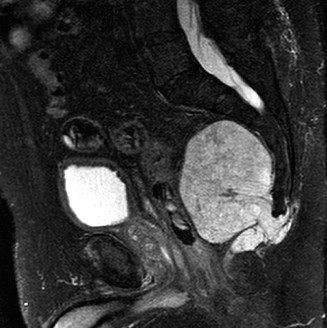
Comprehensive Management of Transverse Plus Posterior Wall Acetabular Fractures: A Case Study
Key Takeaway
A Transverse plus Posterior Wall Acetabular Fracture, often from high-energy trauma, involves a fracture line traversing the acetabulum (transverse component) and a significant posterior wall fragment. Diagnosis relies on detailed clinical examination, orthogonal radiographs, and crucial CT scans with 3D reconstructions to characterize fracture displacement, articular involvement, and guide pre-operative planning, especially after hip dislocation reduction.
Patient Presentation & History
A 42-year-old male, previously fit and active with no significant past medical history, presented to the emergency department following a high-energy motor vehicle accident. He was an unrestrained front-seat passenger involved in a head-on collision, resulting in a direct impact of his right knee against the dashboard. Initial pre-hospital assessment revealed a GCS of 15, stable vital signs, and isolated right hip pain. There was no loss of consciousness or other obvious major trauma.
Upon arrival, the patient complained of severe, incapacitating pain in his right hip and inability to bear weight. He denied paresthesia or weakness distally. His past medical history was unremarkable, with no known allergies and no regular medications. He was a non-smoker and consumed alcohol socially. Pre-injury functional status was independent ambulation without aids, engaging in regular recreational sports.
Clinical Examination
Upon initial assessment, the patient was alert and oriented. General systemic examination revealed stable hemodynamics. Inspection of the right lower limb demonstrated a visibly shortened, internally rotated, and adducted posture of the right hip, consistent with a posterior hip dislocation. Significant swelling and ecchymosis were noted around the greater trochanter and posterior buttock. No open wounds or skin tenting were present.
Palpation elicited exquisite tenderness globally around the right hip joint, particularly over the greater trochanter, posterior aspect of the iliac wing, and ischial tuberosity. The pelvis was stable to anterior-posterior compression and lateral distraction.
Active and passive range of motion of the right hip was severely restricted and painful. Attempted flexion, abduction, and external rotation were met with guarding and intense discomfort.
A comprehensive neurological examination was performed. Distal pulses (femoral, popliteal, dorsalis pedis, posterior tibial) were all palpable, strong, and symmetrical with the contralateral limb. Capillary refill was brisk. Sensory examination revealed intact sensation to light touch and pinprick throughout the dermatomes of the right lower extremity. Motor examination demonstrated full strength (5/5) in ankle dorsiflexion, plantarflexion, toe extension, and hip flexion, abduction, adduction, and knee extension. Of note, specific testing for sciatic nerve integrity, including assessment of hamstring strength and sensation in the peroneal and tibial distributions, was meticulously performed and found to be intact, a critical finding in posterior hip dislocations.
No other gross deformities or injuries were identified on a rapid secondary survey.
Imaging & Diagnostics
Initial imaging in the emergency department commenced with standard orthogonal radiographs.
-
Anteroposterior (AP) Pelvis Radiograph: Demonstrated a right posterior hip dislocation with an associated acetabular fracture. The femoral head appeared congruent in the dislocated position, but a large posterior wall fragment was evident, and there was suspicion of involvement of the posterior column. The fracture lines extended superiorly into the posterior aspect of the ilium. The tear-drop sign was disrupted, and the ilioischial line was involved.

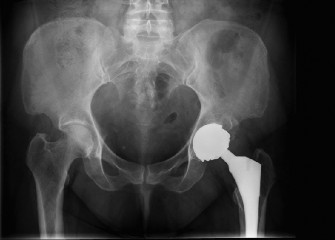
Pre-operative AP pelvis radiograph demonstrating a right posterior hip dislocation with an associated acetabular fracture involving the posterior wall and column, with superior extension into the posterior ilium. -
Judet Views (Iliac Oblique and Obturator Oblique):
- Iliac Oblique View: Confirmed disruption of the posterior column and posterior wall. It provided better visualization of the anterior column, which appeared intact in its entirety, and the anterior wall. The iliac wing component of the fracture was also better delineated.
- Obturator Oblique View: Clearly demonstrated the extent of the posterior column fracture extending into the ischium, with displacement. The anterior column and anterior wall were well-visualized and appeared undisplaced. The "spur sign," indicative of an associated both column fracture, was intact, confirming that this was not an associated both column injury. The fracture pattern was initially categorized as a Transverse plus Posterior Wall fracture, with a significant posterior column component.
-
Computed Tomography (CT) Scan with 3D Reconstructions: Following closed reduction of the hip dislocation (which was performed under conscious sedation and resulted in a stable reduction), a CT scan was obtained. This was crucial for detailed characterization of the complex fracture pattern. The CT scan confirmed a Transverse plus Posterior Wall Acetabular Fracture (Letournel & Judet classification).
- Transverse Component: The fracture line traversed the acetabulum from the greater sciatic notch to the pubic ramus, separating the superior weight-bearing dome from the inferior portion. This component was significantly displaced.
- Posterior Wall Component: A large, comminuted posterior wall fragment was present, involving approximately 60% of the posterior wall, and there was a significant marginal impaction injury to the posterosuperior articular cartilage of the acetabulum.
- Intra-articular Fragments: Several small osteochondral fragments were identified within the joint space, particularly in the posteroinferior aspect, suggesting articular surface damage.
- Femoral Head: A mild impaction injury to the posterosuperior aspect of the femoral head was noted, but no discrete femoral head fracture (Pipkin classification) was present.
- Quadrilateral Plate: The medial wall (quadrilateral plate) was intact, but significant medialization of the transverse component was observed.
Templating and Pre-operative Planning:
The CT scan with 3D reconstructions was essential for detailed pre-operative planning. This involved:
* Identifying the primary fracture lines and fragments.
* Determining the displacement and rotation of fragments.
* Estimating the size and morphology of plates required (e.g., specific posterior column plates, reconstruction plates).
* Planning screw trajectories to avoid articular penetration and nerve injury (e.g., sciatic nerve, superior gluteal neurovascular bundle).
* Anticipating the need for bone grafting for impacted areas.
* Selecting the optimal surgical approach(es). Given the significant posterior wall and transverse component displacement, a Kocher-Langenbeck approach was planned, with potential for an extensile approach if reduction proved impossible via standard exposure.
Differential Diagnosis
The presentation of a high-energy hip injury requires careful consideration of various complex fracture patterns involving the acetabulum and proximal femur.
| Feature | Transverse + Posterior Wall Acetabular Fracture (Proposed Case) | Associated Both Column Acetabular Fracture | Pipkin Type IV Femoral Head Fracture (with Acetabular Fracture) | High-Energy Proximal Femoral Fracture (e.g., Subtrochanteric) |
|---|---|---|---|---|
| Definition | Fracture traversing the acetabulum (transverse), combined with a posterior wall fragment. | Fracture separating both columns from the intact iliac wing. | Femoral head fracture with an associated acetabular fracture. | Fracture of the proximal femur, typically below the lesser trochanter. |
| Mechanism of Injury | High-energy axial load with hip in flexion/adduction; dashboard injury leading to posterior dislocation. | High-energy axial load with abduction or adduction component, often a direct lateral force. | High-energy axial load with flexion/adduction, femoral head impacts acetabulum. | High-energy direct trauma to the lateral thigh, or indirect rotational forces. |
| Clinical Presentation | Severe hip pain, shortened/internally rotated limb (if dislocated), possible sciatic neuropathy. | Severe hip pain, instability, possible limb shortening/rotation, sciatic neuropathy. | Severe hip pain, marked limitation of motion, often irreducible dislocation, high sciatic risk. | Severe thigh pain, inability to bear weight, significant swelling/deformity. |
| Key X-ray Findings | Transverse line across acetabulum, distinct posterior wall fragment. | Disruption of the "spur sign," involvement of entire anterior and posterior columns. | Femoral head contour irregularity/fracture line, associated acetabular fracture. | Obvious fracture line in subtrochanteric region, often comminuted. |
| CT/3D Reconstruction | Essential for defining transverse trajectory, posterior wall size/comminution, marginal impaction. | Crucial for assessing displacement, intra-articular fragments, quadrilateral plate involvement. | Paramount for assessing femoral head fracture pattern (location, size, step-off), associated acetabular injury. | Defines comminution, fracture geometry, soft tissue involvement. |
| Surgical Goal | Anatomical reduction of transverse and posterior wall components; restore articular congruity and stability. | Anatomical reduction of both columns, restore hip biomechanics, prevent post-traumatic OA. | Anatomical reduction of femoral head fracture, internal fixation, stabilization of acetabulum. | Stable internal fixation to restore mechanical axis and allow early mobilization. |
| Primary Surgical Approach | Kocher-Langenbeck (posterior) or combined approaches for complex transverse. | Often combined anterior (ilioinguinal/Stoppa) and posterior (Kocher-Langenbeck), or extended iliofemoral. | Kocher-Langenbeck (for posterior dislocation/fracture) or surgical hip dislocation (Ganz approach) for direct head access. | IM nailing or plating. |
| Major Complications | Post-traumatic OA, sciatic nerve injury, HO, avascular necrosis, recurrent instability. | Post-traumatic OA, sciatic nerve injury, HO, avascular necrosis, non-union. | Avascular necrosis of femoral head, post-traumatic OA, non-union, sciatic nerve injury. | Non-union, malunion, implant failure, infection, DVT/PE. |
Surgical Decision Making & Classification
The patient's acetabular fracture was classified as a
Transverse plus Posterior Wall
fracture according to the Letournel & Judet classification. The decision for operative intervention was straightforward due to several critical factors:
1.
Displacement:
Both the transverse and posterior wall components were significantly displaced, preventing anatomical reduction and joint congruence.
2.
Joint Instability:
Despite initial closed reduction, the extensive posterior wall comminution and displacement of the transverse component indicated inherent joint instability, predisposing to recurrent dislocation.
3.
Intra-articular Fragments:
The presence of osteochondral fragments within the joint mandated surgical removal to prevent accelerated articular cartilage wear and impingement.
4.
Marginal Impaction:
The posterosuperior marginal impaction injury required direct visualization and reduction to restore the acetabular roof and prevent a chronic defect.
5.
Patient Demographics:
A young, active patient necessitates the most anatomical reduction and stable fixation possible to optimize long-term outcomes and minimize the risk of post-traumatic osteoarthritis (OA).
Timing of Surgery:
The hip dislocation was reduced within 6 hours of injury, reducing the risk of avascular necrosis of the femoral head. Definitive operative fixation was planned after patient stabilization and optimization, approximately 3 days post-injury. This allowed for resolution of initial soft tissue swelling and a thorough pre-operative planning process, including detailed templating. A delay in surgery for highly comminuted acetabular fractures, particularly those without ongoing neurovascular compromise, is often beneficial to allow for soft tissue swelling to subside, making surgical dissection and closure less challenging.
Pre-operative Considerations:
*
Prophylactic Antibiotics:
Cefazolin 2g IV administered 30 minutes prior to incision.
*
DVT Prophylaxis:
Low molecular weight heparin (LMWH) initiated post-reduction and continued peri-operatively.
*
Heterotopic Ossification (HO) Prophylaxis:
Indomethacin 25mg TID commenced immediately post-operatively, continued for 6 weeks, given the high risk with posterior approaches to the hip.
*
Neurophysiological Monitoring:
Intra-operative somatosensory evoked potential (SSEP) and electromyography (EMG) monitoring for sciatic nerve integrity was arranged, given the proximity of the nerve to the surgical field and the mechanism of injury.
*
Blood Availability:
Two units of packed red blood cells were cross-matched and readily available.
Surgical Technique / Intervention
The primary goal of surgical intervention was anatomical reduction of both the transverse and posterior wall components, stable internal fixation, and restoration of articular congruity.
Patient Positioning:
The patient was positioned in a lateral decubitus position on a radiolucent table, carefully padded at all pressure points. The operative limb was draped free to allow for intra-operative manipulation. Fluoroscopy was set up to allow for real-time visualization in AP, inlet, outlet, and oblique (Judet) views.
Surgical Approach:
A
Kocher-Langenbeck approach
was utilized, given the predominant posterior wall and posterior column involvement.
1.
Incision:
A curvilinear incision was made starting from the posterior superior iliac spine, curving laterally over the greater trochanter, and extending distally along the posterior aspect of the thigh for approximately 15-20 cm.
2.
Muscle Dissection:
The gluteus maximus fascia was incised, and its fibers were split longitudinally. The short external rotators (piriformis, gemelli, obturator internus, quadratus femoris) were identified. The piriformis was released from its insertion on the greater trochanter to expose the sciatic nerve.
3.
Sciatic Nerve Protection:
The sciatic nerve was meticulously identified, gently mobilized, and protected throughout the procedure using vessel loops and careful retraction. Its course was vigilantly monitored.
4.
Capsulotomy:
A T-shaped capsulotomy was performed to gain access to the hip joint. The dislocated femoral head was carefully inspected for chondral damage.
5.
Fracture Exposure:
The posterior wall fragments were identified and lifted to expose the underlying transverse fracture line and the articular surface. The marginal impaction injury was clearly visualized.
Reduction Techniques:
1.
Debridement:
All loose osteochondral fragments were meticulously removed from the joint capsule. The impacted articular cartilage and subchondral bone were elevated and reduced using a bone tamp and bone graft (autograft from the iliac crest was harvested for this purpose) to support the reduced surface.
2.
Posterior Column Reduction:
The displaced posterior column was reduced first. This was achieved using direct reduction clamps (e.g., pointed reduction forceps, Farabeuf clamps) applying compression and rotation. A Schantz pin inserted into the ischium served as a joystick for rotation and translation. Intra-operative fluoroscopy confirmed satisfactory reduction of the posterior column and restoration of the ilioischial line.
3.
Transverse Fracture Reduction:
With the posterior column reduced, attention turned to the transverse component. This was often challenging due to muscle pull and displacement. A large Verbrugge clamp was applied across the reduced posterior column and the anterior column (indirectly via the iliac wing) to achieve compression and restore the overall acetabular shape. Direct manipulators and leverage were used to achieve anatomical alignment of the transverse fracture line. The goal was to restore the articular congruity of the dome.
4.
Posterior Wall Reduction:
Once the transverse fracture was provisionally reduced, the large posterior wall fragment(s) were reduced onto the reconstructed posterior column and articular surface. This required careful manipulation to interdigitate the fragments anatomically. K-wires were used for temporary stabilization.
Fixation Construct:
1.
Posterior Column Plate:
A pre-contoured 3.5mm posterior column plate (e.g., Stryker Acetabular Reconstruction Plate or a specific posterior column plate) was applied along the posterior column, extending from the ischium to the posterior iliac wing. Lag screws were used to achieve interfragmentary compression across the posterior column fracture line, followed by position screws for neutralization.
2.
Posterior Wall Buttress Plate:
A second 3.5mm reconstruction plate or a specific buttress plate was contoured and applied to buttress the posterior wall fragment(s) against the reduced posterior column. This provided stability against posterior translation. Lag screws were used to fix individual posterior wall fragments to the main plate and to the underlying bone where possible, ensuring no articular penetration.
3.
Intra-operative Fluoroscopy:
AP, inlet, outlet, and Judet oblique views were obtained multiple times throughout the reduction and fixation process to confirm anatomical reduction, appropriate screw length, and absence of intra-articular screw penetration. A direct arthrotomy of the hip joint was performed to visualize the articular surface and confirm reduction quality and hardware placement.
4.
Final Assessment:
After definitive fixation, the hip was taken through a full range of motion under fluoroscopy to assess stability and confirm no impingement.
Wound Closure:
A large suction drain was placed in the deep tissues. The short external rotators were reattached (if released). The gluteus maximus fascia and subcutaneous layers were closed, followed by skin closure.
Post-Operative Protocol & Rehabilitation
Immediate Post-operative Phase (Days 0-7):
*
Pain Management:
Multimodal analgesia including epidural or regional blocks, oral narcotics, NSAIDs (if not contraindicated), and acetaminophen.
*
DVT Prophylaxis:
Continued LMWH.
*
Antibiotics:
Continued for 24-48 hours post-operatively.
*
HO Prophylaxis:
Indomethacin 25mg TID initiated and continued for 6 weeks.
*
Weight Bearing:
Strict
non-weight bearing (NWB)
on the operative limb for 8-12 weeks to protect the complex reconstruction.
*
Range of Motion:
Gentle, passive and active-assisted range of motion (AAROM) within a protected arc. No active hip flexion beyond 90 degrees, no adduction past midline, and no internal rotation beyond neutral to protect the posterior reconstruction. Avoidance of positions of instability.
*
Drain Management:
Drain typically removed when output is minimal (<50 ml/24h).
*
Neurovascular Monitoring:
Regular checks for sciatic nerve function and distal pulses.
*
Radiographs:
Post-operative AP pelvis and Judet views to confirm hardware position and reduction quality.
Early Rehabilitation (Weeks 2-8):
*
Physical Therapy:
* Continue NWB.
* Progressive gentle passive and active-assisted ROM exercises, focusing on maintaining hip mobility without stressing the repair.
* Isotonic exercises for the non-operative leg and upper extremities.
* Core strengthening exercises.
* Gluteal and quadriceps isometrics on the operative side.
*
Education:
Extensive patient education on weight-bearing restrictions, hip precautions, and transfer techniques.
*
Follow-up:
Clinical and radiographic follow-up at 2 and 6 weeks.
Intermediate Rehabilitation (Weeks 8-16):
*
Weight Bearing:
Gradual progression to
touch-down weight bearing (TDWB)
(10-20% body weight) at 8-10 weeks, progressing to
partial weight bearing (PWB)
with crutches or a walker as tolerated, typically around 12 weeks, pending radiographic evidence of healing.
*
Physical Therapy:
* Continue ROM exercises.
* Initiate gentle closed-chain kinetic exercises.
* Strengthening of hip abductors, extensors, and quadriceps.
* Gait training with protected weight bearing.
*
Radiographs:
Follow-up radiographs at 12 weeks to assess fracture healing.
Advanced Rehabilitation (Months 4-6+):
*
Weight Bearing:
Full weight bearing (FWB) once radiographic union is confirmed and pain allows.
*
Physical Therapy:
* Progress to advanced strengthening, balance, and proprioception exercises.
* Focus on functional activities, stair climbing, and regaining symmetrical gait.
* Initiate return-to-sport specific training for appropriate patients, typically after 6-9 months, with appropriate risk assessment.
*
Monitoring:
Regular clinical and radiographic follow-up every 3-6 months for the first year, then annually, to monitor for complications such as post-traumatic OA, avascular necrosis, or heterotopic ossification.
Pearls & Pitfalls (Crucial for FRCS/Board Exams)
Pearls:
- Comprehensive Pre-operative Planning is Paramount: Never go to the operating theatre for an acetabular fracture without a detailed understanding of the 3D anatomy. CT with 3D reconstructions and meticulous templating are non-negotiable. Plan your approach, reduction maneuvers, and fixation strategy explicitly.
- Judet Views are Essential: Always obtain AP pelvis and both Judet oblique views (iliac and obturator) for initial radiographic assessment. These provide crucial information for classification and planning.
- Early Reduction of Hip Dislocation: Reduce dislocated hips within 6 hours to minimize the risk of avascular necrosis of the femoral head. A post-reduction CT is mandatory to assess congruence, identify intra-articular fragments, and delineate fracture patterns.
- Anatomical Reduction of the Articular Surface: This is the single most important factor determining long-term outcomes. Prioritize articular congruity over absolute perfect cortical apposition if a choice must be made.
- Meticulous Soft Tissue Handling: Excessive retraction or aggressive dissection increases the risk of iatrogenic nerve injury (especially sciatic nerve with posterior approaches), blood loss, and heterotopic ossification.
- Prophylaxis for Heterotopic Ossification (HO): Acetabular fractures, particularly those treated via posterior approaches, have a high incidence of HO. Administer NSAIDs (e.g., Indomethacin) for 4-6 weeks post-operatively, or consider single-dose radiation therapy, especially for high-risk patients.
- Intra-operative Fluoroscopy: Utilize high-quality fluoroscopy with multiple views (AP, inlet, outlet, iliac, obturator oblique) to confirm reduction, hardware position, and rule out articular penetration. Consider direct visualization of the articular surface through an arthrotomy.
- Awareness of Danger Zones: Constantly be aware of the sciatic nerve (posterior approaches) and the superior gluteal neurovascular bundle (extended iliofemoral, some posterior approaches).
- Stable Fixation: The fixation construct must be strong enough to allow for early, controlled rehabilitation while protecting the reduction. This often involves multiple plates and lag screws.
Pitfalls:
- Inadequate Imaging: Relying solely on plain radiographs or not obtaining 3D CT reconstructions can lead to misclassification, missed fracture lines, unidentified intra-articular fragments, or suboptimal surgical planning.
- Delayed Definitive Fixation: While soft tissue swelling must subside, undue delay in operative fixation (beyond 1-2 weeks without compelling reasons) can lead to fracture consolidation in a malreduced position, making subsequent reduction significantly more difficult and increasing complication rates.
- Failure to Address Marginal Impaction: Overlooking or not adequately addressing marginal impaction of the acetabular roof or femoral head can lead to persistent incongruity, early post-traumatic osteoarthritis, and mechanical instability.
- Iatrogenic Neurovascular Injury: Aggressive retraction, errant screw placement, or inadequate protection of critical structures can result in permanent neurological deficit or vascular compromise.
- Insufficient Fixation: Using an inadequate or biomechanically unsound fixation construct can result in loss of reduction, implant failure, and non-union.
- Early or Unrestricted Weight Bearing: Premature weight-bearing can lead to loss of reduction, implant failure, and exacerbation of articular damage, especially in complex fractures requiring prolonged protection.
- Inadequate Post-operative Rehabilitation: Poor patient compliance or an ill-conceived rehabilitation protocol can lead to stiffness, muscle atrophy, and suboptimal functional outcomes despite a technically perfect surgery.
- Missing Associated Injuries: High-energy trauma can involve multiple systems. Failure to identify and address concurrent injuries (e.g., pelvic ring, spinal, intra-abdominal) can significantly impact patient management and outcomes.
- Underestimation of Operative Difficulty: Acetabular fracture surgery is technically demanding and requires specialized training and experience. Attempting these cases without adequate preparation or resources can lead to disastrous results.
You Might Also Like