Understanding the Rami of Spinal Nerves in Posterior Approaches
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Understanding the Rami of Spinal Nerves in Posterior Approaches. The deep posterior musculature of the spine, including the erector spinae and transversospinalis, is segmentally innervated by the posterior dorsal rami of spinal nerves. This vital neural supply provides extensive redundancy to these muscles, contrasting with superficial and intermediate layers supplied by peripheral nerves not encountered through a posterior approach.
Introduction and Epidemiology
The posterior approach to the spine remains the foundational workhorse for orthopedic spine surgeons and neurosurgeons, providing versatile access for decompression, deformity correction, and arthrodesis across the cervical, thoracic, and lumbar regions. Despite the ubiquitous nature of this approach, iatrogenic injury to the paraspinal musculature and its innervation—specifically the posterior dorsal rami of the spinal nerves—remains a significant source of postoperative morbidity. Understanding the precise anatomical course of the dorsal rami is paramount for minimizing denervation atrophy, reducing postoperative axial back pain, and preventing secondary sagittal imbalance.

Epidemiological studies evaluating postoperative outcomes following extensive posterior lumbar spinal fusions demonstrate that up to 30% of patients experience clinically significant paraspinal muscle atrophy, often termed "multifidus lipomatosis" or fatty infiltration. This phenomenon is directly correlated with prolonged retractor times, excessive lateral dissection, and indiscriminate electrocautery, which collectively compromise the medial branches of the dorsal rami. Consequently, modern surgical techniques emphasize tissue-sparing dissection, utilization of internervous planes, and rigorous preservation of the neurovascular pedicles supplying the deep erector spinae and transversospinalis muscle groups.

Surgical Anatomy and Biomechanics
Surface Landmarks and Topographical Anatomy
Superficial landmarks enable gross determination of the anatomic level prior to incision and fluoroscopic localization. Proximally, C7 (vertebra prominens) and T1 possess the largest spinous processes and serve as reliable, palpable anatomic landmarks for cervicothoracic junction procedures. Distally, the intercrestal line (Tuffier's line), which connects the superior margins of the iliac crests, classically approximates the L4-L5 interspace or the L4 spinous process, though this relationship varies based on pelvic morphology and patient positioning.

Muscular Layers of the Posterior Spine
The posterior musculature of the spine is divided into three distinct layers, each with specific origins, insertions, and neurovascular supplies.
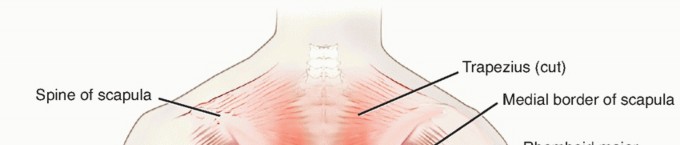
- Superficial Layer: Comprises the trapezius, latissimus dorsi, rhomboid major and minor, and the levator scapulae. The trapezius (innervated by the spinal accessory nerve) and latissimus dorsi (innervated by the thoracodorsal nerve) form the primary superficial coverage. These muscles are primarily involved in appendicular skeletal movement rather than primary spinal stabilization.
- Intermediate Layer: Consists of the superior and inferior serratus posterior and the levatores costarum. These function primarily as accessory muscles of respiration.
- Deep Layer: Comprises the erector spinae (iliocostalis, longissimus, spinalis), transversospinalis (multifidus, semispinalis, rotatores), interspinalis, and the intertransversarii. This layer is critical for dynamic spinal stabilization and extension.

The superficial and intermediate layers receive their nervous supply from peripheral nerves (e.g., dorsal scapular nerve, thoracodorsal nerve), which are generally not encountered or compromised through a standard posterior midline approach. Conversely, the deep layer receives its nervous supply segmentally from the posterior dorsal rami.
Neuroanatomy of the Dorsal Rami
Upon exiting the intervertebral foramen, the mixed spinal nerve promptly divides into a ventral ramus (forming the lumbosacral plexus and intercostal nerves) and a dorsal ramus. The dorsal ramus is the critical neurological structure in posterior spinal surgery.

In the lumbar spine, the dorsal ramus courses posteriorly through the intertransverse space and divides into three branches:
1. Medial Branch: Courses caudally and medially, crossing the junction of the superior articular process (SAP) and the transverse process. It lies in a groove covered by the mamillo-accessory ligament. It provides motor innervation to the multifidus and interspinalis muscles, and sensory innervation to the facet joint at its level and the level below.
2. Intermediate Branch: Innervates the longissimus muscle.
3. Lateral Branch: Innervates the iliocostalis muscle and provides cutaneous sensory branches to the overlying skin (e.g., superior cluneal nerves from L1-L3).
There is a large amount of redundancy in the innervation of the deep layer; however, the medial branch is highly susceptible to iatrogenic injury during lateral subperiosteal dissection or aggressive facet capsule coagulation. The midline approach is a true internervous plane. Nerve injury to the dorsal rami occurs primarily with excessive lateral dissection beyond the facet joints.

Vascular Supply and Ligamentous Structures
The vascular supply to the deep layer is derived from segmental dorsal branches of the aorta (intercostal and lumbar arteries). These vessels course posteriorly and enter the operative field at the level of the intertransverse ligament. They can be a source of significant, difficult-to-control bleeding if avulsed during lateral exposure.

The facet joint capsules have a shiny white appearance, and their individual fibers can be seen inserting onto the lateral edge of the laminar trough. Strict care should be taken to avoid violating the capsular fibers of adjacent segments unless that specific segment is being fused, as capsular incompetence leads to adjacent segment instability.
The ligamentum flavum exhibits a distinct yellow appearance due to its high elastin content, with fibers running in a cephalocaudal direction. The cephalad end of the ligament has a broad insertion from the base of the spinous process to between 50% and 70% of the anterior surface of the lamina. The caudal end of the ligament inserts from the superior edge of the lamina to between 2 and 6 mm of the anterior surface of the lamina.

Laterally, the intertransverse membrane overlies the iliopsoas and protects the ventral neural structures (ventral rami and exiting nerve roots) that lie beneath. Violation of this membrane during transverse process exposure risks injury to the exiting nerve root.
Indications and Contraindications
Selection of a posterior approach—whether a standard midline subperiosteal dissection or a paramedian muscle-sparing (Wiltse) approach—depends heavily on the specific pathology, the required trajectory, and the need to preserve the dorsal rami.
| Indication Category | Operative Indications for Posterior Approach | Non-Operative Management / Contraindications |
|---|---|---|
| Degenerative Pathology | Central canal stenosis, bilateral lateral recess stenosis, degenerative spondylolisthesis requiring decompression and fusion. | Mild stenosis without progressive neurologic deficit; isolated radiculopathy responsive to epidural steroid injections. |
| Trauma | Unstable burst fractures, flexion-distraction injuries, fracture-dislocations requiring posterior tension band restoration. | Stable compression fractures, neurologically intact patients with mechanically stable column injuries. |
| Deformity | Adult spinal deformity, adolescent idiopathic scoliosis requiring pedicle screw fixation and osteotomies (e.g., SPO, PSO). | Flexible, non-progressive deformities; severe anterior column deficiency requiring an anterior-only approach. |
| Infection / Tumor | Epidural abscess with neurological deficit, posterior column tumors, palliative decompression for metastatic disease. | High surgical risk patients (ASA IV/V); anterior predominant pathology better served by corpectomy. |
| Paramedian (Wiltse) Specific | Far lateral disc herniations, extraforaminal pathology, minimally invasive TLIF, placement of percutaneous pedicle screws. | Central canal stenosis requiring wide bilateral laminectomy; severe facet hypertrophy obscuring the lateral pars. |

Contraindications to the standard posterior midline approach are relatively few but include active superficial soft tissue infection over the surgical site or severe anterior column destruction where a posterior-only approach would fail to restore biomechanical stability.

Pre Operative Planning and Patient Positioning
Thorough preoperative planning requires careful evaluation of advanced imaging modalities. Magnetic Resonance Imaging (MRI) is essential for assessing the degree of central and foraminal stenosis, the health of the paraspinal musculature (evaluating for pre-existing multifidus atrophy), and the morphology of the ligamentum flavum. Computed Tomography (CT) is invaluable for evaluating bony anatomy, particularly facet tropism, pars interarticularis defects, and pedicle morphology for planned instrumentation.

Patient Positioning
Patient positioning is a critical phase of the procedure that directly impacts intraoperative hemodynamics and surgical exposure.
- Prone Positioning: The patient is placed prone on a specialized radiolucent spine table (e.g., Jackson table) or a Wilson frame.
- Abdominal Decompression: It is imperative that the abdomen hangs completely free. Any external compression on the abdomen increases intra-abdominal pressure, which is transmitted to the inferior vena cava. This venous engorgement retrogradely fills Batson's epidural venous plexus, leading to intractable intraoperative epidural bleeding.
- Pressure Points: All bony prominences (ulnar nerve at the cubital tunnel, peroneal nerve at the fibular head, patellae, and face) must be meticulously padded. The eyes must be checked to ensure no external pressure is applied, mitigating the risk of postoperative visual loss (ischemic optic neuropathy).
- Fluoroscopic Localization: Prior to incision, orthogonal fluoroscopy is utilized to confirm the surgical level. A spinal needle can be used to mark the exact trajectory, minimizing the required skin incision and subsequent subperiosteal dissection.

Detailed Surgical Approach and Technique
The Midline Subperiosteal Approach
The midline approach exploits the avascular, internervous plane between the bilateral erector spinae muscle groups.
- Incision and Fascial Dissection: A longitudinal incision is made over the spinous processes of the target levels. Dissection is carried down through the subcutaneous adipose tissue using electrocautery until the thick, pearly white lumbodorsal fascia is identified.
- Subperiosteal Dissection: The lumbodorsal fascia is incised precisely in the midline over the tips of the spinous processes. Using a Cobb elevator and electrocautery, the paraspinal muscles are elevated subperiosteally off the spinous processes and laminae. Maintaining a strict subperiosteal plane reduces bleeding and minimizes direct trauma to the muscle bellies.
- Lateral Exposure and the Dorsal Rami: Dissection proceeds laterally to the medial border of the facet joints. Crucial anatomical point: Excessive lateral retraction or aggressive electrocautery over the superior articular process (SAP) and transverse process junction will destroy the medial branch of the dorsal ramus. This denervates the multifidus, leading to postoperative atrophy and weakness. Retractors should be placed carefully, and tension should be released periodically during long cases to prevent ischemic injury to the musculature and nerves.
- L5-S1 Considerations: Particularly at the L5-S1 level, the interlaminar space may be significantly widened, or the posterior bony anatomy may be only partly formed (spina bifida occulta). Extreme care must be exercised when exposing this level, as inadvertent plunging into the spinal canal with a Cobb elevator or Bovie cautery can result in catastrophic dural tears or neural injury.

The Paramedian (Wiltse) Approach
For extraforaminal pathology or minimally invasive pedicle screw placement, the paramedian approach is preferred as it directly spares the medial branch of the dorsal ramus.
- Fascial Incision: The lumbodorsal fascia is incised 3 to 5 cm lateral to the midline.
- Internervous Plane: Blunt finger dissection is used to separate the multifidus muscle (medial, innervated by the medial branch of the dorsal ramus) from the longissimus muscle (lateral, innervated by the intermediate branch of the dorsal ramus).
- Exposure: This natural cleavage plane leads directly to the facet joint, pars interarticularis, and transverse process, providing excellent access for transforaminal lumbar interbody fusion (TLIF) or far-lateral disc herniation excision without stripping the midline tendinous attachments.

Decompression and Ligamentum Flavum Resection
Once exposure is achieved, decompression involves removal of the spinous process, lamina, and ligamentum flavum. The ligamentum flavum is detached from its broad insertion on the anterior surface of the cephalad lamina (50% to 70% coverage) and its narrow insertion on the caudal lamina. Kerrison rongeurs are used to meticulously resect the ligament, exposing the underlying dura and traversing nerve roots.


Complications and Management
Complications in posterior spinal surgery often stem from anatomical disorientation or failure to respect the neurovascular and ligamentous boundaries.
| Complication | Incidence | Etiology / Anatomical Basis | Management / Salvage Strategy |
|---|---|---|---|
| Paraspinal Muscle Atrophy | 15% - 30% | Iatrogenic injury to the medial branch of the dorsal ramus; prolonged retractor ischemia. | Prevention is key (intermittent retractor release, precise electrocautery). Postoperative focused core rehabilitation. |
| Incidental Durotomy | 3% - 10% | Plunging at L5-S1; ossified ligamentum flavum; revision surgery with epidural fibrosis. | Primary watertight repair with 4-0 or 5-0 non-absorbable suture. Augmentation with dural sealants or muscle/fat patch. Bedrest protocol if required. |
| Epidural Hematoma | 0.5% - 1.5% | Inadequate hemostasis of Batson's plexus or segmental vessels at the intertransverse membrane. | Emergent MRI and immediate surgical evacuation if causing progressive neurologic deficit. |
| Adjacent Segment Instability | Variable | Unintentional violation of the facet joint capsule at non-fused adjacent levels. | Strict identification of the facet capsule (shiny white fibers). Avoid electrocautery superior to the planned fusion level. |
| Wrong Level Surgery | < 1% | Failure to adequately localize due to anomalous anatomy (e.g., transitional vertebrae, lumbarized S1). | Mandatory intraoperative fluoroscopy with fixed anatomical landmarks (sacrum or T12 rib). |

Management of Segmental Bleeding
Bleeding from the segmental vessels near the intertransverse ligament can be brisk. If a segmental artery is avulsed, bipolar electrocautery or hemostatic agents (e.g., flowable gelatin matrix, bone wax if near the bony foramen) must be applied promptly. Blind monopolar cauterization in this region is strictly contraindicated due to the proximity of the exiting ventral ramus.


Post Operative Rehabilitation Protocols
Rehabilitation following posterior spinal approaches must account for the inevitable degree of paraspinal muscle trauma. The primary goal is to restore the dynamic stabilizing function of the multifidus and erector spinae muscles.
- Phase 1 (0-4 Weeks - Tissue Healing): Emphasis on early mobilization to prevent deep vein thrombosis and pulmonary complications. Activities are restricted to walking and light isometric core activation. Flexion, extension, and rotational loading are avoided to protect the dural repair and early fusion mass.
- Phase 2 (4-8 Weeks - Dynamic Stabilization): Introduction of active multifidus recruitment exercises. Because the multifidus may suffer partial denervation from dorsal ramus traction, targeted neuromuscular re-education (e.g., bird-dog exercises, pelvic tilts) is initiated.
- Phase 3 (8-12+ Weeks - Functional Restoration): Progressive resistance training focusing on global sagittal alignment and endurance of the deep spinal musculature. Return to occupational and recreational activities is tailored to the extent of the surgical fusion and patient tolerance.





















You Might Also Like