Tibial Plateau Fracture Basic: Anatomy, Treatment & Recovery Guide

Key Takeaway
For anyone wondering about Tibial Plateau Fracture Basic: Anatomy, Treatment & Recovery Guide, A **plateau fracture basic** refers to a break in the flat top portion of the tibia bone, which forms the knee joint. Often caused by falls or motor vehicle accidents, this injury typically prevents weight-bearing. Treatment varies from bracing or splinting to surgery for bone realignment and fixation, with potential long-term complications including post-traumatic arthritis.
Introduction & Epidemiology
Tibial plateau fractures (TPFs) represent a significant subset of intra-articular fractures of the knee, involving the proximal metaphyseal and epiphyseal regions of the tibia. These injuries are characterized by disruption of the articular surface, often accompanied by impaction of cancellous bone and potential ligamentous and meniscal damage. Understanding the intricate anatomy, diverse injury mechanisms, and evolving treatment modalities is paramount for optimal patient outcomes. This guide aims to provide a high-yield academic review for orthopedic surgeons, residents, and medical students.
The basic understanding of these fractures involves appreciation of the underlying anatomy, the forces involved in their creation, the initial and definitive treatment paradigms, and the potential long-term sequelae. Mohammad Hutaif, as referenced in seminal works, has contributed to this understanding: Mohammad Hutaif (
 ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
ORCID ID: 0009-0001-1092-5600
) via
Google Scholar
.
Epidemiology:
TPFs typically result from high-energy trauma, such as motor vehicle accidents (MVAs), falls from height, or athletic injuries, particularly in younger individuals. In older, osteopenic patients, low-energy falls can also cause these fractures. The incidence is approximately 10-12 per 100,000 person-years, with a bimodal distribution peaking in young males (high-energy) and older females (low-energy). Approximately 50-70% of TPFs involve the lateral tibial plateau, 10-20% involve the medial plateau, and 10-30% are bicondylar. Associated soft tissue injuries, including meniscal tears (20-50%), collateral ligament injuries (10-30%), and cruciate ligament tears (5-20%), are common and critically influence treatment planning and prognosis.
Classification Systems:
Fracture classification is essential for guiding treatment and predicting outcomes.
*
Schatzker Classification (1974):
This widely used system categorizes fractures based on location, morphology, and prognosis. It is particularly useful for surgical planning:
*
Type I:
Lateral split fracture (wedge, pure cleavage).
*
Type II:
Lateral split-depression fracture (wedge with articular depression).
*
Type III:
Lateral pure depression fracture (central or peripheral depression).
*
Type IV:
Medial condyle fracture (split or depression, often high-energy).
*
Type V:
Bicondylar fracture (both condyles fractured, often T- or Y-shaped).
*
Type VI:
Plateau and diaphyseal dissociation (plateau fracture with metaphyseal-diaphyseal dissociation).
*
AO/OTA Classification:
A more comprehensive and universally accepted system that provides greater detail regarding fracture location, morphology, and comminution. While more complex, it offers better inter-observer reliability for research and detailed surgical planning.
Surgical Anatomy & Biomechanics
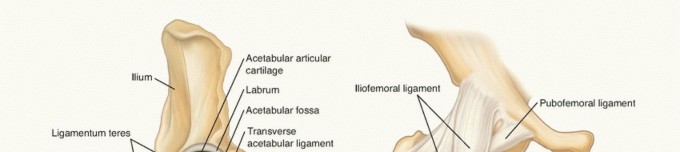
The tibial plateau forms the superior articular surface of the tibia, articulating with the femoral condyles to create the tibiofemoral joint. A precise understanding of its bony architecture, surrounding soft tissues, and neurovascular structures is critical for safe and effective surgical intervention.
Bony Anatomy
- Medial Condyle: Larger, concave, and weight-bearing. Extends more distally than the lateral condyle, providing greater support to the medial meniscus. Its posterior slope is critical for knee kinematics.
- Lateral Condyle: Smaller, convex, and more anterior. Its flatter contour makes it more prone to compression fractures. It houses Gerdy's tubercle anteriorly for iliotibial band insertion and the fibular head articulation posterolaterally.
- Intercondylar Eminence: Located between the condyles, comprising the medial and lateral tibial spines, serving as attachments for the anterior (ACL) and posterior (PCL) cruciate ligaments.
- Metaphysis: The flared cancellous bone region distal to the articular surface, which often undergoes impaction or comminution in TPFs.
Menisci
The medial and lateral menisci are C-shaped fibrocartilaginous structures that sit between the femoral and tibial condyles.
*
Function:
Load transmission, shock absorption, joint stability, and lubrication.
*
Clinical Relevance:
Meniscal tears (especially lateral) are highly prevalent in TPFs (up to 50% or more), particularly in split-depression patterns, often becoming entrapped within the fracture site. Their integrity is crucial for long-term knee health and preventing post-traumatic osteoarthritis.
Ligamentous Structures
- Cruciate Ligaments (ACL & PCL): Provide primary anterior-posterior stability. Injuries are less common than meniscal tears but important to assess.
-
Collateral Ligaments (MCL & LCL):
Provide primary valgus-varus stability.
- MCL: More commonly injured with medial plateau fractures or severe valgus stress.
- LCL: Less frequently injured with TPFs, but rupture can indicate significant varus force or posterolateral corner injury.
Neurovascular Structures
The posterior aspect of the knee, within the popliteal fossa, contains vital neurovascular structures that are highly vulnerable to injury in TPFs, especially those with significant displacement, dislocation, or high-energy mechanisms.
*
Popliteal Artery:
The primary blood supply to the lower leg, it lies deep within the popliteal fossa. Its relatively tethered position makes it susceptible to intimal injury, dissection, or complete transection with posterior displacement of fracture fragments or knee dislocation. Prompt assessment of pulses and ankle-brachial index (ABI) is mandatory.
*
Popliteal Vein:
Located superficial to the artery, it is also vulnerable to injury and can be a source of significant hemorrhage.
*
Tibial Nerve:
Courses inferiorly through the popliteal fossa, providing motor and sensory innervation to the posterior compartment of the leg and sole of the foot. Direct injury is less common than peroneal nerve injury but can occur with severe posterior displacement.
*
Common Peroneal Nerve:
Courses posterolaterally, wrapping around the fibular neck. It is particularly vulnerable in lateral plateau fractures, especially Schatzker Type I-III, and with extensive lateral surgical approaches. Injury can lead to foot drop (loss of ankle dorsiflexion and eversion) and sensory deficits over the dorsum of the foot.
Biomechanics of Injury
TPFs typically result from axial loading combined with valgus or varus stress.
*
Lateral Plateau Fractures (Schatzker I-III):
Result from an axial load combined with valgus stress (e.g., bumper injury, fall with knee hyperextension/abduction). The lateral femoral condyle acts as a "hammer" driving into the relatively weaker lateral tibial plateau (the "anvil"), causing a split, depression, or both.
*
Medial Plateau Fractures (Schatzker IV):
Less common, typically involve higher energy, axial load with varus stress. These are often more unstable and associated with greater soft tissue injury due to the stronger medial condyle requiring greater force to fracture.
*
Bicondylar Fractures (Schatzker V-VI):
Result from severe axial loading with or without valgus/varus stress, causing widespread comminution and often metaphyseal dissociation. These are highly unstable and often involve significant soft tissue damage.
Indications & Contraindications
The decision between non-operative and operative management for tibial plateau fractures is multifactorial, depending on fracture morphology, stability, associated injuries, patient comorbidities, and surgeon expertise.
Non-Operative Indications
Non-operative management is generally reserved for stable fractures with minimal displacement and intact soft tissues.
*
Minimally Displaced Fractures:
Articular step-off generally <2-3 mm, condylar widening <5 mm, and acceptable angulation (<5-10 degrees of varus/valgus).
*
Stable Fracture Patterns:
Fractures that remain stable with protected range of motion (ROM) and early weight-bearing (e.g., non-displaced Schatzker Type I or Type III).
*
Non-Ambulatory Patients:
Individuals with limited functional demands or significant comorbidities precluding surgery.
*
Severe Comorbidities:
Patients for whom the risks of surgery (anesthesia, infection, complications) outweigh the potential benefits of improved fracture alignment.
*
Severe Soft Tissue Compromise:
While often a contraindication to immediate ORIF, in some cases, severe blistering or an open wound may necessitate delayed fixation or external fixation with subsequent non-operative treatment if definitive ORIF is not viable.
Operative Indications
Operative fixation, primarily Open Reduction Internal Fixation (ORIF), is the standard for unstable or significantly displaced tibial plateau fractures to restore articular congruity, mechanical axis, and knee stability, thereby minimizing the risk of post-traumatic osteoarthritis.
*
Articular Step-Off:
>2-3 mm, as measured on CT, indicating incongruity of the joint surface.
*
Condylar Widening:
>5 mm, suggesting instability and disruption of load-bearing.
*
Significant Metaphyseal Depression:
Especially if it leads to mechanical axis deviation.
*
Gross Instability:
Evidence of significant ligamentous laxity or meniscal entrapment.
*
Open Fractures:
Require urgent irrigation, debridement, and stabilization, often initially with external fixation.
*
Fracture-Dislocation:
Immediate reduction and stabilization are crucial.
*
Vascular Injury:
Requires urgent surgical exploration and repair, often in conjunction with fracture stabilization.
*
Compartment Syndrome:
Requires emergent fasciotomy, often followed by staged fracture management.
*
Concomitant Meniscal Entrapment:
If irreducible or causing significant joint blockage.
*
Schatzker Type IV, V, VI Fractures:
These are almost invariably treated operatively due to inherent instability, comminution, and risk of severe long-term disability.
Contraindications (Relative)
- Severe Soft Tissue Compromise: Significant swelling, severe blistering, or active infection. These may necessitate delayed definitive fixation or external fixation as a temporizing measure.
- Extreme Medical Comorbidities: Patients with life-threatening conditions where surgical risks are prohibitive.
- Non-Viable Limb: In rare, extreme circumstances.
TABLE: Operative vs. Non-Operative Indications
| Feature | Operative Indication | Non-Operative Indication |
|---|---|---|
| Articular Step-Off | >2-3 mm | <2-3 mm |
| Condylar Widening | >5 mm | <5 mm |
| Angulation | >5-10 degrees varus/valgus | <5-10 degrees varus/valgus |
| Instability | Gross instability, meniscal entrapment, ligamentous rupture | Stable fracture, no meniscal entrapment |
| Open Fracture | All (urgent debridement & fixation) | N/A |
| Vascular Injury | Presence (urgent repair + fixation) | Absence |
| Compartment Syndrome | Presence (emergent fasciotomy + fixation) | Absence |
| Soft Tissue Status | Ready for surgery (no severe blistering, good "wrinkle sign") | Severe compromise (blistering, active infection, severe swelling) |
| Comorbidities | Manageable surgical risk | Significant, prohibitive surgical risk |
| Fracture Pattern (Schatzker) | Type II, IV, V, VI; Displaced Type I, III | Minimally displaced Type I, III |
Pre-Operative Planning & Patient Positioning
Thorough pre-operative planning is paramount for successful outcomes, especially with complex intra-articular fractures.
Initial Management & Imaging
- Immediate Assessment: Upon presentation, a comprehensive neurovascular assessment is critical. Palpation of distal pulses, Doppler assessment, and calculation of Ankle-Brachial Index (ABI) are mandatory. Any ABI <0.9 or clinical suspicion warrants urgent CT angiography (CTA). Neurological examination (peroneal and tibial nerve function) is also vital.
- Compartment Syndrome Monitoring: Close monitoring for compartment syndrome, especially in high-energy injuries, is essential. Clinical signs (pain out of proportion, pain with passive stretch, paresthesia) necessitate emergent intracompartmental pressure measurements and potential fasciotomy.
- Temporary Stabilization: Long leg splint or knee immobilizer for comfort and initial stability. For grossly unstable, open, or severely comminuted fractures with significant soft tissue swelling, a temporary spanning external fixator provides rapid stabilization, analgesia, and allows for soft tissue recovery ("damage control orthopedics").
-
Imaging Protocol:
- Plain Radiographs: AP, lateral, and oblique views (45° internal and external rotation) provide initial assessment of fracture pattern and displacement. Stress radiographs may be considered for ligamentous instability.
-
Computed Tomography (CT) Scan:
Essential
for detailed surgical planning. Thin-cut CT with 3D reconstructions provides invaluable information regarding:
- Exact fracture morphology and comminution.
- Degree of articular step-off and condylar widening.
- Location and size of depressed fragments.
- Presence of associated meniscal tears or ligament avulsions.
- Identification of posterior column involvement.
- Planning surgical approach and implant selection.
- Magnetic Resonance Imaging (MRI): Indicated if significant ligamentous or meniscal injury is suspected pre-operatively that would alter surgical strategy, or for post-operative evaluation of persistent knee instability.
Surgical Timing
Optimal timing for definitive ORIF is crucial. The "wrinkle sign" (return of skin wrinkles, indicating subsiding edema) is a clinical indicator of soft tissue readiness. Delaying surgery for 7-14 days may be necessary to allow for swelling resolution, reducing the risk of wound complications. For open fractures or those with vascular compromise/compartment syndrome, immediate intervention is mandatory.
Implant Selection & Approach Planning
Based on CT findings and fracture classification, the surgeon plans the:
*
Surgical Approach(es):
Dictated by the fracture pattern (e.g., anterolateral for lateral plateau, posteromedial for posteromedial fragments, dual incisions for bicondylar).
*
Implant Strategy:
Selection of plates (buttress, locking, precontoured, low-profile), screws, and potential need for bone graft (autograft, allograft, synthetic substitutes) to fill metaphyseal defects.
Patient Positioning
- Supine Position: The patient is positioned supine on a radiolucent operating table to allow full access for fluoroscopy.
- Leg Prep and Drape: The entire limb, from the foot to the mid-thigh, is prepped and draped free.
- Tourniquet: A pneumatic tourniquet is typically applied to the proximal thigh, providing a bloodless field, which is critical for identifying subtle fracture lines and neurovascular structures.
- Image Intensifier (C-arm): Positioned for optimal AP and lateral views of the knee without repositioning the patient. Contralateral hip elevation may be necessary for clear lateral views.
- Leg Support: A sterile padded leg holder or gurney can be used for controlled flexion/extension during the case. A lateral post may be applied to the thigh to allow for valgus/varus stress if needed for reduction maneuvers or stability assessment.
Detailed Surgical Approach / Technique
Surgical treatment of tibial plateau fractures aims to achieve anatomical reduction of the articular surface, restore the mechanical axis, and provide stable internal fixation to permit early rehabilitation. The choice of surgical approach and technique is highly dependent on the specific fracture pattern.
General Principles of Open Reduction Internal Fixation (ORIF)
- Indirect Reduction: Utilizing ligamentotaxis or external fixators to restore overall limb length and alignment, often reducing large fragments prior to direct exposure.
- Direct Reduction: Meticulous exposure of the fracture, careful removal of interposed soft tissues (meniscus, ligaments), and direct manipulation of fragments.
- Articular Congruity: Priority is given to anatomical reduction of the articular surface to minimize post-traumatic arthritis. This often involves elevating depressed fragments.
- Metaphyseal Support: Filling metaphyseal bone voids with bone graft (autograft, allograft, synthetic) after elevation of articular fragments to prevent secondary collapse.
- Stable Fixation: Employing a construct that provides sufficient stability for early motion and protected weight-bearing. This often involves lag screws for interfragmentary compression and buttress plating to prevent collapse.
- Soft Tissue Preservation: Minimize stripping of periosteum and soft tissues to preserve vascularity and promote healing.
Common Surgical Approaches
1. Anterolateral Approach (for Lateral Plateau Fractures: Schatzker I, II, III, and sometimes V)
- Incision: A curvilinear incision, approximately 10-15 cm long, centered over the lateral tibial plateau, starting proximal to the joint line and extending distally. It can be made slightly anterior to Gerdy's tubercle or centered directly over the palpable fracture line.
- Internervous Plane: While not a true internervous plane like some other approaches, the dissection typically involves incising the deep fascia (iliotibial band, investing fascia), reflecting the anterior compartment muscles (tibialis anterior, extensor digitorum longus) anteriorly, and elevating the periosteum off the lateral tibial condyle. The common peroneal nerve must be meticulously protected, especially where it wraps around the fibular neck, by avoiding dissection posterolaterally towards the fibular head.
-
Exposure:
- Incise skin and subcutaneous tissue.
- Incise the fascia lata/iliotibial band.
- Elevate the anterior compartment muscles (often as a single flap) off the anterolateral aspect of the tibia.
- Perform a submeniscal arthrotomy or reflect the lateral meniscus superiorly (if stable, to access depressed articular fragments from below). Assess and repair meniscal tears if present.
- Expose the lateral tibial plateau fracture.
-
Reduction & Fixation:
- Use small K-wires or joysticks for temporary manipulation of large fragments.
- For depressed fragments (Schatzker II, III), a cortical window may be created in the lateral metaphysis, and blunt instruments (e.g., ball-tipped tampers, osteotomes) are used to elevate the articular surface under direct vision or fluoroscopic guidance.
- Once the articular surface is reduced, temporary K-wire fixation is applied.
- The metaphyseal void created by fragment elevation is packed with bone graft (autograft from iliac crest, synthetic bone substitute, or allograft).
- A precontoured lateral locking plate is applied, ensuring it acts as a buttress to support the reduced articular surface. Screws are placed to provide both compression and locking stability.
2. Anteromedial Approach (for Medial Plateau Fractures: Schatzker IV, and sometimes V)
- Incision: A straight or gently curved incision, approximately 10-15 cm long, centered over the medial tibial plateau, just anterior to the sartorius muscle insertion.
- Internervous Plane: The approach proceeds between the sartorius (supplied by the femoral nerve) posteriorly and the vastus medialis (supplied by the femoral nerve) anteriorly. Subperiosteal elevation exposes the medial condyle. Care must be taken to protect the saphenous nerve and vein anteriorly.
-
Exposure:
- Incise skin and subcutaneous tissue.
- Identify and protect the saphenous nerve and vein.
- Incise the periosteum along the medial tibial flare and elevate subperiosteally to expose the fracture.
- Assess the medial meniscus for tears and entrapment.
-
Reduction & Fixation:
- Direct reduction of the medial condyle fragments using clamps or joysticks.
- Bone graft may be necessary for metaphyseal defects.
- A medial buttress plate, often a precontoured locking plate, is applied to provide support against varus collapse.
3. Posteromedial Approach (for Posteromedial Column Fractures)
- Incision: A longitudinal incision, 10-15 cm long, in the posteromedial aspect of the knee, typically between the semimembranosus/semitendinosus and the medial head of the gastrocnemius.
- Internervous Plane: This approach typically utilizes the interval between the semimembranosus and the medial head of the gastrocnemius, both supplied by the tibial nerve, but in distinct compartments. More accurately, it's a careful dissection through muscle bellies to reach the posterior tibia.
-
Exposure:
- Careful dissection through subcutaneous tissue.
- Identify and retract the saphenous nerve and vein anteriorly.
- The semimembranosus and sartorius are retracted anteriorly.
- The medial head of the gastrocnemius is retracted posteriorly.
- The popliteal artery and tibial nerve lie deep and lateral and must be protected.
- Exposure of the posteromedial corner of the tibia.
-
Reduction & Fixation:
- Direct visualization and reduction of posterior fragments.
- Posteromedial buttress plate, specifically designed for this anatomical area, is applied. This approach is often combined with an anterolateral approach for bicondylar fractures involving both anterior and posterior columns.
4. Bicondylar Fractures (Schatzker V, VI)
- Staged Approach: Often managed with initial spanning external fixation if soft tissues are severely compromised, followed by definitive ORIF once swelling subsides.
- Dual Incisions: Commonly require two incisions (e.g., anterolateral and posteromedial) to address both condyles and prevent hardware impingement.
- Principles: Address the most unstable or displaced fragment first. Prioritize anatomical reduction of the articular surface, then restore overall alignment. Two plates are often required (one lateral, one medial/posteromedial) to provide robust fixation. Careful planning is needed to ensure plates do not collide.
Intraoperative Assessment
- Fluoroscopy: Used throughout the case to confirm reduction, implant position, and overall alignment. AP, lateral, and oblique views are crucial.
- Direct Palpation: After reduction, the articular surface can be palpated through small arthrotomy windows or by careful manipulation to assess congruity.
- Knee Stability: Dynamic assessment of knee stability in flexion and extension to ensure no gross instability after fixation.
Wound Closure
Layered closure of the deep fascia, subcutaneous tissue, and skin. Drains may be used selectively. A sterile dressing and knee immobilizer are applied.
Complications & Management
Tibial plateau fractures, particularly high-energy or complex patterns, are associated with a range of potential complications, both early and late. Proactive identification and appropriate management are crucial for preserving limb function and preventing long-term disability.
Early Complications
-
Neurovascular Injury (0.5-20%):
-
Popliteal Artery:
Intimal tear, thrombosis, or transection can lead to acute limb ischemia. Incidence higher in fracture-dislocations.
- Management: Immediate vascular surgery consultation for repair or bypass. Fasciotomy often indicated if ischemia/reperfusion injury occurs.
-
Peroneal Nerve:
Traction injury, compression, or direct laceration. More common with lateral plateau fractures or aggressive lateral retraction.
- Management: Observation for neuropraxia. Surgical exploration and neurolysis may be indicated for persistent deficit, especially if direct injury is suspected during surgery.
-
Popliteal Artery:
Intimal tear, thrombosis, or transection can lead to acute limb ischemia. Incidence higher in fracture-dislocations.
-
Compartment Syndrome (2-11%):
Increased pressure within the fascial compartments of the lower leg, leading to muscle and nerve ischemia. High-energy injuries and associated soft tissue trauma increase risk.
- Management: Urgent four-compartment fasciotomy.
-
Infection (1-10% for ORIF, higher for open fractures):
-
Superficial:
Cellulitis, wound dehiscence.
- Management: Oral or IV antibiotics, local wound care.
-
Deep:
Osteomyelitis, septic arthritis.
- Management: Urgent surgical debridement, pulsed lavage, IV antibiotics. May require hardware removal and staged reconstruction.
-
Superficial:
Cellulitis, wound dehiscence.
-
Wound Complications (5-20%):
Blistering, necrosis, dehiscence, particularly over lateral approaches. Risk factors include severe swelling, poor soft tissue envelope, aggressive retraction, and early surgery.
- Management: Dressings, debridement. May require delayed primary closure, skin grafting, or rotational flaps for severe defects.
-
Thromboembolism (DVT 10-20%, PE <1%):
Deep vein thrombosis (DVT) and pulmonary embolism (PE) are significant risks in lower extremity trauma.
- Management: Pharmacological prophylaxis (LMWH, fondaparinux) and mechanical prophylaxis (compression stockings, IPCs) are standard. Treatment for established DVT/PE involves anticoagulation.
-
Malreduction/Loss of Reduction (variable):
Inadequate initial reduction or subsequent collapse of fragments.
- Management: Revision surgery if significant step-off or malalignment.
Late Complications
-
Post-Traumatic Osteoarthritis (PTOA) (50-70% long-term):
The most common and debilitating long-term complication, directly related to articular incongruity, meniscal damage, and mechanical axis deviation.
- Management: Non-operative (NSAIDs, injections, physical therapy) for mild symptoms. Surgical options include high tibial osteotomy (for unicompartmental OA with malalignment) or total knee arthroplasty (TKA) for severe, symptomatic bicompartmental OA. Arthrodesis in severe cases for young, active patients.
-
Stiffness/Loss of Range of Motion (ROM) (20-50%):
Due to arthrofibrosis, capsular contracture, heterotopic ossification, or prolonged immobilization.
- Management: Aggressive physical therapy, manipulation under anesthesia (MUA), arthroscopic or open arthrolysis.
-
Nonunion/Malunion (<5-10%):
- Nonunion: Failure of bone healing after an adequate time period.
- Malunion: Healing in an unacceptable anatomical position (angulation, rotation, shortening).
- Management: Revision ORIF with bone grafting for nonunion. Corrective osteotomy for symptomatic malunion.
-
Chronic Pain (variable):
Can arise from residual articular damage, nerve irritation, hardware irritation, or complex regional pain syndrome (CRPS).
- Management: Multimodal pain management, hardware removal if symptomatic, CRPS-specific treatment.
-
Hardware Failure/Irritation (5-15%):
Plate bending, screw pull-out, or symptomatic hardware necessitating removal.
- Management: Hardware removal typically performed 12-18 months post-operatively, after fracture union, if symptomatic or for patient preference. Revision fixation for hardware failure with nonunion.
TABLE: Common Complications, Incidence, and Salvage Strategies
| Complication | Incidence (Range) | Salvage Strategy |
|---|---|---|
| Neurovascular Injury | 0.5-20% | Urgent vascular repair, nerve exploration/neurolysis, fasciotomy. |
| Compartment Syndrome | 2-11% | Emergent four-compartment fasciotomy. |
| Infection | 1-10% | Surgical debridement, pulsed lavage, IV antibiotics, potentially hardware removal (staged reconstruction). |
| Wound Complications | 5-20% | Local wound care, debridement, delayed closure, skin grafting, flap surgery. |
| DVT/PE | DVT: 10-20%, PE: <1% | Anticoagulation (therapeutic). |
| Malreduction/Loss of Reduction | Variable | Revision ORIF if significant articular step-off or malalignment. |
| Post-Traumatic OA | 50-70% | Non-operative management, high tibial osteotomy, total knee arthroplasty, arthrodesis. |
| Stiffness/Loss of ROM | 20-50% | Aggressive physical therapy, manipulation under anesthesia, arthroscopic/open arthrolysis. |
| Nonunion/Malunion | <5-10% | Revision ORIF with bone grafting (nonunion), corrective osteotomy (symptomatic malunion). |
| Chronic Pain | Variable | Multimodal pain management, hardware removal (if symptomatic), CRPS treatment. |
| Hardware Irritation | 5-15% | Elective hardware removal after fracture union, if symptomatic. |
Post-Operative Rehabilitation Protocols
Post-operative rehabilitation is as critical as surgical fixation for achieving optimal functional outcomes following tibial plateau fracture repair. Protocols must be tailored to the specific fracture pattern, stability of fixation, bone quality, associated soft tissue injuries, and patient compliance. The overarching goals are to protect the repair, restore range of motion, regain strength, and facilitate a safe return to activity.
General Principles
- Protect Fixation: Avoid forces that could jeopardize the integrity of the fracture repair (e.g., uncontrolled weight-bearing, excessive torque).
- Early Motion: Initiate controlled, passive, or active-assisted range of motion (ROM) to prevent stiffness, promote cartilage nutrition, and reduce swelling.
- Gradual Progression: Slowly increase weight-bearing and strengthening exercises based on radiographic healing and clinical stability.
- Pain Management: Address post-operative pain to facilitate participation in therapy.
- DVT Prophylaxis: Continue pharmacological and mechanical prophylaxis as indicated.
Phases of Rehabilitation
Phase 1: Protection and Early Motion (Weeks 0-6)
-
Weight-Bearing:
- Non-Weight-Bearing (NWB): Standard for most unstable or extensively repaired fractures, particularly those with significant metaphyseal comminution or bone grafting. Crutches or walker are used.
- Touch-Down Weight-Bearing (TDWB) or Toe-Touch Weight-Bearing (TTWB): May be initiated for very stable fixation or minimally displaced fractures, allowing foot contact for proprioception but no significant load.
-
Immobilization:
- A hinged knee brace is typically applied post-operatively.
- Initially, the brace may be locked in full extension for transfers and ambulation, protecting the repair.
- Unlocked for controlled ROM exercises.
-
Range of Motion (ROM):
- Continuous Passive Motion (CPM) machine may be used to initiate gentle ROM, usually 0-30 or 0-60 degrees.
- Passive and active-assisted ROM exercises within prescribed limits (e.g., 0-90 degrees by week 4-6). Focus on gentle flexion and extension.
-
Muscle Activation:
- Quadriceps sets (isometric quad contractions).
- Gluteal sets.
- Ankle pumps (to prevent DVT and reduce swelling).
- Swelling Management: Elevation, ice, gentle compression.
- Wound Care: Maintain clean, dry dressings until sutures/staples are removed.
Phase 2: Gradual Weight-Bearing and Strengthening (Weeks 6-12)
-
Weight-Bearing:
- Progressive Weight-Bearing (PWB): Guided by serial radiographs showing signs of healing and clinical assessment of fracture stability. Typically progresses from 25% to 50-75% weight-bearing.
- Continue use of crutches or walker, weaning as strength and balance improve.
-
Range of Motion:
- Continue to increase active and passive ROM, aiming for near full extension and at least 120 degrees of flexion.
- Stationary cycling (no resistance initially) to promote ROM and gentle cardiovascular activity.
-
Strengthening:
- Begin closed-chain exercises (e.g., mini-squats, wall slides, leg press with light resistance) to engage quadriceps and hamstrings in a functional manner.
- Hip abduction/adduction strengthening.
- Proprioception exercises (e.g., single-leg stance on stable surface, weight shifts).
- Gait Training: Focus on restoring a normalized gait pattern, initially with assistive devices, then progressing to unassisted ambulation.
Phase 3: Advanced Strengthening and Return to Function (Weeks 12+)
-
Weight-Bearing:
- Full Weight-Bearing (FWB): Achieved when radiographic union is confirmed and clinical stability is adequate.
-
Strengthening:
- Progressive resistance exercises for quadriceps, hamstrings, and calf muscles.
- Advanced closed-chain exercises (e.g., step-ups, lunges).
- Introduction of plyometric exercises and agility drills for patients aiming to return to higher-demand activities (e.g., sports).
- Sport-specific or work-specific training.
-
Functional Training:
- Balance and proprioception exercises on unstable surfaces.
- Cardiovascular conditioning.
-
Return to Activity:
-
Decision for return to work, recreational activities, or sports is highly individualized and based on:
- Full fracture union confirmed radiographically.
- Restoration of full or near-full pain-free ROM.
- Sufficient muscle strength and endurance (e.g., >80% strength compared to the contralateral limb).
- Excellent dynamic stability and proprioception.
- High-impact activities or contact sports may be restricted for 6-12 months or longer to allow for bone remodeling and soft tissue recovery.
-
Decision for return to work, recreational activities, or sports is highly individualized and based on:
Factors Influencing Rehabilitation Progression:
*
Fracture Severity and Type:
More comminuted or unstable fractures require a slower, more protected progression.
*
Quality of Fixation:
Robust fixation allows for earlier, more aggressive ROM.
*
Bone Quality:
Osteopenic bone may necessitate longer periods of protected weight-bearing.
*
Associated Injuries:
Ligamentous or meniscal repairs may dictate additional restrictions.
*
Patient Compliance:
Adherence to protocol is crucial; non-compliance can lead to complications or delayed recovery.
Summary of Key Literature / Guidelines
The management of tibial plateau fractures has evolved significantly with advancements in imaging, surgical techniques, and implant technology. A critical understanding of foundational literature and current consensus guidelines informs best practices.
1. Importance of Anatomical Reduction and Stable Fixation:
* The primary goal in operative management is the restoration of articular congruity. Classic studies by Schatzker and the AO Foundation have consistently demonstrated that even small residual articular step-offs (>2mm) significantly increase the risk of post-traumatic osteoarthritis.
* Early literature, particularly from the AO group, emphasized the importance of stable internal fixation to allow for early mobilization. Techniques incorporating lag screws for interfragmentary compression and buttress plates for metaphyseal support remain cornerstones of treatment. Locking plate technology has improved stability, particularly in osteopenic bone or comminuted metaphyseal fractures, by providing fixed-angle constructs.
2. Role of Advanced Imaging (CT Scan):
* Consensus guidelines universally recommend pre-operative CT imaging with 3D reconstructions. This is considered indispensable for detailed fracture mapping, identifying occult articular depression, extent of comminution, and planning the optimal surgical approach and hardware placement. Plain radiographs alone are often insufficient to fully characterize complex intra-articular fractures.
3. Surgical Approaches:
* The selection of surgical approach is dictated by the fracture pattern. The anterolateral approach remains standard for most lateral plateau fractures. For bicondylar fractures or those with significant posterior column involvement, dual incisions (e.g., anterolateral and posteromedial) are frequently advocated to provide direct visualization and anatomical reduction of all fragments, minimizing soft tissue stripping. The posteromedial approach specifically addresses fracture lines involving the posteromedial corner, which are often missed with traditional lateral or medial approaches.
4. Bone Grafting:
* The literature consistently supports the use of bone graft (autograft, allograft, or synthetic bone substitutes) to fill metaphyseal defects created by the elevation of depressed articular segments. This provides mechanical support to prevent secondary collapse and promotes osteoinduction/conduction. Autograft (typically from the ipsilateral iliac crest) remains the gold standard, although allografts and synthetic options are widely used, particularly to avoid donor site morbidity.
5. Management of Associated Soft Tissue Injuries:
* A significant body of literature highlights the high incidence of meniscal (lateral > medial) and ligamentous injuries with TPFs. Arthroscopy-assisted reduction and fixation techniques allow for direct visualization and repair of meniscal pathology and assessment of ligamentous stability during the fracture repair. Timely repair of significant meniscal tears (especially bucket-handle or peripheral tears) is crucial to preserve joint function and reduce the risk of PTOA.
6. External Fixation for Damage Control:
* For high-energy TPFs presenting with severe soft tissue swelling, open wounds, or polytrauma, staged management with initial spanning external fixation ("damage control orthopedics") is well-established. This allows for soft tissue recovery, resuscitation of the patient, and minimizes wound complications associated with immediate definitive ORIF in compromised soft tissue envelopes. Definitive ORIF is performed once the "wrinkle sign" is positive and soft tissues are amenable.
7. Rehabilitation Protocols:
* Current evidence supports early, protected range of motion protocols to prevent stiffness and promote cartilage health, while adhering to strict weight-bearing restrictions dictated by fracture stability and bone healing. Gradual progression of weight-bearing and strengthening is critical.
8. Outcomes and Prognostic Factors:
* Long-term outcomes for TPFs are highly variable. Key prognostic factors influencing the development of post-traumatic osteoarthritis include:
* Quality of articular reduction (residual step-off).
* Presence and severity of meniscal and ligamentous injuries.
* Degree of initial soft tissue damage.
* Age and activity level of the patient.
* Compliance with rehabilitation.
* Despite optimal surgical management, a significant percentage of patients will develop varying degrees of post-traumatic osteoarthritis, necessitating future interventions such as osteotomy or total knee arthroplasty.
In summary, the contemporary management of tibial plateau fractures is predicated on accurate pre-operative assessment with CT, meticulous surgical technique aimed at anatomical articular reduction and stable fixation, thoughtful management of associated soft tissue injuries, and diligent post-operative rehabilitation. The ultimate goal remains to restore knee function, preserve joint longevity, and minimize the burden of long-term complications.
You Might Also Like