Neurovascular Island Grafts and the Management of Traumatic Neuromas in the Hand
Key Takeaway
The neurovascular island graft is a critical microsurgical technique used to restore sensibility to essential pinch areas of the hand, particularly the thumb and index finger. By transferring a sensate, vascularized skin paddle from a non-critical donor digit, surgeons can salvage the functional capacity of a "blind" digit. This guide details the indications, preoperative planning, meticulous pedicle dissection, and postoperative sensory re-education required for optimal outcomes.
INTRODUCTION TO SENSORY RESTORATION IN THE HAND
The human hand relies fundamentally on tactile gnosis to perform precise, coordinated motor functions. A digit deprived of sensibility is selectively and unconsciously avoided during use, rendering it functionally amputated despite its physical presence. This phenomenon, often termed the "blind hand" or "blind digit," underscores the principle that motor function is inextricably linked to sensory feedback.
When primary nerve repair or nerve grafting is impossible, or when previous attempts have failed, the restoration of sensibility to critical contact areas—most notably the thumb and the radial aspect of the index finger—becomes a paramount reconstructive challenge. The transfer of a neurovascular island graft provides a reliable, sensate, and vascularized soft-tissue envelope to these critical zones, salvaging the functional utility of the hand.
TRAUMATIC NEUROMAS: PATHOPHYSIOLOGY AND CONTEXT
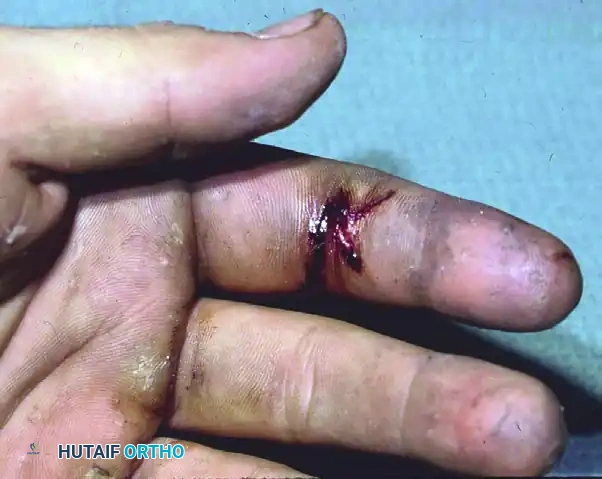
Before addressing sensory reconstruction via tissue transfer, the surgeon must understand the pathology of the injured nerve. Following complete transection or severe crush injury, regenerating axonal sprouts that fail to reach the distal endoneurial tubes form a disorganized, bulbous mass of nerve fibers, Schwann cells, and dense connective tissue—a traumatic neuroma.
In the hand, superficial neuromas are exquisitely painful, often presenting with a hyperactive Tinel’s sign and severe cold intolerance. The pain generated by a neuroma can completely inhibit the use of the affected digit or the entire hand.
CLINICAL PEARL:
The presence of a painful traumatic neuroma must be addressed concurrently with any sensory reconstruction. Simply providing a neurovascular island graft to a distal site will not restore function if a proximal neuroma continues to cause debilitating pain upon contact or movement.
Management of traumatic neuromas typically involves wide excision of the neuroma bulb back to healthy fascicles, followed by relocation of the nerve stump into a deep, protected environment (such as muscle or bone) to prevent mechanical stimulation. Only once the pain generator is neutralized can the surgeon focus on restoring sensibility to the insensate distal skin via a neurovascular island graft.
NEUROVASCULAR ISLAND GRAFTS: PRINCIPLES AND INDICATIONS
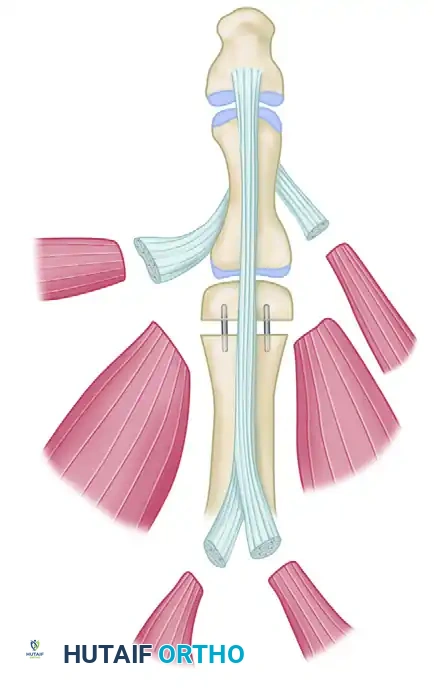
The neurovascular island graft involves the mobilization of a composite island of skin and subcutaneous tissue, pedicled on its native proper digital artery, venae comitantes, and proper digital nerve. This flap is tunneled to a recipient site requiring durable, sensate coverage.
Primary Indications
Transfer of a neurovascular island graft is highly specialized and is generally indicated for:
* Permanent Sensory Deficits: Specifically on the radial side of an otherwise normal index finger, or the critical area of pinch on the distal ulnar aspect of the thumb.
* Osteoplastic Thumb Reconstruction: It is absolutely essential to innervate an osteoplastic reconstruction of the thumb. Without sensate skin, the reconstructed thumb post will be bypassed by the patient during pinch and grasp activities.
* Severe Pulp Loss: Cases where local homodigital flaps are inadequate or unavailable, and cross-finger flaps would provide only insensate coverage.
Preoperative Considerations and Patient Selection
The decision to proceed with a neurovascular island graft is complex. The surgeon must meticulously evaluate the following six factors:
- Dominance of the Involved Hand: Sensory demands are significantly higher in the dominant hand, particularly for fine motor tasks like writing or manipulating small objects.
- Palmar Scarring: The presence of extensive scarring in the palm, through which an incision must be made for channeling the neurovascular bundle, increases the risk of iatrogenic injury to the pedicle and complicates the tunneling process.
- Status of the Ipsilateral Ulnar Nerve: Because the donor site is typically innervated by the ulnar nerve (e.g., the ulnar aspect of the ring finger), a concomitant ulnar nerve palsy is an absolute contraindication, as the donor tissue would already be insensate.
- Condition of the Opposite Hand: In bilateral severe hand trauma, the threshold for complex sensory reconstruction is lowered to maximize the patient's overall independence.
- Age of the Patient: Younger patients exhibit superior cortical plasticity, allowing for better sensory reorientation (cortical remapping) of the transferred flap.
- Experience of the Surgeon: This is a technically demanding procedure requiring microsurgical tissue handling, precise anatomical knowledge, and meticulous dissection.
SURGICAL ANATOMY AND DONOR SITE SELECTION
Early descriptions of this operation suggested transferring skin solely from the ulnar side of the distal phalanx of the ring finger. However, contemporary longitudinal experience dictates a broader approach.
The Ideal Donor Site
The ulnar aspect of the ring finger remains the workhorse donor site. It is chosen because it is a non-contact, non-pinch surface. The radial aspects of the digits (especially the index and middle fingers) and the ulnar aspect of the little finger are critical for pinch and ulnar border stability, respectively, and should be spared.
Flap Design Modifications
Current evidence strongly supports harvesting most of the skin from the entire ulnar side of the donor finger, rather than just the distal phalanx.
* Advantage: This larger transfer significantly increases the area of sensitive skin on the recipient digit.
* Donor Morbidity: It causes no wider functional sensory loss on the donor digit than a smaller flap would. The larger full-thickness skin graft (FTSG) required to cover the donor area is generally of little consequence and heals with acceptable morbidity.
OPERATIVE TECHNIQUE: STEP-BY-STEP
Meticulous surgical technique is the primary determinant of flap survival. While frank necrosis of the transferred neurovascular island pedicle graft is rare, even temporary impairment of the microcirculation (venous congestion or arterial spasm) can cause permanent sensory deficits in the graft, resulting in a partial or complete functional failure of the operation.
1. Preparation and Incision
- The procedure is performed under regional or general anesthesia with a pneumatic tourniquet.
- The recipient site (e.g., the ulnar aspect of the thumb) is prepared first. Scar tissue is excised, and the defect is templated.
- The template is transferred to the ulnar aspect of the ring finger. The flap is designed using a mid-lateral approach, ensuring the volar margin does not cross the flexion creases perpendicularly.
2. Pedicle Dissection
The dissection of the neurovascular bundle is the most critical phase of the operation.
SURGICAL WARNING:
The bundle must be dissected from proximally to distally. This antegrade approach allows the surgeon to identify and properly manage any anatomical anomalies of the common digital vessels or the superficial palmar arch before committing to the flap harvest.
- A zigzag or Brunner-type incision is made in the palm to expose the common digital artery and nerve in the third web space.
- The proper digital artery to the radial side of the little finger is identified, ligated, and divided, thereby mobilizing the common digital artery to supply only the ulnar aspect of the ring finger.
- The common digital nerve is carefully split longitudinally (intraneural dissection) to separate the fascicles supplying the ring finger from those supplying the little finger. This must be done under loupe or microscopic magnification to avoid axonal injury.
3. Preservation of Venous Drainage
A common pitfall in early iterations of this procedure was skeletonizing the artery and nerve, leading to profound venous congestion.
PITFALL:
The neurovascular bundle should never be completely freed from the surrounding fatty tissue, especially at the base of the finger.
- The venous drainage of the island flap relies entirely on the microscopic venae comitantes and the perivascular areolar tissue surrounding the proper digital artery.
- The bundle must be transferred along with a generous cuff of attached fibrofatty tissue to preserve these fragile venous channels.
4. Tunneling and Inset
- A subcutaneous tunnel is created from the proximal palmar incision to the recipient site on the thumb or index finger.
- The tunnel must be exceptionally wide—easily accommodating the surgeon's index finger—to prevent any compression or kinking of the pedicle.
- The flap is gently passed through the tunnel. The surgeon must verify that the pedicle is not twisted (a "barber pole" deformity).
- The tourniquet is deflated prior to final inset to confirm robust arterial inflow and adequate venous outflow.
- The flap is inset with non-absorbable monofilament sutures using a tension-free technique.
5. Donor Site Closure
The donor defect on the ring finger is covered with a full-thickness skin graft, typically harvested from the hypothenar eminence, the groin, or the medial arm. Tie-over bolsters are applied to ensure graft adherence.
SENSORY OUTCOMES AND CORTICAL PLASTICITY
Surgeons must manage patient expectations rigorously. It is a fundamental neurophysiological truth that sensibility in the neurovascular island graft is never normal after transfer.
Objective Sensory Findings
When grafts are critically examined months or years after surgery, objective sensibility testing (e.g., Semmes-Weinstein monofilaments, static two-point discrimination) is invariably abnormal.
* Hyperesthesia: More than 50% of patients report persistently hyperesthetic skin. The transferred skin often feels overly sensitive or dysesthetic upon initial contact.
* Sensory Reorientation: All patients initially lack precise sensory reorientation. When the transferred skin on the thumb is touched, the patient's somatosensory cortex registers the stimulus as originating from the donor ring finger (the phenomenon of "false localization").
Cortical Remapping
Although sensibility need not be perfectly normal to achieve a good functional result, sensory reorientation is crucial for seamless motor integration.
* Reorientation relies on neuroplasticity—the brain's ability to remap the sensory homunculus.
* This remapping improves progressively with time and, most importantly, with active, purposeful use of the reconstructed part.
* Younger patients achieve cortical reorientation much faster and more completely than older adults.
POSTOPERATIVE PROTOCOL AND REHABILITATION
The success of a neurovascular island graft extends far beyond the operating room; it requires a dedicated, structured postoperative rehabilitation program.
Phase 1: Protection and Viability (Weeks 0-3)
- The hand is immobilized in a bulky, non-compressive splint. The wrist is placed in neutral, with the thumb in slight palmar abduction to remove tension from the pedicle.
- Strict elevation is maintained to assist venous drainage.
- Flap monitoring (capillary refill, turgor, color, and temperature) is performed routinely in the first 48 to 72 hours.
- Smoking and the use of vasoconstrictive agents are strictly prohibited.
Phase 2: Mobilization and Early Sensory Re-education (Weeks 3-6)
- Sutures are removed at 14 to 21 days.
- Gentle active range of motion (AROM) of all digits is initiated to prevent tendon adhesions and joint stiffness.
- Phase 1 Sensory Re-education: Begins once the flap is stable. The patient is instructed to look at the reconstructed thumb while touching it with the contralateral hand. This visual-tactile coupling helps the brain associate the tactile stimulus with the new anatomical location, accelerating cortical remapping.
Phase 3: Advanced Integration (Weeks 6+)
- Phase 2 Sensory Re-education: Involves blindfolded object recognition (stereognosis training). The patient practices identifying different textures (velcro, silk, sandpaper) and shapes (coins, keys) using only the reconstructed digit.
- Desensitization techniques (tapping, massage, fluidotherapy) are employed to combat the expected hyperesthesia.
- Strengthening and return to heavy functional use are gradually permitted as tolerated.
CONCLUSION
The neurovascular island graft remains a highly elegant and functionally restorative procedure for the insensate, "blind" digit. While the operation demands exacting microsurgical technique—particularly in the preservation of perivascular venous drainage and the antegrade dissection of the pedicle—the functional dividends are profound. By understanding the limitations of sensory reorientation and committing to rigorous postoperative sensory re-education, the orthopaedic surgeon can successfully reintegrate a severely injured digit back into the functional matrix of the human hand.
You Might Also Like