The Ultimate Guide to Runners: Conquer Knee Pain & Run Stronger
Key Takeaway
Learn more about The Ultimate Guide to Runners: Conquer Knee Pain & Run Stronger and how to manage it. Runner's knee, or patellofemoral pain syndrome (PFPS), is a common condition causing dull, aching pain around the kneecap, prevalent in runners and athletes due to repetitive knee movements. Symptoms include pain with bending, stiffness, or swelling. This comprehensive guide to runners outlines causes, symptoms, and recommended treatments, from rest and icing to professional medical diagnosis and rehabilitation, ensuring effective management and recovery.
Introduction & Epidemiology
Patellofemoral pain syndrome (PFPS), commonly referred to as "runner's knee," represents a prevalent and often recalcitrant musculoskeletal disorder primarily characterized by retropatellar or peripatellar pain. This pain is typically exacerbated by activities involving repetitive knee flexion and extension under load, such as running, jumping, squatting, and ascending/descending stairs. While highly prevalent in athletic populations, particularly runners, adolescents, and military recruits, it can affect individuals across all activity levels.

Epidemiologically, PFPS accounts for approximately 25-40% of all knee pain presentations in sports medicine clinics, with a higher incidence observed in females compared to males. The etiology is multifactorial, commonly attributed to a complex interplay of biomechanical abnormalities, muscular imbalances, overuse, and anatomical predispositions. These factors collectively contribute to altered patellofemoral kinematics and increased stress on the patellofemoral joint, leading to microtrauma and subsequent pain generation within the subchondral bone, synovium, or peripatellar soft tissues.
The diagnosis of PFPS remains a clinical one, primarily based on patient history and physical examination findings, with imaging often utilized to exclude other intra-articular pathologies rather than to confirm PFPS. Despite its high incidence, the precise pathophysiology remains an area of ongoing research, making its management challenging and necessitating a comprehensive understanding of relevant anatomy, biomechanics, and evidence-based therapeutic strategies. This review aims to provide an exhaustive academic perspective for orthopedic professionals, detailing the surgical anatomy, biomechanics, indications for intervention, surgical techniques where applicable, and comprehensive post-operative management strategies.
Surgical Anatomy & Biomechanics
A thorough understanding of patellofemoral anatomy and its intricate biomechanical relationships is paramount for effective diagnosis and management of PFPS. The patellofemoral joint is a trochlear articulation between the patella and the femoral trochlear groove, designed to facilitate efficient quadriceps function and protect the anterior knee.
Osseous Anatomy
- Patella: The largest sesamoid bone, embedded within the quadriceps tendon. Its posterior articular surface is covered with thick hyaline cartilage, typically featuring a vertical ridge dividing medial and lateral facets, with an odd facet medially.
-
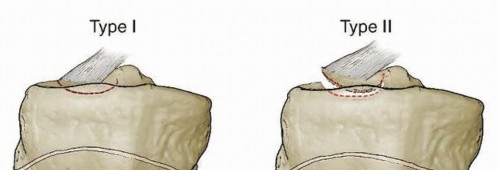
Femoral Trochlea:
A groove on the anterior distal femur, conforming to the patellar articular facets. The lateral trochlear facet is typically more prominent than the medial, contributing to patellar stability. Trochlear dysplasia, characterized by a flattened or convex groove, is a significant risk factor for patellar instability and subsequent PFPS.

Soft Tissue Stabilizers
Patellofemoral stability is maintained by a dynamic equilibrium between static and dynamic stabilizers.
-
Static Stabilizers:
- Medial Patellofemoral Ligament (MPFL): The primary static restraint to lateral patellar translation, originating from the medial femoral epicondyle and inserting onto the superomedial patella. It provides 50-60% of the total resistance to lateral displacement, particularly in early flexion (0-30 degrees).
- Medial Patellotibial Ligament (MPTL) and Medial Patellomeniscal Ligament (MPML): Secondary medial stabilizers contributing to inferior and medial stability.
- Lateral Retinaculum: Comprises the lateral patellofemoral ligament and lateral patellotibial ligament, providing lateral stability. Excessive tightness can contribute to lateral patellar tilt and increased lateral facet pressure.
- Fascial Structures: Iliotibial band (ITB) and retinacular fibers blend into the patella.
-
Dynamic Stabilizers:
-
Quadriceps Femoris Muscle:
Comprising rectus femoris, vastus lateralis (VL), vastus medialis (VM), and vastus intermedius.
- Vastus Medialis Obliquus (VMO): The most distal and oblique fibers of the VM, crucial for medial patellar stabilization, especially during terminal knee extension. Weakness or delayed activation relative to the VL is frequently implicated in PFPS.
- Vastus Lateralis: Exerts a lateral pull on the patella. Imbalance with the VMO can lead to lateral patellar tracking.
- Hip Musculature: Weakness in hip abductors (gluteus medius) and external rotators (gluteus maximus, piriformis) can lead to increased femoral internal rotation and adduction during gait, effectively increasing the Q-angle and lateral stress on the patellofemoral joint.
-
Quadriceps Femoris Muscle:
Comprising rectus femoris, vastus lateralis (VL), vastus medialis (VM), and vastus intermedius.
Patellofemoral Biomechanics and Kinematics
- Patellar Tracking: The patella glides within the trochlear groove during knee flexion and extension. Optimal tracking involves smooth, centered movement without excessive medial or lateral deviation, tilt, or rotation.
- Contact Area and Stress: The patellofemoral contact area shifts throughout the range of motion. In early flexion (0-20 degrees), contact is primarily distal. As flexion increases, contact moves proximally and widens, involving more medial and lateral facets. Peak contact stresses occur around 45-90 degrees of flexion, particularly with weight-bearing activities. Altered kinematics (e.g., lateral maltracking, tilt) can concentrate stress over smaller areas, leading to cartilage overload and pain.
-
Q-Angle (Quadriceps Angle):
The angle formed by a line from the ASIS to the center of the patella and a line from the center of the patella to the tibial tubercle. An elevated Q-angle (typically >15-20 degrees in males, >20-22 degrees in females, depending on measurement technique and reference) is associated with increased lateral patellar pull and higher risk of PFPS.

- Foot Pronation: Excessive foot pronation can lead to internal rotation of the tibia and femur, contributing to a "dynamic Q-angle" increase and altered patellofemoral mechanics.
- ITB Tightness: A tight ITB can increase lateral pull on the patella via its insertion into the lateral retinaculum, contributing to lateral tilt.
- Tibial Tubercle-Trochlear Groove (TT-TG) Distance: A measure of the lateralization of the tibial tubercle relative to the trochlear groove. A TT-TG distance >20mm on MRI or CT is generally considered indicative of significant lateralization and a risk factor for patellar instability and potentially PFPS.
Indications & Contraindications
The vast majority of patellofemoral pain syndrome cases are successfully managed non-operatively. Surgical intervention for PFPS is reserved for a highly selected cohort of patients with specific underlying anatomical derangements, recalcitrant symptoms despite exhaustive conservative management, or concomitant pathologies. It is critical to recognize that PFPS itself is generally not a surgical diagnosis; rather, surgery targets specific, identifiable contributing factors.
Non-Operative Indications
All patients presenting with PFPS should initially undergo a structured non-operative management protocol.
- Initial Presentation: Acute or chronic pain consistent with PFPS without signs of mechanical locking, gross instability, or significant structural damage.
- Absence of Specific Surgical Pathology: No evidence of recurrent patellar dislocation/subluxation, significant trochlear dysplasia, large symptomatic chondral defects amenable to repair, or symptomatic plica syndrome.
- Motivation for Rehabilitation: Patient's willingness and ability to commit to a comprehensive physical therapy program.
Operative Indications
Surgical intervention is considered only after a minimum of 6-12 months of appropriately directed, rigorous non-operative treatment has failed to alleviate symptoms, and a clear, surgically amenable pathology has been identified as the primary driver of the patient's PFPS.
-
Recurrent Patellar Instability with Concomitant Pain:
- Symptomatic recurrent patellar dislocations/subluxations that contribute to chronic anterior knee pain.
- Significant anatomical risk factors for instability (e.g., high TT-TG distance >20mm, trochlear dysplasia, patella alta, MPFL insufficiency).
- This is often the strongest indication for surgical intervention, addressing the instability which secondarily reduces PFPS symptoms.
-
Severe Chondral Lesions:
- Focal, full-thickness patellar or trochlear chondral defects (>1.5-2 cm²) causing mechanical symptoms or recalcitrant pain, especially if associated with maltracking.
- Lesions amenable to cartilage restoration procedures (e.g., microfracture, OATS, ACI/MACI).
-
Symptomatic Plica Syndrome:
- A discrete, thickened, fibrotic medial patellar plica causing mechanical irritation and pain, confirmed by diagnostic injection or arthroscopic findings, and resistant to conservative measures.
- Typically indicated after excluding other causes of anterior knee pain.
-
Persistent Lateral Patellar Compression Syndrome with Lateral Tilt:
- Severe, isolated lateral patellar hyperpressure and tilt despite extensive physical therapy to address quadriceps imbalance and ITB tightness.
- This may rarely warrant a lateral retinacular release, but only with extreme caution and clear indications, as it often fails to resolve symptoms and can exacerbate instability if performed inappropriately. Dynamic patellar tilt (seen on MRI at various flexion angles) may guide this decision.
-
Tibial Tubercle Lateralization/Malalignment:
-
Elevated TT-TG distance (>20mm) contributing to significant lateral patellar overload and pain, particularly in the presence of patella alta. This may be addressed with a tibial tubercle osteotomy (TTO) to medialize and/or distalize the tubercle.


-
Elevated TT-TG distance (>20mm) contributing to significant lateral patellar overload and pain, particularly in the presence of patella alta. This may be addressed with a tibial tubercle osteotomy (TTO) to medialize and/or distalize the tubercle.
Contraindications
- Non-specific PFPS without identifiable surgical pathology: The most common contraindication. Surgery for generalized anterior knee pain without a clear mechanical driver is highly unlikely to be successful.
- Unrealistic Patient Expectations: Patients who expect immediate, complete resolution of pain without commitment to post-operative rehabilitation.
- Unaddressed Biomechanical Deficits: Failure to correct underlying hip weakness, core instability, or gait abnormalities through conservative means.
- Active Infection: Any local or systemic infection.
- Severe Osteoarthritis: While PFPS can lead to OA, advanced, widespread patellofemoral osteoarthritis may require different surgical considerations (e.g., patellofemoral arthroplasty) rather than procedures for PFPS.
- Poor Surgical Candidate: Significant comorbidities precluding safe anesthesia or recovery.
Table: Operative vs. Non-Operative Indications for Patellofemoral Pain Syndrome
| Feature / Indication | Non-Operative Management | Operative Management (Secondary to underlying pathology)
|
Description
|
Non-Operative (Initial)
|
Operative (After Failed Conservative Tx)
Please refer to the following guide for images:

- Use this for MRI or X-ray related to patellar tracking or TT-TG.

- Use for general knee anatomy (bony landmarks).

- Use for Q-angle measurement diagram.

- Use for tibial tubercle osteotomy overview.

- Use for femoral trochlea anatomy or patellar tracking view.

- Use for general intraoperative knee view or arthroscopy portal placement.

- Use for chondral lesion or arthroscopic debridement.

- Use for MPFL reconstruction graft harvest or femoral fixation.

- Use for MPFL reconstruction graft passage or patellar fixation.

- Use for surgical incision or surgical field.

- Use for a biomechanical diagram or force vectors.

- Use for patellar stabilization or tracking.

- Use for anatomical illustration (muscles/ligaments).

- Used in intro for general PFPS.

- Use for patellofemoral joint mechanics or imaging.

- Use for rehab exercise (quads strengthening).

- Use for post-op wound or dressing.

- Use for rehab exercise (hip/core strengthening).
Pre-Operative Planning & Patient Positioning
Meticulous pre-operative planning is essential for any patellofemoral intervention, especially given the diverse underlying pathologies that can contribute to PFPS. This planning integrates clinical assessment with advanced imaging to precisely identify and quantify correctable abnormalities.
Pre-Operative Assessment
- Clinical Evaluation: Re-confirm failure of conservative management (duration, specific interventions, compliance). Thoroughly assess patellofemoral tracking, stability (J-sign, apprehension test), patella alta/baja, Q-angle (static and dynamic), and any signs of malalignment. Evaluate hip and core strength.
-
Imaging Review:
- Radiographs: Weight-bearing AP, lateral (determining patellar height e.g., Insall-Salvati, Caton-Deschamps), and Merchant or Laurin views (patellar tilt, subluxation).
- MRI: Essential for assessing cartilage status (patellar and trochlear), MPFL integrity, trochlear morphology, synovial plica, and any other intra-articular pathology.
-
CT Scan (with specific protocol):
Crucial for accurate measurement of TT-TG distance, quantification of trochlear dysplasia, and femoral/tibial torsion, particularly in cases of recurrent instability or severe malalignment where a TTO is contemplated. Dynamic CT or MRI in varying degrees of flexion can further elucidate patellar tracking.


- Procedure Selection: Based on the identified pathology, determine the most appropriate surgical intervention (e.g., arthroscopic debridement, plica resection, lateral release, MPFL reconstruction, tibial tubercle osteotomy, cartilage restoration). Combinatorial procedures are common.
Patient Positioning
The standard position for most patellofemoral surgeries is supine on a radiolucent operating table.
- Lower Extremity Preparation: The affected limb is typically prepped and draped from the iliac crest to the foot, ensuring ample sterile field for potential graft harvest (e.g., hamstring tendons for MPFL reconstruction) and full range of knee motion.
- Tourniquet: A pneumatic thigh tourniquet is applied high on the thigh. Inflation is typically performed after exsanguination with an Esmarch bandage, set to a pressure appropriate for the patient's blood pressure.
- Foot Positioning: The foot is usually placed in a padded boot or positioned freely to allow for manipulation of the knee joint through its full range of motion during the procedure. A lateral post may be used to provide stability if needed.
- Anesthesia: General or regional anesthesia (spinal/epidural) is acceptable, often supplemented with local anesthetic infiltration for post-operative pain control.
Detailed Surgical Approach / Technique
Surgical intervention for PFPS is not a singular procedure but rather a spectrum of techniques addressing specific underlying pathologies. The following outlines common surgical approaches; the exact procedure chosen is dictated by the precise pre-operative diagnosis.
1. Arthroscopic Evaluation and Debridement / Plica Excision
This is often the initial step or a standalone procedure for specific intra-articular issues.
-
Portal Placement:
Standard anterolateral and anteromedial portals are created. Accessory portals may be required.

- Systematic Evaluation: A comprehensive arthroscopic survey of the entire knee joint is performed to assess menisci, cruciate ligaments, and articular cartilage of the tibiofemoral and patellofemoral compartments. Patellar tracking is observed dynamically through the range of motion.
-
Chondroplasty/Debridement:
If focal chondral fraying or delamination is observed on the patella or trochlea, debridement with a shaver or radiofrequency ablator may be performed to smooth unstable cartilage edges and remove symptomatic flaps. For full-thickness lesions, microfracture or other cartilage restoration techniques (e.g., OATS, ACI/MACI) may be performed depending on lesion size and location.

-
Plica Excision:
If a thickened, symptomatic medial plica (typically causing a "snapping" sensation or localized pain) is identified and impinges on the medial femoral condyle, it is carefully excised using a shaver or electrocautery, ensuring complete release of the restrictive band.

2. Lateral Retinacular Release (LRR)
Historically a common procedure, LRR is now performed with much greater circumspection due to concerns about iatrogenic instability and poor outcomes in isolated PFPS. It is indicated only for truly symptomatic, isolated lateral patellar compression and tilt where dynamic imaging confirms lateral retinacular tightness and significant medial facet unloading.
- Approach: Can be performed arthroscopically or open. Arthroscopically, portals allow for direct visualization of the lateral retinaculum.
- Technique: The lateral retinaculum is sharply divided, typically from the vastus lateralis insertion proximally to the patellar attachment distally, extending into the patellotibial ligament. Care is taken to avoid injury to the vastus lateralis and to preserve the superior lateral genicular artery. Release is performed until patellar tilt is corrected and the patella can be easily everted to 80-90 degrees.
- Caution: Over-release must be avoided as it can cause medial patellar subluxation or dislocation. It is generally contraindicated in patients with patellar instability or risk factors for instability.
3. Medial Patellofemoral Ligament (MPFL) Reconstruction
MPFL reconstruction is the most common procedure for recurrent patellar instability, and by stabilizing the patella, it can secondarily improve PFPS symptoms associated with maltracking or apprehension.
-
Graft Harvest:
Most commonly, an autograft semitendinosus or gracilis tendon is harvested via a small incision over the pes anserinus.

-
Femoral Attachment:
- A small incision is made over the medial femoral epicondyle, identifying Schöttle's point (the isometric point for MPFL attachment, located proximal and posterior to the adductor tubercle).
- A bone tunnel (or two convergent tunnels) is drilled from the medial femoral cortex into the femoral condyle, exiting at Schöttle's point.
- The graft is passed through the tunnel and secured with an interference screw, suture anchor, or cortical button, typically at 30-60 degrees of knee flexion to ensure isometric tension.
-
Patellar Attachment:
- A medial parapatellar incision is made. The MPFL insertion site is usually identified at the superomedial aspect of the patella.
- Either a single patellar tunnel, two convergent tunnels, or suture anchors are used to secure the graft to the patella. The goal is to recreate the broad patellar footprint of the native MPFL.
-
The graft is tensioned with the knee in 30 degrees of flexion to ensure appropriate patellar tracking and stability, avoiding over-tensioning which can cause stiffness or lateral patellar tilt.

-
Closure:
Layered closure of the incisions.


4. Tibial Tubercle Osteotomy (TTO)
TTO involves repositioning the tibial tubercle to correct excessive lateralization (medialization), patella alta (distalization), or both, thereby improving patellar tracking and reducing patellofemoral contact pressure. It is indicated for significant TT-TG distance and/or patella alta, especially in the setting of recurrent instability.
- Incision: A longitudinal incision is made over the anterior aspect of the proximal tibia, centered over the tibial tubercle.
-
Osteotomy:
- The periosteum is incised, and a rectangular or trapezoidal bone block containing the tibial tubercle is marked.
- Osteotomies are performed using an oscillating saw, typically leaving a posteromedial cortical hinge or completing the osteotomy.
- The bone block is carefully freed from the underlying soft tissues, preserving the vascular supply.
-
Repositioning:
- Medialization: The tubercle is translated medially to reduce the TT-TG distance (typically aiming for 9-12mm).
- Distalization: The tubercle is translated distally to correct patella alta.
- Anteriorization: Less common in isolated PFPS, but can be performed to offload patellar chondral lesions.
-
Fixation:
The repositioned bone block is secured to the tibia using two or three cortical lag screws or bicortical screws. Intraoperative fluoroscopy can confirm appropriate placement and patellar tracking.


- Closure: Layered closure, paying attention to the periosteum and subcutaneous tissues.
5. Trochleoplasty
Reserved for severe trochlear dysplasia (e.g., Dejour Type B or D) associated with recurrent patellar instability, trochleoplasty aims to deepen the femoral trochlear groove. This is a complex procedure with a steep learning curve.
- Technique: Involves reshaping the trochlea by either excising a wedge of bone beneath the trochlear cartilage and depressing the cartilage (deepening trochleoplasty) or by raising the lateral facet and deepening the central sulcus (recession trochleoplasty).
- Indications: Very specific and primarily for severe patellar instability where other procedures alone are deemed insufficient. Not a primary procedure for isolated PFPS.
It is crucial that the chosen surgical approach directly addresses the identified pathological biomechanical or anatomical abnormalities contributing to the patient's PFPS. A thorough understanding of the internervous planes (e.g., quadriceps muscle and patella are innervated by the femoral nerve, with the saphenous nerve and branches of the common peroneal nerve in the region) and careful soft tissue handling are essential to minimize iatrogenic damage.
Complications & Management
Despite advancements in surgical techniques, patellofemoral surgery is not without potential complications. A comprehensive understanding of these risks and their management is crucial for all orthopedic surgeons.
General Surgical Complications
-
Infection:
Superficial or deep wound infection. Incidence: 0.5-2%.
- Management: Superficial infections may respond to oral antibiotics and local wound care. Deep infections typically require surgical debridement, irrigation, hardware removal (if applicable), and prolonged intravenous antibiotics.
-
Thromboembolic Events (DVT/PE):
Incidence: <1% with appropriate prophylaxis.
- Management: Mechanical prophylaxis (SCDs), chemical prophylaxis (LMWH, aspirin) depending on patient risk factors and surgical procedure. Symptomatic events require anticoagulation.
-
Neurovascular Injury:
Damage to superficial nerves (e.g., infrapatellar branch of saphenous nerve causing numbness) or major vessels. Incidence: Rare.
- Management: Meticulous dissection. If nerve injury occurs, observation for recovery; surgical exploration and repair may be considered for complete transections. Vascular injury requires immediate repair.
-
Arthrofibrosis/Stiffness:
Post-operative loss of knee range of motion. Incidence: 5-15%, higher with extensive procedures or poor rehabilitation compliance.
- Management: Aggressive physical therapy, potentially manipulation under anesthesia (MUA), or arthroscopic lysis of adhesions.
Specific Patellofemoral Surgical Complications
-
Persistent Patellofemoral Pain:
The most common and frustrating complication, especially following isolated procedures like lateral release or even MPFL reconstruction if underlying issues are not fully addressed or the primary diagnosis was purely PFPS without instability. Incidence: Up to 30-50% for LRR, 10-20% for MPFL reconstruction.
- Salvage Strategy: Re-evaluation of the initial diagnosis and contributing factors. Advanced imaging (dynamic MRI/CT), diagnostic injections, revision surgery targeting residual malalignment, or addressing alternative pain generators (e.g., plica, saphenous nerve irritation).
-
Patellar Instability (Iatrogenic):
-
Medial Instability after LRR:
Over-release of the lateral retinaculum can lead to medial patellar subluxation or dislocation. Incidence: <5% but devastating.
- Salvage Strategy: MPFL reconstruction to stabilize the patella medially, possibly with a lateral tightening procedure.
-
Recurrence of Lateral Instability after MPFL Reconstruction/TTO:
Inadequate correction, graft failure, or underlying severe dysplasia not addressed. Incidence: 5-10%.
- Salvage Strategy: Revision MPFL reconstruction (if graft failure), TTO (if TT-TG was not addressed), or trochleoplasty (for severe dysplasia).
-
Medial Instability after LRR:
Over-release of the lateral retinaculum can lead to medial patellar subluxation or dislocation. Incidence: <5% but devastating.
-
Hardware-Related Complications:
-
Prominent Hardware:
Particularly with TTO screws or MPFL femoral buttons, causing skin irritation or bursitis. Incidence: 5-10%.
- Salvage Strategy: Symptomatic hardware removal after bone healing (typically >6 months post-op).
-
Screw Breakage/Migration:
Rare, but can occur, especially with TTO.
- Salvage Strategy: Surgical removal and potential refixation.
-
Prominent Hardware:
Particularly with TTO screws or MPFL femoral buttons, causing skin irritation or bursitis. Incidence: 5-10%.
-
Fracture:
-
Tibial Tubercle Fracture:
During TTO or post-operatively. Incidence: Rare.
- Salvage Strategy: Open reduction and internal fixation.
-
Patellar Fracture:
Very rare, could occur with patellar tunnel creation.
- Salvage Strategy: Tension band wiring or screw fixation.
-
Tibial Tubercle Fracture:
During TTO or post-operatively. Incidence: Rare.
-
Over-correction/Stiffness post-MPFL Reconstruction:
Over-tensioning the MPFL graft can lead to restricted flexion and increased patellofemoral compression. Incidence: 5-10%.
- Salvage Strategy: Aggressive physical therapy, potentially arthroscopic debridement, or even surgical revision of the MPFL with partial release or complete take-down and revision reconstruction.
-
Anterior Knee Numbness/Neuroma:
Injury to the infrapatellar branch of the saphenous nerve, particularly with medial incisions for MPFL reconstruction or graft harvest. Incidence: 10-20% sensory disturbance, <5% painful neuroma.
- Salvage Strategy: Observation; local anesthetic injections for neuromas; surgical excision of neuroma in refractory cases.
-
Non-union/Mal-union of Osteotomy:
With TTO, failure of the bone block to heal or healing in an incorrect position. Incidence: Rare with good fixation.
- Salvage Strategy: Revision osteotomy with bone grafting and improved fixation.
Table: Common Complications and Salvage Strategies in Patellofemoral Surgery
| Complication | Incidence (Approx.) | Primary Contributing Factor (Example) | Salvage Strategy |
|---|---|---|---|
| Persistent Patellofemoral Pain | 10-50% | Unaddressed underlying pathology, non-specific diagnosis | Re-evaluation, diagnostic injections, revision surgery for specific malalignment, address hip/core deficits, psychological support. |
| Medial Instability (after LRR) | <5% | Over-release of lateral retinaculum | MPFL reconstruction, possibly lateral tightening. |
| Recurrent Lateral Instability | 5-10% | Inadequate correction, graft failure, severe dysplasia | Revision MPFL, TTO, or trochleoplasty. |
| Arthrofibrosis/Stiffness | 5-15% | Over-tensioned MPFL, inadequate rehabilitation | Aggressive PT, MUA, arthroscopic lysis of adhesions. |
| Infection | 0.5-2% | Contamination | Debridement, irrigation, antibiotics, hardware removal. |
| Hardware Irritation/Prominence | 5-10% | Superficial placement, bulky hardware (TTO, MPFL) | Symptomatic hardware removal (after bone healing for osteotomy). |
| Tibial Tubercle Fracture (TTO) | <1% | Intraoperative error, early weight-bearing | ORIF of fracture. |
| Iatrogenic Nerve Injury | 1-20% (sensory) | Infrapatellar branch of saphenous nerve during medial approaches | Observation, local nerve blocks for painful neuromas, surgical excision of neuroma in refractory cases. |
| Over-correction/Over-tension (MPFL) | 5-10% | Inappropriate graft tensioning | Aggressive PT, partial MPFL release, revision MPFL reconstruction. |
| DVT/PE | <1% | Inadequate prophylaxis | Anticoagulation, mechanical prophylaxis. |
| Non-union (TTO) | <1% | Inadequate fixation, vascular compromise, smoking | Revision osteotomy with bone grafting and enhanced fixation. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as the surgical procedure itself for optimizing outcomes and minimizing complications. Protocols are tailored to the specific surgery performed, aiming to restore range of motion, strength, proprioception, and functional capacity while protecting the healing tissues.
General Principles
- Protection of Healing Structures: Respect graft healing (MPFL), osteotomy union (TTO), and cartilage repair.
- Early Motion: Initiate passive and active-assisted range of motion (ROM) as tolerated, typically within the first few days, to prevent stiffness and promote cartilage health.
- Progressive Weight-Bearing (WB): Gradually advance WB status based on procedure and surgeon preference.
- Strength Training: Focus on quadriceps, hip abductors/external rotators, and core musculature.
- Neuromuscular Control: Emphasize proprioception and balance training.
- Gradual Return to Activity: Step-wise progression to sports-specific activities.
Specific Rehabilitation Protocols
1. Arthroscopic Debridement / Plica Excision
-
Phase I (Weeks 0-2): Pain & Swelling Control, Early Motion
- WBAT immediately.
- Cryotherapy, compression, elevation.
- ROM: Passive and active-assisted knee flexion/extension to tolerance.
- Exercises: Quadriceps sets, straight leg raises (SLR) in all planes (without resistance if pain), ankle pumps.
-
Phase II (Weeks 2-6): Restore Full ROM, Basic Strength
- Progress to full ROM.
- Strengthening: Stationary bike (low resistance), hip abduction/adduction, gluteal strengthening, progressive quadriceps strengthening (e.g., knee extensions 90-45 degrees, step-ups).
- Proprioception: Single-leg balance.
-
Phase III (Weeks 6+): Advanced Strengthening, Return to Activity
- Plyometrics, agility drills, sport-specific training as appropriate.
- Gradual return to running based on symptom resolution and strength criteria.
2. Lateral Retinacular Release (LRR)
- Similar to arthroscopic debridement protocols, but with a strong emphasis on immediate and aggressive medial patellar glide mobilization and VMO strengthening to counteract the potential for medial instability.
- Avoid exercises that exacerbate lateral patellar tilt.
3. MPFL Reconstruction
-
Phase I (Weeks 0-6): Protection, Early Motion, Non-Weight Bearing/Partial Weight Bearing
- Bracing: Hinged knee brace locked in extension for ambulation initially (or 0-30 degrees flexion for sitting), weaning as quadriceps control improves.
- WB: NWB or PWB (25%) with crutches for 2-4 weeks, then progressive to WBAT based on surgeon preference and pain.
- ROM: Passive flexion limited to 0-60 degrees for initial 2-3 weeks to protect healing graft, gradually increasing to 90 degrees by week 6. Full extension encouraged.
- Exercises: Quadriceps sets, patellar mobilizations (medial glide), SLR in brace, ankle pumps.
- Avoid resisted knee extension (open kinetic chain) in terminal range (0-30 degrees) for up to 12 weeks to protect graft.
-
Phase II (Weeks 6-12): Restore Full ROM, Intermediate Strength
- Wean from brace/crutches as strength and control allow.
- ROM: Progress to full flexion (120-130 degrees).
- Strengthening: Stationary bike (low resistance), closed kinetic chain exercises (mini-squats, leg press 0-60 degrees), hip strengthening.
- Proprioception: Balance board, single-leg stance.
-
Phase III (Weeks 12-24): Advanced Strengthening, Functional Training
- Progressive resistive exercises (closed kinetic chain squats, lunges), open kinetic chain knee extension (gradual resistance).
- Agility drills, plyometrics (box jumps, hopping), sport-specific drills.
- Initiate return to running program (gradual walk-to-run).
-
Phase IV (Months 6-12): Return to Sport
- Criteria-based return: Full pain-free ROM, symmetrical strength (isokinetic testing >90% contralateral limb), successful completion of sport-specific drills.
-
Continued strength and conditioning maintenance.


4. Tibial Tubercle Osteotomy (TTO)
-
Phase I (Weeks 0-6): Protection, Limited Weight Bearing, Controlled Motion
- Bracing: Hinged knee brace locked in extension or restricted ROM for 4-6 weeks to protect osteotomy.
- WB: NWB or PWB (25%) with crutches for 4-6 weeks until early signs of osteotomy healing are evident on radiographs.
- ROM: Passive and active-assisted ROM as tolerated, often limited to 0-90 degrees for initial weeks. Avoid excessive hamstring tension which can displace the osteotomy.
- Exercises: Quadriceps sets, gentle patellar mobilizations, SLR (in brace), ankle pumps, core stability.
-
Phase II (Weeks 6-12): Progressive Weight Bearing, Restore ROM & Strength
- Gradual progression to full WBAT as osteotomy healing progresses.
- ROM: Progress to full ROM.
- Strengthening: Closed kinetic chain exercises (mini-squats, leg press), hip abductors/external rotators. Avoid direct resistance to quadriceps if a significant anteriorization was performed.
-
Phase III (Weeks 12-24): Advanced Strengthening, Functional Training
- Progressive resistive exercises.
- Initiate low-impact activities like cycling, elliptical.
- Gradual return to impact activities and running based on osteotomy union and pain.
-
Phase IV (Months 6-12+): Return to Sport
- Criteria-based return: Full osteotomy union, pain-free ROM, symmetrical strength, successful completion of sport-specific drills.
- Hardware removal may be considered after 12-18 months if symptomatic.
Rehabilitation should be closely supervised by a physical therapist with expertise in patellofemoral disorders, with ongoing communication between the surgeon and therapist to adjust the protocol based on individual patient progress and potential setbacks.

Summary of Key Literature / Guidelines
The understanding and management of patellofemoral pain syndrome (PFPS) have evolved significantly over recent decades, with current guidelines emphasizing a conservative, evidence-based approach as the primary treatment modality. Surgical intervention, while an option for specific indications, is consistently presented as a secondary consideration.
Key Findings from Literature
-
Conservative Management Efficacy: Numerous systematic reviews and meta-analyses consistently demonstrate the efficacy of multimodal physical therapy for PFPS. Components shown to be most effective include:
- Hip and Core Strengthening: Strong evidence supports targeting hip abductor and external rotator weakness, as well as core stability, to improve lower extremity kinematics and reduce patellofemoral loading (e.g., Crossley et al., 2011; Ferber et al., 2010).
- Quadriceps Strengthening: Strengthening the quadriceps, particularly the vastus medialis obliquus (VMO), is fundamental, but open-kinetic chain exercises in early flexion may increase patellofemoral stress, favoring closed-kinetic chain exercises initially (e.g., Powers et al., 2004).
- Patellar Taping/Bracing: Patellar taping (McConnell technique) or certain braces can provide immediate pain relief and facilitate participation in exercise, but are not standalone treatments (e.g., Warden et al., 2005).
- Foot Orthoses: Custom or off-the-shelf foot orthoses may be beneficial for individuals with excessive foot pronation (e.g., Mills et al., 2012).
- Education and Activity Modification: Patient education regarding pain management, activity modification, and gradual return to activity is crucial.
- Lack of Evidence for Passive Modalities: Limited evidence supports the long-term efficacy of passive modalities such as ultrasound, electrical stimulation, or massage as standalone treatments.
-
Role of Surgery for PFPS:
- General Consensus: Surgery for isolated PFPS, without objective evidence of patellar instability or significant structural pathology (e.g., severe chondral defect, symptomatic plica), has a poor prognosis and is largely discouraged.
- Lateral Retinacular Release (LRR): Studies have demonstrated that isolated LRR for PFPS often yields unsatisfactory results and carries a risk of iatrogenic medial instability. Its use is now highly restricted to specific cases of demonstrable lateral patellar hyperpressure and tilt refractory to conservative measures (e.g., Fulkerson, 2002).
- MPFL Reconstruction and Tibial Tubercle Osteotomy (TTO): These procedures are primarily indicated for recurrent patellar instability with associated predisposing factors (e.g., high TT-TG, patella alta, trochlear dysplasia). When instability is corrected, concomitant PFPS symptoms often resolve. The outcomes for these procedures in selected patients with instability are generally good to excellent (e.g., Dejour et al., 1994; Schöttle et al., 2010).
- Cartilage Restoration: For focal chondral lesions identified as a pain generator, procedures like microfracture, OATS, or ACI/MACI may be considered, but long-term outcomes for patellofemoral chondral lesions remain variable and depend on lesion size, depth, and patient factors (e.g., Mithoefer et al., 2009).
- Plica Excision: Effective for true symptomatic plica syndrome identified as the primary pain source after conservative failure (e.g., Dupuy et al., 2017).
Professional Guidelines
Several professional organizations have published guidelines regarding PFPS management:
-
International Patellofemoral Pain Research Retreat (PFP Summit): A consensus statement (Barton et al., 2015; Willy et al., 2019) highlights that:
- Exercise therapy is the primary treatment for PFPS.
- Foot orthoses and patellar taping can be useful adjuncts.
- Combined interventions are often more effective.
- Strength training should target both knee and hip musculature.
- Surgery should be reserved for cases with clear structural abnormalities (e.g., patellar instability, significant cartilage lesions, symptomatic plica) refractory to comprehensive non-operative management.
- PFP is often a chronic condition requiring long-term self-management strategies.
-
Clinical Practice Guidelines (e.g., Journal of Orthopaedic & Sports Physical Therapy - JOSPT): These guidelines typically recommend a phased approach:
- Phase 1: Patient education, activity modification, pain management.
- Phase 2: Neuromuscular re-education and strengthening (hip abductors/external rotators, quadriceps).
- Phase 3: Integration into functional and sport-specific movements.
- Surgical Referral: Considered only after failure of 6-12 months of appropriate conservative care and identification of a surgically amenable structural abnormality.
In conclusion, the prevailing evidence strongly supports a judicious, conservative approach to PFPS management. Surgical intervention for this condition is rarely a primary treatment and must be carefully considered only when specific, identifiable, and surgically correctable pathologies are present and have failed exhaustive non-operative regimens. The success of any intervention, whether conservative or surgical, hinges upon a precise diagnosis, meticulous technique, and diligent post-operative rehabilitation.
You Might Also Like