Luxatio Erecta (Inferior Glenohumeral Dislocation): Anatomy, Diagnosis & Management
Key Takeaway
Luxatio Erecta, or inferior glenohumeral dislocation, is a rare shoulder injury (0.5% of dislocations) where the arm is fixed in an "erect" position. It's characterized by forceful hyperabduction and a distinct levering mechanism, leading to extensive soft tissue and bony disruptions. This injury mandates meticulous diagnosis due to its high propensity for severe associated neurovascular injuries, particularly to the axillary nerve, brachial plexus, and axillary artery/vein.
Inferior Glenohumeral Dislocation: Symptoms, Diagnosis & Treatment
Inferior glenohumeral dislocation, also known as Luxatio Erecta, represents a distinct and challenging entity within shoulder traumatology. While exceptionally rare, its unique pathomechanics and high propensity for severe associated neurovascular and musculoskeletal injuries mandate a meticulous approach to diagnosis and management. This comprehensive review aims to serve as a high-yield reference for orthopedic surgeons, residents, and medical students grappling with this complex injury.
Introduction & Epidemiology
Inferior glenohumeral dislocation (Luxatio Erecta) is an infrequent injury, constituting approximately 0.5% of all shoulder dislocations. The term "luxatio erecta" descriptively refers to the characteristic clinical presentation where the patient's arm is fixed in an "erect" or "salute" position, typically abducted between 110 and 160 degrees and often in forward elevation.
The original seed content correctly highlights that this very rare injury is more common in elderly individuals. This demographic predisposition is multifactorial, often attributed to age-related changes such as increased capsular and ligamentous laxity, diminished bone quality contributing to associated fractures, and a higher incidence of falls. The mechanism of injury, as noted, is typically a forceful hyperabduction and external rotation of the arm, often combined with an axial load (e.g., falling onto an outstretched arm with the hand above the head, or a direct blow to the adducted elbow). This force causes the neck of the humerus to impinge upon the acromion, which then acts as a fulcrum, levering the humeral head out of the glenoid fossa in an inferior direction.
This distinct levering mechanism often results in extensive soft tissue and bony disruptions that significantly complicate management. The high incidence of associated injuries, including rotator cuff avulsions, pectoralis major injury, proximal humeral fractures, glenoid rim fractures, and critical neurovascular compromise, differentiates luxatio erecta from more common anterior or posterior shoulder dislocations and underscores the importance of a comprehensive diagnostic and treatment strategy.
Surgical Anatomy & Biomechanics
A precise understanding of the glenohumeral joint's stabilizers and the specific neurovascular structures at risk is paramount in managing luxatio erecta. The inherent instability of the glenohumeral joint, a ball-and-socket articulation designed for vast mobility, relies on a complex interplay of static and dynamic restraints.
Static Stabilizers
- Glenoid Labrum: A fibrocartilaginous rim that effectively deepens the shallow glenoid fossa, enhancing congruity and providing attachment for the glenohumeral ligaments and joint capsule. Inferior dislocation commonly causes avulsion of the inferior labrum (Bankart lesion) or, in severe cases, a bony avulsion (bony Bankart lesion) from the inferior glenoid rim.
-
Glenohumeral Ligaments (GHLs):
These are capsular thickenings that play primary roles in static stability.
- Superior Glenohumeral Ligament (SGHL): Contributes to superior and posterior stability.
- Middle Glenohumeral Ligament (MGHL): Important for anterior stability in mid-ranges of abduction.
- Inferior Glenohumeral Ligament (IGHL) Complex: The most critical static stabilizer against anterior and inferior translation, especially when the arm is abducted and externally rotated. It consists of a strong anterior band, a weaker posterior band, and an intervening axillary pouch. In luxatio erecta, the IGHL complex is almost invariably severely disrupted, either avulsed from its glenoid or humeral attachment or torn mid-substance, leading to profound inferior capsular failure.
- Joint Capsule: A thin, fibrous envelope enclosing the joint. Inferior dislocation necessitates extensive tearing of the inferior aspect of the capsule.
- Coracohumeral Ligament (CHL): Contributes to superior stability and prevents inferior subluxation when the arm is adducted.
Dynamic Stabilizers
- Rotator Cuff Muscles: The tendons of the supraspinatus, infraspinatus, teres minor, and subscapularis dynamically compress the humeral head into the glenoid, providing stability throughout the range of motion. Luxatio erecta frequently results in avulsion or tears of the rotator cuff, particularly the inferior capsule's attachment to the humerus or glenoid, and often the subscapularis or teres minor, contributing to functional deficits and potential irreducibility.
- Long Head of Biceps Tendon: Although primarily a humeral head depressor, its role in preventing inferior instability is secondary to the rotator cuff.
Neurovascular Structures at Risk
The high incidence of neurovascular injury is a defining feature and a critical concern with luxatio erecta.
*
Axillary Nerve:
This is the most frequently injured nerve, with reported incidences ranging from 30% to over 60%. It courses around the surgical neck of the humerus, exiting the quadrangular space, rendering it highly susceptible to stretch or direct compression from the inferiorly displaced humeral head or during reduction maneuvers. It innervates the deltoid and teres minor muscles and provides sensory supply to the lateral shoulder.
*
Brachial Plexus:
The entire brachial plexus (C5-T1) can be stretched or directly traumatized, leading to more diffuse neurological deficits involving multiple nerve distributions. The inferior trunks are particularly vulnerable due to their anatomical relationship to the humeral head in its inferiorly displaced position.
*
Axillary Artery and Vein:
These major vessels lie in close proximity, anterior and inferior to the glenohumeral joint. They are at significant risk of direct compression, stretch, intimal tears, thrombosis, pseudoaneurysm formation, or even complete rupture. While less common than nerve injuries, vascular compromise is limb-threatening and requires immediate attention.
Osseous Structures at Risk
-
Humeral Head/Neck:
- Proximal Humeral Fractures: Surgical neck fractures are frequently associated, complicating reduction and increasing the risk of avascular necrosis (AVN) of the humeral head. Greater tuberosity fractures can occur due to avulsion from rotator cuff pull or direct impact.
- Hill-Sachs Lesion: Although classically associated with anterior dislocations, engaging Hill-Sachs lesions can occur if there is an anterior-inferior component during injury or reduction.
-
Glenoid Rim:
- Bony Bankart Lesion: A fracture of the inferior glenoid rim, caused by the humeral head impacting the glenoid.
- Acromion: The acromion acts as the fulcrum for the levering mechanism, and in some cases, can sustain an impaction injury.
Biomechanics of Luxatio Erecta
The specific pathomechanics of luxatio erecta involves a forceful hyperabduction force, often with an element of external rotation. This drives the humeral neck into the acromion, which then serves as a rigid fulcrum. Continued force levers the humeral head inferiorly, causing it to tear through or avulse the inferior joint capsule and the critical IGHL complex from its glenoid or humeral attachments. The humeral head then comes to rest inferior to the glenoid, often subglenoidally or even intrathoracically, with the humeral shaft directed superiorly.
As observed in the original description, "The superior aspect of articular surface is directed inferiorly and is not in contact with the inferior glenoid rim. The humeral shaft is directed superiorly." This characteristic anatomical displacement places immense tension on the surrounding neurovascular structures and musculotendinous units, explaining the high incidence and severity of associated injuries.

Indications & Contraindications
Management of inferior glenohumeral dislocations necessitates a judicious assessment of the injury pattern, associated pathologies, and patient factors to determine the most appropriate course of action—non-operative closed reduction or operative intervention.
Non-Operative Management
Non-operative management primarily involves emergent closed reduction under adequate sedation or anesthesia, followed by a period of immobilization and a structured rehabilitation program.
Indications for Non-Operative Management:
*
Acute, Isolated Dislocation:
Ideal for cases presenting acutely (within hours to days) where initial assessment reveals no compelling indications for immediate surgical intervention.
*
Successful Closed Reduction:
The primary aim. If closed reduction can be safely and concentrically achieved, and the glenohumeral joint demonstrates satisfactory stability post-reduction without redislocation or significant residual subluxation.
*
Absence of Persistent Neurovascular Compromise:
Transient or minor neurological deficits that completely resolve immediately following reduction may allow for non-operative management of the dislocation itself, with continued close monitoring of nerve recovery. Vascular integrity must be confirmed before and after reduction.
*
Absence of Major Associated Fractures:
No significant, unstable proximal humeral fractures (e.g., highly displaced surgical neck fractures, articular involvement >25% of the head) or large, unstable glenoid rim fractures that would inherently compromise joint stability or require surgical fixation.
*
Patient Factors:
In patients with significant medical comorbidities precluding general anesthesia, non-ambulatory status, limited life expectancy, or very low functional demand, non-operative management may be chosen even for more complex injuries after successful closed reduction, prioritizing comfort and basic function.
Operative Management
Operative intervention is frequently required for luxatio erecta due to its complexity and high incidence of associated injuries.
Indications for Operative Management:
*
Irreducible Dislocation:
The most common indication. Closed reduction may fail due to:
*
Soft tissue interposition:
Incarceration of the labrum, biceps tendon, joint capsule, rotator cuff (especially subscapularis), or pectoralis major tendon within the glenoid fossa, mechanically blocking reduction.
*
Bony block:
A large, displaced humeral head fracture fragment or glenoid rim fracture preventing concentric reduction.
*
Chronic dislocation:
Dislocations present for several weeks or months (typically >3 weeks), where extensive scarring, fibrous tissue ingrowth, and capsular contracture render closed reduction futile and potentially dangerous.
*
Persistent or Severe Neurovascular Compromise:
If neurovascular deficits (particularly motor deficits or arterial compromise) do not resolve immediately after attempted or successful closed reduction, surgical exploration is mandatory to decompress, repair, or reconstruct damaged structures. This takes precedence over orthopedic repair.
*
Significant Associated Musculotendinous Injuries Requiring Repair:
*
Large, symptomatic rotator cuff tears:
Especially full-thickness tears that are retracted, avulsed, or causing significant functional impairment, requiring surgical repair (e.g., supraspinatus, subscapularis, teres minor avulsions).
*
Pectoralis major avulsions:
If displaced or causing significant functional deficit.
*
Extensive capsulolabral disruption:
Large Bankart lesions or inferior capsular avulsions that result in gross instability post-reduction, necessitating repair to prevent recurrent dislocation.
*
Unstable Associated Fractures:
*
Displaced proximal humeral fractures:
Surgical neck fractures, greater tuberosity fractures with significant displacement (>5mm or >45 degrees angulation), or head-splitting fractures that disrupt the articular surface and cannot be managed non-operatively.
*
Significant glenoid rim fractures (bony Bankart):
Especially if they involve a large percentage of the glenoid articular surface (>20-25%) or lead to persistent instability after reduction, requiring fixation to restore the glenoid arc.
*
Engaging Hill-Sachs lesions:
Though less common as a primary luxatio erecta indication, if present and causing engagement with the glenoid, may require augmentation (e.g., remplissage or latarjet).
*
Recurrent Dislocations:
While less common for primary luxatio erecta after appropriate initial management, recurrent instability following a luxatio erecta event would warrant surgical stabilization.
Contraindications
Absolute Contraindications:
*
Severe Medical Comorbidities:
Patients who are medically unstable, in extremis, or have acute conditions that absolutely preclude general anesthesia and surgical intervention (e.g., uncontrolled sepsis, recent myocardial infarction).
*
Active Infection:
Active infection within the proposed surgical field.
Relative Contraindications:
*
Unrealistic Patient Expectations:
Patients unwilling to commit to the rigorous and potentially prolonged rehabilitation required.
*
Extensive Tissue Loss/Damage:
Cases where the degree of damage to bone or soft tissue is so profound that anatomical reconstruction is not feasible or would predictably yield poor functional outcomes.
*
Patient Non-compliance:
Patients unlikely to adhere to critical post-operative restrictions and rehabilitation protocols.
Summary of Indications: Operative vs. Non-Operative
| Feature | Non-Operative Management | Operative Management |
|---|---|---|
| Primary Goal | Acute reduction, pain relief, early mobilization | Anatomical reduction, stabilization, repair of associated pathology |
| Dislocation Type | Acute, isolated, reducible via closed means | Irreducible (failed closed reduction), chronic, recurrent |
| Associated Injuries | Minor, stable; no significant neurovascular deficits that persist post-reduction | Irreducible due to soft tissue interposition, significant persistent neurovascular injury, large rotator cuff tears, unstable proximal humeral or glenoid fractures (e.g., displaced greater tuberosity, surgical neck, large bony Bankart), pectoralis major avulsion |
| Patient Factors | Elderly, high surgical risk, non-ambulatory, limited life expectancy, low functional demand | Active, young, good surgical candidate, compliant, high functional demand |
| Neurovascular Status | Intact, or transient/minor deficit fully resolving post-reduction | Persistent or severe neurovascular deficit post-reduction, requiring exploration/repair |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is non-negotiable for luxatio erecta given its rarity, complexity, and high association with critical injuries. This planning encompasses comprehensive diagnostic imaging, meticulous neurovascular assessment, and careful consideration of anesthesia and patient positioning.
Pre-Operative Imaging
-
Radiographic Evaluation: "Trauma series of the affected shoulder: AP, scapular-Y, and axillary views are taken."
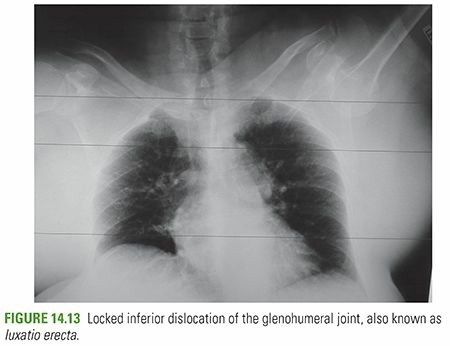
- Anteroposterior (AP) View: "The AP radiograph is typically diagnostic, with inferior dislocation of the humeral head and superior direction of the humeral shaft along the glenoid margin." This view confirms the inferior displacement and the characteristic "salute" or "erect" position.
- Scapular Y View: This view is crucial for confirming the humeral head's inferior relationship to the glenoid, located below the intersection of the coracoid, acromion, and scapular body. It helps differentiate inferior from anterior or posterior dislocations.
- Axillary View: Often challenging to obtain in the acutely painful, abducted position. However, it is essential for confirming the anteroposterior relationship of the humeral head to the glenoid, assessing glenoid rim fractures, and detecting Hill-Sachs lesions. If a true axillary view is not feasible, modified views (e.g., West Point axillary, Velpeau axillary) should be attempted.
- Transthoracic Lateral View: Can provide supplementary information regarding the humeral head's position.
-
Computed Tomography (CT) Scan:
- Indications: Strongly recommended, especially if closed reduction fails or if associated bony injuries are suspected or unclear on plain radiographs.
- Benefits: Provides detailed three-dimensional bony anatomy, accurately identifies and characterizes proximal humeral fractures (surgical neck, greater tuberosity, articular involvement), glenoid rim fractures (bony Bankart), and impaction fractures. It is invaluable for identifying bony interposition (e.g., displaced fracture fragments) that might impede reduction. Three-dimensional (3D) reconstructions are highly beneficial for surgical planning.
- Vascular Assessment: CT angiography (CTA) should be considered if there is any clinical suspicion of arterial injury (e.g., diminished pulses, expanding hematoma), providing rapid and detailed assessment of vessel integrity.
-
Magnetic Resonance Imaging (MRI):
- Indications: While less urgent for immediate diagnosis of dislocation, MRI is crucial for evaluating associated soft tissue injuries once the dislocation is reduced or if operative repair of soft tissues is contemplated.
- Benefits: Excellent for assessing rotator cuff tears (which are common), labral injuries (Bankart lesions, ALPSA lesions), capsular integrity, and the extent of brachial plexus involvement (differentiating stretch from avulsion).
-
Angiography/Doppler Ultrasound:
- Indications: If clinical signs of vascular injury are present (e.g., absent or diminished peripheral pulses, pallor, cold extremity, expanding hematoma, bruits, thrills).
- Benefits: Confirms vascular injury, defines its type (intimal tear, thrombosis, pseudoaneurysm, transection), and guides urgent vascular surgical intervention. Doppler ultrasound can be used as a rapid screening tool. Ankle-Brachial Index (ABI) should be performed if suspicion is high.
Neurovascular Assessment
"A careful neurovascular examination is essential, because neurovascular compromise almost always complicates these dislocations." This statement underscores the paramount importance of thorough assessment. A meticulous neurovascular examination must be performed and documented pre-reduction, immediately post-reduction (if closed reduction is attempted), and certainly pre-operatively if surgery is planned.
*
Neurological Examination:
*
Motor:
Assess specific muscle groups for strength (using MMT 0-5 scale): deltoid (axillary nerve, C5-C6), biceps (musculocutaneous nerve, C5-C6), wrist extensors (radial nerve, C6-C8), wrist flexors (median/ulnar nerve, C7-T1), and intrinsic hand muscles (ulnar/median nerve, C8-T1).
*
Sensory:
Test sensation in the axillary nerve distribution (lateral shoulder "regimental badge" area), musculocutaneous nerve (lateral forearm), median nerve (radial palm, first three digits), ulnar nerve (ulnar palm, fifth digit), and radial nerve (dorsum of hand).
*
Documentation:
Record all findings precisely, as this forms the baseline for monitoring recovery and guiding further management.
*
Vascular Examination:
*
Pulses:
Palpate and grade radial, ulnar, and brachial pulses.
*
Capillary Refill:
Assess capillary refill time in the fingertips.
*
Skin Assessment:
Observe skin temperature, color, and turgor of the entire upper extremity for signs of ischemia.
*
Doppler Assessment:
Use a handheld Doppler to confirm the presence and quality of pulses, especially if palpation is difficult. Compare with the contralateral limb.
Anesthesia Considerations
- General Anesthesia: Typically required for both closed and open reduction due to the severe pain, profound muscle spasm, and the need for complete muscle relaxation.
- Regional Anesthesia: An interscalene brachial plexus block can be a valuable adjunct. It provides excellent pre-operative pain control, reduces intra-operative anesthetic requirements, and facilitates muscle relaxation, thereby aiding in reduction. It also offers excellent post-operative analgesia. However, it is crucial to perform and document a complete neurological examination before administering a regional block, as it can mask existing neurological deficits.
Patient Positioning
Proper patient positioning is critical for optimizing surgical exposure, facilitating reduction maneuvers, and ensuring adequate access for intra-operative fluoroscopy.
-
Beach Chair Position (Most Common):
- Setup: Patient is placed in a semi-recumbent position, typically at a 60-70 degree incline, with the head supported and secured. The operative arm is draped freely to allow unrestricted manipulation.
- Advantages: Provides excellent visualization for the standard deltopectoral approach. Allows for full range of motion of the arm for reduction maneuvers, stability assessment, and identification of associated injuries. Facilitates arthroscopic evaluation if desired.
- Considerations: Careful head positioning is required to prevent cervical hyperextension or brachial plexus stretch. Blood pressure monitoring is crucial due to potential for orthostatic hypotension with head elevation.
-
Lateral Decubitus Position:
- Setup: Patient lies on the unaffected side, secured with a beanbag or bolsters. The operative arm can be suspended in traction from an overhead system, which may assist with reduction.
- Advantages: Can be advantageous for specific posterior or lateral approaches or if severe associated humeral shaft fractures dictate this position.
- Considerations: May make anterior exposure and manipulation more challenging. Potential for pressure sores on the dependent arm and side.
-
Fluoroscopy:
- A C-arm fluoroscopy unit must be readily available and draped sterilely for intra-operative use in either position. It is essential for confirming reduction, assessing fracture alignment and fixation, and guiding hardware placement. The C-arm should be positioned to allow AP and true lateral (scapular Y or axillary equivalent) views without repositioning the patient.
Sterile preparation and draping should encompass the entire shoulder girdle and allow for unrestricted manipulation of the entire upper extremity, from the hand to the axilla. This permits sterile traction and appropriate positioning of the arm during the reduction process and subsequent repair.
Detailed Surgical Approach / Technique
The primary objective in the management of luxatio erecta is prompt, anatomical reduction of the glenohumeral joint, followed by diligent assessment and repair of associated injuries. While closed reduction is always the initial attempt, the high incidence of irreducibility or critical concomitant pathologies often necessitates an open surgical approach.
General Principles for Reduction and Repair
- Adequate Anesthesia and Muscle Relaxation: Deep general anesthesia with profound muscle relaxation is fundamental to overcome muscle spasm and facilitate reduction, whether closed or open. An interscalene block can further augment this.
- Meticulous Neurovascular Protection: Constant vigilance is paramount. During every step of dissection and manipulation, the axillary nerve, brachial plexus, and axillary vessels must be identified, protected, and carefully retracted.
- Systematic Approach: First, achieve reduction. Second, thoroughly assess the stability of the reduction and the integrity of the surrounding structures. Third, systematically identify and address all associated injuries requiring repair or fixation.
Closed Reduction Techniques
Closed reduction should be attempted initially under complete general anesthesia and muscle relaxation. However, it is often challenging and carries a higher risk of iatrogenic injury (fractures, neurovascular damage) in luxatio erecta compared to other shoulder dislocations due to the extreme displacement and high forces involved.
The fundamental principle for reducing luxatio erecta is
traction-countertraction
in the line of deformity, followed by specific maneuvers to disengage and relocate the humeral head.
1.
Preparation:
The patient is supine or semi-recumbent, under full general anesthesia and muscle relaxation. A strong assistant provides continuous countertraction to the patient's thorax.
2.
Traction:
The primary surgeon applies strong, sustained longitudinal traction to the arm, precisely in line with the humeral shaft (i.e., in the fixed abducted and elevated position). The goal is to disimpact the humeral head from its inferiorly displaced position.
3.
Leverage and Rotation (Two-Stage Reduction Concept):
* As sustained traction is applied, the surgeon may attempt gentle external rotation to help disengage the humeral head.
* A common strategy involves a "two-stage" reduction:
*
Stage 1: Convert to Anterior Dislocation:
While maintaining traction, apply a gentle adduction force, aiming to bring the humeral head from its inferior position to an anterior-inferior position relative to the glenoid, effectively converting it into an anterior dislocation. This requires pulling the humeral head distal to the glenoid rim.
*
Stage 2: Reduce Anterior Dislocation:
Once converted to an anterior dislocation, standard anterior reduction maneuvers (e.g., Kocher's maneuver applied carefully, Stimson's technique) can be employed, bringing the arm into adduction and internal rotation.
4.
Caution:
Excessive force, particularly during adduction or internal rotation, can lead to iatrogenic fractures (e.g., humeral neck, glenoid rim) or further neurovascular injury. If significant resistance is encountered after a few careful attempts, repeated forceful maneuvers should be strictly avoided. Immediate consideration should then shift to open reduction.
5.
Post-Reduction Assessment:
Following reduction, immediately re-assess the neurovascular status of the limb. Confirm concentric reduction with intra-operative fluoroscopy or post-reduction radiographs. Gently assess glenohumeral stability through a controlled range of motion.
Open Reduction and Internal Fixation (ORIF)
If closed reduction fails, if there is persistent or severe neurovascular compromise, if significant associated fractures require fixation, or if clear evidence of soft tissue interposition is present, an open surgical approach is indicated without delay.
Surgical Approach: Deltopectoral Approach
The Deltopectoral Approach is the standard and most versatile approach for open reduction of luxatio erecta, providing excellent exposure of the anterior and inferior aspects of the glenohumeral joint and allowing for repair of most associated injuries.
- Incision: A curvilinear incision is made, typically originating from the coracoid process and extending distally along the deltopectoral groove for 8-10 cm.
-
Deltopectoral Interval:
- Identify the cephalic vein, which courses within this interval. It is typically retracted medially with the pectoralis major muscle.
- Develop the interval by retracting the deltoid muscle laterally and the pectoralis major muscle medially. This exposes the underlying clavipectoral fascia.
- Subcoracoid Space Exposure: Deep to the clavipectoral fascia, the conjoined tendon (coracobrachialis and short head of biceps) and the subscapularis muscle are exposed. The coracoid process serves as a key anatomical landmark.
-
Neurovascular Protection:
- Axillary Nerve and Posterior Circumflex Humeral Artery: These structures exit the quadrangular space, posterior and inferior to the surgical neck of the humerus. While not directly in the standard deltopectoral approach, they are at extreme risk due to the inferior displacement of the humeral head and the need for manipulation. Careful identification and protection are paramount. Palpate the axillary nerve as it courses laterally around the surgical neck.
- Axillary Artery and Vein: These major vessels lie medial and inferior to the humeral head. Great care must be taken during retraction, particularly with inferior or medial retractors, to avoid direct injury or compression.
-
Addressing the Humeral Head:
- The humeral head will be identified inferiorly, often deep in the axilla or against the chest wall.
- The inferior joint capsule will inevitably be severely torn or avulsed. The subscapularis tendon may also be torn, avulsed from the lesser tuberosity, or interposed.
- Carefully clear any incarcerated soft tissues (e.g., labrum, torn capsule, biceps tendon, subscapularis tendon, pectoralis major) from the glenoid fossa. This tissue interposition is a common cause of irreducibility.
-
Open Reduction Maneuver:
- Under direct visualization, apply gentle, sustained longitudinal traction to the humerus.
- Utilize a blunt instrument (e.g., a periosteal elevator, broad Hohmann retractor, or bone hook) to carefully lever the humeral head superiorly and laterally, guiding it back towards the glenoid fossa. Simultaneous gentle abduction and external rotation of the arm may aid in disengagement and relocation.
- Avoid excessive force or prying against the glenoid rim to prevent iatrogenic fractures.
- Once the humeral head is approximated to the glenoid, gently internally rotate and adduct the arm to achieve concentric reduction.
-
Assessment of Reduction and Stability:
- Visually confirm concentric reduction.
- Perform intra-operative fluoroscopy to verify reduction and rule out any new fractures.
- Carefully assess glenohumeral stability through a full, controlled range of motion. Identify any positions of apprehension or redislocation.
- Re-assess neurovascular status immediately after reduction.
Addressing Associated Injuries
After successful reduction and confirmation of stability, a systematic evaluation and repair of associated injuries is critical for long-term functional outcome.
-
Rotator Cuff Tears:
- Diagnosis: Inspect all accessible rotator cuff tendons (subscapularis, supraspinatus, infraspinatus/teres minor). Given the mechanism, inferior capsular avulsions and subscapularis tears are highly prevalent.
- Repair: If a significant, repairable full-thickness rotator cuff tear is identified, it should be addressed. Suture anchors are typically used to reattach torn tendons to their respective humeral insertion sites (e.g., lesser tuberosity for subscapularis, greater tuberosity for supraspinatus/infraspinatus) or to the glenoid rim.
-
Capsulolabral Repair (Bankart Lesion):
- Diagnosis: Thoroughly inspect the glenoid rim and labrum for tears or avulsions. Inferior glenoid rim fractures (bony Bankart) and labral tears are common.
- Repair: Reattach the torn labrum and capsule to the glenoid using suture anchors. If a significant bony Bankart fragment is present and displaced, it may require screw fixation or reattachment with suture anchors to restore the glenoid's articular arc and stability.
-
Proximal Humeral Fractures:
- Diagnosis: Carefully inspect the humeral head and neck for fractures (surgical neck, greater tuberosity, articular involvement). These should have been identified on pre-operative CT.
-
Fixation:
- Greater Tuberosity Fractures: If displaced (>5mm or >45 degrees angulation), these are typically fixed with suture anchors or small cannulated screws.
- Surgical Neck Fractures: If stable after reduction, conservative management may be an option. However, displaced or unstable fractures often require open reduction and internal fixation with plates and screws (e.g., PHILOS plate) or intramedullary nailing, depending on the fracture pattern, bone quality, and surgeon preference.
-
Vascular Injuries:
- If a vascular injury (e.g., axillary artery intimal tear, pseudoaneurysm, or transection) is diagnosed pre-operatively or discovered intra-operatively, immediate vascular surgery consultation is mandatory. Repair (e.g., arterial bypass grafting with interposition vein graft, primary repair, thrombectomy) should be performed before or concurrently with orthopedic stabilization, depending on the urgency.
-
Neurological Deficits:
- If severe or persistent neurological deficits are present post-reduction despite the absence of obvious mechanical compression, and especially if an intra-operative nerve injury is suspected, consultation with a peripheral nerve surgeon for potential neurolysis or nerve repair/grafting may be warranted. Most stretch injuries are observed initially.
Closure
- Copious irrigation of the surgical site.
- Repair of the subscapularis and/or capsule if applicable, ensuring meticulous anatomical restoration.
- Close the deltopectoral interval.
- Standard layered closure of subcutaneous tissues and skin.
- Apply a sterile dressing and place the arm in an appropriate immobilizer (e.g., sling and swathe, or abduction pillow brace, depending on the specific repairs performed and post-reduction stability).
Alternative/Supplementary Approaches
- Deltoid Split Approach: Offers limited exposure for inferior dislocations but may be considered for isolated superior or lateral pathology (e.g., isolated greater tuberosity fracture).
- Posterior Approach: Rarely indicated for primary luxatio erecta reduction but might be necessary for chronic dislocations with severe posterior contracture or specific posterior glenoid pathology.
Complications & Management
Luxatio erecta is associated with a markedly high incidence of complications, reflecting the severity of the initial trauma and the extensive tissue disruption. Understanding these potential complications and having a clear management strategy is paramount for improving patient outcomes.
| Complication | Incidence (Approx.) | Salvage / Management Strategy
| |
|
Primary Goal
| Acute reduction, pain relief, early mobilization | Anatomical reduction, stabilization, repair of associated pathology |
|
Dislocation Type
| Acute, isolated, reducible via closed means | Irreducible (failed closed reduction), chronic, recurrent |
|
Associated Injuries
| Minor, stable; no significant neurovascular deficits that persist post-reduction | Irreducible due to soft tissue interposition, significant persistent neurovascular injury, large rotator cuff tears, unstable proximal humeral or glenoid fractures (e.g., displaced greater tuberosity, surgical neck, large bony Bankart), pectoralis major avulsion |
|
Patient Factors
| Elderly, high surgical risk, non-ambulatory, limited life expectancy, low functional demand | Active, young, good surgical candidate, compliant, high functional demand |
|
Neurovascular Status
| Intact, or transient/minor deficit fully resolving post-reduction | Persistent or severe neurovascular deficit post-reduction, requiring exploration/repair |
Detailed Management Strategies
1. Neurovascular Injury
-
Axillary Nerve Palsy:
The most common neurological deficit, manifesting as deltoid weakness (difficulty initiating abduction beyond 30 degrees) and sensory loss over the lateral shoulder ("regimental badge" area). The majority of axillary nerve stretch injuries recover spontaneously within 6-12 months.
- Management: Initial observation with serial clinical examinations. Electrodiagnostic studies (EMG/NCS) are typically performed at 3-6 months post-injury to assess nerve integrity, quantify recovery, and localize the lesion. If there is no discernible sign of recovery by 6-9 months, or if a complete transection is suspected based on intra-operative findings or prior imaging, surgical exploration (neurolysis, nerve grafting, or nerve transfer) may be considered in consultation with a peripheral nerve specialist.
-
Brachial Plexus Injury:
Can range from neurapraxia (stretch) to axonotmesis or neurotmesis (partial or complete tears). Presentation is often more diffuse than isolated axillary nerve palsy.
- Management: Similar to axillary nerve palsy, initial observation is common. EMG/NCS at 3-6 months helps to localize the lesion and assess the extent of axonal integrity. Surgical intervention (exploration, neurolysis, grafting) is reserved for severe injuries without signs of recovery.
-
Axillary Artery/Vein Injury:
A rare but limb-threatening emergency. Clinical signs include absent or diminished pulses, pallor, coldness of the extremity, an expanding hematoma, or distal ischemia.
- Management: Immediate vascular surgery consultation is critical. Diagnostic angiography or CTA is performed. Prompt surgical exploration and repair (primary repair, interposition vein grafting, thrombectomy, or ligation in dire circumstances) are paramount to prevent irreversible ischemia and limb loss. This may precede orthopedic repair.
2. Rotator Cuff Tears
- Incidence: High, particularly avulsions of the inferior capsule and often the subscapularis or teres minor.
- Management: Symptomatic, full-thickness tears identified pre-operatively (MRI) or intra-operatively should be repaired surgically, typically with suture anchors. Repairing significant tears contributes to shoulder stability, restoration of muscle balance, and improved functional outcomes. Small, partial-thickness tears may initially be managed non-operatively with physical therapy, with surgical repair reserved for refractory symptoms.
3. Fractures
-
Proximal Humeral Fractures:
These are common and can involve the surgical neck, greater tuberosity, or articular surface.
- Management: Non-displaced or minimally displaced fractures may be treated non-operatively with sling immobilization and early, protected range of motion, once the dislocation is reduced. Displaced or unstable fractures (e.g., surgical neck fractures, greater tuberosity fractures with >5mm displacement or >45 degrees angulation) require open reduction and internal fixation (ORIF) with plates, screws, or K-wires. In elderly patients with complex 3- or 4-part fractures that severely compromise the articular surface or blood supply, primary hemiarthroplasty or reverse shoulder arthroplasty may be considered.
-
Glenoid Rim Fractures (Bony Bankart):
Avulsion of the inferior glenoid rim.
- Management: Small, stable fragments (<20% of the glenoid width) may be managed non-operatively. Larger fragments (>20-25% of the glenoid width) or those demonstrably causing persistent instability after reduction require surgical fixation (suture anchors, small screws) to restore the glenoid's articular arc and stability.
4. Irreducibility / Failed Reduction
- Management: If closed reduction is unsuccessful despite adequate anesthesia and muscle relaxation, prompt open reduction via a deltopectoral approach is indicated. The surgeon must identify and carefully remove any incarcerated soft tissues (labrum, biceps, subscapularis, capsule) or bony fragments blocking reduction.
5. Recurrent Instability
- Less common after luxatio erecta compared to anterior dislocations if initial reduction is concentric and associated major instability-causing lesions (e.g., large labral tears, bony Bankart) are adequately repaired.
- Management: If symptomatic recurrent instability occurs, a thorough diagnostic work-up (MRI, CT) is necessary to identify the underlying pathology (e.g., un-repaired labral tear, glenoid bone loss, capsular laxity). Surgical stabilization, tailored to the specific pathology (e.g., capsulolabral repair, bone block procedure for glenoid bone loss), would then be considered.
6. Stiffness / Adhesive Capsulitis
- Incidence: High due to the significant soft tissue trauma and the necessary period of post-reduction immobilization.
- Management: Prevention is key, achieved through carefully titrated and progressive post-operative rehabilitation protocols. For established stiffness, aggressive physical therapy focusing on stretching and mobilization, non-steroidal anti-inflammatory drugs (NSAIDs), and judicious use of corticosteroid injections may be employed. For refractory cases, manipulation under anesthesia (MUA) or arthroscopic capsular release may be necessary.
7. Avascular Necrosis (AVN) of the Humeral Head
- Incidence: Higher in cases with associated proximal humeral fractures or prolonged dislocation time due to disruption of the humeral head's tenuous blood supply.
- Management: Initial stages may be observed, sometimes with core decompression. For progressive collapse of the humeral head and intractable pain, definitive treatments include hemiarthroplasty or total shoulder arthroplasty.
8. Infection
- Management: Standard surgical site infection protocols: culture-directed intravenous antibiotics, surgical debridement and irrigation, and potential hardware removal if a deep infection is present.
9. Chronic Pain and Weakness
- Management: A multimodal approach is typically required, including targeted physical therapy to improve strength and range of motion, comprehensive pain management strategies, and addressing any residual anatomical deficits (e.g., incomplete nerve recovery, un-repaired rotator cuff pathology). Psychological support may also be beneficial.
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation following the management of luxatio erecta is a critical determinant of functional outcome, balancing the imperative to protect surgical repairs with the need to restore motion and strength. Protocols must be highly individualized based on the stability achieved, the extent of associated soft tissue and bony repairs, patient factors (age, bone quality, compliance), and the specific surgeon's preference.
General Principles
- Controlled Progression: Rehabilitation advances through defined phases, with increasing demands placed on the shoulder only after adequate tissue healing and stability are confirmed.
- Immobilization: Initial immobilization is essential to protect repairs, but prolonged immobilization should be avoided to minimize joint stiffness.
- Pain Management: Effective pain control is crucial to enable patient participation in therapy.
- Patient Education: Comprehensive patient education regarding precautions, exercises, and the expected recovery timeline is vital for compliance.
- Interdisciplinary Communication: Close collaboration between the orthopedic surgeon, physical therapist, and patient is paramount for successful outcomes.
Phase I: Protection (Weeks 0-6, or longer depending on the extent of repair)
Goals:
* Protect all surgical repairs and maintain glenohumeral reduction.
* Minimize pain, inflammation, and edema.
* Prevent stiffness in the elbow, wrist, and hand.
* Initiate passive range of motion (PROM) for the shoulder within clearly defined, safe limits.
Management:
1.
Immobilization:
The arm is typically immobilized in a sling and swathe for 4-6 weeks, or an abduction pillow brace, particularly if extensive capsular or rotator cuff repair has been performed. The specific position (e.g., slight internal or neutral rotation) may vary depending on the exact structures repaired (e.g., neutral rotation for subscapularis repair).
2.
Pain and Edema Control:
Consistent application of cryotherapy, judicious use of non-steroidal anti-inflammatory drugs (NSAIDs), and appropriate oral analgesics.
3.
Shoulder PROM (Pendulum Exercises):
Gentle pendulum exercises (Codman's exercises) are typically initiated within the first week, performed several times daily. These are gravity-assisted, non-resistive movements aimed at lubricating the joint and preventing capsular adhesions.
4.
Strict Precautions:
Absolutely no active shoulder motion. No lifting, pushing, or pulling with the affected arm. Avoid specific positions that place stress on the repairs (e.g., excessive abduction and external rotation if the inferior glenohumeral ligament or subscapularis was repaired).
5.
Adjacent Joint Mobility:
Active range of motion (AROM) exercises for the elbow, wrist, and hand are encouraged to begin immediately to prevent stiffness in these joints.
6.
Scapular Mobility:
Gentle scapular retraction and protraction exercises can be started to maintain periscapular muscle tone and mobility.
Phase II: Early Motion & Gentle Strengthening (Weeks 6-12)
Goals:
* Gradually restore full pain-free passive range of motion.
* Initiate active range of motion (AROM).
* Begin gentle isometric strengthening of the shoulder musculature.
* Improve neuromuscular control and stability.
Management:
1.
Discontinuation of Immobilization:
The sling is typically discontinued around week 6, though it may be used for comfort or during sleep.
2.
Passive and Assisted Range of Motion (PROM/AAROM):
Progress from PROM to therapist-assisted and self-assisted ROM exercises (e.g., pulley exercises, wand exercises, sustained stretching) to restore full flexion, abduction, and rotational movements.
*
Caution:
Continue to strictly avoid positions that excessively stress the healing repair, particularly extreme external rotation with abduction until at least 10-12 weeks for capsular or anterior labral repairs.
3.
Active Range of Motion (AROM):
Once sufficient PROM is achieved and approved by the surgeon, gentle active shoulder exercises can commence, typically starting with flexion and abduction in the scapular plane (scaption). Initially, gravity-eliminated exercises are preferred.
4.
Isometric Strengthening:
Gentle isometric exercises for the rotator cuff (internal rotation, external rotation) and deltoid can be initiated, performed with the arm in a neutral or protected position. No resistance against movement.
5.
Scapular Stabilization:
Continued emphasis on scapular strengthening exercises to establish a stable base for humeral motion.
Phase III: Progressive Strengthening (Weeks 12-24)
Goals:
* Achieve full pain-free active range of motion.
* Progressive strengthening of the rotator cuff, deltoid, and periscapular musculature.
* Improve muscular endurance and functional use of the arm.
Management:
1.
Dynamic Strengthening:
Introduce light resistance exercises using elastic bands, light weights, or therapeutic putty for the rotator cuff and deltoid.
* Progress from isolated movements to compound movements, incorporating diagonal patterns.
* Emphasize eccentric control in exercises.
2.
Proprioception and Neuromuscular Control:
Incorporate exercises using balance boards for the hand, plyometric balls, or rhythmic stabilization drills to enhance joint position sense and motor control.
3.
Functional Activities:
Gradually reintroduce functional activities related to daily living, work, and light recreational pursuits.
4.
Aerobic Conditioning:
Encourage maintenance of overall cardiovascular fitness.
Phase IV: Return to Activity / Sport-Specific Training (Weeks 24+)
Goals:
* Maximize strength, power, and endurance.
* Refine neuromuscular control and sport-specific movement patterns.
* Facilitate safe return to unrestricted activities, including competitive sports, if appropriate.
Management:
1.
Advanced Strengthening:
Continue progressive resistance exercises, incorporating overhead activities, plyometrics, and more sport-specific movements if indicated.
2.
Sport-Specific Drills:
For athletes, implement a structured, gradual return-to-sport program, including throwing mechanics, overhead activities, and contact drills, meticulously tailored to their particular sport.
3.
Maintenance Program:
Establish a long-term home exercise program to maintain strength, flexibility, and stability.
4.
Return to Activity:
Full return to high-demand activities or contact sports requires comprehensive clinical assessment, objective functional testing (e.g., Functional Movement Screen, Y-Balance Test, isokinetic testing), and explicit surgeon clearance. This typically occurs no earlier than 6 months post-surgery, and often longer for overhead athletes or following complex reconstructions.
Important Considerations:
*
Neurovascular Recovery:
For patients with pre-existing neurovascular deficits, rehabilitation protocols must be carefully adjusted. Nerve recovery can be prolonged, and specific therapies (e.g., neuromuscular electrical stimulation) may be integrated.
*
Associated Fractures:
If fractures were treated operatively, radiographic confirmation of bone healing is required before progressing to resistive exercises that could compromise fixation.
*
Patient Compliance:
Reinforce the critical importance of adherence to the prescribed protocol and strict avoidance of unguided progression, which could jeopardize surgical outcomes.
*
Monitoring for Complications:
Continuously monitor for any signs of developing stiffness, recurrent instability, persistent pain, or signs of nerve/vascular compromise that may necessitate adjustments to the rehabilitation program or further medical/surgical intervention.
Summary of Key Literature / Guidelines
Inferior glenohumeral dislocation (luxatio erecta) stands as a challenging injury, distinguished by its rarity, characteristic clinical presentation, and a high incidence of severe associated injuries. The existing academic literature, while not as voluminous as for more common shoulder pathologies, consistently provides key insights into its diagnosis, management, and potential outcomes.
-
Epidemiology and Mechanism:
- Literature consistently reports luxatio erecta as accounting for approximately 0.5% of all glenohumeral dislocations (Kummel, 1875; Thomason et al., 1998, Journal of Orthopaedic Trauma ).
- The mechanism is well-established: a forceful hyperabduction often with axial loading, causing the humeral neck to abut the acromion, which then acts as a fulcrum to lever the humeral head inferiorly (Freund, 1859; Garcia et al., 2012, Journal of Shoulder and Elbow Surgery ). This unique "levering effect" is crucial for understanding the widespread damage.
- A higher incidence in the elderly is widely recognized, likely due to diminished capsular and ligamentous elasticity and poorer bone quality (Levy et al., 2000, Journal of Orthopaedic Trauma ).
-
Clinical Presentation and Diagnosis:
- The "salute" position—arm locked in 110-160 degrees of abduction and often external rotation—is considered pathognomonic (Pippin and DeCarlo, 1999, Sports Medicine and Arthroscopy Review ).
- Radiographic Series: The affected shoulder's trauma series (AP, scapular-Y, and axillary views) is fundamental for diagnosis. The AP view is typically diagnostic, confirming the humeral head's inferior displacement with the humeral shaft directed superiorly. However, obtaining a diagnostic axillary view can be challenging due to patient pain and fixed abduction (Rockwood et al., 2019, Rockwood and Green's Fractures in Adults , 9th ed.).
- Advanced Imaging: CT scans are highly recommended pre-operatively, especially if closed reduction fails, to accurately define associated bony injuries (proximal humeral fractures, glenoid rim fractures) and to identify potential soft tissue interposition preventing reduction (Ogden, 2018, Skeletal Trauma , 5th ed.). MRI provides superior delineation of soft tissue injuries, such as rotator cuff tears, labral avulsions, and potential brachial plexus involvement. CT angiography (CTA) is crucial if vascular injury is suspected.
-
Associated Injuries:
- A hallmark of luxatio erecta is the exceedingly high incidence of concomitant injuries, reported in 60-80% of cases (Levy et al., 2000; Paschal et al., 2014, Hand Clinic ).
- Neurovascular Injuries: The axillary nerve is the most frequently injured structure, with reported palsy rates ranging from 30% to over 60% (Paschal et al., 2014; Rockwood et al., 2019). Brachial plexus and axillary artery injuries, though less common (<5% for arterial injury), are critical and require immediate attention, as vascular compromise is limb-threatening (D’Alessandro et al., 1999, Journal of Trauma ).
- Musculotendinous Injuries: Rotator cuff tears (especially subscapularis and inferior capsular avulsions) and pectoralis major tears are frequent due to the severe hyperabduction mechanism (Mallon et al., 1990, Clinical Orthopaedics and Related Research ).
- Bony Injuries: Proximal humeral fractures (surgical neck, greater tuberosity) and glenoid rim fractures (bony Bankart) are common and contribute significantly to irreducibility and post-reduction instability (Thomason et al., 1998).
-
Management Strategies:
- Closed Reduction: Always the initial treatment attempt under adequate general anesthesia and muscle relaxation. Techniques often involve sustained traction in line with the humeral shaft, followed by cautious levering and adduction to convert the inferior dislocation into an anterior one, then a standard anterior reduction maneuver (Freedman and Southwick, 1989, Journal of Bone and Joint Surgery Am ). However, forceful or repeated attempts must be avoided due to the high risk of iatrogenic fractures or neurovascular damage (Paschal et al., 2014).
- Open Reduction: Indicated for failed closed reduction, persistent neurovascular compromise after reduction, or significant associated fractures requiring fixation. The deltopectoral approach is the standard, providing excellent access for reduction, debridement of interposed soft tissues, and repair of associated injuries (e.g., rotator cuff, labrum, fractures) (Rockwood et al., 2019; Ogden, 2018).
- Vascular Injury Management: Immediate vascular surgery consultation is critical. Repair should be prioritized, often preceding or occurring concurrently with orthopedic stabilization (D’Alessandro et al., 1999).
- Nerve Injury Management: Most axillary nerve stretch injuries recover spontaneously. Electrodiagnostic studies (EMG/NCS) at 3-6 months guide prognosis. Surgical exploration and nerve repair/grafting are reserved for severe, non-recovering deficits (Levy et al., 2000).
-
Outcomes and Complications:
- Despite successful reduction, functional outcomes can be variable due to the severity and combination of associated injuries.
- Stiffness/Adhesive Capsulitis: A common sequela, necessitating a structured and progressive post-operative rehabilitation program (Thomason et al., 1998).
- Avascular Necrosis (AVN) of the humeral head: A recognized risk, particularly with prolonged dislocation or associated proximal humeral fractures, due to disruption of the humeral head's blood supply (Levy et al., 2000).
- Recurrent Instability: Less common after luxatio erecta compared to anterior dislocations, provided the initial reduction is concentric and major associated instability-causing lesions are adequately addressed.
- Functional Limitations: Residual pain, weakness (especially if nerve recovery is incomplete), and limitations in range of motion are not uncommon (Paschal et al., 2014).
Key Guidelines and Recommendations:
*
High Index of Suspicion:
Always anticipate and actively evaluate for concomitant neurovascular and musculoskeletal injuries.
*
Comprehensive Imaging:
Standard radiographs, followed by CT scan for bony detail, and MRI for soft tissue assessment. CTA for suspected vascular injury is imperative.
*
Meticulous Neurovascular Assessment:
Document findings thoroughly pre- and post-reduction, and throughout the peri-operative course.
*
Gentle Reduction Techniques:
Avoid excessive force during closed reduction attempts. If resistance is significant, proceed directly to open reduction.
*
Address Associated Pathology:
Intra-operative identification and repair of significant rotator cuff tears, labral injuries, and unstable fractures are crucial for long-term stability and optimal function.
*
Tailored Rehabilitation:
Implement a structured, progressive rehabilitation program, carefully balancing protection of repairs with early, controlled motion to mitigate stiffness and maximize functional recovery.
In summary, luxatio erecta demands a comprehensive, systematic, and often multidisciplinary approach. Effective management hinges on prompt and accurate diagnosis, early recognition and management of critical associated injuries, judicious reduction techniques, and meticulous surgical repair when indicated, all underpinned by a disciplined and individualized rehabilitation protocol.
