Clinodactyly: Understanding Pathology, Biomechanics, and Management Options
Key Takeaway
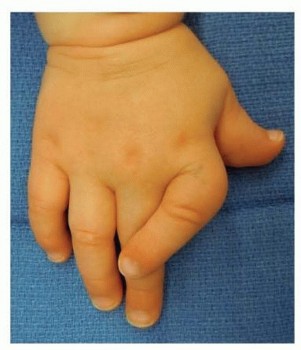
Clinodactyly is a congenital digit angulation, often of the small finger, caused by an abnormal physis like a delta phalanx. Surgical intervention is considered for angulations greater than 15-20 degrees causing functional impairment, progressive deformity, adjacent finger impingement, or significant aesthetic/psychosocial distress, balancing risks with patient-specific needs.
Is Clinodactyly Surgical Treatment Right for You?
Introduction & Epidemiology
Clinodactyly refers to an abnormal radioulnar angulation of a digit, typically defined as greater than 15 degrees in the coronal plane. While any digit can be affected, the small finger is most commonly observed, often presenting bilaterally. This congenital or developmental deformity, frequently overlooked in its mild forms, warrants meticulous evaluation when considering intervention.
The epidemiology of clinodactyly is challenging to ascertain precisely due to the high incidence of asymptomatic cases that do not present for medical evaluation. Reported prevalence rates vary widely, generally ranging from 1-10% of the population, often as an incidental finding. It is an autosomal dominant condition with variable penetrance, meaning that affected individuals have a 50% chance of passing the gene to their offspring, but the severity of expression can differ significantly even within the same family.
Clinodactyly may present as an isolated anomaly or as a component of various genetic syndromes. While often sporadic, its association with conditions such as Down syndrome (Trisomy 21), Apert syndrome, Poland syndrome, Fanconi anemia, and other chromosomal abnormalities underscores the importance of thorough clinical and genetic workup, particularly in cases of severe or multiple digit involvement. The angulation can significantly impact hand function, particularly precision grip and power grasp, and may lead to adjacent finger impingement, snagging, or aesthetic concerns that affect a patient's self-image and psychosocial well-being. The decision for surgical correction is therefore multifaceted, weighing functional impairment, progressive deformity, cosmetic considerations, and the patient's age and overall health.
Surgical Anatomy & Biomechanics
The finger consists of three phalanges: the proximal (p1), middle (p2), and distal (p3), with the exception of the thumb, which typically has two. The normal phalangeal physis (growth plate) is located at the proximal portion of each phalanx, responsible for longitudinal bone growth. In clinodactyly, the angulation is a result of abnormal development of one of the phalanges, most commonly the middle phalanx (p2) of the small finger.
Pathogenesis of Angulation
The anatomical basis for clinodactyly frequently involves an irregular physis, often referred to as a longitudinal bracket epiphysis or a delta phalanx . This anomaly is characterized by a C-shaped or triangular epiphysis that extends longitudinally along the metaphysis, effectively tethering one side of the phalanx. The tethering effect of this bracket epiphysis on the radial or ulnar side of the finger causes asymmetrical growth of the phalanx, resulting in a triangular or trapezoidal shape. This abnormal growth pattern leads to the characteristic radioulnar angulation. In some cases, extra ossicles or supernumerary phalanges may also be encountered, further complicating the anatomy and contributing to the deformity.
Finger Biomechanics
The intricate biomechanics of the hand rely on the precise alignment and coordinated movement of its constituent parts. Clinodactyly disrupts this delicate balance.
*
Grip and Pinch:
Angulation, particularly in the small finger, can significantly impair the ability to form a complete and powerful grip. The deviating digit may interfere with the adjacent ring finger, reducing the effective contact surface during power grasp. Precision pinch, vital for fine motor tasks, can also be compromised if the angulation affects the ability to oppose the thumb effectively or if it causes the finger to "hook" or snag objects.
*
Rotational Deformity:
While primarily a coronal plane deformity, the abnormal growth of the delta phalanx can also induce a rotational component, further exacerbating functional limitations and cosmetic concerns.
*
Adjacent Joint Mechanics:
Chronic angulation can lead to adaptive changes in the soft tissues and articular cartilage of adjacent interphalangeal joints, potentially predisposing to premature degenerative changes.
*
Neurovascular Bundles:
The neurovascular bundles run along the radial and ulnar aspects of each digit, supplying sensation and blood flow. During surgical correction, these structures are critically important to identify and protect. The digital nerves are particularly susceptible to traction or direct injury during subperiosteal dissection or osteotomy.
Natural History
The natural history of clinodactyly is variable and, owing to the large number of asymptomatic cases, poorly documented in its entirety. Angulation may remain stable throughout life, particularly if the physeal involvement is minimal or if the deformity is mild. However, it can also be rapidly progressive, especially during periods of accelerated skeletal growth (e.g., infancy, early childhood, and adolescent growth spurts). The extent of physeal involvement and/or the presence of extra phalanges are key determinants of progression. Close clinical and radiographic monitoring is essential, particularly in pediatric patients with open physes, to identify rapidly progressing deformities that may warrant earlier intervention.
Indications & Contraindications
The decision to proceed with surgical correction of clinodactyly is highly individualized, balancing the severity of the deformity, functional impairment, psychosocial impact, and patient/parent expectations against the potential risks and benefits of surgery.
Non-Operative Indications
- Mild Angulation: Deformities less than 15-20 degrees that are not causing functional limitation or aesthetic distress are generally managed non-operatively.
- Asymptomatic Presentation: Absence of pain, impingement, or difficulty with daily activities.
- Stable Deformity: Documented evidence of non-progression over time, particularly outside periods of rapid growth.
- Patient/Parent Preference: A well-informed decision to observe, accepting the current state of the digit.
- Absence of Associated Deformities: No other hand conditions requiring surgical correction concurrently.
Operative Indications
- Progressive Angulation: Documented increase in the degree of deformity over time, especially during growth spurts. This is a strong indicator for surgical intervention, often favoring growth modulation techniques in skeletally immature patients.
- Significant Angulation: Deformities typically exceeding 15-20 degrees, and particularly those >30 degrees, regardless of current functional impact, due to the high likelihood of future issues.
-
Functional Impairment:
- Impediment to Grip/Pinch: The affected digit physically interferes with the function of adjacent fingers or prevents effective grasping of objects (e.g., "hooking" or snagging).
- Difficulty with Tool Use: Impaired ability to hold pens, utensils, or other instruments.
- Adjacent Finger Impingement: The deviating digit pushes against or is trapped by an adjacent finger, causing discomfort or preventing full flexion.
- Cosmetic Concerns: While subjective, significant cosmetic deformity that causes psychological distress or social anxiety, particularly in adolescents, can be a valid indication for surgery. This must be balanced against objective functional concerns and realistic expectations.
- Pain: Although less common, pain can result from chronic impingement or stress on soft tissues.
- Associated Deformities: Clinodactyly occurring as part of a complex hand malformation where overall functional improvement necessitates its correction.
Contraindications
- Mild, Non-Progressive, Asymptomatic Cases: No compelling reason for surgical intervention.
- Significant Medical Comorbidities: Conditions that preclude safe anesthesia or surgery, or significantly increase perioperative risks.
- Unrealistic Patient/Parent Expectations: Inability to achieve a satisfactory outcome due to pre-existing conditions or patient expectations that cannot be met. A thorough discussion of potential outcomes, including residual deformity, is crucial.
- Active Local or Systemic Infection: Requires resolution prior to elective surgery.
- Very Young Age: In certain scenarios, waiting until the child is older for a more definitive correction or to better assess growth potential may be preferred, though growth modulation techniques can be performed in younger children.
Operative vs. Non-Operative Indications
| Indication Category | Operative Treatment | Non-Operative Treatment |
|---|---|---|
| Angulation Severity | >15-20 degrees (especially >30 degrees); objectively increasing deformity. | <15-20 degrees; stable deformity. |
| Progression | Documented progression of angulation over time, particularly during growth spurts. | No documented progression; stable over follow-up periods. |
| Functional Impairment | Interference with grip, pinch, object manipulation; adjacent finger impingement; snagging; pain. | No functional limitations; full range of motion; no pain or impingement. |
| Cosmetic Concern | Significant cosmetic deformity leading to psychosocial distress (especially in adolescents). | Mild cosmetic concern or patient/parent acceptance of the appearance. |
| Patient Age | Skeletally immature patients (for growth modulation); skeletally mature patients (for osteotomy). | Very young patients where monitoring is preferred before definitive intervention; patients nearing skeletal maturity with mild, stable deformities. |
| Associated Pathology | Clinodactyly contributing to overall hand dysfunction in complex syndromic conditions. | Isolated clinodactyly without other significant hand anomalies or systemic conditions requiring correction. |
| Expectations | Realistic expectations for improved function and cosmesis, understanding potential for residual deformity and complications. | Patient/parent understanding and acceptance of the condition, opting for observation and management of any secondary issues (e.g., skin irritation). |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is paramount for successful outcomes in clinodactyly correction. This involves a comprehensive clinical assessment, detailed imaging, and careful surgical strategy development.
Clinical Assessment
- Detailed History: Ascertain the age of onset, progression of deformity, presence of pain, functional limitations (e.g., difficulty with fine motor tasks, grip, or adjacent finger impingement), and any associated medical conditions or genetic syndromes. Family history of clinodactyly or other congenital anomalies is pertinent.
-
Physical Examination:
- Inspection: Assess the degree of angulation in the coronal plane, note any rotational component, examine the skin for creases or dimples that may indicate underlying skeletal abnormalities, and look for associated digital or hand deformities. Note which phalanx is primarily affected (most often the middle phalanx).
- Palpation: Check for tenderness or unusual bony prominences.
- Range of Motion: Evaluate active and passive range of motion of the affected digit's interphalangeal and metacarpophalangeal joints, as well as adjacent digits, to assess for stiffness or compensatory movements.
- Neurovascular Status: Document sensation and capillary refill.
- Hand Function: Observe the patient performing various tasks such as grasping, pinching, and making a full fist to identify specific functional limitations.
- Bilateral Assessment: Always examine the contralateral hand, as clinodactyly is frequently bilateral.
Imaging
-
Radiographs:
-
Standard Views:
High-quality anteroposterior (AP), lateral, and oblique views of the affected digit and the entire hand. These images are crucial for:
- Confirming the diagnosis and identifying the involved phalanx.
- Measuring the degree of angulation.
- Assessing the morphology of the physis (delta phalanx, longitudinal bracket epiphysis).
- Evaluating bone age and physeal status (open, closing, or closed).
- Identifying any associated skeletal anomalies (e.g., extra ossicles, brachydactyly, syndactyly).
- Full Length Phalangeal Views: To accurately measure angulation and plan osteotomy sites.
- Stress Views: Rarely necessary, but can be helpful in ambiguous cases to assess flexibility or instability.
-
Standard Views:
High-quality anteroposterior (AP), lateral, and oblique views of the affected digit and the entire hand. These images are crucial for:
-
Specialized Imaging:
- Computed Tomography (CT) Scan: Indicated for complex delta phalanges or significant rotational deformities to provide a detailed 3D reconstruction of the bone morphology, aiding in precise osteotomy planning.
- Magnetic Resonance Imaging (MRI): Useful in younger patients to assess the status of the growth plate, detect physeal bars, and differentiate cartilaginous anomalies not visible on plain radiographs.
-

Surgical Strategy
The surgical approach is determined by the patient's age, the degree of deformity, the presence and morphology of a delta phalanx, and the status of the physes.
-
Skeletally Immature Patients (Open Physes):
- Growth Modulation: Excision of the delta phalanx (physeal bar resection) with or without fat/silicone interposition is preferred to allow for continued physiological growth and gradual correction. This is often indicated for progressive deformities or significant angulation in young children.
- Corrective Osteotomy: May be considered if angulation is severe or if growth modulation alone is unlikely to achieve full correction, though typically delayed until nearer skeletal maturity to minimize recurrence.
-
Skeletally Mature Patients (Closed Physes) or Near-Mature Adolescents:
- Corrective Osteotomy: The primary method for correction, typically a closing wedge osteotomy, to acutely correct the angulation. The osteotomy type (closing wedge, opening wedge, dome) and fixation method (K-wires, screws, plates) are planned based on the specific deformity and surgeon preference.
Patient Positioning
- Supine Position: The patient is positioned supine on the operating table.
- Hand Table: The affected upper extremity is placed on a dedicated hand table, ensuring comfortable and stable positioning.
- Tourniquet: A pneumatic upper arm tourniquet is applied to provide a bloodless field, typically inflated to 250-300 mmHg or 100 mmHg above systolic pressure.
- Padding: All pressure points are carefully padded to prevent nerve injury.
- C-arm: Fluoroscopy (C-arm) should be readily available and draped sterilely for intraoperative verification of correction and hardware placement.
- Magnification: Surgical loupes (2.5x to 4x) are highly recommended for detailed dissection and protection of neurovascular structures.
Detailed Surgical Approach / Technique
The surgical correction of clinodactyly requires precision, meticulous dissection, and careful attention to digital anatomy. The choice of technique depends heavily on the patient's age, the etiology of the deformity, and the severity of angulation.
General Principles
- Aseptic Technique: Strict adherence to sterile principles is paramount.
- Magnification: Use of surgical loupes (2.5x to 4x) is strongly advised to facilitate visualization of delicate neurovascular structures and precise osteotomy cuts.
- Delicate Tissue Handling: Gentle handling of soft tissues, particularly the periosteum and digital neurovascular bundles, is essential to minimize scarring and complications.
- Bloodless Field: A pneumatic tourniquet is used to optimize visualization.
Approach to Delta Phalanx / Growth Modulation (Skeletally Immature Patients)
For younger patients with an open physis and a demonstrable delta phalanx, the goal is to excise the tethering abnormal physis to allow the unaffected side of the growth plate to "catch up."
- Incision: A longitudinal incision is made over the concave (tethered) aspect of the affected phalanx, typically centered over the middle phalanx (p2). A zigzag or curvilinear incision may be preferred to avoid scar contracture.
- Dissection: Careful dissection through the subcutaneous tissue. The digital neurovascular bundles, running along the radial and ulnar aspects of the digit, must be identified and gently retracted. In a small finger clinodactyly with radial angulation, the radial digital nerve and artery will be in the immediate vicinity of the planned resection.
- Periosteal Incision: The periosteum is incised longitudinally over the delta phalanx and carefully elevated subperiosteally to expose the abnormal physis.
-
Excision of Delta Phalanx / Physeal Bar Resection:
Under fluoroscopic guidance, the longitudinally oriented cartilaginous or bony bar (delta phalanx) responsible for the tethering is identified. A high-speed burr or fine osteotome is used to excise this abnormal physeal tissue. The goal is complete removal of the tethering bar while preserving the remaining healthy physis on the convex side. The bone edges should be smoothed.
-
 - The cavity created by the excision can be filled with an interposition material such as fat graft harvested locally, silicone, or even bone wax, to prevent recurrence of the physeal bar. This prevents bony bridging and allows for continued growth.
-
- Temporary K-wire Stabilization (Optional): In some cases, a single smooth K-wire may be placed across the osteotomy site or across the interphalangeal joint to maintain alignment temporarily, especially if significant acute correction was achieved.
- Closure: The periosteum is loosely closed, followed by subcutaneous tissue and skin closure.
Corrective Osteotomy (Skeletally Mature or Near-Mature Patients)
For older patients with closed or near-closed physes, an osteotomy is the primary method to achieve acute correction of the angular deformity.
- Incision: Similar to the growth modulation approach, a longitudinal or zigzag incision is made over the affected phalanx, typically on the dorsoradial or dorsoulnar aspect depending on the direction of angulation.
- Dissection & Neurovascular Protection: Subcutaneous dissection to identify and protect the digital neurovascular bundles.
- Periosteal Incision & Exposure: The periosteum is incised longitudinally and elevated subperiosteally to expose the bone.
-
Osteotomy Planning:
The precise location and orientation of the osteotomy are crucial. It is typically performed at the apex of the deformity, which is often in the middle phalanx. Pre-operative templating using radiographs helps determine the size and shape of the wedge to be resected.
-
Closing Wedge Osteotomy:
This is the most common technique. A wedge of bone, with its base on the concave side of the deformity, is resected. The size of the wedge is calculated to achieve the desired correction. The cuts are made using a fine osteotome or oscillating saw. Care must be taken to prevent thermal necrosis.
-
 -

-
- Opening Wedge Osteotomy: Less frequently used, primarily if a slight lengthening effect is desired or if there is significant soft tissue contracture on the concave side. This requires bone grafting from a suitable donor site (e.g., distal radius, olecranon, iliac crest).
- Dome Osteotomy: A curvilinear or dome-shaped osteotomy offers the advantage of allowing for multiplanar correction (angulation and rotation) and avoids sharp bony corners, which can be beneficial for stability and periosteal healing. However, it requires precise execution and a specialized saw.
-
Closing Wedge Osteotomy:
This is the most common technique. A wedge of bone, with its base on the concave side of the deformity, is resected. The size of the wedge is calculated to achieve the desired correction. The cuts are made using a fine osteotome or oscillating saw. Care must be taken to prevent thermal necrosis.
-
Correction & Fixation:
- Once the osteotomy is performed, the phalanx is carefully manipulated to correct the angulation.
-
K-wires:
Smooth or threaded K-wires (typically 0.028" to 0.045" or 0.7mm to 1.1mm) are the most common method of fixation. They are inserted across the osteotomy site in a cross-pin or parallel fashion to achieve rotational and angular stability. The pins are bent and cut externally.
-

-
- Screws: Small fragment screws (e.g., 1.5mm or 2.0mm cortical screws) can provide more rigid internal fixation, particularly in larger digits or if early mobilization is desired. However, they require precise placement and adequate bone stock.
- Mini-Plates: Rarely used for isolated clinodactyly in digits, but may be considered for complex multi-fragment osteotomies or revisions.
- Intraoperative Fluoroscopy: Essential to confirm accurate correction of angulation and stable placement of fixation hardware.
- Soft Tissue Release (Adjunctive): If severe soft tissue contracture is present on the concave side, a limited release of the skin, fascia, or joint capsule may be performed to facilitate correction, but this is uncommon for isolated clinodactyly.
- Closure: The periosteum is loosely approximated if possible, followed by subcutaneous tissue and skin closure.
Pearls and Pitfalls
- Neurovascular Injury: The most critical pitfall. Always visualize and protect digital neurovascular bundles. Dissect parallel to these structures.
- Incomplete Correction: Due to inadequate wedge resection or insufficient physeal bar removal. Re-evaluation with fluoroscopy is crucial before closure.
- Overcorrection: Can lead to a compensatory deformity in the opposite direction. Careful pre-operative planning and intraoperative assessment prevent this.
- Unstable Fixation: Can lead to loss of correction, nonunion, or malunion. Ensure adequate K-wire purchase in both fragments.
- Physeal Damage: In skeletally immature patients, aggressive dissection or misdirected K-wires can damage the remaining healthy physis, leading to growth arrest or secondary deformity.
Complications & Management
Despite meticulous surgical technique, complications can arise in the management of clinodactyly. Understanding their incidence and having robust salvage strategies is crucial.
General Surgical Complications
- Infection: Superficial or deep wound infection. Incidence is low in elective hand surgery (<2-5%). Management involves wound care, antibiotics, and potentially debridement.
- Hematoma: Accumulation of blood, leading to swelling and pain. Management typically involves compression, elevation, and rarely, evacuation.
- Nerve Injury: Direct trauma, traction, or compression to digital nerves. Incidence is low but significant. Management ranges from observation for neuropraxia to microsurgical repair for transection.
- Vascular Injury: Damage to digital arteries, leading to ischemia. Rare. Management involves microsurgical repair.
Specific Complications in Clinodactyly Surgery
-
Recurrence of Deformity:
- Incidence: Varies depending on age and technique, higher in younger patients with unaddressed physeal activity. Reported rates can be 5-30%.
- Etiology: Incomplete resection of the delta phalanx/physeal bar, inadequate initial correction, continued asymmetrical growth if the entire physis was not addressed or if a subtle longitudinal bracket epiphysis was missed.
- Salvage Strategy: Re-evaluation with radiographs. For skeletally immature patients, repeat physeal bar resection and interposition. For skeletally mature patients, revision corrective osteotomy.
-
Overcorrection/Undercorrection:
- Incidence: Reflects planning errors, potentially 5-10%.
- Etiology: Inaccurate wedge resection, misjudgment of physeal growth potential.
- Salvage Strategy: Revision osteotomy once bone healing is stable.
-
Nonunion/Malunion:
- Incidence: Low with stable fixation (1-5%).
- Etiology: Inadequate fixation, infection, poor bone healing potential, excessive motion, or reamed bone loss.
- Salvage Strategy: Nonunion requires revision surgery with stable fixation, bone grafting (autograft or allograft), and sometimes plate fixation. Malunion may require corrective osteotomy.
-
Physeal Arrest/Growth Disturbance:
- Incidence: Specific to growth modulation techniques, can occur if the healthy portion of the physis is inadvertently damaged during surgery.
- Etiology: Thermal injury during osteotomy, direct trauma from instruments or K-wires, infection.
- Salvage Strategy: If growth arrest leads to significant angular deformity or shortening, late corrective osteotomy or epiphysiodesis of the contralateral side of the physis may be considered.
-
Stiffness/Reduced Range of Motion (ROM):
- Incidence: Common to some degree after any digital surgery requiring immobilization, especially if prolonged. Up to 20%.
- Etiology: Prolonged immobilization, scar formation around tendons or joint capsules, direct trauma to joints.
- Salvage Strategy: Intensive hand therapy, including active and passive ROM exercises, scar massage, dynamic splinting. Tenolysis or capsulectomy are rare, late options.
-
Hardware Complications:
- Incidence: Common with K-wires (migration, breakage, pin tract infection) up to 10-20%.
- Etiology: Insufficient K-wire purchase, patient activity, inadequate pin care.
- Salvage Strategy: Early K-wire removal if infected or migrating. Replacement if fixation is lost. Oral antibiotics for pin tract infections.
-
Neurovascular Injury:
- Incidence: Rare but potentially devastating.
- Etiology: Direct transection, crushing, or traction injury during dissection or osteotomy.
- Salvage Strategy: Immediate microsurgical repair for transection. Observation for neuropraxia. Symptomatic management for chronic nerve pain.
- Bone Overgrowth: Especially at the site of delta phalanx resection, can lead to recurrence.
Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Approx.) | Etiology | Salvage Strategy |
|---|---|---|---|
| Recurrence of Deformity | 5-30% | Incomplete delta phalanx resection; unaddressed physeal activity; inadequate initial correction. | Revision physeal bar resection (immature); revision corrective osteotomy (mature). |
| Undercorrection/Overcorrection | 5-10% | Planning errors; inaccurate osteotomy; misjudgment of growth. | Revision osteotomy once bone healing is stable. |
| Nonunion/Malunion | 1-5% | Unstable fixation; infection; poor bone healing; excessive motion. | Revision fixation; bone grafting for nonunion; corrective osteotomy for malunion. |
| Physeal Arrest/Growth Disturb. | Varies, specific to growth modulation | Trauma to healthy physis during surgery; infection. | Late corrective osteotomy; contralateral epiphysiodesis if significant limb length discrepancy. |
| Stiffness/Reduced ROM | Up to 20% | Prolonged immobilization; scar formation; direct joint trauma. | Intensive hand therapy; dynamic splinting; rarely tenolysis/capsulectomy. |
| Hardware Complications | 10-20% | K-wire migration/breakage; pin tract infection; screw loosening. | Early K-wire removal/replacement; oral antibiotics for infection; hardware removal post-healing. |
| Neurovascular Injury | Rare | Direct trauma (transection, crush); traction. | Microsurgical repair for transection; observation for neuropraxia; symptomatic management for chronic pain. |
| Infection | <2-5% | Contamination during surgery; inadequate wound care. | Antibiotics; wound care; debridement if deep; hardware removal if infected. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is crucial for optimizing functional outcomes, preventing stiffness, and ensuring proper bone healing after clinodactyly correction. Protocols vary slightly based on the specific surgical technique, stability of fixation, and surgeon preference, but generally follow a phased approach.
1. Immobilization Phase (0-3 or 0-6 weeks)
- Duration: Typically 3-6 weeks. For K-wire fixation, immobilization is maintained until radiographic evidence of initial bone healing and removal of wires. For stable screw/plate fixation, earlier protected motion may be initiated.
- Immobilization Method: A well-padded plaster or thermoplastic splint (e.g., dorsal blocking splint, protective resting splint) that holds the corrected digit in a functional position, typically slight flexion, without tension on the repair. The adjacent digits are usually left free or included depending on the extent of swelling and need for protection.
- Pain Management: Multimodal analgesia, including NSAIDs, acetaminophen, and short-term opioids if necessary.
- Wound Care: Keep the surgical site clean and dry. Monitor for signs of infection (redness, swelling, purulent discharge). K-wire pin sites require daily cleaning with antiseptic solution.
- Edema Control: Strict elevation of the hand above heart level, gentle active range of motion (AROM) of uninvolved joints (shoulder, elbow, wrist), and compression garments (if appropriate for swelling) are encouraged to minimize post-operative swelling.
- Neurovascular Monitoring: Regular checks for sensation, capillary refill, and signs of digital ischemia.
2. Early Motion Phase (After Hardware Removal/Initial Healing, ~3-6 weeks post-op)
- Hardware Removal: K-wires are typically removed in clinic after 3-6 weeks, once radiographs confirm adequate bony consolidation.
- Initiation of Therapy: Referral to a certified hand therapist (CHT) is highly recommended at this stage.
- Goals: Restore active and passive range of motion of the interphalangeal and metacarpophalangeal joints of the affected digit, reduce swelling, and manage scar tissue.
-
Exercises:
- Gentle AROM: Initiated first, focusing on flexion and extension of the affected digit, ensuring pain-free motion.
- Passive Range of Motion (PROM): Progressed carefully by the therapist, respecting tissue healing and avoiding excessive force.
- Blocking Exercises: To isolate movement at individual joints.
- Scar Management: Deep tissue massage, silicone gel sheets, or topical emollients to prevent hypertrophic scarring and improve tissue pliability.
- Edema Management: Continued elevation, retrograde massage, light compression.
- Splinting: Dynamic or static progressive splinting may be used as an adjunct to therapy to address persistent stiffness or achieve further gains in motion, particularly for flexion contractures. Night splinting for protection.
3. Strengthening & Functional Integration Phase (~6-12 weeks post-op)
- Goals: Gradually increase strength, endurance, and fine motor coordination, and integrate the digit back into functional activities.
-
Exercises:
- Progressive Strengthening: Using therapeutic putty, resistance bands, and light weights for grip and pinch strengthening.
- Dexterity Exercises: Bead stringing, picking up small objects, buttoning, writing.
- Endurance Activities: Repetitive gripping and releasing, sustained light gripping.
- Proprioceptive Training: Balance and coordination tasks.
- Activity Modification: Gradually return to activities of daily living (ADLs), work, and recreational activities. Avoid heavy lifting or direct trauma to the healing bone until complete radiographic union is confirmed.
- Continued Scar Management: As needed.
4. Return to Full Activity (3-6 months post-op)
- Criteria: Full radiographic union, pain-free full range of motion, return of strength to near pre-injury levels (or baseline for congenital cases), and ability to perform desired functional activities.
- Long-Term Monitoring: Especially for pediatric patients who underwent growth modulation, regular clinical and radiographic follow-up is essential to monitor for potential recurrence of deformity or growth disturbances until skeletal maturity.
- Patient Education: Reinforce the importance of protecting the hand and reporting any new symptoms or changes.
Throughout all phases, patient compliance and close communication between the surgeon, patient, and hand therapist are paramount for achieving optimal results and addressing any challenges proactively.
Summary of Key Literature / Guidelines
The literature on clinodactyly, while extensive in its descriptive and syndromic associations, presents a somewhat fragmented landscape regarding definitive surgical guidelines, reflecting the variability of the condition and the individualized approach required.
Historical Perspectives and Evolution of Treatment:
Early descriptions of clinodactyly focused primarily on its anatomical presentation. Initial surgical interventions were often reserved for severe cases and largely involved simple osteotomies. The seminal work by
S. M. M. M. W. (S. Mark) van der Hoeve (1916)
and later
J. P. B. (Jan Pieter Bernard) van der Hoeve (1927)
on the association of brachydactyly and clinodactyly with syndromic presentations laid the groundwork for understanding its etiology. The concept of the "delta phalanx" as a cause of progressive angulation was further elucidated by
Waugh and Flatt (1960s)
and
Theander and Carstam (1970s)
, shifting focus toward growth modulation techniques for pediatric patients.
Key Surgical Debates and Principles:
-
Timing of Intervention:
- Younger Patients (Open Physes): The consensus generally favors earlier intervention for progressive deformities in very young children with a delta phalanx, utilizing physeal bar resection with fat, cartilage, or silicone interposition. The goal is to release the tether and allow for catch-up growth on the unaffected side, potentially avoiding a more complex osteotomy later. Watson and Boyes (1967) and Flatt (1977, 1994) have been instrumental in advocating for this approach. The efficacy of fat interposition has been demonstrated in several case series and small comparative studies, showing good long-term results in correcting angulation and preventing recurrence.
- Older Patients (Closed or Near-Closed Physes): For adolescents and adults, corrective osteotomy remains the gold standard. The osteotomy is typically delayed until skeletal maturity to prevent recurrence due to residual growth.
-
Type of Osteotomy:
- Closing Wedge Osteotomy: The most commonly employed technique, particularly for the middle phalanx, offering a predictable correction. Literature generally supports its effectiveness in achieving angular correction with good stability using K-wires or small screws.
- Opening Wedge Osteotomy: Less favored due to the need for bone grafting and potential for delayed union, but considered in specific cases where digital lengthening is also desired.
- Dome Osteotomy: Proposed by Miura (1981) , this technique offers theoretical advantages in multiplanar correction and smoother bone contact, potentially reducing the risk of nonunion. It requires more technical skill and specialized instrumentation. Comparative studies on osteotomy types are limited, with choice often based on surgeon familiarity and specific deformity characteristics.
-
Degree of Correction:
- Most authors aim for full correction to an anatomical axis. However, some acknowledge that achieving a near-normal appearance and function (e.g., <5-10 degrees residual angulation) is often a successful outcome. Overcorrection should be avoided.
-
Associated Conditions:
- The literature emphasizes the importance of screening for syndromic associations, particularly Down syndrome, as these patients may have unique surgical challenges (e.g., ligamentous laxity, anesthetic risks, compliance issues).
Long-Term Outcomes and Patient Satisfaction:
Studies on long-term outcomes for clinodactyly correction demonstrate high rates of patient and parent satisfaction, particularly when functional improvements are achieved. Recurrence remains a concern, especially after physeal bar resections, highlighting the need for careful patient selection and thorough removal of the abnormal physis. Stiffness, though generally mild, can be a lingering issue, underscoring the importance of post-operative hand therapy.
Current Guidelines and Future Directions:
While no single universally adopted guideline exists, the general consensus is:
*
Observation
for mild, non-progressive, asymptomatic cases.
*
Growth modulation (physeal bar resection)
for progressive deformities in skeletally immature patients with delta phalanges.
*
Corrective osteotomy
for skeletally mature patients or those with severe angulation not amenable to growth modulation.
Future research should focus on:
* Developing more precise diagnostic tools for early identification of subtle physeal abnormalities.
* Longitudinal, multi-center studies to compare outcomes of different surgical techniques across larger cohorts and track long-term recurrence rates.
* Elucidating the molecular and genetic mechanisms underlying delta phalanx formation to explore potential non-surgical or preventative strategies.
In conclusion, the management of clinodactyly remains an individualized process, heavily reliant on thorough clinical evaluation, precise radiographic assessment, and an understanding of the underlying pathogenesis. The choice of surgical intervention, if indicated, should align with the patient's age, the extent of deformity, and functional demands, with a clear focus on restoring alignment and improving hand function while minimizing complications.
