Traumatic Knee Dislocations: Comprehensive Surgical Management and Posteromedial Approaches
Key Takeaway
Traumatic knee dislocations are severe, limb-threatening injuries often complicated by spontaneous reduction prior to clinical evaluation. This comprehensive guide details the critical assessment of popliteal artery and peroneal nerve injuries, particularly in ultralow-velocity dislocations among morbidly obese patients. It provides a step-by-step masterclass on the posteromedial surgical approach for posterior cruciate ligament reconstruction, emphasizing neurovascular protection, precise capsular exposure, and evidence-based postoperative rehabilitation protocols.
TRAUMATIC KNEE DISLOCATIONS: PATHOLOGY AND EPIDEMIOLOGY
In comparison to other ligamentous injuries of the knee, true traumatic knee dislocations are relatively uncommon. However, the true incidence is likely underestimated because a significant number of knee dislocations undergo spontaneous reduction prior to medical evaluation. A knee dislocation is defined by the complete disruption of the tibiofemoral articulation, which inherently requires the rupture of multiple primary static stabilizers—typically both cruciate ligaments and at least one collateral ligament complex.
In an acutely dislocated knee that remains unreduced, the diagnosis is usually obvious due to gross clinical deformity, profound pain, and massive soft-tissue swelling. However, the diagnostic challenge increases exponentially in specific clinical scenarios: morbidly obese patients, patients whose knees have spontaneously reduced at the scene of the accident, and polytrauma patients where distracting injuries may mask the knee pathology.
Clinical Pitfall: Failure to correctly diagnose a spontaneously reduced knee dislocation diminishes the likelihood of recognizing a concomitant injury to the popliteal artery. Missed popliteal artery injuries lead to devastating, irreversible complications, including profound tissue ischemia, compartment syndrome, and the need for above-knee amputation.
Mechanisms of Injury: High-Velocity vs. Low-Velocity
Historically, traumatic knee dislocations have been dichotomized into high-velocity and low-velocity injuries based on the energy imparted to the joint:
- High-Velocity Dislocations: These are typically the result of immense kinetic energy transfer. Common mechanisms include high-speed motor vehicle accidents, falls from significant heights, or severe industrial crush injuries. These patients frequently present with concomitant life-threatening polytrauma, open fractures, and severe soft-tissue degloving.
- Low-Velocity Dislocations: These injuries most often occur during athletic endeavors. Sports involving high-impact collisions (e.g., American football, rugby) or high-velocity pivoting (e.g., skiing, gymnastics) are common culprits. While the systemic trauma is lower, the joint-specific damage remains catastrophic.
THE "ULTRALOW-VELOCITY" DISLOCATION IN THE MORBIDLY OBESE
Recent epidemiological shifts have highlighted a highly specific and dangerous subset of knee dislocations occurring in morbidly obese patients. These are termed ultralow-velocity knee dislocations. Unlike sports or motor vehicle trauma, these injuries occur during routine activities of daily living (ADLs), such as stepping off a curb, descending a single stair, or simply experiencing a mechanical fall while walking.
The biomechanical reality is that in a patient with extreme body mass, the kinetic energy generated by a simple ground-level fall is sufficient to completely rupture the multiligamentous complexes of the knee.

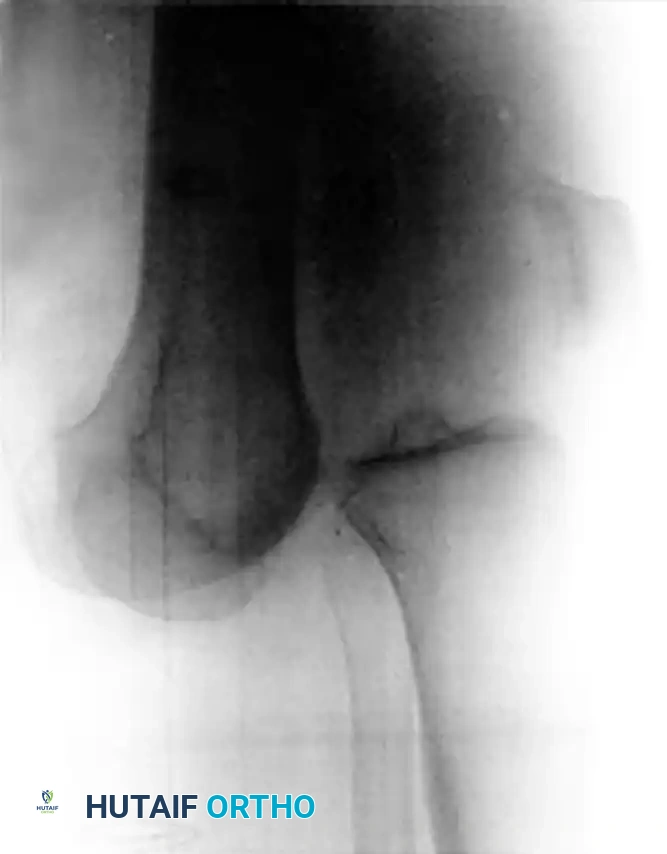
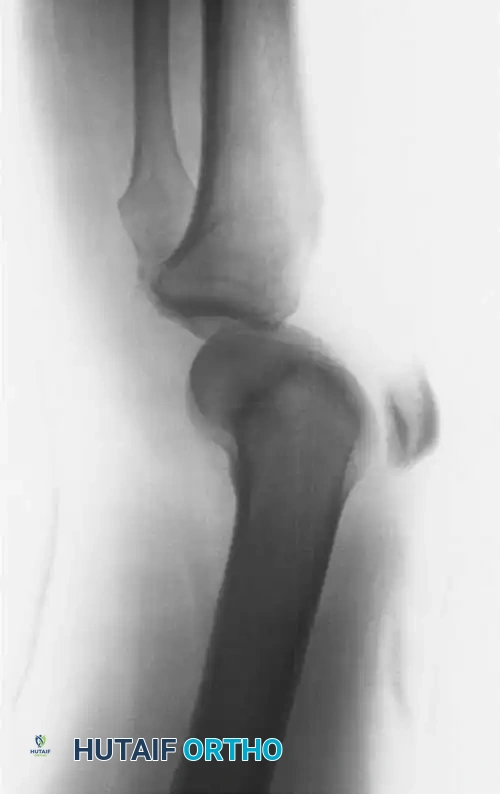
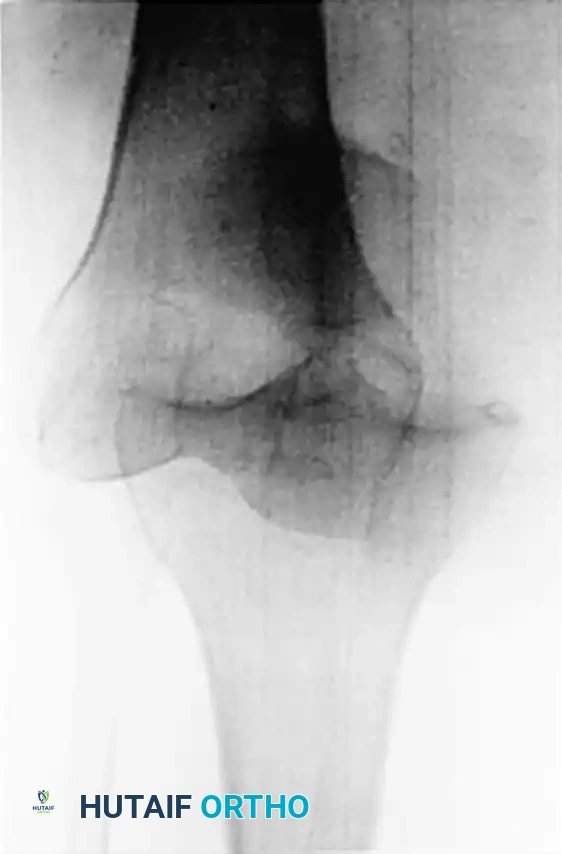
Figure 45-145: Anteroposterior (A) and Lateral (B) radiographs demonstrating an ultralow-velocity knee dislocation in a morbidly obese patient. Note the complete loss of tibiofemoral congruity.
Clinical Correlation: BMI and Neurovascular Injury Severity
A landmark institutional review of 17 patients (11 women and 6 men) with ultralow-velocity dislocations revealed alarming statistics regarding morbidity. The average age of this cohort was 28.6 years, and all 17 patients were clinically obese, presenting with an average Body Mass Index (BMI) of 48 (clinical obesity is defined as a BMI ≥ 30).
The incidence of neurovascular compromise in this specific demographic is exceptionally high:
* Popliteal Artery Injuries: Occurred in 7 of the 17 patients (41%).
* Neurological Injuries (Peroneal Nerve): Occurred in 7 of the 17 patients (41%).
* Amputation Rate: Two patients who underwent vascular repairs ultimately required above-knee amputations due to irreversible tissue ischemia.
A direct, positive correlation exists between the patient's BMI and the severity of the associated neurovascular injury:
* No Vascular or Nerve Injury: Average BMI of 39.58 (6 patients).
* Isolated Nerve Injury: Average BMI of 48.26.
* Isolated Vascular Injury: Average BMI of 56.28.
* Combined Nerve and Vascular Injuries: Average BMI of 60.29.
Surgical Warning: The morbidly obese patient presenting with knee pain after a low-energy fall must be treated with a high index of suspicion for a spontaneously reduced knee dislocation. The massive soft-tissue envelope can easily mask joint instability, and the risk of limb-threatening popliteal artery injury is statistically higher in this population than in athletic cohorts.
CLINICAL EVALUATION AND DIAGNOSTIC IMAGING
The initial evaluation of any suspected knee dislocation must prioritize limb viability. The popliteal artery is firmly tethered proximally at the adductor hiatus and distally at the soleal arch. During a dislocation—particularly hyperextension or posterior translation injuries—the artery is subjected to severe traction, leading to intimal tearing, thrombosis, or complete transection.
Vascular Assessment Protocol
- Immediate Pulse Check: Assess dorsalis pedis and posterior tibial pulses.
- Ankle-Brachial Index (ABI): An ABI must be performed on all suspected knee dislocations. An ABI < 0.9 is highly sensitive for arterial injury and mandates immediate advanced imaging.
- CT Angiography (CTA): The gold standard for diagnosing popliteal artery injury. If hard signs of vascular injury are present (expanding hematoma, pulsatile bleeding, absent pulses, cold/pale limb), surgical exploration by a vascular surgeon should not be delayed for imaging.
Pediatric Considerations
In skeletally immature patients, the physes are biomechanically weaker than the surrounding ligamentous structures. A suspected knee dislocation in a child or adolescent may actually represent a displaced distal femoral or proximal tibial physeal fracture.
* Stress Radiographs: In the skeletally immature patient with a clinically unstable knee but normal static radiographs, stress radiographs under anesthesia should be obtained to rule out an occult physeal injury (Salter-Harris type I or II) before diagnosing a pure ligamentous dislocation.
SURGICAL MANAGEMENT: THE POSTEROMEDIAL APPROACH
Once life- and limb-threatening injuries have been addressed, definitive surgical reconstruction of the multiligamentous knee is required. Regardless of the patient's BMI, those who undergo comprehensive ligament reconstructions—especially those including posterolateral corner (PLC) repair or reconstruction—demonstrate significantly better subjective and objective functional outcomes compared to those managed nonoperatively or with incomplete reconstructions.
Reconstruction of the posterior cruciate ligament (PCL) often requires direct visualization of the posterior tibial footprint. The posteromedial approach provides excellent, safe exposure to the posterior joint capsule, the posterior horn of the medial meniscus, and the tibial attachment of the PCL.
Indications for the Posteromedial Approach
- Tibial inlay PCL reconstruction (e.g., the Berg technique).
- Repair of posterior capsular avulsions.
- Fixation of posterior tibial plateau fractures.
- Excision of posterior compartment loose bodies or tumors.
Patient Positioning and Anesthesia
- Anesthesia: General anesthesia with complete neuromuscular blockade is preferred to allow for uninhibited manipulation of the limb and retraction of the robust posterior musculature.
- Positioning: The patient is placed in the prone position. All bony prominences must be meticulously padded.
- Tourniquet: A high-thigh tourniquet is applied. The leg is prepped and draped free to allow for full flexion and extension of the knee during the procedure.
Step-by-Step Surgical Technique
1. Incision and Superficial Dissection
- Palpate the posterior joint line and the medial border of the gastrocnemius muscle.
- Make a curvilinear or "hockey-stick" incision. The vertical limb of the incision should overlie the medial aspect of the medial head of the gastrocnemius muscle.
- Carry the dissection sharply through the subcutaneous tissues down to the deep fascial layer.
- Incise the deep fascia vertically, directly over the medial head of the gastrocnemius.
Surgical Pearl: Neurological Protection
Meticulously identify and protect the medial sural cutaneous nerve (the posterior cutaneous nerve of the calf). This nerve usually perforates the deep fascia distal to the horizontal limb of the incision. Iatrogenic injury to this nerve will result in painful neuromas and sensory deficits over the posterior calf.
2. Deep Dissection and Interval Development
- Identify the medial border of the medial head of the gastrocnemius.
- Bluntly develop the internervous and intermuscular interval between the medial gastrocnemius and the semimembranosus tendon.
- Retract the semimembranosus medially and the medial head of the gastrocnemius laterally.
Surgical Pearl: Motor Branch Protection
By applying strictly lateral retraction on the medial head of the gastrocnemius, no tension is directly applied to the motor branch innervating it. This motor branch is the only branch from the tibial nerve in the popliteal fossa that traverses medially. Furthermore, the thick muscle belly of the laterally retracted gastrocnemius acts as a physical barrier, protecting the central neurovascular bundle (popliteal artery, popliteal vein, and tibial nerve) as the posterior capsule is exposed. Dissection on this protected medial side of the popliteal fossa is therefore relatively safe.
3. Capsular Exposure and Vascular Control
- As the interval is deepened, the posterior joint capsule will come into view.
- The middle geniculate artery is frequently encountered piercing the mid-posterior capsule to supply the cruciate ligaments. This vessel can cause troublesome bleeding and should be isolated, clamped, and ligated (or cauterized) if necessary to maintain a clear surgical field.
- Expose the posterior aspect of the proximal tibia and the posterior margins of the medial femoral condyle.
4. Enhancing the Exposure
- If further lateral exposure of the posterior intercondylar notch is necessary, the surgeon may release a portion of the tendinous origin of the medial head of the gastrocnemius from the posterior distal femur and the joint capsule.
- Note: Slight knee flexion (10 to 15 degrees) will relax the posterior structures and significantly aid exposure. Complete sectioning of the medial head of the gastrocnemius is rarely, if ever, needed.
5. Arthrotomy and PCL Footprint Identification
- Make a vertical incision directly through the posterior capsule.
- Retract the capsular leaflets to expose the contents of the posterior intercondylar notch.
- Identify the tibial attachment (footprint) of the posterior cruciate ligament. This footprint is located in the PCL facet, extending distally over the posterior "drop-off" of the proximal tibia.
- From this point, the surgeon may proceed with the definitive reconstruction, such as the tibial inlay technique described by Berg, which involves securing a bone block into a surgically created trough at the PCL footprint.
6. Closure
- Following definitive fixation, thoroughly irrigate the posterior compartment to remove all bone debris.
- Suture the vertical capsular incision using heavy absorbable sutures.
- Release the retractors and allow the medial head of the gastrocnemius to settle back into its anatomical position. If the tendinous origin was partially released, it may be repaired with heavy sutures.
- Approximate the deep fascia and subcutaneous layers to eliminate dead space.
- Close the skin in a routine fashion using non-absorbable sutures or surgical staples.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The postoperative management of a multiligamentous knee reconstruction is complex and must be tailored to the specific ligaments repaired, the quality of the tissue, and the patient's compliance.
- Immobilization: The knee is typically immobilized in a hinged knee brace locked in full extension for the first 2 to 4 weeks to protect the posterior capsular repair and the PCL reconstruction from posterior tibial sag.
- Weight-Bearing: Patients are generally restricted to non-weight-bearing or toe-touch weight-bearing for the first 4 to 6 weeks to protect the articular cartilage and the graft fixation sites.
- Range of Motion (ROM): Early, controlled passive range of motion is critical to prevent arthrofibrosis, a common complication following multiligamentous knee injuries. Prone passive flexion limits posterior tibial translation and protects the PCL graft.
- Strengthening: Quadriceps activation is encouraged immediately. Hamstring strengthening is typically delayed for 3 to 4 months to prevent posterior sheer forces on the healing PCL graft.
In conclusion, traumatic knee dislocations represent a formidable orthopedic challenge. The rising incidence of ultralow-velocity dislocations in the morbidly obese population necessitates a heightened clinical awareness of occult neurovascular injuries. When surgical intervention is indicated, a meticulous posteromedial approach provides safe, highly effective access to the posterior knee, ensuring optimal outcomes in complex multiligamentous reconstructions.
You Might Also Like