Management of Posterior Cruciate Ligament Injuries: A Comprehensive Surgical Guide
Key Takeaway
The management of posterior cruciate ligament (PCL) injuries remains highly controversial due to its variable natural history. While isolated Grade I and II tears often respond favorably to structured nonoperative rehabilitation, high-grade or combined ligamentous injuries necessitate surgical intervention. This guide delineates the biomechanical rationale, strict indications, and step-by-step surgical techniques—including avulsion fracture fixation and arthroscopically assisted reconstruction—required to optimize clinical outcomes and mitigate long-term osteoarthritic degeneration.
THE CONTROVERSY AND NATURAL HISTORY OF PCL INJURIES
The treatment of posterior cruciate ligament (PCL) injuries remains one of the most controversial topics in contemporary knee surgery. This controversy stems primarily from an incomplete understanding of the injury's natural history, compounded by literature that frequently conflates acute and chronic injuries, as well as isolated and multiligamentous trauma. Formulating an evidence-based treatment algorithm requires a profound understanding of the long-term biomechanical consequences of PCL deficiency and the realistic outcomes of both conservative and surgical interventions.
The true incidence of PCL injuries is difficult to ascertain, though it is estimated to comprise between 3% and 20% of all knee ligament injuries. Because many isolated PCL injuries are clinically silent or go undetected in the acute phase, epidemiological data is inherently skewed.
Dejour’s Phases of PCL Deficiency
While short-term functional instability is often minimal—allowing up to 85% of patients to return to sports regardless of objective laxity—long-term studies demonstrate a clear trajectory toward joint deterioration. Dejour et al. elegantly described the natural history of isolated PCL rupture in three distinct phases:
1. Functional Adaptation (3 to 18 months): The patient modifies kinematics and muscle recruitment to compensate for posterior laxity.
2. Functional Tolerance (15 to 20 years): The knee remains relatively asymptomatic during activities of daily living, though microtrauma accumulates.
3. Osteoarthritic Deterioration (>25 years): Disabling symptoms emerge, characterized by pain with walking long distances, standing, climbing, squatting, knee stiffness, and episodes of giving way.
Clinical Pearl: Do not be falsely reassured by a patient's excellent short-term function following an isolated PCL tear. The absence of acute instability does not preclude the insidious onset of medial compartment and patellofemoral osteoarthritis over the subsequent decades.
BIOMECHANICS AND PATHOANATOMY
The worsening of symptoms and the eventual development of osteoarthritis in the PCL-deficient knee are directly attributable to abnormal joint reaction forces. The PCL is the primary restraint to posterior tibial translation. When compromised, the articular surfaces of all knee compartments are subjected to deleterious shear and compressive forces.
Kinematic Alterations in the PCL-Deficient Knee
In vivo biomechanical studies, such as those by Castle et al., demonstrate that PCL rupture results in obligate posterior subluxation of the tibia. During deep flexion activities (e.g., ascending or descending stairs), the patella and patellar ligament are forced to act as secondary restraints to posterior tibial translation.
This abnormal posterior tibial "sag" produces a shortened moment arm for the quadriceps muscle group, drastically reducing its mechanical advantage. Consequently, the quadriceps must generate significantly higher forces to achieve extension. Cadaveric sequential sectioning studies confirm that patellofemoral pressures and quadriceps loads are greatly elevated following PCL sectioning.
Furthermore, Logan et al. utilized open-access MRI to evaluate tibiofemoral motion under weight-bearing conditions through an arc of flexion (0 to 90 degrees). They observed that PCL rupture alters medial compartment kinematics, leading to persistent posterior subluxation of the medial tibia. As a result, the medial femoral condyle rides up the anterior slope of the medial tibial plateau. This fixed subluxation is statistically significant at all flexion angles, explaining the high incidence of isolated medial compartment osteoarthritis in chronic PCL deficiency. Interestingly, lateral compartment kinematics remain largely unaltered.
NONOPERATIVE MANAGEMENT
Traditionally, nonoperative management has been the gold standard for isolated PCL tears. Proven methods for anatomical reconstruction are technically demanding, and historically, surgical results have been unpredictable in eliminating posterior laxity.
Indications and Patient Selection
Magnetic Resonance Imaging (MRI) is critical in the acute setting to evaluate concomitant meniscal or chondral pathology and to classify the tear as interstitial or partial. Interstitial tears have a robust healing capacity; reports indicate that over a 6-month period, posterior laxity can reduce from a Grade II (2+) posterior drawer to a Grade I (1+) or even a trace.
The strictly defined criteria for nonoperative treatment of an isolated PCL injury include:
* Posterior Drawer < 10 mm (Grade I or II): Measured with the tibia in neutral rotation. (Note: Posterior drawer excursion naturally decreases with internal rotation of the tibia due to the tightening of the intact posteromedial structures).
* Abnormal Rotary Laxity < 5 degrees: Specifically, abnormal external rotation of the tibia with the knee flexed at 30 degrees must be minimal, ruling out a concomitant posterolateral corner (PLC) injury.
* No Significant Varus-Valgus Laxity: Confirming the absence of collateral ligament involvement.
Experienced surgeons, such as Shelbourne and Clancy, advocate for nonoperative treatment of most acute Grade I and II isolated tears. Clancy emphasizes that no current studies definitively prove that PCL reconstruction prevents the development of articular cartilage degeneration. This is supported by Gill et al., who demonstrated in cadaveric models that while PCL deficiency significantly increases peak patellofemoral contact pressures, standard reconstruction techniques fail to significantly reduce these elevated pressures back to baseline.
Rehabilitation Protocols
Nonoperative management is not benign neglect; it requires a highly structured rehabilitation program.
* Acute Phase: Focus on reducing effusion and regaining full range of motion (ROM). The knee may be braced in extension to prevent posterior tibial sag.
* Strengthening Phase: Rehabilitation is heavily quadriceps-focused. The quadriceps act as dynamic antagonists to posterior tibial translation.
* Hamstring Restriction: Active hamstring exercises must be strictly avoided in the early phases, as hamstring contraction directly exacerbates posterior tibial translation and stresses the healing PCL.
Pitfall: Failing to recognize a combined PCL and Posterolateral Corner (PLC) injury is the most common reason for "failed" nonoperative management. Always assess the dial test at 30 and 90 degrees of flexion.
OPERATIVE MANAGEMENT
Surgical intervention is generally reserved for high-demand athletes with symptomatic Grade II or greater laxity, combined multiligamentous injuries, bony avulsion fractures, and chronic symptomatic knees where conservative measures have failed.
Preoperative Planning and Timing
For acute injuries requiring surgery, reconstruction is typically delayed for 1 to 2 weeks. This delay allows the painful intra-articular inflammatory reaction to subside, capsular defects to seal, and the patient to regain full motion and baseline quadriceps strength, thereby minimizing the risk of postoperative arthrofibrosis.
Surgical Indications and Algorithms
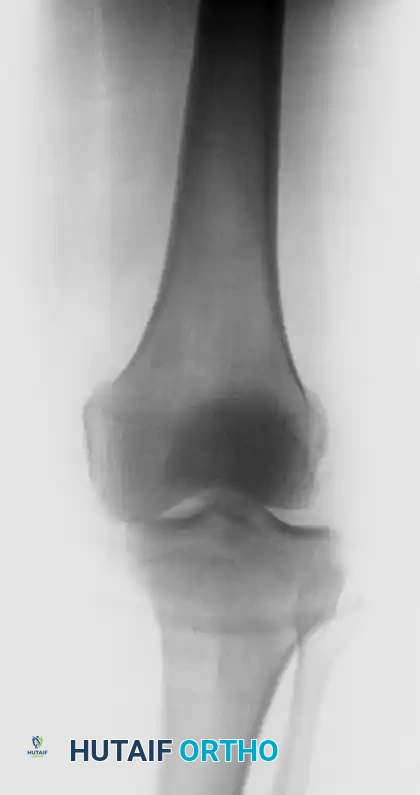
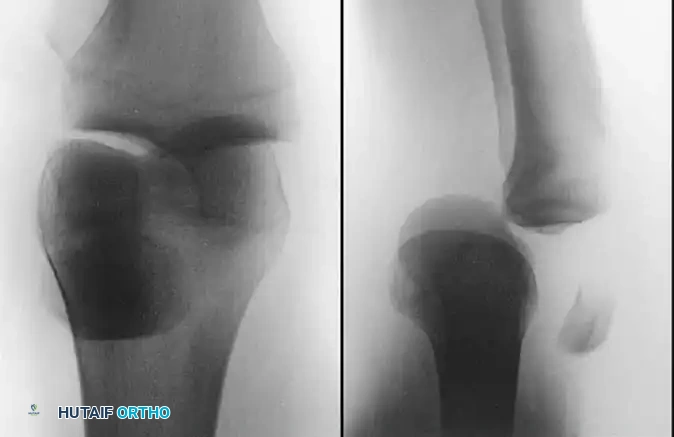
- Bony Avulsions: "Clinically isolated" acute PCL disruptions are repaired primarily if the ligament is avulsed with a substantial fragment of bone from the tibial insertion.
- Femoral "Peel-Off" Lesions: Frequently seen in knee dislocations, the PCL may avulse cleanly from its femoral origin. Acute surgical repair of these specific lesions yields excellent results.
- Mid-Substance Tears: Primary repair of mid-substance tears is contraindicated. Suture alone cannot withstand the immense forces applied to the knee, and augmentation techniques (e.g., semitendinosus wrapping) have proven inadequate. These require formal reconstruction.
Treatment Algorithm for PCL Avulsion Fractures
- Large Fragment: Open Reduction and Internal Fixation (ORIF).
- Small Fragment with Posterior Tibial Translation < 10 mm: Quadriceps-focused rehabilitation.
- Small Fragment with Posterior Tibial Translation > 10 mm: Formal PCL reconstruction.
SURGICAL TECHNIQUES
As with anterior cruciate ligament (ACL) surgery, a diagnostic arthroscopy is performed prior to any open procedure to evaluate and address intra-articular pathology (e.g., meniscal tears, chondral defects).
Open Reduction and Internal Fixation of PCL Avulsion Fractures
Bony avulsions of the PCL from the posterior tibia represent a unique subset of injuries amenable to anatomic repair.
- Positioning: The patient is positioned prone. A tourniquet is applied to the proximal thigh.
- Surgical Approach: The classic Burks and Schaffer posteromedial approach is utilized. An inverted L-shaped incision is made over the popliteal fossa.
- Superficial Dissection: The deep fascia is incised. The interval between the medial head of the gastrocnemius and the semimembranosus is identified and developed.
- Deep Dissection: The medial gastrocnemius is retracted laterally, which safely protects the neurovascular bundle (popliteal artery and vein) located lateral to the muscle belly.
- Fixation: The posterior joint capsule is incised to expose the avulsed tibial facet. The fracture bed is debrided of hematoma. The fragment is reduced anatomically and fixed using one or two cannulated lag screws with soft-tissue washers. If the fragment is comminuted, heavy non-absorbable sutures can be passed through the ligament substance and tied over a bone bridge on the anterior tibia via drill holes.
Surgical Warning: The popliteal artery lies directly posterior to the posterior capsule, often within millimeters of the PCL tibial attachment. Meticulous retraction of the medial gastrocnemius laterally is paramount to shield the neurovascular structures during the posteromedial approach.
Primary Repair of Femoral "Peel-Off" Lesions
In the setting of an acute knee dislocation where the PCL is avulsed from the medial femoral condyle, primary repair can be performed. Suture anchors are placed into the anatomic footprint on the lateral aspect of the medial femoral condyle. Heavy non-absorbable sutures are woven through the proximal stump of the PCL using a Krackow or whipstitch technique and tied securely, restoring the native ligament tension.
Arthroscopically Assisted PCL Reconstruction
For mid-substance tears or chronic insufficiency, reconstruction is required. Autogenous bone-patellar tendon-bone (BPTB), Achilles tendon allograft, or quadrupled hamstring autografts are commonly utilized.
- Graft Selection: BPTB provides excellent bone-to-bone healing but can exacerbate patellofemoral pain—a significant concern given the already elevated patellofemoral pressures in PCL-deficient knees. Achilles allograft provides a robust bone block for the femoral tunnel and ample soft tissue for the tibial tunnel.
- Tibial Tunnel Preparation: This is the most critical and dangerous step. Viewing from a posteromedial portal is highly recommended. A PCL tibial guide is inserted through the anteromedial portal and hooked over the posterior facet of the tibia, approximately 1 cm distal to the joint line.
- Drilling the Tibia: A guide pin is drilled from the anteromedial tibia to the posterior footprint. Fluoroscopic confirmation is mandatory to ensure the pin does not penetrate too far posteriorly, endangering the popliteal artery. A curette is placed over the tip of the guide pin posteriorly to protect the neurovascular structures while the reamer is advanced.
- Femoral Tunnel Preparation: The femoral footprint is identified on the lateral aspect of the medial femoral condyle. An outside-in or inside-out technique can be used to drill the femoral tunnel, ensuring placement mimics the native anterolateral bundle of the PCL (which is tight in flexion).
- Graft Passage and Fixation: The graft is passed, usually from distal to proximal. The femoral side is fixed first (e.g., interference screw). The knee is then cycled. Tibial fixation is performed with the knee at 90 degrees of flexion while an anterior drawer force is applied to restore the normal anatomic tibial step-off.
POSTOPERATIVE PROTOCOLS AND OUTCOMES
Rehabilitation Following Reconstruction
Postoperative rehabilitation following PCL reconstruction is inherently more conservative than ACL rehabilitation to protect the graft from the posterior pull of gravity and the hamstring muscles.
* Immobilization: The knee is locked in full extension in a dynamic PCL brace for 2 to 4 weeks. The brace applies an anteriorly directed force to the posterior calf, preventing tibial sag.
* Weight-Bearing: Touch-down weight-bearing is maintained for the first 4 to 6 weeks.
* Range of Motion: Passive prone ROM is initiated early to prevent arthrofibrosis, strictly limiting flexion to 90 degrees for the first 6 weeks to avoid stretching the graft.
* Strengthening: Closed-chain quadriceps exercises begin early. Active hamstring curls are strictly prohibited for at least 3 to 4 months.
Long-Term Outcomes and Complications
The success of surgical reconstruction in terms of restoring absolute stability remains variable. Long-term results after PCL reconstruction with autogenous BPTB grafts have shown a reduction in posterior laxity to approximately Grade 1.0 to 1.5; however, posterior laxity is rarely eliminated entirely.
Despite improvements in objective stability, the ability of PCL reconstruction to halt the progression of osteoarthritis remains unproven. Patients must be counseled that while surgery may alleviate symptoms of instability and improve kinematics, the long-term risk of medial compartment and patellofemoral arthrosis remains a clinical reality. Close longitudinal observation for functional deterioration is mandatory for all patients, regardless of whether they are managed operatively or nonoperatively.
You Might Also Like