Scapulothoracic Bursitis: Unmasking a Mimic of Refractory Lateral Epicondylitis
Key Takeaway
Scapulothoracic bursitis diagnosis often involves a comprehensive physical exam, revealing tenderness, crepitus, and scapular dyskinesis, particularly after conservative treatments for conditions like lateral epicondylitis fail. MRI is crucial, demonstrating fluid and soft tissue thickening within the bursa, confirming the true origin of persistent pain in the scapulothoracic region.
Patient Presentation & History
A 48-year-old right-hand dominant male presented with a 14-month history of progressive right lateral elbow pain. He described the pain as dull aching, exacerbated by repetitive forearm rotation, gripping, and overhead activities, and occasionally radiating distally into the forearm and proximally towards the shoulder. The pain had significantly impacted his occupational duties as a carpenter and his recreational tennis activities.
Initial diagnosis elsewhere was refractory lateral epicondylitis. He had undergone multiple conservative treatments, including activity modification, non-steroidal anti-inflammatory drugs (NSAIDs), corticosteroid injections into the lateral epicondyle, and a 6-month course of physical therapy focusing on eccentric strengthening of the wrist extensors. These interventions provided transient, partial relief at best, with symptoms consistently recurring and worsening. There was no history of acute trauma to the elbow.
Further inquiry revealed a remote history (approximately 5 years prior) of a fall directly onto his right shoulder, which resulted in significant bruising but no documented fracture. Since then, he reported intermittent, mild discomfort along the medial border of his right scapula, often described as a "grinding" sensation during specific movements, which he attributed to muscle stiffness and had largely ignored due to the more dominant elbow pain. He denied any overt neurological symptoms such as numbness, tingling, or weakness in the hand or arm. He was a non-smoker, with no significant medical comorbidities.
Clinical Examination
Inspection
On static examination, the patient demonstrated subtle right shoulder droop and mild scapular protraction and abduction. During dynamic evaluation, a discernible dyskinesis of the right scapula was observed. Specifically, a type II scapular dyskinesis (inferior medial border prominence) was noted during the eccentric phase of arm elevation and a subtle increase in internal rotation of the scapula. No overt muscle atrophy was visible. No skin changes, erythema, or gross swelling were apparent around the elbow or shoulder.
Palpation
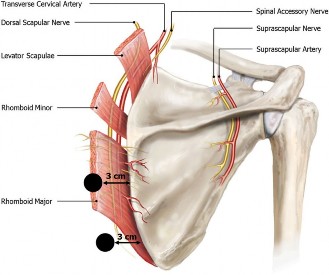
Localized tenderness was present over the lateral epicondyle, consistent with prior diagnoses. However, a more critical finding on thorough examination was significant tenderness upon deep palpation along the superomedial aspect of the scapular border and over the scapulothoracic interval. Palpable crepitus was elicited with passive scapular manipulation, particularly during protraction and retraction. The muscles of the shoulder girdle, notably the rhomboids and trapezius, exhibited diffuse tenderness and spasm. No palpable masses or bony abnormalities were detected.
Range of Motion
- Elbow: Full, pain-free active and passive range of motion. Resisted wrist extension and resisted supination elicited significant pain at the lateral epicondyle.
- Shoulder: Active and passive glenohumeral range of motion was full and pain-free. However, active elevation beyond 90 degrees was accompanied by compensatory scapular motion and a subtle "hitch" in the scapulohumeral rhythm, indicative of scapular dyskinesis.
- Scapulothoracic: Specific tests for scapular stability and control revealed deficits. The Scapular Assistance Test (SAT) provided partial relief of pain during active shoulder abduction, suggesting compromised scapular kinematics. A positive Wall Push-up Test demonstrated increased right scapular winging. Kibler's lateral slide test showed a significant difference ( >1.5 cm) in the resting position of the inferior angle of the scapula relative to the thoracic spine compared to the contralateral side.
Neurological/Vascular Assessment
Distal neurovascular status of the right upper extremity was intact. Sensation to light touch was normal throughout the radial, ulnar, and median nerve distributions. Motor strength was 5/5 in all major muscle groups distal to the elbow. Deep tendon reflexes (biceps, triceps, brachioradialis) were symmetrical and normal (2+). A comprehensive cervical spine examination was unremarkable, ruling out cervical radiculopathy as a primary pain generator. Radial tunnel syndrome tests were equivocal, with slight tenderness over the radial head but no clear motor deficits or specific provocative signs for posterior interosseous nerve (PIN) entrapment.
Imaging & Diagnostics
X-ray Findings
- Right Elbow: Anteroposterior (AP) and lateral views of the right elbow demonstrated mild degenerative changes at the lateral epicondyle, consistent with chronic lateral epicondylitis, but no acute bony pathology.
- Right Shoulder & Scapula: AP, lateral, and scapular Y-views of the right shoulder and scapula revealed no fractures, dislocations, or overt bony abnormalities. However, a subtle increase in the scapulothoracic interval was observed on the AP view compared to the contralateral side, suggesting potential soft tissue thickening or instability. No significant osteophytes or prominent bony spurs were noted along the medial scapular border or thoracic cage.
CT/MRI Indications
Given the persistent, refractory elbow symptoms despite localized treatment, and the new findings of scapular dyskinesis and palpable crepitus, further imaging focusing on the scapulothoracic interface was indicated to investigate the proximal origin of the symptoms.
-
MRI of the Right Shoulder and Scapulothoracic Region: This was the cornerstone diagnostic modality. The MRI demonstrated significant fluid signal and thickening of the soft tissues within the scapulothoracic bursa, consistent with scapulothoracic bursitis . Mild edema was noted in the surrounding rhomboid and serratus anterior musculature, indicative of chronic inflammatory changes and muscular strain. No rotator cuff tears or significant glenohumeral pathology were identified. Crucially, the MRI revealed no significant bony exostoses or other structural lesions that would typically cause snapping scapula syndrome, suggesting the bursitis was primarily inflammatory due to altered biomechanics.
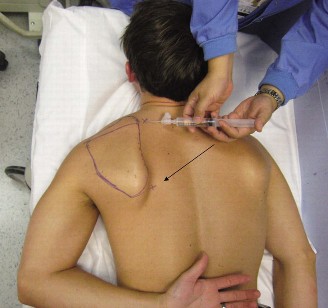
Figure 1: Coronal T2-weighted MRI demonstrating high signal intensity (arrow) within the scapulothoracic bursa, consistent with significant bursal fluid and inflammation.
Templating
Not applicable for this soft tissue pathology.
Differential Diagnosis
The presentation of chronic elbow pain, especially when refractory to conventional treatment, necessitates a comprehensive differential diagnosis that considers not only local pathology but also referred pain patterns and kinetic chain dysfunctions.
| Condition | Key Diagnostic Features | Differentiating Factors from Scapulothoracic Bursitis |
|---|---|---|
| Lateral Epicondylitis | Localized tenderness at lateral epicondyle, pain with resisted wrist extension/supination. | Absence of scapular dyskinesis, no tenderness/crepitus at scapulothoracic interface. MRI negative for scapulothoracic bursitis. |
| Posterior Interosseous Nerve (PIN) Entrapment | Deep, aching forearm pain, weakness of wrist/finger extensors (late stage), tenderness 4 cm distal to lateral epicondyle. | Pain typically localized to forearm. Sensory examination normal (PIN is purely motor). EMG/NCS may show denervation. Absence of scapulothoracic findings. |
| Cervical Radiculopathy (C5/C6) | Neck pain with radiation to shoulder/arm/elbow, dermatomal sensory changes, motor weakness in specific myotomes, positive Spurling's maneuver. | Positive neurological signs in neck/arm. MRI cervical spine shows nerve root compression. No specific scapulothoracic crepitus/tenderness. |
| Scapulothoracic Bursitis | Tenderness/crepitus along medial scapular border, scapular dyskinesis, pain with overhead/repetitive activities. MRI confirms bursal inflammation. | Present in this case as the primary driver of symptoms and biomechanical dysfunction. Elbow pain is often secondary or referred. |
| Scapular Dyskinesis | Abnormal scapulohumeral rhythm, winging/tipping of scapula, often associated with muscle imbalance (serratus anterior, rhomboids, trapezius weakness). | Primarily a movement dysfunction, often leads to secondary conditions like bursitis or impingement syndromes. Imaging negative for bursitis per se . |
| Snapping Scapula Syndrome | Auditory and/or palpable "snapping" or "grinding" with scapular motion. Can be bony (osteochondroma, Luschka's tubercle) or soft tissue (bursitis). | Specific bony lesions identified on X-ray/CT (if bony type). If soft tissue, indistinguishable from bursitis. |
| Rotator Cuff Pathology | Shoulder pain, weakness with active elevation/rotation, positive impingement signs, specific rotator cuff tests. MRI shows tendon tear/tendinopathy. | Shoulder-centric pain. While it can cause secondary scapular dyskinesis, the primary pathology is in the rotator cuff tendons. |
Surgical Decision Making & Classification
The decision for surgical intervention was predicated on:
1.
Failure of exhaustive conservative management:
The patient had undergone over a year of appropriate non-operative treatments for his presumed lateral epicondylitis with minimal, transient relief.
2.
Clear diagnostic shift:
The comprehensive evaluation, particularly the MRI findings, unequivocally identified significant scapulothoracic bursitis and associated scapular dyskinesis as a primary pathology, likely contributing to or causing the refractory elbow pain through altered kinetic chain mechanics and referred pain.
3.
Positive diagnostic injection:
A targeted injection of lidocaine and corticosteroid into the scapulothoracic bursa under ultrasound guidance provided significant, albeit temporary, relief of both the scapular and the patient's perceived "elbow" pain. This confirmed the bursal inflammation as a major pain generator.
4.
Functional Impairment:
The patient's pain significantly limited his occupational and recreational activities, leading to a diminished quality of life.
While there are no specific classification systems for scapulothoracic bursitis that dictate surgical management, the underlying scapular dyskinesis could be classified by Kibler types. In this case, a Type II dyskinesis (inferior medial border prominence) was noted. Surgical intervention was deemed necessary to address the chronic inflammation within the bursa and to debride any potential fibrotic tissue or irritants, thereby facilitating effective rehabilitation of scapular mechanics. The elbow symptoms were considered secondary to the proximal dysfunction.
Surgical Technique / Intervention
The primary intervention was an arthroscopic scapulothoracic bursectomy and debridement.
Patient Positioning
The patient was positioned in a lateral decubitus position with the affected right arm prepped and draped free, allowing full manipulation. A beanbag was used to stabilize the torso, and the arm was draped over a padded arm rest, allowing for various degrees of abduction and flexion. This position provided excellent access to the scapulothoracic interval.
Approach
A posterior arthroscopic approach was utilized. Two primary portals were established:
1.
Inferior Portal:
Established first, approximately 2-3 cm superior and 2 cm medial to the inferior angle of the scapula. This portal served as the primary viewing portal.
2.
Superior Portal:
Established under arthroscopic visualization, approximately 2-3 cm superior to the superomedial angle of the scapula. This portal served as the working portal.
Fluid extravasation is a known concern in this region, thus, precise portal placement and careful management of pump pressure were paramount.
Reduction Techniques / Debridement
- Initial Visualization: Upon entering the scapulothoracic space, significant hypertrophic and inflamed bursal tissue was identified. The medial border of the scapula and the underlying posterior thoracic cage (ribs and intercostal musculature) were clearly visualized. The serratus anterior muscle was also observed.
- Bursectomy: A motorized shaver was introduced through the superior working portal. The hypertrophic, inflamed bursal tissue was systematically debrided. Care was taken to remove all inflamed synovium, ensuring adequate decompression of the space.
- Identification of Irritants: During debridement, no significant bony spurs or osteochondromas were found along the medial scapular border or the posterolateral chest wall that would contribute to a "snapping" phenomenon. The primary pathology was confirmed to be chronic inflammation and thickening of the bursa.
- Debridement of Fibrotic Tissue: Any evident fibrotic bands or adhesions within the bursa were meticulously released to ensure free gliding of the scapula over the chest wall.
- Hemostasis: Prior to closure, thorough electrocautery was used to achieve hemostasis.

Figure 2: Intra-operative endoscopic view during a scapulothoracic bursectomy. The shaver is debriding hypertrophic, inflamed bursal tissue (B) along the medial border of the scapula (S), with the underlying serratus anterior muscle (SA) visible.
Fixation Construct
Not applicable for this soft tissue procedure.
Closure
Portals were closed with simple sutures (e.g., 3-0 nylon), and a sterile dressing was applied. A gentle compressive dressing was applied to minimize post-operative swelling.
Post-Operative Protocol & Rehabilitation
The post-operative protocol was designed to facilitate early return to motion, progressively strengthen the scapular stabilizers, and integrate the entire upper extremity kinetic chain.
Phase I: Immediate Post-operative (Weeks 0-2)
- Immobilization: Arm in a sling for comfort only, typically for the first 3-5 days. Encouraged to remove for exercises.
- Pain Management: Oral analgesics and NSAIDs as needed.
-
Early Motion:
- Scapular ROM: Gentle passive and active-assisted scapular protraction/retraction, elevation/depression exercises (e.g., scapular shrugs, scapular clocks).
- Shoulder ROM: Pendulum exercises, passive range of motion of the glenohumeral joint in all planes, ensuring no provocative movements of the scapula.
- Elbow/Wrist/Hand ROM: Active range of motion exercises to prevent stiffness.
- Manual Therapy: Gentle soft tissue mobilization around the scapulothoracic region, avoiding direct pressure on the surgical sites.
Phase II: Intermediate Strengthening (Weeks 2-6)
- Focus: Regaining full, non-painful active scapular and shoulder range of motion. Initiating scapular stabilization and rotator cuff strengthening.
-
Scapular Stabilization:
- Isometrics for serratus anterior (wall push-ups against light resistance), rhomboids (scapular squeezes), and trapezius (shrugs, horizontal abduction).
- Progress to dynamic exercises with light resistance: prone Ys, Ts, Ws.
- Emphasis on establishing proper scapulohumeral rhythm.
- Rotator Cuff Strengthening: Light resistance internal and external rotation, scaption exercises.
- Core Stability: Initiation of core strengthening exercises to improve proximal stability, which is crucial for overall kinetic chain function.
- Elbow/Forearm: Continued gentle strengthening of forearm musculature, avoiding heavy gripping or provocative elbow movements.
Phase III: Advanced Strengthening & Return to Activity (Weeks 6-12+)
- Focus: Progressive strengthening of the entire upper kinetic chain, functional retraining, and sport-specific drills.
- Advanced Scapular Strengthening: Progress resistance for serratus anterior (dynamic push-ups, punch-outs), rhomboids, and trapezius. Plyometric exercises if appropriate for activity level.
- Proprioception and Neuromuscular Control: Closed kinetic chain exercises, rhythmic stabilization drills.
- Functional Progression: Gradual introduction of activity-specific movements, incorporating proper biomechanics and kinetic chain principles. For the carpenter, this would involve simulated tool use; for the tennis player, progressive racket drills.
- Sport/Work-Specific Drills: Progressive return to demanding activities, with meticulous attention to scapular mechanics and avoidance of compensatory patterns.
- Ergonomic Assessment: Review of occupational and recreational ergonomics to prevent recurrence.
Throughout rehabilitation, close communication between the surgeon and physical therapist is essential to tailor the program to the patient's progress and address any residual symptoms or biomechanical deficits. The patient's initial elbow symptoms resolved concurrently with the improved scapulothoracic function, underscoring the interconnectedness of the upper limb kinetic chain.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Think Proximal for Distal Symptoms: Refractory distal upper extremity pain, particularly at the elbow, should always prompt a thorough evaluation of the entire kinetic chain, especially the shoulder girdle and scapulothoracic region. Scapulothoracic dysfunction can manifest as referred pain or altered biomechanics contributing to distal pathology.
- Comprehensive Clinical Examination is Key: Beyond standard elbow evaluations, meticulous assessment of scapular posture, dynamic movement patterns (scapulohumeral rhythm, winging, tipping), and palpation of the scapulothoracic interface for crepitus or tenderness is paramount. Special tests like the Scapular Assistance Test and Wall Push-up Test provide invaluable information.
- MRI as the Definitive Soft Tissue Diagnostic: While X-rays rule out gross bony pathology, MRI is indispensable for visualizing soft tissue inflammation, identifying bursal fluid, and ruling out other intrinsic shoulder pathologies or specific bony lesions causing snapping.
- Diagnostic Injection Confirms Pain Source: A precise, image-guided injection of anesthetic and corticosteroid into the scapulothoracic bursa can be both diagnostic and therapeutic, confirming the bursitis as a primary pain generator.
- Holistic Rehabilitation: Surgical decompression addresses the local inflammation, but long-term success hinges on a comprehensive post-operative rehabilitation program focused on restoring scapular stabilizer strength, optimal scapulohumeral rhythm, and kinetic chain control. Address underlying muscle imbalances (e.g., weak serratus anterior, tight pectoralis minor).
Pitfalls
- Tunnel Vision on the Symptom Location: Focusing solely on the elbow as the source of pain and repeatedly treating it without addressing the underlying proximal dysfunction. This leads to recurrent symptoms and patient dissatisfaction.
- Missing Scapular Dyskinesis: Failure to recognize subtle scapular dyskinesis, which can be the mechanical culprit driving bursal irritation and altered upper extremity biomechanics.
- Inadequate Imaging: Relying solely on X-rays or only imaging the elbow, thereby missing critical soft tissue pathology in the scapulothoracic region.
- Ignoring Concomitant Pathology: While less common, overlooking primary bony lesions (e.g., osteochondroma, Sprengel's deformity) or other causes of snapping scapula that may require specific excision.
- Insufficient Post-operative Rehabilitation: Surgical bursectomy is only one component. Neglecting the structured, progressive rehabilitation of the scapular musculature will likely result in incomplete recovery or recurrence of symptoms. The entire kinetic chain must be re-educated.
- Overlooking Cervical Spine Pathology: Always exclude cervical radiculopathy as a potential source of referred upper extremity pain, especially in complex or recalcitrant cases.
Clinical & Radiographic Imaging

You Might Also Like