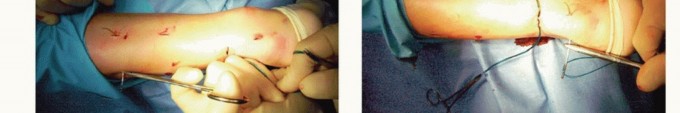
Achilles Tendon Open Lengthening: What to Expect & Recovery
Key Takeaway
Your ultimate guide to Achilles Tendon Open Lengthening: What to Expect & Recovery starts here. **Achilles tendon open** lengthening is a surgical procedure to correct equinus deformity, a plantarflexed position of the calcaneus relative to the tibia. This condition results from shortening of the Achilles tendon or gastrocsoleus complex. The procedure specifically addresses rigid, fixed deformities that do not correct with passive manipulation, aiming to restore proper foot alignment and function.
Introduction and Epidemiology
Shortening of the Achilles tendon, the gastrocsoleus complex (triceps surae), or a combination of both, results in an equinus (plantarflexed) position of the calcaneus relative to the tibia. Equinus deformity represents one of the most common musculoskeletal pathologies encountered in both pediatric and adult orthopedic surgery. The deformity is broadly categorized as either congenital or acquired, and its clinical presentation is further subdivided into dynamic or rigid contractures. A dynamic deformity, often driven by spasticity, will correct with passive manipulation or under anesthesia, whereas a rigid or fixed deformity involves structural shortening of the myotendinous units and does not correct passively.
The pathogenesis of congenital equinus is frequently associated with complex limb deformities, including idiopathic clubfoot (talipes equinovarus) or congenital vertical talus. In these scenarios, the Achilles contracture is a primary component of the multiplanar deformity. Acquired equinus deformity is most classically observed secondary to cerebral palsy (CP). In CP, upper motor neuron lesions lead to muscle spasticity and dynamic imbalance, which, over time, causes a failure of longitudinal muscle growth and subsequent rigid contracture of the Achilles tendon and gastrocsoleus complex.
The specific pattern of deformity in CP depends on the anatomic distribution of spasticity. Muscle imbalance and spasticity in spastic diplegic cerebral palsy frequently result in an equinoplanovalgus deformity, where the midfoot breaks down to compensate for hindfoot equinus. Conversely, spastic hemiplegic cerebral palsy typically presents with an equinovarus deformity due to the overactivity of the posterior tibialis coupled with the triceps surae.
Beyond cerebral palsy, compensatory balance mechanisms required to maintain ambulation in patients with Duchenne muscular dystrophy frequently result in an equinus deformity. Posttraumatic equinus can arise from severe burns leading to posterior scar contracture, prolonged postburn positioning, anterior leg muscle loss (e.g., compartment syndrome), or continued tibial growth in the presence of a rigid posterior scar. Furthermore, talocrural and subtalar capsular adhesions, along with abnormal tibiotalar articulations, may contribute significantly to the loss of dorsiflexion.
The natural history of a fixed equinus deformity dictates that it will not correct spontaneously. It necessitates prescribed stretching, orthotic management, chemical denervation (e.g., botulinum toxin), or surgical intervention. Equinus associated with cerebral palsy is notably progressive. Despite conservative and surgical treatments, the deformity can recur due to persistent spasticity, muscle imbalance, or continued skeletal growth. Uncorrected equinus deformity results in significant gait pathology, characterized by altered ankle kinematics, decreased anterior translation of the tibia over the foot during the stance phase, premature heel rise, and impaired push-off kinetics.
Surgical Anatomy and Biomechanics
A profound understanding of the triceps surae anatomy is critical for executing an Achilles tendon open lengthening while minimizing morbidity. The triceps surae consists of the two heads of the gastrocnemius muscle and the deeper soleus muscle. The medial and lateral heads of the gastrocnemius originate on the posterior aspect of the medial and lateral condyles of the distal femur, respectively, making the gastrocnemius a biarticular muscle that crosses both the knee and the ankle.
The muscle fibers of the gastrocnemius terminate at a broad, flat muscle-tendon junction at the midcalf. From this aponeurosis, the Achilles tendon is formed and is subsequently joined by tendon fibers originating from the posterior aspect of the soleus muscle, which is uniarticular, originating from the posterior tibia and fibula.
As the Achilles tendon courses distally, its morphology changes significantly. Proximally, the tendon is broad and flat. As it progresses to its midsection, it becomes increasingly rounded and undergoes a distinct 90-degree internal rotation before its insertion on the posterosuperior third of the calcaneus.

This internal rotation is of paramount biomechanical and surgical importance. The rotation causes the medial fibers of the proximal tendon to insert on the posterior portion of the calcaneus, while the anterior fibers rotate laterally.

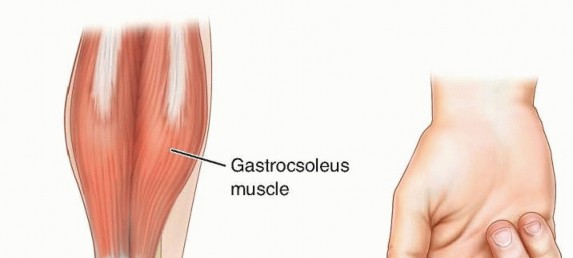
This alignment can be conceptualized as being similar to a crossed index and middle finger. The insertion footprint on the calcaneus is delta-shaped, and a small, distinct portion of the distal fibers courses inferiorly to interdigitate with the origin of the plantar fascia, creating a continuous myofascial chain.
The blood supply of the Achilles tendon is notably limited, rendering it susceptible to both spontaneous rupture and postoperative wound healing complications. The proximal portion of the tendon is supplied by intramuscular arterial branches from the gastrocnemius and soleus. The distal portion receives its vascularity from the tendon-bone interface at the calcaneus. The critical mid-substance of the tendon—often referred to as the watershed zone, located approximately 2 to 6 centimeters proximal to the calcaneal insertion—relies entirely on the surrounding paratenon for perfusion.

The Achilles tendon lacks a true synovial sheath. Instead, it is enveloped by the paratenon, a layer of loose connective tissue that supplies the mid-substance via discrete branches from the posterior tibial artery and, to a lesser extent, the peroneal artery. Preservation of the paratenon during surgical exposure is absolutely critical to maintain this tenuous blood supply and facilitate tendon healing.
Additionally, two distinct synovial bursae are located at the Achilles tendon insertion site. The subcutaneous calcaneal bursa is situated between the skin and the posterior aspect of the tendon, while the deep retrocalcaneal bursa is located between the anterior aspect of the tendon and the posterosuperior prominence of the calcaneus (Haglund's deformity).
Biomechanically, the triceps surae is the primary plantarflexor of the ankle. During a normal gait cycle, the gastrocnemius and soleus contract eccentrically during the second rocker (tibial advancement over the plantigrade foot) to control the forward progression of the tibia. During the third rocker (terminal stance), they contract concentrically to generate the power necessary for push-off. Over-lengthening of this complex severely compromises push-off power and leads to a catastrophic calcaneal gait or crouch gait, particularly in patients with neuromuscular disorders.
Indications and Contraindications
Patient selection and precise identification of the anatomic level of contracture are the most critical steps in managing equinus deformity. The decision to perform an open Achilles tendon lengthening versus an isolated gastrocnemius recession depends entirely on whether the contracture involves the entire triceps surae or is isolated to the gastrocnemius.
The Silfverskiöld test is the cornerstone of clinical evaluation. The ankle is dorsiflexed with the knee fully extended, and then dorsiflexed again with the knee flexed to 90 degrees. If equinus is present with the knee extended but corrects when the knee is flexed, the contracture is isolated to the biarticular gastrocnemius muscle. In this scenario, an isolated gastrocnemius recession (e.g., Strayer or Baumann procedure) is indicated. If the equinus contracture persists regardless of knee position, the contracture involves both the gastrocnemius and the uniarticular soleus muscle, necessitating a lengthening of the Achilles tendon itself.

Operative vs Non Operative Management
| Parameter | Indications | Contraindications / Alternatives |
|---|---|---|
| Non-Operative | Dynamic equinus, mild spasticity, age < 4 years (in CP), reducible deformity. | Fixed rigid contracture, midfoot break developing, severe gait impairment. |
| Achilles Lengthening (Open) | Rigid equinus present with knee flexed AND extended (positive Silfverskiöld for combined tightness). Severe clubfoot equinus. | Isolated gastrocnemius tightness (requires gastroc recession). Over-lengthened or weak triceps surae. |
| Gastrocnemius Recession | Rigid equinus present ONLY with the knee extended. | Combined gastrocsoleus contracture (will under-correct). |
Surgical intervention is indicated when conservative measures—such as physical therapy, serial casting, ankle-foot orthoses (AFOs), and botulinum toxin injections—have failed to halt the progression of the deformity or improve gait kinematics. In cerebral palsy, surgery is typically delayed until the child is at least 4 to 6 years old to allow for a more mature gait pattern to develop and to reduce the risk of recurrence due to subsequent longitudinal skeletal growth.
Contraindications to Achilles tendon lengthening include dynamic equinus that is fully correctable passively, underlying profound weakness of the triceps surae, and the presence of a crouch gait pattern. Lengthening the Achilles in a patient with an unrecognized crouch gait will exacerbate the crouch, leading to severe functional deterioration.
Pre Operative Planning and Patient Positioning
Preoperative planning begins with a meticulous physical examination and, ideally, a formalized 3D computerized gait analysis. Gait analysis provides objective kinematic and kinetic data, quantifying the degree of dynamic equinus, the presence of premature heel rise, and the power generated during push-off. It also helps differentiate primary equinus from compensatory equinus (e.g., secondary to hamstring contracture or knee flexion deformity).
Weight-bearing radiographs of the foot and ankle (anteroposterior and lateral views) are mandatory. The lateral radiograph is assessed for the presence of a midfoot break (rocker-bottom deformity), which occurs when the hindfoot is locked in equinus and the forefoot dorsiflexes through the transverse tarsal joints to achieve plantigrade contact. If a midfoot break is present, isolated Achilles lengthening may be insufficient, and concomitant midfoot stabilization or osteotomy may be required. Radiographs also rule out bony blocks to dorsiflexion, such as an anterior distal tibial osteophyte or a flattened talar dome.

For the procedure, the patient is placed in the prone position on a radiolucent operating table. General anesthesia is typically utilized. All pressure points, particularly the anterior superior iliac spines, patellae, and face, must be meticulously padded. A thigh tourniquet is applied to the operative extremity to provide a bloodless surgical field, though some surgeons prefer a calf tourniquet or no tourniquet to avoid ischemic muscle contracture that could alter intraoperative tensioning.
The entire lower extremity from the toes to the proximal thigh is prepped and draped in a standard sterile fashion. The ability to freely manipulate the knee and ankle intraoperatively is essential for assessing the adequacy of the lengthening.
Detailed Surgical Approach and Technique
The open Z-lengthening (Z-plasty) of the Achilles tendon is the gold standard for achieving a controlled, titratable correction of severe gastrocsoleus equinus. While percutaneous sliding techniques (e.g., Hoke triple hemisection) exist, the open approach provides superior visualization, allowing for precise control of the tendon rotation and meticulous repair of the paratenon.
Incision and Dissection
A longitudinal posteromedial incision is made, typically 5 to 8 centimeters in length, centered over the distal aspect of the Achilles tendon. The posteromedial approach is preferred over a direct posterior or posterolateral approach to avoid injury to the sural nerve, which courses lateral to the tendon in the distal third of the leg.

Subcutaneous tissues are sharply dissected. Hemostasis is achieved using bipolar electrocautery to prevent thermal injury to the underlying paratenon. The paratenon is identified as a distinct, thin layer of vascularized connective tissue enveloping the tendon.

A longitudinal incision is made precisely through the paratenon, and it is carefully elevated off the underlying epitenon using blunt dissection or tenotomy scissors. Retraction of the paratenon must be gentle; preserving this tissue is the most critical step in preventing postoperative wound breakdown and tendon necrosis.
Tendon Hemisection and Lengthening
Once the Achilles tendon is fully exposed, the planned Z-plasty cuts are marked. The orientation of the hemisections can be tailored to address concomitant coronal plane deformities (varus or valgus). Because of the 90-degree internal rotation of the tendon fibers, the distal medial fibers originate from the posterior gastrocnemius, while the distal lateral fibers originate from the anterior soleus.

For a standard lengthening, a longitudinal split is created in the midline of the tendon using a #15 blade, extending approximately 3 to 5 centimeters depending on the required lengthening.
* To correct an associated varus deformity, the distal cut is directed medially and the proximal cut is directed laterally.
* To correct an associated valgus deformity, the distal cut is directed laterally and the proximal cut is directed medially.
The transverse hemisections are then completed at the proximal and distal extents of the longitudinal split.

Following the completion of the cuts, the ankle is gently dorsiflexed. The surgeon will feel the tendon ends slide past one another. The goal of lengthening is to achieve a neutral ankle position (0 degrees of dorsiflexion) or a maximum of 5 to 10 degrees of dorsiflexion with the knee fully extended. Over-lengthening must be strictly avoided.
Tendon Repair and Closure
Once the desired length is achieved, the overlapping ends of the tendon are sutured together. A heavy, absorbable or non-absorbable suture (e.g., #1 or #2 Vicryl or FiberWire) is used.

Multiple figure-of-eight sutures or a modified Krackow technique can be employed to secure the tendon ends. The repair must be robust enough to withstand resting muscle tone and prevent postoperative elongation during the immobilization phase.

Following the tendon repair, the ankle is taken through a range of motion to ensure stability of the construct and confirm the elimination of the equinus contracture. The paratenon is then meticulously closed over the tendon using a fine absorbable suture (e.g., 3-0 or 4-0 Vicryl). This layer serves as a biological barrier, preventing adhesions to the overlying skin and restoring the vascular supply to the tendon. The subcutaneous tissue and skin are closed in a layered fashion.
Complications and Management
Complications following open Achilles tendon lengthening can be neurologically and functionally devastating if not recognized and managed promptly. The most catastrophic complication, particularly in the cerebral palsy population, is over-lengthening.
Common Complications and Salvage Strategies
| Complication | Incidence / Risk Factors | Prevention and Management Strategies |
|---|---|---|
| Over-Lengthening (Crouch Gait) | High risk in CP patients with unrecognized hamstring contractures. | Prevention: Strict adherence to neutral dorsiflexion during repair. Treat concurrent knee/hip flexor contractures. Management: Ground reaction AFOs; operative shortening (difficult and unpredictable). |
| Under-Correction / Recurrence | Common in growing children, severe spasticity. | Prevention: Ensure adequate release of both gastroc and soleus fibers. Management: Serial casting, bracing, revision lengthening if rigid. |
| Wound Breakdown / Infection | Higher risk in patients with poor vascularity, smoking, or diabetes. | Prevention: Meticulous paratenon closure, minimize electrocautery on skin edges. Management: Local wound care, antibiotics; flap coverage for exposed tendon. |
| Sural Nerve Injury | Risk increases with lateral incisions or blind percutaneous cuts. | Prevention: Posteromedial incision; direct visualization. Management: Gabapentinoids, surgical excision of painful neuroma if conservative treatment fails. |
| Tendon Rupture | Rare in open Z-plasty; higher in percutaneous sliding techniques. | Prevention: Robust suture repair, strict adherence to postoperative immobilization. Management: Open primary repair or reconstruction with FHL transfer if chronic. |
Over-lengthening results in a loss of plantarflexion power, leading to a calcaneal stance and progressive crouch gait. As the triceps surae weakens, the patient requires excessive knee flexion to maintain balance, placing immense stress on the patellofemoral joint and dramatically increasing the energy expenditure of ambulation. Salvage of an over-lengthened Achilles tendon is notoriously difficult and often requires complex orthotic management (e.g., ground reaction AFOs) or technically demanding tendon shortening procedures.
Wound complications are also a significant concern due to the tenuous blood supply of the posterior ankle skin and the underlying tendon watershed zone. Ischemia of the skin edges can lead to dehiscence, exposing the Achilles tendon and risking deep infection. Strict adherence to atraumatic soft tissue handling and meticulous paratenon closure are the best defenses against this complication.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the tendon repair while it heals, followed by a structured restoration of range of motion, strength, and gait mechanics.
Phase 1 Immobilization (Weeks 0 to 4)
Immediately following surgery, the patient is placed in a well-padded short leg cast or a rigid fracture boot. The ankle is immobilized in the newly corrected position, typically neutral (0 degrees). The knee is left free to allow for early mobilization and prevent stiffness. During this phase, the patient is strictly non-weight-bearing (NWB) on the operative extremity. Elevation is critical to manage edema and reduce tension on the posterior incision.
Phase 2 Protected Weight Bearing (Weeks 4 to 8)
At approximately 4 weeks postoperatively, the cast is removed, and the wound is inspected. If healing is progressing appropriately, the patient is transitioned to a removable controlled ankle motion (CAM) boot. Weight-bearing status is advanced from partial weight-bearing to weight-bearing as tolerated (WBAT). Active and active-assisted range of motion exercises for dorsiflexion and plantarflexion are initiated. Passive stretching into extreme dorsiflexion is strictly avoided to prevent elongation of the healing tendon.
Phase 3 Strengthening and Proprioception (Weeks 8 to 12)
By 8 weeks, the tendon has achieved sufficient tensile strength to begin formal strengthening. The CAM boot is weaned, and the patient transitions to regular footwear, often supplemented with a solid or articulated ankle-foot orthosis (AFO), particularly in patients with cerebral palsy, to maintain the correction and prevent recurrence. Physical therapy focuses on concentric and eccentric strengthening of the gastrocsoleus complex, core stability, and proprioceptive training.
Phase 4 Return to Baseline Activity (Months 3 to 6)
In the final phase of rehabilitation, the focus shifts to gait normalization and the return to baseline functional activities. Dynamic activities, such as single-leg heel raises, are integrated as tolerated. In the pediatric neuromuscular population, nighttime bracing may be continued indefinitely until skeletal maturity is reached to counteract the continuous deforming forces of spasticity and skeletal growth.
Summary of Key Literature and Guidelines
The surgical management of equinus deformity has evolved significantly over the past century, guided by foundational anatomical and biomechanical studies. The differentiation between isolated gastrocnemius contracture and combined gastrocsoleus contracture was first articulated by Silfverskiöld in 1924, and his eponymous clinical test remains the absolute standard for surgical decision-making today.
In the context of cerebral palsy, the work of Gage and Bleck has been instrumental in defining the indications for operative intervention. Bleck emphasized the danger of over-lengthening the Achilles tendon, coining the concept that "a little equinus is better than a calcaneal gait." This principle underscores the modern guideline that the Achilles should rarely be lengthened beyond neutral dorsiflexion in the spastic patient.
Recent literature, including systematic reviews comparing open Z-lengthening to percutaneous sliding techniques, demonstrates that while percutaneous techniques offer smaller incisions and potentially faster initial recovery, open lengthening provides superior precision in titrating the exact amount of lengthening and correcting coronal plane malalignments. The American Academy of Orthopaedic Surgeons (AAOS) and the Pediatric Orthopaedic Society of North America (POSNA) guidelines reinforce the necessity of comprehensive preoperative gait analysis and conservative management exhaustion prior to surgical lengthening in neuromuscular equinus.
Clinical & Radiographic Imaging











You Might Also Like