Congenital Anomalies of the Lower Extremity: Surgical Management of Polydactyly
Key Takeaway
Congenital polydactyly of the foot occurs in approximately two per 1,000 live births, presenting primarily as an isolated autosomal dominant trait. Surgical intervention is indicated to alleviate pain, facilitate normal shoe wear, and improve cosmesis. Operative management requires meticulous preoperative radiographic evaluation to identify accessory metatarsals. Surgical techniques range from simple disarticulation to complex capsular reconstructions, ensuring optimal biomechanical alignment and preventing postoperative deformities such as hallux varus.
Congenital Anomalies of the Lower Extremity: An Overview
The management of congenital anomalies of the foot and lower extremity requires a profound understanding of pediatric biomechanics, embryological development, and longitudinal growth patterns. While congenital anomalies of the hip, pelvis, trunk, and upper extremities present their own unique reconstructive challenges, pedal anomalies directly impact the developing child's gait mechanics, weight-bearing distribution, and future shoe wear.
The most frequently encountered congenital anomaly of the forefoot is polydactyly—the presence of supernumerary digits. Other notable anomalies include syndactyly (webbed toes), macrodactyly (enlarged toes), cleft foot (partial adactyly), and congenital contractures or angulations. Surgical intervention for these conditions is rarely purely cosmetic; it is fundamentally reconstructive. When evaluating a pediatric patient for forefoot reconstruction, the orthopaedic surgeon must balance three primary objectives: the alleviation of pain, the facilitation of standard shoe wear, and the optimization of cosmesis. A satisfactory clinical result must comprehensively address all three parameters without compromising the biomechanical integrity of the foot.
Polydactyly of the Foot
Polydactyly of the toes is a relatively common congenital deformity, with an overall incidence of approximately two cases per 1,000 live births. While it may manifest as a component of established genetic syndromes (such as Ellis-van Creveld syndrome, Trisomy 13, or Bardet-Biedl syndrome), it most frequently occurs as an isolated trait. In its isolated form, pedal polydactyly typically demonstrates an autosomal dominant inheritance pattern with variable phenotypic expression and incomplete penetrance.
Embryology and Pathoanatomy
The embryological insult resulting in polydactyly occurs between the fourth and eighth weeks of gestation during the formation of the apical ectodermal ridge (AER) and the zone of polarizing activity (ZPA). Abnormalities in the Sonic Hedgehog (SHH) signaling pathway, which regulates the anteroposterior axis of the limb bud, lead to the duplication of digital rays.
Biomechanically, the presence of a supernumerary digit disrupts the transverse metatarsal arch and widens the forefoot splay. This widening is the primary culprit behind shoe-wear difficulties. Furthermore, shared tendinous insertions or bifurcated metatarsal heads can alter the windlass mechanism, leading to dysfunctional push-off during the terminal stance phase of gait.
Clinical Evaluation and Classification
Clinical assessment must begin with a thorough family history and a systemic examination to rule out syndromic associations. The physical examination of the foot should document the exact number of digits, the presence of syndactyly, the active and passive range of motion of the involved joints, and the vascular integrity of the toes.

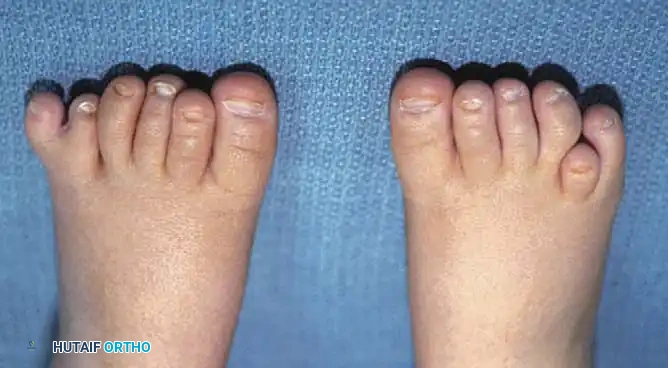
Bilateral polydactyly in a 6-month-old infant. Note the widening of the forefoot and the postaxial location of the supernumerary digits, which will inevitably complicate standard shoe wear.
The Venn-Watson Classification is the most widely utilized system for categorizing pedal polydactyly, directing the surgeon's attention to the anatomical location and the underlying skeletal morphology:
1. Preaxial Polydactyly: Duplication involving the first ray (hallux).
2. Central Polydactyly: Duplication involving the second, third, or fourth rays.
3. Postaxial Polydactyly: Duplication involving the fifth ray (most common).
Venn-Watson further subclassified these based on the metatarsal configuration:
* T-shaped metatarsal
* Y-shaped metatarsal
* Complete duplication of the metatarsal
* Soft tissue duplication only (floating digit)
Radiographic Evaluation
Standard weight-bearing (or simulated weight-bearing in infants) anteroposterior, lateral, and oblique radiographs of the foot are mandatory.
Clinical Pearl: Never proceed with the amputation of a supernumerary digit based on clinical appearance alone. Preoperative radiographs are critical to detect any extra metatarsals, bifurcated metatarsal heads, or shared articular surfaces. Failure to resect an accessory metatarsal will result in a persistent bony prominence, defeating the purpose of the surgery.
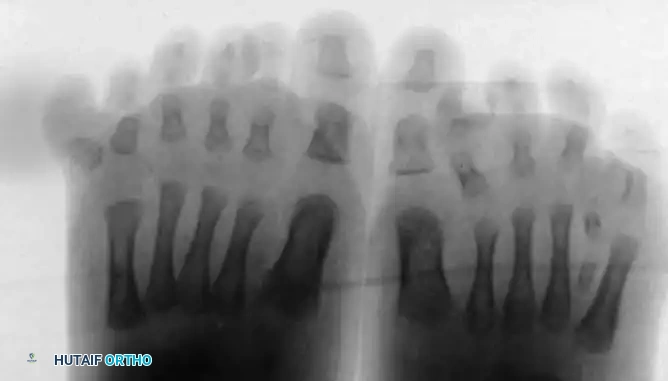
Radiograph of the left foot demonstrating an accessory metatarsal articulating with the supernumerary digit. This entire accessory ray must be resected to achieve a functional and cosmetic narrowing of the forefoot.
Indications and Timing of Surgery
The primary indications for surgical intervention are:
* Inability to fit into standard, commercially available footwear.
* Pain associated with impingement or rubbing of the extra digit.
* Psychosocial and cosmetic concerns.
Timing: Surgery is optimally performed when the child is between 9 and 12 months of age. At this stage, the child is large enough to safely undergo general anesthesia, the anatomical structures are sufficiently developed for meticulous dissection, and the intervention occurs prior to the onset of independent ambulation, thereby preventing the development of abnormal gait patterns.
Surgical Management Strategies
The surgical approach is dictated by the Venn-Watson classification and the specific pathoanatomy of the duplication.
Preaxial Polydactyly Reconstruction
Preaxial duplication presents a unique challenge due to the critical biomechanical role of the hallux in weight-bearing and propulsion. The duplication may involve the distal phalanx, proximal phalanx, or the entire first ray.
In the majority of preaxial polydactyly cases, the most medial great toe is excised. The lateral duplicated toe is typically preserved because it usually maintains a more congruent articulation with the first metatarsal and preserves the critical first web space.
Surgical Warning: Excision of the medial digit inevitably detaches the abductor hallucis tendon and the medial collateral ligament of the metatarsophalangeal (MTP) joint. Failure to meticulously reconstruct these medial structures will result in a progressive, iatrogenic hallux varus deformity.
Key Steps in Preaxial Reconstruction:
1. Incision: A medial longitudinal or racquet-shaped incision is utilized.
2. Soft Tissue Dissection: The abductor hallucis tendon is carefully identified and tagged before the medial digit is disarticulated.
3. Capsulorrhaphy: Following excision of the medial digit and any prominent medial metatarsal condyle, the medial capsule must be imbricated.
4. Tendon Transfer: The abductor hallucis is advanced and sutured to the base of the proximal phalanx of the retained lateral hallux to provide dynamic medial stability.
5. Fixation: The MTP joint is stabilized with a transarticular Kirschner wire (K-wire) for 4 to 6 weeks to protect the soft tissue repair.
Complex Polydactyly-Syndactyly
Occasionally, polydactyly is complicated by concurrent syndactyly (webbing) of the adjacent digits. These combined deformities require highly individualized, complex surgical planning.
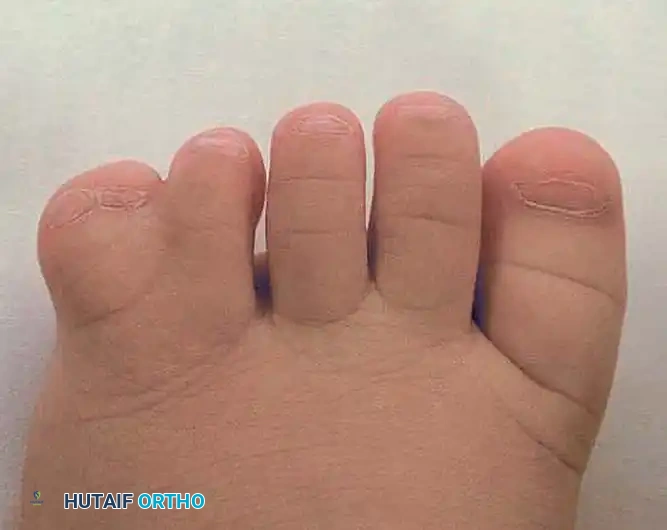
Complex polydactyly-syndactyly of the left fifth toe, demonstrating both bony and soft-tissue syndactyly. Such presentations require meticulous preoperative planning to ensure adequate skin coverage following resection.
In cases of complex polydactyly-syndactyly, simple amputation is insufficient. The surgeon must often resect the more peripheral or dysplastic digit while carefully harvesting its skin as a vascularized flap to reconstruct the commissure and provide coverage for the retained digit.
In rare instances of central duplication with shared articular surfaces, a Bilhaut-Cloquet procedure may be indicated. This involves the central wedge resection of the duplicated bone and soft tissues, followed by the amalgamation of the two lateral halves to create a single, appropriately sized digit. While technically demanding, it preserves the collateral ligaments and neurovascular bundles of the outer margins.
Operative Technique: Amputation of an Extra Toe (Postaxial/Central)
The following technique describes the standard approach for the amputation of a postaxial or central supernumerary digit, ensuring complete removal of the accessory ray and appropriate contouring of the forefoot.
Preoperative Setup and Positioning
- Anesthesia: General anesthesia is preferred for pediatric patients, supplemented by a regional ankle block or popliteal block for postoperative analgesia.
- Positioning: Supine position. A well-padded calf tourniquet is applied to provide a bloodless surgical field, which is critical for identifying delicate pediatric neurovascular structures.
- Preparation: Standard orthopaedic skin preparation and draping.
Step-by-Step Surgical Technique
1. Incision Design:
* At the base of the toe to be amputated, design an oval or racquet-shaped incision through the skin and superficial fascia.
* The handle of the racquet should extend proximally over the dorsal aspect of the metatarsal if an accessory metatarsal requires resection.
* Pearl: Ensure the plantar skin flap is slightly longer than the dorsal flap to keep the final suture line dorsal to the weight-bearing surface.
2. Tendon Management:
* Deepen the incision to identify the extensor and flexor tendons of the supernumerary digit.
* Apply traction to the tendons, drawing them distally as far as possible.
* Divide the tendons under tension so they retract proximally into the soft tissues, preventing tethering or bowstringing.
3. Joint Disarticulation:
* Identify the capsule of the metatarsophalangeal (MTP) joint.
* Incise the capsule transversely. Carefully dissect the capsule away from the metatarsal head.
* Disarticulate the joint, removing the supernumerary phalanges in their entirety.
* Warning: Carefully protect the neurovascular bundles supplying the adjacent, retained digit during this dissection.
4. Bony Contouring:
* Inspect the remaining metatarsal head. Often, the metatarsal head will have a widened, bifurcated, or protruding articular facet that supported the amputated phalanx.
* Using a sharp pediatric osteotome or bone-cutting forceps, sharply resect this protruding bone.
* The goal is to create a smooth, contoured metatarsal head that matches the normal anatomy and prevents a painful adventitial bursa from forming postoperatively. Smooth the edges with a fine rasp.
5. Resection of Accessory Metatarsal (If Present):
* If preoperative radiographs revealed a complete extra metatarsal (as seen in Venn-Watson complete duplications), continue the incision proximally along the lateral or dorsal aspect of the foot.
* Perform a subperiosteal dissection of the accessory metatarsal.
* Disarticulate the accessory metatarsal at its tarsometatarsal joint.
* Pearl: Avoid leaving a proximal metatarsal stump, as this can lead to a painful plantar prominence as the child grows.
6. Closure:
* Release the tourniquet and achieve meticulous hemostasis using bipolar electrocautery. Hematoma formation is a primary cause of wound dehiscence and infection in pediatric foot surgery.
* Perform a layered closure. Repair the deep transverse metatarsal ligament if it was divided, as this prevents splaying of the remaining toes.
* Close the skin with interrupted, absorbable sutures (e.g., 4-0 or 5-0 chromic gut or Vicryl Rapide) to avoid the need for suture removal in an awake child.
Postoperative Protocol and Rehabilitation
- Immobilization: A bulky, compressive soft dressing is applied immediately postoperatively. For simple disarticulations, a short-leg cast or a rigid postoperative shoe is utilized for 3 to 4 weeks to protect the incision.
- K-Wire Management: If a K-wire was utilized (e.g., in preaxial reconstructions to prevent hallux varus), it is bent outside the skin, capped, and incorporated into a short-leg cast. The pin is typically removed in the clinic at 4 to 6 weeks postoperatively.
- Weight-Bearing: The patient is kept non-weight-bearing or heel-weight-bearing for the first 3 to 4 weeks, depending on the child's age and compliance.
- Follow-Up: Clinical evaluation at 2 weeks for wound check. Radiographs are obtained at 6 weeks to confirm the maintenance of alignment and the absence of heterotopic ossification.
Complications and Pitfalls
While generally highly successful, surgical management of polydactyly carries specific risks:
1. Residual Bony Prominence: The most common complication, resulting from inadequate resection of a bifurcated metatarsal head or an unrecognized accessory metatarsal. This leads to painful shoe wear and often requires revision surgery.
2. Hallux Varus: A devastating complication following preaxial polydactyly excision, caused by failure to reconstruct the medial collateral ligament and abductor hallucis.
3. Neuroma Formation: Inadequate proximal resection of the digital nerves can lead to painful stump neuromas.
4. Angular Deformities: Damage to the physis of the retained digit during dissection can result in progressive angular deformities as the child grows. Meticulous, tissue-sparing surgical technique is paramount.
You Might Also Like