Preventing EPL Tendon Injury in Distal Radius Fractures: Advanced Techniques, Anatomy & Biomechanics
Key Takeaway
Preventing EPL tendon rupture after volar locking plate fixation for distal radius fractures involves meticulous surgical technique. Understanding risk factors like prominent screws and Lister's tubercle impingement is crucial. Advanced strategies focus on precise anatomical knowledge of the third extensor compartment and innovative approaches to mitigate friction and preserve EPL tendon integrity, ensuring optimal patient outcomes.
Advanced Surgical Technique: Preventing EPL Tendon Injury in Distal Radius Fractures with Volar Locking Plates
Introduction & Epidemiology
Distal radius fractures constitute one of the most prevalent fractures in adults, accounting for 15-20% of all fractures. With an aging global population and increasing expectations for functional recovery, surgical intervention, particularly fixation with volar locking plates (VLP), has become the standard of care for unstable distal radius fractures. VLP technology is widely favored due to its capacity to provide robust internal fixation, facilitate early mobilization, and effectively restore anatomical alignment and articular congruity. Despite significant advancements in VLP technology, post-operative complications remain a considerable challenge for orthopedic surgeons.
Among these complications, extensor tendon injury, specifically rupture of the Extensor Pollicis Longus (EPL) tendon, represents a critical concern. EPL tendon rupture leads to significant thumb dysfunction, severely impairing fine motor skills and grip strength, often necessitating complex reconstructive procedures such as tendon transfer or grafting. Literature reports the incidence of EPL tendon rupture following volar plating to range from 0.29% to 5.7%. While the absolute numbers may appear low, the profound impact on hand function underscores its clinical significance.
Key risk factors for EPL tendon injury include prominent dorsal screws, iatrogenic drilling injury during surgery, and the presence of dorsal distal radius fracture fragments, particularly those involving or adjacent to Lister's tubercle. Lister's tubercle serves as a pivotal fulcrum for the EPL tendon, and anatomical variations or the formation of fracture fragments in this region can directly compromise tendon integrity. Traditional prophylactic strategies, such as using monocortical screws or deliberately avoiding dorsal cortical penetration, may, in certain fracture patterns (e.g., comminuted fractures or osteoporotic bone), compromise the mechanical stability required for adequate fixation, where bicortical purchase is often essential. Therefore, the development of novel techniques that simultaneously ensure fracture stability and effectively mitigate the risk of EPL tendon injury holds substantial clinical value. This review aims to comprehensively explore an advanced surgical technique designed to minimize the risk of EPL tendon rupture by directly addressing the EPL tendon within the third extensor compartment, without necessarily shortening screws or excising dorsal fracture fragments.
Surgical Anatomy & Biomechanics
A thorough understanding of the intricate anatomy and biomechanical properties of the distal radius is fundamental to comprehending the mechanisms of EPL tendon injury and developing effective preventive strategies.
Distal Radius Anatomy
The distal radius is a complex, irregularly shaped bony structure that forms a crucial anatomical link between the hand and forearm. It encompasses several important articular surfaces and bony landmarks:
*
Radial Styloid:
Located on the lateral aspect of the radius, it serves as the attachment point for the radial collateral ligament and is a key palpation site for the radial artery.
*
Lister's Tubercle (Dorsal Radial Tubercle):
This prominent bony ridge is situated on the dorsal aspect of the distal radius. It defines the ulnar border of the third dorsal extensor compartment and the radial border of the second compartment. Its unique anatomical position renders it a critical hypomochlion for the EPL tendon, facilitating its change in direction from the forearm to the thumb. Consequently, Lister's tubercle is intimately involved in the pathophysiology of EPL tendon injuries.
*
Sigmoid Notch:
Located on the ulnar aspect of the distal radius, it articulates with the ulnar head to form the distal radioulnar joint (DRUJ).
*
Lunate and Scaphoid Facets:
These articular surfaces, covered by hyaline cartilage, articulate with the lunate and scaphoid bones, respectively, to form the radiocarpal joint.
The distal radius typically exhibits a mean palmar tilt of 11-12° and a radial inclination of 21-23°. These specific angular relationships are critical for maintaining normal wrist range of motion and load-bearing function.
Third Dorsal Extensor Compartment and EPL Tendon
The dorsal aspect of the wrist is characterized by six extensor tendon compartments, delineated by fibrous septa originating from the extensor retinaculum, a thickened band of deep fascia.
*
Third Dorsal Extensor Compartment:
Located just ulnar to Lister's tubercle, this compartment contains the Extensor Pollicis Longus (EPL) tendon. The bony floor of this compartment on the dorsal radius is typically a shallow groove, specifically designed for the EPL tendon.
*
EPL Tendon:
Originating from the posterior surface of the ulna and the interosseous membrane, the EPL tendon traverses the third compartment, makes a sharp turn around the ulnar side of Lister's tubercle, and then courses radially and volarly to insert onto the dorsal aspect of the distal phalanx of the thumb. This oblique course and sharp angulation around Lister's tubercle make the EPL particularly susceptible to friction and impingement. The functional integrity of the EPL tendon is paramount for active thumb extension, particularly at the interphalangeal joint, and contributes significantly to the forceful extension and abduction of the thumb, enabling precise pinch and grasp. Disruption of this tendon severely compromises these critical hand functions.
Biomechanically, the EPL tendon's pathway around Lister's tubercle is a high-stress area. Any irregularity on the dorsal cortex, such as prominent screw heads, screw tips penetrating the dorsal cortex, or sharp edges of dorsal fracture fragments, can act as a direct irritant or create an abrasive surface against which the EPL tendon repeatedly glides during thumb and wrist movements. Over time, this chronic attrition leads to tendinosis, fraying, and ultimately, spontaneous rupture. The critical proximity of the EPL tendon to the dorsal cortex, especially in relation to the distal fixation screws of a volar locking plate, highlights the necessity for meticulous surgical technique to prevent iatrogenic injury.
Figure 1: Dorsal view of the distal radius illustrating Lister's tubercle and the anatomical course of the EPL tendon within the third extensor compartment.
Indications & Contraindications
The decision to proceed with surgical fixation of a distal radius fracture with a volar locking plate, particularly employing techniques aimed at EPL protection, depends on a comprehensive evaluation of fracture characteristics, patient factors, and functional demands.
Indications for Operative Management (Volar Locking Plate)
Operative management with VLP is primarily indicated for unstable distal radius fractures that are unlikely to achieve satisfactory reduction and maintenance of anatomical alignment with non-operative methods. Specific indications include:
*
Intra-articular Fractures (AO type C, B3):
Displaced or comminuted intra-articular fractures with articular step-off >2mm or significant gap.
*
Extra-articular Fractures (AO type A):
Unstable extra-articular fractures with significant dorsal angulation (>20°), excessive radial shortening (>3-5mm), or loss of radial inclination (<15°).
*
Associated Injuries:
Fractures associated with carpal instability, DRUJ instability, or significant soft tissue compromise requiring open reduction.
*
Patient Demands:
Active individuals with high functional demands where restoration of precise anatomical alignment is critical for optimal long-term outcomes.
*
Osteoporotic Bone:
In osteoporotic patients, VLP offers superior stability compared to casting alone or external fixation, often requiring bicortical screw fixation for durable construct rigidity.
Contraindications for Operative Management
Absolute contraindications are rare but include:
*
Active Infection:
Cellulitis or osteomyelitis at the surgical site.
*
Severe Comorbidities:
Patients with medical conditions precluding safe anesthesia and surgery.
*
Non-displaced / Stable Fractures:
Fractures that are stable and anatomically aligned, amenable to non-operative treatment.
Relative contraindications include:
*
Open Fractures (Gustilo Type III):
While not an absolute contraindication, these often require staged procedures, aggressive debridement, and careful soft tissue management.
*
Extensive Soft Tissue Injury:
Poor skin integrity or extensive soft tissue damage that may compromise wound healing.
*
Patient Non-compliance:
Patients unwilling or unable to participate in post-operative rehabilitation.
The advanced technique specifically targeting EPL protection is indicated in all VLP cases, but particularly emphasized when:
* Fracture patterns involve the dorsal cortex, especially near Lister's tubercle (e.g., dorsal die-punch, dorsal rim fragments).
* Anticipated bicortical screw purchase, particularly with screws projecting dorsally.
* Revision surgeries where prior hardware may have caused irritation or where a higher index of suspicion for EPL vulnerability exists.
Table: Operative vs. Non-Operative Indications for Distal Radius Fractures
| Feature / Criteria | Non-Operative Management | Operative Management (Volar Locking Plate) |
|---|---|---|
| Fracture Displacement | Minimally displaced (<2mm) or stable anatomic reduction | Unstable, displaced (>2mm articular step-off/gap) |
| Dorsal Angulation | <10-15° dorsal angulation (or acceptable palmar tilt) | >10-15° dorsal angulation, loss of palmar tilt |
| Radial Shortening | <3-5mm radial shortening | >3-5mm radial shortening |
| Radial Inclination | >15° radial inclination | <15° radial inclination |
| Articular Involvement | No significant articular step-off or gap | Intra-articular fractures (B3, C) with step-off >2mm |
| DRUJ Instability | Stable DRUJ | Unstable DRUJ |
| Comminution | Minimal to moderate, stable | Significant comminution (dorsal/volar), highly unstable |
| Soft Tissue | Intact, healthy | Open fractures, severe swelling, compartment syndrome (relative) |
| Patient Factors | Low functional demand, significant comorbidities precluding surgery | High functional demand, active lifestyle |
| Associated Injuries | None | Carpal ligament injuries, median nerve compromise |
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning and appropriate patient positioning are crucial for successful outcomes and minimization of complications in distal radius fracture fixation.
Pre-Operative Planning
- Clinical Assessment: A comprehensive history and physical examination are paramount. Evaluate neurovascular status, pre-existing hand/wrist pathology, and patient comorbidities. Document any pre-existing nerve deficits or tendon issues.
-
Imaging Review:
- Plain Radiographs: Standard anteroposterior, lateral, and oblique views are essential. Assess fracture pattern, displacement, comminution, articular involvement, and integrity of the DRUJ.
- Computed Tomography (CT) Scan: Highly recommended for all intra-articular fractures, complex extra-articular patterns, and especially for fractures involving the dorsal cortex near Lister's tubercle. CT provides detailed information regarding articular step-off, comminution, and the orientation of dorsal fragments, which helps in anticipating potential EPL irritation from prominent hardware or bone edges. 3D reconstructions can be particularly helpful.
- Magnetic Resonance Imaging (MRI): Rarely indicated acutely for distal radius fractures unless there is suspicion of significant soft tissue injury (e.g., TFCC tear, ligamentous disruption) that would influence the surgical plan.
- Templating: Utilize radiographs and CT scans to pre-select appropriate plate size and screw lengths. Consider specific plate designs (e.g., variable angle, extended shaft) based on fracture morphology. Pre-operative templating also aids in anticipating the trajectory of distal screws and their potential proximity to the dorsal cortex, especially around Lister's tubercle.
- Anesthesia Consultation: Evaluate patient fitness for regional or general anesthesia. A supraclavicular or axillary block can provide excellent post-operative analgesia.
- Tourniquet Planning: A pneumatic tourniquet on the upper arm is standard to ensure a bloodless field, typically inflated to 250-300 mmHg or 100 mmHg above systolic pressure.
Patient Positioning
- Operating Table: The patient is positioned supine on the operating table.
- Arm Board: The affected arm is abducted and placed on a hand table or radiolucent arm board. This allows for optimal access to the volar aspect of the wrist and facilitates intraoperative fluoroscopy.
- Tourniquet: A sterile tourniquet is applied high on the upper arm.
- Finger Traps (Optional but Recommended): For comminuted or significantly displaced fractures, sterile finger traps (traction apparatus) applied to the index and middle fingers (or index, middle, and ring fingers) can provide continuous longitudinal traction (5-10 lbs) via an overhead frame. This helps to ligamentotax the fracture, restore length, and facilitate indirect reduction, thereby reducing the need for excessive soft tissue stripping and improving visualization. The wrist is typically held in slight extension to facilitate volar exposure.
- C-Arm Positioning: The C-arm fluoroscope should be positioned on the contralateral side of the patient to allow for unhindered access to the operative field and obtain true AP, lateral, and oblique views without repositioning the patient or the arm. Ensure sterility of the C-arm drape.
- Sterile Preparation: The entire limb, from the hand to above the tourniquet, is surgically prepped and draped to maintain sterility and allow for manipulation of the arm during surgery.
Detailed Surgical Approach / Technique
The standard volar approach to the distal radius, typically utilizing the Modified Henry approach, provides excellent exposure for VLP fixation. The advanced technique for EPL protection focuses on meticulous soft tissue handling, precise hardware placement, and a targeted dorsal assessment/protection step, particularly around Lister's tubercle.
1. Incision and Dissection
- Skin Incision: A longitudinal skin incision is made on the volar aspect of the distal forearm, centered over the flexor carpi radialis (FCR) tendon. The incision typically extends from the distal wrist crease proximally for approximately 5-7 cm. A slightly curved incision following skin creases can also be considered for cosmetic reasons, but must provide adequate exposure.
- Subcutaneous Dissection: Careful subcutaneous dissection is performed, identifying and protecting branches of the palmar cutaneous branch of the median nerve and radial sensory nerve to minimize the risk of iatrogenic neuropathy.
-
Internervous Plane:
The critical internervous plane for the Modified Henry approach lies between the
flexor carpi radialis (FCR)
tendon (innervated by the median nerve) and the
radial artery
.
- The FCR tendon is identified and retracted ulnarly. The radial artery, lying just radial to the FCR, is carefully identified and protected, usually retracted radially.
- Deep to the FCR tendon, the flexor pollicis longus (FPL) tendon is identified. The pronator quadratus muscle lies deep to the FPL.
- Exposure of Pronator Quadratus: The FPL tendon is retracted ulnarly, allowing access to the pronator quadratus muscle. The median nerve lies ulnar and deep to the FPL tendon and must be protected.
2. Fracture Reduction and Stabilization
- Subperiosteal Exposure: The pronator quadratus muscle is carefully incised in an L-shaped or transverse fashion along its radial and distal attachments to the radius. This subperiosteal elevation exposes the volar aspect of the distal radius. It is crucial to elevate the pronator quadratus as a flap to preserve its integrity for later repair, which aids in covering the plate.
- Indirect Reduction (Ligamentotaxis): If finger traps are used, continuous traction often provides initial reduction.
-
Direct Reduction:
- De-impaction of articular fragments using specialized elevators or bone tampers.
- Manipulation of the fracture fragments using small K-wires, blunt elevators, or reduction clamps.
- Correction of Dorsal Tilt and Radial Shortening: Apply dorsal pressure to the distal fragment while maintaining traction and pronation to restore palmar tilt. Fluoroscopy is used to confirm anatomical reduction in AP, lateral, and oblique views.
- Articular Congruity: Pay meticulous attention to restoring articular congruity, especially in intra-articular fractures. Small K-wires can be temporarily placed to hold articular fragments.
3. Volar Locking Plate Application
- Plate Positioning: The volar locking plate is positioned on the volar aspect of the distal radius. The distal edge of the plate should be placed approximately 2-3 mm proximal to the watershed line to minimize flexor tendon irritation. Optimal plate positioning is critical to avoid impingement on surrounding soft tissues and achieve adequate screw purchase.
- Initial Fixation: A temporary K-wire is used to secure the plate to the radial shaft after confirming appropriate position under fluoroscopy.
-
Distal Screw Placement:
- Crucial Step for EPL Protection: Carefully select drill trajectory and screw length. The goal is to achieve strong distal fixation, often with bicortical purchase, while preventing dorsal cortical penetration or prominence.
- Fluoroscopic Control: Use multiple fluoroscopic views (AP, lateral, 20° oblique views) for every distal screw. On the lateral view, ensure screws are not penetrating the dorsal cortex. On the AP view, ensure screws are not violating the DRUJ or radiocarpal joint. The oblique views are particularly important for assessing screw depth relative to the dorsal cortex and Lister's tubercle region.
- Tactile Feedback: As each screw is advanced, feel for bicortical purchase. If resistance suddenly drops or a palpable "pop" suggests dorsal cortical penetration, consider immediate reassessment with fluoroscopy and potentially shortening the screw.
- Variable Angle Screws: If using a variable angle plate, strategically direct screws away from the Lister's tubercle region if feasible, or optimize their trajectory to be parallel to the dorsal cortex rather than perpendicular.
- Proximal Screw Placement: Once distal fixation is achieved, proximal locking screws are inserted into the radial shaft to complete the construct.
Figure 2: Intraoperative view during a standard volar approach, showing reduction of a distal radius fracture and initial plate positioning on the volar cortex.
4. Advanced Technique: Direct EPL Tendon Protection
The innovative aspect of this technique focuses on direct intervention to protect the EPL tendon, especially when potential dorsal screw prominence or sharp dorsal bone edges are a concern, without necessarily sacrificing bicortical purchase or removing fracture fragments. This can be achieved through a targeted dorsal exploration or specific interpositional material.
-
Intraoperative Assessment (Post-Plating):
After the volar plate is fully secured, perform a comprehensive fluoroscopic assessment of all distal screws in all planes, with particular attention to the dorsal cortex around Lister's tubercle.
If any screw is noted to be proud dorsally, even subtly, or if a sharp dorsal fracture fragment is still present in the EPL groove, the advanced protection technique is initiated.
- Clinical Maneuver: Perform active and passive thumb extension/flexion while observing for any tendon catching or palpable crepitus over the dorsal radius. This dynamic assessment can often highlight areas of potential impingement.
-
Targeted Dorsal Mini-Incision:
- Make a small (2-3 cm) longitudinal skin incision directly over Lister's tubercle on the dorsal aspect of the wrist.
- Carefully dissect through the subcutaneous tissue. Identify the third dorsal extensor compartment.
- Longitudinally incise the extensor retinaculum over the third compartment to expose the EPL tendon.
- Gently retract the EPL tendon radially to visually inspect the dorsal radial cortex and Lister's tubercle groove.
- Direct Visualization: Directly inspect for any prominent screw tips from the volar plate, sharp fracture edges, or excessive callus formation within the EPL groove.
Figure 3: Close-up anatomical view highlighting the critical relationship between the EPL tendon (yellow) and Lister's tubercle. The dotted line indicates the potential course of a prominent screw from a volar plate, impacting the tendon.
-
Periosteal Flap or Interpositional Material:
- If prominent screws or sharp bone edges are identified: Elevate a small, vascularized local periosteal flap from an adjacent non-critical dorsal bone area. Carefully transpose this flap to interpose it between the EPL tendon and the problematic screw head/tip or sharp bone edge. Secure the flap with fine, absorbable sutures (e.g., 5-0 PDS) to the surrounding soft tissues (e.g., retinaculum remnants or adjacent periosteum) to ensure stable coverage.
- Alternative Interposition: If a local periosteal flap is not feasible or robust enough, consider using a small graft of fascia (e.g., harvested from the extensor retinaculum in a non-critical area), or a bioabsorbable membrane (e.g., collagen membrane) as an interpositional barrier. This barrier is meticulously secured to create a smooth, protective gliding surface for the EPL tendon.
- Advantages: This technique directly addresses the mechanical irritation without compromising the stability of the volar fixation (by avoiding screw shortening) or altering the fracture fragments (by avoiding excision of critical bone). It creates a physical barrier to protect the tendon from chronic attrition.
Figure 4: Illustration of the advanced technique. A small periosteal flap (shown in pink/red) is elevated and transposed to cover a prominent screw tip or sharp bone edge in the EPL groove, providing a smooth gliding surface for the EPL tendon.
5. Wound Closure
- Dorsal Closure: The extensor retinaculum is loosely approximated (if opened), followed by subcutaneous tissue and skin closure with absorbable sutures and skin staples/sutures respectively.
-
Volar Closure:
- The pronator quadratus muscle is meticulously repaired over the volar plate using absorbable sutures. This provides an important barrier between the plate and the flexor tendons, reducing the risk of tendinitis or rupture.
- Subcutaneous tissues are approximated, and the skin incision is closed in layers.
- A sterile dressing is applied.
6. Post-Operative Radiographs
Obtain final intraoperative or immediate post-operative radiographs (AP and lateral) to confirm satisfactory reduction, plate position, and screw lengths. Special attention is given to the relationship between the distal screws and the dorsal cortex, ensuring no overt prominence, especially after the dorsal protective procedure.
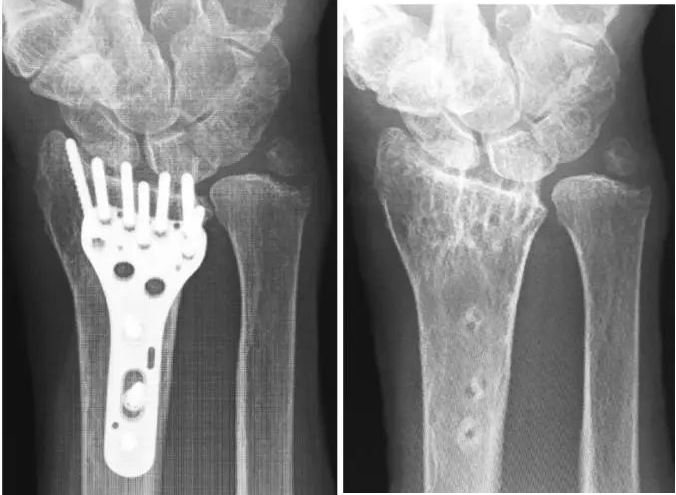
Figure 5 & 6: Post-operative AP and lateral radiographs demonstrating stable internal fixation of a distal radius fracture with a volar locking plate. Note the position of the distal screws relative to the articular surface and dorsal cortex. The advanced technique aims to mitigate any potential EPL tendon irritation from the dorsal aspect of the plate/screws, even if radiographically acceptable.
Complications & Management
Despite meticulous surgical technique, complications can arise following volar locking plate fixation of distal radius fractures. Awareness of these potential issues and strategies for their management is crucial.
1. Extensor Pollicis Longus (EPL) Tendon Rupture
- Incidence: 0.29% to 5.7% (variable based on study and technique).
- Mechanism: Most commonly due to chronic attrition against prominent dorsal hardware, sharp dorsal bone edges (especially Lister's tubercle), or iatrogenic injury during drilling/screw placement. The advanced technique described aims to specifically reduce this risk.
- Presentation: Delayed onset (weeks to months post-op) sudden inability to actively extend the thumb IP joint. Often preceded by localized pain or crepitus over Lister's tubercle.
-
Management:
- Conservative: Not effective for established rupture.
-
Surgical:
- Tendon Repair: Direct repair is often not possible due to chronic attrition and retraction.
- Tendon Transfer: Most common salvage procedure. The Extensor Indicis Proprius (EIP) is the preferred donor tendon, transferred to the distal stump of the EPL. Other options include Palmaris Longus graft if there is a significant gap, or Flexor Carpi Radialis if the EIP is unavailable.
- Hardware Removal: Essential to remove any offending hardware during tendon reconstruction.
2. Malunion
- Incidence: Variable, depending on fracture severity and definition of malunion (e.g., >5mm shortening, >10° dorsal tilt, >2mm articular step). Can be up to 10-20% in complex fractures.
- Mechanism: Inadequate reduction or loss of reduction post-operatively.
- Presentation: Persistent pain, decreased range of motion, grip weakness, cosmetic deformity, DRUJ dysfunction.
-
Management:
- Conservative: Activity modification, physical therapy, pain management for mild symptoms.
-
Surgical:
- Corrective Osteotomy: For symptomatic malunion, osteotomy with revision fixation is performed to restore anatomical alignment. This is a complex procedure often requiring bone grafting.
3. Nonunion
- Incidence: Rare in distal radius fractures treated with VLP (<1-2%).
- Mechanism: Severe comminution, soft tissue interposition, infection, inadequate fixation, biological factors (e.g., smoking, poor bone quality).
- Presentation: Persistent pain, tenderness, instability at the fracture site beyond 4-6 months, often with radiographic evidence of non-bridging callus.
-
Management:
- Surgical: Revision surgery with debridement of fibrous tissue, bone grafting (autograft or allograft), and rigid internal fixation.
4. Hardware-Related Complications
- Incidence: Up to 20-30%, but significant complications requiring removal are lower (5-10%).
- Mechanism: Prominent plate edge (flexor irritation/tendonitis), screw loosening/breakage, intra-articular screw penetration, painful hardware.
- Presentation: Volar wrist pain, decreased grip strength, flexor tendon irritation/rupture (especially FPL), carpal tunnel syndrome, palpable hardware.
-
Management:
- Surgical: Hardware removal. If flexor tendon irritation is severe, immediate removal is indicated. Revision fixation if fracture stability is compromised.
5. Infection
- Incidence: Low, <1-2% for clean cases.
- Mechanism: Contamination during surgery, immunocompromise.
- Presentation: Erythema, swelling, pain, purulent discharge, fever.
-
Management:
- Superficial: Oral antibiotics, local wound care.
- Deep: Surgical debridement, intravenous antibiotics, irrigation. May require hardware removal in chronic cases, often after fracture union.
6. Nerve Injuries
-
Incidence:
- Median Nerve: ~5-10% (paresthesias/carpal tunnel syndrome), direct injury rare.
- Radial Sensory Nerve: ~5-10% (neuroma, paresthesias from incision).
- Mechanism: Direct trauma during dissection, retraction, nerve compression (e.g., carpal tunnel syndrome from swelling or malunion).
- Presentation: Numbness, tingling, pain, motor weakness.
-
Management:
- Acute Post-op: Observe, steroid injection for carpal tunnel syndrome.
- Persistent: Nerve conduction studies. Surgical decompression (carpal tunnel release), neuroma excision, or neurolysis if indicated.
7. Distal Radioulnar Joint (DRUJ) Instability
- Incidence: ~5-15%, often related to associated TFCC injury or malunion.
- Mechanism: Direct injury to TFCC or associated ligaments during fracture, malreduction of the sigmoid notch, persistent ulnar positive variance after radial shortening.
- Presentation: Ulnar-sided wrist pain, clicking, instability with forearm rotation.
-
Management:
- Conservative: Immobilization, physical therapy, activity modification.
- Surgical: TFCC repair/reconstruction, ulnar shortening osteotomy, Darrach procedure, Sauve-Kapandji procedure, or DRUJ arthroplasty for chronic instability or arthritis.
8. Reflex Sympathetic Dystrophy (CRPS Type I)
- Incidence: 1-5%.
- Mechanism: Idiopathic, likely multifactorial involving sympathetic nervous system dysfunction after trauma or surgery.
- Presentation: Severe pain out of proportion to injury, allodynia, hyperalgesia, swelling, skin discoloration, temperature changes, trophic changes.
-
Management:
- Early Diagnosis & Aggressive Multimodal Treatment: Physical therapy, pain management (NSAIDs, gabapentin, tricyclic antidepressants), sympathetic nerve blocks, psychotherapy.
Table: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (approx.) | Common Mechanism | Salvage Strategy |
|---|---|---|---|
| EPL Tendon Rupture | 0.29-5.7% | Chronic attrition (prominent hardware/bone) | EIP tendon transfer, Palmaris Longus graft, hardware removal |
| Malunion | 10-20% | Inadequate reduction, loss of reduction | Corrective osteotomy, revision fixation |
| Nonunion | <1-2% | Inadequate fixation, infection, biological factors | Debridement, bone grafting, rigid revision fixation |
| Hardware Irritation/Prominence | 5-10% (symptomatic) | Plate position, prominent screw heads | Hardware removal, re-positioning (rarely) |
| Flexor Tendon Irritation/Rupture | <1% | Plate prominence, inadequate pronator quadratus repair | Hardware removal, tendon repair/transfer |
| Infection (Deep) | <1-2% | Intraoperative contamination | Debridement, IV antibiotics, hardware removal (if needed) |
| Median Nerve Neuropathy/CTS | 5-10% | Direct trauma, swelling, compression | Carpal tunnel release, observation |
| Radial Sensory Nerve Injury | 5-10% | Direct trauma during incision/dissection | Observation, local steroid, neuroma excision |
| DRUJ Instability | 5-15% | TFCC injury, malunion, ligamentous disruption | TFCC repair, ulnar shortening, DRUJ reconstruction |
| CRPS Type I | 1-5% | Unclear, sympathetic dysfunction | Multimodal pain management, PT, nerve blocks |
Post-Operative Rehabilitation Protocols
A structured and progressive post-operative rehabilitation protocol is critical for maximizing functional recovery and minimizing complications after distal radius VLP fixation, especially with the advanced EPL protection technique. The goal is to restore strength, motion, and function while protecting the healing fracture and soft tissue repairs.
Phase 1: Immobilization and Early Protected Motion (Weeks 0-2)
- Goal: Protect fracture fixation and soft tissue repairs, control pain and swelling.
-
Immobilization:
- Immediate post-op: Volar splint or sugar tong splint for comfort and initial protection.
- Duration: Typically 1-2 weeks, depending on fracture stability and surgeon preference.
- Position: Wrist in neutral to slight flexion. Avoid excessive wrist extension.
-
Pain and Swelling Management:
- Elevation of the hand above heart level.
- Cryotherapy (ice packs).
- Analgesics as prescribed.
-
Early Gentle Active Range of Motion (AROM):
- Fingers: Immediate initiation of gentle active flexion and extension of all fingers (including thumb IP and MCP joints) to prevent stiffness and promote tendon gliding. Crucial for EPL function after advanced protection.
- Elbow and Shoulder: Full AROM to prevent stiffness.
- Forearm: Gentle active pronation and supination as tolerated, ensuring stability of the DRUJ (avoid forced rotation against pain).
- Wound Care: Daily dressing changes as instructed, monitoring for signs of infection. Suture/staple removal at 10-14 days.
Phase 2: Early Mobilization and Strengthening (Weeks 2-6)
- Goal: Gradually increase wrist range of motion, initiate light strengthening, protect healing tissues.
- Transition to Removable Splint: A removable custom-molded thermoplastic splint or commercial wrist brace is typically used for comfort and protection during activity, but removed for exercises.
-
Progressive Range of Motion:
- Wrist: Gradual progression of active and passive wrist flexion, extension, radial and ulnar deviation. Focus on restoring pain-free motion.
- Forearm: Continue and progress active pronation and supination.
- Thumb: Continue and progress active thumb range of motion, emphasizing EPL function (thumb IP extension) to ensure smooth gliding over the protected Lister's tubercle area.
-
Light Strengthening (Initiate around Week 4-6, if pain allows and fracture healing evident):
- Isometric exercises for wrist and forearm musculature.
- Gentle grip strengthening with soft putty or sponge.
- Light finger exercises.
- Scar Management: Gentle scar massage to prevent adhesion formation.
- Neuromuscular Re-education: Begin proprioceptive exercises.
Phase 3: Advanced Strengthening and Return to Activity (Weeks 6-12+)
- Goal: Restore full strength, endurance, and function; gradually return to activities of daily living (ADLs) and recreational activities.
-
Progressive Strengthening:
- Gradual increase in resistance exercises for wrist flexors, extensors, pronators, and supinators (e.g., light weights, resistance bands).
- Advanced grip strengthening.
- Thumb strengthening exercises.
- Functional Activities: Incorporate activities that mimic daily tasks, work, or recreational demands.
- Impact Loading: Gradually introduce weight-bearing activities through the wrist, as tolerated and only when radiographic evidence of fracture union is observed (typically after 8-12 weeks).
-
Return to Sport/Work:
- Light, non-impact activities usually permitted around 3 months.
- Contact sports or heavy manual labor may require 4-6 months, depending on fracture severity, patient healing, and functional recovery.
- Long-term Monitoring: Continue to monitor for any signs of EPL irritation (pain, catching, weakness in thumb extension). If present, early intervention (e.g., steroid injection into the sheath, further physical therapy, or consideration of hardware removal) is crucial.
Throughout all phases, a close collaboration between the surgeon and a hand therapist is paramount for individualized progression and addressing specific patient needs and challenges. Regular radiographic follow-up is necessary to monitor fracture healing and plate stability.
Summary of Key Literature / Guidelines
The management of distal radius fractures with volar locking plates has evolved significantly, guided by extensive research and consensus from professional organizations. The primary goal remains anatomical reduction and stable fixation to restore optimal function, while minimizing complications, particularly tendon irritation and rupture.
AO Principles and VLP Advancement: The AO Foundation's principles of fracture management emphasize anatomical reduction, stable internal fixation, preservation of blood supply, and early active mobilization. Volar locking plates align well with these principles, offering excellent stability even in osteoporotic bone due to their fixed-angle screw constructs. Early generations of volar plates were associated with higher rates of flexor tendon irritation or rupture due to plate prominence. Modern low-profile anatomical plates, coupled with meticulous pronator quadratus repair, have largely mitigated this specific issue.
EPL Tendon Injury Literature:
The literature consistently highlights EPL tendon rupture as a significant, albeit less common, complication of VLP fixation. Meta-analyses and systematic reviews indicate a cumulative incidence ranging from 0.29% to 5.7%. Key risk factors identified include:
*
Dorsal cortical penetration:
Even subtle screw prominence can lead to chronic attrition. Studies using cadaveric models and clinical correlation demonstrate the close proximity of distal volar plate screws to the third extensor compartment.
*
Fracture patterns involving Lister's tubercle:
Displaced dorsal fragments or comminution around this anatomical landmark can create sharp edges.
*
Plate design and placement:
While modern plates are low-profile, the most distal screws still project towards the dorsal aspect of the bone. Plates placed too distally, too dorsally on the volar surface, or angled too dorsally, can increase the risk.
*
Lack of soft tissue interposition:
Failure to adequately cover the plate with the pronator quadratus muscle and periosteum may increase flexor tendon irritation, but specific soft tissue protection for the EPL tendon dorsally has been less emphasized in standard VLP techniques.
Current Guidelines and Best Practices:
*
Meticulous Surgical Technique:
Emphasize precise reduction, appropriate plate positioning (2-3mm proximal to the watershed line), and careful selection of screw lengths under fluoroscopic guidance (true lateral and oblique views are essential for dorsal screw assessment).
*
Soft Tissue Coverage:
Repair of the pronator quadratus over the plate is considered a standard and critical step to protect flexor tendons.
*
Avoid Dorsal Cortical Breaching:
While bicortical screw purchase is desirable for stability, it must not compromise dorsal soft tissues. If screw penetration is unavoidable or suspected, shortening the screw is a traditional method, though it may reduce fixation strength.
*
Consideration of Adjunctive Measures:
The presented advanced technique of a targeted dorsal assessment and local periosteal/fascial interposition addresses a recognized gap in standard practice for specific high-risk scenarios. While not universally adopted, the concept aligns with surgical principles of protecting vulnerable soft tissues from hardware-related irritation. Literature on similar protective strategies (e.g., using bioabsorbable membranes or periosteal flaps) for dorsal issues (e.g., extensor tendinitis over K-wires) supports the biomechanical rationale of creating a smooth, protective barrier.
*
Prophylactic Retinacular Release:
Some surgeons advocate for routine third compartment retinacular release, especially in high-risk cases, to potentially reduce pressure on the EPL tendon. However, this may contribute to bowstringing and other complications, and is not a universally accepted prophylactic measure. The described advanced technique is more targeted to specific hardware or bone prominence issues rather than a general prophylactic release.
In conclusion, while volar locking plates have revolutionized distal radius fracture management, the vigilance against EPL tendon injury remains paramount. The detailed advanced technique, focusing on intraoperative dorsal assessment and direct soft tissue interposition around Lister's tubercle, offers a targeted strategy to minimize this challenging complication without sacrificing fracture stability, thereby further enhancing the safety and efficacy of VLP fixation for distal radius fractures. Continued research, including comparative studies of such advanced techniques, will further refine best practices in this evolving field.
Clinical & Radiographic Imaging
