the sinus tarsi (branches from the dorsalis pedis and peroneal arteries). Other contributions come from the artery of the tarsal canal (from the posterior tibial artery), the deltoid branch (from the posterior tibial artery, supplying the medial talus), and branches from the lateral tarsal artery. This intricate and somewhat tenuous vascularity, especially to the dome, explains the challenges in OLT healing and the rationale behind marrow stimulation techniques like microfracture.
Muscular Intervals
While less critical for direct microfracture, understanding muscular intervals helps in safe portal placement. For instance, the anteromedial portal is typically placed medial to the tibialis anterior tendon, while the anterolateral portal navigates between the extensor digitorum longus and peroneus tertius. The key is always blunt dissection through the subcutaneous tissues and capsule to protect nerves and vessels.
Preoperative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of a successful outcome. We leave nothing to chance.
Imaging Review and Templating
Our review of all imaging studies, especially MRIs and limited CT scans, is the most crucial step. We use these to precisely identify the OLT's size, location, topical geography (medial vs. lateral, anterior vs. posterior), and depth. This detailed understanding dictates our approach—which portals we’ll use, and whether we anticipate any challenges in accessing the lesion. A CT scan, even a limited one, offers superior characterization of the osseous portion and exact dimensions, which is invaluable for staging. MRI, as you know, is the method of choice for suspected OLTs, defining occult subchondral bone and cartilage injuries, and identifying associated edema or stress fractures.
We use the Dipaola et al. MRI classification, based on Berndt and Harty's original radiographic system, to stage the lesion:
* Stage I: Thickening of articular cartilage and low signal changes.
* Stage II: Articular cartilage breached, low-signal rim behind the fragment indicating fibrous attachment.
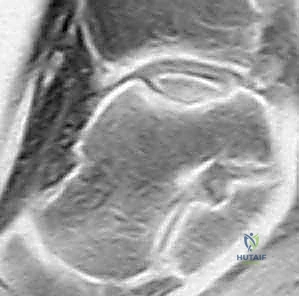
* Stage III: Articular cartilage breached, high-signal changes behind the fragment indicating synovial fluid between the fragment and underlying subchondral bone. (This is what we see in our current case.)
*
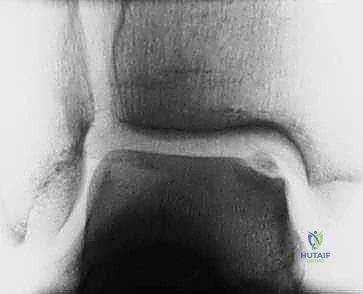
* FIG 3 • Sagittal MRI (T2-SE-2000/90) showing an osteochondral lesion stage III.
* Stage IV: Loose body.
Patient Positioning and OR Setup
Our patient is positioned supine on the operating table.
- Anesthesia: General anesthesia is administered.
- Tourniquet: A pneumatic tourniquet is placed high on the ipsilateral thigh. We will inflate this to 250-300 mmHg after exsanguination to create a bloodless field, typically for no more than 90-120 minutes.
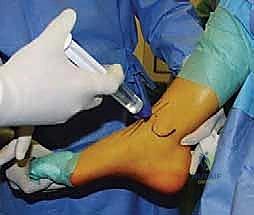
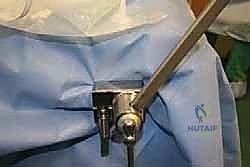
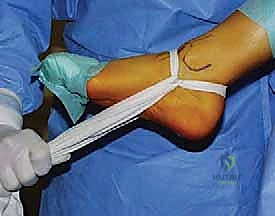
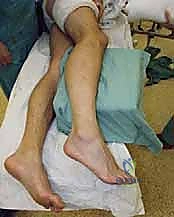
- Leg Holder: Crucially, we utilize a leg holder that allows the gastrocnemius-soleus complex to be fully relaxed. This permits maximum plantarflexion and dorsiflexion, which is essential for visualizing and accessing the talar dome.
* FIG 4 • Patient positioned with a leg holder to relax the gastrocnemius–soleus complex.
4. Fluoroscopy: The C-arm is brought in and positioned to allow for quick and easy AP, lateral, and mortise views of the ankle. We’ll use this sparingly, primarily for confirmation of lesion location or guide certain instruments if needed, though microfracture itself is typically performed under direct arthroscopic visualization.
5. Draping: The limb is prepped and draped in a sterile fashion, allowing full range of motion of the ankle joint.
Examination Under Anesthesia (EUA)
Before incision, a thorough examination under anesthesia is performed. This is critical for assessing coexisting ankle instability, which may not be apparent in a conscious patient due to guarding. We perform:
* Anterior Drawer Test: To assess anterior talofibular ligament (ATFL) integrity.
* Varus Stress Test: To evaluate calcaneofibular ligament (CFL) and ATFL laxity.
* Valgus Stress Test: To check deltoid ligament integrity.
* Range of Motion: We assess active and passive dorsiflexion and plantarflexion, with the knee flexed to eliminate gastrocnemius restriction. Any limitations due to synovitis or effusion will be noted.
Step-by-Step Intraoperative Execution: Ankle Arthroscopy and Microfracture
Alright, fellows, scalpel please. Let's begin.
1. Portal Placement and Joint Access
We’ll start with our standard portals. Remember, precise placement and careful soft tissue dissection are key to avoiding neurovascular injury.
- Anteromedial Portal:
- Identify the tibialis anterior tendon and the medial malleolus.
- Make a small skin incision, approximately 1 cm, just medial to the tibialis anterior tendon at the level of the ankle joint line.
- Use a mosquito clamp to bluntly dissect down to the joint capsule. Feel for the capsule.
- Insert the blunt trocar and cannula into the joint. You should feel a distinct pop as you penetrate the capsule.
- Confirm intra-articular placement with saline inflow.
- Surgical Warning:
> Surgical Warning: Always be mindful of the great saphenous vein and saphenous nerve, which lie subcutaneously in this region. Blunt dissection minimizes risk.
- Anterolateral Portal (Working Portal):
- With the arthroscope in the anteromedial portal, identify the lateral gutter and the extensor digitorum longus tendons.
- Transilluminate from the anteromedial portal to guide your placement.
- Make a 1 cm skin incision just lateral to the peroneus tertius tendon, again at the joint line.
- Bluntly dissect with a mosquito clamp. This is where the superficial peroneal nerve is most vulnerable.
- Insert the blunt trocar and cannula.
- Surgical Warning:
> Surgical Warning: The superficial peroneal nerve is extremely vulnerable here. Always use blunt dissection, and if necessary, palpate its course or perform a small incision to visually identify it before proceeding. - We can also consider a third, more lateral portal if needed for better access to lateral lesions, often termed the anterocentral portal or third portal.
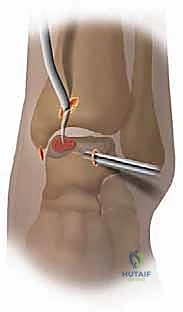
* FIG 5 • Standard anteromedial and anterolateral portals for ankle arthroscopy.
*
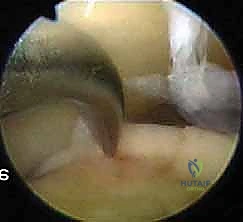
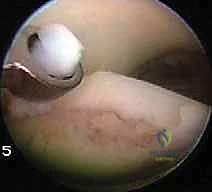
* FIG 6 • Arthroscopic view of the ankle joint.
2. Diagnostic Arthroscopy and Lesion Characterization
Now that we're in, let's perform a systematic diagnostic arthroscopy.
* Initial Survey: Systematically visualize the entire joint: the tibial plafond, medial and lateral gutters, talar dome, and the anterior and posterior aspects of the joint. Look for synovitis, loose bodies, impingement lesions (soft tissue or bony), and any associated pathology.
* Locating the OLT: Our preoperative MRI indicated a medial talar dome lesion. We'll use a probing hook to precisely locate and characterize it.
* Assess the size (length and width).
* Evaluate the depth of the cartilage defect.
* Determine the stability of the surrounding cartilage and the lesion itself. Use the probe to gently push on the lesion. Is it soft? Is it delaminated? Is there an intact cartilage surface over a subchondral cyst?
* Our current patient has a Stage III lesion, meaning the articular cartilage is breached, and we expect to find synovial fluid between the fragment and the underlying subchondral bone. This is ideal for microfracture.
* Surgical Warning:
> Surgical Warning: If you encounter an OLT that is primarily cystic with an intact cartilage surface, as suggested by MRI, nonoperative management or retrograde drilling might be considered over microfracture. However, retrograde drilling lacks high-level evidence and carries risks of heat necrosis and missing smaller lesions. If the chondral surface is softened and easily detachable, débridement is indicated.
3. Débridement of Unstable Cartilage and Lesion Preparation
Our goal here is to create a stable, healthy bed for the microfracture.
* Remove Unstable Cartilage: Using a small-joint shaver (e.g., 2.9 mm), a curette, or basket forceps, meticulously débride all unstable, delaminated, or fibrillated cartilage around the OLT. We want to create a stable, perpendicular shoulder of healthy cartilage surrounding the defect.
* Remove Fibrous Tissue: Any fibrous tissue within the lesion bed must be completely removed to expose the underlying subchondral bone. This is crucial for allowing marrow elements to egress.
* Prepare Subchondral Bone: Gently remove any calcified cartilage layer overlying the subchondral bone. The goal is to expose a firm, healthy subchondral bone plate without damaging it excessively.
*
* FIG 7 • Débridement of unstable cartilage and fibrous tissue from the OLT bed.
4. Microfracture Technique
This is the core of our procedure, designed to stimulate fibrocartilage formation. We use dedicated small-joint microfracture awls.
* Awl Selection: Choose an awl with an appropriate angle and tip to access the lesion effectively. We want a sharp, precise instrument to create clean perforations. The advantage of awls over drills or burrs is the avoidance of thermal necrosis.
* Penetration:
* Hold the awl perpendicular to the lesion surface. This is critical to ensure the holes are straight and allow maximal marrow access.
* Gently tap or push the awl into the subchondral bone.
* The depth of penetration should be 2 to 4 mm, just deep enough to penetrate the subchondral bone plate and reach the vascularized marrow space. Going too deep risks creating subchondral cysts or weakening the bone.
* Surgical Warning:
> Surgical Warning: Avoid creating excessively deep holes, which can weaken the subchondral bone and potentially lead to cyst formation. Conversely, too shallow holes will not reach the vascularized marrow.
* Spacing: Create a series of holes, typically 3 to 4 mm apart, across the entire débrided OLT surface. The goal is to create a "champagne effect," where blood and marrow elements visibly egress from each hole. This indicates successful penetration into the vascularized bone marrow.
*
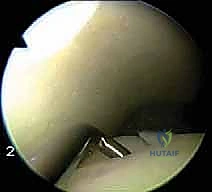
* FIG 8 • Microfracture awl being used to penetrate the subchondral bone.
*
* FIG 9 • Close-up arthroscopic view of microfracture holes with marrow egress.
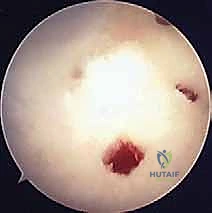
*
* FIG 10 • Another view of the completed microfracture pattern.
* Marrow Egress: Observe for the outflow of blood, indicating the release of pluripotent, marrow-derived mesenchymal stem cells. These cells will form a fibrin clot within the defect, which then differentiates into fibrocartilage.
*
* FIG 11 • The 'champagne effect' indicating successful marrow stimulation.
5. Addressing Associated Pathology and Final Lavage
- Synovectomy/Debridement: If significant synovitis or impingement was noted, perform a partial synovectomy or debride any impinging soft tissues.
- Loose Body Removal: Ensure all loose bodies are identified and removed.
- Lavage: Thoroughly lavage the joint to remove any debris.
- Tourniquet Release: Release the tourniquet and inspect for hemostasis.
6. Wound Closure
- Close the portal incisions with a single suture or sterile strips.
- Apply sterile dressings.
Pearls and Pitfalls
Pearls:
- Preoperative Planning is Paramount: Never skip the detailed review of MRI and CT scans. Know your lesion's exact location, size, and depth.
- Blunt Dissection: Always use blunt dissection for portal placement to protect neurovascular structures.
- Systematic Diagnostic Arthroscopy: Don't rush. Explore the entire joint to identify all pathologies.
- Complete Débridement: Ensure all unstable cartilage and fibrous tissue are removed to expose a healthy subchondral bone bed.
- Perpendicular Awl Penetration: Maintain a perpendicular angle to the lesion surface for optimal marrow access.
- "Champagne Effect": Verify marrow egress from each microfracture hole. This is your visual confirmation of effective marrow stimulation.
- Adequate Spacing: Space holes 3-4 mm apart to maximize coverage and stem cell delivery without compromising subchondral bone integrity.
Pitfalls and Salvage Strategies:
- Neurovascular Injury: If a nerve is transected, immediate repair by a microsurgeon is indicated. If a vessel is injured, direct pressure, electrocautery, or ligation may be necessary. Prevention is key through careful anatomy and blunt dissection.
- Inadequate Débridement: If unstable cartilage remains, the fibrocartilage repair will not adhere properly. Go back in and complete the débridement.
- Too Shallow/Too Deep Microfracture: If holes are too shallow, marrow stimulation is insufficient. If too deep, subchondral bone may be weakened. Use appropriate awls and ensure consistent depth. If the repair fails due to this, a repeat microfracture might be considered, but often salvage procedures like MACI or OATS are then indicated.
- Thermal Necrosis: This is why we prefer awls over drills. If drills are used, ensure copious irrigation and low-speed settings. Thermal necrosis can impair healing.
- Missed Lesions or Associated Pathology: Thorough diagnostic arthroscopy and preoperative imaging prevent this. If persistent symptoms post-op, re-evaluate with imaging and consider repeat arthroscopy.
- Persistent Pain/Failed Microfracture: If symptoms persist despite adequate rehabilitation, a repeat microfracture may be effective in select cases. However, in our hands, especially if we performed the index procedure, we move towards salvage with Matrix-based Autologous Chondrocyte Implantation (MACI) or Osteochondral Autograft Transfer System (OATS)/Mosaicplasty.
- MACI: Involves culturing autologous chondrocytes and implanting them within a scaffold. It's technically less demanding than first-generation ACI but is costly and lacks FDA approval in the US.
- **OATS/
REFERENCES
- Assenmacher JA, Kelikian AS, Gottlob C, et al. Arthroscopically assisted autologous osteochondral transplantation for osteochondral lesions of the talar dome: an MRI and clinical follow-up study. Foot Ankle Int 2001;22:544–551.

You Might Also Like