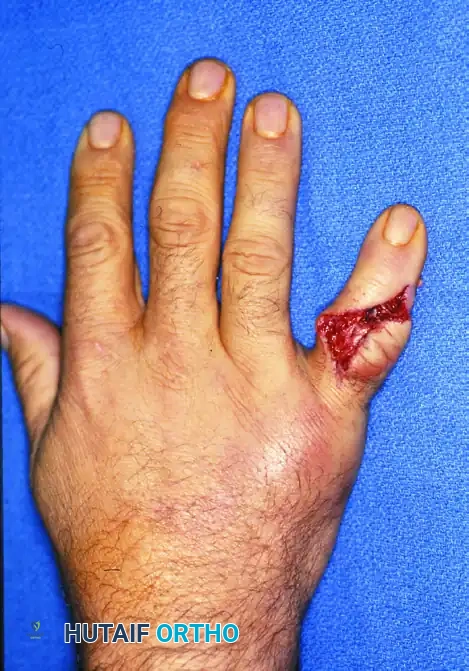
Management of Open Hand Fractures & Dislocations
Key Takeaway
Open fractures and dislocations of the hand demand meticulous surgical debridement, copious irrigation, and stable skeletal fixation. Immediate management prioritizes infection prevention and soft tissue preservation. Fixation constructs must maintain anatomic length and rotational alignment while permitting unrestricted access for serial wound inspections. Early mobilization is paramount; therefore, the chosen osteosynthesis method should provide sufficient stability to allow immediate active range of motion once soft tissue healing permits.
OPEN FRACTURES AND DISLOCATIONS OF THE HAND
The management of open fractures and dislocations in the hand presents a complex surgical challenge that requires a delicate balance between aggressive infection control and the meticulous preservation of functional anatomy. Unlike long bone trauma, the hand possesses a highly compact architecture where bones, tendons, neurovascular bundles, and specialized soft tissues exist in intimate proximity. Consequently, massive trauma to the hand may require extensive reconstructive efforts to restore bony integrity and functional kinematics.
The primary objectives in treating these injuries are the prevention of sepsis, the restoration of skeletal stability, the provision of durable soft tissue coverage, and the facilitation of early rehabilitation.
Emergency Department Evaluation and Initial Management
The initial assessment of an open hand injury must follow advanced trauma life support (ATLS) principles, as high-energy mechanisms (e.g., crush injuries, ballistic trauma, industrial accidents) are frequently associated with concomitant systemic injuries.
Once life-threatening injuries are ruled out, a systematic examination of the hand is mandatory. This includes a rigorous assessment of the vascular status (capillary refill, Allen test), neurologic function (two-point discrimination), and musculotendinous integrity.
Clinical Pearl: We no longer routinely culture acute open hand injuries in the emergency department, unless gross contamination (e.g., agricultural debris, marine exposure) is present. Superficial swabbing of acute wounds primarily isolates colonizing skin flora rather than the true deep-tissue pathogens responsible for subsequent osteomyelitis.
Initial Interventions:
* Antibiotic Prophylaxis: Intravenous antibiotics should be administered as soon as possible. A first-generation cephalosporin (e.g., cefazolin) is standard. For highly contaminated wounds or severe crush injuries, an aminoglycoside (e.g., gentamicin) is added. Penicillin is indicated for farm-related injuries to cover Clostridium species.
* Tetanus Prophylaxis: Administered based on the patient's immunization history and wound severity.
* Wound Care: Gross debris should be gently removed, and the wound covered with a sterile, saline-soaked dressing.
* Splinting: The hand should be immobilized in a safe position (intrinsic-plus) to minimize further soft tissue trauma and reduce pain during transport to the operating room.
Surgical Principles: Débridement and Irrigation
The cornerstone of managing open fractures and dislocations is meticulous, systematic surgical débridement combined with copious irrigation. This must be performed in the operating room under optimal lighting, tourniquet control, and appropriate anesthesia.
Tourniquet Application:
The limb should be elevated for exsanguination rather than using an Esmarch bandage, which can inadvertently force contaminants and hematoma proximally into uninjured tissue planes.
Wound Extension and Exploration:
Severely traumatized hands commonly are accompanied by soft tissue defects, and additional incisions usually are unnecessary to access the fracture. The traumatic wound itself often provides an adequate window for fracture management. However, if extension is required, incisions should follow Brunner's zigzag principles or mid-axial lines to prevent subsequent flexion contractures.
Management of Open Dislocations:
A critical, often overlooked scenario involves the self-reduced open dislocation. If an open dislocation is self-reduced and a contaminant is suspected (e.g., a bite wound or a fall into soil), redislocation and thorough wound cleansing must be done. Failure to expose the joint surfaces and irrigate the intra-articular space can lead to catastrophic septic arthritis and rapid cartilage destruction.
Tissue Viability Assessment:
Débridement proceeds from superficial to deep. All devitalized skin, subcutaneous fat, and necrotic muscle must be excised until healthy, bleeding tissue is encountered. Bone fragments devoid of soft tissue attachments that do not contribute to articular congruity should generally be removed, though large structural fragments may be retained after rigorous decontamination if they are critical for stability.
Operative Technique: Skeletal Stabilization
Following adequate débridement, the fracture or dislocation must be reduced and stabilized. The choice of fixation is dictated by the fracture pattern, the degree of bone loss, and the condition of the soft tissue envelope.
Surgical Warning: Fixation should permit wound inspection or dressing changes without loss of fracture alignment. Bulky external fixators or poorly planned percutaneous pins that obstruct wound access will severely complicate subsequent soft tissue management.
Fixation Strategies:
1. Percutaneous Kirschner Wires (K-wires): Ideal for minimally comminuted fractures or when the soft tissue envelope is too tenuous to support internal hardware. They can be placed percutaneously or under direct vision through the traumatic wound.
2. Mini-Fragment Plates and Screws: Provide rigid internal fixation, allowing for immediate mobilization. However, they require adequate soft tissue coverage and should be avoided if the wound is grossly contaminated or if primary closure is impossible.
3. External Fixation: Reserved for highly comminuted fractures, severe bone loss, or massive crush injuries where length and alignment must be maintained while allowing unrestricted access to complex soft tissue wounds.
Management of Segmental Bone Defects:
High-energy trauma, such as ballistic injuries, frequently results in intercalary bone loss. Segmental defects of tubular bones may be held to length by wire spacers or rods to prevent collapse while the wound is healing. Maintaining the anatomic length of the metacarpal or phalanx is critical to preserve the tension of the intrinsic and extrinsic musculature. Polymethylmethacrylate (PMMA) cement spacers (with or without antibiotics) can also be utilized to maintain the defect space and induce a pseudo-synovial membrane (the Masquelet technique) for future bone grafting.
Intraoperative Assessment of Rotational Alignment
Malrotation is a devastating complication of hand fractures, particularly in the metacarpals and proximal phalanges. Even a few degrees of rotational deformity can lead to significant digital overlap (scissoring) during flexion, severely impairing grip function.
Because the hand is often draped out and the patient is paralyzed or under regional anesthesia, active motion cannot be used to assess alignment. Therefore, the surgeon must rely on passive tenodesis and anatomic landmarks.
To ensure accurate reduction, the fingers must be passively flexed at the metacarpophalangeal, proximal interphalangeal, and distal interphalangeal joints and compared with the adjacent uninjured finger or fingers before definitive rotational control is achieved, especially if there are doubts regarding correct fracture rotational alignment. All fingertips should point toward the scaphoid tubercle during passive flexion.
Clinical Case Example: High-Energy Ballistic Trauma
The following case illustrates the principles of managing severe open fractures with segmental bone loss and significant soft tissue compromise.
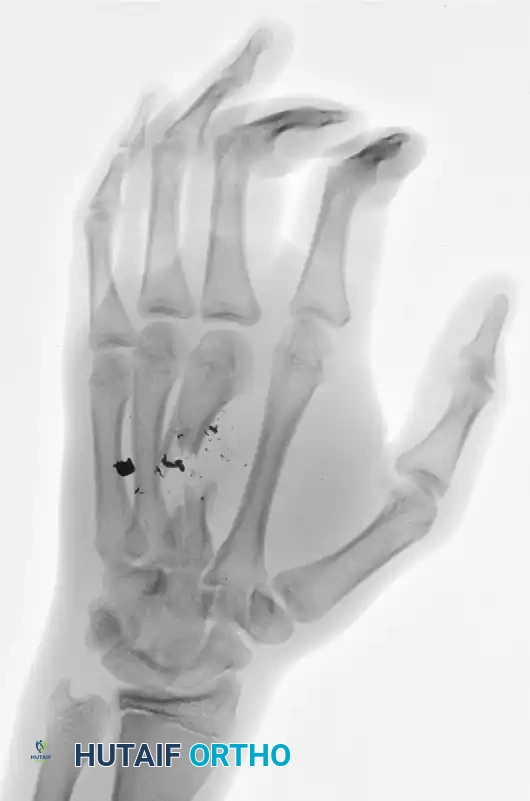
FIGURE 67-4 A and B: Comminuted middle finger metacarpal shaft fracture with intercalary bone loss from a self-inflicted handgun injury in a 17-year-old boy.

Figure 67-4 A: Anteroposterior (AP) radiograph demonstrating a highly comminuted fracture of the third metacarpal with significant segmental bone loss and retained ballistic fragments.
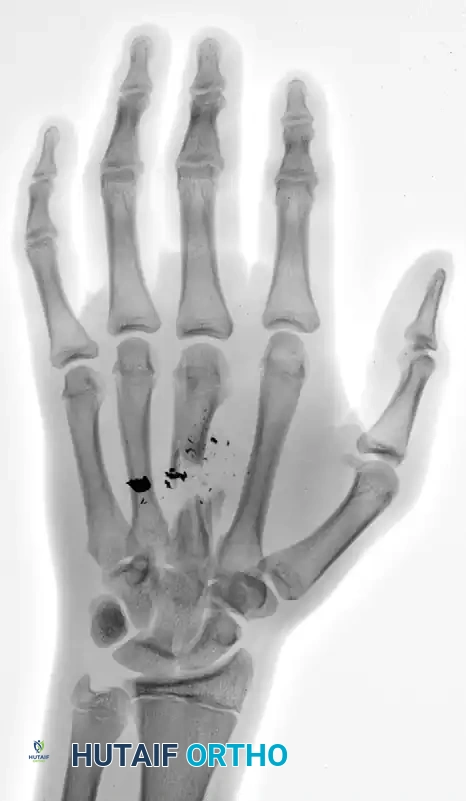
Figure 67-4 B: Oblique radiograph confirming the extent of the intercalary defect and the disruption of the longitudinal arch of the hand.
C and D: Clinical appearance of the hand before débridement.
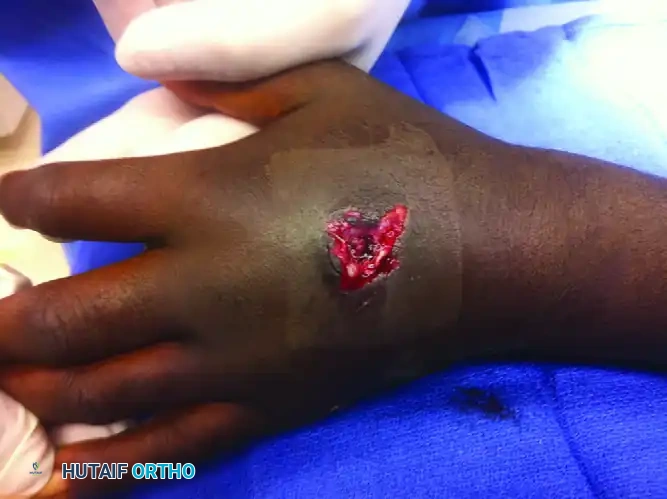
Figure 67-4 C: Dorsal view of the hand demonstrating the entry wound with surrounding soft tissue contusion and thermal injury characteristic of close-range ballistic trauma.
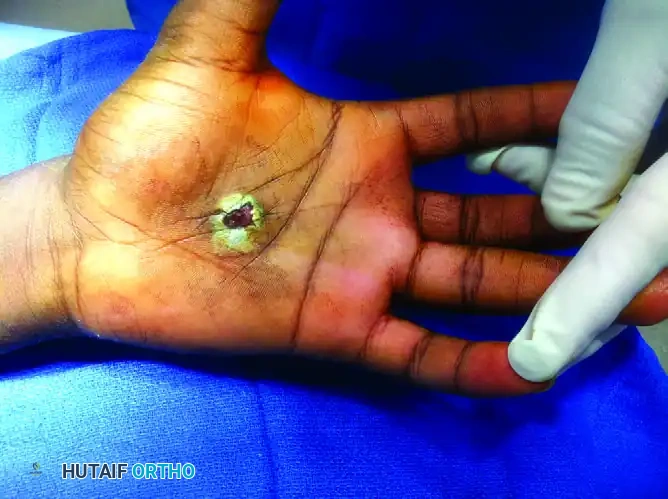
Figure 67-4 D: Volar view demonstrating the exit wound. Note the stellate tearing of the palmar skin and the extrusion of hematoma and devitalized tissue.
In this scenario, the initial procedure must focus on aggressive débridement of the ballistic tract, removal of devitalized bone and debris, and stabilization of the third ray to prevent collapse. A wire spacer or spanning external fixator would be ideal to maintain length while the soft tissue envelope is managed.
Soft Tissue Management and Wound Closure
The timing and method of wound closure require significant clinical judgment. The surgeon must determine whether the wound is sufficiently clean to permit primary closure or whether it should be left open for repeat débridement and irrigation.
The Danger of Primary Closure Under Tension:
If primary closure is attempted, loose skin-edge approximation is recommended because soft tissue edema over the next 48 hours will further increase tension on the traumatized tissues and possibly compromise otherwise viable flaps. Tight sutures will inevitably lead to marginal necrosis, wound breakdown, and exposure of underlying hardware or tendons.
Delayed Primary Closure and Second-Look Procedures:
For contaminated wounds, crush injuries, or wounds with questionable tissue viability, the wound should be packed open with non-adherent dressings or managed with negative pressure wound therapy (NPWT). At 48 hours, the wound can be reevaluated in the operating room and plans made at that time for closure. This "second look" allows the surgeon to identify and excise any tissue that has demarcated and necrosed since the index procedure.
The Reconstructive Window:
The goal is to close the wound within the first 4 to 5 days before granulation tissues form and contractures develop. Prolonged open management in the hand leads to desiccation of vital structures, severe stiffness, and fibrotic contractures that are exceptionally difficult to salvage.
Management of Exposed Tendons:
Exposed tendons without their paratenon or sheath soon necrose without appropriate coverage. Tendons rely on a delicate intrinsic blood supply and diffusion from surrounding synovial fluid. If the paratenon is lost, the tendon will rapidly desiccate and rupture. In such cases, simple skin grafting is insufficient, as grafts will not take over bare tendon. These defects mandate coverage with local, regional, or free vascularized flaps to provide a healthy, gliding tissue bed.
Postoperative Protocol and Rehabilitation
The ultimate success of open hand fracture management hinges on the postoperative rehabilitation protocol. The hand is uniquely prone to stiffness due to the rapid formation of adhesions between the fracture callus, tendon sheaths, and overlying skin.
Early Mobilization:
Finger motion should begin as soon as soft tissue healing and fracture and joint stability permit. The paradigm has shifted away from prolonged immobilization toward early active motion. If rigid internal fixation was achieved, active range of motion (AROM) can often begin within 3 to 5 days postoperatively, guided by a specialized hand therapist.
Edema Control:
Postoperative edema is the enemy of hand function. It increases the diffusion distance for cellular nutrition, promotes fibrosis, and mechanically restricts joint flexion. Aggressive edema control utilizing strict elevation, compressive dressings (e.g., Coban wrapping), and active muscle pumping is mandatory.
Orthotic Management:
Between exercise sessions, the hand should be splinted in the intrinsic-plus position (wrist extended 20-30 degrees, metacarpophalangeal joints flexed 70-90 degrees, and interphalangeal joints fully extended). This position maintains the collateral ligaments of the MCP joints at their maximal length, preventing extension contractures, while preventing flexion contractures at the PIP joints.
Complications and Pitfalls
- Infection: Deep space infections or osteomyelitis require immediate return to the operating room for radical débridement, hardware removal (if loose), and culture-directed intravenous antibiotics.
- Malunion and Nonunion: Often the result of inadequate initial fixation or premature loss of reduction. Rotational malunions require corrective osteotomies. Nonunions, particularly in areas of segmental bone loss, require structural bone grafting once the soft tissue envelope is pristine.
- Tendon Adhesions: The most common complication following open hand fractures. Prevention through early motion is key. Established adhesions may require secondary tenolysis, but only after skeletal union is solid and soft tissues are supple.
- Joint Stiffness: A direct consequence of prolonged immobilization, intra-articular scarring, or capsular contracture. Aggressive hand therapy is the first line of treatment, followed by surgical capsulotomy for refractory cases.
In conclusion, the management of open fractures and dislocations of the hand is a demanding endeavor that requires a meticulous, staged approach. By adhering to the principles of aggressive débridement, stable skeletal fixation, timely soft tissue coverage, and early functional rehabilitation, the orthopedic surgeon can optimize outcomes and restore meaningful function to the traumatized hand.
You Might Also Like