Posterolateral Spinal Decompression and Transpedicular Corpectomy: A Comprehensive Surgical Guide
Key Takeaway
Posterolateral decompression via a transpedicular approach is a powerful surgical technique for addressing complex spinal pathology involving the anterior, middle, and posterior columns. By avoiding the morbidity of a formal anterior thoracotomy, surgeons can achieve circumferential decompression and stabilization through a single posterior incision. This guide details the biomechanical rationale, step-by-step surgical execution, and critical pearls for safely resecting pedicles, reducing retropulsed fragments, and reconstructing the anterior column.
Introduction to Posterolateral Decompression
The management of complex spinal pathology—particularly lesions involving the anterior, middle, and posterior columns simultaneously—presents a formidable biomechanical and surgical challenge. Historically, circumferential spinal cord compression necessitated a combined anterior and posterior approach, often requiring a morbid thoracotomy or retroperitoneal exposure followed by posterior stabilization.
However, the evolution of the posterolateral transpedicular approach has revolutionized the surgical management of these complex cases. This technique allows for simultaneous neural decompression, tumor resection, and 360-degree spinal stabilization through a single posterior incision. It is particularly invaluable for patients with significant medical comorbidities who cannot tolerate the physiological insult of an anterior approach, or in cases where anterior pathology is predominant but posterior stabilization is absolutely mandated.
This comprehensive masterclass details the indications, biomechanical principles, and step-by-step surgical execution of posterolateral decompression and transpedicular corpectomy, synthesizing foundational evidence from landmark studies (such as the Maine Lumbar Spine Study) with advanced operative techniques.
Indications and Patient Selection
The posterolateral transpedicular approach is a highly versatile technique, though it requires meticulous patient selection. It is primarily indicated for:
- Spinal Neoplasms: Metastatic or primary tumors involving all three columns of the spine, where circumferential decompression is required.
- Traumatic Burst Fractures: Severe retropulsion of the posterior vertebral body wall into the spinal canal where an anterior approach is contraindicated.
- Severe Degenerative Spinal Stenosis with Instability: Cases complicated by degenerative spondylolisthesis, fixed sagittal imbalance, or massive synovial cysts requiring extensive facetectomy and pedicle resection.
- Infectious Spondylodiscitis: Epidural abscesses with extensive vertebral body destruction requiring debridement and stabilization.
- High-Risk Surgical Candidates: Patients with severe pulmonary or cardiovascular comorbidities who are unable to tolerate the single-lung ventilation or physiological stress of a thoracotomy.
⚠️ Surgical Warning: Vascular Considerations
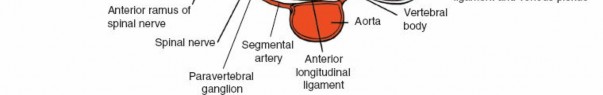
A direct anterior approach to the vertebral body may be impossible or highly morbid due to the risk of injury to the opposite segmental vessels, the aorta, or the vena cava, particularly in revision settings or highly vascularized tumors. The posterolateral approach mitigates these visceral and major vascular risks, though epidural venous bleeding can be substantial.
Biomechanical Rationale and Preoperative Planning
The Destabilization-Stabilization Paradigm
The posterolateral approach inherently destabilizes the spine. Resection of the lamina, facet joints, and the pedicle completely disrupts the posterior tension band and the middle column's load-sharing capacity. Consequently, instrumentation is an absolute necessity.
The timing of instrumentation is critical. Placing pedicle screws before the destabilizing decompression prevents catastrophic intraoperative subluxation and protects the neural elements. Pedicle screw fixation avoids the spinal canal compromise associated with sublaminar wires or hooks and provides rigid three-column control.
Preoperative Imaging
- Magnetic Resonance Imaging (MRI): Essential for evaluating the extent of neural compression, tumor margins, and the integrity of the posterior longitudinal ligament (PLL).
- Computed Tomography (CT): Mandatory for assessing bone stock, pedicle morphometry, and the exact location of retropulsed bone fragments.
- Angiography and Embolization: For hypervascular tumors (e.g., renal cell carcinoma, thyroid metastasis), preoperative selective arterial embolization within 24–48 hours of surgery significantly reduces intraoperative blood loss.
Surgical Technique: Posterolateral Decompression (Transpedicular Approach)
The following technique outlines the systematic approach to a posterolateral decompression and transpedicular corpectomy.
1. Positioning and Exposure
- Positioning: The patient is placed prone on a radiolucent Jackson spinal table. The abdomen must hang free to decrease intra-abdominal pressure, thereby reducing epidural venous engorgement and intraoperative bleeding.
- Incision: A standard midline longitudinal incision is made, centered over the pathological level.
- Exposure: Subperiosteal dissection is carried out laterally to the tips of the transverse processes in the lumbar spine, or the costotransverse junctions in the thoracic spine. Meticulous hemostasis is maintained.
- Localization: Intraoperative fluoroscopy is utilized to definitively confirm the correct pathological level.
2. Early Posterior Instrumentation
Because of the profound destabilization that occurs with laminectomy and pedicle resection, posterior instrumentation must be placed before the completion of the decompression.
💡 Clinical Pearl: Prophylactic Stabilization
We prefer to place pedicle screws before any exposure of the spinal canal. This minimizes the risk of incidental dural tears during implant placement and provides immediate anchor points. Early placement of implants can also be utilized to gently distract the ligamentous structures and disc space, facilitating easier decompression.
3. Laminectomy and Pedicle Identification
- If adequate decompression requires a full laminectomy, this is performed prior to the transpedicular decompression.
- Alternatively, a wide hemilaminectomy is highly effective for exposing the medial border of the pedicle and the lateral aspect of the thecal sac, helping to avoid inadvertent medial penetration during pedicle resection.
- The pedicle leading into the tumor or pathology is identified and sounded using a pedicle probe.
4. Transpedicular Decompression and Resection
- Pedicle Resection: Begin by resecting the lateral wall of the pedicle using a Leksell rongeur or a high-speed burr. Removing the lateral wall allows for the medialization of curets and instruments, keeping them away from the exiting nerve root and thecal sac.
- Medial Wall Resection: If the posterior vertebral body wall is retropulsed, the medial border of the pedicle must also be resected to gain access to the ventral epidural space.
- Bilateral Compression: If the neural compression is bilateral, a bilateral transpedicular approach is mandatory.
5. Ventral Decompression and Decancellation
This is the most critical and technically demanding phase of the operation.
- Decancellation: Before attempting to reduce retropulsed bone or tumor, the middle and anterior columns must be decancellated. Sequentially larger curets and a high-speed burr are used through the pedicle access site to hollow out the vertebral body, creating a ventral void.
- Fragment Reduction: Once a cavity is created within the vertebral body, a reverse-angle curet or a Posterior Lumbar Interbody Fusion (PLIF) tamp is carefully passed ventral to the dura.
- The instrument is placed against the tumor mass or retropulsed posterior vertebral wall. The pathology is then gently tamped or pushed anteriorly (away from the spinal cord) into the newly created void within the vertebral body.
- Resection: Once the retropulsed material is pushed anteriorly and the thecal sac is decompressed, the material is resected using straight and angled pituitary rongeurs.
🛑 Surgical Pitfall: Dural Manipulation
Never retract the spinal cord or thecal sac to access ventral pathology, especially in the thoracic spine. The transpedicular approach relies on creating a cavity in front of the cord and dropping the pathology into that cavity. Retraction of the cord will result in irreversible ischemic injury.
6. Anterior Column Reconstruction
Following a transpedicular corpectomy, the anterior column is left severely deficient.
* If a large portion of the anterior vertebral body was resected, a structural device (e.g., an expandable titanium cage or structural allograft) must be placed via the posterolateral corridor to support the anterior column.
* Graft Placement: Morcellized autograft or allograft is packed around the structural device.
* Critical Warning: Extreme care must be taken to ensure that morcellized graft is not retropulsed back into the spinal canal after placement, which would recreate the exact neural compression the procedure was intended to correct.
7. Pleural Evaluation and Closure
In the thoracic or thoracolumbar spine, the pleura may be inadvertently breached during the lateral exposure or corpectomy.
* The Valsalva Maneuver: Before closure, fill the surgical wound with warm saline irrigation until the lateral gutters are covered. Ask the anesthesiologist to momentarily maintain positive-pressure ventilation (Valsalva maneuver).
* Inspect the fluid for bubbling, which indicates a pleural leak. If a significant leak is identified, placement of a chest tube or a dedicated pleural drain is necessitated.
* Closure: Standard multilayered closure is performed over subfascial drains to prevent postoperative epidural hematoma.
Postoperative Protocol and Rehabilitation
- Neurological Monitoring: Strict neurological observations are required every 1–2 hours for the first 24 hours to monitor for evolving epidural hematomas.
- Mobilization: Because rigid segmental pedicle screw fixation is utilized, patients are typically mobilized on postoperative day 1 or 2.
- Bracing: Thoracolumbosacral orthosis (TLSO) bracing may be utilized depending on the surgeon's assessment of bone quality (e.g., severe osteoporosis) and the inherent stability of the construct, though rigid modern instrumentation often negates the absolute need for bracing.
- Radiographic Follow-up: Upright AP and lateral radiographs are obtained prior to discharge to confirm the maintenance of alignment and hardware integrity.
Evidence-Based Outcomes in Spinal Stenosis and Decompression
The surgical management of spinal stenosis and complex spinal lesions is heavily guided by decades of robust clinical research. Understanding the literature is paramount for the academic orthopedic surgeon.
Surgical vs. Conservative Management
Landmark prospective studies, including the Maine Lumbar Spine Study (Atlas et al., 1996, 2000, 2005) and the 10-year prospective study by Amundsen et al. (2000), have consistently demonstrated that surgical decompression provides superior long-term relief of leg pain and functional improvement compared to conservative management in patients with severe, symptomatic lumbar spinal stenosis. While conservative measures (epidural steroids, physical therapy) are appropriate first-line treatments, surgical intervention remains the definitive treatment for refractory neurogenic claudication.
The Role of Fusion
The necessity of fusion in conjunction with decompression has been extensively debated. Grob et al. (1995) and Fox et al. (1996) highlighted that decompression alone in the presence of preoperative instability (e.g., degenerative spondylolisthesis) leads to poor clinical outcomes and progressive deformity.
In the context of the posterolateral transpedicular approach described herein, fusion is not merely an option; it is a biomechanical imperative. As demonstrated by Goel (1998) and Gurr et al. (1988), the resection of the posterior elements and the pedicle drastically alters spinal kinematics. Rigid posterior instrumentation restores immediate stability, facilitates early mobilization, and provides the necessary mechanical environment for a solid arthrodesis, thereby preventing late kyphotic collapse and hardware failure.
Adjacent Segment Disease
Surgeons must remain cognizant of adjacent segment failure following rigid instrumentation. Etebar and Cahill (1999) noted that rigid fixation alters the stress distribution at adjacent levels, potentially accelerating degeneration. Meticulous surgical technique—specifically avoiding disruption of the adjacent level facet capsules during screw placement and exposure—is critical to minimizing this long-term complication.
Conclusion
Posterolateral decompression via a transpedicular approach is a highly demanding but exceptionally rewarding technique in the armamentarium of the complex spine surgeon. By adhering to strict biomechanical principles—namely, early instrumentation, meticulous decancellation, and avoidance of neural retraction—surgeons can safely achieve circumferential decompression and robust stabilization without the profound morbidity associated with anterior thoracotomy. Mastery of this technique ensures optimal outcomes for patients facing the most challenging spinal pathologies.
You Might Also Like