Complex Intra-Articular Distal Humerus Fracture: Diagnostic & Surgical Challenges
Key Takeaway
Complex comminuted intra-articular distal humerus fractures are diagnosed through detailed clinical examination for pain, deformity, and neurovascular status. Imaging is critical: X-rays reveal fracture patterns, while CT scans with 3D reconstructions precisely delineate fragment size, displacement, articular involvement, and bone loss, guiding comprehensive pre-operative planning for these high-energy elbow traumas.
Patient Presentation & History
Good morning, everyone. Today, we'll delve into a complex elbow trauma case, focusing on the diagnostic and surgical challenges of a comminuted intra-articular distal humerus fracture.
Our patient is a 58-year-old right-hand dominant male who presented to the emergency department after a fall from a height of approximately 8 feet while working on a ladder. He landed directly on his outstretched right arm. He reported immediate, severe pain, inability to move his elbow, and noticeable deformity.
His medical history includes well-controlled hypertension and Type 2 Diabetes Mellitus, managed with oral hypoglycemics. He denies any history of osteoporosis or prior elbow injuries. He is an active, independent individual, working as a carpenter, which places significant functional demands on his upper extremities. He is a non-smoker and reports occasional alcohol consumption. The mechanism of injury suggests high-energy trauma, necessitating a thorough evaluation for associated injuries.
Clinical Examination
Upon presentation, the patient was in significant distress from pain.
- Inspection: The right elbow presented with gross swelling, significant ecchymosis extending proximally to the distal humerus and distally into the forearm. There was a palpable deformity around the elbow joint, particularly evident posteriorly. The skin overlying the joint was intact, without any open wounds, tenting, or signs of impending compartment syndrome.
- Palpation: Diffuse tenderness was elicited over the entire distal humerus, olecranon, and radial head. Palpation revealed crepitus with any attempt at passive motion, indicating significant bony disruption. The medial and lateral epicondyles were difficult to delineate due to swelling and comminution.
- Range of Motion (ROM): Both active and passive range of motion of the elbow were severely limited and exquisitely painful. The patient guarded against any movement. Attempts at gentle flexion and extension yielded only a few degrees of motion, and pronation/supination were similarly restricted.
- Neurological Assessment: A meticulous neurological examination was performed given the proximity of major nerves to the elbow joint. Sensation was intact to light touch in all dermatomes of the hand and forearm, including the median (thumb, index, middle finger radial aspect), ulnar (little finger, ring finger ulnar aspect), and radial nerve distributions (dorsal first web space). Motor function was difficult to assess accurately due to pain, but gross motor power for wrist flexion, extension, and finger movements appeared preserved. Specifically, intrinsic hand muscles (ulnar nerve) and wrist extensors (radial nerve) could be gently tested and showed no gross deficits. However, the ulnar nerve was identified as being particularly at risk in this type of injury, necessitating careful monitoring.
- Vascular Assessment: Radial and ulnar arterial pulses at the wrist were palpable, strong, and symmetrical compared to the contralateral limb. Capillary refill in all digits was brisk, less than 2 seconds. No signs suggestive of arterial compromise or evolving compartment syndrome were observed, although serial assessments were planned.
Imaging & Diagnostics
Following the initial clinical assessment, imaging studies were promptly obtained to characterize the injury.
-
X-rays:
- Antero-posterior (AP) and lateral views of the elbow were the initial radiographs. These revealed a highly comminuted, intra-articular fracture of the distal humerus.
- The AP view demonstrated significant disruption of both the medial and lateral columns of the distal humerus, with a clear supracondylar component and extension into the trochlea and capitellum. The fracture line extended into the coronoid fossa and olecranon fossa.
- The lateral view showed posterior displacement and angulation of the distal fragments relative to the humeral shaft. There was clear involvement of the articular surface, making it an AO/OTA 13-C type fracture, highly suggestive of a C3 subtype given the extensive comminution. Oblique views were difficult to obtain due to patient pain but would typically be employed for further delineation of fragment morphology.
-
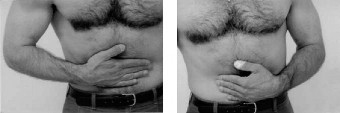
Computed Tomography (CT) Scan:
- Given the complexity and intra-articular nature of the fracture seen on plain radiographs, a CT scan with 3D reconstructions was deemed essential for comprehensive pre-operative planning.
- The CT scan confirmed the extensive intra-articular comminution, involving both the trochlea and capitellum. It clearly delineated the dissociation of the medial and lateral columns from the humeral shaft and from each other.
- Axial, coronal, and sagittal reconstructions provided invaluable information regarding fragment size, displacement, rotation, and articular step-off. 3D reconstructions were particularly beneficial in visualizing the overall fracture morphology and planning the sequence of reduction and fixation. There was significant bone loss noted in areas of severe comminution.
- The CT scan ruled out any associated radial head or coronoid fractures, which can often accompany distal humerus injuries.

-
Magnetic Resonance Imaging (MRI):
- An MRI was not indicated in the acute setting for primary surgical planning, as the critical bony anatomy was sufficiently characterized by CT. MRI may be considered in cases of persistent neurovascular deficits after reduction, or if there is concern for extensive ligamentous or soft tissue damage not evident on other imaging, but this was not the primary concern here.
-
Templating:
- Pre-operative templating was performed meticulously using the CT images and 3D reconstructions. This involved estimating appropriate plate lengths, screw sizes, and determining the optimal configuration of the dual plating system (e.g., parallel vs. orthogonal construct, number of screws required for adequate fixation in each column). This step is crucial for anticipating challenges and minimizing intraoperative surprises.
Differential Diagnosis
The clinical presentation of a severely painful, swollen, and deformed elbow following high-energy trauma necessitates a broad differential diagnosis. However, detailed imaging rapidly narrows the possibilities.
| Feature | Complex Distal Humerus Fracture (AO/OTA 13-C3) | Terrible Triad Injury (Elbow Dislocation, Radial Head Fracture, Coronoid Fracture) | Monteggia Fracture-Dislocation (Proximal Ulna Fracture, Radial Head Dislocation) | High-Energy Olecranon Fracture with Intra-articular Extension |
|---|---|---|---|---|
| Mechanism | High-energy, direct impact, or fall onto outstretched hand (FOOSH) | FOOSH, valgus/supination injury | Direct blow to posterior elbow or FOOSH with hyperpronation | Direct trauma, FOOSH |
| Clinical Presentation | Severe pain, gross swelling, significant deformity, crepitus, loss of ROM | Severe pain, marked swelling, obvious dislocation, limited ROM | Pain, swelling, palpable ulna deformity, limited ROM, radial head tenderness | Severe pain, swelling, tenderness over olecranon, limited ROM |
| Plain Radiographs | Comminuted intra-articular distal humerus fracture (supracondylar, epicondylar, trochlear, capitellar involvement), column dissociation | Elbow dislocation (typically posterior), radial head fracture (often comminuted), coronoid tip avulsion/fracture | Ulnar shaft fracture (various patterns), anterior/posterior dislocation of radial head | Olecranon fracture (transverse, oblique, comminuted), often intra-articular |
| CT Scan Findings | Extensive intra-articular comminution of trochlea/capitellum, medial/lateral column fractures, metaphyseal extension | Confirms dislocation, precise radial head (Mason classification) and coronoid (Regan & Morrey classification) fracture patterns | Confirms ulna fracture, degree of radial head displacement | Detailed fracture pattern, comminution, articular involvement |
| Primary Pathoanatomy | Bony disruption of distal humerus articular and metaphyseal segments | Bony (radial head, coronoid) and ligamentous (MCL, LCL) disruption, joint instability | Ulnar diaphyseal fracture and associated radio-capitellar joint instability | Fracture of the olecranon process, often involving the trochlear notch |
| Surgical Management | ORIF with dual plating (medial and lateral columns), articular reconstruction | ORIF radial head/coronoid, LCL repair/reconstruction, +/- MCL repair, external fixation for stability | ORIF ulna, reduction of radial head (often stable after ulna fixation), +/- annular ligament repair | ORIF (tension band, plate and screws) |
| Potential Complications | Stiffness, HO, nonunion/malunion, ulnar nerve neuropathy, infection, hardware failure | Stiffness, HO, chronic instability, recurrent dislocation, ulnar nerve neuropathy | Nonunion, malunion, radial head instability, posterior interosseous nerve palsy | Stiffness, nonunion, hardware irritation, ulnar nerve neuropathy |
Surgical Decision Making & Classification
Operative vs. Non-operative Management
The decision to proceed with operative management for this patient's distal humerus fracture was straightforward and unequivocally indicated.
*
Fracture Type:
The fracture was classified as an AO/OTA 13-C3 injury – a complete articular, multifragmentary fracture of the distal humerus involving both the medial and lateral columns. This implies extensive disruption of the articular surface and significant displacement.
*
Goals of Treatment:
The primary goals for managing such complex injuries are:
1. Anatomical reduction and stable fixation of the articular surface to restore a smooth joint congruence.
2. Restoration of overall elbow stability.
3. Allowing for early, controlled range of motion to prevent post-traumatic stiffness, which is a common and debilitating complication of elbow fractures.
4. Protection of neurovascular structures.
*
Non-operative Limitations:
Non-operative treatment for AO/OTA C-type distal humerus fractures typically results in severe functional limitations, including gross stiffness, malunion, nonunion, chronic pain, and early degenerative changes. It is generally reserved for frail, non-ambulatory patients with very low functional demands, or those with absolute contraindications to surgery. Our patient's age, activity level, and functional demands as a carpenter made non-operative treatment unacceptable.
Classification Systems
-
AO/OTA Classification:
As previously mentioned, this fracture falls under the
AO/OTA 13-C3
designation:
- 13: Denotes distal humerus.
- C: Signifies a complete articular fracture, meaning the fracture extends into the articular surface and separates the articular segment from the diaphysis.
- 3: Indicates a multifragmentary articular and multifragmentary metaphyseal fracture, representing the most complex and comminuted form of distal humerus fracture.
- Bryan and Morrey Classification: While less commonly used than AO/OTA for overall fracture pattern, this system can provide further descriptive insight into the configuration of the articular split, such as T-type, Y-type, or H-type fractures. The extensive comminution in our case made it a complex H-type or comminuted T-type pattern.
- Jupiter Classification: Focuses on column involvement (medial and lateral). Our patient presented with a fracture involving both columns.
The collective understanding from these classifications and imaging underscored the need for open reduction and internal fixation (ORIF) to achieve a stable, anatomically reduced construct that could withstand early rehabilitation protocols.
Surgical Technique / Intervention
The surgery was performed approximately 48 hours after the injury to allow for initial soft tissue swelling to subside and for thorough pre-operative planning.
- Anesthesia: General anesthesia combined with a regional interscalene brachial plexus block was utilized for excellent perioperative analgesia and intraoperative muscle relaxation.
-
Patient Positioning: The patient was positioned in a prone position on the operating table, with the right arm draped freely over a padded arm board, allowing for full flexion and extension of the elbow. This setup provides excellent access to the posterior aspect of the elbow and allows for manipulation of the forearm for pronation/supination. A pneumatic tourniquet was applied to the upper arm.
-
Surgical Approach: A posterior approach with an olecranon osteotomy was chosen. This approach provides optimal exposure of the entire distal humerus articular surface and both columns, which is paramount for highly comminuted C3 type fractures.
- A straight posterior skin incision was made, centered over the olecranon.
- The ulnar nerve was identified proximally in the cubital tunnel, carefully dissected free, and gently transposed anteriorly throughout the procedure, ensuring its protection. This is a critical step to prevent iatrogenic injury.
- A chevron-type olecranon osteotomy was performed with an oscillating saw, approximately 2 cm distal to the tip of the olecranon. The osteotomy fragment, along with its triceps attachment, was retracted proximally, exposing the posterior aspect of the distal humerus and the elbow joint.
- The elbow joint capsule was incised longitudinally to fully expose the fracture fragments.
-
Fracture Reduction:
- The primary goal was to reconstruct the articular surface first. This involved meticulous identification and reduction of the trochlear and capitellar fragments. Small K-wires were used temporarily to hold these fragments together, often in conjunction with headless compression screws or lag screws if fragment size allowed. The goal was to restore the anatomical congruity of the articular block.
- Once the articular block was reconstructed, it was reduced to the humeral metaphysis and diaphysis. This was achieved by carefully applying traction and rotational forces, ensuring correct alignment in terms of length, rotation, and valgus/varus. The intact contralateral elbow films served as a guide.
- The medial and lateral columns were then anatomically reduced to the articular block and to the humeral shaft. Direct reduction techniques using clamps and bone hooks were employed.
-
Fixation Construct:
- Dual plating was utilized, specifically pre-contoured locking plates for the distal humerus. The "column theory" dictates stable fixation of both medial and lateral columns.
- Lateral Column Fixation: A long, pre-contoured locking plate was applied along the posterolateral aspect of the lateral column, extending well proximally onto the humeral shaft.
- Medial Column Fixation: A second, pre-contoured locking plate was applied along the medial column, typically on the medial aspect.
- Orthogonal Plating: In this case, an orthogonal plating configuration was chosen, with the lateral plate applied posterolaterally and the medial plate applied medially. This provides a strong biomechanical construct, resisting forces in multiple planes, and often allows for more screws in the articular fragments compared to parallel plating.
- Screws were directed through the plates, ensuring capture of as many articular fragments as possible, and engaging the opposite cortex for bicortical purchase where feasible. Locking screws were used in the distal fragments to maximize stability in comminuted bone. Interfragmentary compression screws were applied where possible, independent of the plates, to further compress specific fracture lines.
- At least three bicortical locking screws were placed in the distal fragments and at least three bicortical locking screws were placed proximally in the humeral shaft for each plate to achieve robust fixation.

-
Bone Grafting: Due to areas of significant comminution and potential bone voids after reduction, cancellous autograft harvested from the ipsilateral olecranon (prior to osteotomy repair) or iliac crest was considered. In this case, local bone fragments were carefully preserved and packed into any defects, along with synthetic bone graft material, to augment healing.
-
Closure:
- The olecranon osteotomy was meticulously repaired using a tension band wiring technique (two K-wires and an 18-gauge wire) to ensure stable fixation and allow for early triceps activation.
- The joint capsule was loosely repaired.
- The ulnar nerve was assessed for any tension or compression after fixation and was typically transposed anteriorly beneath the flexor-pronator mass to prevent post-operative irritation.
- Layered closure of the subcutaneous tissues and skin. A sterile dressing was applied, followed by a well-padded posterior splint holding the elbow in approximately 90 degrees of flexion.
Post-Operative Protocol & Rehabilitation
The success of ORIF for complex distal humerus fractures is highly dependent on a well-structured and aggressive post-operative rehabilitation protocol.
-
Initial Post-Operative Period (Days 0-7):
- Immobilization: The elbow was immobilized in a well-padded posterior splint at 90 degrees of flexion for approximately 3-5 days to allow for initial soft tissue healing and swelling reduction.
- Pain Management: Aggressive pain management, including multimodal analgesia and continued use of the regional block if appropriate.
- Neurovascular Monitoring: Strict monitoring of neurovascular status, particularly ulnar nerve function.
-
Early Motion Phase (Weeks 1-6):
- Splint Removal: The bulky splint was typically removed around day 5-7, and a hinged elbow brace was fitted.
- CPM Machine: Initiation of Continuous Passive Motion (CPM) machine for 4-6 hours daily, gradually increasing arc of motion as tolerated.
- Physical Therapy: Immediate referral to an experienced hand and elbow therapist. Active-assisted range of motion (AAROM) exercises were initiated, focusing on gentle flexion, extension, pronation, and supination within a pain-free range. The brace settings were adjusted weekly to allow for increasing arcs of motion (e.g., initial 30-90 degrees, gradually progressing to 0-140 degrees).
- Goals: Prevent stiffness, improve circulation, and maintain soft tissue mobility. No active strengthening during this phase.
-
Intermediate Phase (Weeks 6-12):
- Radiographic Assessment: Follow-up X-rays at 6 weeks to assess for early signs of union and hardware integrity.
- Active Range of Motion (AROM): Progress from AAROM to full AROM as tolerated, continuing brace use for protection during activities of daily living and sleep.
- Gentle Strengthening: Isometric exercises for elbow flexors, extensors, pronators, and supinators were initiated. Light resistance band exercises, focusing on muscular endurance rather than heavy lifting.
- Goals: Restore functional range of motion (aiming for 30-130 degrees flexion/extension and 50-50 degrees pronation/supination), improve early strength.
-
Advanced Strengthening & Return to Activity (Weeks 12-24+):
- Radiographic Union: Further X-rays at 10-12 weeks to confirm progressive radiographic union. The brace may be weaned off as stability and confidence improve.
- Progressive Resistance: Gradual progression to light, then moderate, resistance exercises. Focus on building strength and endurance.
- Proprioception and Dexterity: Incorporate specific exercises to improve proprioception and fine motor control.
- Activity-Specific Training: For a carpenter, this would involve simulating work-related tasks, gradually increasing load and complexity.
- Return to Work/Sport: Typically, return to light duty may be possible around 4-6 months, with full return to heavy labor or impact sports requiring 6-12 months, contingent on complete radiographic union and full strength recovery.
-
Potential Complications & Management:
- Stiffness: The most common complication. Aggressive therapy is crucial. If conservative measures fail, serial casting or dynamic splinting may be used. Surgical intervention (capsulectomy) may be considered after 6-12 months if a functional arc of motion is not achieved.
- Heterotopic Ossification (HO): Prophylaxis with NSAIDs (e.g., Indomethacin) for 3-6 weeks post-operatively, especially in high-risk patients (e.g., TBI, spinal cord injury, prolonged surgery, burns). Low-dose radiation therapy is an alternative for very high-risk cases.
- Ulnar Nerve Neuropathy: Can occur from intraoperative injury, post-operative swelling, or scarring. Management ranges from observation to neurolysis or revision anterior transposition.
- Nonunion/Malunion: Rare with stable fixation but may require revision surgery.
- Hardware Failure/Irritation: If symptomatic, hardware removal may be indicated after complete union (typically 12-18 months post-op).
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls
- Pre-operative Planning is Paramount: Thorough analysis of CT scans (including 3D reconstructions) is essential to understand the complex fracture pattern, plan plate placement, and anticipate challenges. Templating helps choose appropriate hardware.
- Articular Reconstruction First: Always prioritize anatomical reduction and fixation of the articular segment (trochlea and capitellum) before connecting it to the humeral metaphysis/diaphysis. The "bag of bones" technique for articular fragments can be useful.
- Ulnar Nerve Management: Meticulous identification, isolation, and anterior transposition of the ulnar nerve are mandatory to prevent iatrogenic injury and post-operative irritation. This should be one of the very first steps after exposure.
- Stable Dual Plating: Utilize two plates (medial and lateral columns) for robust fixation. Pre-contoured locking plates are preferred for their biomechanical advantage in comminuted, osteoporotic bone. Orthogonal plating often provides superior stability to parallel plating.
- Early Motion: Begin controlled, early range of motion as soon as soft tissues allow (typically within 3-7 days) to prevent debilitating stiffness. This requires a strong, stable surgical construct.
- Bone Grafting: Don't hesitate to use autograft or allograft for significant bone voids, especially in the metaphysis, to augment healing and prevent collapse.
- Experience with Approaches: Be proficient with various posterior approaches (e.g., olecranon osteotomy, triceps-sparing/reflecting) to choose the best one for exposure tailored to the fracture pattern.
Pitfalls
- Inadequate Visualization: Attempting to reconstruct a complex intra-articular fracture through a limited approach, leading to malreduction of the articular surface and poor outcomes. The olecranon osteotomy, while adding another fixation, provides unparalleled exposure.
- Insufficient Fixation: Using only one plate or inadequate screws, leading to construct failure, loss of reduction, and nonunion, especially in osteoporotic bone. Suboptimal screw length or purchase can also compromise stability.
- Ignoring the Ulnar Nerve: Failing to identify, protect, or transpose the ulnar nerve, resulting in post-operative neuropathy. The ulnar nerve is highly vulnerable.
- Aggressive Early Passive ROM without Stable Fixation: While early motion is key, it must be balanced with the stability of the fixation. Too aggressive motion with an unstable construct can lead to loss of reduction and hardware failure.
- Failure to Address Heterotopic Ossification (HO): Not instituting prophylaxis in high-risk patients can lead to severe HO, which significantly limits range of motion.
- Neglecting Post-operative Stiffness: Failing to engage the patient in an aggressive and supervised physical therapy program, or not addressing early signs of stiffness proactively, which can result in long-term functional deficits.
- Improper Reduction of Articular Surface: Even slight incongruity (step-off > 2mm) of the articular surface can lead to post-traumatic arthritis and pain. The articular block must be perfectly restored.
- Poor Soft Tissue Handling: Excessive retraction, devascularization, or damage to the soft tissue envelope can increase the risk of infection and compromise healing.
Thank you. I am open to any questions.
Clinical & Radiographic Imaging

You Might Also Like