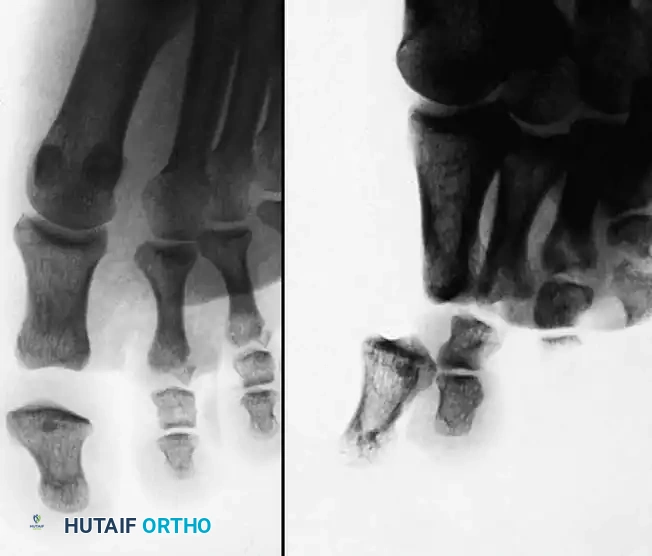
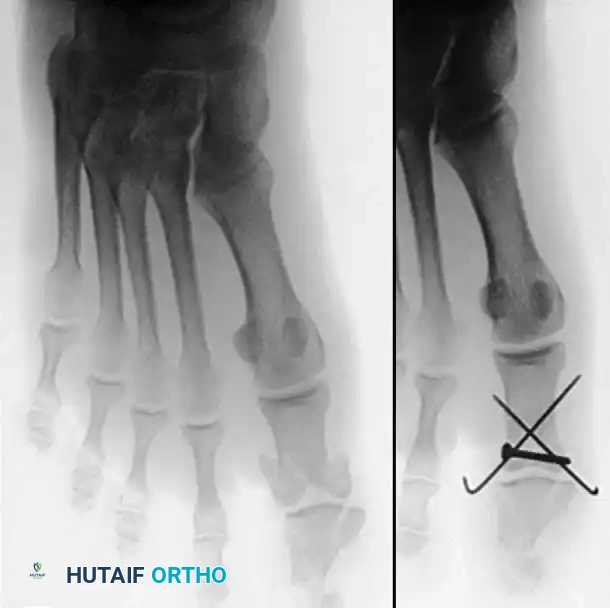
Mastering Acute Hand Trauma: Comprehensive History, Clinical Examination, and Intraoperative Wound Assessment
Key Takeaway
The initial evaluation of acute hand trauma dictates the trajectory of functional recovery. A meticulous history detailing the mechanism and timing of injury must precede a systematic clinical examination. Radiographic, neurovascular, and tendinous assessments are mandatory before surgical exploration. In the operating theater, rigorous debridement, foreign body removal, and anatomical tissue viability assessment form the cornerstone of preventing infection and enabling successful primary or delayed reconstruction.
Introduction to Acute Hand Trauma Evaluation
The management of acute hand trauma demands a rigorous, systematic approach. The hand is an unforgiving anatomical region where the gliding planes of tendons, the delicate arborization of neurovascular bundles, and the intricate osteoarticular architecture exist in extreme proximity. An oversight during the initial history, clinical examination, or intraoperative assessment can lead to catastrophic functional deficits, chronic infection, or limb loss. This comprehensive guide delineates the postgraduate-level protocols for evaluating and preparing the traumatized hand for surgical reconstruction.
Comprehensive History Taking in Hand Trauma
The history is not merely a preliminary formality; it is the foundation upon which the entire surgical strategy is constructed. A meticulously obtained history provides critical data regarding the zone of injury, the degree of contamination, and the physiological status of the patient. The history must accurately and concisely capture the following six domains:
1. Temporal Factors and the "Golden Window"
The exact time of injury must be established to determine the interval before treatment. This temporal data dictates the urgency of surgical intervention.
* Ischemic Time: In cases of vascular compromise or amputations, warm versus cold ischemia times are critical determinants of replantation viability. Muscle tissue undergoes irreversible necrosis after 4 to 6 hours of warm ischemia, whereas digits (lacking muscle bellies) may tolerate longer periods.
* Infection Risk: The time elapsed since injury directly correlates with bacterial proliferation. Immediate, urgent surgery is mandated for severely contaminated wounds, suspected deep space infections, and open fractures.
2. Prehospital Care and First Aid
The surgeon must ascertain what first aid measures were administered, by whom, and in what environment.
* Hemostasis: Was a tourniquet applied? If so, what type, and for how long? Prolonged, unmonitored tourniquet application can induce profound ischemic neuropathy and myonecrosis.
* Wound Coverage: Were the wounds covered with sterile dressings or unsterile materials? Was the amputated part appropriately preserved (wrapped in saline-moistened gauze, placed in a plastic bag, and set on ice—never directly on ice)?
3. Pharmacological History
The nature, amount, and timing of any medication received pre-hospital or in the emergency department must be documented.
* Anticoagulants: Knowledge of antiplatelet agents or anticoagulants is vital for intraoperative hemostasis planning.
* Analgesia: Prior administration of narcotics may mask clinical symptoms during the physical examination, particularly regarding compartment syndrome.
4. Mechanism of Injury (Kinematics and Tissue Transfer)
Understanding the exact mechanism of injury allows the surgeon to predict the "zone of injury"—the area of microscopic tissue damage that extends beyond the macroscopic wound.
* Sharp Lacerations: Typically present with a narrow zone of injury, making primary repair of tendons and nerves highly successful.
* Crush Injuries: Impart massive kinetic energy, leading to extensive microvascular thrombosis, severe edema, and a high risk of compartment syndrome. The zone of injury is wide, and tissues that initially appear viable may demarcate and necrose over subsequent days.
* Avulsion Injuries: Often result in extensive intimal damage to blood vessels far proximal and distal to the visible wound, complicating microvascular anastomosis.
* High-Pressure Injection Injuries: These are surgical emergencies.
🚨 SURGICAL WARNING: High-Pressure Injection Injuries
High-pressure injection injuries (e.g., paint, grease, hydraulic fluid) often present with a deceptively benign puncture wound. However, the fluid dissects rapidly along tendon sheaths and fascial planes, causing severe chemical necrosis and compartment syndrome. These require immediate, aggressive, and extensive surgical decompression and debridement. Never underestimate a high-pressure injection injury based on the surface wound.
5. Anesthetic Considerations (NPO Status)
The nature, time, and amount of food and liquid taken by the patient must be recorded. This information is non-negotiable for the anesthesiologist when selecting between regional blocks, monitored anesthesia care (MAC), or general anesthesia, particularly balancing the risk of aspiration against the urgency of the surgical intervention.
6. Patient Demographics and Functional Demands
The patient’s age, occupation, place of employment, handedness, and general health status (e.g., diabetes, smoking history, peripheral vascular disease) profoundly influence surgical decision-making. A complex reconstructive procedure requiring prolonged immobilization and extensive rehabilitation may be appropriate for a young, compliant musician but contraindicated for an elderly, non-compliant patient with severe medical comorbidities.
Preoperative Clinical Examination
Even before the hand wound is directly examined or manipulated, a structured, non-invasive evaluation must be conducted. This preliminary assessment provides up to 90% of the information required to formulate a definitive treatment plan.
Radiographic Evaluation
Standard posteroanterior (PA), true lateral, and oblique radiographs of the hand and wrist are mandatory.
* Osteoarticular Assessment: Evaluate for fractures, dislocations, and subluxations. Pay close attention to articular congruity and bone loss.
* Foreign Bodies: Radiographs are essential for identifying radiopaque foreign objects (e.g., metal, glass, gravel). Note that some materials, such as wood or certain plastics, are radiolucent and may require ultrasound or MRI for detection, though high clinical suspicion warrants surgical exploration regardless of imaging.
Neurovascular Assessment
Vascular and neurologic function must be evaluated and documented before the administration of any local anesthetic.
* Vascular Function: Assess capillary refill, skin color, and temperature. Perform an Allen's test (or digital Allen's test) to evaluate the patency of the radial and ulnar arteries and the integrity of the superficial and deep palmar arches. A handheld Doppler probe is invaluable for assessing arterial flow in the traumatized extremity.
* Neurologic Function: Evaluate both sensory and motor components of the median, ulnar, and radial nerves. Two-point discrimination (static and moving) is the gold standard for assessing digital nerve integrity. Normal static two-point discrimination is less than 6 mm.
Musculotendinous Evaluation
Motor function of the hand must be systematically evaluated to detect possible tendon injuries.
* Observation: Observe the natural resting cascade of the hand. A disruption in the normal flexed posture of the digits strongly suggests a flexor tendon laceration.
* Tenodesis Effect: Passive extension of the wrist should cause spontaneous flexion of the fingers, and passive flexion of the wrist should cause extension. Loss of this effect indicates tendon discontinuity.
* Active Testing: Isolate and test the Flexor Digitorum Superficialis (FDS) and Flexor Digitorum Profundus (FDP) independently. Test the extensor compartments systematically.
💡 CLINICAL PEARL: The Painful Arc
If a patient can actively move a digit but experiences significant pain against resistance, suspect a partial tendon laceration. Partial lacerations greater than 60% of the tendon's cross-sectional area typically require surgical repair to prevent delayed rupture or triggering.
Pre-Surgical Interventions and Patient Counseling
Based on the initial assessment, immediate medical interventions are initiated (e.g., broad-spectrum antibiotics, tetanus prophylaxis, and appropriate analgesia).
Before sedatives or narcotics are administered, the surgeon must engage in a frank, detailed discussion with the patient. The patient must be fully informed regarding:
* The extent of the injuries.
* The proposed surgical plan.
* The prognosis for functional recovery.
* The possibility of amputation: Consent for amputation or terminalization must be obtained if there is any risk that a digit or limb is unsalvageable.
* The need for complex reconstruction: The patient must be forewarned if skin grafts, local flaps, or distant pedicled/free flaps are anticipated.
Surgical Wound Preparation and Debridement
The transition to the operating room marks the shift from assessment to intervention. The primary goal of the initial surgical phase is to convert a contaminated traumatic wound into a clean, surgically manageable field.
Principles of Wound Irrigation and Cleansing
Wound cleaning must never be hurried. Thoroughness is the ultimate defense against postoperative infection. Primary healing without infection is an absolute prerequisite to limit scar formation and to facilitate early rehabilitation or subsequent reconstructive stages.
* Irrigation: Copious irrigation with sterile normal saline is the most effective method for reducing bacterial load. While pulsatile lavage can be used for highly contaminated long bone fractures, gentle gravity flow or low-pressure syringe irrigation is preferred in the hand to avoid driving debris deeper into delicate tissue planes.
* Debridement: Devitalized tissue must be meticulously excised. However, the skin of the hand is highly specialized and irreplaceable. Unlike the aggressive excision of wound edges practiced in lower extremity trauma, complete excision of wound edges is usually unnecessary and contraindicated in the hand. Only frankly necrotic skin should be sharply debrided.
Foreign Body Identification and Extraction
As the deeper parts of the wound are cleansed, they are systematically explored for foreign materials.
* High clinical suspicion must be maintained for retained broken glass, wood splinters, or pieces of the patient's clothing or gloves.
* Gunshot wounds require careful assessment for retained wadding or clothing, which are highly niduses for infection, even if the bullet itself is sterile.
The "Redraping" Protocol
Once the rigorous cleaning and debridement phase is complete, the surgical field is considered transitioned from "dirty" to "clean." At this juncture, all instruments, gloves, and drapes used during the debridement process are discarded. The surgical team changes gowns and gloves, and the hand is formally re-prepped and redraped. This strict adherence to aseptic technique prevents the cross-contamination of deep anatomical structures during the reconstructive phase.
Intraoperative Anatomical Assessment
After converting the contaminated wound into a clean surgical field, the wound is systematically reexamined under tourniquet control and optimal lighting (often utilizing surgical loupes or an operating microscope).
Skin Viability and Soft Tissue Envelope
Evaluating skin damage is paramount because primary wound closure—and the protection of underlying structures—depends entirely on skin viability.
* Assessment Techniques: The circulatory status of the skin is assessed by observing color, capillary refill, and dermal bleeding after a needle or scalpel puncture. A Doppler probe can be utilized to confirm flow in larger vessels.
* The Illusion of Skin Loss: Frequently, skin appears to be missing when, in reality, it has merely retracted due to the elasticity of the dermal network. This is especially true of L-shaped lacerations or avulsion flaps on the dorsum of the hand.
* Crush vs. Avulsion: When skin is crushed or avulsed, the subdermal plexus is often destroyed. Flaps that appear pink initially may suffer from venous congestion or delayed arterial insufficiency. If viability is questionable, the surgeon must decide between delayed primary closure, application of a dermal regeneration template, or immediate flap coverage.
🚨 PITFALL: Tension in Hand Closure
Never close a hand wound under tension. The resulting edema will inevitably lead to skin necrosis, exposure of underlying tendons or hardware, and catastrophic infection. If the soft tissue envelope is inadequate, utilize skin grafts, local rotational flaps, or leave the wound open for delayed closure.
Osteoarticular Evaluation
Bones and joints are inspected directly to assess the true extent of the injury, which is often underestimated by plain radiographs.
* Bone Loss and Comminution: Assess the degree of cortical bone loss and the stability of the fracture fragments.
* Periosteal Stripping: The extent of periosteal stripping dictates the biological healing potential of the fracture. Severe stripping requires meticulous preservation of remaining soft tissue attachments.
* Fixation Strategy: This evaluation allows the surgeon to determine the advisability of internal fixation (e.g., K-wires, mini-fragment plates, or external fixation). Rigid internal fixation is often preferred in hand trauma to allow for early active mobilization of the joints, thereby preventing tendon adhesions and joint contractures.
Tendon, Nerve, and Vascular Exploration
Conclusions drawn from the preoperative clinical examination in the emergency department may be inaccurate due to patient pain, swelling, or lack of cooperation. Therefore, suspected tendon and nerve injuries must be definitively confirmed by direct visual inspection.
* Underestimation of Damage: It is a surgical axiom that the extent of deep tissue damage is usually underestimated preoperatively.
* Systematic Exploration: Tissues in the depths of the wound must be assessed in an orderly, anatomical manner. Trace the neurovascular bundles proximally and distally to the zone of injury.
* Tendon Retraction: Flexor tendons, particularly those lacerated in Zone II, may retract significantly into the palm or even the distal forearm due to the pull of the muscle belly. Retrieval must be performed atraumatically, often requiring proximal counter-incisions, to avoid damaging the delicate vincula and epitenon.
Conclusion
The initial evaluation and intraoperative assessment of acute hand trauma require a synthesis of anatomical mastery, biomechanical understanding, and meticulous surgical technique. By adhering to strict protocols for history taking, clinical examination, aggressive yet tissue-sparing debridement, and systematic anatomical exploration, the orthopedic surgeon lays the critical groundwork for successful reconstruction. The ultimate goal remains the restoration of a painless, stable, and functionally sensate hand, a process that begins the moment the patient enters the trauma bay.
You Might Also Like