Proximal Humerus Fractures: Epidemiology, Advanced Anatomy & Biomechanics
Key Takeaway
Proximal humerus fractures are complex injuries with bimodal epidemiology. Management is individualized, guided by Neer or AO/OTA classification. Crucial surgical anatomy includes the humeral head's blood supply, tuberosities, and vital neurovascular structures like the axillary nerve. Understanding deforming biomechanical forces is essential for effective anatomical reduction and fixation.
Introduction & Epidemiology
Proximal humerus fractures represent a significant burden on orthopedic trauma services, accounting for approximately 5-6% of all fractures and 45% of all humeral fractures. Their incidence exhibits a bimodal distribution, with younger patients typically sustaining high-energy trauma, and older, osteopenic individuals experiencing fragility fractures often from low-energy falls. The increasing life expectancy and prevalence of osteoporosis globally contribute to a rising incidence, particularly in postmenopausal women, making these fractures a growing public health concern.
The management of proximal humerus fractures is complex and highly individualized, dictated by patient factors (age, functional demand, bone quality, comorbidities), fracture characteristics (displacement, comminution, angulation, articular involvement), and surgeon experience. Non-operative management remains the cornerstone for the majority of minimally displaced and stable fractures. However, advancements in surgical techniques, implant design, and rehabilitation protocols have expanded the indications for operative intervention in more complex patterns, aiming to restore anatomy, preserve function, and minimize long-term sequelae such as stiffness, pain, and malunion.
Classification systems are indispensable for communication, prognostication, and guiding treatment. The Neer classification, though widely used, suffers from moderate inter- and intra-observer reliability. It categorizes fractures based on the displacement of four major segments: the humeral head, greater tuberosity, lesser tuberosity, and humeral shaft. A fracture is considered "displaced" if there is greater than 1 cm of displacement or 45 degrees of angulation between any two segments. This system informs the choice between one-part, two-part, three-part, and four-part fractures, with increasing complexity generally correlating with poorer outcomes and higher rates of avascular necrosis (AVN). Other systems, such as the AO/OTA classification, offer a more detailed morphological description, classifying fractures from simple (Type A) to multifragmentary articular (Type C).
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy of the proximal humerus is paramount for successful surgical intervention. The proximal humerus comprises the humeral head, greater tuberosity, lesser tuberosity, and the surgical neck.
-
Humeral Head
: Articulates with the glenoid fossa. Its blood supply is critical for survival after fracture. The dominant blood supply to the humeral head is often described as originating from the ascending branch of the anterior circumflex humeral artery (ACHA) and branches from the posterior circumflex humeral artery (PCHA), forming an arcuate artery system. The posteromedial vessels, particularly the arcuate artery, are considered the most significant. Fractures disrupting these vessels, especially multi-part fractures with significant displacement or dislocation, place the humeral head at high risk of avascular necrosis.

- Greater Tuberosity : Located laterally, it serves as the insertion site for the supraspinatus, infraspinatus, and teres minor tendons (SIT). Fractures involving the greater tuberosity are often associated with rotator cuff dysfunction and can lead to impingement if malreduced.
- Lesser Tuberosity : Located anteriorly, it is the insertion site for the subscapularis tendon. Displaced lesser tuberosity fractures can result in internal rotation weakness and instability.
- Surgical Neck : The region distal to the tuberosities and superior to the insertion of the pectoralis major. This is a common site for fractures, often involving angular displacement due to muscle pull.
Neurovascular Structures:
The proximal humerus is intimately associated with critical neurovascular structures:
*
Axillary Nerve
: Courses circumferentially around the surgical neck, approximately 5-7 cm distal to the acromion, often referred to as the "safe zone." It innervates the deltoid and teres minor, providing sensation over the lateral deltoid region. It is vulnerable during lateral surgical approaches, hardware placement, and even closed reduction maneuvers.
*
Musculocutaneous Nerve
: Pierces the coracobrachialis muscle, innervating the biceps and brachialis. It is typically less at risk but can be injured in very proximal approaches or if dissection extends too medially.
*
Radial Nerve
: Lies more distally in the spiral groove, typically not directly at risk in isolated proximal humerus fractures, but can be involved in associated humeral shaft injuries or extensive soft tissue dissection.
*
Brachial Plexus
: Located superior and medial to the humeral head, vulnerable in dislocations or severe trauma.
*
Posterior Circumflex Humeral Artery (PCHA)
: Accompanies the axillary nerve posteriorly around the surgical neck. Damage can lead to significant hemorrhage.
*
Anterior Circumflex Humeral Artery (ACHA)
: Travels anteriorly around the surgical neck. Its ascending branch is crucial for humeral head blood supply.
Biomechanics:
The rotator cuff muscles exert significant deforming forces on fracture fragments:
*
Supraspinatus, Infraspinatus, Teres Minor (Greater Tuberosity)
: Tend to pull the greater tuberosity fragment superiorly and posteriorly.
*
Subscapularis (Lesser Tuberosity)
: Tends to pull the lesser tuberosity fragment medially and anteriorly.
*
Deltoid and Pectoralis Major
: Exert deforming forces on the humeral shaft, often pulling it medially and anteriorly relative to the humeral head.
Understanding these forces is crucial for achieving anatomical reduction and stable fixation, particularly for tuberosity reattachment, which is fundamental for restoring rotator cuff function. The bone quality, especially in osteoporotic patients, influences the stability of fixation, necessitating implants with enhanced locking mechanisms and careful screw placement.
Indications & Contraindications
The decision-making process for proximal humerus fractures involves a careful consideration of patient-specific factors and fracture characteristics. While non-operative treatment remains the gold standard for many, operative intervention is increasingly considered for displaced and complex patterns to optimize functional outcomes.
Non-Operative Indications
- Minimally displaced fractures (<1 cm displacement, <45 degrees angulation).
- Stable one-part or impacted two-part fractures.
- Elderly patients with low functional demands and significant comorbidities that preclude surgery.
- Patients with poor bone quality where fixation may be precarious.
- Patients who decline surgery.
Operative Indications
- Displaced two-part surgical neck fractures : Especially in active patients, significant angulation or displacement can lead to malunion and functional impairment.
- Displaced two-part anatomical neck fractures : High risk of AVN, often managed with arthroplasty in elderly.
- Displaced two-part greater tuberosity fractures : Displacements >5mm (or 3mm if subacromial impingement) in active patients, leading to rotator cuff dysfunction and impingement.
- Displaced two-part lesser tuberosity fractures : Rare, but can cause internal rotation weakness or block shoulder motion.
- Three-part and four-part fractures : Typically considered for operative management due to instability, high displacement, and significant risk of functional impairment if malunited.
- Fracture-dislocations : Requires reduction of the dislocation and stabilization of the fracture.
- Open fractures : Require emergent debridement and stabilization.
- Associated neurovascular injury : May require surgical exploration and repair, with fracture stabilization as a concomitant goal.
- Failure of non-operative treatment : Progressive displacement, unacceptable pain, or functional limitation.
Contraindications for Operative Treatment
-
Absolute Contraindications
:
- Active infection (local or systemic).
- Severe overlying soft tissue compromise or devitalization (relative, may require delay or external fixation).
- Severe medical comorbidities precluding safe anesthesia and surgery.
- Patient unwillingness or inability to comply with post-operative rehabilitation.
-
Relative Contraindications
:
- Extremely poor bone quality (osteoporosis) where stable fixation is unlikely.
- Significant comminution rendering reconstructive surgery impractical or with very high risk of failure (may favor arthroplasty).
- Long-standing untreated fractures (>3 weeks, making reduction difficult).
- Severe uncorrectable coagulopathy.
Summary of Operative vs. Non-Operative Indications
| Factor | Non-Operative Management | Operative Management |
|---|---|---|
| Fracture Pattern | One-part, stable impacted two-part (surgical neck) | Displaced two-part (surgical neck, tuberosity), three-part, four-part |
| Displacement | <1 cm displacement | >1 cm displacement or >5mm for tuberosity fractures |
| Angulation | <45 degrees angulation | >45 degrees angulation |
| Patient Age | Elderly, low functional demand | Younger, active patients, high functional demand |
| Bone Quality | Severe osteoporosis (may lead to poor fixation) | Adequate bone quality for stable fixation |
| Comorbidities | Numerous, high anesthetic risk | Few, acceptable anesthetic risk |
| Soft Tissues | Intact, minimal compromise | Open fractures, significant compromise |
| Associated Injury | Isolated injury | Neurovascular injury, dislocation, rotator cuff tear |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is critical for anticipating surgical challenges, selecting appropriate implants, and minimizing operative time and complications.
Pre-Operative Planning
-
Imaging Review
:
- Standard Radiographs : AP, lateral (scapular Y or true axillary), and often a Neer trauma series (AP, scapular Y, axillary views) are essential to classify the fracture, assess displacement, and identify associated dislocations.
- Computed Tomography (CT) : Highly recommended for complex fracture patterns (three-part, four-part), articular involvement, or comminution. CT with 3D reconstructions provides invaluable information regarding fragment orientation, tuberosity comminution, and glenoid involvement, aiding in surgical strategy.
- MRI : Rarely needed acutely, but can be useful for assessing rotator cuff integrity, particularly in greater tuberosity fractures where cuff avulsion is suspected.
- Templating : Using contralateral radiographs or specific implant templates, determine appropriate plate length and screw sizes. This helps in estimating the need for bone graft and anticipating potential pitfalls.
-
Implant Selection
:
- Locking Plate Osteosynthesis (LPO) : Most common for ORIF of displaced two-, three-, and four-part fractures. Modern locking plates (e.g., PHILOS plate, Zimmer Biomet Peri-Loc, Synthes LCP) offer angular stability, which is advantageous in osteopenic bone and comminuted metaphyses.
- Intramedullary Nailing : Less commonly used for proximal humerus fractures due to challenges with rotational control and fixation of tuberosity fragments, but can be considered for certain surgical neck fractures, particularly in younger patients.
- Arthroplasty : Hemiarthroplasty or reverse total shoulder arthroplasty (rTSA) are options for highly comminuted four-part fractures, head-splitting fractures, fracture-dislocations with irreparable rotator cuff, and osteopenic elderly patients, especially in fracture patterns with a high risk of AVN.
- Surgical Approach Selection : Predominantly the deltopectoral approach for ORIF. Deltoid-splitting approaches are generally avoided for plate fixation due to the risk of axillary nerve injury and deltoid damage, but may be used for IM nailing or limited internal fixation of isolated greater tuberosity fractures.
Patient Positioning
The choice of patient positioning depends on the planned surgical approach and surgeon preference.
1.
Beach Chair Position (Semi-Fowler)
:
*
Advantages
: Excellent exposure for deltopectoral approach, allows for easy transition to arthroplasty if needed, reduces venous pressure, and allows for intraoperative assessment of shoulder motion. The arm is draped freely.
*
Setup
: Patient is seated at a 60-70 degree angle, with the head secured in a padded headrest (e.g., Mayfield clamp). The back is elevated, and the knees are slightly flexed. The ipsilateral arm is draped free to allow for manipulation. The torso may be rotated slightly away from the surgeon to enhance exposure. Care must be taken to prevent cerebral hypoperfusion, especially in elderly patients with compromised cerebral autoregulation.
2.
Lateral Decubitus Position
:
*
Advantages
: Provides good access to the posterior aspect of the shoulder, useful for posterior dislocations or certain approaches. Can utilize a traction tower for indirect reduction.
*
Setup
: Patient lies on the contralateral side, secured with axillary roll, hip and knee supports. The ipsilateral arm is often suspended in traction using finger traps, allowing for controlled distraction and manipulation. This setup is less common for standard ORIF of proximal humerus fractures via deltopectoral approach.
Key considerations for all positions
:
*
Padding
: All pressure points must be adequately padded to prevent nerve palsies (ulnar, peroneal, etc.) or skin breakdown.
*
Fluoroscopy Access
: Ensure clear access for intraoperative imaging in at least two planes (AP and axillary/Y-view). The C-arm must be able to move freely.
*
Sterile Field
: Broad sterile draping to allow for extensive exposure and potential extension of the incision.
Detailed Surgical Approach / Technique
The most common and versatile approach for open reduction and internal fixation (ORIF) of proximal humerus fractures is the deltopectoral approach .
Deltopectoral Approach (Right Shoulder Example)
- Incision : A curvilinear incision is made from the tip of the coracoid process (or slightly more medial) curving distally along the deltopectoral groove for approximately 10-15 cm, centered over the expected fracture site.
- Dissection to Deltopectoral Groove : Subcutaneous dissection identifies the deltopectoral groove. The cephalic vein, which lies within this groove, is identified. Typically, the vein is retracted laterally with the deltoid, but it can be ligated and divided if necessary for exposure or if it is injured.
- Internervous Plane : The deltopectoral groove is a true internervous plane between the deltoid muscle (innervated by the axillary nerve, posterior cord of brachial plexus) laterally and the pectoralis major muscle (innervated by the medial and lateral pectoral nerves, medial and lateral cords of brachial plexus) medially.
-
Deep Dissection
:
- The fascia over the pectoralis major and deltoid is incised.
- The pectoralis major is retracted medially.
- The deltoid is retracted laterally. Care must be taken not to excessively retract the deltoid laterally or distally to avoid traction injury to the axillary nerve, which enters the deep surface of the deltoid approximately 5-7 cm distal to the acromion.
- Subdeltoid Space Entry : The clavipectoral fascia is identified deep to the deltopectoral groove. It is incised longitudinally to expose the underlying structures. The coracoacromial ligament may be visible superiorly.
-
Exposure of Fracture
: The bicipital groove and its contents (long head of biceps tendon) are identified. The conjoined tendon (short head of biceps and coracobrachialis) lies medial to the bicipital groove. The fracture fragments are exposed. Hematoma is evacuated.
Reduction and Fixation (using Locking Plate Osteosynthesis)
- Indirect Reduction : Initial reduction often involves gentle longitudinal traction on the arm, which helps to disimpact fragments and align the shaft. External rotation can assist in bringing the humeral head out of internal rotation.
-
Direct Reduction
:
- Humeral Head : For displaced humeral heads, joy sticks (K-wires inserted into the head fragment) can be used to manipulate it into anatomical position. Care is taken to avoid violating critical blood supply to the head.
- Shaft : The humeral shaft fragment is typically pulled medially and anteriorly by the pectoralis major. It can be reduced to the head using bone clamps, reduction forceps, or a Hohmann retractor around the shaft.
- Tuberosities : The greater and lesser tuberosities are often displaced by rotator cuff pull. They must be anatomically reduced and secured to the humeral head. Sutures (non-absorbable, high-strength) passed through the rotator cuff tendons and tuberosity bone, then through plate eyelets or drill holes, are critical for robust fixation, especially in osteoporotic bone.
- Temporary Fixation : K-wires are used to provisionally hold the reduced fragments. Two K-wires diverging from the anterior aspect of the humeral head into the glenoid can stabilize the head, or K-wires can fix the shaft to the head and tuberosities.
-
Plate Application
:
- A pre-contoured locking plate (e.g., PHILOS plate) is selected. The plate is typically positioned laterally, along the anterolateral aspect of the proximal humerus, centered on the bicipital groove or slightly posterior to it.
- The superior border of the plate should be approximately 5-8 mm distal to the superior aspect of the greater tuberosity to avoid impingement against the acromion.
- The plate is held against the bone, and its position is verified with fluoroscopy (AP and axillary views) to ensure it is not too prominent and allows for adequate screw length.
-
Proximal Screw Placement (Humeral Head)
:
- Locking screws are inserted into the humeral head. These screws provide angular stability and do not rely on compression across the fracture site.
- Aim for bicortical purchase where possible, but carefully measure screw length to avoid penetration of the articular surface. Use fluoroscopy in multiple planes to confirm screw tip position.
- Target screws should be placed to capture maximum bone stock in the humeral head, especially supporting the calcar (inferomedial aspect of the head) to prevent varus collapse. A common pattern involves divergent screws to enhance stability.
-
Distal Screw Placement (Humeral Shaft)
:
- Cortex screws are often used first for compression and lag screw effect across the surgical neck fracture (if applicable) to draw the shaft to the head.
- Locking screws are then placed in the shaft, ensuring bicortical purchase. A minimum of 3-4 bicortical screws are desirable in the shaft for adequate working length and stability.
-
Tuberosity Fixation (Suture Augmentation)
:
- After the main head-shaft fixation, the greater and lesser tuberosities are definitively secured. High-strength non-absorbable sutures are passed through the rotator cuff insertions on the tuberosities.
- These sutures are then brought through specific eyelets in the plate or through drill holes created in the plate, and tied over the plate or a dedicated suture button. This robust suture augmentation is crucial for resisting rotator cuff muscle pull and promoting tuberosity union.
- Sutures can also be passed directly through the shaft bone to provide additional tuberosity fixation ("suture bridge").
-
Final Assessment
:
- Intraoperative fluoroscopy in AP and axillary views confirms reduction, plate position, and screw lengths. Check for articular penetration, especially with shoulder rotation.
- Assess shoulder range of motion passively to ensure no impingement of hardware against the acromion or glenoid, and to confirm stability of fixation.
- Wound Closure : The wound is irrigated. A drain may be placed in cases of significant comminution or bleeding. The deltopectoral interval is loosely closed. Subcutaneous tissues and skin are closed in layers.
Special Considerations for Arthroplasty (Hemiarthroplasty/rTSA)
For highly comminuted four-part fractures, head-splitting fractures, or in elderly patients with poor bone quality, arthroplasty may be indicated.
*
Hemiarthroplasty
: Replaces the humeral head with a prosthetic component. Crucial for success is anatomic reattachment of the tuberosities to the prosthesis. The tuberosities are typically secured to the stem using sutures, and often bone grafting is placed within the stem-tuberosity interface.
*
Reverse Total Shoulder Arthroplasty (rTSA)
: Increasingly preferred in elderly patients with displaced four-part fractures, particularly if the rotator cuff is deficient or at high risk of failure. rTSA provides greater stability and functional outcomes independent of rotator cuff and tuberosity healing, though tuberosity reattachment is still attempted to optimize external rotation. The glenoid is replaced with a sphere (glenosphere), and the humeral component is a socket.
Complications & Management
Proximal humerus fractures, especially those treated operatively, are associated with a range of potential complications that can significantly impact long-term outcomes. Proactive identification and appropriate management are crucial.
Common Complications
| Complication | Incidence (%) | Management Strategy |
|---|---|---|
| Avascular Necrosis (AVN) | 5-30% (higher in 3- and 4-part fractures) |
Prevention
: Gentle soft tissue handling, preserve blood supply, anatomical reduction.
Early Stage : Observation, pain management. Late Stage (collapse) : Hemiarthroplasty or rTSA (especially with failed tuberosities), depending on patient age and rotator cuff status. |
| Nonunion/Malunion | 5-20% (higher in osteoporotic bone, smoking) |
Nonunion
: Revision ORIF with bone grafting (autograft/allograft), intramedullary fibular graft, or conversion to arthroplasty if fixation fails or bone stock is poor.
Malunion : Osteotomy with internal fixation, or arthroplasty for severe symptomatic cases (e.g., impingement, limited ROM). |
| Screw Cutout/Failure of Fixation | 5-15% (especially in osteoporotic bone, varus collapse) |
Prevention
: Calcar support screws, adequate proximal screw density, proper plate positioning, robust tuberosity fixation.
Management : Revision ORIF, revision with longer screws, conversion to arthroplasty (hemi/rTSA). |
| Infection | 1-5% (superficial or deep) |
Superficial
: Oral antibiotics, local wound care.
Deep : Surgical irrigation and debridement, targeted intravenous antibiotics, hardware retention (if stable and early) or removal (if unstable/late), possibly two-stage revision. |
| Stiffness/Adhesive Capsulitis | 10-30% (common post-immobilization) |
Prevention
: Early supervised rehabilitation.
Management : Aggressive physical therapy, judicious corticosteroid injections, manipulation under anesthesia (MUA), arthroscopic capsular release for refractory cases. |
| Nerve Injury | 2-10% (most commonly axillary nerve) |
Prevention
: Careful dissection, avoid excessive retraction, identify nerve.
Management : Observation (most neurapraxias resolve), electrodiagnostic studies, nerve repair/grafting for complete transections, tendon transfers for persistent deficits. |
| Rotator Cuff Pathology | 5-20% (tear or failure of tuberosity healing) |
Prevention
: Anatomical tuberosity reduction and strong suture fixation.
Management : Physical therapy for minor dysfunction. Surgical repair for symptomatic non-healing tuberosity or significant rotator cuff tears, or conversion to arthroplasty (especially rTSA). |
| Hardware Impingement/Prominence | 5-10% |
Prevention
: Correct plate positioning (inferior to greater tuberosity), flush screw heads.
Management : Hardware removal after fracture healing, if symptomatic. |
| Pain | Variable (can be chronic) | Management : Multimodal pain management, physical therapy, consider hardware removal, evaluate for other complications (nonunion, impingement, AVN), psychological support. |
Specific Considerations:
- Varus Collapse : A common failure mode for locking plate fixation, particularly in osteoporotic bone. The humeral head collapses into varus, leading to screw cutout and loss of reduction. Prevention involves strong calcar support (medial cortical column), judicious use of impaction bone grafting, and robust tuberosity repair.
- Loss of Reduction : May occur early post-operatively due to unstable fixation, inadequate bone purchase, or premature aggressive rehabilitation. Requires reassessment and potentially revision surgery.
- Heterotopic Ossification (HO) : Can occur in muscle or soft tissues around the shoulder, leading to pain and stiffness. Prophylaxis with NSAIDs or low-dose radiation may be considered in high-risk patients (e.g., head injury, severe burns).
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical procedure itself for achieving optimal functional outcomes and preventing stiffness or re-injury. Protocols are individualized based on fracture stability, fixation strength, bone quality, patient compliance, and surgical findings (e.g., tuberosity healing, rotator cuff repair).
General Principles
- Protect Fixation : Balance early motion with protection of the repair.
- Restore Range of Motion (ROM) : Prevent stiffness, especially external rotation and abduction.
- Regain Strength : Gradually restore rotator cuff and deltoid strength.
- Functional Return : Progress to activities of daily living and sport-specific movements.
Phased Rehabilitation Approach
Phase 1: Immediate Post-operative (Weeks 0-6)
- Goals : Pain and edema control, protect fixation, allow soft tissue healing, gentle passive range of motion.
- Immobilization : Arm typically in a sling (e.g., UltraSling, shoulder immobilizer) for 4-6 weeks, removing for exercises. Elbow, wrist, and hand ROM exercises should begin immediately.
- Pain Management : Multimodal analgesia.
-
Passive Range of Motion (PROM)
:
- Codman's Pendulum Exercises : Begin within the first week, performed several times daily. These provide gentle distraction and movement without active muscle contraction.
- Supine Passive Flexion : Gravity-assisted, performed with the elbow bent or straight, to tolerance (e.g., 60-90 degrees flexion).
- Passive External Rotation : Performed with the arm adducted to the side, to tolerance (e.g., 0-30 degrees).
- Passive Abduction : Limited to avoid stressing tuberosity repair, often not initiated until later in this phase or in Phase 2.
- Precautions : NO active shoulder motion, NO lifting, NO pushing or pulling, NO weight-bearing through the arm. Avoid hyperextension and combined abduction-external rotation.
Phase 2: Early Mobilization (Weeks 6-12)
- Goals : Gradually increase PROM, introduce active-assisted ROM (AAROM) and gentle active ROM (AROM), improve muscle activation.
- Immobilization : Discontinue sling use gradually as tolerated, except for sleep or in crowded environments.
-
AAROM
:
- Pulley exercises : For flexion and abduction.
- Wand exercises : For internal/external rotation, flexion, and abduction within limits.
-
AROM
:
- Initiate gentle AROM for flexion and abduction, gradually increasing over time.
- Rotator cuff isometrics (gentle, submaximal) can be introduced if tuberosity healing is progressing well (e.g., after 8-10 weeks).
- Scapular Stabilization : Exercises to promote scapular control (e.g., scapular squeezes, protraction/retraction).
- Precautions : Avoid sudden movements or heavy lifting. Continue to avoid resistance training that could stress the healing fracture site.
Phase 3: Strengthening and Advanced Motion (Weeks 12-24)
- Goals : Full AROM, initiate progressive strengthening, improve endurance.
- Range of Motion : Work towards full pain-free ROM in all planes. May require sustained stretching or mobilization techniques.
-
Strengthening
:
- Rotator Cuff Strengthening : Begin with light resistance (theraband, light weights) for internal/external rotation, abduction, scapular plane elevation.
- Deltoid Strengthening : Light resistance for flexion, abduction, extension.
- Biceps/Triceps Strengthening : As tolerated.
- Proprioceptive Exercises : Balance and coordination drills.
- Precautions : Progress resistance gradually. Monitor for pain or signs of impingement. Avoid high-impact or overhead activities that could overload the healing bone.
Phase 4: Return to Activity/Sport-Specific (Months 6+)
- Goals : Restore full strength and power, return to full functional activities and sport.
- Advanced Strengthening : Progress to heavier weights, functional movement patterns, plyometrics (if appropriate for sport).
- Sport-Specific Training : Gradually reintroduce sport-specific drills and activities, emphasizing proper form and technique.
- Maintenance Program : Ongoing exercise program to maintain strength and flexibility.
Important Considerations
:
*
Bone Healing
: Radiographic evidence of healing (callus formation, bridging bone) guides progression, particularly for resistance exercises.
*
Pain
: Pain should be a guide. Exercises should not significantly increase pain.
*
Individualization
: The protocol must be adapted to the individual patient's response, fracture stability, and co-morbidities. Osteoporotic bone, for example, may necessitate a more conservative progression.
*
Surgeon Communication
: Close communication between the surgeon and physical therapist is essential.
Summary of Key Literature / Guidelines
The management of proximal humerus fractures has been the subject of extensive research, with evolving consensus and ongoing debate regarding optimal treatment strategies, particularly for complex patterns in the elderly.
-
Non-Operative vs. Operative Management :
- The PROXIMAL trial (2015, BMJ ) was a landmark randomized controlled trial (RCT) comparing surgery (ORIF or hemiarthroplasty) with non-surgical treatment for displaced proximal humerus fractures in adults. It found no significant difference in patient-reported functional outcomes (Oxford Shoulder Score) at 2 years between the operative and non-operative groups, challenging the widespread use of surgery for these fractures.
- Critiques of PROXIMAL often point to heterogeneity in fracture types and surgical techniques, and potential limitations in power to detect differences in specific subgroups. Nevertheless, it underscored the importance of selecting operative candidates carefully and highlighted that non-operative management often yields acceptable results for many displaced fractures.
- Subsequent meta-analyses and systematic reviews have echoed this, suggesting that for many two- and three-part fractures, non-operative management can achieve similar functional outcomes to ORIF, albeit with potentially higher rates of malunion but fewer complications related to surgery.
-
Surgical Techniques (ORIF vs. Arthroplasty) :
- Locking Plate Osteosynthesis (LPO) : Has become the dominant technique for ORIF due to its angular stability, which is beneficial in osteopenic bone. Studies comparing LPO to conventional plating or tension band wiring have shown improved stability and lower rates of cutout, though complications like AVN, nonunion, and screw cutout remain concerns. The importance of medial calcar support (either through specific screw placement, impaction grafting, or an intramedullary fibular strut graft) to prevent varus collapse is emphasized across the literature.
- Hemiarthroplasty (HA) : Traditionally reserved for four-part fractures, head-splitting fractures, or fractures with a high risk of AVN, especially in the elderly. Success hinges on accurate tuberosity reattachment. Studies comparing HA to ORIF in elderly patients with four-part fractures often show similar functional outcomes but higher complication rates with ORIF.
- Reverse Total Shoulder Arthroplasty (rTSA) : Gaining increasing popularity, especially for displaced four-part fractures in osteopenic patients over 65-70 years, or when rotator cuff integrity is compromised. Studies indicate superior functional outcomes (especially active elevation) and lower reoperation rates compared to HA for comminuted fractures in this demographic, primarily due to bypassing the need for tuberosity healing. However, it carries its own set of potential complications, including glenoid loosening and infection.
-
Tuberosity Fixation :
- Regardless of the operative technique (ORIF or HA), robust fixation and healing of the tuberosities are paramount for restoring rotator cuff function and achieving good outcomes. Suture augmentation techniques (suture bridges, sutures through plate eyelets) are standard practice to enhance tuberosity stability.
-
Rehabilitation :
- Early, supervised rehabilitation with a focus on gradual progression of motion is crucial to prevent stiffness while protecting the healing fracture. Immobilization periods are tailored to fracture stability. There is a general consensus that protracted immobilization leads to worse outcomes.
-
Future Directions :
- Ongoing research focuses on refining indications for rTSA in younger elderly populations, optimizing locking plate designs and techniques, and developing patient-specific implants. The role of biomaterials and bone graft substitutes in enhancing fracture healing, especially in osteoporotic bone, continues to be explored. Functional outcomes and patient-reported measures are increasingly prioritized in research.
In summary, while non-operative management remains viable for a significant proportion of proximal humerus fractures, complex and displaced patterns often benefit from surgical intervention. The choice of surgery hinges on meticulous patient and fracture assessment, balancing the desire for anatomical restoration and functional recovery with the risks of complications. Modern approaches emphasize stable fixation, preservation of blood supply, robust tuberosity repair, and a structured rehabilitation program.
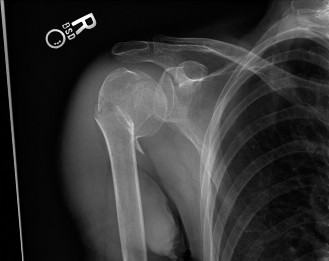
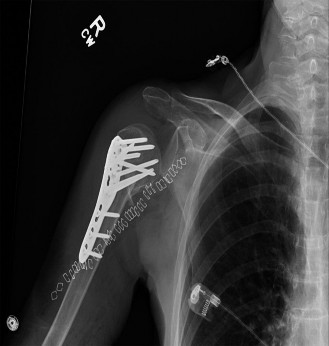
Clinical & Radiographic Imaging

