Mastering Complex Upper Extremity Trauma: Tissue Repair, Arterial Management, and Soft Tissue Reconstruction
Key Takeaway
The management of complex upper extremity trauma requires a systematic approach to tissue repair, prioritizing skeletal stabilization followed by vascular, neural, and tendinous reconstruction. This guide outlines evidence-based protocols for managing arterial injuries, executing primary and delayed wound closures, and utilizing skin grafts. Emphasizing biomechanical restoration and meticulous soft tissue handling, these principles are essential for orthopedic surgeons aiming to maximize functional recovery and minimize complications in severe hand and forearm injuries.
PRINCIPLES OF UPPER EXTREMITY TRAUMA MANAGEMENT
The management of complex upper extremity trauma demands a rigorous, systematic approach to restore both the anatomical architecture and the intricate biomechanical function of the limb. Severe injuries—often involving a combination of osseous, vascular, neural, and soft tissue compromise—require the orthopedic surgeon to make critical intraoperative decisions regarding the sequence of repair, the viability of soft tissue envelopes, and the indications for limb salvage versus amputation.
This comprehensive guide delineates the evidence-based protocols for prioritizing tissue repair, managing major and minor arterial injuries, executing meticulous wound closures, and utilizing skin grafts and flaps in the traumatized upper extremity.
ORDER OF TISSUE REPAIR
Setting strict priorities for the repair of injured structures is the cornerstone of successful upper extremity reconstruction. A haphazard approach inevitably leads to compromised functional outcomes, severe contractures, and potential limb loss.
1. Radical Débridement and Wound Preparation
Before any reconstructive effort begins, the wound must be meticulously cleaned and débrided. The surgical field must be converted from a contaminated traumatic wound into a clean surgical wound. All devitalized tissue, foreign debris, and severely crushed margins must be excised.
Surgical Warning: Inadequate débridement is the primary cause of deep postoperative infection and reconstructive failure. When in doubt regarding tissue viability, err on the side of excision, or plan for a delayed primary closure after a 24- to 48-hour "second look."
2. Immediate Skeletal Stabilization
Once the wound is adequately prepared, the bony architecture must be reestablished immediately, or at the latest, within a few days after the wound becomes definitively clean.
Biomechanical Rationale:
Failure to achieve prompt skeletal stabilization allows the surrounding soft tissues to contract rapidly. Once soft tissue contracture occurs, delayed bone repair becomes technically demanding, often impossible without intercalary bone grafting, and significantly increases the risk of neurovascular tethering during reduction maneuvers. Even if definitive soft tissue closure is not immediately possible, rigid or semi-rigid skeletal stabilization must be achieved.
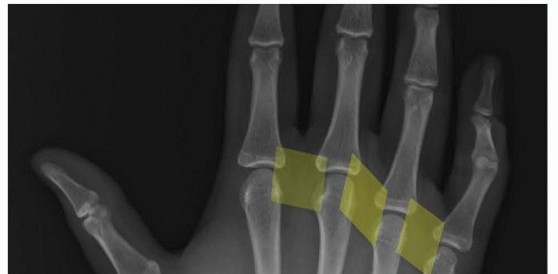
When reconstructing the hand, the surgeon must prioritize the stabilization of specific digital rays based on their primary biomechanical roles:
* The Thumb: Must be stabilized in a functional position to restore opposition, the foundation of all prehensile activities.
* The Index and Long Fingers: Must be stabilized to restore precise pinch and manipulation.
* The Ring and Small Fingers: Must be stabilized to restore power grasp.
3. Tendon and Nerve Repair
If the injury severity and wound conditions permit, tendons and nerves should be repaired at the time of primary or secondary skin closure (ideally within the first 5 days).
If immediate repair is contraindicated due to severe contamination or segmental loss, the surgeon must anticipate the inevitable retraction of these structures. Nerves, particularly in the fingers and palm, contract rapidly while awaiting delayed repair.
Clinical Pearl: To prevent severe retraction and facilitate future reconstruction, tag the transected nerve ends with a small, non-absorbable monofilament suture (e.g., 6-0 Prolene) anchored to the adjacent stable soft tissues of the palm or forearm. This simple step drastically reduces the dissection required during secondary reconstructive procedures.
MANAGEMENT OF ARTERIAL INJURIES
Vascular compromise in the upper extremity dictates the immediate trajectory of surgical intervention. The approach varies significantly depending on the anatomical level of the injury.
Major Proximal Arterial Trauma
Injuries to the major proximal vessels—specifically the subclavian, axillary, and brachial arteries—threaten the survival of the entire limb.
* Indications: Immediate diagnosis is paramount. Hard signs of arterial injury (pulsatile bleeding, expanding hematoma, absent distal pulses, palpable thrill/bruit, or distal ischemia) mandate emergent intervention.
* Protocol: Management includes emergent angiography (often performed on-table in the hybrid operating room) followed by immediate surgical exploration. Temporary vascular shunting may be required to restore perfusion while skeletal stabilization is performed, followed by definitive autogenous vein grafting or primary repair.
Forearm and Wrist Arterial Injuries (Radial and Ulnar)
The optimal management of isolated or combined injuries to the radial and ulnar arteries remains highly controversial.
The Role of the Palmar Arch:
If the superficial and deep palmar arterial arches are anatomically complete, hand survival and basic function are generally maintained even if one or both primary forearm arteries are transected. Unrepaired single-artery injuries typically cause insignificant changes in resting hand circulation.
Long-Term Sequelae and Cold Intolerance:
Despite adequate collateral perfusion for tissue survival, patients with unrepaired vessels frequently develop debilitating long-term symptoms.
* Cold Intolerance: At a 10-year follow-up, cold sensitivity that actively limited daily activities was reported by 78% of patients with various hand vascular injuries.
* Combined Injuries: The combination of an arterial transection with an adjacent peripheral nerve injury (e.g., ulnar artery and ulnar nerve at the wrist) exponentially increases the risk of disabling pain, weakness, and severe cold intolerance.
Surgical Pitfall: Do not dismiss a single-vessel injury simply because the hand appears well-perfused. In young, active patients, or those with concomitant nerve injuries, microsurgical repair of the radial or ulnar artery is strongly recommended to mitigate long-term cold sensitivity and claudication.
SOFT TISSUE COVERAGE AND WOUND CLOSURE
The ultimate goal of soft tissue management is to achieve a healed, pliable envelope that permits early tendon gliding and joint mobilization.
Primary Skin Closure
Primary skin closure is highly desirable and should be executed in all sharply incised, clean wounds.
* Benefits: Obtains early healing, prevents secondary infection, halts excessive granulation tissue formation, minimizes edema, and reduces hypertrophic scar production.
* Technique: Most clean lacerations without underlying tendon or nerve involvement can be closed by simple direct suture. The subcutaneous tissue is usually not sutured separately in the hand to avoid foreign body reactions, but meticulous care must be taken to avoid inversion of the skin edges. Careful hemostasis is non-negotiable; postoperative hematomas are a primary catalyst for infection and delayed healing.
Suture Considerations:
Sutures are, by definition, foreign bodies. They generate an inflammatory response, can interfere with local microcirculation, and increase the risk of infection. Therefore, the number and diameter of sutures used for wound closure should be kept to the absolute minimum necessary to approximate the edges without tension.
Dorsal Hand Defects:
The skin on the dorsal surface of the hand is highly mobile. A small, irregular skin defect in this region can often be converted into a transverse elliptical defect.
* Positioning: By extending the wrist fully, the dorsal skin is placed on maximum slack, allowing this transverse elliptical defect to be closed in a transverse line with minimal tension.
Contraindications to Primary Closure
Misjudgment in wound closure leads to catastrophic complications, including deep space infections, compartment syndrome, and the need for repeated, morbid débridements.
NEVER close the following wounds primarily:
1. Severely contaminated wounds.
2. Crush injuries caused by farm machinery or industrial augers.
3. Human or animal bites.
4. High-velocity missile or combat wounds.
5. Tornado missile injuries.
6. Wounds contaminated with feces or agricultural fertilizer.
Delayed Primary Closure and Negative Pressure Wound Therapy
When in doubt regarding contamination or tissue viability, the wound must be left open after careful anesthetic débridement.
- The "Second Look" Protocol: Within 24 to 48 hours, the patient is returned to the operating room. The wound is reinspected, re-débrided if necessary, and if sufficiently clean, closed by direct suture or skin grafting. Ideally, definitive closure should be achieved within 5 days of the initial injury.
- Negative Pressure Wound Therapy (NPWT): The use of a vacuum-assisted closure (VAC) system is highly beneficial in the interim. NPWT reduces wound volume, obliterates dead space, manages exudate, and promotes a robust granular bed.
- Secondary Intention: Generally, upper extremity wounds should not be left open to granulate and heal by secondary intention, as this leads to severe, restrictive scarring. The only exception is a wound that cannot be made sufficiently clean to accept a graft or flap.
SKIN GRAFTS AND FLAP CONSIDERATIONS
When primary closure is impossible due to tissue loss, but no deep avascular structures (bare nerves, tendons without paratenon, open joints, or cortical bone without periosteum) are exposed, the defect should be replaced immediately with a skin graft.
Autografts
Skin grafts obtained from the patient are categorized as either split-thickness skin grafts (STSG) or full-thickness skin grafts (FTSG). STSGs provide reliable coverage for large defects, while FTSGs are preferred for palmar surfaces to prevent severe secondary contracture.
Evaluating Flap Viability and Venous Congestion
Traumatic wounds often present with distally attached (retrograde) flaps of skin and subcutaneous tissue. While these flaps may appear to have enough surface area for primary closure, their survival is entirely dependent on adequate venous drainage.
The Pathophysiology of Flap Failure:
A distally based flap often lacks sufficient venous outflow. This deficient drainage causes rapid capillary engorgement and venous distention. If left unaddressed, this progresses to microvascular thrombosis and frank necrosis.
* Clinical Signs: The surgeon must monitor the color of the flap meticulously. A failing flap transitions from a deep blue (congestion) to purple (ischemia) and finally to black (necrosis).
Retrograde Flaps:
Retrograde flaps resulting from crushing, avulsion, or tearing injuries are at an exceptionally high risk of failure due to the microscopic intimal damage within the flap's pedicle.
* Anatomical Risk: A retrograde flap on the dorsal surface of the hand or forearm is significantly less likely to survive than a similarly sized flap on the highly vascularized palm.
* Surgical Decision: If any doubt exists regarding the viability or venous drainage of a traumatic flap, the compromised skin should be sharply excised and immediately replaced with a split-thickness skin graft.
CONSIDERATIONS FOR AMPUTATION
Despite the advanced reconstructive techniques detailed above, amputation remains a necessary consideration in the severely mangled upper extremity. The decision to amputate versus salvage is complex and must be individualized.
Key Indications for Amputation:
1. Life Over Limb: In the polytraumatized patient, prolonged reconstructive surgeries that threaten hemodynamic stability are contraindicated.
2. Irreversible Ischemia: Warm ischemia times exceeding 6 to 8 hours with massive muscle necrosis.
3. Complete Anatomical Disruption: Severe crush injuries with multi-level segmental bone loss, complete avulsion of the brachial plexus, and destruction of the soft tissue envelope where functional recovery is deemed impossible.
The ultimate goal of any upper extremity intervention—whether complex reconstruction or formal amputation—is to provide the patient with a painless, functional limb or residual stump that maximizes their quality of life and independence.
POSTOPERATIVE PROTOCOLS AND REHABILITATION
The success of complex upper extremity trauma surgery relies heavily on meticulous postoperative care.
* Immobilization and Elevation: Immediately post-surgery, the limb must be strictly elevated above heart level to minimize edema, which can compromise microvascular circulation and increase tension on surgical incisions.
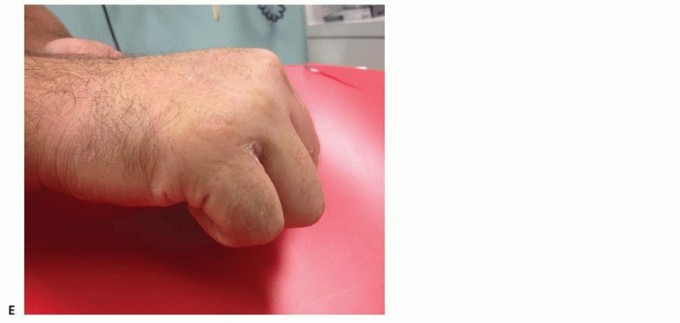
* Splinting: The hand should be splinted in the "intrinsic-plus" (safe) position—wrist extended 20-30 degrees, metacarpophalangeal (MCP) joints flexed 70-90 degrees, and interphalangeal (IP) joints fully extended—to prevent collateral ligament contracture.
* Early Motion: Under the guidance of a specialized hand therapist, early controlled passive or active motion protocols should be initiated as soon as skeletal and tendinous stability allows, preventing the debilitating adhesions that commonly plague severe hand trauma.
You Might Also Like