Deciphering Syndrome Autosomal Recessive: Genetics Explained
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Deciphering Syndrome Autosomal Recessive: Genetics Explained. An autosomal recessive syndrome is a genetic disorder manifested when an individual inherits two copies of a mutant recessive allele (aa). Such conditions typically involve biochemical or enzymatic defects. Parents are usually unaffected heterozygotes, with a 25% chance of transmitting the syndrome to offspring. This inheritance pattern affects males and females equally.
-
Cellular and Molecular Biology and Immunology
-
Chromosomes
- 46 chromosomes in 23 pairs: 22 pairs of autosomes, 1 pair of sex chromosomes
- Composed of DNA coiled around histone proteins
- DNA has a double-helix structure with linked nucleotides (adenine linked to thymine; guanine linked to cytosine) on a sugar-phosphate backbone
-
Three nucleotides = 1 codon, which corresponds to one amino acid


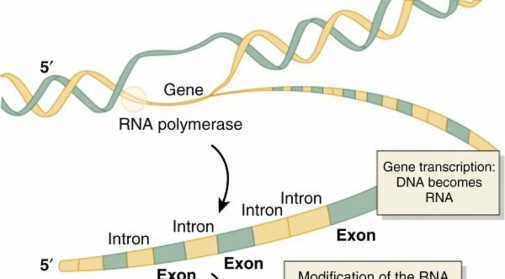
FIG. 1.47 DNA information is transcribed into RNA in the nucleus. Messenger RNA is then transported to the cytoplasm, where ribosomes complete translation into proteins. From Jorde LB et al, editors: Medical genetics, ed 2, St Louis, 1999, Mosby. - String of codons code for a string of amino acids = protein
- Gene : a section of DNA that codes for one protein Transcription—DNA to mRNA ( Fig. 1.47 ) 1. Unwinding of DNA for transcription occurs by DNA topoisomerase.
-
Topoisomerase-1 (scl-70) antibodies are seen in scleroderma and CREST (calcinosis, Raynaud phenomenon, sclerodactyly, telangiectasia) syndrome.
- RNA polymerase “reads” unwound DNA and builds corresponding mRNA
- RNA : single-stranded ribose sugar composed of nucleotides adenine, guanine, cytosine, and uracil
- Uracil in RNA links to adenine of DNA because there is no thymine in RNA
- Posttranscription modification
- Exons are regions of DNA that code for mRNA (mnemonic: EXons are EXpressed).
- Introns are regions of DNA that are between exons; 97% of the human genome consists of noncoding DNA.
- Splicing is the processing and removal of introns along with the combining of exons to make final mRNA used in translation.
- Small nuclear ribonucleoproteins (snRNPs) are RNA-protein complexes that mediate this posttranscriptional modification.
- Examples of these proteins are the U1 and Smith proteins.
- Anti-Smith antibodies are specific to SLE.
- Anti–U1-RNP antibodies are seen in mixed connective tissue disease.
-
Translation (see Fig. 1.47)
- Building of a protein out of amino acids from mRNA template
- Transfer RNA carries a specific amino acid to the ribosome, based on the mRNA codon.
-
Antibodies to tRNA synthetase (anti–Jo-1 antibodies) are seen in
dermatomyositis.
- Cell cycle and ploidy
-
Genetics
- Ploidy is the number of sets of chromosomes in a cell annotated by XN.
- The cell cycle entails the events within a cell that result in DNA duplication, with production of two daughter cells.
- Growth 0 (G0)—stable phase of cells with diploid (2N) DNA content
- Growth 1 (G1)—upon stimulus, cells begin growth but remain diploid (2N).
- Synthesis (S)—period of DNA replication resulting in tetraploidy (4N)
- Growth 2 (G2)—phase of cell growth and protein synthesis that is tetraploid (4N) throughout
- Mitosis (M)—sequence of events that result in two identical daughter cells that are each 2N
- Separation of chromosomal material for daughter cells occurs by spindle fibers’ attachment to centromeres that link sister chromatids
-
Anticentromere antibodies are seen in CREST syndrome.
- Certain proteins regulate progression through the cell cycle. Genetic defects and alterations of these tumor suppressor proteins can predispose a cell to dysregulated growth.
- pRb-1 (retinoblastoma protein) undergoes progressive cell cycle–regulated phosphorylation.
- Targets E2F, a transcription factor that regulates genes important for cell cycle control.
-
Implicated in retinoblastoma and osteosarcoma
- p53—prevents entry to S phase
- Implicated in osteosarcoma, rhabdomyosarcoma, and chondrosarcoma 1. Mendelian inheritance
- Due to transmission of alleles to offspring
- Phenotype refers to the features (traits) exhibited because of genetic makeup (genotype).
-
Mendelian traits may be inherited by one of four modes (Tables
1.30
and 1.31). -
Autosomal dominant (AD)
- Involves a gene on an autosomal chromosome; one of the two alleles for the chromosome pair must be abnormal for the disease phenotype to occur.
- Examples: syndactyly/polydactyly, Marfan syndrome, hereditary multiple exostoses (HME), malignant hyperthermia, Ehlers-Danlos syndrome, achondroplasia, osteogenesis imperfecta (types I and IV) 2. Autosomal recessive (AR) (most enzyme/biochemical deficiencies)
- Involves a gene on an autosomal chromosome; both alleles for the chromosome pair must be abnormal for the disease phenotype to occur.
- Example: diastrophic dysplasia, due to a mutation in the DTDST (SLC26A2) gene on chromosome 5 that encodes for a sulfate transport protein
- X-linked dominant
Table 1.30 Mendelian Inheritance Inheritance Pattern | Description | Punnett Square(s) | ---|---|---| Autosomal | Autosomal dominant disorders typically represent structural defects. Disorder is manifested in the heterozygous state (Aa).
Affects 50% of offspring (assuming only one parent is affected)
Normal offspring do not transmit the condition.
There is no gender preference.
| |

---
dominant• A is the mutant dominant allele. Autosomal recessive•
| Autosomal recessive disorders typically represent
biochemical or
| |

---
a is the
|
enzymatic defects. mutant recessive allele.
| Disorder is manifested in the
homozygous state (aa).
Parents are unaffected (they are most commonly heterozygotes).
| Affects 25% of offspring (assuming each parent is a heterozygote).
There is no gender preference.
| ---|---|---
X-linked dominant• X′ is the mutant dominant X allele.
| X-linked dominant disorders are manifested in the heterozygous state (X′X or X′Y).
Affected female (mating with unaffected male) transmits the X-linked gene to 50% of daughters and 50% of sons.
Affected male (mating with unaffected female) transmits the X-linked gene to all daughters and no sons.
| |

---
X-linked recessive• X is the mutant recessive X allele.
| Heterozygote (X′Y) male manifests the condition.
Heterozygote (X′X) female is unaffected.
Affected male (mating with unaffected female) transmits the X-linked gene to all daughters (who are carriers) and no sons.
Carrier female (mating with unaffected male) transmits the X-linked gene to 50% of daughters (who are carriers) and 50% of sons (who are affected).
| |

Table 1.31 Comprehensive Compilation of Inheritance Pattern, Defect, and Associated Gene in Musculoskeletal Disorders Disorder Inheritance Pattern Defect Associated Gene ---
Dysplasias
Achondroplasia
| Autosomal dominant
| Defect in the fibroblast growth factor receptor 3
|
FGF3R
Diastrophic dysplasia
| Autosomal recessive
| Mutation of a gene coding for a sulfate transport protein
|
DTDST
Kniest dysplasia
| Autosomal dominant
| Defect in type II collagen
|
COL 2A1
Laron dysplasia (pituitary dwarfism)
| Autosomal recessive
| Defect in the growth hormone
| |
| receptor
| ---|---|---|---
McCune-Albright syndrome (polyostotic fibrous dysplasia, café-au-lait spots, precocious puberty)
| Sporadic mutation
| Germline defect in the Gsα protein
|
Mutation of Gsα subunit of th receptor/aden cyclase–coup G proteins Metaphyseal chondrodysplasia:
| |
|
Jansen form
| Autosomal dominant
| |
PTH ; PTH-related protein
McKusick form
| Autosomal recessive
| |
RMRP
Schmid-tarda form
| Autosomal dominant
| Defect in type X collagen
|
COL 10A1
Multiple epiphyseal dysplasia
| Autosomal dominant (most commonly)
| Cartilage
oligomeric matrix protein
|
COMP
Spondyloepiphyseal dysplasia
| Autosomal
dominant (congenita form)
X-linked recessive (tarda form)
| Defect in type II collagen
| Linked to Xp22.1 p22.31,
SEDL
(tarda), and
C 2A1
(congenit
Achondrogenesis
| Autosomal recessive
| Fetal cartilage fails to mature
|
Apert syndrome
| Sporadic
mutation/autosomal dominant
| |
FGF2R
Chondrodysplasia punctata
| |
|
Conradi-Hünerman
| Autosomal dominant
| |
Rhizomelic form
| Autosomal recessive
| Defect in
subcellular organelles (peroxisomes)
|
Cleidocranial dysplasia (dysostosis)
| Autosomal dominant
| Mutation of a gene coding for a protein related to
|
CBFA1
| |
osteoblast function
| ---|---|---|---
Dysplasia epiphysealis hemimelica (Trevor disease)
| Unknown
| |
Ellis–van Creveld syndrome (chondroectodermal dysplasia)
| Autosomal recessive
| |
EVC
Table Conti
Disorder Inheritance Pattern Defect Associa
---
Fibrodysplasia ossificans progressiva
| Sporadic
mutation/autosomal dominant
| |
Geroderma osteodysplastica (Walt Disney dwarfism)
| Autosomal recessive
| |
Grebe chondrodysplasia
| Autosomal recessive
| |
Hypochondroplasia
| Sporadic
mutation/autosomal dominant
| |
FGF3R
Kabuki makeup syndrome
| Sporadic mutation
| |
Mesomelic dysplasia (Langer type)
| Autosomal recessive
| |
Mesomelic dysplasia
| |
|
Nievergelt type
| Autosomal dominant
| |
Reinhardt-Pfeiffer type
| Autosomal dominant
| |
Werner type
| Autosomal dominant
| |
Metatrophic dysplasia
| Autosomal recessive
| |
Progressive diaphyseal dysplasia (Camurati-Engelmann disease)
| Autosomal dominant
| |
Pseudoachondroplastic dysplasia
| Autosomal dominant
| |
COMP
Pyknodysostosis
| Autosomal recessive
| |
Spondylometaphyseal chondrodysplasia
| Autosomal dominant
| |
Spondylothoracic dysplasia (Jarcho-Levin syndrome)
| Autosomal recessive
| |
| ---|---|---|---|
Thanatophoric dwarfism
| Autosomal dominant
| |
FGF3R
Tooth-and-nail syndrome
| Autosomal dominant
| |
Treacher Collins syndrome (mandibulofacial dysostosis)
| Autosomal dominant
| |
Metabolic Bone Diseases
Hereditary vitamin D–dependent rickets
| Autosomal recessive
|
See
Table 1.16
|
Hypophosphatasia
| Autosomal recessive
|
See
Table 1.16
|
PHEX
Hypophosphatemic rickets (vitamin D–resistant rickets)
| X-linked dominant
|
See
Table 1.16
|
PHEX
Osteogenesis imperfecta
| Autosomal
dominant (types I and IV)
Autosomal
recessive (types II and III)
| Defect in type I collagen (abnormal cross-linking)
|
COL IA
IA2
Albright hereditary osteodystrophy (pseudohypoparathyroidism)
| Uncertain
| PTH has no effect at the target cells (in the kidney, bone, and intestine)
|
Infantile cortical hyperostosis (Caffey disease)
| Unknown
| |
Ochronosis (alkaptonuria)
| Autosomal recessive
| Defect in the homogentisic acid oxidase system
|
Osteopetrosis
| Autosomal
dominant (mild, tarda form)
Autosomal
recessive (infantile, malignant form)
| |
CLCN7,
Connective Tissue Disorders
Marfan syndrome
| Autosomal dominant
| Fibrillin
abnormalities (some patients also have type I
|
FBN1 o
βR2
| |
collagen abnormalities)
| ---|---|---|---
Ehlers-Danlos syndrome (there are at least 13 varieties)
| Autosomal dominant (most common)
| Defects in types I and III collagen have been described for some varieties; lysyl oxidase abnormalities
|
COL
( I c
COL
( Homocystinuria
| Autosomal recessive
| Deficiency of the enzyme cystathionine β-synthase
| Mucopolysaccharidosis
Hunter syndrome (gargoylism)
| X-linked recessive
| |
Hurler syndrome
| Autosomal recessive
| Deficiency of the enzyme α-L-iduronidase
|
Maroteaux-Lamy syndrome
| Autosomal recessive
| |
Morquio syndrome
| Autosomal recessive
| |
Sanfilippo syndrome
| Autosomal recessive
| |
Scheie syndrome
| Autosomal recessive
| Deficiency of the enzyme α-L-iduronidase
| Muscular Dystrophies
Duchenne muscular dystrophy
| X-linked recessive
| Defect on the short arm of the X chromosome
| Dystrop
Becker dystrophy
| X-linked recessive
| |
Fascioscapulohumeral dystrophy
| Autosomal dominant
| |
Limb-girdle dystrophy
| Autosomal recessive
| |
Steinert disease (myotonic dystrophy)
| Autosomal dominant
| |
Table C
Disorder Inheritance Defect Associated Gene Pattern
---
Hematologic Disorders
Hemophilia (A and B)
| X-linked
recessive
| Hemophilia A: factor VIII deficiency
Hemophilia B: factor IX deficiency
|
Sickle cell anemia
| Autosomal
recessive
| Hemoglobin abnormality (presence of hemoglobin S)
|
Gaucher disease
| Autosomal
recessive
|
Deficient activity of the enzyme β-glucosidase (glucocerebrosidase)
|
Hemochromatosis
| Autosomal
recessive
| |
Niemann-Pick disease
| Autosomal
recessive
| Accumulation of sphingomyelin in cellular lysosomes
|
Smith-Lemli-Opitz syndrome
| Uncertain
| |
Thalassemia
| Autosomal
recessive
| Abnormal production of hemoglobin A
|
von Willebrand disease
| Autosomal
dominant
| |
Chromosomal Disorders With Musculoskeletal Abnormalities
Down syndrome
| |
Trisomy of
chromosome 21
|
Angelman syndrome
| |
Chromosome 15 abnormality
|
Clinodactyly
| |
Associated with many genetic anomalies, including trisomy of chromosomes 8 and
21
|
Edward syndrome
| |
Trisomy of
chromosome 18
|
Fragile X syndrome
| X-linked trait (does not follow the typical
| |
Xq27-28
| pattern of an X-linked trait)
| |
| ---|---|---|---|
Klinefelter syndrome (XXY)
| |
An extra X
chromosome in affected boys and men
|
Langer-Giedion syndrome
| Sporadic
mutation
| Chromosome 8 abnormality
|
Nail-patella syndrome
| Autosomal
dominant
| |
LMX1B
Patau syndrome
| |
Trisomy of
chromosome 13
|
Turner syndrome (XO)
| |
One of the two X chromosomes missing in affected girls and women
|
SHOX
Neurologic Disorders
Charcot-Marie-Tooth disease
| Autosomal
dominant (most common)
|
Chromosome 17 defect for encoding peripheral myelin protein-22
|
PMP22
Congenital insensitivity to pain
| Autosomal
recessive
| |
Dejerine-Sottas disease
| Autosomal
recessive
| |
Friedreich ataxia
| Autosomal
recessive
| |
Huntington disease
| Autosomal
dominant
| |
Menkes syndrome
| X-linked
recessive
| Inability to absorb and use copper
|
Pelizaeus-Merzbacher disease
| X-linked
recessive
| Defect in the gene for proteolipid (a component of myelin)
|
Riley-Day syndrome
| Autosomal
recessive
| |
Spinal muscular atrophy (Werdnig-Hoffman disease and Kugelberg-
| Autosomal
recessive
| |
Welander disease)
| |
| ---|---|---|---
Sturge-Weber syndrome
| Sporadic
mutation
| |
Tay-Sachs disease
| Autosomal
recessive
| Deficiency in the enzyme hexosaminidase A
| Diseases Associated with Neoplasias
Ewing sarcoma
| |
| 11;22
chromosomal translocation (
EWS/FL11
fusion gene)
Multiple endocrine neoplasia (MEN):
| |
|
Type I
| Autosomal
dominant
| |
RET
Type II
| Autosomal
dominant
| |
Type III
| Autosomal
dominant
| Chromosome 10 abnormality
|
Neurofibromatosis (von Recklinghausen disease) type 1 (NF1) and type 2 (NF2)
| Autosomal
dominant
|
NF1: chromosome 17 defect; codes for neurofibromin
NF2: chromosome 22 defect
|
NF1, NF2
Synovial sarcoma
| |
| (X;18) (p11;q11)
chromosomal translocations (
STT/SSX
fusion gene)
Miscellaneous Disorders
Malignant hyperthermia
| Autosomal
dominant
| |
Osteochondromatosis
| Autosomal
dominant
| |
Postaxial polydactyly
| Autosomal
dominant
| |
GLI3(types
A, A/B)
| |
|
GJA1(type IV)
| ---|---|---|---|
Camptodactyly
| Autosomal
dominant
| |
Table Continued
Disorder Inheritance Pattern Defect Associa
---
Cerebrooculofacioskeletal syndrome
| Autosomal recessive
| |
Congenital contractural arachnodactyly
| |
| Fibrillin
(chr 5)
Distal arthrogryposis syndrome
| Autosomal dominant
| |
Dupuytren contracture
| Autosomal dominant (with partial sex limitation)
| |
Fabry disease
| X-linked recessive
| Deficiency of α-galactosidase A
|
Fanconi pancytopenia
| Autosomal recessive
| |
Freeman-Sheldon syndrome (craniocarpotarsal dysplasia; whistling face syndrome)
| Autosomal
dominant Autosomal
recessive
| |
GM1 gangliosidosis
| Autosomal recessive
| |
Hereditary anonychia
| Autosomal dominant
| |
Holt-Oram syndrome
| Autosomal dominant
| |
Humeroradial synostosis
| Autosomal dominant
| |
Autosomal recessive
| |
Klippel-Feil syndrome
| |
Faulty development of spinal segments along the embryonic neural tube
|
Klippel-Trénaunay-Weber syndrome
| Sporadic mutation
| |
Krabbe disease
| Autosomal recessive
| Deficiency of galactocerebroside β-galactosidase
|
Larsen syndrome
| Autosomal
dominant Autosomal
recessive
| |
| ---|---|---|---|
Lesch-Nyhan disease
| X-linked trait
| Absence of the enzyme hypoxanthine guanine phosphoribosyl transferase
|
Madelung deformity
| Autosomal dominant
| |
Mannosidosis
| Autosomal recessive
| Deficiency of the enzyme α-mannosidase
|
Maple syrup urine disease
| Autosomal recessive
| Defective metabolism of the amino acids leucine, isoleucine, and valine
|
Meckel syndrome (Gruber syndrome)
| Autosomal recessive
| |
Möbius syndrome
| Autosomal dominant
| |
Mucolipidosis (oligosaccharidosis)
| Autosomal recessive
| A family of enzyme deficiency diseases
|
Multiple exostoses
| Autosomal dominant
| |
EXT
r EXT
Multiple pterygium syndrome
| Autosomal recessive
| |
Noonan syndrome
| Sporadic mutation
| |
Oral-facial-digital (OFD) syndrome
| |
|
OFD
l
OFD
s a r
Osler-Weber-Rendu syndrome (hereditary hemorrhagic
| Autosomal dominant
| |
telangiectasia)
| |
| ---|---|---|---
Pfeiffer syndrome (acrocephalosyndactyly)
| Sporadic
mutation/autosomal dominant
| |
FGF2R
Phenylketonuria
| Autosomal recessive
| Enzyme deficiency characterized by the inability to convert phenylalanine to tyrosine because of a chromosome 12 abnormality
|
Phytanic acid storage disease
| Autosomal recessive
| |
Progeria (Hutchinson-Gilford progeria syndrome)
| Autosomal dominant
| |
Proteus syndrome
| Autosomal dominant
| |
Prune-belly syndrome
| Uncertain
| Localized
mesodermal defect
|
Radioulnar synostosis
| Autosomal dominant
| |
Rett syndrome
| Sporadic mutation/X-linked dominant
| |
Roberts syndrome (pseudothalidomide syndrome)
| Sporadic
mutation/autosomal recessive
| |
Russell-Silver syndrome
| Sporadic mutation (possibly X-linked)
| |
Saethre-Chotzen syndrome
| Autosomal dominant
| |
Sandhoff disease
| Autosomal recessive
| Enzyme deficiency of hexosaminidases A and B
|
Schwartz-Jampel syndrome
| Autosomal recessive
| |
Seckel syndrome (so-called bird-headed dwarfism)
| Autosomal recessive
| |
Table
Disorder
|
Inheritance Pattern
|
Defect
|
Associated Gene
| ---|---|---|---|
Stickler syndrome (hereditary progressive arthroophthalmopathy)
| Autosomal
dominant
| Collagen
abnormality
| |
| |
Thrombocytopenia-aplasia of radius (TAR) syndrome
| Autosomal
recessive
| |
| ---|---|---|---|
Tarsal coalition
| Autosomal
dominant
| |
Trichorhinophalangeal syndrome
| Autosomal
dominant
| |
Argininemia
| Autosomal
recessive
| |
Argininosuccinic aciduria
| Autosomal
recessive
| |
Carbamyl phosphate synthetase deficiency
| Autosomal
recessive
| |
Citrullinemia
| Autosomal
recessive
| |
Ornithine transcarbamylase deficiency
| X-linked
| |
VATER association
| Sporadic
mutation
| |
Werner syndrome
| Autosomal
recessive
| |
Zygodactyly
| Autosomal
dominant
| |
TGF-βR2, TGF-β receptor 2; VATER, vertebral defects, imperforate anus, tracheoesophageal fistula, and radial and renal dysplasia.
1. Example: hypophosphatemic rickets, due to
PHEX
gene mutation (Xp.22)
1. #### X-linked recessive
1. Examples:
Duchenne and Becker muscular dystrophies, Hunter syndrome, hemophilia, spondyloepiphyseal dysplasia (SED) tarda
1. Nonmendelian traits may be inherited through “polygenic” transmission caused by the action of several genes
1. Charcot-Marie-Tooth disease (AD, AR, and X-linked forms)
2. Osteopetrosis (AD and AR)
3. Osteogenesis imperfecta (AD and AR)
4. Neurofibromatosis (AD and AR)
5. SED (AD and X-linked)
2. Mutations
1. Genetic disorders arise from alterations (mutations) in the
genetic material.
1. Most skeletal dysplasias are single-gene mutations.
1. Collagen type I (bone) defects
1. Osteogenesis imperfecta (types I–IV)—
COL1A1
and
COL1A2
genes
2. Ehlers-Danlos—
COL5A1
and
COL5A2
genes
2. Collagen type II (cartilage) defects
1. SED—
COL2A1
gene
,
usually random mutations
3. Epigenetics
1. Others
2. Multiple epiphyseal dysplasia—
COMP
(cartilage oligomeric matrix protein) gene; also associated with pseudoachondroplasia)
3. Marfan syndrome
—
FBN1
(fibrillin-1) gene
4. Achondroplasia—
FGFR3
(fibroblast growth factor receptor) gene
5. Spinal muscular atrophy
—
SMN1
(survival motor neuron-1) gene
1. Genetic alterations that are not caused by mutations in DNA sequence
1. DNA methylation
2. Histone posttranslational modifications
3. Genomic imprinting (parent-of-origin phenotypes)
1. An example of genomic imprinting is the loss of a region in chromosome 15 with Prader-Willi syndrome (paternal; obesity, hypogonadism, hypotonia) and Angelman syndrome (maternal; epilepsy, tremors, smiling)
1. Chromosomal abnormalities
1. Disruptions in the normal arrangement or number of chromosomes
2. Trisomy: one chromosome pair has an extra chromosome (total: 47 chromosomes)
1. #### Trisomy 21 (Down syndrome)—ligamentous laxity, atlantoaxial instability, patellar and hip dislocations, severe flatfoot, and bunions
3. Deletion: absence of a section of one chromosome (in a chromosome pair).
4. Duplication: presence of an extra section of one chromosome (in a chromosome pair).
5. #### Translocation: exchange of a portion of one chromosome with a portion of another chromosome
6. Inversion: a broken portion of a chromosome reattaches to the same chromosome in the same location but in a reverse direction.
2.
Genetics of musculoskeletal conditions and abnormalities are summarized in
Table 1.31.
3. Techniques used to study genetic (inherited) disorders
1. Restriction enzymes
1. Used to cut DNA at precise, reproducible cleavage locations
2. Identify polymorphisms (alternative gene expressions)
2. Agarose gel electrophoresis
1. Molecules are suspended in agarose gel that is exposed to an electric field.
2. Molecules move through the gel according to size and polarity
1. Southern blot: detects DNA
2. Northern blot: detects RNA
3. Western blot: detects protein
3. Plasmid vectors
1. A plasmid is a small, extrachromosomal, circular piece of DNA that replicates independently of the host DNA. Plasmids can confer antibiotic resistance between bacteria.
2. The recombinant plasmid is inserted into a bacterium (the vector) by a process called
transformation
. The bacterium then produces a recombinant protein encoded by the inserted gene
.
4. Cytogenetic analysis

 FIG. 1.48 Innate immunity and adaptive immunity. The mechanisms of innate immunity provide the initial defense against infections. Adaptive immune responses develop later and consist of activation of lymphocytes.
FIG. 1.48 Innate immunity and adaptive immunity. The mechanisms of innate immunity provide the initial defense against infections. Adaptive immune responses develop later and consist of activation of lymphocytes.
From Abbas AK et al:
Cellular and molecular immunology,
ed 6, Philadelphia, 2009, Saunders.
1. Gross examination of chromosomes under microscope with the use of techniques of banding and fluorescent in situ hybridization
2. #### Used to detect chromosomal translocations
1. #### t(X;18)—in synovial sarcoma
2. #### t(11;22)—in Ewing sarcoma
3. #### t(2;13)—in rhabdomyosarcoma
4. #### t(12;16)—in myxoid liposarcoma
5. #### t(12;22)—in clear cell sarcoma
5. Transgenic animals
1. Bred to investigate the function of cloned genes.
6. PCR amplification
1. Repetitive synthesis (amplification) of a specific DNA sequence in vitro
2. Screening DNA for gene mutations (e.g., prenatal diagnosis of sickle cell)
7. Reverse transcription PCR (RT-PCR)
1. Reverse transcriptase is used to “reverse transcribe” RNA to complementary DNA.
2. Typically used to study RNA viruses
8. #### Silencing RNA (siRNA)
1. #### Blocks transcription of mRNA in order to study
result of gene’s loss of function
You Might Also Like


