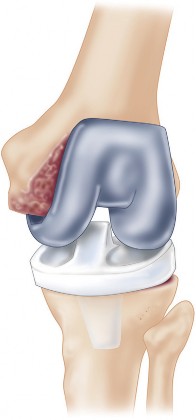
Total Joint Arthroplasty: Prosthesis Designs, Biomechanics, and Patient Indications
Key Takeaway
Successful total joint arthroplasty hinges on mastering prosthesis designs, understanding joint biomechanics, and judicious patient selection. Key factors include biomaterial science (metals, polymers, ceramics), fixation principles (cemented, cementless), load transmission, and specific anatomical considerations for joints like the hip. These ensure optimal function, durability, and minimized complications.
Introduction & Epidemiology
Total joint arthroplasty (TJA) represents one of the most successful and impactful surgical interventions in modern medicine, consistently demonstrating significant improvements in pain relief, functional restoration, and quality of life for patients suffering from end-stage degenerative or inflammatory arthropathies. The topic of "Mastering Various Prosthesis Designs & Patient Indications" is critical for the practicing orthopedic surgeon, resident, and medical student, as the landscape of arthroplasty continues to evolve with advancements in implant metallurgy, polymer science, surgical techniques, and patient-specific considerations.
The global burden of musculoskeletal diseases, particularly osteoarthritis (OA), is substantial and growing. Projections indicate a sustained increase in the demand for primary and revision total hip arthroplasty (THA) and total knee arthroplasty (TKA) over the coming decades. In the United States alone, the annual volume of primary THA and TKA procedures is estimated to exceed 1 million, driven by an aging population, rising prevalence of obesity, and expanding indications for surgery. This epidemiological trend necessitates a deep understanding of current implant technologies, their biomechanical principles, and the judicious selection of the most appropriate prosthesis for each individual patient to optimize long-term outcomes and minimize complications.
The historical progression of arthroplasty has seen revolutionary shifts, from early attempts with interpositional arthroplasty and metallic caps, through the pioneering work of Charnley and Marmor, to the highly specialized implant systems available today. These advancements have been characterized by improvements in biomaterial compatibility, fixation strategies (cemented, cementless, hybrid), bearing surface options (metal-on-polyethylene, ceramic-on-polyethylene, ceramic-on-ceramic), and component designs tailored to various anatomical and pathological presentations. A comprehensive mastery of these designs and their specific patient indications is paramount for achieving durable, functional results and mitigating common pitfalls.
Surgical Anatomy & Biomechanics
A thorough understanding of the surgical anatomy and joint biomechanics is foundational to successful arthroplasty. This knowledge guides prosthesis selection, surgical approach, bone preparation, and soft tissue balancing, all of which contribute to implant longevity and functional outcomes.
General Biomechanics of Joint Replacement
The primary goals of arthroplasty are to restore joint kinematics, achieve mechanical stability, distribute loads optimally across the prosthetic interface, and minimize wear.
*
Load Transmission & Stress Shielding:
Prostheses are designed to transmit physiological loads to the periprosthetic bone. Discrepancies in stiffness between the implant and bone can lead to stress shielding, potentially causing bone remodeling, bone loss, and aseptic loosening. Cementless stems, particularly those with proximal loading designs, aim to mitigate this.
*
Joint Contact Mechanics & Wear:
The interaction between bearing surfaces (e.g., femoral head and acetabular liner in THA, femoral condyles and tibial insert in TKA) dictates wear rates. High contact stresses can accelerate wear, leading to particulate debris, osteolysis, and implant failure. Modern materials like highly cross-linked polyethylene (XLPE) and ceramics are engineered to reduce wear.
*
Fixation Principles:
*
Cemented Fixation:
Relies on polymethylmethacrylate (PMMA) bone cement to create an immediate mechanical interlock with the bone. It's often favored in older patients with poorer bone quality (e.g., Dorr type C femur), where rapid mobilization is desired, and for its proven long-term results, particularly in the knee.
*
Cementless (Biologic) Fixation:
Utilizes porous or textured implant surfaces to encourage bony ingrowth (osseointegration). This requires good bone quality and an initial press-fit stability. Common in younger, more active patients with good bone stock. Coatings like hydroxyapatite or titanium plasma spray enhance osseointegration.
*
Material Science:
*
Metals:
Cobalt-chromium (CoCr) alloys for articulating surfaces and titanium (Ti) alloys for stems/shells due to excellent strength, corrosion resistance, and biocompatibility. Titanium alloys (e.g., Ti-6Al-4V) are particularly favored for cementless applications due to their lower modulus of elasticity, closer to bone, reducing stress shielding.
*
Polymers:
Ultra-high molecular weight polyethylene (UHMWPE) remains the gold standard for bearing surfaces. Advances in cross-linking and vitamin E incorporation have significantly reduced wear rates and oxidative degradation, respectively, in highly cross-linked polyethylene (XLPE).
*
Ceramics:
Alumina (Al2O3) and Zirconia (ZrO2) ceramics offer exceptional hardness, scratch resistance, and hydrophilicity, leading to very low wear rates, particularly in ceramic-on-ceramic (CoC) bearings. However, they carry a small risk of fracture and 'squeaking'.
Specific Joint Considerations
While the general principles apply, specific anatomical and biomechanical nuances dictate prosthesis design and selection for individual joints.
Hip Arthroplasty
- Acetabular Anatomy: Understanding native acetabular version (typically 15-20° anteversion) and inclination (40-45°) is crucial for optimal component placement, stability, and wear. Deformities such as protrusio acetabuli or severe dysplasia require specific consideration.
- Femoral Anatomy: Proximal femoral anatomy varies significantly (e.g., femoral offset, neck-shaft angle, femoral anteversion, canal shape - Dorr classification). Femoral stem designs (tapered wedge, cylindrical, anatomic, short stems) aim to restore offset and leg length while achieving stable fixation. Bone quality, particularly in the proximal femur, guides the choice between cemented and cementless stems.
- Soft Tissue Tension: Proper tensioning of the abductor mechanism and restoration of leg length are critical for preventing dislocation and restoring functional gait.
Knee Arthroplasty
- Alignment: Restoration of the mechanical axis of the limb, through precise bone cuts and soft tissue balancing, is paramount. This involves balancing varus/valgus alignment, flexion/extension gaps, and patellofemoral tracking.
- Ligamentous Stability: The integrity of the medial collateral ligament (MCL), lateral collateral ligament (LCL), and posterior cruciate ligament (PCL) significantly influences TKA design. Cruciate-retaining (CR) designs require a functional PCL, whereas posterior-stabilized (PS) designs resect the PCL and use a cam-post mechanism to provide posterior stability.
- Tibial Slope: Restoration of the native tibial slope is important for kinematics, particularly in CR knees.
- Patellofemoral Joint: Proper patellar tracking is essential to prevent anterior knee pain and periprosthetic fracture. Patellar component design and rotational alignment of femoral and tibial components impact this.

Indications & Contraindications
The decision to proceed with arthroplasty and the selection of a specific prosthesis design are complex, multifactorial choices based on a comprehensive assessment of the patient's symptoms, functional limitations, radiographic findings, comorbidities, and individual circumstances.
Primary Indication (General)
The overarching indication for total joint arthroplasty is symptomatic end-stage arthropathy (e.g., osteoarthritis, rheumatoid arthritis, avascular necrosis, post-traumatic arthritis, or other inflammatory arthritides) that is refractory to an adequate trial of non-operative management and significantly impairs the patient's quality of life, ambulation, and ability to perform activities of daily living.
Factors Influencing Prosthesis Choice
The selection of a specific prosthesis design is highly individualized and considers:
-
Patient Factors:
- Age: Younger, more active patients often receive cementless implants with durable bearing surfaces (e.g., XLPE, ceramic) to maximize longevity. Older, less active patients with poorer bone quality may benefit from cemented components.
- Activity Level: High-demand patients require robust designs and bearing surfaces with low wear rates.
- Bone Quality: Assessed by radiographs (e.g., Dorr classification for femur) and intra-operative findings. Poor bone stock may necessitate cemented fixation or specific implant geometries.
- Comorbidities: Renal failure, diabetes, immunosuppression, or significant cardiovascular disease can influence implant choice (e.g., avoiding MoM bearings in patients with renal impairment due to ion concerns) and surgical risk.
- Surgeon Experience & Preference: Familiarity with a particular system often correlates with better outcomes.
-
Disease Factors:
- Etiology of Arthritis: OA, RA, AVN, post-traumatic arthritis each have specific patterns of bone loss and deformity.
- Joint Deformity: Severe varus/valgus deformity, fixed contractures, or significant bone defects may require constrained prostheses, augments, or specific bone grafting techniques.
- Ligamentous Stability: Crucial for TKA; intact PCL for CR designs, otherwise PS or even more constrained options.
- Prior Surgeries: Previous osteotomies, fusions, or hardware may complicate exposure and necessitate specific revision implant designs.
Specific Prosthesis Designs & Indications
Total Hip Arthroplasty (THA)
-
Femoral Stem Designs:
- Cemented Stems: Indicated for older patients, poor bone quality (Dorr type C), or revision settings where cementless fixation is not achievable. Designs vary (e.g., polished taper slip, matte finish).
- Cementless Stems: Indicated for younger, active patients with good bone quality (Dorr type A/B). Designs include tapered wedge, cylindrical, fully coated, proximally coated, and short stems. Short stems aim to preserve proximal femoral bone stock and may be suitable for younger patients with proximal femoral anatomy that allows for stable fixation.
- Revision Stems: Longer, often extensively coated, or fluted stems for fixation distal to areas of bone loss in revision cases.
-
Acetabular Components:
- Cementless Shells: Porous-coated shells promoting osseointegration, often with modular liners. Standard for most primary THAs due to excellent long-term results.
- Cemented Cups: Rarely used in primary THA, primarily for patients with extremely poor bone quality where cementless fixation is not feasible, or in specific revision scenarios.
-
Bearing Surfaces:
- Metal-on-Polyethylene (MoP): Most common. XLPE has significantly reduced wear compared to conventional UHMWPE. Indicated across a broad patient demographic.
- Ceramic-on-Polyethylene (CoP): Combines the low wear of ceramic heads with XLPE liners. Increasingly popular, especially in younger patients, due to very low wear.
- Ceramic-on-Ceramic (CoC): Lowest wear rates, theoretically highest longevity. Indicated for very young, active patients with high expectations. Small risk of squeaking and brittle fracture.
- Metal-on-Metal (MoM): Largely abandoned due to concerns regarding metal ion release, pseudotumor formation, and high failure rates, particularly with large diameter heads. Historical context only.
Total Knee Arthroplasty (TKA)
- Cruciate Retaining (CR): Retains the PCL. Indicated when the PCL is healthy, balanced, and the patient has good patellar tracking. Aims to restore more natural knee kinematics.
- Posterior Stabilized (PS): Sacrifices the PCL. Utilizes a cam-post mechanism to provide posterior stability and prevent hyperextension. Indicated when the PCL is compromised, contracted, or when more robust stability is desired, or in cases of severe deformity.
- Unicompartmental Knee Arthroplasty (UKA): Replaces only the diseased compartment (medial or lateral). Indicated for isolated, end-stage unicompartmental arthritis with intact ligaments, correctable deformity (<10-15 degrees), absence of patellofemoral symptoms, and no inflammatory arthropathy. Benefits include less bone resection, faster recovery, and more natural kinematics.
- Constrained/Hinged Knee Systems: Used for cases with severe ligamentous insufficiency, significant bone loss, or complex revision scenarios where standard CR/PS implants cannot provide stability. These systems have a mechanical linkage between femoral and tibial components.
- Patellofemoral Arthroplasty (PFA): Replaces only the patellofemoral joint. Indicated for isolated patellofemoral arthritis without evidence of tibiofemoral involvement and good extensor mechanism.
General Contraindications
Absolute Contraindications:
* Active infection (local or systemic), including osteomyelitis, septic arthritis, or active skin infections near the surgical site.
* Rapidly progressive neurological disease that could lead to unstable joints or inability to participate in rehabilitation.
* Severely compromised extensor mechanism (for TKA).
* Recent myocardial infarction or stroke (within 3-6 months).
* Uncontrolled coagulopathy.
Relative Contraindications:
* Morbid obesity (BMI >40 kg/m²) due to increased risk of complications (infection, dislocation, loosening).
* Uncontrolled medical comorbidities (e.g., severe diabetes, renal failure, cardiac disease, pulmonary disease).
* Severe peripheral vascular disease.
* Severe psychiatric illness, substance abuse, or non-compliance.
* Severe malnutrition or obesity (can be optimized pre-operatively).
* Skeletally immature patients.
* Lack of patient motivation or inadequate social support for rehabilitation.
Operative vs. Non-Operative Indications
| Indication Category | Operative (Arthroplasty) | Non-Operative |
|---|---|---|
| Pain | Severe, chronic, disabling, refractory to conservative treatment | Mild-to-moderate, intermittent, responsive to conservative measures |
| Function | Significant impairment of ADLs, gait, mobility, and quality of life | Mild-to-moderate limitation, amenable to activity modification, physical therapy |
| Radiographic OA | Kellgren-Lawrence Grade III-IV, significant joint space narrowing, osteophytes, subchondral sclerosis/cysts, bone-on-bone | K-L Grade I-II, minimal changes, no significant deformity |
| Deformity | Fixed, progressive, significant varus/valgus malalignment (>10-15 degrees), flexion contracture | Correctable, minor malalignment, mild contracture, amenable to bracing |
| Ligamentous Stability | Joint instability causing functional impairment requiring prosthetic constraint or repair (e.g., PS TKA, revision TKA) | Stable joint, no significant laxity impacting function |
| Failed Prior Treatment | Yes (e.g., failed osteotomy, arthroscopy, prolonged conservative measures) | Initial presentation of symptoms, not yet exhausted conservative options |
| Patient Factors | Medically optimized, motivated, good bone stock (for uncemented), reasonable life expectancy, amenable to rehabilitation | Uncontrolled comorbidities, poor bone stock (may favor cemented or specific design), very high/low activity demands, poor compliance |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are critical for minimizing intra-operative complications, ensuring accurate implant placement, and achieving optimal outcomes.
Patient Optimization
- Medical Workup: Comprehensive medical evaluation by a primary care physician or internist to identify and optimize comorbidities (e.g., diabetes, hypertension, cardiac disease).
- Dental Clearance: Required to rule out dental pathology that could be a source of bacteremia and potential periprosthetic joint infection (PJI).
- Nutritional Status: Address malnutrition (e.g., albumin <3.5 g/dL) or severe obesity, as these are risk factors for complications. Pre-operative weight loss programs may be recommended for morbidly obese patients.
- Smoking Cessation: Patients should ideally cease smoking for at least 4-6 weeks pre-operatively to improve wound healing and reduce infection risk.
- Anemia Correction: Pre-operative iron supplementation or erythropoietin may be indicated to reduce the need for blood transfusions.
- Patient Education: Discuss realistic expectations, rehabilitation pathway, and potential risks and benefits.
Radiographic Templating
- Imaging: Standard AP pelvis (with calibration ball), lateral hip, full-length standing AP mechanical axis view of the lower extremities (for TKA, with patellae facing forward), and specific views like Rosenberg (flexion weight-bearing) or Merchant (patellofemoral) for knee planning.
-
Digital Templating:
Essential for accurate pre-operative sizing and positioning of components. It helps determine:
- THA: Femoral stem size and type, acetabular component size, leg length, femoral offset, and center of rotation.
- TKA: Femoral and tibial component sizes, restoration of mechanical axis, anticipated bone resections, and implant rotation.
- Templating assists in preventing leg length discrepancy, optimizing soft tissue tension, and ensuring appropriate implant inventory is available.
Surgical Approach Selection
The choice of surgical approach depends on the joint, planned prosthesis, surgeon's expertise, patient anatomy, and deformity.
*
THA Approaches:
*
Direct Anterior Approach (DAA):
Internervous plane (between sartorius/tensor fascia lata and rectus femoris/gluteus medius). Allows for supine positioning, potential for reduced gait disturbance, and intra-operative fluoroscopy for leg length and offset. Requires specialized instrumentation and experience.
*
Posterior Approach:
Internervous plane (between gluteus maximus and gluteus medius/minimus). Excellent extensile exposure, preserves abductor mechanism. Requires repair of external rotators and posterior capsule. Higher dislocation risk if repair is inadequate.
*
Direct Lateral/Anterolateral Approaches:
May be associated with a higher incidence of abductor weakness or limping. Less common for primary THA now.
*
TKA Approaches:
*
Medial Parapatellar:
Most common, excellent exposure.
*
Subvastus/Midvastus:
Muscle-sparing approaches, potentially less pain and faster recovery, but may be technically more challenging, especially in obese or muscular patients.
Instrument Selection & Setup
Ensure the specific implant system and corresponding instrumentation for the selected prosthesis designs are available and sterile. Pre-operative communication with the surgical team regarding implant preferences is crucial.
Patient Positioning
Proper positioning prevents iatrogenic injury (e.g., nerve compression, skin breakdown) and ensures optimal surgical exposure.
*
THA:
*
Supine (for DAA/Anterolateral):
May use a specialized traction table. Ensure careful padding of feet, knees, and elbows.
*
Lateral Decubitus (for Posterior/Direct Lateral):
Ensure stable support, careful padding of bony prominences (e.g., fibular head to prevent peroneal nerve palsy), axillary roll to prevent brachial plexus compression.
*
TKA:
*
Supine:
Standard. A bump or bolster under the ipsilateral hip allows for internal rotation. A foot block can assist with knee flexion/extension. Tourniquet application (high thigh) is standard practice. Careful padding of the contralateral limb and bony prominences.
Prophylaxis
- Antibiotic Prophylaxis: Administer intravenous antibiotics (typically a first-generation cephalosporin, e.g., Cefazolin) within 60 minutes prior to incision, and consider re-dosing for long procedures.
- DVT/PE Prophylaxis: Risk assessment for venous thromboembolism (VTE) to guide prophylaxis (mechanical compression devices, aspirin, DOACs, LMWH). Guidelines vary but emphasize combination therapy and early mobilization.
Detailed Surgical Approach / Technique
This section will detail general principles applicable to arthroplasty, followed by specific step-by-step techniques for THA (posterior approach) and TKA (medial parapatellar approach). The core tenets include meticulous soft tissue handling, precise bone preparation, accurate implant positioning, and appropriate soft tissue balancing.
General Principles
- Exposure: Adequate exposure is paramount but must balance visualization with minimizing soft tissue trauma.
- Hemostasis: Careful electrocautery and tissue dissection to minimize blood loss.
- Bone Preparation: Precise bone resections using jigs, guides, or navigation/robotics to achieve planned alignment and fit.
- Implant Insertion: Correct orientation and impaction/cementing technique are critical for primary stability and long-term fixation.
- Soft Tissue Balancing: Critical for stability, range of motion, and kinematics, especially in TKA.
Total Hip Arthroplasty (Example: Posterior Approach)
- Incision: A curvilinear incision centered over the greater trochanter, extending proximally towards the posterior superior iliac spine and distally along the femoral shaft.
-
Dissection:
- Skin and subcutaneous tissue.
- Incision of the fascia lata in line with the skin incision.
- Blunt splitting of the gluteus maximus fibers, identifying the underlying short external rotators.
- Internervous Plane: The posterior approach utilizes an internervous plane between the gluteus maximus (innervated by the inferior gluteal nerve) and the gluteus medius/minimus (innervated by the superior gluteal nerve). The sciatic nerve typically lies anterior to the piriformis and external rotators, deep to the gluteus maximus. Careful retraction is essential to protect it.
- Capsulotomy & External Rotator Release: Identify and tag the piriformis and conjoint tendons (gemelli, obturator internus, quadratus femoris) where they insert onto the greater trochanter. These are sharply released from their insertions, along with the posterior capsule, to allow for hip dislocation. Tagging these for later repair is crucial for post-operative stability.
- Femoral Neck Osteotomy: Dislocate the hip. Using pre-operative templating, measure from a reliable landmark (e.g., lesser trochanter) to determine the level of the femoral neck cut. Perform the osteotomy using an oscillating saw.
-
Acetabular Preparation:
- Expose the acetabulum using retractors.
- Progressively ream the acetabulum with hemispherical reamers, aiming for removal of diseased cartilage and subchondral bone, leaving a bleeding bone bed. The goal is to achieve an appropriate size for press-fit stability and the correct orientation (typically 40-45° inclination and 15-20° anteversion) using guides.
- Insert the cementless acetabular shell with impaction, ensuring initial press-fit. Ancillary screws may be used for additional fixation if primary stability is suboptimal.
- Insert the chosen polyethylene liner into the shell.
-
Femoral Preparation:
- Address the femoral canal. Remove remaining femoral neck osteophytes.
- Using femoral rasps (broaches) matching the chosen stem design, progressively ream the femoral canal to prepare for stem insertion. The final broach should provide a stable, snug fit.
- Perform trial reduction with trial components (femoral head, stem, acetabular liner). Assess stability, range of motion, and leg length. Adjust head length or stem size as needed.
- Insert the definitive femoral stem (cemented or uncemented). For cemented stems, meticulous cement technique is paramount (canal lavage, cement restrictor, pressurization). For cementless stems, firm impaction for primary press-fit stability.
- Attach the chosen femoral head to the stem taper.
- Reduction & Stability Assessment: Reduce the hip. Carefully assess for stability throughout the range of motion (flexion, extension, rotation). Test for impingement and re-verify leg length. The posterior capsule and external rotators are then repaired to the greater trochanter through drill holes or sutures, which is a critical step for reducing dislocation risk.
- Closure: Layered closure, including repair of the deep fascia, subcutaneous tissue, and skin.
Total Knee Arthroplasty (Example: Medial Parapatellar Approach)
- Incision: A straight anterior midline incision from several centimeters proximal to the patella to several centimeters distal to the tibial tubercle.
-
Arthrotomy & Patellar Eversion:
- Skin and subcutaneous tissue dissection.
- Medial parapatellar arthrotomy: Incision through the quadriceps tendon, medial retinaculum, and joint capsule, extending distally to the medial aspect of the patellar tendon.
- Evert the patella laterally to expose the femoral condyles and tibial plateau.
-
Bone Resections (Using Resection Jigs):
- Distal Femoral Resection: Use an intramedullary or extramedullary guide to determine the flexion-extension axis and resect the distal femur to restore the mechanical axis. This cut dictates the extension gap.
- Proximal Tibial Resection: Use an extramedullary guide to resect the proximal tibia, aiming for neutral varus/valgus alignment (typically 0-3 degrees varus) and appropriate posterior slope (3-7 degrees). This cut dictates the extension gap.
- Posterior Condylar Resections: Use guides to resect the posterior femoral condyles, which influences femoral rotation and the flexion gap.
-
Gap Balancing:
Crucial step for TKA. Assess the extension and flexion gaps with laminar spreaders or spacers.
- Extension Gap: Should be rectangular and symmetrical. Release tight structures (e.g., superficial MCL, posteromedial capsule for varus deformity; lateral capsule, popliteus, LCL for valgus deformity) as needed.
- Flexion Gap: Should also be rectangular and symmetrical. Femoral component rotation is critical here. External rotation of the femoral component relative to the epicondylar axis helps balance the flexion gap.
- The goal is to achieve symmetrical and balanced flexion and extension gaps.
-
Trial Components:
Insert trial femoral, tibial, and patellar components.
- Assess stability throughout the range of motion.
- Evaluate patellar tracking (the patella should track centrally without tilting or excessive lateral pull).
- Check for impinging soft tissues.
-
Implant Insertion:
- Prepare bone surfaces for cementation (pulse lavage, drying).
- Apply bone cement to the components and prepared bone surfaces (tibial baseplate, femoral component, patellar component).
- Insert the definitive components, ensuring proper orientation and seating. Remove excess cement.
- Insert the polyethylene tibial insert (fixed or mobile bearing).
- Closure: Layered closure. Carefully repair the medial parapatellar arthrotomy, ensuring adequate tension to prevent patellar instability. Close subcutaneous tissue and skin.
Complications & Management
Despite significant advancements, total joint arthroplasty is not without potential complications. A comprehensive understanding of these risks, their incidence, and effective management strategies is paramount for optimal patient care.
Intra-operative Complications
- Periprosthetic Fracture: Can occur during broaching, stem insertion, or reaming. Management depends on location, fracture pattern, and implant stability; may require wiring, plating, or revision to a longer stem.
- Neurovascular Injury: Rare but devastating. Popliteal artery injury during TKA or sciatic/femoral nerve palsy during THA. Prevention via careful retraction and anatomical awareness. Management involves urgent vascular or neural repair.
- Malpositioning of Components: Incorrect version/inclination of acetabular cup (THA) or malalignment of femoral/tibial components (TKA). Can lead to dislocation, impingement, accelerated wear, or stiffness. May require early revision if severe.
- Cement Extravasation: Especially in THA, cement can extravasate into surrounding soft tissues or pelvic structures. Managed by careful technique; severe cases may require removal if causing neurological symptoms.
Early Post-operative Complications
- Infection (Periprosthetic Joint Infection - PJI): The most feared complication. Can be superficial (wound infection) or deep (PJI). Diagnosis involves synovial fluid aspiration (cell count, differential, culture), serum inflammatory markers (ESR, CRP).
- Deep Vein Thrombosis (DVT) / Pulmonary Embolism (PE): Risk is reduced with prophylaxis, but remains a concern. Symptoms include leg swelling, pain, dyspnea, chest pain. Diagnosis via duplex ultrasound (DVT) or CT pulmonary angiography (PE).
- Dislocation (THA): Most common in the early post-operative period due to soft tissue laxity or non-compliance with precautions. Managed by closed reduction, but recurrent dislocations may require open reduction, soft tissue repair, or revision with more constrained components (e.g., dual mobility, larger heads).
- Wound Complications: Hematoma, seroma, dehiscence, necrosis. Managed with local wound care, drainage, debridement, or plastic surgery consultation.
- Periprosthetic Fracture: Occurs post-operatively, often due to falls. Classified (e.g., Vancouver classification for THA, Lewis-Rorabeck for TKA) and managed based on stability of implant and fracture pattern (ORIF vs. revision arthroplasty).
- Leg Length Discrepancy (THA): Perceived or actual. Up to 1-2 cm may be tolerated. Significant discrepancy (>2 cm) can cause gait disturbance, back pain. Management ranges from shoe lifts to revision.
- Stiffness / Arthrofibrosis (TKA): Limited range of motion. Can be due to inadequate rehabilitation, infection, or aggressive fibrotic response.
Late Post-operative Complications
- Aseptic Loosening: The most common long-term failure mechanism, resulting from breakdown of the bone-implant interface without infection. Often caused by wear debris leading to osteolysis. Symptoms include pain with activity. Diagnosed with radiographs, bone scan.
- Chronic Infection (PJI): Presents insidiously with chronic pain, swelling, or sinus tract. Requires aggressive management as detailed below.
- Wear: Polyethylene wear can lead to osteolysis (bone loss) and aseptic loosening. Ceramic wear is minimal but ceramics can fracture.
- Osteolysis: Periprosthetic bone loss due to inflammatory reaction to wear particles. Can compromise implant stability and lead to fracture.
- Periprosthetic Fracture: Often results from minor trauma in patients with osteolysis or stress risers.
- Component Subsidence: Particularly with cementless femoral stems. Early subsidence within the first 6-12 weeks can be acceptable if stable, but progressive subsidence indicates failure.
- Heterotopic Ossification (HO): Formation of mature bone in soft tissues around the joint. Can lead to stiffness and pain. Prophylaxis with NSAIDs or radiation, especially in high-risk patients.
Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (approx.) | Salvage Strategies |
|---|---|---|
| Periprosthetic Joint Infection (PJI) | 0.5-2% |
Acute (symptoms <3-6 weeks):
Debridement, antibiotics, implant retention (DAIR) if implant is stable and organism susceptible.
Chronic (symptoms >3-6 weeks): Two-stage exchange arthroplasty (explant, antibiotic spacer, prolonged IV antibiotics, reimplant); One-stage exchange (selected cases); Resection arthroplasty (salvage); Amputation (rare ultimate salvage). |
| Dislocation (THA) | 1-5% | Closed reduction; Open reduction with soft tissue repair/component revision (if malposition or soft tissue laxity); Dual mobility components or constrained liners (for recurrent dislocations). |
| Aseptic Loosening | 5-10% (10-15yr) | Component revision (femoral, acetabular, or both) with longer/different fixation stems, augments for bone loss; Address osteolysis. |
| Periprosthetic Fracture | 0.5-2% |
Stable implant, non-displaced fracture:
ORIF with plate/screws.
Unstable implant or displaced fracture: Revision arthroplasty with longer stem/constrained components, often with cable/plate fixation. |
| Deep Vein Thrombosis (DVT) / PE | 0.5-2% (symptomatic) | Therapeutic anticoagulation (LMWH, DOACs, Warfarin); Inferior Vena Cava (IVC) filter for recurrent PE or contraindications to anticoagulation. |
| Neurovascular Injury | <1% | Conservative management (e.g., nerve palsy, usually resolves); Surgical exploration/repair (rarely indicated, for transection or severe compression). Urgent vascular repair for arterial injury. |
| Arthrofibrosis/Stiffness (TKA) | 1-5% | Aggressive physiotherapy, often with dynamic splinting; Manipulation Under Anesthesia (MUA); Arthroscopic or open lysis of adhesions; Revision arthroplasty in recalcitrant cases. |
| Leg Length Discrepancy (THA) | 1-2 cm common, >2 cm problematic | Shoe lift for minor/moderate cases; Revision for severe functional impairment or recurrent dislocation (rarely). |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is an integral component of successful arthroplasty, aiming to restore strength, range of motion, and functional independence. Protocols are tailored to the joint, prosthesis design, surgical approach, and individual patient factors.
General Principles
- Early Mobilization: Initiating movement and weight-bearing as soon as safely possible helps prevent complications like DVT/PE, muscle atrophy, and joint stiffness.
- Pain Management: Adequate pain control is crucial to facilitate participation in physical therapy. A multimodal approach (opioids, NSAIDs, acetaminophen, nerve blocks) is typically employed.
- Progressive Weight-Bearing: Typically weight-bearing as tolerated (WBAT) immediately for most primary THA and TKA. Specific restrictions may apply for certain revision cases or unstable fixation.
- Range of Motion (ROM): Focus on achieving functional ROM specific to the joint.
- Strengthening: Progressive exercises to restore muscle strength around the joint.
- Patient Education: Reinforce precautions, activity modifications, and the importance of adherence to the exercise program.
Phase-Based Approach
Phase I (Acute Hospital Phase - Days 0-5)
- Goals: Pain control, DVT prophylaxis, independent transfers, initial ambulation, basic ROM exercises.
-
Interventions:
- Pain Management: Epidural, regional blocks, oral analgesics.
- DVT Prophylaxis: Mechanical (sequential compression devices) and pharmacological (aspirin, DOACs, LMWH).
- Mobility: Out of bed to chair on post-op day 0 or 1. Ambulation with assistive devices (walker) with weight-bearing as tolerated (WBAT) or specific restrictions.
- Exercises: Ankle pumps, isometric quadriceps sets, gluteal sets.
- THA Specific: Adherence to hip precautions (e.g., for posterior approach: no hip flexion > 90°, no adduction past midline, no internal rotation).
- TKA Specific: Continuous Passive Motion (CPM) machine may be used to aid flexion/extension, although evidence for its routine use is mixed. Active-assisted ROM exercises.
Phase II (Early Outpatient / Home Therapy - Weeks 1-6)
- Goals: Wean off assistive devices, improve gait pattern, increase ROM and strength, manage wound healing.
-
Interventions:
- Gait Training: Progress from walker to crutches/cane, then unassisted ambulation as tolerated. Focus on normal heel-toe pattern.
- Strengthening: Light resistance exercises (e.g., straight leg raises, hip abduction/adduction, knee flexion/extension with bands, partial squats).
- ROM: Continue active and passive ROM exercises. For TKA, target 0-120° flexion.
- Balance & Proprioception: Standing balance exercises, single-leg stance.
- Scar Management: Gentle massage once incision is healed.
- THA Specific: Continue hip precautions; focus on abductor strengthening.
- TKA Specific: Emphasize full knee extension; address patellar mobility.
Phase III (Advanced Outpatient - Weeks 6-12+)
- Goals: Return to functional activities, progress to higher-level strengthening and endurance, optimize overall functional capacity.
-
Interventions:
- Strengthening: Increased resistance, closed-chain exercises (e.g., wall squats, lunges), eccentric training.
- Cardiovascular Endurance: Stationary cycling, swimming, elliptical trainer.
- Functional Training: Stair climbing, uneven surfaces.
- Return to Activities: Gradual return to light recreational activities (e.g., walking, golf, doubles tennis - avoiding high-impact sports).
- Patient Education: Long-term implant care, activity modification to prolong implant life, recognition of potential complications.
Specific Considerations
- THA (Direct Anterior Approach): May have less restrictive precautions post-operatively, allowing for earlier return to some activities, but careful attention to abductor strength is still important.
- Revision Arthroplasty: Protocols may be more conservative, with delayed or protected weight-bearing depending on bone quality, fixation stability, and implant type.
- Unicompartmental Arthroplasty (UKA): Often associated with faster recovery and less intensive rehabilitation due to less invasive surgery and preservation of healthy tissues.
Summary of Key Literature / Guidelines
The practice of arthroplasty is constantly evolving, driven by ongoing research and evidence-based medicine. Staying abreast of key literature and clinical guidelines is essential for providing optimal patient care.
Evidence-Based Practice
The shift towards evidence-based medicine mandates that surgical decisions and rehabilitation protocols are supported by high-quality research. Level I evidence (meta-analyses of randomized controlled trials) provides the strongest support for interventions. Key areas of ongoing research include:
*
Implant Design & Materials:
Innovations in bearing surfaces (e.g., highly cross-linked polyethylene, vitamin E-blended polyethylene), stem geometries, and porous coatings continue to be investigated for their impact on wear, osteolysis, and implant longevity.
*
Surgical Approaches:
Comparative effectiveness of different surgical approaches (e.g., DAA vs. posterior for THA) on outcomes such as dislocation rates, functional recovery, and pain.
*
Pain Management:
Optimal multimodal analgesia protocols, including regional nerve blocks and pre-emptive analgesia, to reduce opioid consumption and improve early rehabilitation.
*
Infection Prevention:
Development of comprehensive surgical site infection (SSI) bundles, including skin preparation, antibiotic prophylaxis, surgical environment controls, and wound management.
*
Technology Integration:
The role of computer navigation, robotics, and patient-specific instrumentation in improving component alignment and potentially long-term outcomes.
Major Societal Guidelines
Several professional organizations provide clinical practice guidelines (CPGs) that synthesize current evidence and offer recommendations for arthroplasty. Adherence to these guidelines helps standardize care and improve outcomes.
- American Academy of Orthopaedic Surgeons (AAOS): Publishes comprehensive CPGs for THA and TKA, covering indications, pre-operative optimization, VTE prophylaxis, infection prevention, and rehabilitation. These guidelines are regularly updated.
- National Institute for Health and Care Excellence (NICE): UK-based organization providing evidence-based guidelines, including those for hip and knee replacement, often with a focus on cost-effectiveness and patient pathways.
- American Heart Association (AHA) / American College of Cardiology (ACC): Provides guidelines for cardiac evaluation and management in non-cardiac surgery, relevant for pre-operative medical optimization.
- Infectious Diseases Society of America (IDSA): Offers guidelines for the diagnosis and management of periprosthetic joint infections, which are critical for timely and effective treatment.
Landmark Studies & Concepts
- Charnley's Work: Pioneering work in low-friction arthroplasty established the principles of modern THA using cement fixation and metal-on-polyethylene bearings, demonstrating the durability of cemented implants.
- Evolution of Polyethylene: The development of highly cross-linked polyethylene (XLPE) in the late 1990s and early 2000s marked a significant advance in reducing wear rates and subsequent osteolysis, revolutionizing the longevity expectations for THA and TKA. Subsequent research into vitamin E blending further mitigated oxidative degradation.
- Cemented vs. Cementless Fixation: Ongoing debate, with evidence suggesting excellent long-term outcomes for both. Cemented THA remains highly successful in older patients, while cementless THA is favored in younger, active patients with good bone quality. TKA predominantly utilizes cemented fixation, with cementless TKA having niche indications.
- THA Surgical Approaches: Studies comparing DAA, posterior, and lateral approaches continue to refine understanding of their respective benefits and risks regarding dislocation, functional recovery, and complications.
- PCL Retention vs. Sacrifice (TKA): While PS designs (PCL sacrificing) have historically been more common, CR designs (PCL retaining) are often chosen to restore more natural kinematics in select patients. Functional outcomes tend to be similar in many series.
- Robotics and Navigation: Meta-analyses and randomized trials are increasingly demonstrating the capability of robotic and navigation systems to improve implant alignment and accuracy in both THA and TKA, though the long-term clinical benefits in terms of patient-reported outcomes and implant survival are still being rigorously evaluated.
The landscape of arthroplasty remains dynamic, underscoring the necessity for orthopedic surgeons to engage in continuous learning, critically evaluate new technologies, and adhere to established, evidence-based practices to ensure the best possible outcomes for our patients.
You Might Also Like