Operative Management of Congenital Foot and Toe Anomalies
Key Takeaway
The operative management of congenital foot and toe anomalies requires a profound understanding of pediatric biomechanics and pathoanatomy. This comprehensive guide details evidence-based surgical interventions for conditions such as talipes equinovarus, metatarsus adductus, and complex toe deformities. Emphasizing both soft-tissue releases and osseous reconstructions, it provides orthopedic surgeons with step-by-step protocols to optimize functional outcomes and minimize recurrence in the pediatric patient.
Introduction to Congenital Foot and Toe Deformities
The surgical management of congenital anomalies of the foot and toes represents one of the most intricate domains of pediatric orthopedics. Historically characterized by aggressive, extensive soft-tissue releases, the paradigm has shifted toward a profound respect for biomechanics, tissue-sparing techniques, and the preservation of joint kinematics. Conditions ranging from isolated digital anomalies (macrodactyly, polydactyly) to complex multi-planar deformities (talipes equinovarus, metatarsus adductus) require a meticulous, stage-specific approach.
This masterclass delineates the pathoanatomy, operative indications, surgical techniques, and postoperative protocols for the most frequently encountered congenital foot and toe anomalies, synthesizing decades of evidence-based literature into a definitive guide for the practicing orthopedic surgeon.
Congenital Anomalies of the Toes
Digital anomalies of the foot, while sometimes functionally benign, often present significant challenges regarding shoe wear, ambulation, and cosmesis. Surgical intervention must balance aesthetic improvement with the preservation of a painless, plantigrade forefoot.
Macrodactyly (Macrodystrophia Lipomatosa)
Macrodactyly of the foot is a rare, non-hereditary congenital enlargement of the digits, often associated with lipofibromatosis and neurofibromatosis. The hypertrophy typically follows the distribution of the medial or lateral plantar nerves.
- Pathoanatomy: Involves the proliferation of mesenchymal elements, particularly adipose tissue, within the nerve sheaths. The condition can be static (growing proportionally with the child) or progressive (growing disproportionately).
- Indications for Surgery: Difficulty with shoe wear, progressive angular deformity, and recurrent ulceration.
- Surgical Approaches:
- Soft-Tissue Debulking: Performed in a staged manner (one side of the digit at a time to preserve vascularity). Involves meticulous excision of the fibrofatty tissue surrounding the neurovascular bundles.
- Epiphysiodesis: Proximal phalangeal epiphysiodesis is indicated to arrest longitudinal growth once the toe reaches the length of the adult parent's corresponding toe.
- Ray Resection: In severe, progressive cases where the digit is grotesquely enlarged and non-functional, a complete ray amputation provides the most definitive and functional outcome, allowing for normal shoe wear.
Surgical Pitfall: Aggressive single-stage bilateral debulking of a macrodactylic digit carries an unacceptably high risk of vascular compromise and subsequent necrosis. Always stage debulking procedures at least 3 to 6 months apart.
Cleft Foot Deformity (Lobster-Claw Deformity)
Cleft foot is a longitudinal deficiency characterized by the absence of the central rays (second, third, or fourth). It is often inherited in an autosomal dominant pattern and may be associated with cleft hand or syndromic conditions.
- Classification: The Blauth and Borisch classification is utilized, based on radiographic morphology and the number of remaining metatarsals.
- Surgical Reconstruction: The primary goal is to close the cleft, provide a broad weight-bearing surface, and prevent progressive splaying of the forefoot.
- Technique: A plantar-advancement skin flap or a simple V-Y closure is utilized. The opposing articular surfaces of the adjacent metatarsals are denuded, and heavy non-absorbable sutures or a transverse K-wire are used to approximate the metatarsals (surgical syndactyly).
- Timing: Surgery is optimally performed between 1 and 2 years of age, prior to the establishment of mature walking patterns.
Overlapping Fifth Toe and Curly Toes
- Overlapping Fifth Toe: Characterized by dorsiflexion, adduction, and external rotation of the fifth toe, often overriding the fourth toe. If conservative taping fails and the child experiences pain with shoe wear, surgical correction is indicated. The Butler Arthroplasty (a dorsal racquet incision with extensive capsulotomy and tendon lengthening) or the Lapidus Procedure (extensor tendon transfer) are the procedures of choice.
- Curly Toes: Typically involves flexion and varus rotation of the lesser toes. Most resolve spontaneously. For persistent, symptomatic cases, a simple open flexor tenotomy at the level of the proximal interphalangeal joint yields excellent results.
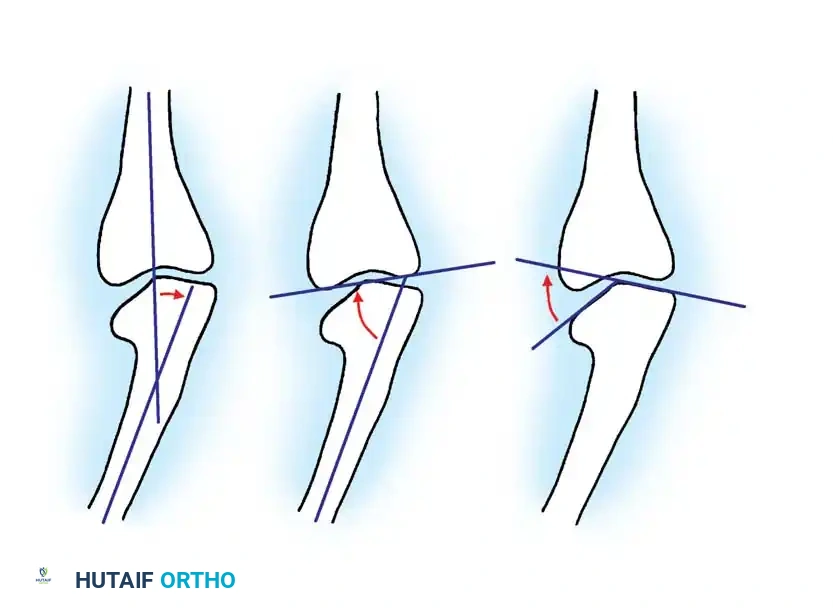
Congenital Metatarsus Adductus
Metatarsus adductus is the most common congenital foot deformity, characterized by medial deviation of the forefoot relative to the hindfoot at the tarsometatarsal (Lisfranc) joint.
Biomechanics and Indications
The hindfoot is typically in neutral or slight valgus, distinguishing it from clubfoot. While 90% of cases resolve spontaneously or with serial casting, rigid deformities persisting beyond 4 to 5 years of age require surgical intervention to prevent a painful, skewed foot in adulthood.
Soft-Tissue Procedures
- Abductor Hallucis Release (Lichtblau Procedure): Indicated for younger children (2-4 years) with a dynamic deforming force. The abductor hallucis tendon is sectioned near its insertion, releasing the medial tether.
- Tarsometatarsal Mobilization (Heyman-Herndon Procedure): Historically popular, this involves a complete capsulotomy of all five tarsometatarsal joints.
- Warning: This procedure has largely fallen out of favor due to high rates of premature physeal closure, joint stiffness, and degenerative arthritis of the Lisfranc complex.
Osseous Reconstructions (The Berman-Gartland Procedure)
For rigid metatarsus adductus in children over 5 years of age, multiple metatarsal osteotomies are the gold standard.
- Positioning: Supine with a bump under the ipsilateral hip. Tourniquet control is essential.
- Approach: Two or three dorsal longitudinal incisions are made to access all five metatarsal bases.
- Osteotomy Technique: Dome-shaped or crescentic osteotomies are performed at the bases of the metatarsals, distal to the physis. The dome shape allows for multi-planar correction without shortening the metatarsal.
- Fixation: The forefoot is abducted to a neutral position. The first and fifth metatarsals are typically stabilized with smooth K-wires driven retrogradely or antegrade across the osteotomy sites.
- Postoperative Protocol: A non-weight-bearing short leg cast is applied for 6 weeks, followed by K-wire removal and transition to a weight-bearing cast or boot for an additional 4 weeks.
Clinical Pearl: When performing metatarsal osteotomies, always ensure the osteotomy of the first metatarsal is strictly distal to the proximal physis to prevent growth arrest and subsequent brachymetatarsia.
Congenital Talipes Equinovarus (Clubfoot)
Clubfoot is a complex, three-dimensional deformity encompassing four distinct components, easily remembered by the acronym CAVE: Cavus (midfoot), Adductus (forefoot), Varus (hindfoot), and Equinus (ankle).
The Paradigm Shift: Conservative Management
The Ponseti Method is the universally accepted gold standard for initial management, boasting success rates exceeding 90%. It involves serial manipulation and casting, sequentially correcting the cavus, adductus, varus, and finally the equinus (often requiring a percutaneous Achilles tenotomy).
However, operative intervention remains critical for:
1. Syndromic or teratologic clubfeet (e.g., Arthrogryposis, Spina Bifida).
2. Neglected clubfeet presenting in older children.
3. Relapsed clubfeet resistant to repeat casting.
Comprehensive Posteromedial Release (PMR)
When soft-tissue release is indicated, the comprehensive posteromedial release addresses the contracted medial and posterior structures.
- Positioning: The patient is placed prone to allow simultaneous access to the posterior ankle and medial foot.
- Incision: The Cincinnati Incision is preferred. It is a transverse incision extending from the anteromedial aspect of the foot (navicular-cuneiform joint), curving horizontally around the posterior heel just above the heel crease, to the anterolateral aspect of the foot (distal to the lateral malleolus).
- Surgical Steps:
- Superficial Dissection: The sural nerve and short saphenous vein are protected laterally. The neurovascular bundle (posterior tibial artery and tibial nerve) is identified medially and protected with a vessel loop.
- Tendon Lengthening: Z-lengthening of the Achilles tendon (tendoachilles) is performed. The tibialis posterior, flexor digitorum longus (FDL), and flexor hallucis longus (FHL) tendons are identified and lengthened if severely contracted.
- Posterior Release: A posterior capsulotomy of the tibiotalar and subtalar joints is performed. The posterior talofibular and calcaneofibular ligaments are sectioned.
- Medial Release: The talonavicular joint capsule is opened. The spring ligament (plantar calcaneonavicular ligament) and the superficial deltoid ligament are released to allow the navicular to reduce laterally onto the talar head.
- Plantar Release: If severe cavus is present, a plantar fasciotomy is performed.
- Reduction and Fixation: The talonavicular and subtalar joints are anatomically reduced and held with smooth K-wires.
- Closure: The skin is closed loosely. If tension is excessive, the wound may be left partially open to heal by secondary intention, or a V-Y advancement flap may be utilized to prevent skin necrosis.
Surgical Pitfall: Over-correction during a posteromedial release can lead to a devastating "over-released" or planovalgus foot. Always pin the joints in a neutral, plantigrade position, resisting the temptation to force the foot into excessive valgus or dorsiflexion.
Management of the Relapsed or Neglected Clubfoot
Dynamic Supination: Tibialis Anterior Tendon Transfer (TATT)
A common presentation of relapsed clubfoot is dynamic supination during the swing phase of gait, caused by an overpowering tibialis anterior muscle in the setting of a weakened peroneal compartment.
* Procedure: The entire tibialis anterior tendon is detached from its insertion on the medial cuneiform, routed subcutaneously beneath the extensor retinaculum, and transferred to the lateral cuneiform or cuboid. This converts the muscle from a supinator to a pure dorsiflexor.
The "Bean-Shaped" Foot: Osseous Procedures
In older children (typically >4 years) with recurrent adductus and midfoot breach, soft-tissue procedures are insufficient. The lateral column is relatively long, and the medial column is short.
* Lateral Column Shortening: A closing wedge osteotomy of the cuboid (or cuboid decancellation) is performed.
* Medial Column Lengthening: An opening wedge osteotomy of the medial cuneiform is performed simultaneously, often utilizing the bone graft harvested from the cuboid.
Severe Neglected Deformities: The Ilizarov Method
For severe, rigid, neglected clubfeet in older children or adolescents, acute surgical correction carries a high risk of neurovascular compromise and skin necrosis.
* Technique: The application of a circular external fixator (Ilizarov or Taylor Spatial Frame) allows for gradual, multi-planar distraction histogenesis. Osteotomies (such as a V-osteotomy of the midfoot or supramalleolar osteotomies) may be incorporated. This method safely stretches the neurovascular bundle and soft tissues while correcting the bony architecture.
Salvage Procedures
In the skeletally mature patient with a rigid, painful, arthritic clubfoot, joint-sparing procedures are no longer viable.
* Triple Arthrodesis: Fusion of the subtalar, talonavicular, and calcaneocuboid joints provides a stable, plantigrade, and pain-free foot, albeit at the cost of hindfoot inversion/eversion.
* Talectomy (Astragalectomy): Reserved as a definitive salvage procedure for severe, rigid equinovarus deformities, particularly in patients with arthrogryposis or spina bifida, where the talus is severely deformed and the skin is compromised.
Postoperative Protocols and Rehabilitation
The success of any operative intervention for congenital foot anomalies relies heavily on rigorous postoperative care.
- Immobilization: Following major soft-tissue releases or osteotomies, the foot is immobilized in a long-leg cast with the knee flexed at 90 degrees to prevent the child from kicking off the cast and to relax the gastrocnemius.
- Pin Management: K-wires used for joint stabilization are typically removed in the clinic at 4 to 6 weeks postoperatively.
- Bracing: Once casting is complete, a strict bracing protocol is initiated. For clubfoot, a foot abduction orthosis (e.g., Denis Browne splint) is worn for 23 hours a day for 3 months, followed by nighttime wear until the age of 4 to 5 years to prevent recurrence.
- Physical Therapy: Gait training, proprioceptive re-education, and active range-of-motion exercises are instituted once bony union is achieved and soft tissues have healed.
Conclusion
The operative management of congenital foot and toe anomalies demands a highly individualized approach. While the advent of the Ponseti method has drastically reduced the need for extensive surgical releases in clubfoot, the orthopedic surgeon must remain proficient in a wide armamentarium of soft-tissue and osseous procedures. By adhering to strict biomechanical principles, respecting the delicate pediatric soft-tissue envelope, and ensuring rigorous postoperative bracing, surgeons can achieve the ultimate goal: a painless, plantigrade, and functional foot that serves the patient throughout their lifetime.
You Might Also Like