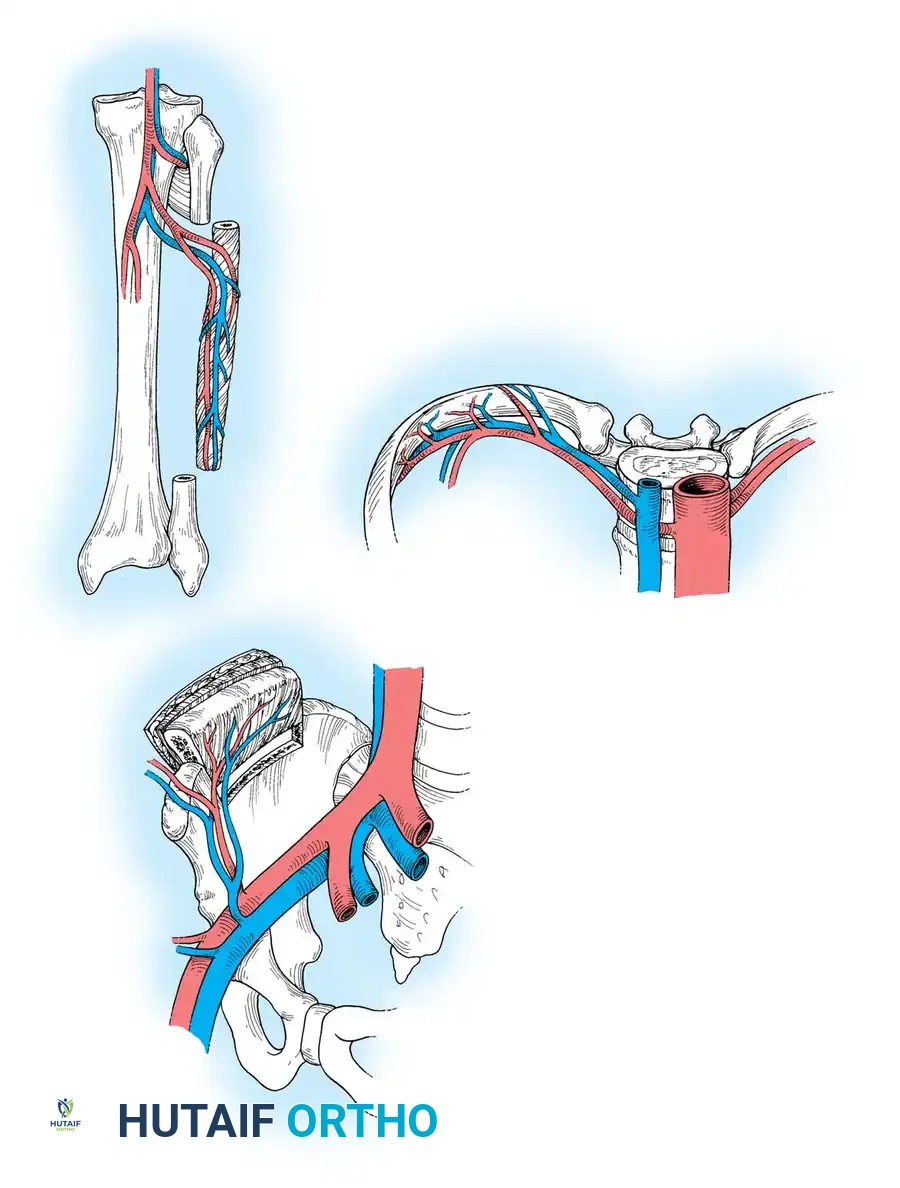
Revascularization and Salvage Techniques in Hand Surgery
Key Takeaway
Revascularization of the partially amputated or devitalized hand requires meticulous assessment of tissue ischemia. While management parallels replantation, revascularization tolerates longer ischemic intervals. For distal fingertip amputations where microvascular anastomosis is impossible, salvage procedures such as the ipsilateral palmar pocket technique or arteriovenous anastomosis offer viable alternatives to preserve digit length, function, and sensation while minimizing donor-site morbidity and joint stiffness.
PRINCIPLES OF HAND AND DIGIT REVASCULARIZATION
Partial amputation or severe devitalization of tissues resulting from serious vascular interruption frequently occurs without the complete detachment of the affected part. While some of these partially attached parts with impaired circulation may ultimately survive through collateral flow or venous congestion tolerance, persistent ischemia is a critical threat. If left unaddressed, chronic ischemia initiates a cascade of fibrotic changes that later manifest as disabling cold intolerance, profound atrophy, and severe contracture of the intrinsic muscles of the hand.
The clinical hallmark of a digit with critically impaired circulation is an extremely slow return of normal pink color following blanching by pressure (prolonged capillary refill time), often accompanied by loss of turgor and diminished pulp temperature.
The surgical management of these complex hand injuries is essentially analogous to that of complete replantation. However, because there is often a residual bridge of tissue providing minimal venous drainage or lymphatic outflow, a longer interval from the time of the accident to the microvascular anastomosis of the vessels may be tolerated. Furthermore, unlike multi-digit replantations that often require a two-team approach to minimize ischemia time, revascularization procedures can frequently be executed efficiently by a single highly trained microsurgical team.
💡 Clinical Pearl: Assessing Viability
Do not rely solely on color. A congested, cyanotic digit may have adequate arterial inflow but compromised venous outflow, whereas a pale, cool digit indicates arterial insufficiency. Use a handheld Doppler probe to assess the digital arteries, and perform a meticulous pinprick test at the sterile matrix to evaluate the nature of bleeding (bright red vs. dark venous blood).
Wrist-Level Arterial Injuries
When major vascular interruptions occur at the level of the wrist—specifically involving the severance of the radial and ulnar arteries—the fundamental rule of hand perfusion dictates that at least one of these major vessels must be repaired to restore the superficial and deep palmar arches.
If the viability of the hand remains questionable after the repair of a single artery (e.g., due to an incomplete superficial palmar arch or extensive zone of injury), both the radial and the ulnar arteries must be meticulously repaired. Restoring dual inflow significantly reduces the risk of intrinsic muscle necrosis and subsequent Volkmann-like ischemic contractures of the hand.
SALVAGE TECHNIQUES FOR DISTAL FINGERTIP AMPUTATIONS
Distal fingertip amputations (Ishikawa Subzones I and II) present a unique microsurgical challenge. In these distal zones, the digital arteries arborize into a subdermal plexus, and the dorsal veins become too diminutive for standard microvascular anastomosis. When microvascular repair is technically impossible, alternative salvage techniques must be employed to preserve digit length, maintain tactile sensation, and avoid the morbidity of terminal amputation.
The Evolution of the "Pocket Technique"
To salvage composite amputations of the distal fingertip, Brent originally described the classic "pocket technique." This procedure involves aggressively débriding and deepithelializing the amputated part, reattaching it to the stump as a composite graft, and subsequently burying the entire construct in a subcutaneous pocket created on the contralateral chest wall. The digit remains buried for 3 weeks to allow for neovascularization from the highly vascularized chest wall bed. Once angiogenesis is established, the digit is removed from the pocket, and the viable tip is skin grafted.
While innovative, this technique has undergone several modifications due to inherent limitations:
* Abdominal Pockets: Lee et al. modified the procedure by utilizing an abdominal pocket, which provided a thicker subcutaneous bed but still required awkward immobilization.
* Anatomic Limitations: Muneuchi et al. critically evaluated the pocket technique and reported poor results in a series of seven fingers. They concluded that the technique is highly unreliable and strictly do not recommend it for injuries occurring at or proximal to the lunula. The tissue volume at this proximal level exceeds the angiogenic capacity of the pocket, leading to central ischemic necrosis before a new blood supply can be established.
⚠️ Surgical Warning: The Lunula Boundary
Attempting a pocket technique salvage for amputations proximal to the lunula carries an unacceptably high rate of failure. The metabolic demand of the composite tissue (bone, nail bed, pulp) outpaces the rate of capillary ingrowth from the pocket, resulting in liquefactive necrosis and severe infection.
The Ipsilateral Palmar Pocket Modification
To circumvent the significant morbidity associated with chest or abdominal pockets—namely, severe shoulder and elbow stiffness resulting from 3 weeks of rigid immobilization—Arata et al. introduced a brilliant modification: utilizing the ipsilateral palm as the pocket site.
By burying the deepithelialized fingertip into the thenar or hypothenar eminence of the same hand, the patient retains full range of motion of the shoulder and elbow. In their seminal series of 16 patients, complete survival of the composite graft was achieved in 13 patients, with the remaining three exhibiting only partial necrosis that healed by secondary intention.
Arteriovenous Anastomosis (Venous Perfusion)
Another sophisticated technique described for replanting distal fingertip amputations when arterial targets are unavailable involves the creation of an arteriovenous (AV) anastomosis.
Described by Yabe et al., this technique involves anastomosing a volar radial vein of the amputated part to the proximal digital artery of the stump. This creates a reverse-flow perfusion model where arterial blood is driven into the venous system of the fingertip. Because the venous valves initially impede retrograde flow, the high arterial pressure eventually renders them incompetent, allowing perfusion of the capillary beds.
To prevent catastrophic venous congestion (as the normal venous outflow tracts are now being used for arterial inflow), venous drainage is accomplished by making a transverse tip incision. This allows the digit to continuously "bleed out" the deoxygenated blood. Yabe et al. reported successful salvage in three out of four fingertip replantations using this method, with only one developing partial necrosis.
SURGICAL TECHNIQUE: IPSILATERAL PALMAR POCKET PROCEDURE (ARATA ET AL.)
The ipsilateral palmar pocket technique is a highly reliable, two-stage procedure for distal fingertip salvage. Strict adherence to the surgical steps is paramount to ensure graft survival and prevent donor site morbidity.
Stage I: Preparation and Implantation
1. Anesthesia and Preparation
* Administer a regional block (wrist block or upper arm brachial plexus block) to ensure profound anesthesia and sympathectomy, which maximizes vasodilation.
* Apply a pneumatic tourniquet to the upper arm.
* Copiously irrigate and wash both the amputated part and the amputation stump with normal saline.
* Carefully extract and remove the nail plate. This reduces the metabolic demand of the tissue, prevents subungual infection, and exposes the sterile matrix for deepithelialization.
2. Skeletal Stabilization
* Meticulously reduce the fractured bone segments.
* Stabilize the distal phalanx using fine Kirschner wires (0.028 or 0.035 inch).
* Crucial Step: Cut the K-wires as short as possible, ensuring they do not protrude significantly. Protruding wires will damage the delicate palmar pocket tissues and cause severe pain during the 3-week implantation period.
3. Reattachment and Deepithelialization
* Reattach the amputated part to the amputation stump. No vascular anastomosis is performed at this stage.
* Using a No. 15 scalpel blade, carefully deepithelialize the amputated part down to the mid-dermal layer.
* Surgical Rationale: Deepithelialization must be precise. Removing the epidermis prevents the formation of inclusion cysts within the pocket, while preserving the deep dermis maintains the adnexal structures necessary for future re-epithelialization and exposes the dermal capillary plexus to encourage rapid angiogenesis from the palmar bed.
4. Pocket Creation and Insertion
* Identify an appropriate site on the ipsilateral palm (typically the thenar eminence for radial digits or the hypothenar eminence for ulnar digits) that allows the injured finger to flex naturally into the palm without excessive tension.
* Make a 2-cm transverse incision in the palmar skin.
* Using blunt dissecting scissors, undermine the subcutaneous layer to form a vascularized pocket. Ensure the pocket is wide enough to accommodate the digit without compressing it.
* Insert the reattached, deepithelialized part into the palmar pocket.
* Suture the injured finger to the palmar skin approximately 2 mm proximal to the reattachment level. This anchoring suture is critical to prevent the inserted digit from inadvertently pulling out of the pocket during sleep or accidental movement.
5. Postoperative Dressing
* Apply a light, non-adherent compressive gauze dressing.
* Do not apply a rigid splint. Allowing micro-motion prevents severe joint stiffness, and the natural resting posture of the hand keeps the digit securely within the pocket.
🛑 Pitfall: Pocket Tension
If the palmar pocket is created too superficially or is too tight, the resulting pressure will cause ischemic necrosis of both the implanted digit and the overlying palmar skin. The pocket must be situated in the compliant subcutaneous fat layer.
Stage II: Release and Rehabilitation
1. Division and Release
* The second operation is scheduled 16 to 20 days after the initial implantation. By this time, robust neovascularization from the palmar bed into the dermal plexus of the amputated part has occurred.
* Under local anesthesia, carefully incise the anchoring sutures and gently remove the replanted part from the palmar pocket.
* Meticulously irrigate and suture the palmar skin incision.
2. Wound Care and Mobilization
* The newly released fingertip will appear raw and deepithelialized. Apply a wet-to-moist dressing (e.g., saline-soaked gauze or a non-adherent hydrogel dressing) to promote a moist wound-healing environment.
* Immediately encourage active range-of-motion exercises of the injured finger to glide the flexor and extensor tendons and restore joint kinematics.
3. Final Maturation
* At approximately 2 weeks following the second operation, secondary epithelialization of the fingertip should be complete.
* The replanted part will gradually gain structural stability, and sensory re-education can commence.
POSTOPERATIVE PROTOCOLS AND COMPLICATION MANAGEMENT
Whether managing a major wrist-level revascularization or a distal fingertip salvage, the postoperative environment must be strictly controlled to optimize perfusion.
Environmental and Pharmacological Management
- Temperature Control: The patient's room must be kept warm (above 75°F / 24°C) to prevent vasospasm. The patient should be instructed to avoid smoking and caffeine, as both are potent vasoconstrictors.
- Positioning: For standard revascularizations, the hand is typically elevated slightly above heart level to promote venous drainage while maintaining adequate arterial inflow.
- Anticoagulation: Depending on the extent of the vascular injury and the quality of the anastomosis, a regimen of intravenous Heparin, low-molecular-weight dextran, or daily aspirin (81 mg - 325 mg) may be instituted.
- Leech Therapy (Hirudotherapy): In cases of arteriovenous anastomosis (Yabe technique) or severe venous congestion where the transverse tip incision ceases to bleed adequately, medicinal leeches (Hirudo medicinalis) may be applied. The leech saliva contains hirudin (a direct thrombin inhibitor) and a histamine-like vasodilator, which promotes continuous oozing and relieves congestion until venous collateral circulation develops (typically 5 to 8 days). Prophylactic antibiotics (e.g., Ciprofloxacin or Trimethoprim-Sulfamethoxazole) must be administered to prevent Aeromonas hydrophila infection.
Monitoring and Intervention
Continuous monitoring of the revascularized digit is mandatory for the first 72 hours. Objective monitoring tools such as continuous surface temperature probes or laser Doppler flowmetry are highly recommended. A drop in surface temperature of more than 2°C compared to an adjacent normal digit, or an absolute temperature falling below 30°C, is a highly sensitive indicator of impending vascular thrombosis and warrants immediate clinical evaluation and potential surgical re-exploration.
You Might Also Like