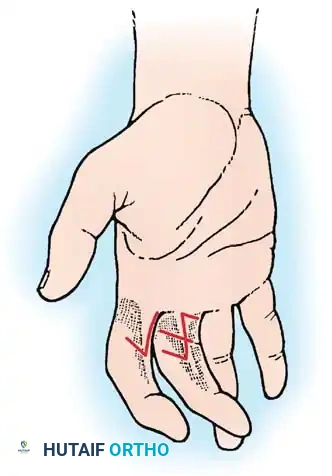
Centralization of the Hand: Transverse Ulnar Incision Technique
Key Takeaway
Centralization of the hand using a transverse ulnar incision is a foundational technique for correcting radial longitudinal deficiency. Pioneered by Manske, McCarroll, and Swanson, this approach addresses the complex pathoanatomy of the radial clubhand by repositioning the carpus over the distal ulna. This guide details the surgical indications, precise soft-tissue balancing, carpal preparation, and Kirschner wire fixation required to achieve stable, long-term alignment while preserving ulnar growth potential.
Introduction to Radial Longitudinal Deficiency and Centralization
Radial longitudinal deficiency (RLD), historically referred to as radial clubhand, represents a complex spectrum of congenital upper extremity anomalies characterized by hypoplasia or complete aplasia of the radius and its associated preaxial soft-tissue structures. The resulting pathoanatomy is profound: the unsupported carpus subluxates radially and volarly, the ulna is typically shortened and bowed, and the extrinsic flexor and extensor tendons become secondary deforming forces.
Centralization of the hand over the distal ulna remains the cornerstone of surgical reconstruction for Bayne and Klug Type III (partial absence of the radius) and Type IV (total absence of the radius) deficiencies. The primary goals of centralization are to correct the severe radial deviation, balance the deforming soft-tissue forces, stabilize the wrist to improve digital flexor mechanics, and maximize the functional length of the upper extremity.
The technique described by Manske, McCarroll, and Swanson utilizing a transverse ulnar incision is particularly advantageous. It directly addresses the redundant, bulbous soft-tissue mass on the ulnar aspect of the wrist, provides excellent exposure for ulnar-sided tendon transfers, and utilizes the skin closure itself as a dynamic tether to maintain ulnar alignment.

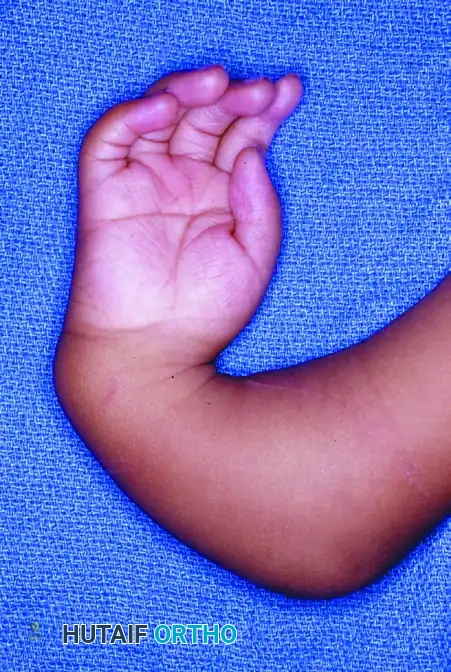
Preoperative clinical presentation of a severe radial clubhand deformity, demonstrating the characteristic radial deviation, volar subluxation, and prominent ulnar styloid region.
Indications and Preoperative Optimization
Patient Selection
Surgical intervention is typically performed between 6 and 12 months of age. Operating within this window allows for correction before the deforming soft-tissue contractures become rigidly fixed and takes advantage of the remodeling potential of the pediatric carpus.
Indications:
* Bayne and Klug Type III and IV radial longitudinal deficiency.
* Adequate elbow flexion. (A stiff, extended elbow is a strict contraindication to centralization, as the patient relies on the radial deviation of the hand to reach the mouth for feeding).
* Failure of conservative management (serial casting/splinting) to maintain carpal alignment.
Preoperative Soft-Tissue Management
Successful centralization relies heavily on preoperative soft-tissue stretching. Serial casting or splinting should begin shortly after birth to stretch the tight radial structures (radial collateral ligament, brachioradialis, and radial wrist flexors/extensors). In severe, neglected cases, or in older children, preliminary soft-tissue distraction using a uniplanar or multiplanar external fixator may be required prior to formal open centralization to prevent excessive compressive forces on the distal ulnar physis during reduction.
⚠️ Surgical Warning: The Distal Ulnar Physis
The distal ulnar physis is the primary growth center for the forearm in patients with RLD. Excessive compression during carpal reduction, or direct iatrogenic injury during surgical preparation, will result in premature physeal arrest, exacerbating the already severe forearm shortening characteristic of this condition.
Surgical Anatomy and Biomechanics
The transverse ulnar approach exploits the unique pathoanatomy of the radial clubhand. As the hand deviates radially, a redundant fold of skin and subcutaneous fat develops over the distal ulna. By utilizing a transverse incision across this "bulbous mass," the surgeon can excise the excess tissue. When the wound is closed longitudinally (or simply approximated after wedge excision), the skin envelope itself acts as a tension band, resisting recurrent radial deviation.
Furthermore, the extensor carpi ulnaris (ECU) and the hypothenar musculature are often displaced or mechanically disadvantaged. Advancing the ECU distally and the hypothenar origin proximally creates a dynamic ulnar-sided muscular tether, counteracting the strong radial pull of the anomalous preaxial musculature.
Surgical Technique: Step-by-Step Guide
1. Positioning and Incision
The patient is placed supine with the affected upper extremity extended on a radiolucent hand table. A well-padded pediatric pneumatic tourniquet is applied to the proximal arm.
- Incision Design: Begin the incision just radial to the midline on the dorsum of the wrist, precisely at the level of the distal ulna.
- Proceed ulnarward in a transverse direction, extending to a point radial to the pisiform at the volar wrist crease.
- Pass the incision directly through the bulbous soft-tissue mass on the ulnar side of the wrist. This will require incising a considerable volume of redundant fat and subcutaneous tissue.
2. Superficial Dissection and Nerve Preservation
As the subcutaneous tissues are divided, meticulous hemostasis is maintained. The anatomy in RLD is highly variable, and standard neurovascular landmarks are often distorted.
- Ulnar Nerve Identification: Identify and meticulously preserve the dorsal sensory branch of the ulnar nerve. In the radial clubhand, this nerve is often found deep in the subcutaneous tissue, lying in close proximity to the extensor retinaculum. It may be stretched over the prominent distal ulna.
- Volar Structures: It is generally not necessary to formally identify or dissect the main ulnar artery or the volar ulnar nerve trunk on the volar aspect of the wrist, provided the dissection remains strictly within the defined ulnar and dorsal zones.
3. Deep Exposure and Tendon Management
Once the superficial tissues are cleared, the deep fascial layers and musculotendinous units are addressed to mobilize the carpus.
- Retinaculum and Muscle Origins: Expose the extensor retinaculum and the base of the hypothenar muscles.
- ECU Mobilization: Identify the extensor carpi ulnaris (ECU) tendon at its insertion on the base of the fifth metacarpal. Dissect it free from its sheath, detach it from its insertion, and retract it proximally. Tag the tendon with a non-absorbable suture for later transfer.
- EDC Retraction: Identify the extensor digitorum communis (EDC) tendons. Retract them radially to protect them and to expose the dorsal and ulnar aspects of the wrist capsule.
- Capsulotomy: Incise the wrist capsule transversely. This exposes the distal ulna and the ulnar aspect of the carpus.
4. Carpal Preparation and Notch Creation
In the infant, the carpal bones are entirely cartilaginous, presenting as a confluent, unossified mass deep in the wound on the radial side of the ulna.
- Identifying the Articulation: The carpoulnar junction is most easily and safely identified by dissecting from proximal to distal along the radial side of the distal ulna.
- Avoid Intercarpal Joints: Do not mistake one of the intercarpal articulations (e.g., the lunocapitate joint) for the carpoulnar junction. Entering an intercarpal joint will destabilize the carpus and lead to a suboptimal centralization.
- Creating the Notch: Once the true proximal carpal row is defined, excise a square segment from the midportion of the cartilaginous carpal mass. This notch should measure approximately 1 cm in width and depth, designed specifically to accommodate the squared-off distal ulna. Typically, this involves excising portions of the lunate and capitate anlagen.
💡 Clinical Pearl: Carpal Resection
The depth of the carpal notch is a delicate balance. It must be deep enough to provide intrinsic bony stability to the distal ulna, but not so deep that it completely obliterates the midcarpal joint or compromises the vascularity of the remaining carpal cartilages.
5. Ulnar Preparation
The distal ulna must be prepared to seat congruently within the newly created carpal notch.
- Soft Tissue Clearance: Dissect the distal ulnar epiphysis free from the adjacent adherent soft tissues.
- Squaring the Epiphysis: Carefully square off the distal ulnar epiphysis by shaving the cartilage perpendicular to the long axis of the ulnar shaft.
- Physeal Protection: This shaving must be strictly limited to the articular cartilage. Absolute care must be taken to avoid any injury to the distal ulnar physis or its attached perichondrial ring.
6. Reduction and Kirschner Wire Fixation
With the carpus and ulna prepared, the hand is centralized.
- Reduction: Place the squared-off distal ulna directly into the prepared carpal defect. Ensure the hand is neutrally rotated and aligned with the forearm.
- Pin Placement: Stabilize the reduction with a smooth, stout Kirschner wire (typically 0.045 or 0.062 inches, depending on the child's size).
- Retrograde/Antegrade Technique: In practice, this is most reliably accomplished by passing the Kirschner wire proximally down the medullary canal of the distal ulna to emerge at the olecranon. (If the ulna is severely bowed, the wire may need to exit the midshaft cortex).
- Once the wire exits proximally, the drill is moved to the proximal end of the wire. The hand is held in perfect centralization, and the wire is driven distally across the carpal notch, through the carpus, and into the medullary canal of the third metacarpal.
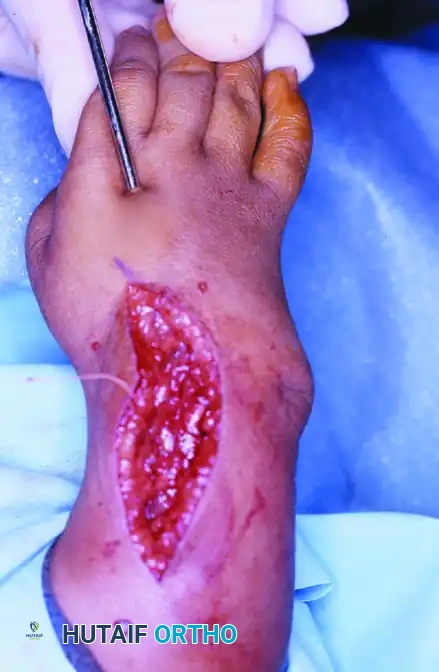
Intraoperative photograph demonstrating the centralized hand stabilized with a longitudinal Kirschner wire passing through the third metacarpal, carpus, and into the ulnar shaft.
- Pin Management: Cut the proximal end of the Kirschner wire beneath the skin at the olecranon to prevent pin-track infections and allow for prolonged retention.
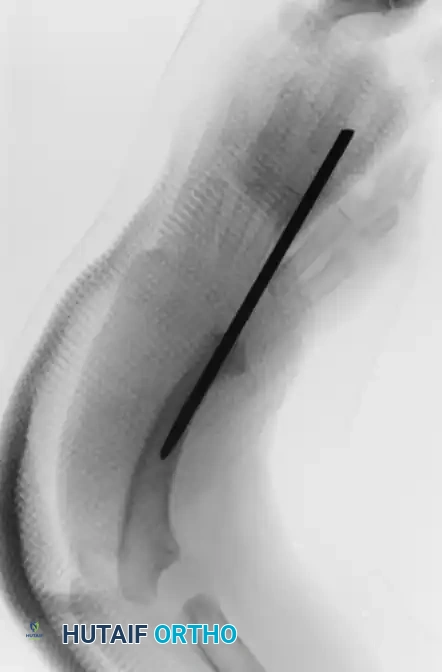
Postoperative radiograph confirming the correction of the deformity. The smooth Kirschner wire maintains the alignment of the third metacarpal, the carpal mass, and the distal ulna.
7. Soft-Tissue Balancing and Tendon Transfers
Bony alignment alone is insufficient; dynamic soft-tissue balancing is mandatory to prevent recurrence.
- Capsulorrhaphy: Stabilize the ulnar side of the wrist by tightly imbricating the redundant dorsal and ulnar capsule. Alternatively, suture the distal capsule directly to the periosteum of the distal ulnar shaft. If the distal capsule is insufficient, pass heavy absorbable sutures directly through the cartilaginous carpal bones and anchor them to the ulnar periosteum.
- ECU Advancement: Obtain critical dynamic stabilization by advancing the previously tagged extensor carpi ulnaris (ECU) tendon distally. Reattach it under tension to the base of the fourth or fifth metacarpal. This converts the ECU into a strong ulnar deviator and dorsiflexor.
- Hypothenar Advancement: Advance the origin of the hypothenar musculature proximally and suture it securely to the ulnar shaft periosteum. This provides an additional volar-ulnar stabilizing force.
8. Closure
- Tissue Excision: Excise the remaining bulbous excess of skin and subcutaneous fat from the ulnar incision margins.
- Skin Suture: Close the skin meticulously. The excision of this wedge of tissue not only results in a highly pleasing cosmetic contour but inherently tightens the ulnar skin envelope, acting as a static restraint to help stabilize the hand in the corrected ulnar position.
Postoperative Protocol and Rehabilitation
Rigid postoperative immobilization is critical to allow the capsulorrhaphy and tendon transfers to heal securely.
- Immediate Postoperative Phase (0-6 Weeks): The wrist and forearm are immobilized in a well-padded, long-arm plaster cast. The elbow is typically included to control forearm rotation and prevent the child from pulling the cast off. The hand is held in neutral to slight ulnar deviation.
- Intermediate Phase (6-12 Weeks): At 6 weeks, the plaster cast is removed. The arm is transitioned into a custom-molded, removable Orthoplast splint.
- Hardware Removal: The intramedullary Kirschner wire is typically removed in the operating room or clinic between 6 to 12 weeks postoperatively, depending on the stability of the soft tissues and radiographic evidence of carpal seating.
- Long-Term Management: Children are strongly encouraged to wear the Orthoplast splint at night (and during high-risk activities) until they reach skeletal maturity. The natural history of RLD involves a constant soft-tissue pull toward radial deviation; prolonged splinting is the most effective method to mitigate recurrence.
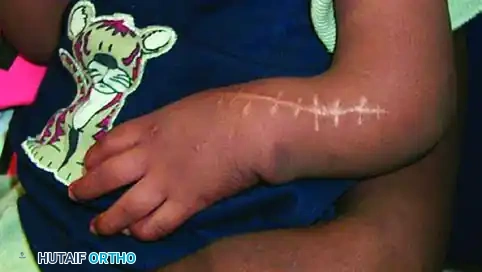
Clinical photograph taken one year after surgery. The transverse ulnar incision has healed with a cosmetically pleasing scar, and the hand remains well-aligned over the distal ulna.
Complications and Pitfalls
Despite meticulous surgical technique, centralization for radial clubhand carries a high rate of long-term complications, primarily due to the relentless underlying biology of the deformity.
- Recurrent Radial Deviation: This is the most common complication. It occurs due to inadequate initial soft-tissue release, failure of the ulnar tendon transfers, or poor compliance with postoperative splinting. If recurrence is severe and interferes with function, revision centralization or eventual wrist arthrodesis (after skeletal maturity) may be required.
- Physeal Arrest of the Distal Ulna: Iatrogenic injury to the distal ulnar physis during carpal notch preparation or from excessive compression will stunt the already limited growth of the forearm. Surgeons must respect the cartilaginous anlage and avoid aggressive resection.
- Pin Migration or Breakage: The longitudinal K-wire can migrate proximally or distally. Cutting the pin beneath the skin at the olecranon reduces the risk of infection and accidental extraction. If the pin breaks within the medullary canal, it can often be left in place unless it causes symptomatic prominence.
- Stiffness: While centralization improves alignment, it inherently reduces wrist range of motion. Parents must be counseled preoperatively that the goal is a stable, functional, and cosmetically acceptable hand, not a wrist with normal kinematics.
You Might Also Like