Unlock Surgical Success: Lumbar Spines Applied Anatomy Guide
Key Takeaway
Here are the crucial details you must know about Unlock Surgical Success: Lumbar Spines Applied Anatomy Guide. Understanding the posterior muscles of the thoracic and **lumbar spines applied** surgically involves recognizing three layers: superficial, intermediate, and deep. These layers clarify dissection, despite not always being visually distinct during surgery. The superficial and intermediate layers, responsible for upper extremity attachment and accessory respiration, are generally safe during midline dissection. The deep intrinsic back muscles, however, risk partial denervation with excessive lateral dissection.
Unlock Surgical Success Lumbar Spines Applied Anatomy Guide
Introduction and Epidemiology
Surgical intervention in the lumbar spine remains a cornerstone of treatment for a diverse range of pathological conditions, including degenerative diseases, traumatic injuries, deformities, and oncological processes. The success of these procedures is inherently tethered to a profound understanding of applied surgical anatomy. Despite advancements in imaging, navigation, and minimally invasive techniques, the fundamental principles of anatomical dissection and neurovascular preservation continue to dictate operative outcomes. This guide aims to provide a high-yield, comprehensive review of the applied surgical anatomy of the posterior lumbar spine, emphasizing practical considerations for orthopedic surgeons, residents, and medical students. The epidemiology of lumbar spine pathology underscores its significant socioeconomic burden, with low back pain being a leading cause of disability globally. Degenerative conditions, such as disc herniation, spinal stenosis, and spondylolisthesis, represent the most frequent indications for surgical intervention, necessitating meticulous anatomical precision to achieve effective decompression and stable fusion while minimizing iatrogenic sequelae.
Surgical Anatomy and Biomechanics
Overview of Posterior Musculature
The posterior muscles of the thoracic and lumbar spines are arranged in distinct layers, a conceptual framework critical for methodical surgical exposure and minimizing iatrogenic damage. While these layers may not always be sharply demarcated during a subperiosteal dissection, understanding their arrangement and innervation guides the surgical approach.
- Superficial layer: Primarily mooring muscles that connect the upper extremity to the axial skeleton. These include the trapezius and latissimus dorsi. A deeper component of this layer comprises the rhomboid major and minor. These muscles are typically encountered during more extensive thoracolumbar exposures or in cases requiring access to the posterior thoracic wall, but are largely undisturbed by a standard midline lumbar approach.
- Intermediate layer: Composed of the serratus posterior superior and serratus posterior inferior. These are small, flat, laterally placed muscles that attach to the ribs and vertebrae. Their primary role is in accessory respiration. Similar to the superficial layer, these muscles are generally not within the direct field of a posterior midline lumbar surgical approach and thus their innervation and integrity are usually preserved.
- Deep layer: This constitutes the intrinsic muscles of the back, collectively known as the paraspinal muscle system. These muscles are intimately involved in spinal stability and movement and are directly encountered during posterior lumbar exposure. This layer includes:
- Sacrospinalis muscles (Erector Spinae): The largest and most superficial group within the deep layer, running longitudinally. Composed of iliocostalis (lateral), longissimus (intermediate), and spinalis (medial) columns. These muscles are stripped subperiosteally off the posterior elements during a standard midline approach.
- Transversospinalis group: A deeper, obliquely running layer consisting of the semispinalis, multifidus, and rotator muscles. The multifidus is particularly well-developed in the lumbar region and plays a critical role in segmental stability. These muscles span multiple vertebral segments (semispinalis), 2-4 segments (multifidus), or a single segment (rotatores).
The nerve supply to these layers is distinct and has significant surgical implications. The superficial layer muscles are supplied by peripheral nerves (e.g., trapezius by the spinal accessory nerve, rhomboids by the dorsal scapular nerve from C5, latissimus dorsi by the thoracodorsal nerve). The intermediate layer muscles are supplied by the anterior primary rami. Critically, the deep layer muscles are supplied segmentally at each level of the spine by the posterior rami of the thoracic and lumbar nerves. While a careful subperiosteal dissection aims to minimize disruption, excessive lateral dissection, particularly beyond the facet capsules and lateral to the transverse processes, carries a risk of partial denervation or devascularization of these vital stabilizing muscles, potentially contributing to postoperative paraspinal muscle atrophy and "failed back surgery syndrome."
Osteology and Ligamentous Structures
A comprehensive understanding of lumbar osteology is paramount for pedicle screw placement, decompression, and fusion.
* Vertebral Body: Large, kidney-shaped, primary weight-bearing structure.
* Pedicles: Strong, short bony processes extending posteriorly from the vertebral body, forming the lateral walls of the vertebral foramen. They serve as the primary conduit for pedicle screw fixation. Pedicle morphology (length, width, angulation) varies segmentally and between individuals, necessitating careful preoperative planning.
* Laminae: Flat plates of bone extending posteromedially from the pedicles, uniting in the midline to form the spinous process. These form the posterior boundary of the vertebral canal. Laminectomy or laminotomy involves resection of these structures.
* Spinous Processes: Project posteriorly and inferiorly from the junction of the laminae. Serve as attachment points for ligaments and muscles, and as landmarks for midline incision and initial dissection.
* Transverse Processes: Project laterally from the pedicle-lamina junction. Provide attachment for muscles and serve as potential sites for posterolateral fusion.
* Articular Processes (Facets): Superior and inferior articular processes extend from the lamina-pedicle junction, forming the facet joints. The lumbar facet joints are typically oriented in a sagittal plane, limiting rotation and guiding flexion/extension. The integrity of the facet joints is crucial for spinal stability; excessive resection during decompression can lead to iatrogenic instability.
Key ligaments stabilizing the lumbar spine include:
* Ligamentum Flavum: Strong, elastic ligament connecting adjacent laminae, preserving the neural canal diameter and assisting in extension. Hypertrophy contributes to spinal stenosis.
* Interspinous Ligament: Connects adjacent spinous processes.
* Supraspinous Ligament: Connects the tips of the spinous processes from C7 to the sacrum, merging with the thoracolumbar fascia.
* Anterior and Posterior Longitudinal Ligaments (ALL/PLL): Run along the anterior and posterior aspects of the vertebral bodies, respectively. The PLL provides some containment for disc material but is narrower in the lumbar spine than the ALL, particularly posteriorly.
* Capsular Ligaments: Enclose the facet joints.
Neural Elements
The neural structures within the lumbar spinal canal are highly vulnerable during posterior surgical approaches.
* Conus Medullaris: In adults, the spinal cord typically terminates as the conus medullaris around the L1-L2 vertebral level. Surgical procedures above this level carry a direct risk of spinal cord injury.
* Cauda Equina: Below the conus, the spinal canal contains the cauda equina, a bundle of lumbar and sacral nerve roots bathed in cerebrospinal fluid within the dural sac. While more resilient than the spinal cord, these nerve roots can be injured by direct trauma, excessive retraction, or compression.
* Dura Mater and Arachnoid Mater: The outer dura mater and inner arachnoid mater enclose the cerebrospinal fluid and neural elements. Dural tears are a common intraoperative complication, requiring meticulous repair to prevent CSF leakage.
* Nerve Roots: Lumbar nerve roots typically exit below their correspondingly numbered pedicle (e.g., L4 nerve root exits below the L4 pedicle). However, understanding the traversing and exiting roots within the spinal canal and neural foramen is critical for targeted decompression. The dorsal root ganglion (DRG), particularly sensitive to compression, is typically located within the neural foramen.
* Posterior Primary Rami: These small nerves innervate the deep paraspinal muscles, facet joints, and posterior ligaments. They emerge laterally from the main spinal nerve, deep to the transverse process. Their preservation during lateral dissection is crucial for minimizing postoperative denervation.
Vascular Supply
The vascularity of the lumbar spine, though often overlooked until bleeding is encountered, is critical for both spinal health and surgical planning.
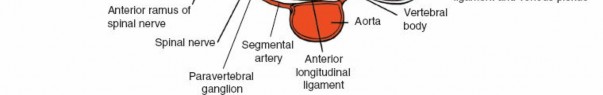
* Segmental Arteries: Paired segmental arteries arise from the posterior aspect of the aorta, typically at each vertebral level. These travel around the vertebral body, giving off branches to the muscles, ligaments, and neural structures. They give rise to radicular arteries that supply the nerve roots and contribute to the anterior and posterior spinal arteries.
* Anterior and Posterior Spinal Arteries: Longitudinal arteries running the length of the spinal cord, supplied by reinforcing radicular arteries. Damage to a major reinforcing radicular artery (e.g., artery of Adamkiewicz, though more common in the thoracolumbar region) can lead to spinal cord ischemia.
* Venous Plexuses: Extensive epidural venous plexuses (anterior and posterior) are located within the spinal canal. These are valveless and can become engorged with increased abdominal pressure, leading to significant intraoperative bleeding. Careful patient positioning is crucial to decompress the abdomen and minimize this engorgement. External venous plexuses also exist in the paraspinal musculature. Meticulous hemostasis is vital.
Biomechanics of Lumbar Spine
The lumbar spine is engineered for substantial load-bearing and a balance of mobility and stability.
* Load Bearing: The large vertebral bodies and thick intervertebral discs are adapted to bear significant axial loads.
* Motion: Predominantly flexion and extension, with limited rotation and lateral bending, due to the sagittal orientation of the facet joints.
* Stability: Provided by a complex interplay of osseous structures (facet joints), ligaments (ligamentum flavum, interspinous, supraspinous, ALL, PLL, capsular), and the intrinsic deep paraspinal muscles. Damage to any of these components, particularly during decompression or extensive facetectomy, can compromise stability and potentially necessitate fusion. Surgical strategies aim to restore or maintain this biomechanical balance.
Indications and Contraindications
Surgical intervention in the lumbar spine is considered when conservative measures fail or in the presence of severe neurological deficits. Patient selection is paramount for optimal outcomes.
Degenerative Conditions
- Lumbar Disc Herniation (LDH): Radiculopathy (unremitting, severe, progressive, or intractable) unresponsive to conservative management. Cauda equina syndrome constitutes an absolute surgical emergency.
- Lumbar Spinal Stenosis: Neurogenic claudication or radicular pain severely impacting quality of life, refractory to non-operative treatment. Can be central, lateral recess, or foraminal.
- Degenerative Spondylolisthesis: Instability (dynamic imaging) or significant symptoms (pain, radiculopathy, claudication) unresponsive to conservative management. Typically requires decompression and fusion.
- Degenerative Scoliosis: Progressive deformity, intractable axial back pain, or radicular/neurogenic symptoms associated with coronal or sagittal imbalance.
Traumatic Injuries
- Lumbar Fractures: Unstable fractures (e.g., burst fractures with canal compromise, distraction injuries, translational injuries) requiring stabilization and/or decompression. Neurological deficit or impending neurological compromise is a strong indication.
- Lumbar Dislocations: Almost invariably unstable and associated with neurological deficit, requiring urgent reduction and stabilization.
Deformity
- Adult Spinal Deformity (Scoliosis, Kyphosis): Progressive deformity, significant pain, functional impairment, or neurological compromise due to imbalance.
Tumors and Infections
- Primary and Metastatic Spinal Tumors: Instability, neurological compression, intractable pain, or necessity for biopsy/debulking.
- Spinal Infections (Osteomyelitis, Discitis, Epidural Abscess): Progressive neurological deficit, unremitting pain, systemic sepsis, or failed medical management.
Contraindications for Posterior Lumbar Surgery
- Absolute Contraindications:
- Severe medical comorbidities that preclude safe anesthesia or surgical tolerance (e.g., uncontrolled cardiac failure, severe respiratory insufficiency).
- Active systemic infection or sepsis (may be a relative contraindication for local infection, requiring initial antibiotic management).
- Unrealistic patient expectations or significant psychosocial factors unaddressed.
- Relative Contraindications:
- Uncontrolled coagulopathy.
- Severe osteoporosis (impacts instrumentation purchase).
- Active tobacco use (significantly impairs fusion rates).
- Obesity (increases surgical complexity and complication rates).
- Psychiatric comorbidities, opioid dependence, or secondary gain issues.
Operative vs Non Operative Indications
| Condition | Operative Indications | Non-Operative Indications |
|---|---|---|
| Lumbar Disc Herniation | Cauda equina syndrome (emergency), progressive neurological deficit, intractable radiculopathy > 6 weeks refractory to conservative care. | Radiculopathy with improvement, mild neurological deficits, symptoms < 6 weeks, no cauda equina. |
| Spinal Stenosis | Progressive neurogenic claudication, severe functional limitation, intractable pain refractory to conservative care. | Mild symptoms, stable symptoms, response to physical therapy, epidural injections. |
| Degenerative Spondylolisthesis | Progressive slip, intractable pain, radiculopathy, neurogenic claudication, instability on dynamic imaging. | Mild symptoms, stable slip, response to conservative management. |
| Lumbar Fractures | Unstable fracture patterns (e.g., burst with >50% canal compromise, distraction, translational), progressive neurological deficit. | Stable compression fractures, no neurological deficit, managed with bracing and rehabilitation. |
| Spinal Tumors | Spinal cord compression, instability, intractable pain, pathological fracture, biopsy required. | Asymptomatic incidental findings, amenable to radiation/chemotherapy without urgent decompression. |
| Spinal Infections | Neurological deficit, epidural abscess, progressive instability, failed antibiotic therapy. | Early infection without neurological compromise, responsive to IV antibiotics. |
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is crucial for anticipating challenges, ensuring appropriate resources, and optimizing patient safety.
Imaging Review
- Plain Radiographs: Anteroposterior, lateral, and flexion/extension views are essential for assessing overall alignment, disc space height, vertebral body morphology, and dynamic instability (e.g., spondylolisthesis).
- Magnetic Resonance Imaging (MRI): The gold standard for evaluating neural compression, disc pathology, ligamentous integrity, and soft tissue abnormalities (tumors, infections). Sagittal and axial T1, T2, and STIR sequences are typically reviewed.
- Computed Tomography (CT): Provides detailed assessment of bony anatomy, cortical integrity, facet joint degeneration, osteophyte formation, and fusion status. Useful for pedicle screw trajectory planning, especially in deformity or revision cases.
- CT Myelogram: May be indicated when MRI is contraindicated or inconclusive, offering excellent visualization of the neural canal and nerve root compression.
Surgical Planning
- Level Identification: Precise identification of the surgical level(s) is paramount. This involves correlating preoperative imaging with anatomical landmarks and intraoperative fluoroscopy or navigation.
- Instrumentation Planning: Based on imaging, determine appropriate pedicle screw length and diameter, rod contour, interbody cage size and lordotic angle, and bone graft material. Consider construct stiffness and length based on fusion requirements.
- Contingency Planning: Anticipate potential complications such as dural tears, excessive bleeding, or difficult screw trajectories, and prepare appropriate instruments and materials.
Patient Positioning
Proper patient positioning is critical to optimize surgical exposure, minimize complications, and ensure adequate C-arm access.
* Prone Position: The patient is positioned prone on a specialized spinal frame (e.g., Jackson table, Wilson frame, Relton-Hall frame). The primary goal is to minimize abdominal compression, which reduces epidural venous engorgement and thereby decreases intraoperative blood loss.
* Padding: All pressure points (cheeks, eyes, breasts, iliac crests, knees, feet) must be meticulously padded to prevent neuropathies, skin breakdown, and compartment syndrome.
* Head Positioning: Neutral head position to prevent cervical strain and brachial plexus stretch.
* Arm Positioning: Arms are typically abducted and externally rotated on arm boards, ensuring the shoulders are not protracted and the brachial plexus is not stretched.
* Abdominal Decompression: The frame should allow the abdomen to hang freely.
* C-arm Access: Ensure unrestricted access for intraoperative fluoroscopy in both anteroposterior and lateral planes, particularly critical for pedicle screw placement.
* Prepping and Draping: Wide sterile prep and drape from the mid-thoracic region to the buttocks, encompassing bilateral iliac crests if bone graft harvest is anticipated.
Detailed Surgical Approach and Technique
The posterior midline approach to the lumbar spine remains the workhorse for most decompression and fusion procedures. Meticulous technique, guided by anatomical precision, is essential.
Incision and Superficial Dissection
- Incision: A vertical midline incision is typically made directly over the spinous processes of the target levels. The length of the incision is dictated by the number of levels involved and the complexity of the procedure. For minimal access procedures, a smaller incision or multiple mini-incisions can be utilized.
- Subcutaneous Dissection: The subcutaneous fat is incised, and bleeding vessels are cauterized.
- Thoracolumbar Fascia: The thoracolumbar fascia, a robust posterior aponeurosis, is identified and incised in the midline, directly over the tips of the spinous processes. This midline raphe is relatively avascular and separates the paraspinal muscles.
Muscle Exposure and Subperiosteal Dissection
- Subperiosteal Reflection: Using electrocautery and periosteal elevators (e.g., Cobb elevators), the erector spinae muscles (sacrospinalis group) are systematically reflected subperiosteally off the spinous processes, laminae, and facet capsules. This dissection should be carried out from medial to lateral, staying strictly on bone.
- Exposure Extent: The dissection proceeds laterally to the tips of the transverse processes if a posterolateral fusion is planned, or to the lateral aspect of the facet joints for decompression or interbody fusion. For pedicle screw placement, the junction of the transverse process and the superior articular process serves as a key landmark.
- Internervous Plane Preservation: The posterior rami of the spinal nerves supply the deep paraspinal muscles and facet joints. These nerves typically emerge laterally from the intertransverse space. Excessive lateral dissection, particularly beyond the tips of the transverse processes, can inadvertently denervate these critical muscles, leading to atrophy and functional deficits. Maintaining the subperiosteal plane minimizes muscle damage and preserves vascularity.
- Hemostasis: Meticulous hemostasis is maintained throughout the muscle dissection using electrocautery, topical hemostatic agents, and careful packing.
Laminectomy and Decompression
- Level Confirmation: Once the posterior elements are exposed, the surgical level(s) must be unequivocally confirmed using intraoperative fluoroscopy, typically by counting up from the sacrum or down from a clearly identifiable anatomical landmark (e.g., L1 transverse process).
- Laminectomy/Laminotomy: Bone removal techniques vary depending on the pathology. A laminotomy involves partial removal of the lamina, typically at the inferior edge, to access the ligamentum flavum. A laminectomy involves complete removal of the lamina and spinous process. High-speed burrs, Kerrison rongeurs, and osteotomes are used carefully to remove bone while protecting the underlying dura and neural elements.
- Ligamentum Flavum Resection: The ligamentum flavum is meticulously resected, often using a combination of Kerrison rongeurs and specialized elevators. This typically involves dissecting it off the dura, taking care not to perforate the dural sac.
- Facetectomy: Medial facetectomy is often necessary to achieve adequate neural decompression, particularly in cases of lateral recess stenosis or foraminal stenosis. Excessive facetectomy can lead to iatrogenic instability, necessitating fusion. Foraminotomy involves enlarging the neural foramen to decompress the exiting nerve root.
- Discectomy: For disc herniations, the nerve root is gently retracted, and the annular fibers are incised. Disc material, particularly extruded or sequestrated fragments, is removed using pituitary rongeurs. Care is taken to avoid excessive disc space preparation if an interbody fusion is not planned, to prevent iatrogenic instability.
Instrumentation and Fusion
- Pedicle Screw Placement: The entry point for pedicle screws is typically at the intersection of the transverse process and the superior articular process, or slightly superolateral to the facet joint. A high-speed burr or osteotome is used to create a cortical breach. A pedicle probe is then used to create a pilot hole, palpating all five pedicle walls (superior, inferior, medial, lateral, anterior) to ensure an intraosseous trajectory. Taps are used to prepare the bone, and screws are inserted under fluoroscopic guidance or with navigation.
- Rod Contouring and Insertion: After screw placement, rods are contoured to restore or maintain physiological lordosis and connect the screws. Reduction maneuvers (e.g., direct vertebral derotation, cantilever, compression/distraction) are performed as needed to correct deformity or reduce spondylolisthesis. Set screws are then tightened to secure the construct.
- Interbody Fusion (TLIF, PLIF):
- Transforaminal Lumbar Interbody Fusion (TLIF): Involves unilateral facetectomy (usually the side of worse symptoms or greater nerve root compromise) to access the disc space. The disc is removed, endplates are prepared, and an interbody cage (filled with bone graft) is inserted obliquely into the disc space. This restores disc height and provides anterior column support.
- Posterior Lumbar Interbody Fusion (PLIF): Involves bilateral laminectomy and bilateral neural retraction to insert two cages into the disc space. While offering potentially broader anterior column support, it carries a higher risk of neural injury due to greater retraction.
- Posterolateral Fusion (PLF): Autograft or allograft bone is placed in the posterolateral gutters (between the transverse processes and the facet joints) after decortication of the transverse processes and laminae. This provides a broad bed for bone healing and fusion. Often performed in conjunction with interbody fusion to enhance fusion rates.
- Bone Graft: Autograft (e.g., local bone from decompression, iliac crest) remains the gold standard. Allograft (cadaveric bone) and various bone graft substitutes (e.g., DBM, BMPs) are also utilized.
Wound Closure
- Irrigation: The wound is thoroughly irrigated to remove bone dust, blood clots, and debris.
- Dural Repair: Any dural tears are meticulously repaired primarily with sutures, often reinforced with dural sealants or fascia.
- Drain Placement: A closed suction drain may be placed in the deep fascial layer to reduce hematoma formation, particularly after extensive procedures or in patients at higher risk of bleeding.
- Fascial Closure: The thoracolumbar fascia is meticulously reapproximated with strong absorbable sutures. This is the most critical layer for preventing wound dehiscence and pseudomeningocele.
- Subcutaneous and Skin Closure: Subcutaneous tissues are closed, followed by skin closure with staples or sutures.
Complications and Management
Despite meticulous technique, complications can occur following posterior lumbar spine surgery. Prompt recognition and appropriate management are crucial.
Neurological Injury
- Nerve Root Injury: Can manifest as new or worsened radiculopathy, motor weakness, or sensory deficits. Causes include direct trauma, excessive retraction, thermal injury from cautery, or screw malposition. Management involves prompt identification, revision surgery if instrumentation is the cause, and corticosteroids for inflammation.
- Cauda Equina Syndrome (CES): A rare but devastating complication involving bowel/bladder dysfunction, saddle anesthesia, and bilateral lower extremity weakness. Requires immediate surgical re-exploration and decompression.
- Dural Tear: Incidence varies from 3-17%. Can lead to CSF leak, pseudomeningocele, orthostatic headaches, and increased risk of infection (meningitis). Intraoperative recognition is key, with primary repair (sutures), dural sealants, and often bed rest and restricted activity postoperatively.
Vascular Injury
- Major Vessel Laceration: Extremely rare but potentially catastrophic, involving the aorta, vena cava, or iliac vessels, typically during anterior penetration of the vertebral body by a pedicle screw or during anterior column instrumentation. Requires immediate vascular surgery consultation and repair.
- Epidural Venous Bleeding: Common, especially if abdominal decompression is inadequate. Managed with careful packing, bipolar cautery, and topical hemostatic agents.
Infection
- Surgical Site Infection (SSI): Can be superficial (managed with antibiotics, wound care) or deep (requires surgical debridement, washout, IV antibiotics, potentially instrumentation removal in chronic cases). Prophylactic antibiotics, meticulous sterile technique, and careful wound closure are vital for prevention.
- Discitis/Osteomyelitis: Infection of the intervertebral disc space or vertebral body. Managed with prolonged IV antibiotics and often surgical debridement and stabilization if severe or progressive.
Instrumentation Failure
- Screw Pullout/Loosening: Can occur in osteoporotic bone or with inadequate purchase. May lead to loss of correction, pseudarthrosis, or recurrent instability, often requiring revision surgery.
- Rod Fracture: Signifies pseudarthrosis and excessive stress on the instrumentation. Requires revision surgery with concomitant fusion augmentation.
- Pseudarthrosis (Non-union): Failure of bone fusion. May be asymptomatic or cause persistent pain and progressive deformity. Diagnosis can be challenging (CT scan, dynamic X-rays). Revision surgery with decortication, bone grafting, and potentially re-instrumentation is often required.
Other Complications
- Hematoma/Seroma: Can cause local pain, swelling, and rarely neural compression. Drains help reduce incidence.
- Persistent Pain/Failed Back Surgery Syndrome: Multifactorial, including inadequate decompression, pseudarthrosis, adjacent segment disease, deconditioning, psychosocial factors, or residual neuropathy.
- Adjacent Segment Disease (ASD): Degeneration at levels adjacent to a fusion. May require further surgery.
- Medical Complications: Deep vein thrombosis (DVT), pulmonary embolism (PE), pneumonia, urinary tract infection, cardiac events. Prophylaxis and close monitoring are essential.
Complications Incidence and Salvage Strategies
| Complication | Incidence (%) | Salvage Strategies |
|---|---|---|
| Dural Tear | 3-17 | Primary repair (suture), dural patch/sealant, fibrin glue, bed rest, CSF drain (rarely). |
| Nerve Root Injury | 1-5 | Revision for hardware malposition or inadequate decompression, corticosteroids, physical therapy. |
| Superficial SSI | 1-3 | Oral/IV antibiotics, local wound care, wound debridement (if abscess). |
| Deep SSI | 0.5-2 | Surgical debridement and washout, IV antibiotics, hardware removal (in chronic cases). |
| Instrumentation Failure | 2-10 | Revision surgery with stronger construct, additional levels, bone grafting, consideration of biologics. |
| Pseudarthrosis | 5-20 (fusion) | Revision fusion with decortication, bone grafting, biologics, possibly different approach. |
| Major Vascular Injury | <0.1 | Immediate vascular surgeon consultation, direct repair, tamponade. |
| Hematoma | 1-5 | Observation, wound drainage (if symptomatic or compressive), evacuation. |
| Adjacent Segment Disease | 2-4 per year | Conservative management initially, decompression +/- fusion of affected segment if symptoms persist. |
Post Operative Rehabilitation Protocols
Postoperative rehabilitation is an integral component of recovery, aiming to restore function, minimize pain, and facilitate return to activity. Protocols vary based on the surgical procedure (decompression vs. fusion), patient comorbidities, and surgeon preference.
Immediate Postoperative Period (Days 0-7)
- Pain Management: Multimodal analgesia including opioids, NSAIDs, acetaminophen, and muscle relaxants to facilitate early mobilization.
- Early Mobilization: Ambulation typically begins within 24 hours post-decompression and 24-48 hours post-fusion, often with physical therapist assistance. Emphasis on proper body mechanics and posture.
- Bracing: May be prescribed for fusion patients (e.g., rigid thoracolumbosacral orthosis - TLSO) to provide external support and limit motion, particularly in multi-level fusions, osteoporotic patients, or revision cases. The duration varies but is typically 6-12 weeks. Not generally required after single-level decompressions.
- Activity Restrictions: Avoidance of bending, lifting (typically >5-10 lbs), and twisting (BLT precautions). Spinal precautions are enforced.
Early Rehabilitation (Weeks 1-6)
- Progression of Ambulation: Gradually increase walking distance and duration.
- Gentle Core Activation: Initiate isometric core exercises (e.g., transverse abdominis bracing) and pelvic tilts to improve stability without stressing the surgical site.
- Postural Education: Reinforce ergonomic principles for sitting, standing, and sleeping.
- Avoidance: Continue strict BLT precautions. Avoid high-impact activities.
Intermediate Rehabilitation (Weeks 6-12)
- Physical Therapy: Formal physical therapy sessions are typically initiated.
- Gradual Increase in Activity: Progressive increase in resistance and range of motion exercises as tolerated, under therapist guidance.
- Strengthening: Focus on strengthening of core musculature (abdominal and paraspinal muscles), gluteals, and lower extremities.
- Proprioceptive Training: Balance and coordination exercises to improve neuromuscular control.
- Scar Mobilization: Gentle massage of the incision site once well-healed to prevent adhesions.
Advanced Rehabilitation (Beyond 12 Weeks)
- Return to Sport/Work-Specific Activities: Gradually incorporate activities relevant to the patient's occupation or recreational pursuits. This stage focuses on functional training and endurance.
- High-Impact Activities: Introduction of higher impact activities or heavy lifting only after achieving robust strength, stability, and surgeon clearance, typically after 6 months to a year for fusion patients, once radiographic evidence of fusion is confirmed.
- Long-term Spine Hygiene: Continued emphasis on proper body mechanics, regular exercise, weight management, and activity modification to prevent recurrence or new issues.
Summary of Key Literature and Guidelines
The field of lumbar spine surgery is continually evolving, driven by ongoing research and technological innovation. Evidence-based guidelines from professional organizations such as the North American Spine Society (NASS), the American Academy of Orthopaedic Surgeons (AAOS), and the Scoliosis Research Society (SRS) provide critical frameworks for clinical decision-making.
For lumbar disc herniation, numerous randomized controlled trials and meta-analyses consistently demonstrate that surgical discectomy provides faster and more complete relief of radicular symptoms compared to conservative management in carefully selected patients who fail initial non-operative treatment. However, long-term outcomes at 1-2 years often show similar results between surgical and non-surgical groups, highlighting the importance of proper patient selection and timing. The Spine Patient Outcomes Research Trial (SPORT) is a landmark study providing robust evidence for surgical efficacy in both disc herniation and spinal stenosis.
In lumbar spinal stenosis, decompression, with or without fusion, has been shown to improve function and reduce pain more effectively than non-operative care in patients with moderate to severe symptoms refractory to conservative measures. The decision to fuse in degenerative stenosis is often guided by the presence of preoperative instability, iatrogenic instability created by extensive decompression, or concomitant deformity.
For degenerative spondylolisthesis, current evidence suggests that decompression combined with fusion yields superior outcomes regarding pain and functional improvement compared to decompression alone, particularly in cases with demonstrable instability or when extensive facetectomy is required for decompression.
The literature consistently emphasizes the critical role of meticulous surgical technique and a thorough understanding of applied anatomy in minimizing complications and optimizing outcomes. Minimally invasive approaches, while offering potential benefits in terms of reduced muscle dissection and faster recovery, still necessitate a profound anatomical knowledge and specific training to navigate the smaller surgical corridors safely. Advances in navigation and intraoperative imaging (e.g., O-arm, CT navigation) have enhanced pedicle screw accuracy but do not supplant the need for a deep anatomical foundation.
In conclusion, surgical success in the lumbar spine is multifaceted, relying on a judicious combination of appropriate patient selection, rigorous preoperative planning, an exhaustive understanding of applied surgical anatomy, precise execution of surgical technique, and comprehensive postoperative rehabilitation. Continued adherence to these principles, informed by evolving literature and guidelines, remains paramount for achieving predictable and durable patient benefit.
Clinical & Radiographic Imaging
You Might Also Like