Mastering the Surgical Repair of Irreducible Knee Dislocation
Key Takeaway
We review everything you need to understand about Mastering the Surgical Repair of Irreducible Knee Dislocation. The surgical repair of irreducible congenital dislocation of the knee addresses a rare birth deformity where the tibia is subluxed or anteriorly dislocated on the femur, and spontaneous resolution is not expected. This intervention corrects the deformity, which is often due to shortened, fibrosed quadriceps and tight anterior capsules. Surgery aims to restore knee flexion, enabling proper ambulation for patients.
Introduction and Epidemiology
Congenital dislocation of the knee is a rare but profoundly debilitating musculoskeletal deformity that presents immediately at birth. Characterized by severe recurvatum and anterior displacement of the tibia on the femur, this condition demands prompt recognition and specialized orthopedic intervention. The incidence of congenital dislocation of the knee is estimated at approximately 1 per 100,000 live births, which constitutes roughly 1% of the incidence of developmental dysplasia of the hip. Despite its rarity, the condition carries significant implications for the child's ambulatory potential and overall lower extremity biomechanics.

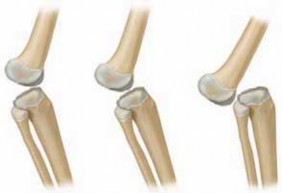
The deformity exists on a spectrum of severity, traditionally classified into three distinct grades: simple hyperextension, subluxation, and complete anterior dislocation of the tibia on the femur. While simple hyperextension may respond favorably to conservative measures, irreducible subluxations and complete dislocations invariably require meticulous surgical reconstruction to restore joint congruity and function.

Pathogenesis and Etiology
The precise etiology of congenital dislocation of the knee remains multifactorial, encompassing both intrinsic genetic anomalies and extrinsic mechanical factors. A genetic basis is strongly supported by familial occurrences and its frequent association with other congenital musculoskeletal anomalies. Patients presenting with congenital dislocation of the knee have a high concurrent incidence of developmental dysplasia of the hip, idiopathic clubfoot, and congenital vertical talus.

Extrinsic mechanical factors play a pivotal role in isolated cases. Aberrations in intrauterine positioning, particularly frank breech presentation, subject the developing fetal knee to chronic, abnormal mechanical forces. This positioning slowly stretches the hamstrings and posterior capsular structures while simultaneously allowing the quadriceps to contract and fibrose. Severe, syndromic presentations of congenital dislocation of the knee are frequently associated with global neuromuscular imbalances or connective tissue disorders. Notable associations include myelodysplasia, arthrogryposis multiplex congenita, Larsen syndrome, Ehlers-Danlos syndrome, Streeter dysplasia, and severe oligohydramnios sequences.

Natural History and Clinical Presentation
The natural history is entirely dependent on the initial severity of the deformity. Simple hyperextension often resolves spontaneously or with a brief period of serial casting and splinting. However, in cases of true subluxation or complete dislocation, spontaneous resolution is exceedingly rare. Left untreated, these patients face profound ambulatory deficits. The inability to flex the knee precludes normal gait mechanics, leading to severe compensatory abnormalities at the hip and ankle.

Clinical examination at birth reveals striking physical findings. The knee is locked in severe hyperextension, occasionally to such an extreme degree that the infant's foot rests against the anterior torso or face. Deep transverse skin creases are typically present over the anterior aspect of the knee, reflecting chronic in utero hyperextension. In subluxated or dislocated states, passive flexion is markedly restricted and elicits a firm, mechanical block.
Surgical Anatomy and Biomechanics
A profound understanding of the distorted anatomy in congenital dislocation of the knee is the cornerstone of successful surgical management. The pathology is not merely a displacement of normal structures but involves significant contractures, hypoplasia, and biomechanical alterations of the entire knee joint complex.

The Extensor Mechanism
The fundamental pathologic feature resides within the quadriceps muscle and the extensor mechanism. The absolute volume of the quadriceps muscle is typically diminished. More importantly, the quadriceps femoris tendon is severely shortened, fibrosed, and densely adherent to the anterior distal femur. This fibrosis is generally considered a secondary consequence of the chronic dislocated position rather than the primary cause, but it acts as the primary tether preventing reduction.
The patella is frequently hypoplastic and laterally displaced, riding high above the joint line. The lateral retinaculum is contracted and adherent to the underlying femoral condyle. Furthermore, the suprapatellar pouch—essential for normal gliding of the extensor mechanism during flexion—is invariably hypoplastic, obliterated, or entirely absent, necessitating surgical recreation during operative repair.

Capsuloligamentous Structures
The anterior articular capsule of the knee is severely contracted and thickened, forming an impenetrable barrier to posterior translation of the tibia. Conversely, the posterior capsule is stretched and redundant.
The biomechanics of the hamstring tendons are profoundly altered. Due to the chronic severe hyperextension, the hamstrings subluxate anteriorly past the mechanical axis of rotation of the knee joint. Once anterior to the center of rotation, the hamstrings undergo a functional inversion, acting as paradoxical knee extensors rather than flexors. This exacerbates the recurvatum deformity and creates a dynamic block to reduction.

Intraarticular structures exhibit variable pathology. The menisci are typically present and structurally normal, though their anatomic position may be distorted by the tibial subluxation. The cruciate ligaments demonstrate significant variability. They may be entirely normal, elongated, attenuated, or completely absent, particularly in syndromic cases such as Larsen syndrome.
Indications and Contraindications
The decision algorithm for managing congenital dislocation of the knee relies on the rigidity of the deformity, patient age, and the presence of associated syndromic conditions. Initial management for almost all presentations involves an attempt at gentle serial casting. Surgical intervention is reserved for cases that fail conservative management or present with rigid, irreducible deformities.

| Clinical Scenario | Management Strategy | Rationale and Considerations |
|---|---|---|
| Simple Hyperextension (Reducible) | Non-Operative | Serial casting and splinting usually yield excellent results. Deformity is flexible and responds to mechanical creep. |
| Subluxation (Partially Reducible) | Trial Non-Operative, Progress to Operative | Initial trial of casting. If 90 degrees of flexion cannot be achieved within 4 to 6 weeks, surgical release is indicated. |
| Complete Dislocation (Irreducible) | Operative | Dense fibrosis and capsular contracture preclude closed reduction. Forced closed reduction risks iatrogenic physeal fracture or vascular compromise. |
| Syndromic Presentation (Arthrogryposis) | Early Operative | Conservative measures universally fail due to dense, teratologic muscle fibrosis and rigid joint contractures. |
| Associated DDH | Staged Operative | The knee must be addressed first to allow for appropriate positioning (Pavlik harness or spica cast) required for subsequent hip management. |
Contraindications to immediate surgical intervention include active systemic infection, extreme prematurity with associated severe medical comorbidities precluding safe anesthesia, and compromised anterior soft tissue envelopes that cannot tolerate surgical incisions.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is essential to anticipate the extent of soft tissue release required and to manage concurrent orthopedic issues.

Imaging Modalities
Plain radiography remains the standard imaging modality. True lateral radiographs of the knee demonstrate the relationship of the proximal tibial ossification center to the distal femoral ossification center. In complete dislocations, the tibia sits entirely anterior and proximal to the femoral condyles. Anteroposterior radiographs help assess concurrent coronal plane deformities and the position of the patella.
Ultrasonography is highly valuable in the neonatal period before significant ossification occurs. It allows for dynamic assessment of the unossified cartilaginous anlagen, providing precise visualization of the degree of subluxation and the integrity of the extensor mechanism. Magnetic Resonance Imaging is rarely required for isolated cases but may be indicated in complex syndromic presentations to evaluate the cruciate ligaments and intraarticular congruity.

Operating Room Setup
The patient is positioned supine on a radiolucent operating table to facilitate intraoperative fluoroscopy. A sterile pneumatic tourniquet is applied to the proximal thigh to ensure a bloodless surgical field, which is critical for identifying delicate neurovascular structures and internervous planes in the infant knee.

The entire lower extremity, from the toes to the tourniquet, is meticulously prepped and draped free to allow for full manipulation of the limb. Intraoperative fluoroscopy should be positioned on the contralateral side of the table, ready to be brought in for orthogonal views to confirm concentric reduction.
Detailed Surgical Approach and Technique
The surgical objective is to achieve a concentric, stable reduction of the tibiofemoral joint while obtaining a minimum of 90 degrees of passive knee flexion. The most widely accepted and successful surgical technique is the extensive anterior approach with V-Y quadricepsplasty, as popularized by Curtis and Fisher.

Incision and Superficial Dissection
A generous anterior longitudinal midline incision is utilized, extending from the middle third of the anterior thigh, passing directly over the patella, and terminating at the tibial tubercle. In cases of severe lateral patellar subluxation, the incision may be slightly curved to accommodate the displaced anatomy.
Full-thickness fasciocutaneous flaps are elevated medially and laterally. It is imperative to maintain thick flaps to prevent postoperative skin necrosis, a recognized complication in this procedure. Dissection is carried down to expose the entire extensor mechanism, the medial and lateral retinacula, and the iliotibial band.

Extensor Mechanism Mobilization and Quadricepsplasty
The rectus femoris tendon is identified and isolated. An inverted V-shaped incision is made through the quadriceps tendon, with the apex of the V located proximally in the tendinous portion of the rectus femoris, and the limbs extending distally toward the medial and lateral borders of the patella.
The quadriceps mechanism is then sharply elevated from the anterior distal femur. In congenital dislocation of the knee, the muscle is densely adherent to the periosteum. Meticulous subperiosteal dissection is required to free the extensor mechanism, effectively recreating the obliterated suprapatellar pouch. The vastus medialis and vastus lateralis are mobilized from the intermuscular septa to allow distal excursion of the extensor mechanism.

Arthrotomy and Intraarticular Release
A comprehensive anterior capsulotomy is performed. The incision extends medially and laterally along the joint line, effectively detaching the anterior capsule from the tibia. The lateral structures, including the tight iliotibial band and the lateral retinaculum, are systematically released or lengthened via Z-plasty.
Attention is then directed to the hamstrings. The medially and laterally displaced hamstring tendons, which have subluxated anterior to the axis of rotation, must be identified. The surrounding fascial adhesions are released, allowing the hamstrings to drop back into their anatomic position posterior to the femoral condyles. This step is critical to eliminate their paradoxical extensor function.

Intraarticular inspection is performed to assess the menisci and cruciate ligaments. The anterior cruciate ligament may be contracted, tethering the tibia anteriorly. In such cases, fractional lengthening or judicious release may be necessary, though every effort should be made to preserve its stabilizing function.
Joint Reduction and Temporary Fixation
With all anterior tethering structures released and the hamstrings relocated posteriorly, the tibia is gently translated posteriorly and the knee is flexed. The reduction must be concentric and tension-free. Forced reduction against tight structures will inevitably lead to proximal tibial physeal injury or vascular compromise.

Once 90 degrees of flexion is achieved and concentric reduction is confirmed via intraoperative fluoroscopy, the joint is temporarily stabilized. A smooth, stout Kirschner wire (typically 1.6mm or 2.0mm depending on the infant's size) is driven retrograde from the anterior tibia, across the joint space, and into the distal femur, locking the knee in approximately 45 to 60 degrees of flexion.
The quadriceps tendon is then repaired in its lengthened position using a V-Y advancement technique. The limbs of the V are sutured together to form the stem of the Y, utilizing robust, non-absorbable or slowly absorbable sutures. The medial and lateral retinacula are repaired only if they do not restrict flexion. The wound is closed in layers over a closed suction drain to prevent hematoma formation.

Complications and Management
Surgical management of irreducible congenital dislocation of the knee is technically demanding and carries a distinct risk profile. Anticipation and early recognition of complications are vital for optimizing outcomes.
| Complication | Incidence | Etiology and Risk Factors | Prevention and Salvage Strategy |
|---|---|---|---|
| Skin Necrosis / Wound Dehiscence | Moderate (10-15%) | Thin skin flaps, excessive tension on closure over a flexed knee. | Maintain thick full-thickness flaps. If tension is excessive, limit initial flexion angle and increase flexion gradually during serial casting post-operatively. |
| Extensor Lag | High (30-50%) | Over-lengthening of the quadriceps tendon, inherent muscle weakness. | Careful titration of the V-Y advancement. Intensive post-operative physical therapy. Most lags improve with growth and strengthening. |
| Recurrent Dislocation or Subluxation | Low to Moderate (5-10%) | Inadequate soft tissue release, failure to relocate hamstrings posteriorly. | Ensure complete release of anterior capsule and iliotibial band. Revision surgery required if subluxation is rigid. |
| Joint Stiffness / Loss of Flexion | Moderate (15-20%) | Intraarticular adhesions, prolonged immobilization. | Limit transarticular pinning to 3-4 weeks. Initiate early, aggressive physical therapy and dynamic splinting. |
| Proximal Tibial Physeal Arrest | Rare (<5%) | Iatrogenic injury from transarticular K-wire or forced reduction. | Use smooth K-wires, central placement. Ensure soft tissue releases are complete so reduction requires minimal force. |

Vascular compromise is a catastrophic but exceedingly rare complication. The popliteal artery is stretched during reduction and flexion. Capillary refill and distal pulses must be meticulously assessed immediately after reduction and prior to applying the final cast. If vascular compromise is suspected, the knee must be extended until perfusion is restored, and the flexion angle increased gradually over subsequent weeks.
Post Operative Rehabilitation Protocols
The postoperative rehabilitation phase is as critical as the surgical execution. The protocol is designed to protect the extensor mechanism repair while preventing intraarticular adhesions and maintaining the achieved flexion.
Immediate Post Operative Phase
Postoperatively, the patient is placed in a well-padded long leg cast with the knee immobilized at the angle of fixation (typically 45 to 60 degrees of flexion). The transarticular Kirschner wire is left in place for 3 to 4 weeks to maintain concentric reduction while the anterior capsulotomy and soft tissues heal.
At 3 to 4 weeks, the patient is taken to the outpatient clinic or operating room for cast removal and pin extraction. A gentle manipulation under anesthesia may be performed to assess stability and range of motion. A new long leg cast is applied, increasing the flexion angle to 90 degrees if tolerated without tension on the skin or vascular compromise.

Long Term Follow Up and Functional Recovery
Following 6 to 8 weeks of total cast immobilization, the patient is transitioned to a Knee-Ankle-Foot Orthosis (KAFO). The orthosis is typically locked in 30 degrees of flexion during weight-bearing activities to prevent recurrent hyperextension, but unlocked during physical therapy.
Intensive physical therapy is initiated, focusing on active and passive range of motion, with a specific emphasis on hamstring strengthening and quadriceps re-education. Nighttime splinting in flexion may be required for up to a year to counteract the inherent tendency toward recurvatum.
Long-term follow-up is mandatory until skeletal maturity. These patients require vigilant monitoring for the development of secondary deformities, including valgus alignment, patellar instability, and leg length discrepancies. In syndromic patients, the functional outcome is often dictated by the severity of their underlying condition rather than the knee reconstruction itself.
Summary of Key Literature and Guidelines
The surgical management of congenital dislocation of the knee has evolved significantly, though the foundational principles established in the mid-20th century remain highly relevant.
The seminal work by Curtis and Fisher established the V-Y quadricepsplasty and extensive anterior release as the gold standard for irreducible deformities. Their approach addressed the fundamental pathology—the fibrotic extensor mechanism and the obliterated suprapatellar pouch—allowing for anatomic reduction without excessive tension.
Modern systematic reviews and clinical guidelines emphasize a step-wise approach. Non-operative management with serial casting is universally recommended as the first line of treatment for simple hyperextension and flexible subluxations. However, literature consistently demonstrates that rigid dislocations, particularly those associated with arthrogryposis or Larsen syndrome, are refractory to closed management and require early surgical intervention to optimize outcomes.
Recent studies highlight the importance of addressing concurrent developmental dysplasia of the hip. The current consensus dictates that the knee deformity must be resolved first—either via casting or surgery—to allow for the requisite 90 degrees of knee flexion necessary to safely apply a Pavlik harness or spica cast for hip reduction. Failure to coordinate the management of these concurrent conditions invariably leads to suboptimal outcomes in both joints.
Clinical & Radiographic Imaging




















You Might Also Like


